Cardiovascular Disease in the Setting of HIV Infection

























- Slides: 51

Cardiovascular Disease in the Setting of HIV Infection Kathleen Fitch, MSN, FNP-BC Massachusetts General Hospital and Harvard Medical School 2018 Michigan Clinical Nursing Conference for HIV and STD Care May 31 st, 2018

Disclosures • None 2

Learning Goals • Improve understanding of heightened cardiovascular disease (CVD) risk in the setting of HIV • Delineate unique pathophysiology of CVD in the setting of HIV • Understand assessment for and management on CVD in the setting of HIV, including those of an investigative nature • Explore areas of future research • Explore patient education strategies for HIVassociated CVD 3

Outline • Epidemiology of CVD in the setting of HIV • Pathophysiology of CVD and HIV • Role of traditional risk factors • Role of inflammation/immune activation • Management of CVD in HIV • CVD risk prediction • CVD prevention/treatment • Novel risk factors • Traditional risk factors 4

Background • In the past several years we have observed many advances in the care for people living with HIV: – Improved treatment – Rapid initiation of antiretroviral therapy (ART) – Decreased rates of AIDS-related deaths (UNAIDS 2013) – Increased life expectancy (Legarth JAIDS 2016; Siddiqi JAIDS 2016) • However, as the population with HIV ages, rates of non-AIDS complications (NCDs) such as CVD are increasingly prevalent (Deeks Lancet 2013; Guaraldi CID 2011) 5

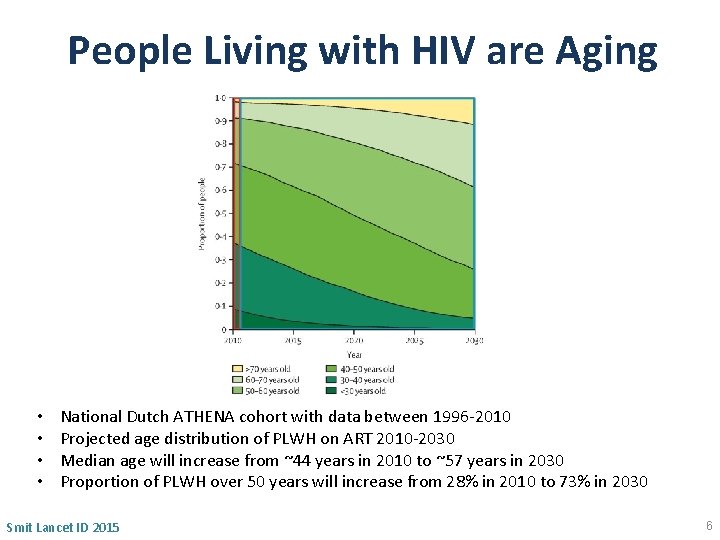
People Living with HIV are Aging • • National Dutch ATHENA cohort with data between 1996 -2010 Projected age distribution of PLWH on ART 2010 -2030 Median age will increase from ~44 years in 2010 to ~57 years in 2030 Proportion of PLWH over 50 years will increase from 28% in 2010 to 73% in 2030 Smit Lancet ID 2015 6

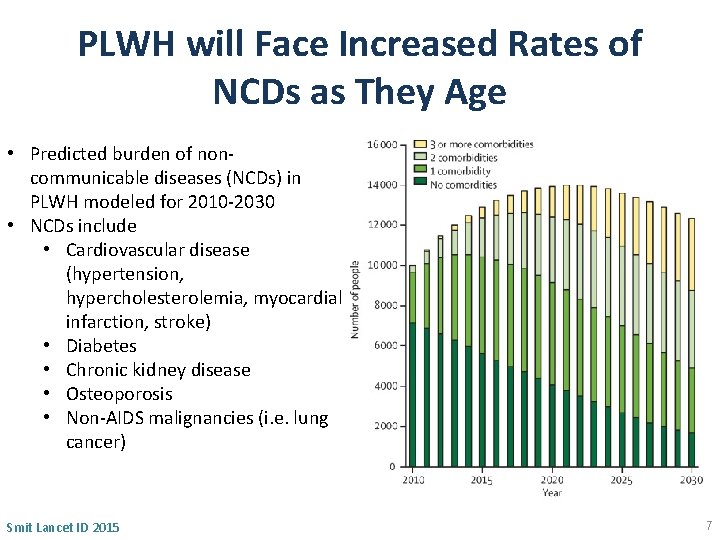
PLWH will Face Increased Rates of NCDs as They Age • Predicted burden of noncommunicable diseases (NCDs) in PLWH modeled for 2010 -2030 • NCDs include • Cardiovascular disease (hypertension, hypercholesterolemia, myocardial infarction, stroke) • Diabetes • Chronic kidney disease • Osteoporosis • Non-AIDS malignancies (i. e. lung cancer) Smit Lancet ID 2015 7

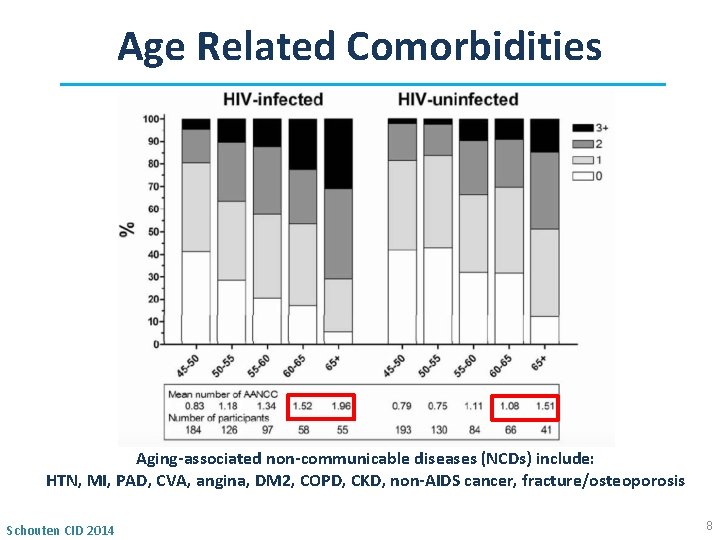
Age Related Comorbidities Aging‐associated non‐communicable diseases (NCDs) include: HTN, MI, PAD, CVA, angina, DM 2, COPD, CKD, non‐AIDS cancer, fracture/osteoporosis Schouten CID 2014 8

Outline • Epidemiology of CVD in the setting of HIV • Pathophysiology of CVD and HIV • Role of traditional risk factors • Role of inflammation/immune activation • Management of CVD in HIV • CVD risk prediction • CVD prevention/treatment • Novel risk factors • Traditional risk factors 9

