Cardiovascular Blueprint PANCE Blueprint Dilated Cardiomyopathy Defined as
Cardiovascular Blueprint PANCE Blueprint
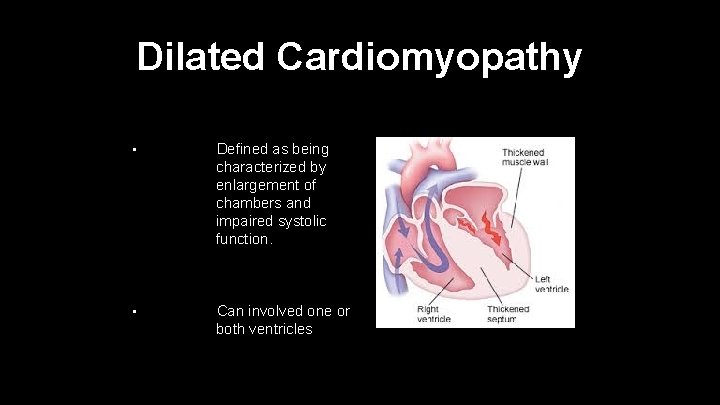
Dilated Cardiomyopathy • Defined as being characterized by enlargement of chambers and impaired systolic function. • Can involved one or both ventricles
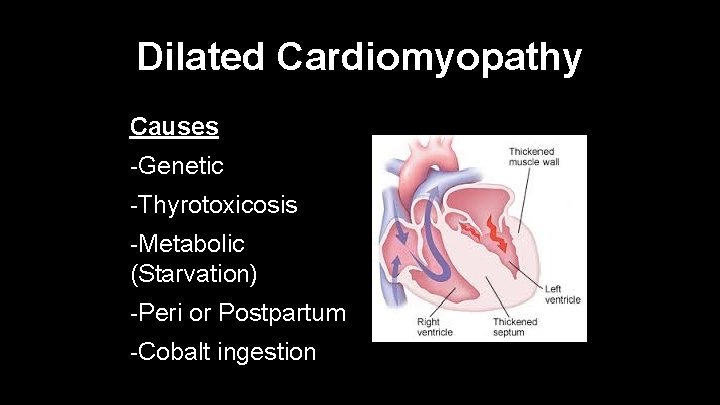
Dilated Cardiomyopathy Causes -Genetic -Thyrotoxicosis -Metabolic (Starvation) -Peri or Postpartum -Cobalt ingestion
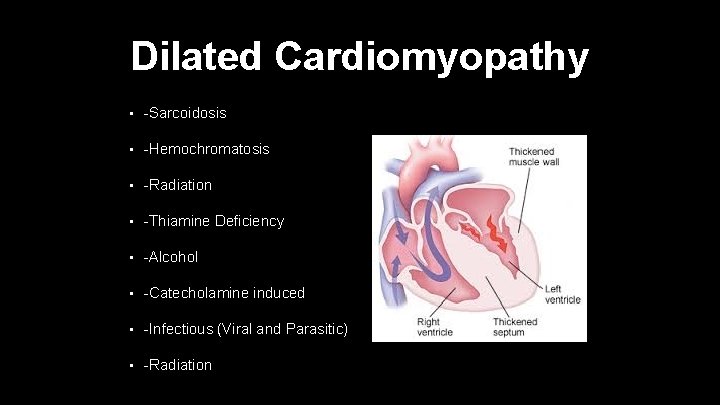
Dilated Cardiomyopathy • -Sarcoidosis • -Hemochromatosis • -Radiation • -Thiamine Deficiency • -Alcohol • -Catecholamine induced • -Infectious (Viral and Parasitic) • -Radiation

Dilated Cardiomyopathy Big Picture-can be idiopathic but can be caused by ingestion of toxins, radiation, infection, or metabolic disorders -Physical Exam similar to a patient with heart failure -EKG may show some LVH or RVH -ECHO is necessary for diagnosis -Cardiac biopsy only for those who may have treatable cause -Treatment is similar to heart failure targeted at increasing preload and decreasing afterload. -ACE inhibitors and Beta Blockers are ideal for those patients who can tolerate them
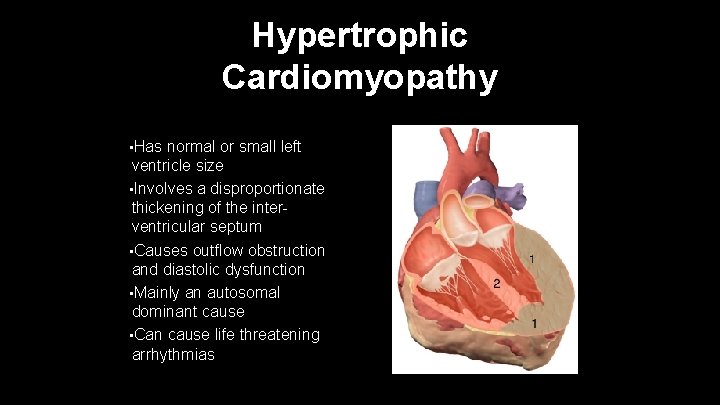
Hypertrophic Cardiomyopathy • Has normal or small left ventricle size • Involves a disproportionate thickening of the interventricular septum • Causes outflow obstruction and diastolic dysfunction • Mainly an autosomal dominant cause • Can cause life threatening arrhythmias
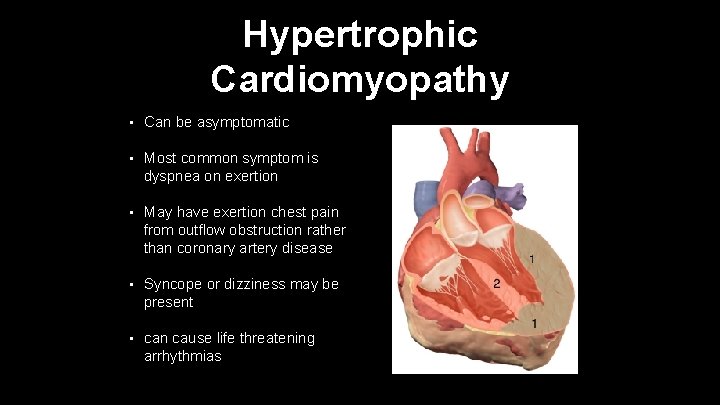
Hypertrophic Cardiomyopathy • Can be asymptomatic • Most common symptom is dyspnea on exertion • May have exertion chest pain from outflow obstruction rather than coronary artery disease • Syncope or dizziness may be present • can cause life threatening arrhythmias

Hypertrophic Cardiomyopathy • Can hear an S 3 if left ventricular systolic problems. S 4 gallop from increased ventricular stiffness • ECHO is needed for diagnostic confirmation and to determine the severity • May need cath to rule out concomitant coronary artery disease • Treatment is targeted at improving diastolic dysfunction • Calcium channel blockers are ideal • Beta blockers can be used to • These increase preload and allow the ventricle to fill better
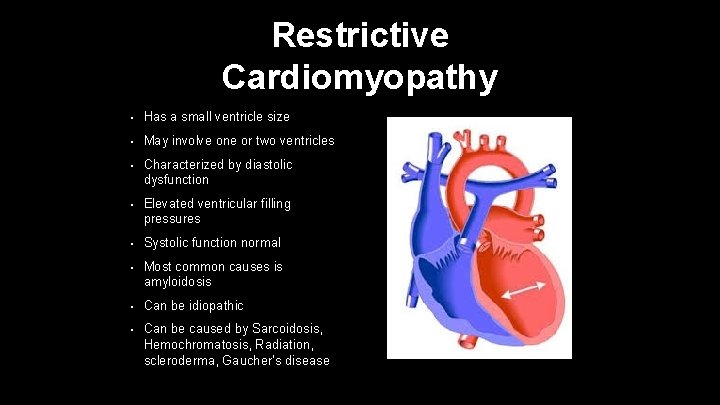
Restrictive Cardiomyopathy • Has a small ventricle size • May involve one or two ventricles • Characterized by diastolic dysfunction • Elevated ventricular filling pressures • Systolic function normal • Most common causes is amyloidosis • Can be idiopathic • Can be caused by Sarcoidosis, Hemochromatosis, Radiation, scleroderma, Gaucher’s disease

Restrictive Cardiomyopathy Physical exam-signs of right heart failure are present Elevated right sided heart pressures and dilated neck veins ECHO is needed in the diagnosis Right heart cath sometimes needed to make sure it is not constrictive pericarditis Treatment is similar to heart failure Diuretics help decrease systemic vascular resistance

Cardiomyopathy Summary Dilated Cardiomyopathy-systolic dysfunction, may affect one or both ventricles. Symptoms similar to CHF. Dilated chambers Hypertrophic Cardiomyopathy-diastolic problem, small chambers can cause outflow obstruction. Can cause DOE or chest pain with activity Restrictive Cardiomyopathy-diastolic problem, elevated right heart pressures, amyloidosis most common cause, treatment similar to heart failure
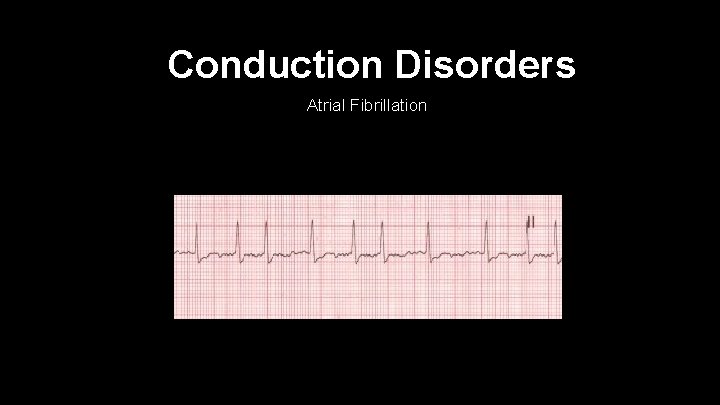
Conduction Disorders Atrial Fibrillation

Atrial Fibrillation • Irregularly, irregular rhythm • Fibrillation is caused by rapid discharges from numerous ectopic foci • The rate is 350 -450 per minute of atrial discharges • Goal INR is between 2. 0 -3. 0 • Rate control is key. Cardizem, Beta Blockers and Digoxin are helpful • If patient not anti-coagulated, risk for cerebral vascular event • IV Cardizem good for A-Fib with RVR
Atrial Flutter

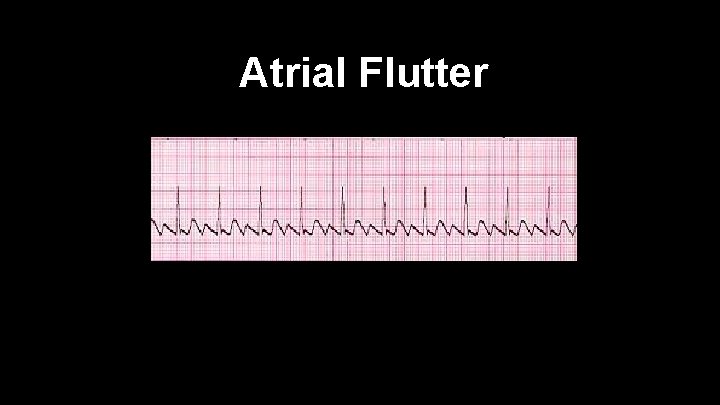
Atrial Flutter Characterized by saw tooth pattern at baseline Atrial rate fires at rate of 250 -350 per minute Can have a 2: 1 to 4: 1 conduction delay Treated just like A-Fib
First Degree AV Block

