Cardiovascular Anatomy Physiology Objectives Function n Anatomy n

Cardiovascular. Anatomy & Physiology

Objectives Function n Anatomy n Cells n Cardiac Output n Oxygen Transport n Pathologies n
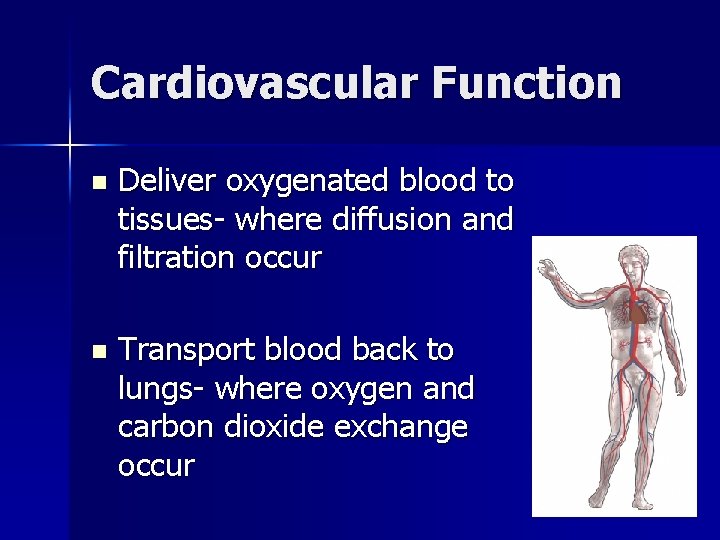
Cardiovascular Function n Deliver oxygenated blood to tissues- where diffusion and filtration occur n Transport blood back to lungs- where oxygen and carbon dioxide exchange occur
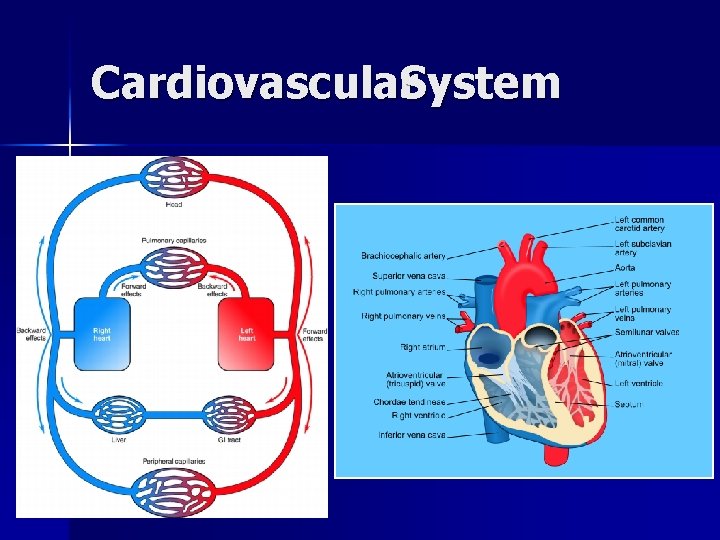
Cardiovascular. System
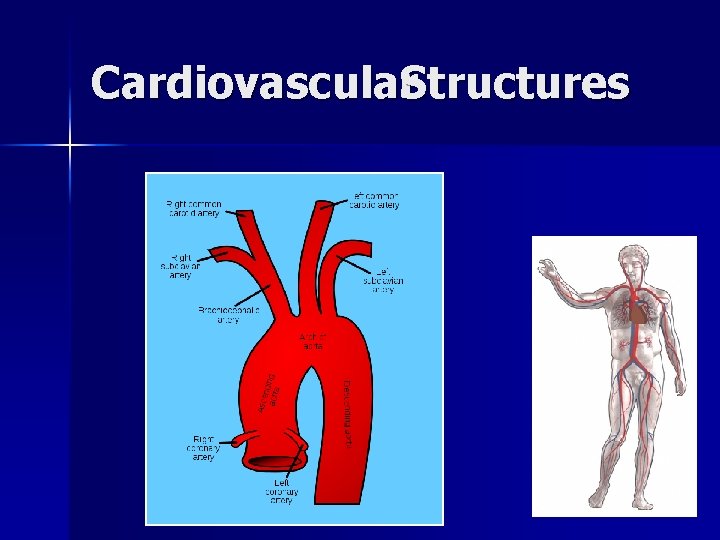
Cardiovascular. Structures
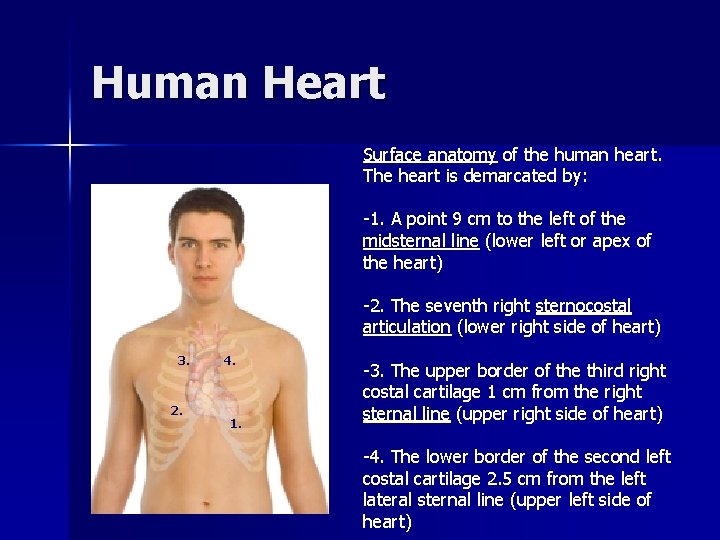
