CARDIOVASCULAR SURGERY PATIENTS PULMONARY REHAB Jamie Luecke APN

CARDIOVASCULAR SURGERY PATIENTS & PULMONARY REHAB Jamie Luecke, APN, CNP Nurse Practitioner Cardiovascular and Thoracic Surgery

PRESENTATION OVERVIEW q. Cardiovascular surgeons and supporting teams q. Overview of PAD, carotid disease, CAD, aortic disease q. Overview of some imaging done on Cardiovascular patients q. Overview of surgical interventions done by CVS team q. Barriers to cardiovascular patients in pulmonary rehab

CARDIOVASCULAR TEAM Vascular Surgery Team Surgeon s: • Dr. Wheatley • Dr. Beeman • Dr. Osborne • • • APP team OR team IR team Nursing team: CT 6 B, CVICU, Clinic Ancillary Team: therapy, respiratory, social services, Cardiothoracic Surgery Team Surgeons : • Dr. Geiss • Dr. Clancy • Dr Derrick • • APP team OR team Nursing team: CT 6 B, CVICU, Clinic Ancillary Team: therapy, respiratory, social services, chaplain

CARDIOVASCULAR SURGERIES Vascular Surgeries q. Abdominal Aortic Aneurysm repair Endovascular Open q. Descending Aortic Aneurysm or Dissection Repair q. Venous Procedures q. Permanent Dialysis Access Arteriovenous fistula or graft q. Carotid Endarterectomy Carotid stenting q. PAD-Peripheral Arterial Disease Femoral-popliteal bypass Femoral-femoral bypass Aorta-bi-femoral bypass Cardiothoracic Surgeries q. CABG-coronary artery bypass q. MVR-mitral valve repair or replacement q. AVR-aortic valve replacement TAVR q Ascending Thoracic Aortic Aneurysm or Dissection Repair q Pneumonectomy q Thoracotomy q Chest tube insertion
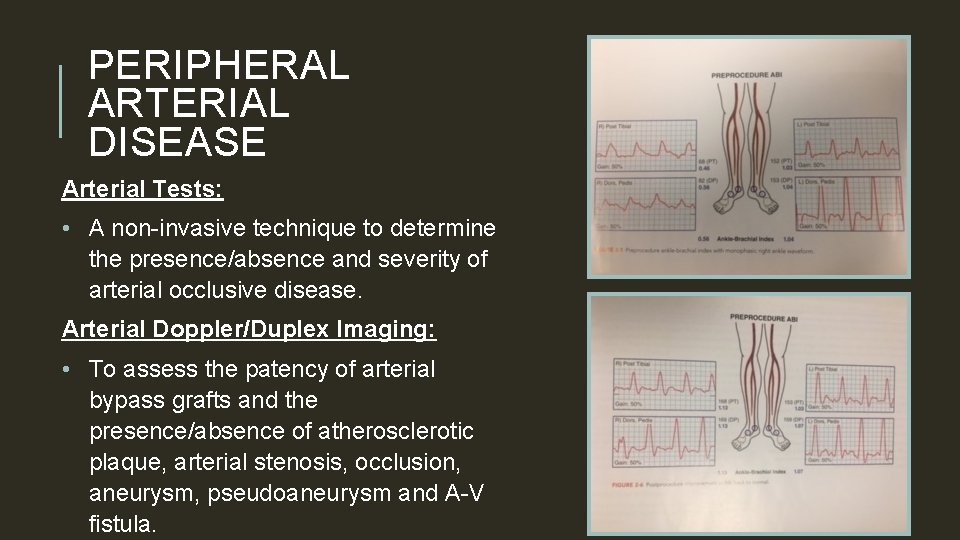