10

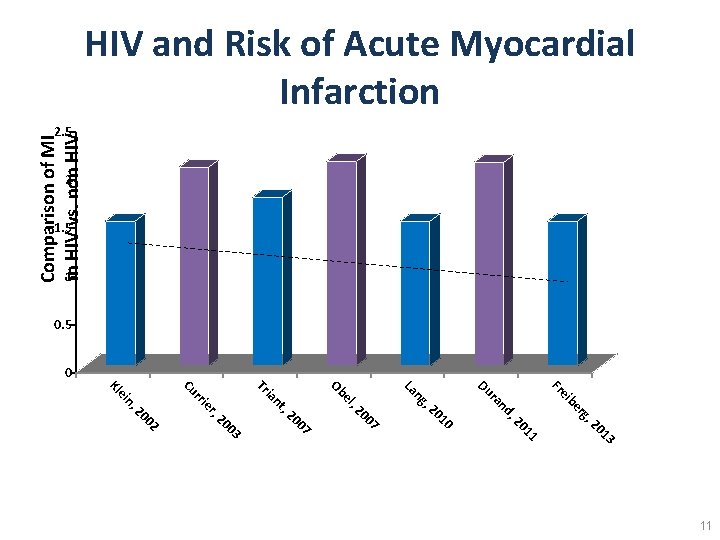
Comparison of MI in HIV vs. non HIV and Risk of Acute Myocardial Infarction 2. 5 2 1. 5 1 0. 5 0 Fr 3 11 01 10 20 , 2 rg be ei d, 20 an r Du g, n La 7 00 , 2 el 7 00 , 2 nt ia Ob Tr 03 02 20 20 r, ie rr Cu n, ei Kl 11

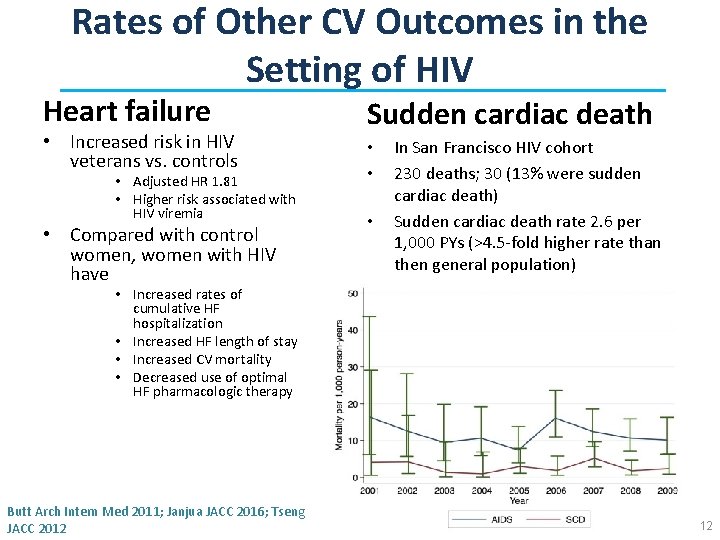
Rates of Other CV Outcomes in the Setting of HIV Heart failure • Increased risk in HIV veterans vs. controls • Adjusted HR 1. 81 • Higher risk associated with HIV viremia • Compared with control women, women with HIV have Sudden cardiac death • • • In San Francisco HIV cohort 230 deaths; 30 (13% were sudden cardiac death) Sudden cardiac death rate 2. 6 per 1, 000 PYs (>4. 5 -fold higher rate than then general population) • Increased rates of cumulative HF hospitalization • Increased HF length of stay • Increased CV mortality • Decreased use of optimal HF pharmacologic therapy Butt Arch Intern Med 2011; Janjua JACC 2016; Tseng JACC 2012 12

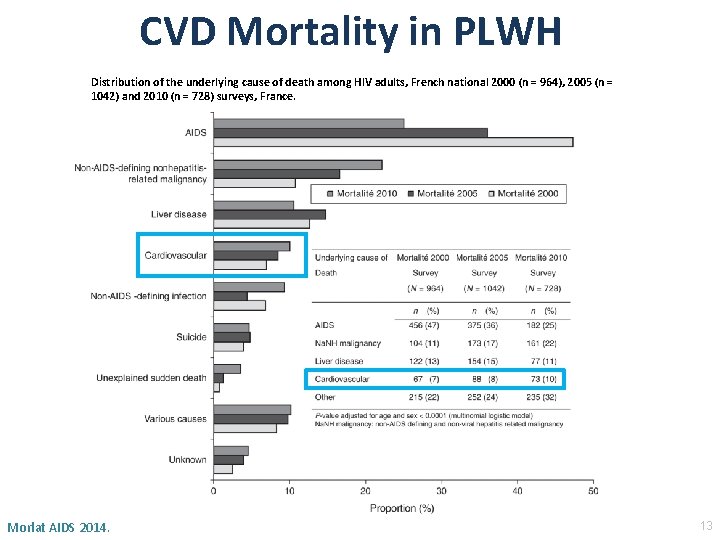
CVD Mortality in PLWH Distribution of the underlying cause of death among HIV adults, French national 2000 (n = 964), 2005 (n = 1042) and 2010 (n = 728) surveys, France. Morlat AIDS 2014. 13

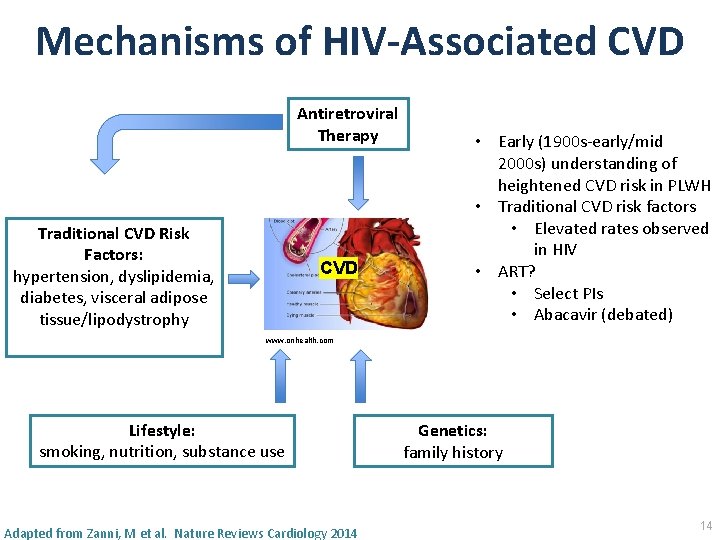
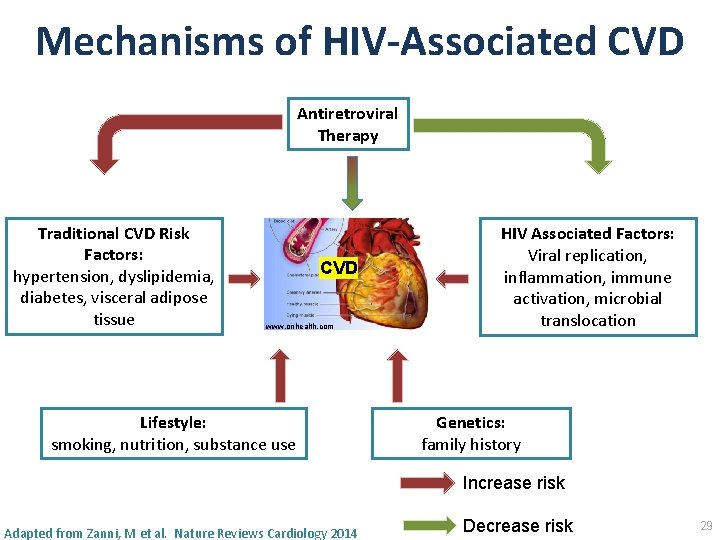
Mechanisms of HIV‐Associated CVD Antiretroviral Therapy Traditional CVD Risk Factors: hypertension, dyslipidemia, diabetes, visceral adipose tissue/lipodystrophy CVD • Early (1900 s-early/mid 2000 s) understanding of heightened CVD risk in PLWH • Traditional CVD risk factors • Elevated rates observed in HIV • ART? • Select PIs • Abacavir (debated) www. onhealth. com Lifestyle: smoking, nutrition, substance use Adapted from Zanni, M et al. Nature Reviews Cardiology 2014 Genetics: family history 14