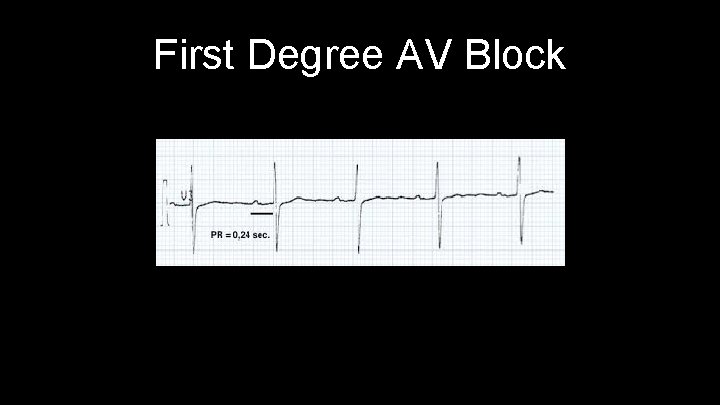
First Degree AV Block Characterized by lengthened PR interval greater than 0. 2 seconds Something blocking the conduction through the AV node No dropped QRS complexes No Treatment Necessary
Second Degree AV Block Type I

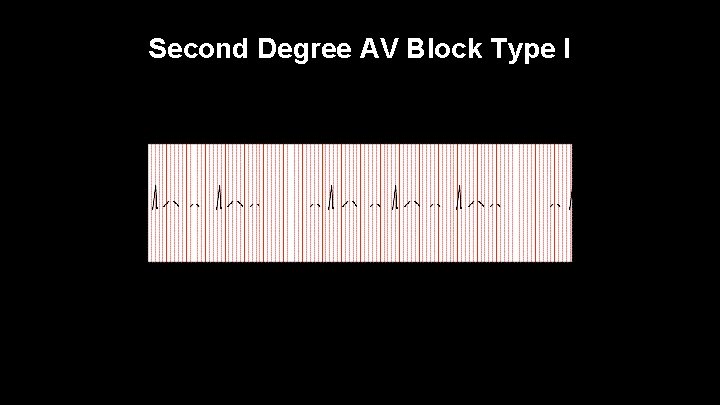
Second Degree AV Block Type I Also called Wenckebach/Mobitz Type I Characterized by lengthening PR interval until the QRS complex drops This rhythm usually does not cause symptoms Usually just observe
Second Degree AV Block Type II

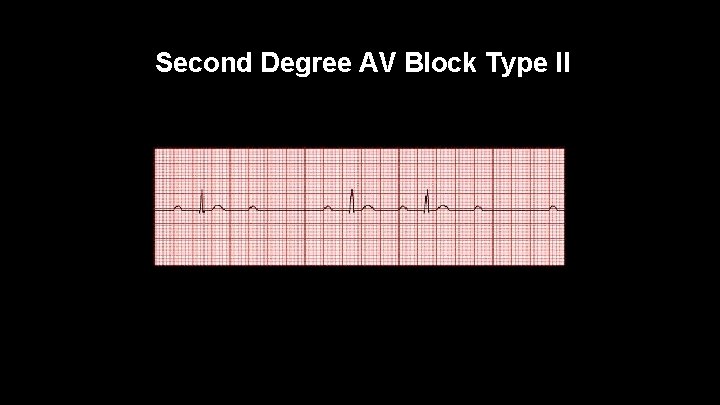
Second Degree AV Block Type II Characterized by normal PR interval and a dropped QRS Complex Also called Mobitz Type II Usually symptomatic and can be associated with syncope or pre syncope May progress to 3 rd Degree Block It may be present because of ischemia or infarction Can be caused by medications that slow heart

Third Degree AV Block

Third Degree AV Block Also called complete heart block None of the atrial impulses conduct to the ventricles Key characteristics is the P waves are equal distance and QRS complex are equal distance with calipers. They are dissociated. Can be caused from congenital abnormality, infection, post op problem, or structural problem Needs a pacer

Bundle Branch Blocks

Right Bundle Branch Block • -If there is a R, R' waves in V 1 or V 2 there is a right bundle branch block • -If it is only present in one of the leads it is an incomplete right bundle branch block
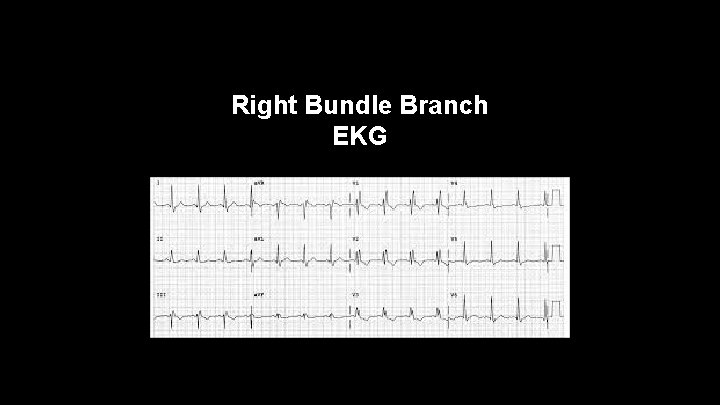
Right Bundle Branch EKG

Left Bundle Branch Block • -Sometimes the R R' waves will only be seen as notch in the wide QRS complex in V 5 and V 6 • -In a left bundle branch block the left ventricle fires late so the first portion of the QRS complex is right ventricle activity. We cannot see Q waves originating from the left ventricle because they are buried in the QRS complex
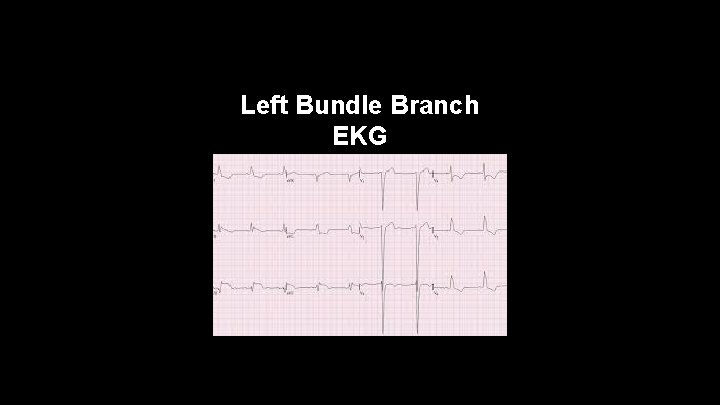
Left Bundle Branch EKG

Hemi-blocks • -These are blocks of the anterior and posterior division of the left bundle branch • -These are mostly due to loss of blood supply to the anterior or posterior branches of the left bundle branch

Paroxysmal Supraventricular Tachycardia (PSVT) • A rapid sudden heart rate originating from an ectopic focus from on of the atria. The rate is usually between 150 -250 beats per minute. • Narrow complex tachycardia
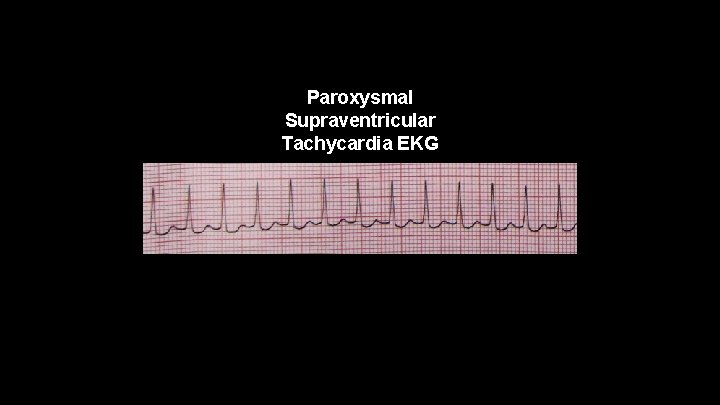
Paroxysmal Supraventricular Tachycardia EKG

Premature Beats

Premature Atrial Contractions • Premature Atrial Contraction (PAC)-originates from an ectopic focus in the atrium that appears much earlier than normal P wave on an EKG • Compensatory pause after beat
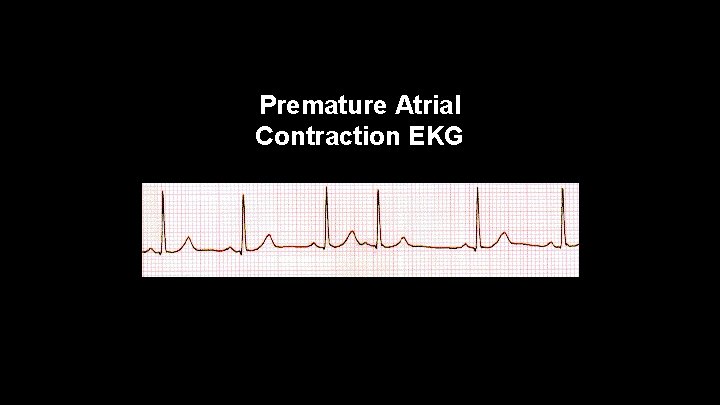
Premature Atrial Contraction EKG

Premature Junctional Contractions (PJC’s) • Originates in an ectopic focus in the AV junction which fires before the normal cycle. Usually inverted P wave occurring before, during, or immediately after the QRS complex • Compensatory pause after beat
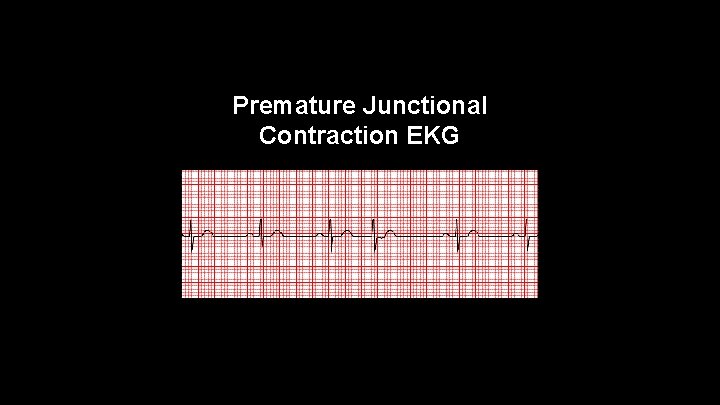
Premature Junctional Contraction EKG

Premature Ventricular Contraction (PVC) • originates from an ectopic focus, and occurs very early before a P wave. • has a compensatory pause
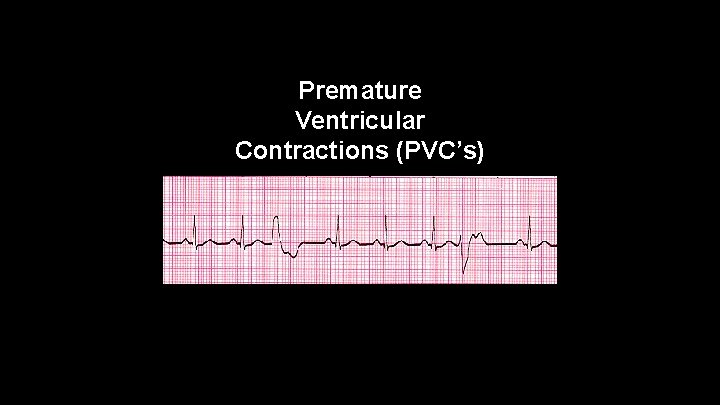
Premature Ventricular Contractions (PVC’s)