Human Heart Surface anatomy of the human heart. The heart is demarcated by: -1. A point 9 cm to the left of the midsternal line (lower left or apex of the heart) -2. The seventh right sternocostal articulation (lower right side of heart) 3. 2. 4. 1. -3. The upper border of the third right costal cartilage 1 cm from the right sternal line (upper right side of heart) -4. The lower border of the second left costal cartilage 2. 5 cm from the left lateral sternal line (upper left side of heart)
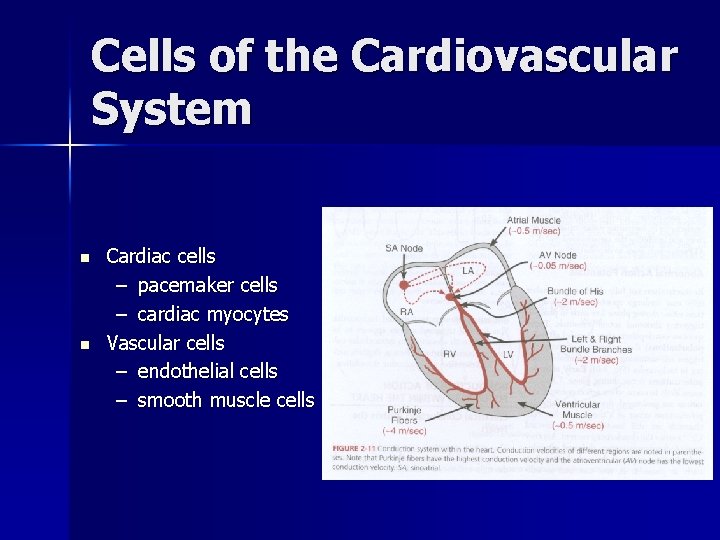
Cells of the Cardiovascular System n n Cardiac cells – pacemaker cells – cardiac myocytes Vascular cells – endothelial cells – smooth muscle cells