Smoking in HIV • Heightened rates – 56% (D: A: D) – 54% (SFGH) – 47% (US cohort) – 69% (French cohort) • 85% lifetime history • Significantly higher than people without HIV Burkhalter Nicotine Tob Res 2005; Friis-Moller AIDS 2003; Mamary AIDS Pt Care STDs 2002; Gritz Nicotine Tob Res 2004; Vittecoq AIDS 2003; Saves CID 2003; Lifson AJPH 2010. 15

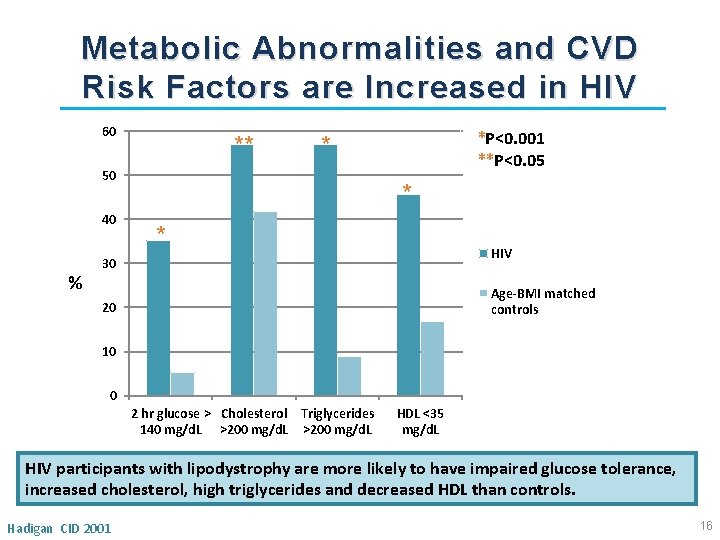
Metabolic Abnormalities and CVD Risk Factors are Increased in HIV 60 ** 50 40 % 30 ** *P<0. 001 **P<0. 05 * * * HIV Age‐BMI matched controls 20 10 0 2 hr glucose > Cholesterol Triglycerides 140 mg/d. L >200 mg/d. L HDL <35 mg/d. L HIV participants with lipodystrophy are more likely to have impaired glucose tolerance, increased cholesterol, high triglycerides and decreased HDL than controls. Hadigan CID 2001 16

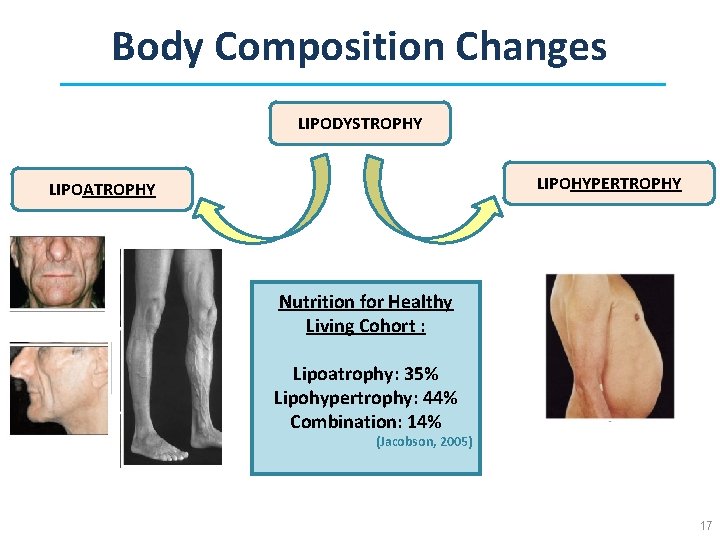
Body Composition Changes LIPODYSTROPHY LIPOHYPERTROPHY LIPOATROPHY Nutrition for Healthy Living Cohort : Lipoatrophy: 35% Lipohypertrophy: 44% Combination: 14% (Jacobson, 2005) Reduced SAT (Subcutaneous Adipose Tissue) Increased VAT (Visceral Adipose Tissue) 17

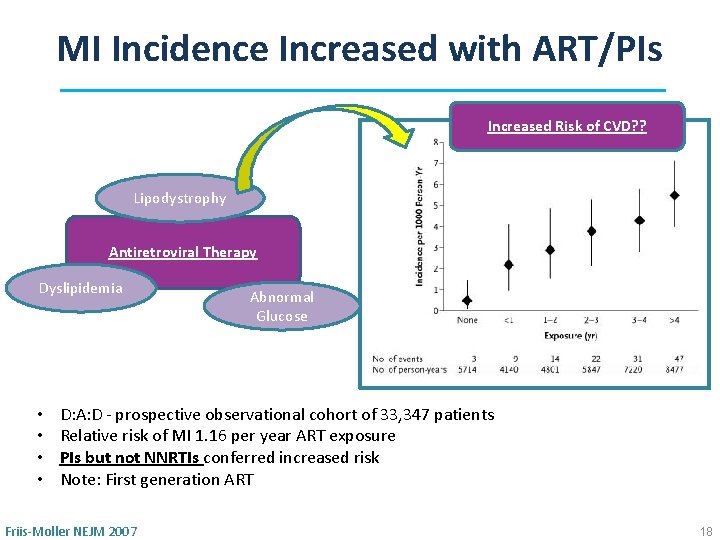
MI Incidence Increased with ART/PIs Increased Risk of CVD? ? Lipodystrophy Antiretroviral Therapy Dyslipidemia • • Abnormal Glucose D: A: D - prospective observational cohort of 33, 347 patients Relative risk of MI 1. 16 per year ART exposure PIs but not NNRTIs conferred increased risk Note: First generation ART Friis-Moller NEJM 2007 18