Sick Sinus Syndrome • an unhealthy SA node quits pacing activity for at least one complete cycle. The P waves before and after the block are identical because the same SA node pacemaker is functioning before and after the pause.
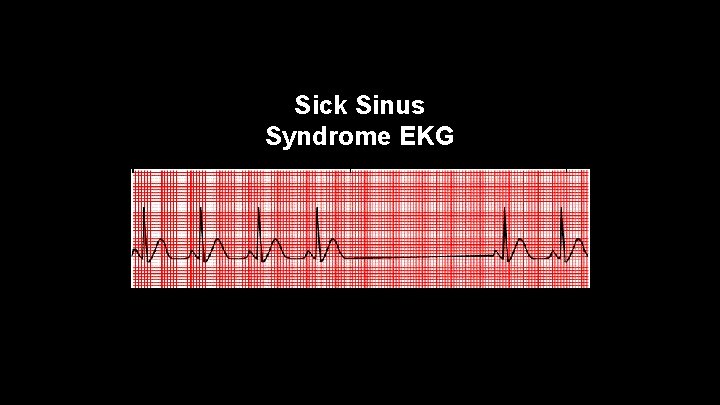
Sick Sinus Syndrome EKG

Ventricular Tachycardia • -appears like a run of PVC's • -usually is significant for coronary artery disease or poor oxygenation of the coronaries • -originates from a single ventricular ectopic focus • -rate 150 -250 beats per minute
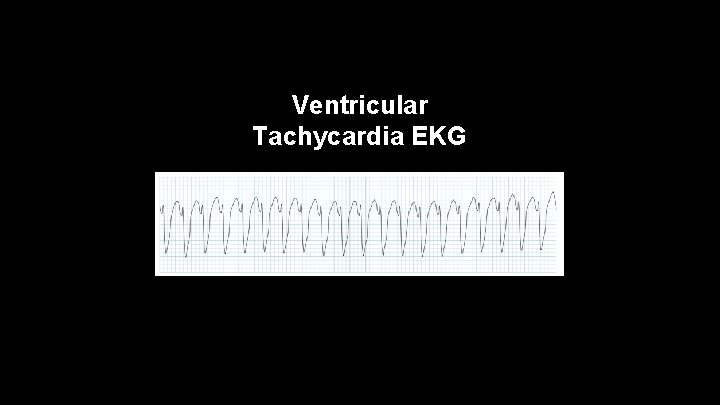
Ventricular Tachycardia EKG

Ventricular Fibrillation • -disorganized rhythm of multiple ectopic ventricular foci • -needs to be defibrillated
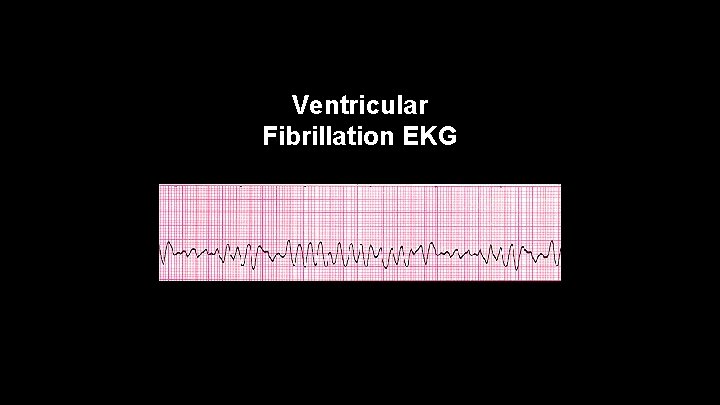
Ventricular Fibrillation EKG

Torsades de Pointes • -Essentially V-Fib. Needs defibrillated. • -"Turning on a point" • -Can be from magnesium deficiency
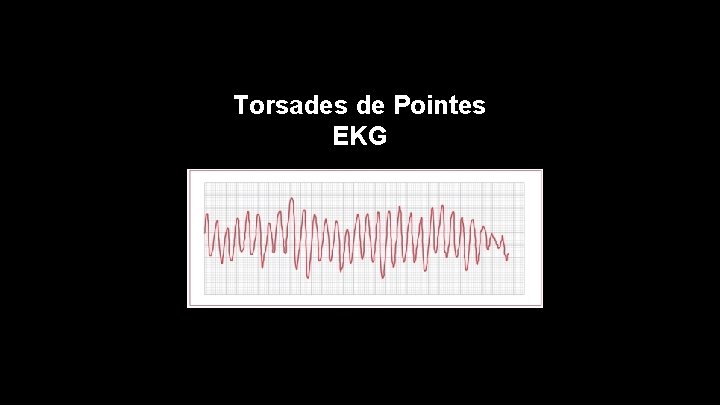
Torsades de Pointes EKG

Congenital Heart Defects
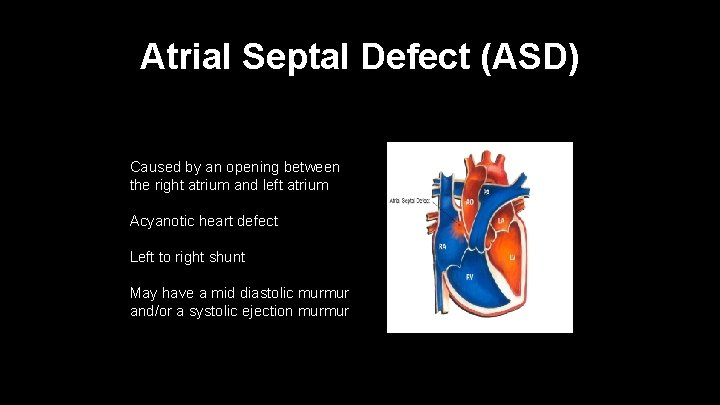
Atrial Septal Defect (ASD) Caused by an opening between the right atrium and left atrium Acyanotic heart defect Left to right shunt May have a mid diastolic murmur and/or a systolic ejection murmur
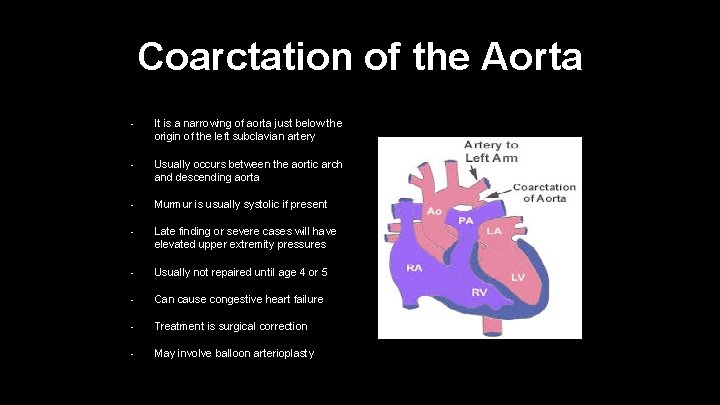
Coarctation of the Aorta • It is a narrowing of aorta just below the origin of the left subclavian artery • Usually occurs between the aortic arch and descending aorta • Murmur is usually systolic if present • Late finding or severe cases will have elevated upper extremity pressures • Usually not repaired until age 4 or 5 • Can cause congestive heart failure • Treatment is surgical correction • May involve balloon arterioplasty
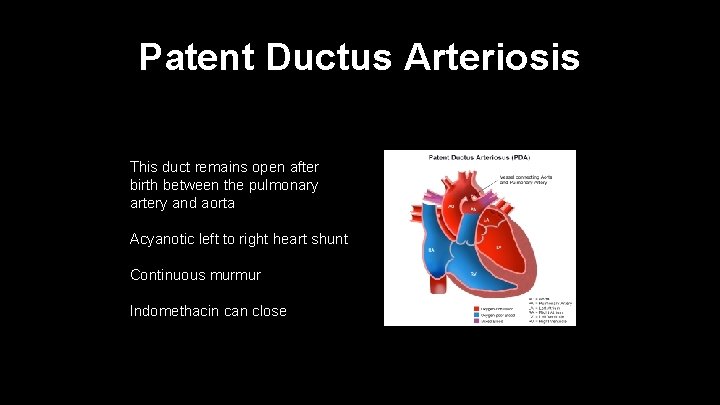
Patent Ductus Arteriosis This duct remains open after birth between the pulmonary artery and aorta Acyanotic left to right heart shunt Continuous murmur Indomethacin can close
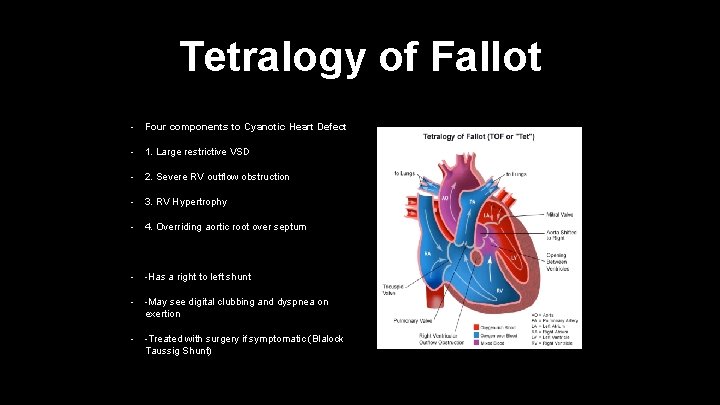
Tetralogy of Fallot • Four components to Cyanotic Heart Defect • 1. Large restrictive VSD • 2. Severe RV outflow obstruction • 3. RV Hypertrophy • 4. Overriding aortic root over septum • -Has a right to left shunt • -May see digital clubbing and dyspnea on exertion • -Treated with surgery if symptomatic (Blalock Taussig Shunt)
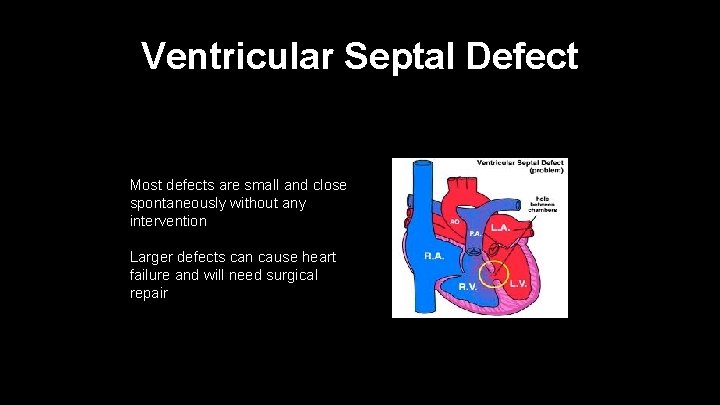
Ventricular Septal Defect Most defects are small and close spontaneously without any intervention Larger defects can cause heart failure and will need surgical repair

Heart Failure
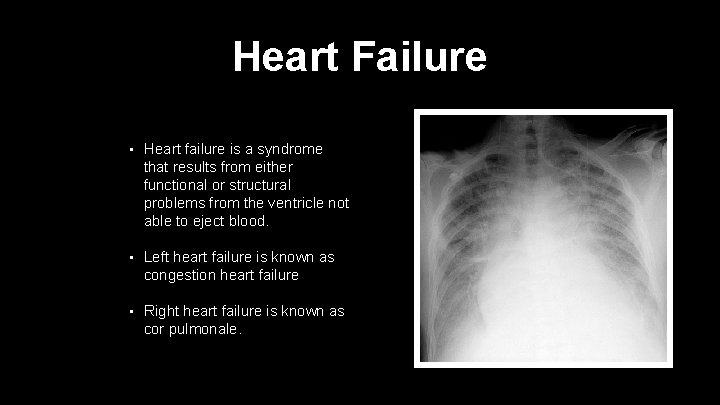
Heart Failure • Heart failure is a syndrome that results from either functional or structural problems from the ventricle not able to eject blood. • Left heart failure is known as congestion heart failure • Right heart failure is known as cor pulmonale.