PERIPHERAL ARTERIAL DISEASE Arterial Tests: • A non-invasive technique to determine the presence/absence and severity of arterial occlusive disease. Arterial Doppler/Duplex Imaging: • To assess the patency of arterial bypass grafts and the presence/absence of atherosclerotic plaque, arterial stenosis, occlusion, aneurysm, pseudoaneurysm and A-V fistula.
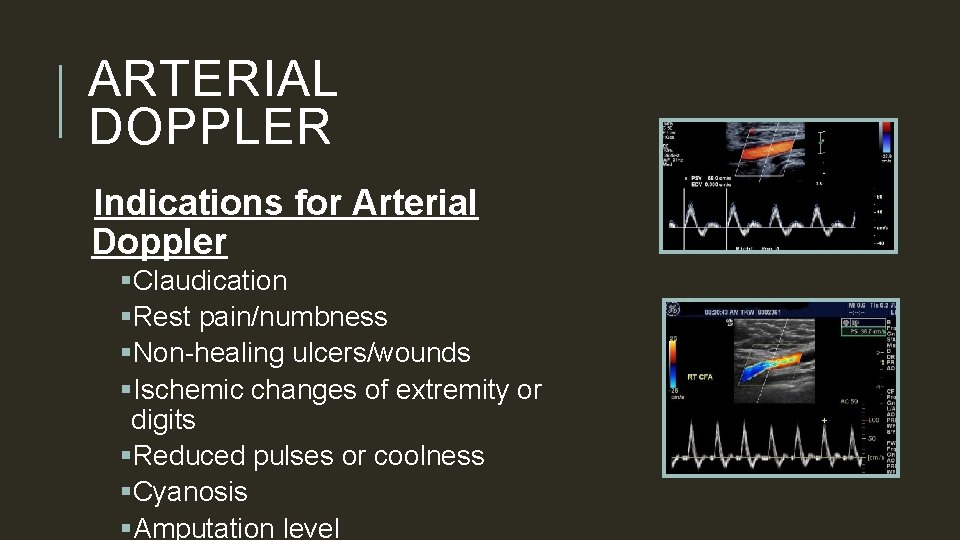
ARTERIAL DOPPLER Indications for Arterial Doppler §Claudication §Rest pain/numbness §Non-healing ulcers/wounds §Ischemic changes of extremity or digits §Reduced pulses or coolness §Cyanosis §Amputation level
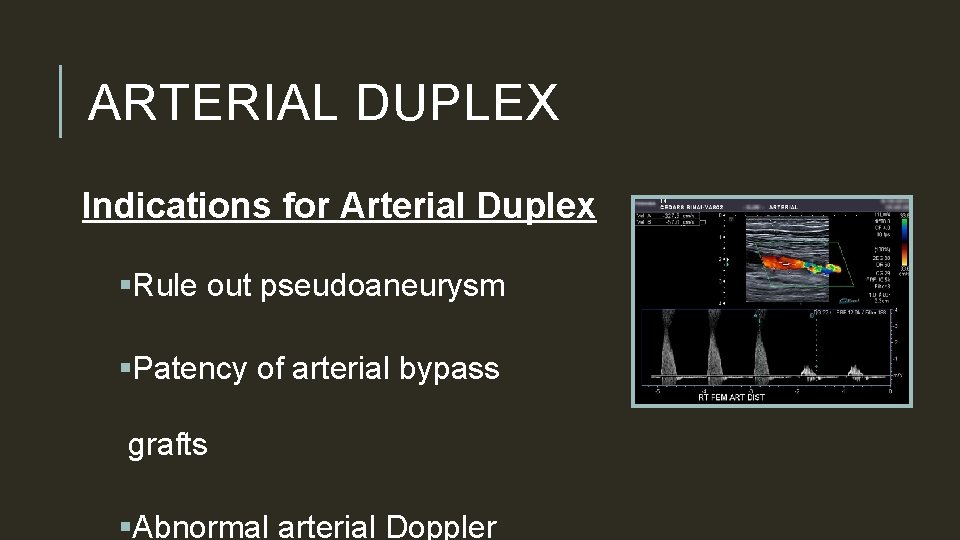
ARTERIAL DUPLEX Indications for Arterial Duplex §Rule out pseudoaneurysm §Patency of arterial bypass grafts §Abnormal arterial Doppler

VALUES FOR ARTERIAL STUDIES Arterial Doppler §The resting systolic blood pressure at the ankle is compared with the systolic brachial pressure, and the ratio of the two pressures defines the ankle-brachial index. This index provides a measure of the severity of disease. §Normal ABI is >0. 91 to as high as 1. 3 §An ABI >1. 3 suggests the presence of calcified vessels (diabetic, renal patient) §An ABI ≤ 0. 9 is diagnostic of occlusive arterial disease in patients with symptoms of claudication or other signs of ischemia §An ABI of 0. 4 to 0. 9 suggests a degree of arterial obstruction often associated with claudication §An ABI below 0. 4 represents multilevel disease (any combination of iliac, femoral or tibial vessel disease) and may be associated with non-healing ulcerations, ischemic rest pain, or pedal gangrene §Transcutaneous oxygen measurements TCP 02 should be measured to evaluate local tissue perfusion, >40 mm. HG likely will heal a wound anything less than