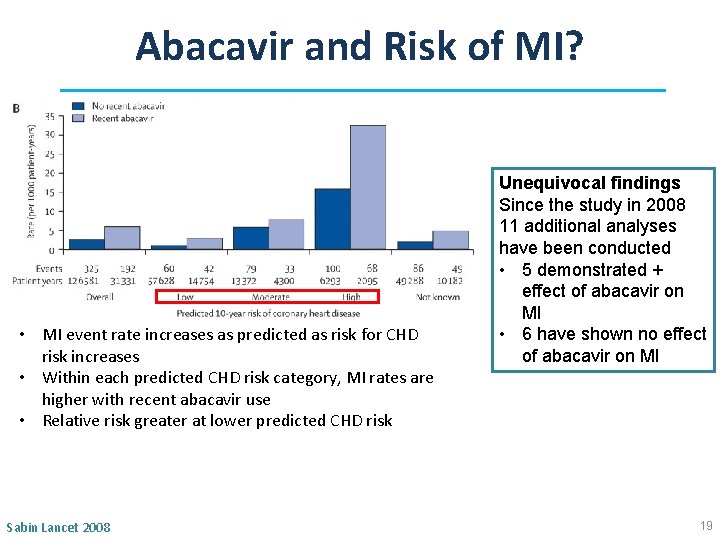
Abacavir and Risk of MI? • MI event rate increases as predicted as risk for CHD risk increases • Within each predicted CHD risk category, MI rates are higher with recent abacavir use • Relative risk greater at lower predicted CHD risk Sabin Lancet 2008 Unequivocal findings Since the study in 2008 11 additional analyses have been conducted • 5 demonstrated + effect of abacavir on MI • 6 have shown no effect of abacavir on MI 19

Contemporary ART and CVD Risk • Cumulative use of DRV/r but not ATV/r associated with increased CVD risk • Strength of association similar to that of IDV and LPV/r but not modified by dyslipidemia • Limitations: – – – No adequately powered randomized trial has yet to be conducted Unclear how NRTIs including abacavir accounted for Unmeasured confounding Cannot prove causality No dose data No gender-stratified analyses • Clinical implications potentially significant further randomized controlled trials are needed • More data favors using ART to prolong life and PIs are an important component of the regimen Tyom et al. Abstract 128 LB. CROI 2017; Lundgren Current Opinion 2018. 20

Traditional Risk Factors Do Not Tell the Whole Story • Increased MI risk persists despite accounting for established CVD risk factors and ART use – Traditional risk factors only account for 10 -25% of risk in large cohorts – Persistent 40 -80% increased risk of MI in PLWH • Persistently increased risk thought to be driven by HIV-specific inflammation and immune activation supported by extensive data – SMART study – Biomarkers of inflammation linked to surrogate markers of CVD – Low CD 4 and high HIV viral load linked to CVD events • In treated and suppressed HIV patients – Reduced but persistent inflammation/immune activation and CVD risk 21

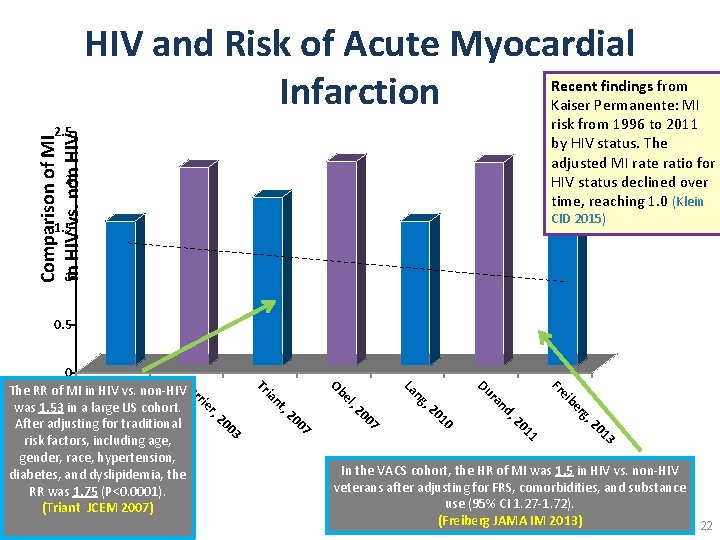
HIV and Risk of Acute Myocardial Infarction Recent findings from Kaiser Permanente: MI risk from 1996 to 2011 by HIV status. The adjusted MI rate ratio for HIV status declined over time, reaching 1. 0 (Klein Comparison of MI in HIV vs. non HIV 2. 5 2 CID 2015) 1. 5 1 0. 5 Fr 3 01 11 20 10 , 2 rg be d, 20 an ei r Du g, n La 7 00 , 2 03 02 20 20 r, ie nt el ia Ob Tr rr n, ei Kl Cu 0 The RR of MI in HIV vs. non-HIV was 1. 53 in a large US cohort. After adjusting for traditional risk factors, including age, gender, race, hypertension, diabetes, and dyslipidemia, the RR was 1. 75 (P<0. 0001). (Triant JCEM 2007) In the VACS cohort, the HR of MI was 1. 5 in HIV vs. non-HIV veterans after adjusting for FRS, comorbidities, and substance use (95% CI 1. 27 -1. 72). (Freiberg JAMA IM 2013) 22

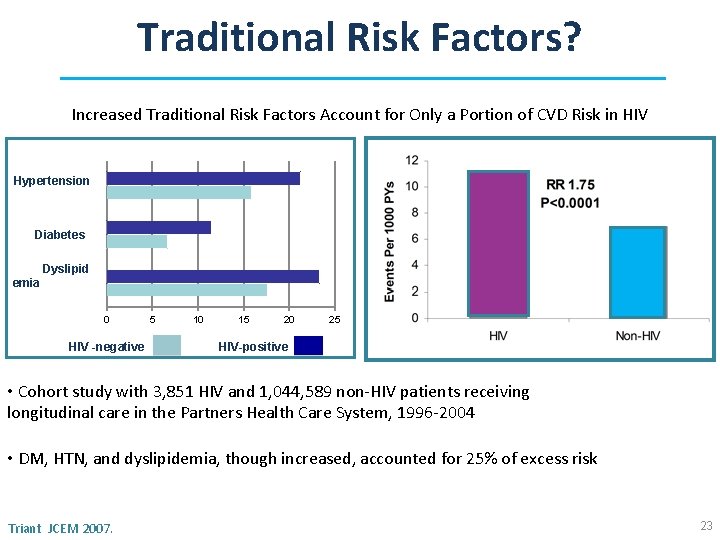
Traditional Risk Factors? Increased Traditional Risk Factors Account for Only a Portion of CVD Risk in HIV Hypertension Diabetes Dyslipid emia 0 HIV -negative 5 10 15 20 25 HIV-positive • Cohort study with 3, 851 HIV and 1, 044, 589 non-HIV patients receiving longitudinal care in the Partners Health Care System, 1996 -2004 • DM, HTN, and dyslipidemia, though increased, accounted for 25% of excess risk Triant JCEM 2007. 23