Heart Failure • Heart Failure can be caused by problems with myocardium, heart valves, blood vessels, pericardium problems, endocardial problems, or other metabolic disorders. • Patients who have a left Ventricular ejection fraction less than 40 percent have systolic heart failure • Patients who have a left ventricular ejection fraction greater than 40 percent have diastolic heart failure

Heart Failure • New York Heart Association (NYHA) Classes of CHF- • Class I-Patients with heart disease without resulting in limitation of physical activity • Class II-Patients with heart disease with slight limitation of physical activity. No symptoms at rest • Class III-Patient with heart disease with marked limitation of physical activity. No symptoms at rest • Class IV-Patients with heart disease results in the inability to carry on physical activity without discomfort
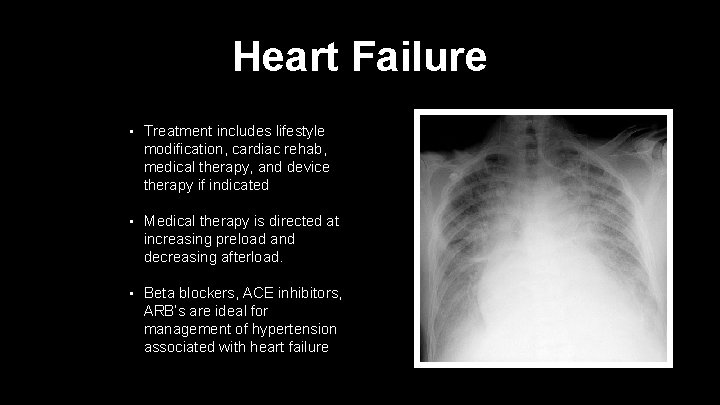
Heart Failure • Treatment includes lifestyle modification, cardiac rehab, medical therapy, and device therapy if indicated • Medical therapy is directed at increasing preload and decreasing afterload. • Beta blockers, ACE inhibitors, ARB’s are ideal for management of hypertension associated with heart failure

Heart Failure • Patients need to stop smoking, reduce alcohol consumption, and reduce drug use • Salt restriction is generally recommended • Weight reduction to be within 10 percent of ideal body weight • AICD may be indicated for those with documented ventricular arrhythmias • Loop diuretics are recommended with those that are volume overloaded or have pulmonary edema • Digoxin can help with rate control and inatropic activity.
Hypertension -For adults over 18 defined as SBP > 140 mm Hg and DBP > 90 mm. Hg -Diagnosis requires elevated reading on 3 separate visits -Essential HTN known as Primary Hypertension -Defined as hypertension with no identifiable cause

Secondary Hypertension • Caused by an underlying problem • -Renal Parenchymal Disease • -Renal Artery Stenosis • -Aortic Coarctation • -Carcinoid Syndrome • -Pregnancy • -Hypothyroid or Hyperthyroidism • -Hyperparathyroidism • -Cushing Syndrome • -Pheochromocytoma

Secondary HTN Causes • Hormone Replacement Therapy • Brain Tumor • Pain, stress, and anxiety • Sleep Apnea • Porphyria • Lead Poisoning

Secondary Causes Hypertension • Hypoglycemia • Alcohol withdrawal • NSAIDS • Alcohol • Ephedrine • MAO inhibitors • Corticosteroids
Hypertension Treatment • HTN Treatment • Lifestyle Modifications • JNC Guidelines • Stage I HTN (SBP 140 -159 or DBP 90 -99) Thiazide Diuretics first • May also consider ACE inhibitors, ARB’s, Beta Blockers or Calcium Channel Blockers • Stage 2 HTN (SBP >160 mm. Hg or DBP >100 mm. Hg) • 2 Drug Combination for most • Combination with ACE inhibitor, ARB, Beta Blocker or Calcium Channel Blockers

Accelerated Hypertension Also known as hypertensive urgency SBP >200 mm. Hg and DBP >120 mm. Hg. May need admitted

Hypertensive Urgency When patients have elevated blood pressure (>200 SBP and DBP > 120 mm. Hg) and have evidence of end organ damage May reverse when BP is lowered
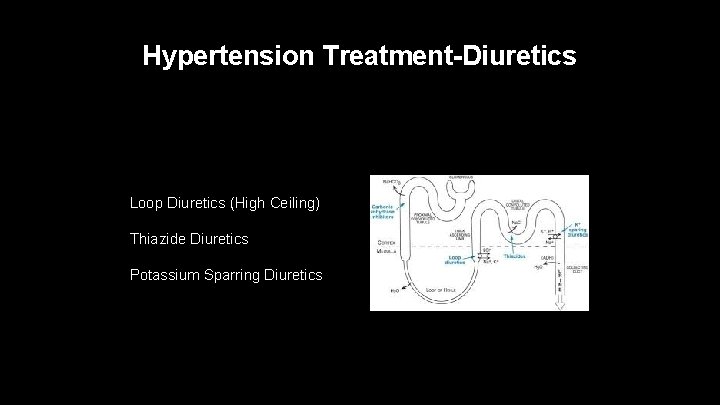
Hypertension Treatment-Diuretics Loop Diuretics (High Ceiling) Thiazide Diuretics Potassium Sparring Diuretics

Loop Diuretics Furosemide, Demedex and Bumex Mechanism-works on the ascending loop of Henle to block reabsorption of sodium and chloride This then prevents passive reabsorption of water Reserved for when there is a need for fluid removal Adverse Effects-hyponatremia, dehydration, hypotension, hypokalemia, ototoxicity, hyperglycemia, and elevated uric acid levels

Thiazide Diuretics Hydrochlorothiazide (Hctz) Mechanism-blocks the reabsorption of sodium and chloride in the early segment of the distal convoluted tubule This passively causes an increase of flow of water and increased urinary output Generally considered first line in essential hypertension Other indication is benign peripheral edema Adverse effects-low Na, Cl, and low K. Also dehydration, hyperglycemia, and elevated uric acid levels

Potassium Sparing Diuretics -Spironolactone and Triamterene -Mechanism-blocks the sodium potassium exchange in the distal nephron -Indicated for hypertension or benign peripheral edema -Adverse Effects -hyperkalemia, leg cramps, and dizziness Caution when in use with ACE inhibitors

Osmotic Diuretics Mannitol Mechanism-creates osmotic force within the lumen of the nephron Indications reduction of intracranial pressure (ICP), intraocular pressure, and prophylaxis of renal failure Adverse Effects Headache Nausea and Vomiting Fluid and electrolyte imbalances
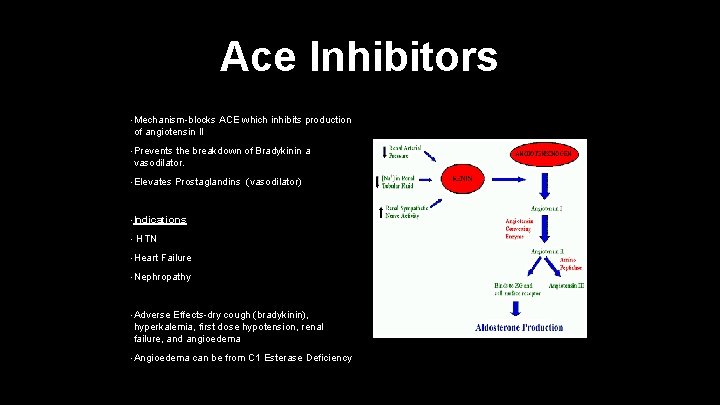
Ace Inhibitors • Mechanism-blocks ACE which inhibits production of angiotensin II • Prevents the breakdown of Bradykinin a vasodilator. • Elevates Prostaglandins (vasodilator) • Indications • HTN • Heart Failure • Nephropathy • Adverse Effects-dry cough (bradykinin), hyperkalemia, first dose hypotension, renal failure, and angioedema • Angioedema can be from C 1 Esterase Deficiency

Angiotensin Receptor Blockers (ARB’s) • Block • No Angiotensin II Receptor elevated Bradykinin Elevation • Vasodilator • Indications • Hypertension • Heart Failure • Myocardial • Renal Infarction Impairment • Adverse Effects • Dizziness • No dry cough because of no Bradykinin elevation

Calcium Channel Blockers (CCB’s) Classifications -Dihydropyridines (Nifedipine) -Non Dihydropyridines -Phenylalkamines (Verapamil) -Benzothiazepines (Diltazem)

Calcium Channel Blockers -Dihydropyridines-dilate arterioles. Nifedipine, Amlodipine, Nicardipine, and Felodipine -Non Dihydropyridines- diltazem and verapamil block calcium channels in the heart and arterioles (slows heart and dilates arterioles) -Adverse Effects-constipation, bradycardia, edema, AV Blocks -Can also cause gingival hyperplasia -Diltazem and Verapamil good for rate control with Atrial Fibrillation -Verapamil used for Prinzmetal’s Angina

Vasodilators Hydralazine-selectively dilates arterioles Indications-HTN, Hypertensive crisis, and Heart Failure Adverse effects-reflex tachycardia, increase in blood volume, and hypotension, and dizziness

Nitroprusside Dilates the venous and arterial systems. Used for hypertensive urgency Metabolizes can accumulate and cause cyanide poisoning. Adverse effect-hypotension, cyanide poisoning and thiocyanate toxicity

Nitroglycerin Dilation of venous system predominately Used to treat angina, heart failure and myocardial infarction Oral form is isosorbide

Alpha Adrenergic Blocking Agents (ex Prazosin) Prevent stimulation of alpha adrenergic receptors on veins and arterioles Used in HTN, Peripheral Vascular Disease, and pheochromocytoma

Centrally Acting Agents (ex Methyldopa and Clonidine) Inhibit outflow of impulses along sympathetic nerves Used for hypertension Can cause rebound hypertension if discontinued abruptly.