VALUES FOR ARTERIAL STUDIES §Arterial Duplex: a noninvasive ultrasound that measures the velocities in the peripheral arteries that detects focal increases in blood flow velocity indicative of stenosis; will report patency of bypass grafts as well

CHRONIC VENOUS INSUFFICIENCY PATIENTS § Venous Duplex: A duplex ultrasound is a noninvasive test that uses sound waves to create pictures of venous structures and blood flow. It can help determine where reflux is occurring and diagnose venous thrombus.

VENOUS DUPLEX Indications for Venous Duplex: § rule out venous thrombus § rule out venous insufficiency Leg Symptoms §Tiredness, fatigue §Swelling of legs/ankles §Throbbing §Heaviness §Itching/burning §Leg cramps §Aching/pain

VENOUS INSUFFICIENCY The presence of superficial reflux is noted in the body of the report as follows: § (+) for reflux greater than 0. 5 seconds and (-) for absence or reflux or less than 0. 5 seconds. § The presence of deep reflux is noted in the body of the report when flow § reversal is greater than 1. 0 second. § Interpretation will normally specify where if any reflux or insufficiency is noted.

VENOUS DUPLEX FOR RULE OUT THROMBUS § Interpretation will state if a deep or superficial thrombus is noted or not. § If DVT or SVT is noted, the ordering provider should address this. Most patient’s diagnosed with DVT will be on some form of anticoagulation and can be placed in compression. Activity is recommended.

TREATMENT FOR DVT q DVT treatment: first line is anticoagulation (Heparin, Coumadin, Rivaroxaban (Xarelto), Apixaban (Eliquis), Dabigatran (Pradaxa) §Purpose of treatment to is restore blood flow in a vein and prevent a pulmonary embolism from forming. §Goal is to control the size of the clot and prevent more clots from forming. q Thrombolysis: procedure used to dissolve large clot, catheter is placed in the vein and TPA (clot busting medication) is delivered directly to the clot through the catheter q Inferior Vena Cava Filter: a filter is placed in the inferior vena cava via catheter, purpose is to trap thrombus or clots in the lower body and preventing a pulmonary embolism
TREATMENT FOR VENOUS INSUFFICIENCY q. Conservative management: compression for 6 weeks q. Endovenous ablation q. Sclerotherapy q. Stripping Illustration: Sclerotherapy

WARNINGS SIGNS TO LOOK OUT FOR IN PAD AND VEIN PATIENTS Peripheral Artery Disease Venous insufficiency/Venous thrombus §Ischemic rest pain § Severity of symptoms: do they affect ADL §Claudication § Venous ulcers §Cold feet/legs § Discoloration §Discoloration § If DVT present is pt on anticoagulation §Ulcers or gangrene § Fall risk