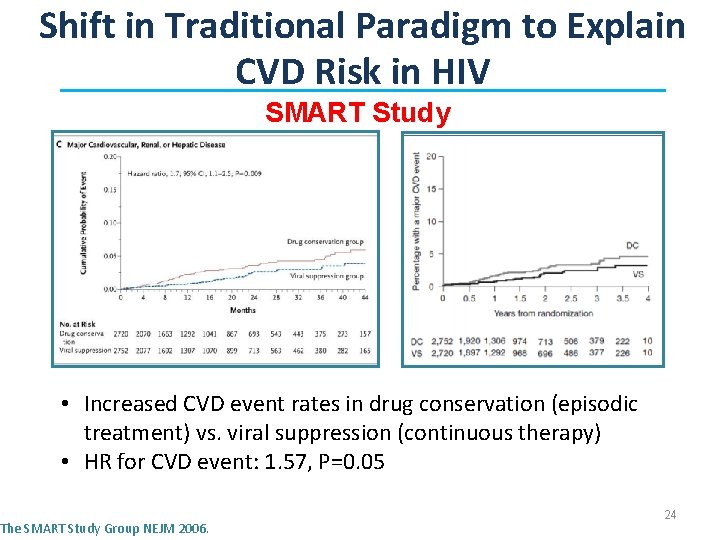
Shift in Traditional Paradigm to Explain CVD Risk in HIV SMART Study • Increased CVD event rates in drug conservation (episodic treatment) vs. viral suppression (continuous therapy) • HR for CVD event: 1. 57, P=0. 05 The SMART Study Group NEJM 2006. 24

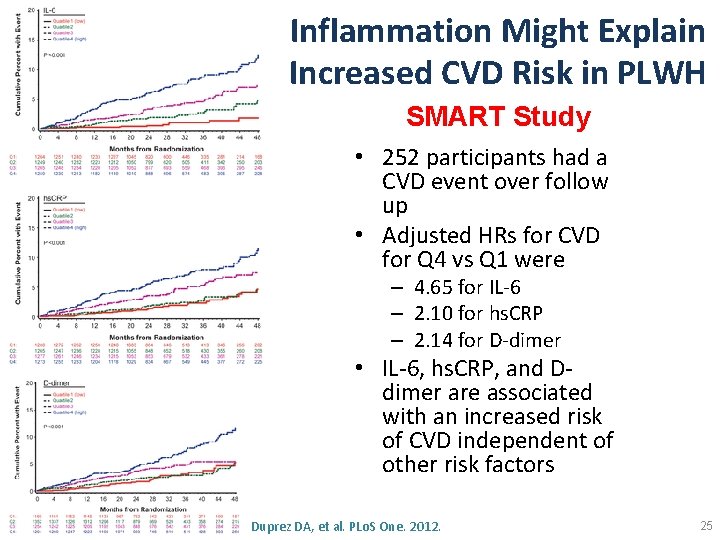
Inflammation Might Explain Increased CVD Risk in PLWH SMART Study • 252 participants had a CVD event over follow up • Adjusted HRs for CVD for Q 4 vs Q 1 were – 4. 65 for IL-6 – 2. 10 for hs. CRP – 2. 14 for D-dimer • IL-6, hs. CRP, and Ddimer are associated with an increased risk of CVD independent of other risk factors Duprez DA, et al. PLo. S One. 2012. 25

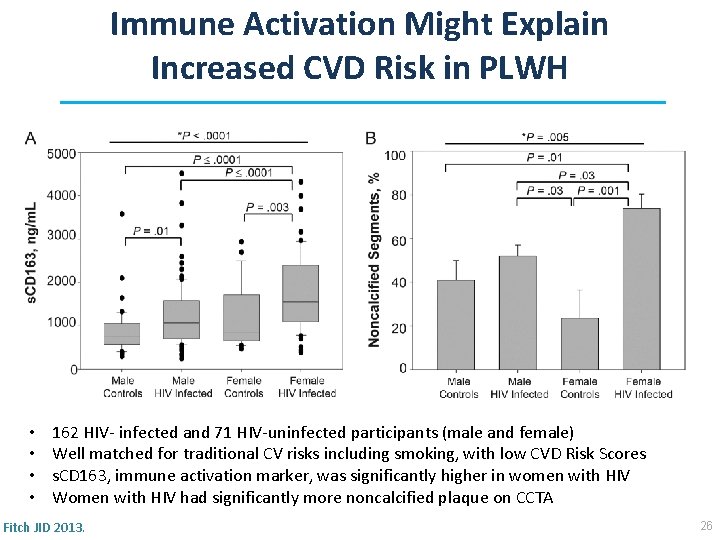
Immune Activation Might Explain Increased CVD Risk in PLWH • • 162 HIV- infected and 71 HIV-uninfected participants (male and female) Well matched for traditional CV risks including smoking, with low CVD Risk Scores s. CD 163, immune activation marker, was significantly higher in women with HIV Women with HIV had significantly more noncalcified plaque on CCTA Fitch JID 2013. 26

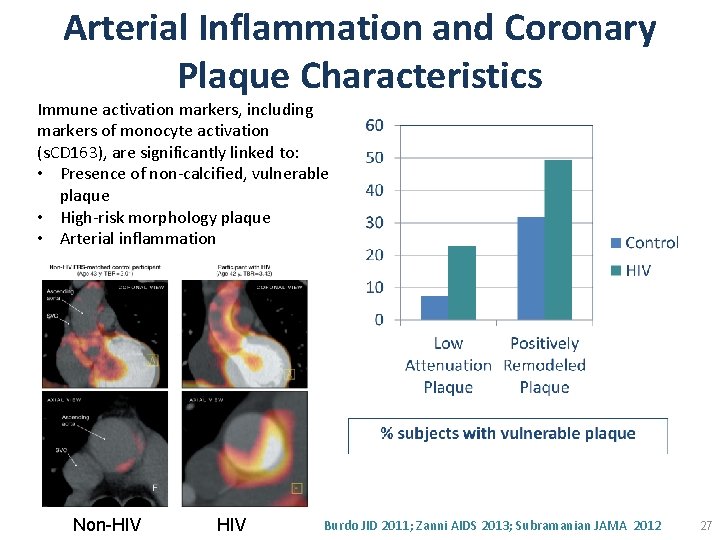
Arterial Inflammation and Coronary Plaque Characteristics Immune activation markers, including markers of monocyte activation (s. CD 163), are significantly linked to: • Presence of non-calcified, vulnerable plaque • High-risk morphology plaque • Arterial inflammation Non-HIV Burdo JID 2011; Zanni AIDS 2013; Subramanian JAMA 2012 27