Beta Blockers (ex Metoprolol, Atenolol, & Propranolol) Work by blocking primary Beta 1 receptors in the heart and slow heart rate Indications-HTN, MI, CAD, CHF, Tachycardia, SVT, severe recurrent VT, migraines, and stage fright Adverse effects-AV block, bradycardia, bronchospasm, heart failure
Hypotension
Cardiogenic Shock • -Defined as widespread failure of inadequate tissue perfusion resulting in metabolic demands not being met • -Caused by inadequate cardiac output • -Usually form left sided heart failure except with right ventricular infarct • -Hypotension and Tachycardia present • -Signs of left side failure-JVD, pulmonary edema, diaphoresis

Cardiogenic Shock Primary cause-myocardial ischemia Valvular dysfunction, persistent tachycardia, or trauma can cause Treat by supporting blood pressure, correcting underlying cause, and oxygenation May need to intubate and place on mechanical ventilator Support blood pressure with vasopressors (dopamine, levophed)

Orthostatic Hypotension • Means a decrease in both systolic and diastolic pressure on standing. • Most clinicians consider a 20 mm. Hg drop positive • Can be acute or chronic • Causes for acute orthostatic hypotension • anatomic • altered • drug variation body chemistry effect • -Volume depletion ***** • Antidepressants • -Physical exhaustion • Pregnancy

Orthostatic Hypotension Chronic-can be idiopathic or secondary to another disease state Diseases-adrenal insufficiency, diabetes, porphyria, intracranial tumors, cerebral infarcts, Wernicke's encephalopathy Treatment can include volume replacement, stopping offending medicine if possible, or treating underlying disease Make sure fall precautions are in place
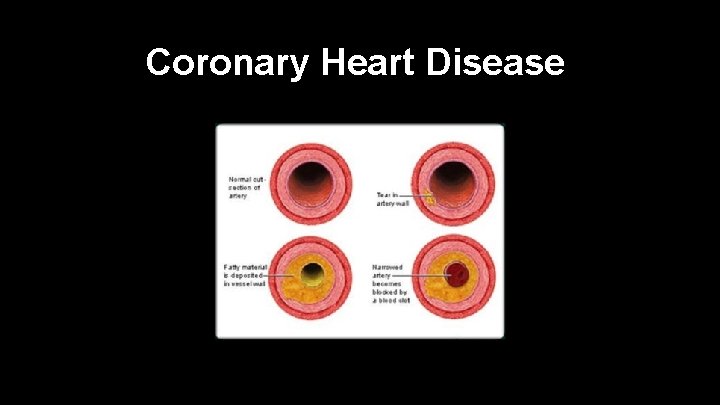
Coronary Heart Disease

CAD Risk Factors • Non Modifiable Risk Factors • Age • Male Sex • Family history of Premature Heart Disease • Hyperhomocysteinemia • High Elevated Lipoprotein A • Elevated Fibrinogen Levels • Decreased Fibrinolytic Activity

CAD Risk Factors (Modifiable) Smoking Hyperlipidemia DM HTN Obesity and Inactivity
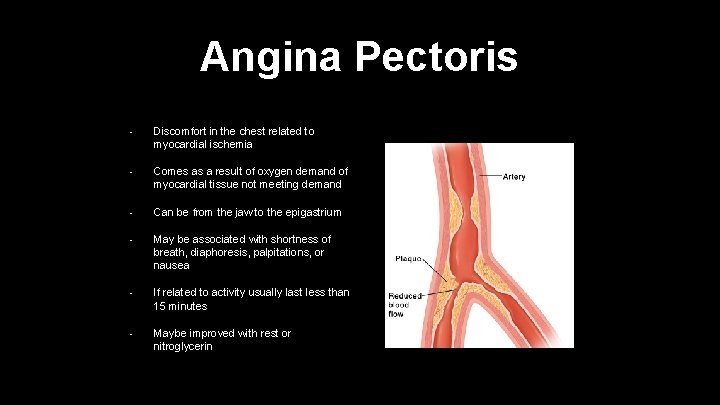
Angina Pectoris • Discomfort in the chest related to myocardial ischemia • Comes as a result of oxygen demand of myocardial tissue not meeting demand • Can be from the jaw to the epigastrium • May be associated with shortness of breath, diaphoresis, palpitations, or nausea • If related to activity usually last less than 15 minutes • Maybe improved with rest or nitroglycerin
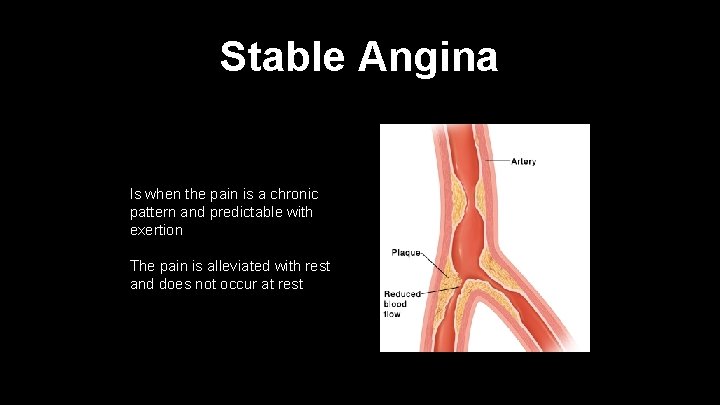
Stable Angina Is when the pain is a chronic pattern and predictable with exertion The pain is alleviated with rest and does not occur at rest
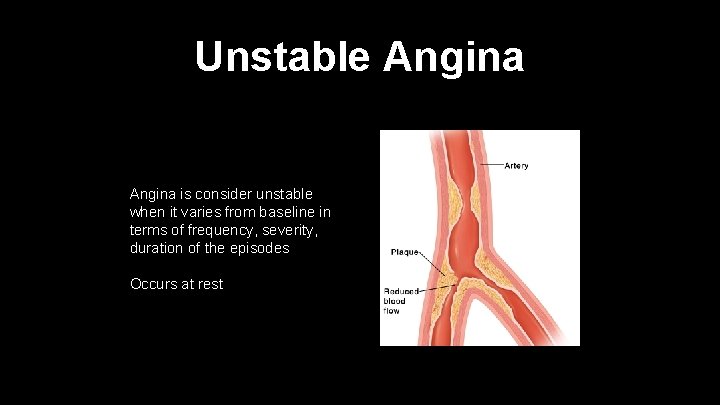
Unstable Angina is consider unstable when it varies from baseline in terms of frequency, severity, duration of the episodes Occurs at rest
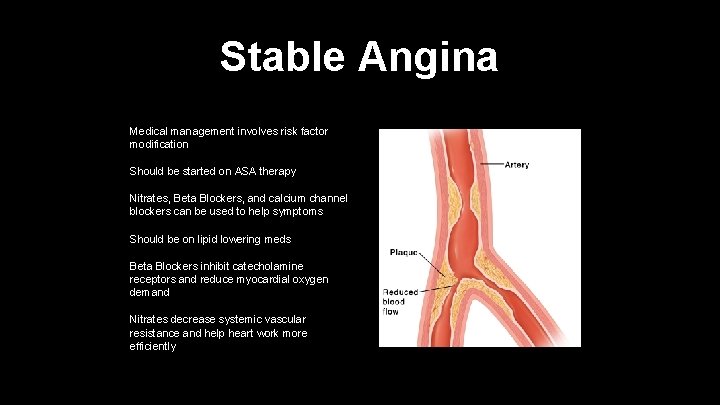
Stable Angina Medical management involves risk factor modification Should be started on ASA therapy Nitrates, Beta Blockers, and calcium channel blockers can be used to help symptoms Should be on lipid lowering meds Beta Blockers inhibit catecholamine receptors and reduce myocardial oxygen demand Nitrates decrease systemic vascular resistance and help heart work more efficiently
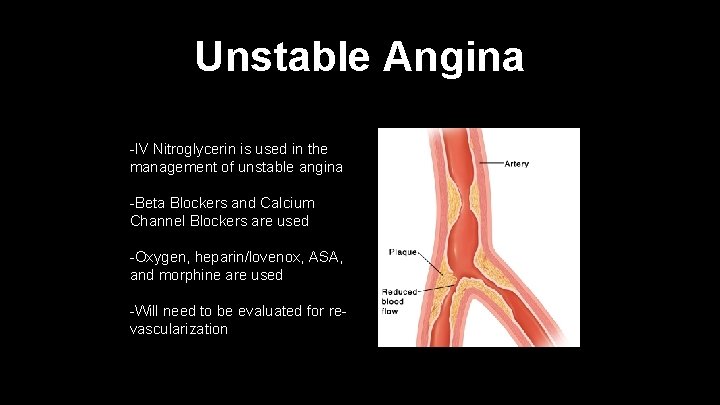
Unstable Angina -IV Nitroglycerin is used in the management of unstable angina -Beta Blockers and Calcium Channel Blockers are used -Oxygen, heparin/lovenox, ASA, and morphine are used -Will need to be evaluated for revascularization

Cardiac Catheterization Indications Unacceptable response to medical therapy Abnormal non invasive testing Angina in the setting of depressed LV function STEMI Chest pain with new onset LBBB

Prinzmetal’s Angina Also called variant angina Caused by coronary artery spasm Presents similar to angina by discomfort described as a pain and episodes tend to occur at rest Treated with calcium channel blockers
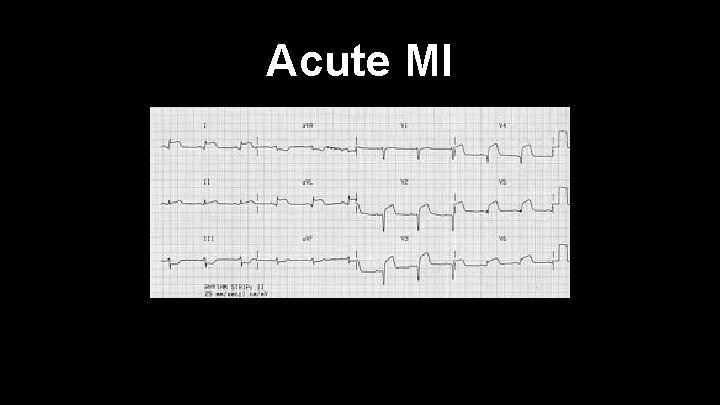
Acute MI

ST elevation MI (STEMI) EKG shows ST elevation MI in two contiguous leads New ST elevation at the J Point at least 2 contiguous leads of >2 mm is diagnostic of with chest pain New LBBB with chest pain is a STEMI Treatment-ASA 325 mg PO, O 2, Nitroglycerin, Morphine, Heparin, Beta Blockers. Also glycoprotein IIb/IIIa inhibitors Patients need reperfusion therapy ASAP TPA should be reserved for when reperfusion therapy not readily