BARRIERS TO PULMONARY REHAB IN PAD AND VEIN PATIENTS Venous PAD Insufficiency/Thrombu s § Patients with severe PAD and claudication may not be able to participate in endurance activities. § Symptoms may be severe enough that patients are unable to participate in endurance activities. § PAD patients are either on antiplatelet therapy (Plavix, Effient, Brilinta, Aspirin, etc. ) or anticoagulation (Coumadin, Xarelto, Eliquis, Pradaxa etc. ) § Be aware of anticoagulation status, risk of falls etc.
CAROTID ARTERY DISEASE q Carotid arteries carry blood to the brain. When plaque builds up in the arteries it affects blood flow to the brain which can cause TIA or Stroke. Vascular surgeons can intervene on patients with carotid artery disease to help prevent TIA or stroke with a carotid endarterectomy or carotid stent. q Risk factors for carotid artery disease include smoking, diabetes, high blood pressure, sedentary lifestyle and family history.
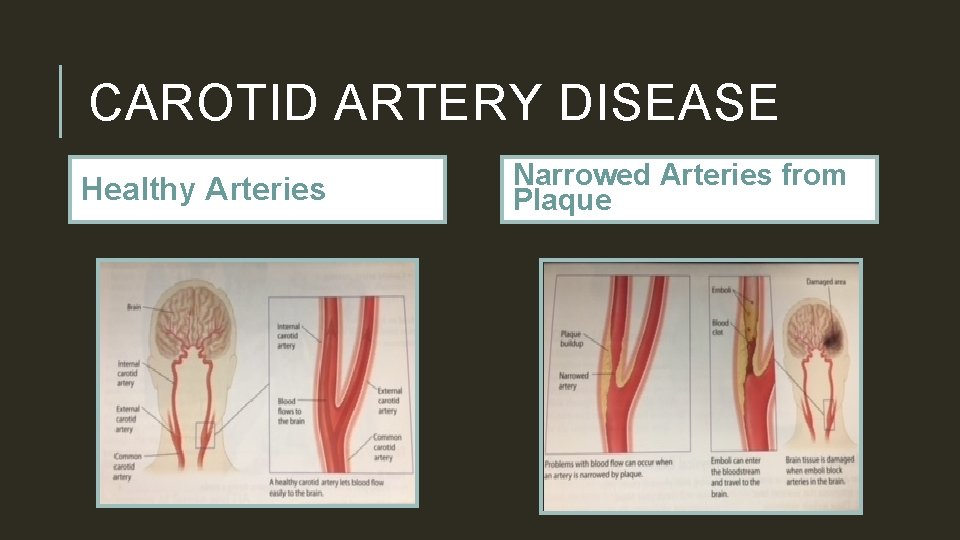
CAROTID ARTERY DISEASE Healthy Arteries Narrowed Arteries from Plaque
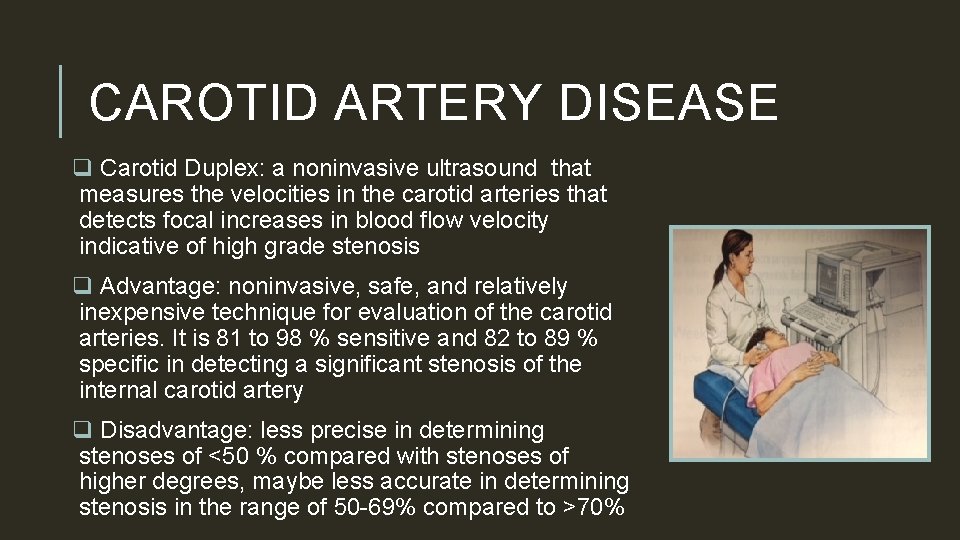
CAROTID ARTERY DISEASE q Carotid Duplex: a noninvasive ultrasound that measures the velocities in the carotid arteries that detects focal increases in blood flow velocity indicative of high grade stenosis q Advantage: noninvasive, safe, and relatively inexpensive technique for evaluation of the carotid arteries. It is 81 to 98 % sensitive and 82 to 89 % specific in detecting a significant stenosis of the internal carotid artery q Disadvantage: less precise in determining stenoses of <50 % compared with stenoses of higher degrees, maybe less accurate in determining stenosis in the range of 50 -69% compared to >70%

CAROTID ARTERY DISEASE q There a number of reasons that patients can have a TIA or Stroke. If a patient had a stroke or TIA and it is determined that the cause is carotid artery stenosis, then the Vascular team is consulted. Symptoms of Transient Ischemic Attack or Cerebral Vascular Accident §Sudden unilateral numbness or weakness of the face, arms, or legs §Sudden confusion, trouble speaking, or trouble understanding §Sudden visual changes, amaurosis fugax §Sudden trouble walking, dizziness or loss of balance