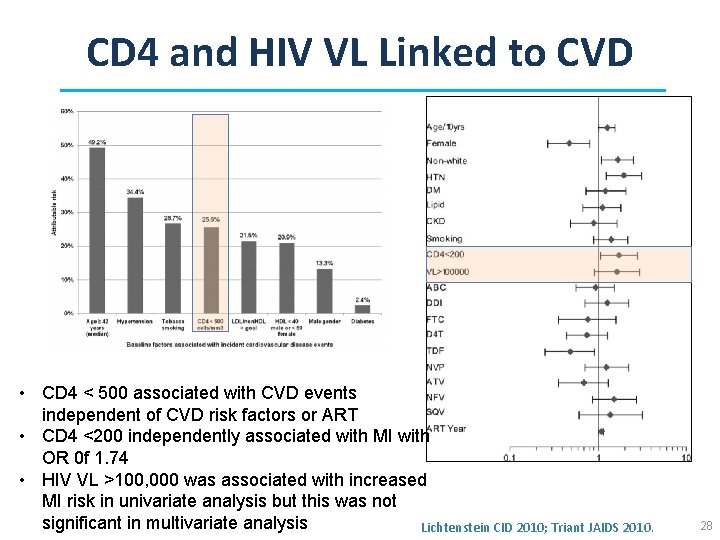
CD 4 and HIV VL Linked to CVD • CD 4 < 500 associated with CVD events independent of CVD risk factors or ART • CD 4 <200 independently associated with MI with OR 0 f 1. 74 • HIV VL >100, 000 was associated with increased MI risk in univariate analysis but this was not significant in multivariate analysis Lichtenstein CID 2010; Triant JAIDS 2010. 28

Mechanisms of HIV‐Associated CVD Antiretroviral Therapy Traditional CVD Risk Factors: hypertension, dyslipidemia, diabetes, visceral adipose tissue CVD www. onhealth. com Lifestyle: smoking, nutrition, substance use HIV Associated Factors: Viral replication, inflammation, immune activation, microbial translocation Genetics: family history Increase risk Adapted from Zanni, M et al. Nature Reviews Cardiology 2014 Decrease risk 29

Outline • Epidemiology of CVD in the setting of HIV • Pathophysiology of CVD and HIV • Role of traditional risk factors • Role of inflammation/immune activation • Management of CVD in HIV • CVD risk prediction • CVD prevention/treatment • Novel risk factors • Traditional risk factors 30

Current Challenges in Preventing and Treating CVD in HIV • Understanding of mechanisms has not yet translated into tailored clinical interventions – Area of intensive investigation – Intervention must address both traditional and immunerelated risk factors • Unclear applicability of general population guidelines • Limitations of HIV-specific guidelines • As of right now, we do not have a strategy uniquely tailored in HIV 31

Dube CID 2003; Lundgren HIV Med 2008; Aberg CID 2014. 32

ACC/AHA CVD Risk Guidelines Add Complexity to Risk Prediction in HIV • New ACC/AHA guidelines on CVD risk estimation released in 2013 • New CVD risk prediction equation employed (Pooled cohorts equation) • Reports of overestimation of CVD risk in the general population Goff Circulation 2014. 33

What Do We Know About CVD Risk Prediction in HIV? • 3 calculators have been used for CVD risk prediction in HIV – Framingham risk calculator • Not developed for PLWH • Estimates 10 year CVD risk – D: A: D risk calculator • Developed for PLWH • Estimates 5 year CVD risk • Incorporates exposure to IDV, LPV, abacavir – ACC/AHA ASCVD risk calculator • Not developed for PLWH • Estimates 10 year CVD risk • EACH of these calculators tends to underestimate CVD risk in PLWH 34

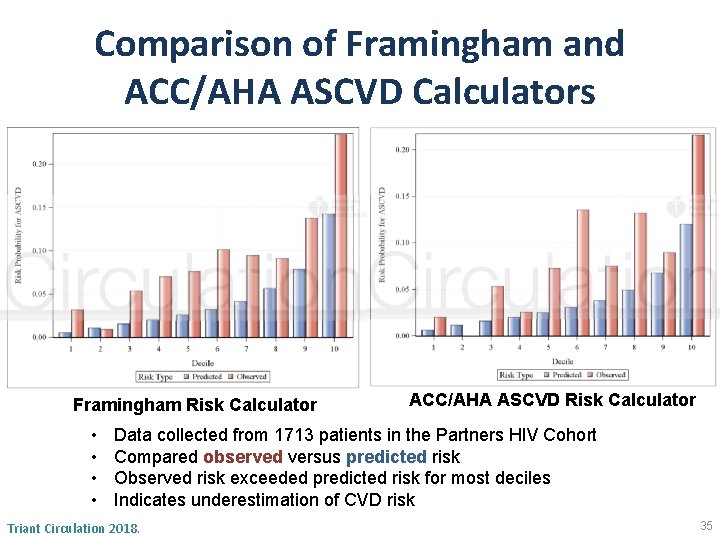
Comparison of Framingham and ACC/AHA ASCVD Calculators Framingham Risk Calculator • • ACC/AHA ASCVD Risk Calculator Data collected from 1713 patients in the Partners HIV Cohort Compared observed versus predicted risk Observed risk exceeded predicted risk for most deciles Indicates underestimation of CVD risk Triant Circulation 2018. 35