Non ST Elevation MI Non Q Wave MI usually do not have occlusion of the infarct related coronary artery Elevated Troponin without ST elevation on EKG. Must also have Angina type chest pain Medical management involves ASA, Beta Blockers, nitrates, oxygen, and morphine Oral diltazem may decrease risk of reinfarction ACE inhibitors for those with decreased ejection fraction
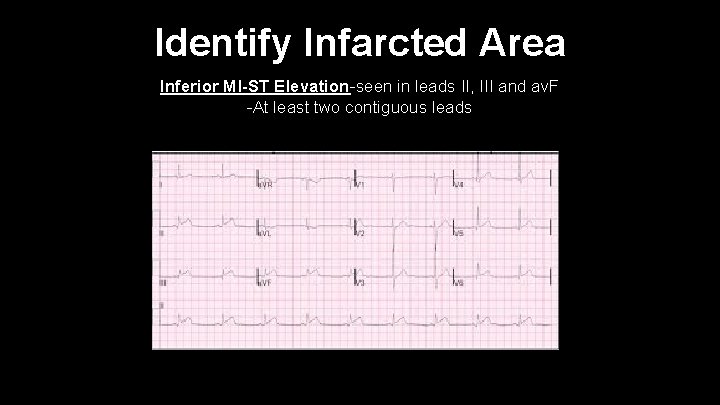
Identify Infarcted Area Inferior MI-ST Elevation-seen in leads II, III and av. F -At least two contiguous leads
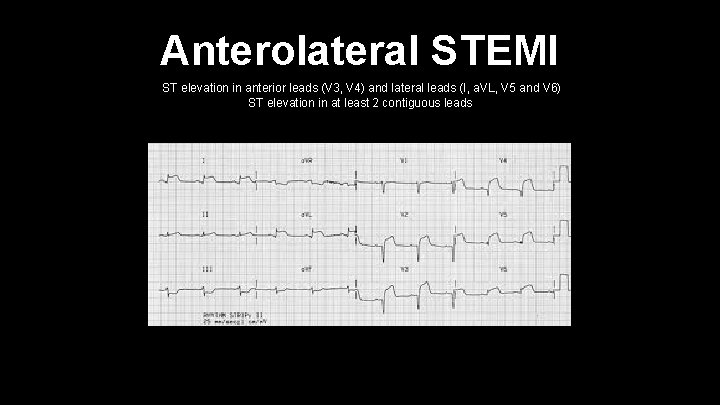
Anterolateral STEMI ST elevation in anterior leads (V 3, V 4) and lateral leads (I, a. VL, V 5 and V 6) ST elevation in at least 2 contiguous leads
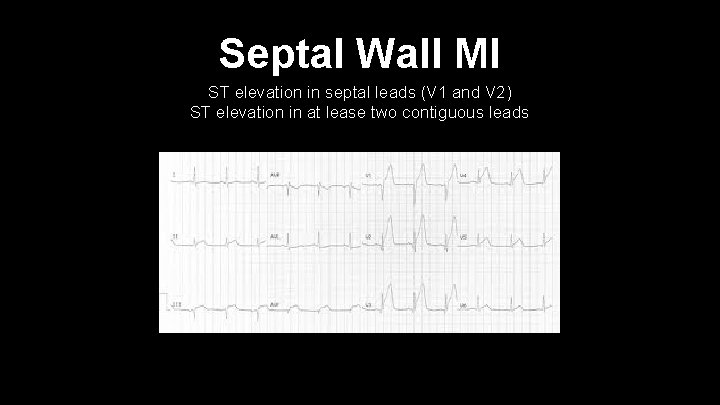
Septal Wall MI ST elevation in septal leads (V 1 and V 2) ST elevation in at lease two contiguous leads
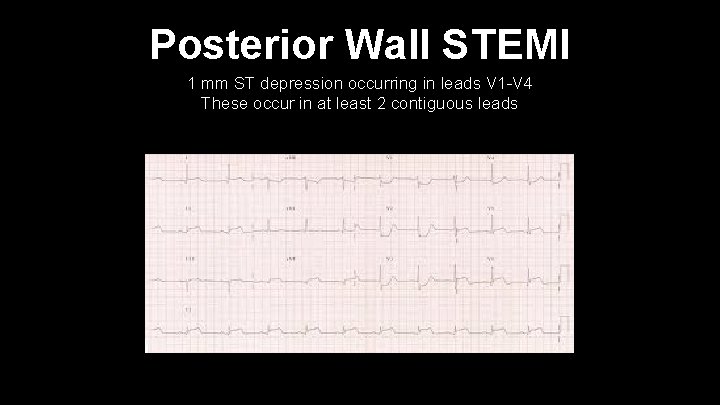
Posterior Wall STEMI 1 mm ST depression occurring in leads V 1 -V 4 These occur in at least 2 contiguous leads

Vascular Diseases
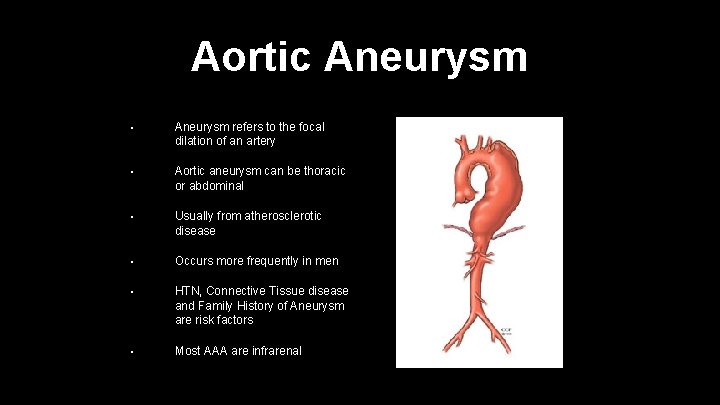
Aortic Aneurysm • Aneurysm refers to the focal dilation of an artery • Aortic aneurysm can be thoracic or abdominal • Usually from atherosclerotic disease • Occurs more frequently in men • HTN, Connective Tissue disease and Family History of Aneurysm are risk factors • Most AAA are infrarenal

Aortic Aneurysm • Diagnosis of Aneurysm can be made on ultrasound in abdomen • Transesophageal ECHO (TEE) can diagnose Thoracic Aneurysms • CT or MRI may be used to diagnose Aneurysm • CT with IV contrast or TEE needed for dissection • AAA >5 cm should be resected • Iliac artery aneurysms greater than 3 cm should be resected • May try percutaneously placed prosthetic grafts
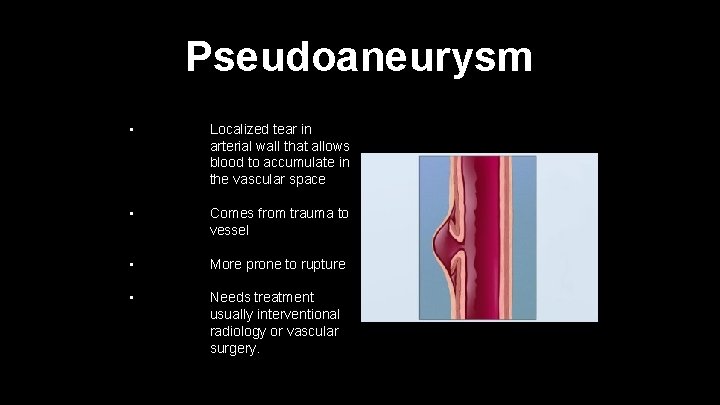
Pseudoaneurysm • Localized tear in arterial wall that allows blood to accumulate in the vascular space • Comes from trauma to vessel • More prone to rupture • Needs treatment usually interventional radiology or vascular surgery.
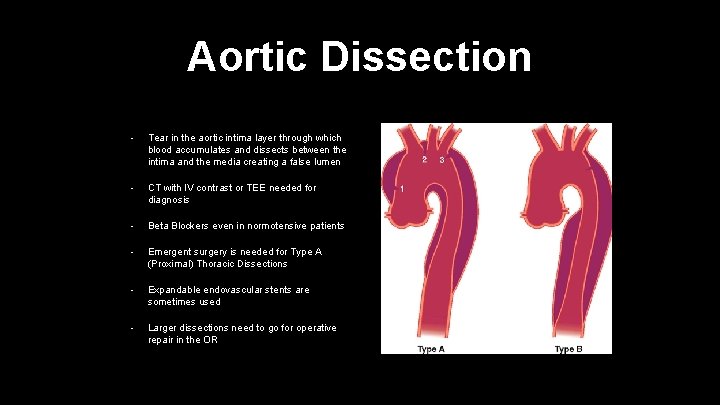
Aortic Dissection • Tear in the aortic intima layer through which blood accumulates and dissects between the intima and the media creating a false lumen • CT with IV contrast or TEE needed for diagnosis • Beta Blockers even in normotensive patients • Emergent surgery is needed for Type A (Proximal) Thoracic Dissections • Expandable endovascular stents are sometimes used • Larger dissections need to go for operative repair in the OR

Arterial Embolism & Thrombosis • Presents as sudden onset of pain involved extremity • The P’s of arterial occlusion pain, pallor, paresthesias, paralysis, and pulselessness • Emboli originate from the heart (A-Fib) or atherosclerotic changes of vessel • Thromboectomy or Thrombolysis need to be don with ischemic extremity. • Can also place stent in certain areas • Long term anticoagulation needed after revascularization • Thromboangiitis obliterans (Buerger’s Disease)-disease of small arteries and veins in upper and lower extremities • Common <40 in heavy smokers • Needs risk factor modification
Giant Cell Arteritis • May either present as Takayasu’s Arteritis or Temporal Arteritis

Takayasu’s Arteritis Usually effects young women and likes to affect the aortic arch and the great vessels Treatment is systemic corticosteroids. Surgery is rarely needed to bypass affected vascular bed

Temporal Arteritis is another type of Giant Cell Presents with temporal headaches and unilateral vision changes Presents in older patients ESR usually >100 mm/hr Definitive dx is biopsy. Treatment steroids
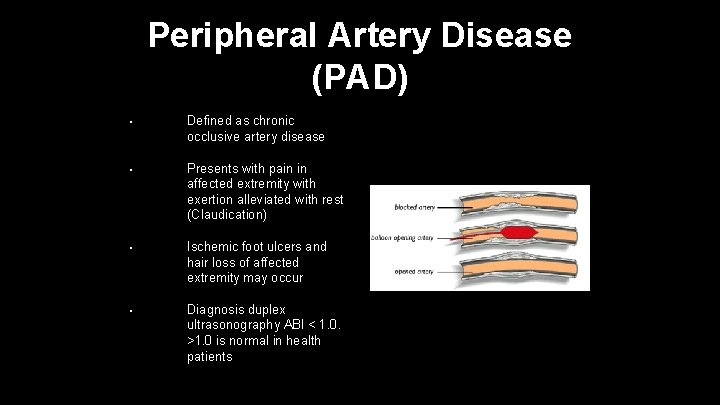
Peripheral Artery Disease (PAD) • Defined as chronic occlusive artery disease • Presents with pain in affected extremity with exertion alleviated with rest (Claudication) • Ischemic foot ulcers and hair loss of affected extremity may occur • Diagnosis duplex ultrasonography ABI < 1. 0. >1. 0 is normal in health patients