CAROTID ARTERY DISEASE Indications to treat § Asymptomatic stenosis ≥ 70 § Symptomatic stenosis 50 -69% Purpose of intervening on carotid artery stenosis is to prevent future TIA or CVA, intervention does not reverse any damage previously done to brain.
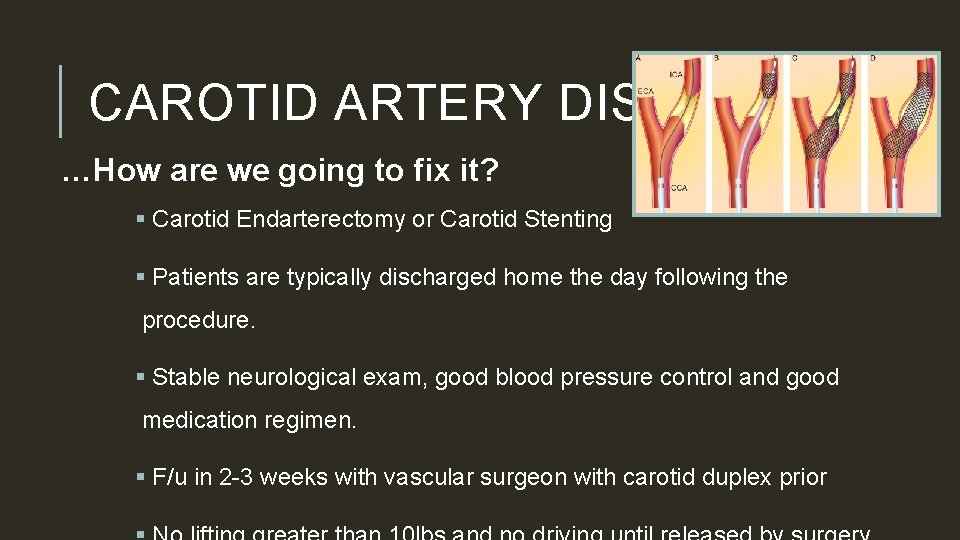
CAROTID ARTERY DISEASE …How are we going to fix it? § Carotid Endarterectomy or Carotid Stenting § Patients are typically discharged home the day following the procedure. § Stable neurological exam, good blood pressure control and good medication regimen. § F/u in 2 -3 weeks with vascular surgeon with carotid duplex prior

BARRIERS TO PULMONARY REHAB IN CAROTID ARTERY DISEASE PATIENTS q Patients should wait about 4 weeks post procedure before participating on pulmonary rehab. They should be cleared to participate by vascular surgery team. q If a patient had a CVA and has neurological deficits, their deficits can be a barrier to their activity in rehab. Not all patients who have a CVA have deficits. The potential barrier will vary patient to patient.

ABDOMINAL AORTIC ANEURYSM q. An abdominal aortic aneurysm is an enlarged area in the lower part of your aorta. An aneurysm is defined as a segmental, full thickness dilation of the a blood vessel that is 50% greater than normal vessel diameter. In most adults if the aortic diameter is greater than 3. 0 cm it is considered aneurysmal. Risk factors for AAA § Smoking § Male gender § Hypertension § Caucasian race § Close relative (parent or sibling with hx) § Other large body aneurysm (iliac, § Older age >65 femoral, popliteal)
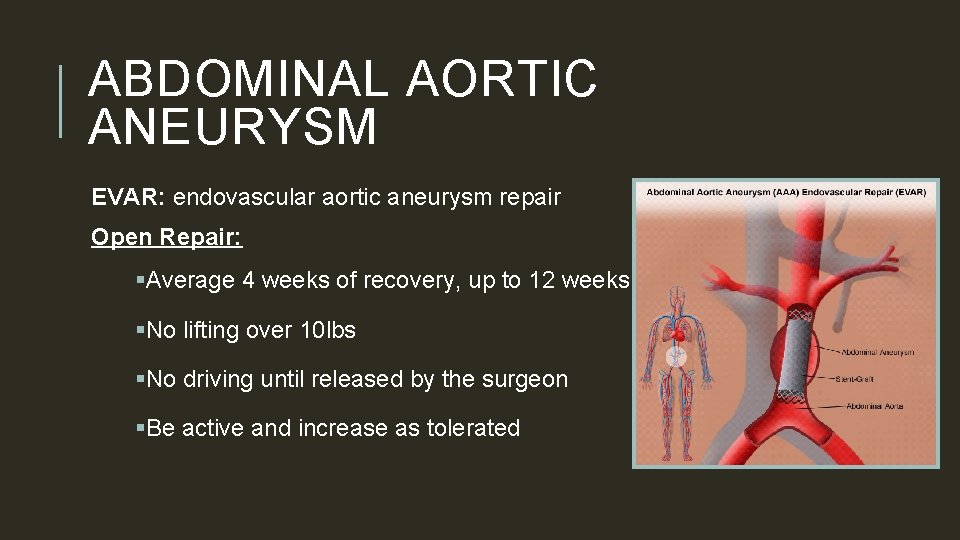
ABDOMINAL AORTIC ANEURYSM EVAR: endovascular aortic aneurysm repair Open Repair: §Average 4 weeks of recovery, up to 12 weeks §No lifting over 10 lbs §No driving until released by the surgeon §Be active and increase as tolerated