Cardiac Myocytes Conduct AP cell-to-cell via gap junctions n Are packed with contractile elements n Have well developed sarcoplasmic reticulum which sequesters calcium n Are dependent on extracellular calcium for contraction n

How does membrane depolarization lead to mechanical contraction? Action Potential Calcium influx from ECF Calcium release from SR Increased intracellular free calcium actin-myosin crossbridging myocardial cell shortening
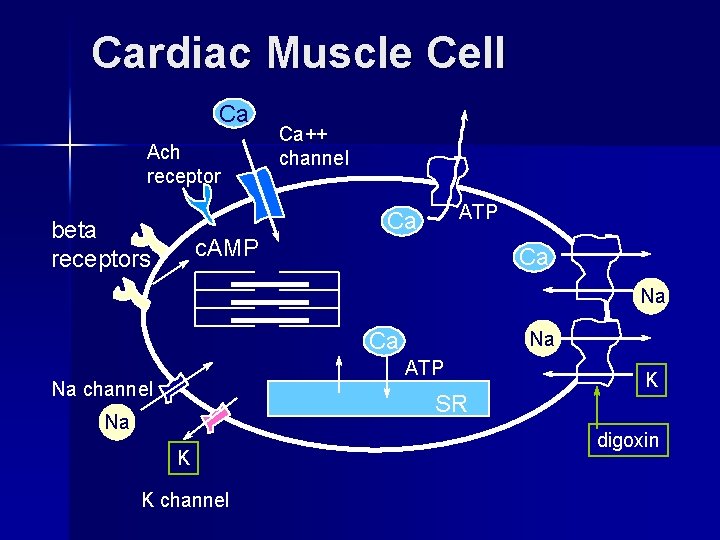
Cardiac Muscle Cell Ca Ach receptor Ca++ channel ATP Ca beta receptors c. AMP Ca Na ATP Na channel SR Na K K channel K digoxin
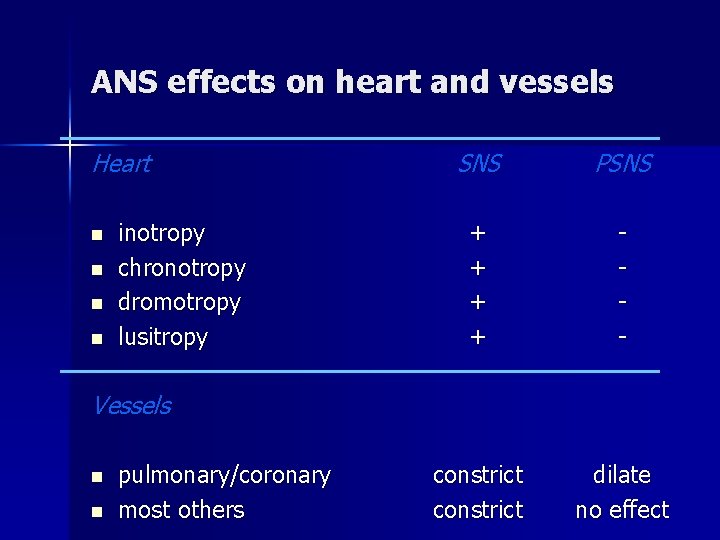
ANS effects on heart and vessels Heart n n inotropy chronotropy dromotropy lusitropy SNS PSNS + + - constrict dilate no effect Vessels n n pulmonary/coronary most others

Cardiac Output THE most important variable in cardiac function! CO = HR x SV
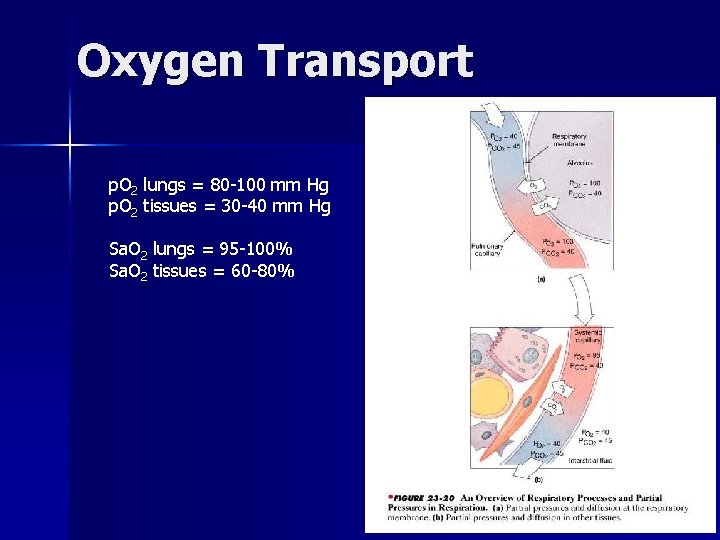
Oxygen Transport p. O 2 lungs = 80 -100 mm Hg p. O 2 tissues = 30 -40 mm Hg Sa. O 2 lungs = 95 -100% Sa. O 2 tissues = 60 -80%
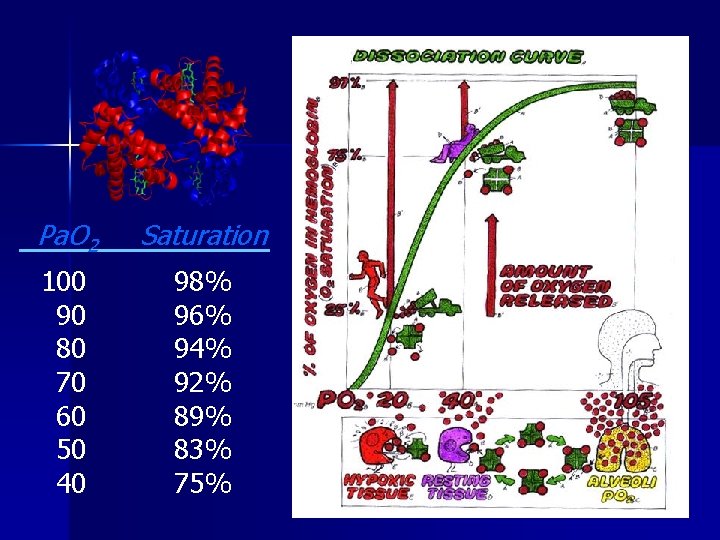
Pa. O 2 Saturation 100 90 80 70 60 50 40 98% 96% 94% 92% 89% 83% 75%