Peripheral Artery Disease (PAD) Treatment is usually conservative Pentoxifyline (vasodilation and decreased platelet aggregation) or Cilostazol (vasodilation and decreased platelet aggregation) Treatment also involves risk factor modification (smoking cessation and weight loss) Revascularization when disabling symptoms, ischemic ulceration, gangrene, or acute arterial occlusion
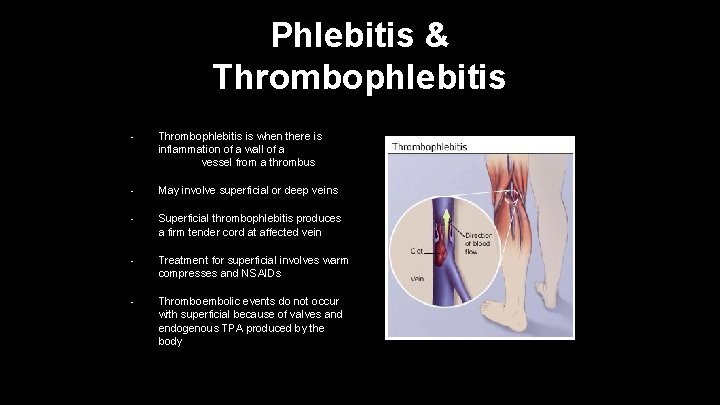
Phlebitis & Thrombophlebitis • Thrombophlebitis is when there is inflammation of a wall of a vessel from a thrombus • May involve superficial or deep veins • Superficial thrombophlebitis produces a firm tender cord at affected vein • Treatment for superficial involves warm compresses and NSAIDs • Thromboembolic events do not occur with superficial because of valves and endogenous TPA produced by the body
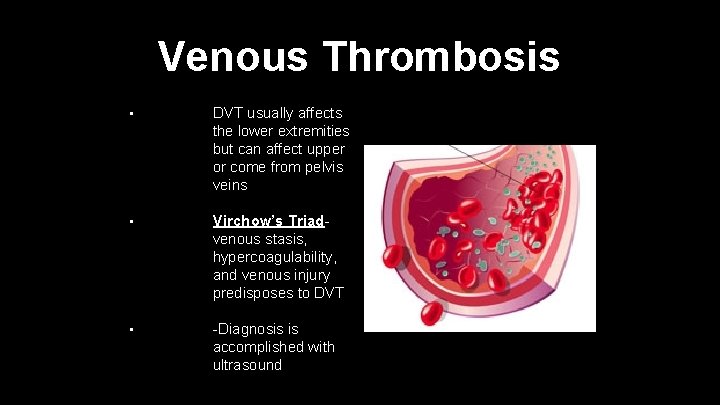
Venous Thrombosis • DVT usually affects the lower extremities but can affect upper or come from pelvis veins • Virchow’s Triadvenous stasis, hypercoagulability, and venous injury predisposes to DVT • -Diagnosis is accomplished with ultrasound

DVT Risk Factors Pregnancy and Oral Contraception (with smoking) Surgery Malignancy Immobility Inherited Hypercoagulable States Trauma Lupus anticoagulant Central Venous catheters

DVT Anticoagulation is initially accomplished with bolus of heparin or lovenox. Xarelto can also be used. Warfarin is started then until INR is 2. 0 -3. 0 Warfarin is continued for 3 -6 months Pregnancy requires lovenox. No warfarin in that it crosses placental barrier Consider repeating doppler study prior to discontinue treatment Second DVT requires lifelong treatment and/or Greenfield filter
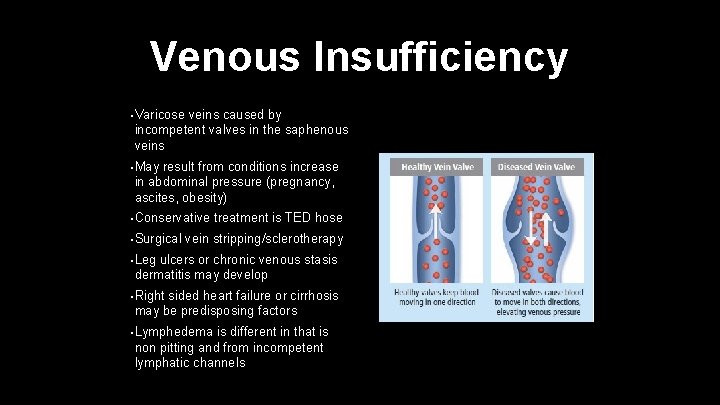
Venous Insufficiency • Varicose veins caused by incompetent valves in the saphenous veins • May result from conditions increase in abdominal pressure (pregnancy, ascites, obesity) • Conservative • Surgical treatment is TED hose vein stripping/sclerotherapy • Leg ulcers or chronic venous stasis dermatitis may develop • Right sided heart failure or cirrhosis may be predisposing factors • Lymphedema is different in that is non pitting and from incompetent lymphatic channels

Valvular Heart Disease
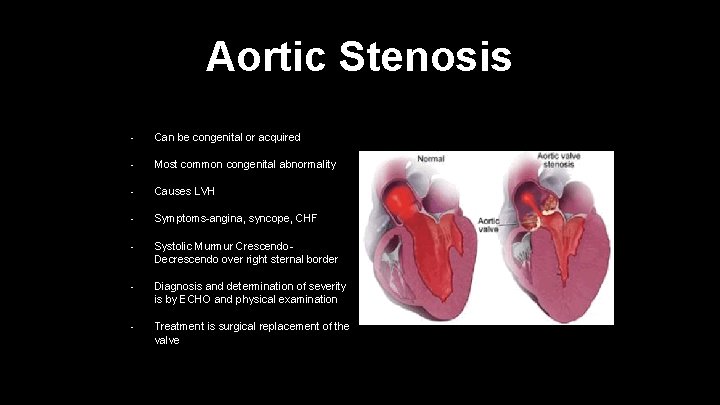
Aortic Stenosis • Can be congenital or acquired • Most common congenital abnormality • Causes LVH • Symptoms-angina, syncope, CHF • Systolic Murmur Crescendo. Decrescendo over right sternal border • Diagnosis and determination of severity is by ECHO and physical examination • Treatment is surgical replacement of the valve
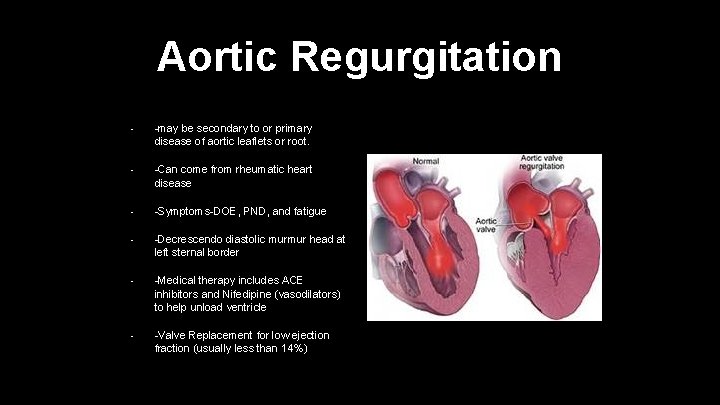
Aortic Regurgitation • -may be secondary to or primary disease of aortic leaflets or root. • -Can come from rheumatic heart disease • -Symptoms-DOE, PND, and fatigue • -Decrescendo diastolic murmur head at left sternal border • -Medical therapy includes ACE inhibitors and Nifedipine (vasodilators) to help unload ventricle • -Valve Replacement for low ejection fraction (usually less than 14%)
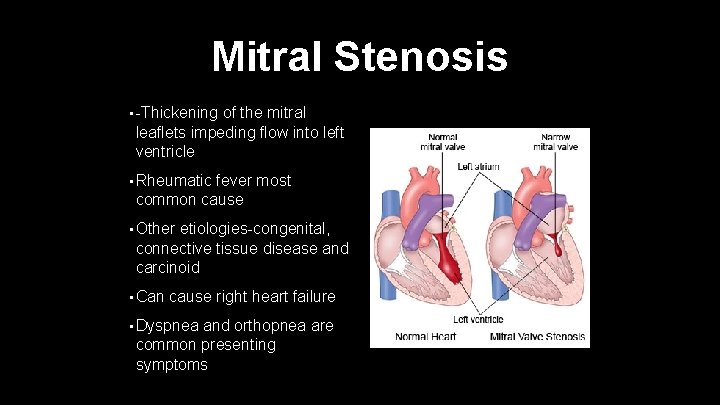
Mitral Stenosis • -Thickening of the mitral leaflets impeding flow into left ventricle • Rheumatic fever most common cause • Other etiologies-congenital, connective tissue disease and carcinoid • Can cause right heart failure • Dyspnea and orthopnea are common presenting symptoms
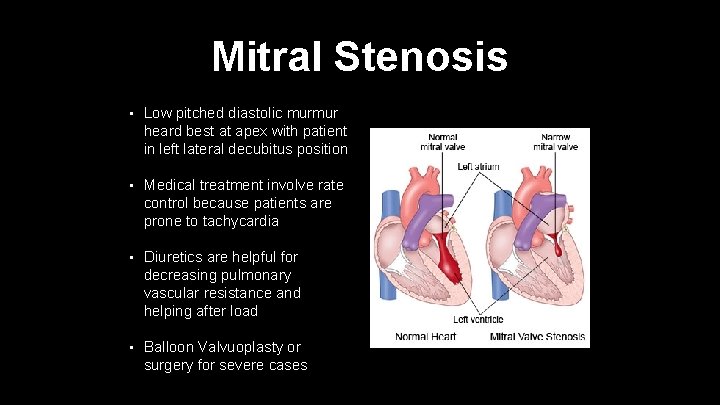
Mitral Stenosis • Low pitched diastolic murmur heard best at apex with patient in left lateral decubitus position • Medical treatment involve rate control because patients are prone to tachycardia • Diuretics are helpful for decreasing pulmonary vascular resistance and helping after load • Balloon Valvuoplasty or surgery for severe cases
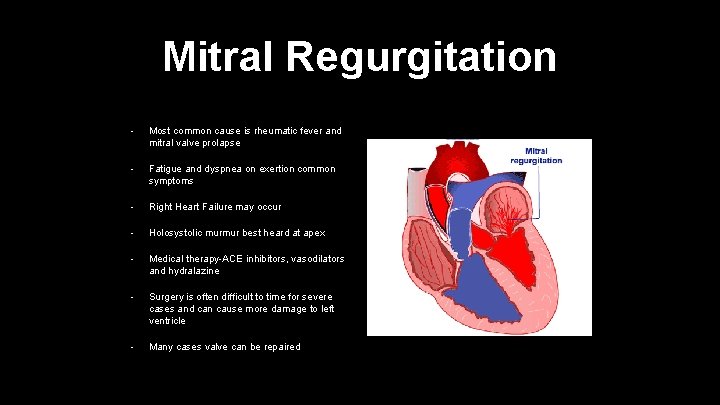
Mitral Regurgitation • Most common cause is rheumatic fever and mitral valve prolapse • Fatigue and dyspnea on exertion common symptoms • Right Heart Failure may occur • Holosystolic murmur best heard at apex • Medical therapy-ACE inhibitors, vasodilators and hydralazine • Surgery is often difficult to time for severe cases and can cause more damage to left ventricle • Many cases valve can be repaired
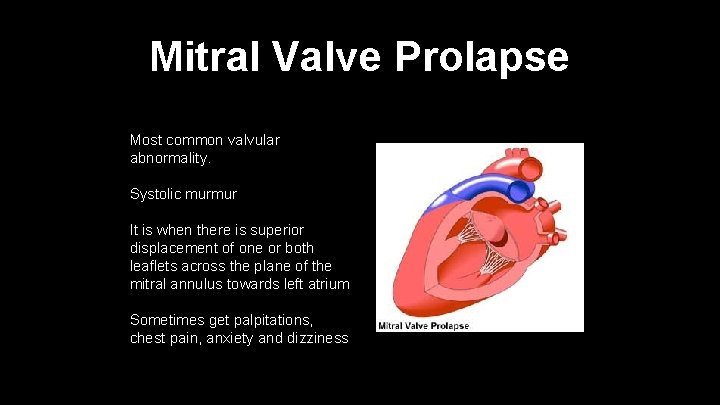
Mitral Valve Prolapse Most common valvular abnormality. Systolic murmur It is when there is superior displacement of one or both leaflets across the plane of the mitral annulus towards left atrium Sometimes get palpitations, chest pain, anxiety and dizziness
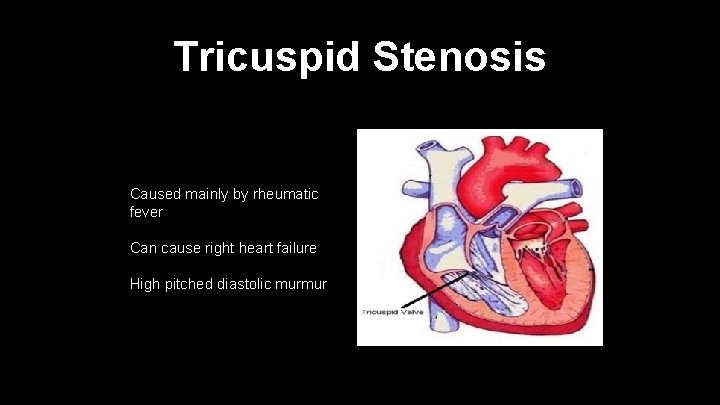
Tricuspid Stenosis Caused mainly by rheumatic fever Can cause right heart failure High pitched diastolic murmur
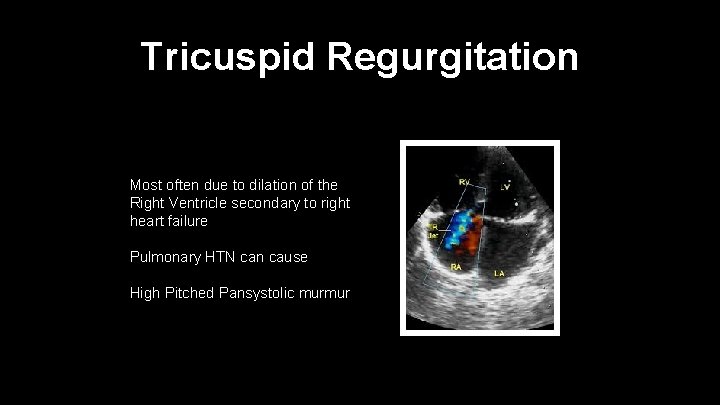
Tricuspid Regurgitation Most often due to dilation of the Right Ventricle secondary to right heart failure Pulmonary HTN can cause High Pitched Pansystolic murmur
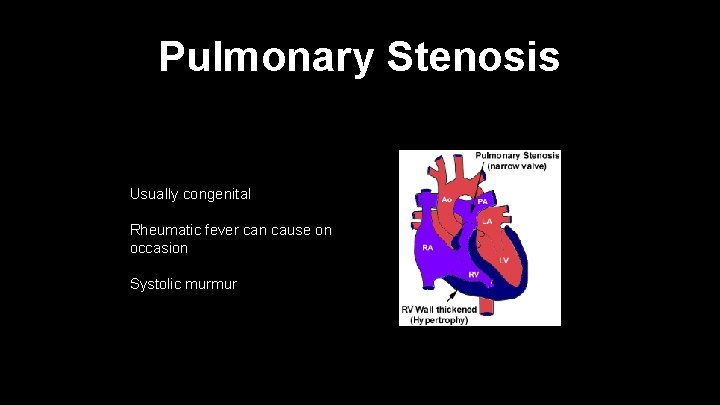
Pulmonary Stenosis Usually congenital Rheumatic fever can cause on occasion Systolic murmur
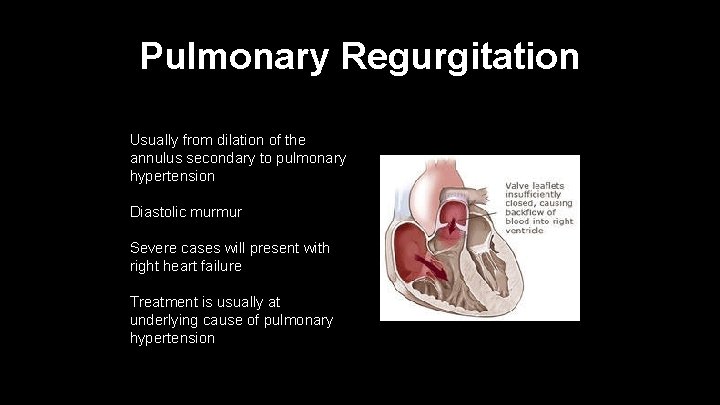
Pulmonary Regurgitation Usually from dilation of the annulus secondary to pulmonary hypertension Diastolic murmur Severe cases will present with right heart failure Treatment is usually at underlying cause of pulmonary hypertension