AORTIC ANEURYSM q Ascending Aortic Aneurysm: over 3 cm abnormal; over 5. 5 needs fixed or >1 cm growth within one year; connective tissue disorder (Marfan’s) may fix around 4. 5 cm; bicuspid aortic valve greater risk for dissection so they are fixed around 5 cm q Open repair similar to open heart surgery with dacron graft q Descending Aortic Aneurysm: these are typically repaired endovascular approach q TEVAR: thoracic endovascular aortic aneurysm repair
CORONARY ARTERY DISEASE Risk factors for CAD Symptoms of CAD § Diabetes § Angina (pain, pressure, aching, tingling or burning radiating to chest, back, shoulders, throat, jaw, or arms) § Smoking § Tiredness or lack of energy § Family history § SOB § Age § Dizziness § High blood pressure § High cholesterol § Nausea/vomiting
CORONARY ARTERY DISEASE q. Cardiac catheterization is performed to evaluate or confirm the presence of heart disease (coronary artery disease, heart valve disease, or aortic disease). q. Echocardiogram: transthoracic or transesophageal q. Stress testing: treadmill stress testing, dobutamine stress echo, NM stress test q. Viability test: NM or MRI q. EKG, holter monitor, event monitor

CORONARY ARTERY BYPASS SURGERY q. Surgical intervention for CAD is CABG (coronary artery bypass grafting) q. During bypass surgery a healthy vessel is taken from a patient’s chest or limbs and used to bypass the blockage to restore or improve blood flow to the heart. § Left/right internal mammary q. Vessels used for grafts: artery § Greater saphenous vein § Radial arteries

CORONARY ARTERY BYPASS SURGERY q Chest incision: an incision is made in the chest and the breastbone is divided and held open throughout the procedure in order to access the heart q Leg/arm incisions: incisions made in limbs for harvesting vein or artery; length of incision will depend on if the harvest was endovascular or open q On or Off pump: a heart and lung machine may be used during the surgery; the blood is circulated through the heart and lung machine

CABG POSTOPERATIVE COURSE Recovered in Cardiac ICU: § Intubated § Chest tubes § Central lines, arterial lines § Foley catheter q. Transferred to Cardiac Surgery floor when pt is extubated and not requiring high flow oxygen, hemodynamically stable: no arterial line, no pressors or balloon pump. q. Chest tubes removed when drainage is decreasing and chest xrays stable. § Temporary pacing wires § Intra-aortic balloon pump q. Pacing wires are removed when heart rhythm is stable.

CABG POST-OPERATIVE COURSE q Hospital course is different patient to patient but on average is 5 -7 days. q Many patients are discharged to ECF or inpatient rehab for physical and occupational therapy. q Patients who go home are discharged with home health PT/OT/nursing. q F/u with CVS in 2 -3 weeks post operatively with chest x-ray and labs q Once patient has been discharged from therapy services and CVS team declares them stable, they are enrolled in Cardiac Rehab. (actually initiated in hospital but pt must be cleared to begin by provider)

CABG POST-OPERATIVE COURSE Sternal Precautions § 6 -8 weeks to heal post CABG §Avoid motions that strain your arms or chest; no pushing, pulling or lifting heavy objects §Avoid reaching behind you or high above your head §Avoid pushing with your arms when standing up §Avoid sexual positions that put stress on your chest or arms