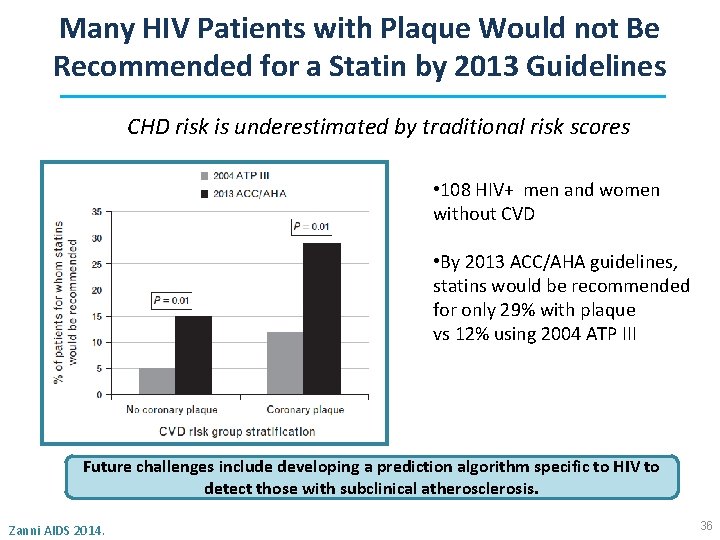
Many HIV Patients with Plaque Would not Be Recommended for a Statin by 2013 Guidelines CHD risk is underestimated by traditional risk scores • 108 HIV+ men and women without CVD • By 2013 ACC/AHA guidelines, statins would be recommended for only 29% with plaque vs 12% using 2004 ATP III Future challenges include developing a prediction algorithm specific to HIV to detect those with subclinical atherosclerosis. Zanni AIDS 2014. 36

Clinical Strategy • Calculate ASCVD risk score and consider the score as lower estimate of risk • Patients with 10 -year ASCVD risk score >7. 5% merit: – Suppressive ART if not already started – Aggressive CVD risk factor reduction – Strong consideration for statin 37

Paradigm Shift in Role of ART in Relation to CVD Risk in HIV • 2010 IAS-USA HIV treatment guidelines – Recommend initiation of ART specifically for patients with HIV CV risk regardless of CD 4 count – Endorse aggressive management of modifiable CVD risk factors • 2012 DHHS HIV treatment guidelines – Recommend antiretroviral therapy for all HIV-infected individuals – The recommendation to initiate therapy at CD 4 count >500 cells/mm 3 is based on growing awareness that untreated HIV infection or uncontrolled viremia may be associated with development of many non-AIDS defining diseases, including cardiovascular disease (CVD), kidney disease, liver disease, neurologic complications, and malignancy Thompson JAMA 2010; ACCF/AHA/ACP Circulation 2009; https: //aidsinfo. nih. gov/contentfiles/lvguidelines/Adultand. Adolescent. GL. pdf 38

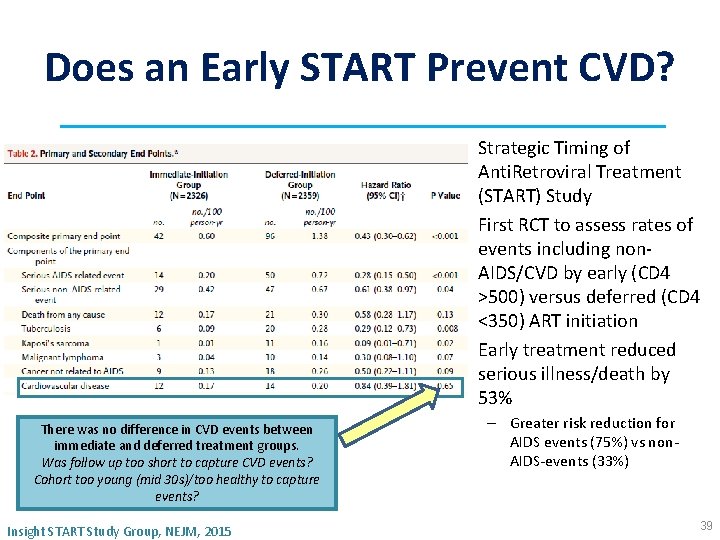
Does an Early START Prevent CVD? • Strategic Timing of Anti. Retroviral Treatment (START) Study • First RCT to assess rates of events including non. AIDS/CVD by early (CD 4 >500) versus deferred (CD 4 <350) ART initiation • Early treatment reduced serious illness/death by 53% There was no difference in CVD events between immediate and deferred treatment groups. Was follow up too short to capture CVD events? Cohort too young (mid 30 s)/too healthy to capture events? Insight START Study Group, NEJM, 2015 – Greater risk reduction for AIDS events (75%) vs non. AIDS-events (33%) 39

ART and CVD Risk: Strategies • Treat HIV to reduce CVD risk • CVD-related benefit from virologic suppression and immune reconstitution achieved by treating HIV thought to outweigh possible proatherogenic effects of individual medications Clinical Strategy • Treat HIV to reduce inflammation, immune activation and associated CVD risk • Consider underlying CVD risk when selecting specific drugs, as individual ART may have varying risk Thompson JAMA 2010 40

Statins in HIV • Dyslipidemia in HIV – – Prevalent, with higher rates than people without HIV Distinctive pattern of low HDL and high triglycerides May be more difficult to treat with statins Drug interactions with ART • Statins are mainstay of treatment and may reduce both traditional and non-traditional risk factors • Statin in HIV: – Effectively lower LDL – Decrease immune activation Hadigan CID 2001; Riddler JAMA 2003; Silverberg Ann Int Med 2009; Lo Lancet HIV 2015 41

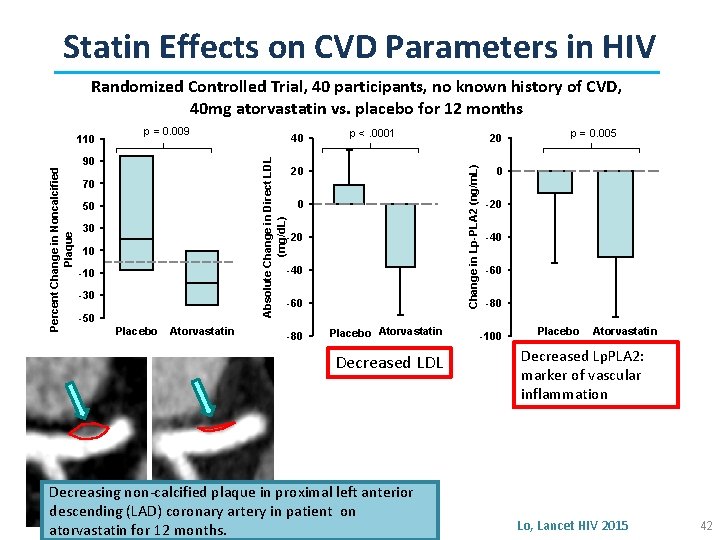
Statin Effects on CVD Parameters in HIV Randomized Controlled Trial, 40 participants, no known history of CVD, 40 mg atorvastatin vs. placebo for 12 months 90 40 70 50 30 10 -30 -50 Placebo Atorvastatin p <. 0001 20 0 -20 -40 -60 -80 20 Change in Lp-PLA 2 (ng/m. L) p = 0. 009 Absolute Change in Direct LDL (mg/d. L) Percent Change in Noncalcified Plaque 110 Placebo Atorvastatin Decreased LDL Decreasing non-calcified plaque in proximal left anterior descending (LAD) coronary artery in patient on atorvastatin for 12 months. p = 0. 005 0 -20 -40 -60 -80 -100 Placebo Atorvastatin Decreased Lp. PLA 2: marker of vascular inflammation Lo, Lancet HIV 2015 42