Other Forms of Heart Disease
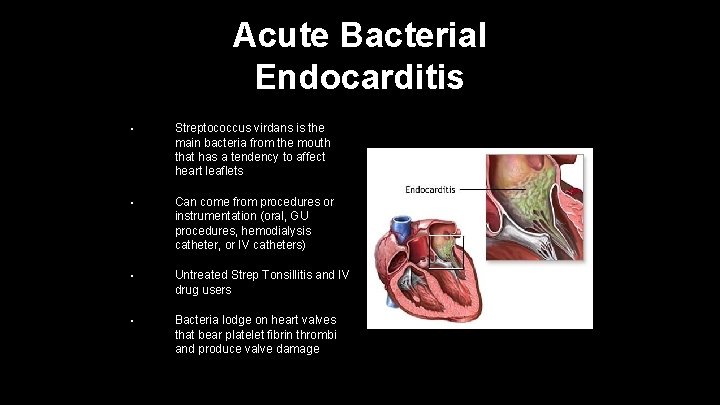
Acute Bacterial Endocarditis • Streptococcus virdans is the main bacteria from the mouth that has a tendency to affect heart leaflets • Can come from procedures or instrumentation (oral, GU procedures, hemodialysis catheter, or IV catheters) • Untreated Strep Tonsillitis and IV drug users • Bacteria lodge on heart valves that bear platelet fibrin thrombi and produce valve damage

Acute Bacterial Endocarditis • The ability to adhere fibrin thrombi comes from production of extracellular dextran by streptococcal strains • May present 2 -5 weeks after precipitating procedure or infection • If organism slow growing symptoms may be slower up to 6 months • Symptoms-fever, chills, shortness of breath, night sweats, weight loss, and anorexia

Acute Bacterial Endocarditis • TEE is useful for assessing vegetation • Penicillin G and Gentamicin is ideal • Vancomycin also helpful • Surgery is needed for refractory infection or valvular heart damage

Acute Bacterial Endocarditis • Major Criteria • Carditis (Pleuritic pain, friction rub, heart failure • Polyarthritis • Chorea • Erythema Marginatum • Subcutaneous Nodules • Minor Criteria • Fever • Arthralgias • Previous Rheumatic Fever or rheumatic heart disease

Acute Bacterial Endocarditis Acute rheumatic fever can be diagnosed if 2 major, or 1 major and 2 minor criteria are met Penicillin is indicated to treat strep infection Salicylates are helpful for fever and arthritis symptoms
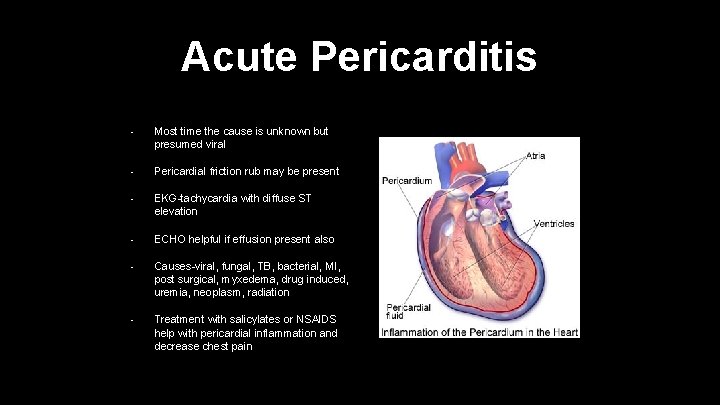
Acute Pericarditis • Most time the cause is unknown but presumed viral • Pericardial friction rub may be present • EKG-tachycardia with diffuse ST elevation • ECHO helpful if effusion present also • Causes-viral, fungal, TB, bacterial, MI, post surgical, myxedema, drug induced, uremia, neoplasm, radiation • Treatment with salicylates or NSAIDS help with pericardial inflammation and decrease chest pain
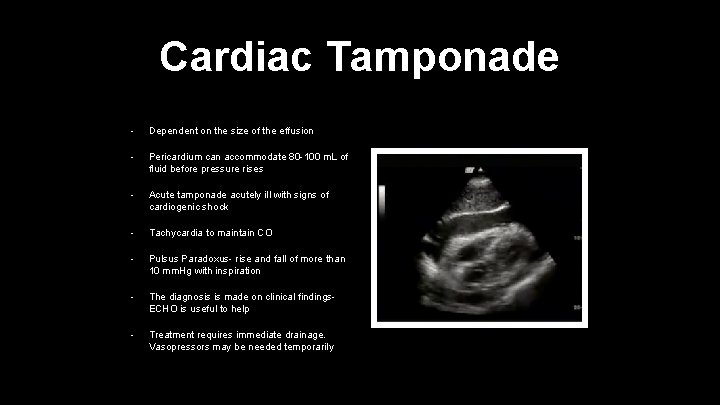
Cardiac Tamponade • Dependent on the size of the effusion • Pericardium can accommodate 80 -100 m. L of fluid before pressure rises • Acute tamponade acutely ill with signs of cardiogenic shock • Tachycardia to maintain CO • Pulsus Paradoxus- rise and fall of more than 10 mm. Hg with inspiration • The diagnosis is made on clinical findings. ECHO is useful to help • Treatment requires immediate drainage. Vasopressors may be needed temporarily
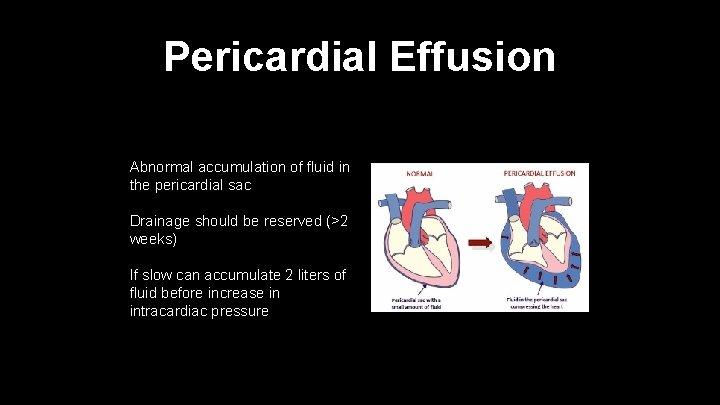
Pericardial Effusion Abnormal accumulation of fluid in the pericardial sac Drainage should be reserved (>2 weeks) If slow can accumulate 2 liters of fluid before increase in intracardiac pressure
- Slides: 138