CABG POST-OPERATIVE COURSE q. Monitor blood pressure and heart rate (irregular or palpitations) q. Daily weights q. Monitor incisions for any signs of infection or dehiscence q. Pain, tightness or discomfort in chest, jaw, neck, arms or back q. Exertional or unusual SOB q. Excessive fatigue after exercise q. Fevers or chills
HEART VALVE SURGERY q Stenosis: a valve does not open all the way; not allowing good blood flow through the valve q Regurgitation: valve does not close tightly; “leaky”; blood leaks backward q. If the valves are not functioning correctly this can cause heart failure.
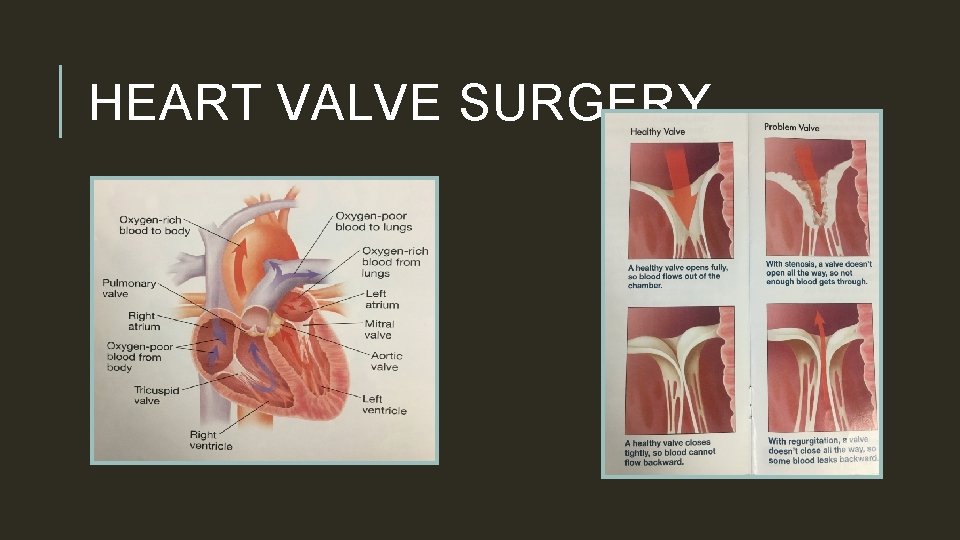
HEART VALVE SURGERY
HEART VALVE SURGERY q Mechanical or tissue valves q. Anticoagulation or antiplatelet therapy q. Post-operative course, discharge planning and sternal precautions are the same as CABG patients
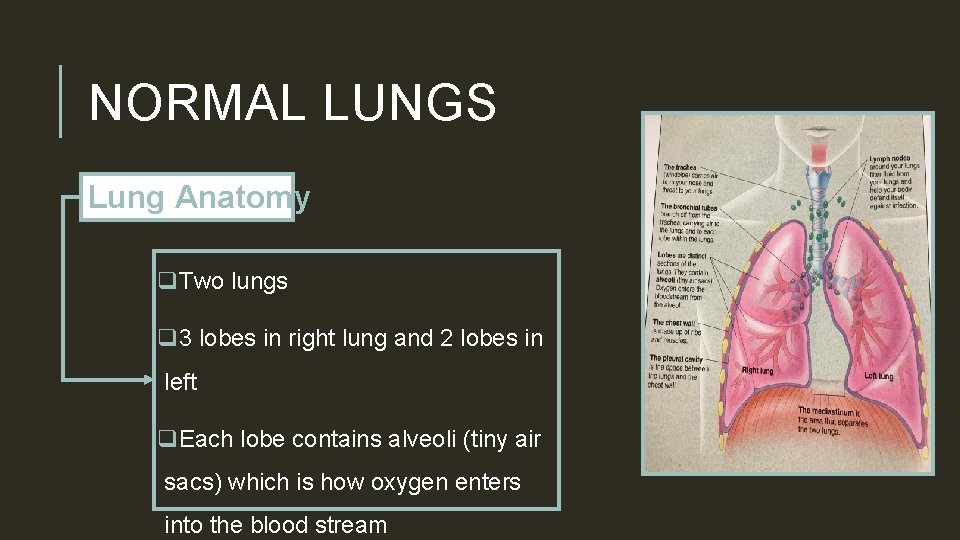
NORMAL LUNGS Lung Anatomy q. Two lungs q 3 lobes in right lung and 2 lobes in left q. Each lobe contains alveoli (tiny air sacs) which is how oxygen enters into the blood stream
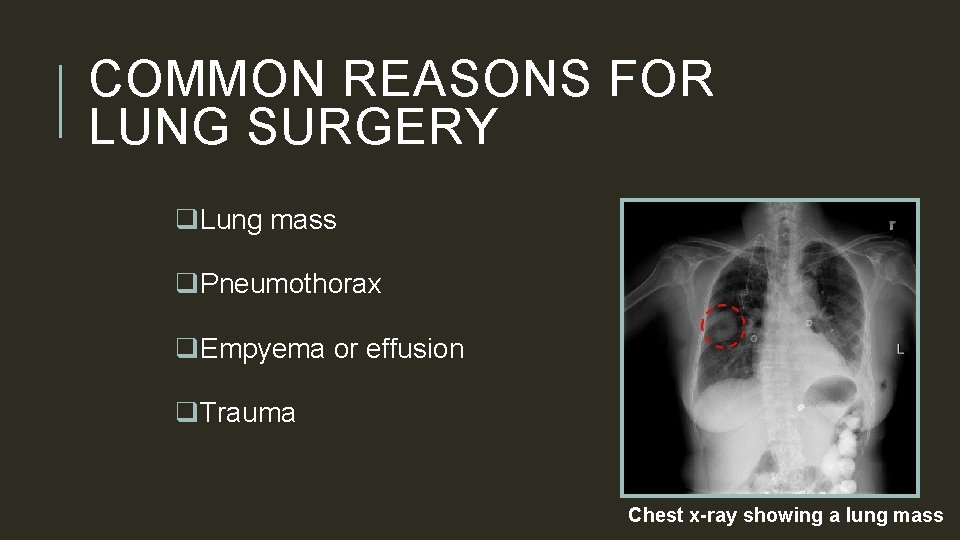
COMMON REASONS FOR LUNG SURGERY q. Lung mass q. Pneumothorax q. Empyema or effusion q. Trauma Chest x-ray showing a lung mass