Challenges in Applying ACC/AHA Cholesterol Guidelines to HIV Dose-adjustment in HIV (with PIs) Awaiting further study in HIV Contraindicated in HIV (with PIs) Stone Circulation 2014 43

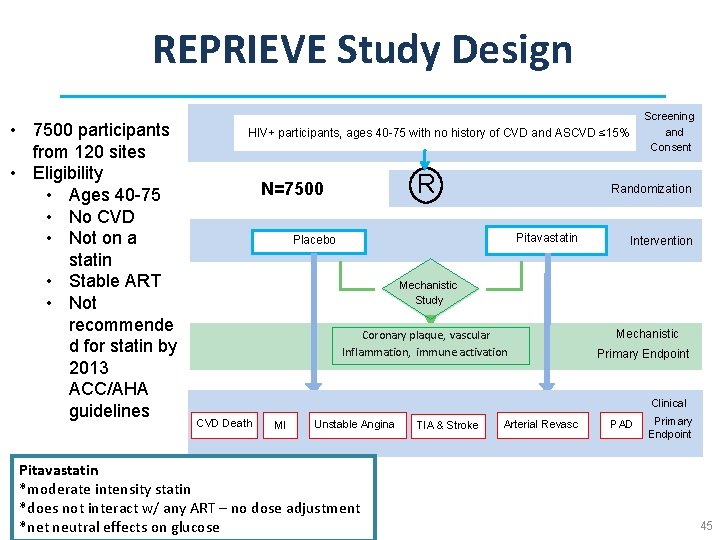
www. reprievetrial. org • The first large-scale randomized clinical trial to test a strategy for preventing heart-related disease among PLWH • Hypothesis: statins will prevent CVD in HIV-infected patients, among participants at low-moderate risk not meeting current guidelines for clinical use of statins but at risk based on unique features of HIV 44

REPRIEVE Study Design • 7500 participants from 120 sites • Eligibility • Ages 40 -75 • No CVD • Not on a statin • Stable ART • Not recommende d for statin by 2013 ACC/AHA guidelines Screening and Consent HIV+ participants, ages 40 -75 with no history of CVD and ASCVD ≤ 15% R N=7500 Randomization Pitavastatin Placebo Intervention Mechanistic Study Coronary plaque, vascular Inflammation, immune activation Mechanistic Primary Endpoint Clinical CVD Death MI Unstable Angina Pitavastatin *moderate intensity statin *does not interact w/ any ART – no dose adjustment *net neutral effects on glucose TIA & Stroke Arterial Revasc PAD Primary Endpoint 45

Clinical Strategies • Early patient education to modify lifestyle (keep it simple, address barriers) – – Weight maintenance Diet modification Smoking cessation Physical activity • Monitor for dyslipidemia – Check fasting lipids • At HIV diagnosis • Prior to and within 1 -3 months after starting or changing ART • Every 6 -12 months – Consider starting statin based on ACC/AHA cholesterol guidelines – Consider fibrate if triglycerides >500 mg/d. L Dube CID 2003; Aslangul AIDS 2010; Aberg CID 2014 46

Clinical Strategies • Diabetes – Check fasting glucose or Hb. A 1 c at HIV diagnosis, 103 months after starting or changing ART, and every 6 -12 months – Hb. A 1 c may be used for screening • Consider cutoff 5. 8% • Hb. A 1 c may underestimate glycemia in HIV – Check Hb. A 1 c every 6 months in DM • Hypertension – Check blood pressure annually – Follow existing Hypertension Guidelines for the general population • No HIV-specific guidelines – Consider drug interactions • Use of some calcium-channel blockers contraindicated with PIs Aberg CID 2014; Lundgren HIV Med 2008 47

Novel Interventions Targeting Inflammation and Immune Activation • • • ART treatment intensification Methotrexate CCR 5 antagonists Rifaximin Sevelamer Mesalamine Pentoxifylline Hydroxychloroquine IL-1β inhibition with canakinumab Hatano JAIDS 2012; Gahdhi JAIDS 2012; Stein JAMA 2012; Jones Br J Pharmacol 2011; Cipriani Circulation 2013; Tenorio CROI 2014; Sandler JID 2014; Somsouk CROI 2014; Gupta PLo. S One 2013; Paton JAMA 2012 48

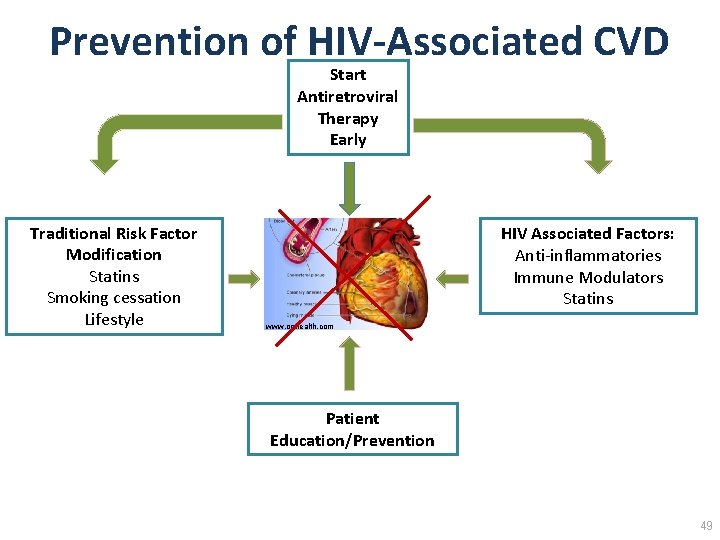
Prevention of HIV‐Associated CVD Start Antiretroviral Therapy Early Traditional Risk Factor Modification Statins Smoking cessation Lifestyle HIV Associated Factors: Anti-inflammatories Immune Modulators Statins www. onhealth. com Patient Education/Prevention 49

Implications and Questions • There is a significant impact of CVD in HIV populations that is related to inflammation and immune activation • Current treatment guidelines do not reflect this pathophysiology • Recommended strategies – Treat HIV infection to reduce CVD risk – Build CVD risk assessment into practice—understanding limitations – Educate about traditional CVD risk factors early and manage risk factors aggressively (smoking cessation) – Start appropriate statin if needed • Future questions – How is CVD risk most accurately predicted in HIV? – What is the role of statins and immunomodulatory agents to reduce CVD risk in HIV? – Should HIV be considered a CV risk equivalent? 50

Questions? 51