LUNG SURGERIES q Lobectomy: removal of entire lung q Pneumonectomy: removal of entire lung q Wedge resection: deep wedge for tumor resection; removal of small portion of lobe q Pleurodesis: chemical or mechanical q Bleb resection: bleb disease (balloon pops on lung, causing air leak which causes collapsed lung) superficial wedge resection or stitched q Decortication for severe pneumonia or lung abscesses (peeling of exudate over the lung) q Approach depends on surgeon: thoracotomy or video assisted thoracoscopy (VATS)
CHEST VISUALIZATION/BIOPSY EXAMS q. Bronchoscopy q. Mediastinoscopy: visualize mediastinal lymph nodes q. Needle biopsy

LUNG SURGERIES q Incisional care q Pain management q Incentive spirometry, pulmonary hygiene q 4 -6 weeks pt should be able to participate in pulmonary rehab q Biopsy results are often pending

SUMMARY q Several surgeries performed by Cardiovascular Surgeons q Once patients recover from surgery, they will be released by surgical team to start rehab programs. q. Warnings signs and barriers to look out for in cardiovascular patients in pulmonary rehab

THANK YOU FOR LISTENING Jamie Luecke, APN, CNP Nurse Practitioner Cardiovascular and Thoracic

REFERENCES Dean, S. M. , Bhagwan, S. , Abraham, W. T. (2014). Color Atlas and Synopsis of Vascular Disease. New York, NY: Mc. Graw-Hill Education. Krames Staywell, LLC. (2013). Coronary artery bypass surgery: understanding surgery and managing CAD risk factors. www. kramesstaywell. com Krames Staywell, LLC. (2010). Lung surgery: treatment for lung problems. www. kramesstaywell. com Krames Staywell, LLC. (2011). Procedures for abdominal aortic aneurysm. www. kramesstaywell. com Krames Staywell, LLC. (2014). Procedures for carotid artery problems. www. kramesstaywell. com

REFERENCES Krames Staywell, LLC. (2013). Procedures for peripheral arterial disease. www. kramesstaywell. com Krames Staywell, LLC. (2003). Understanding artery problems. www. kramesstaywell. com. Krames Staywell, LLC. (2010). Understanding vein problems. www. kramesstaywell. com Up. To. Date. Furie, K. L. (2016). Evaluation of carotid artery stenosis. Retrieved from Upto. Date.
- Slides: 47