Shifts in Hb-O 2 Affinity n Shift to right: affinity – acidemia – hyperthermia – hypercarbia – increased 2, 3 DPG n Shift to left: affinity – alkalemia – hypothermia – hypocarbia – decreased 2, 3 DPG
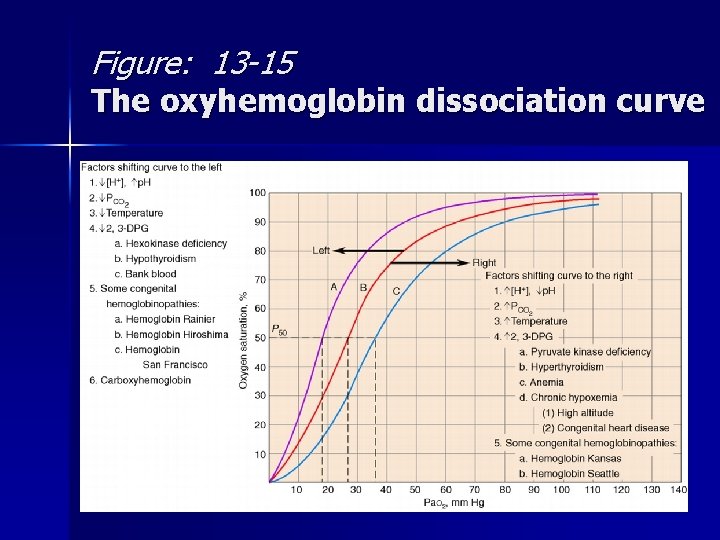
Figure: 13 -15 The oxyhemoglobin dissociation curve

Carbon Dioxide Transport Physical Solution: (5%) Pa. CO 2 X. 06 Carbaminohemoglobin: (15%) HB N H COOBicarbonate ion (80%) CO 2 + H 2 O H 2 CO 3 H+ + HCO 3 -

Red Cell Production iron n folate n vitamin B 12 n erythropoietin n functional stem cells n
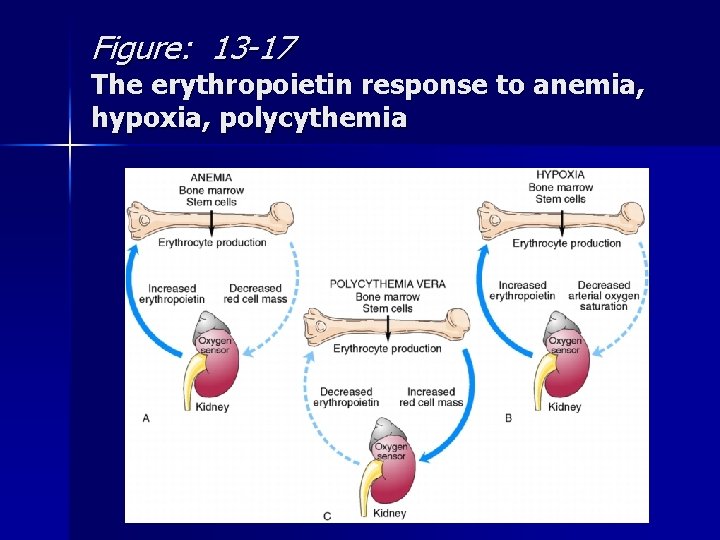
Figure: 13 -17 The erythropoietin response to anemia, hypoxia, polycythemia
Cardiovascular Pathology Anemia n Heart Failure n Valvular Defects n Cardiomyopathies n Congenital Defects n Vascular Insufficiency n

General Signs and Symptoms of Anemia Increased respiration n Increased heart rate n Fatigue n Decreased activity tolerance n Pallor n Murmur n

Heart Failure n n Def: Inability to effectively PUMP the amount of blood delivered to the heart Left ventricular ejection fraction (EF) – Normal values: 60 -80% – Important measure of heart failure n Etiologies: Many, but 2 main causes are hypertension and ischemia – – – MI CIHD Valve Disease Congenital Defects Cardiomyopathy
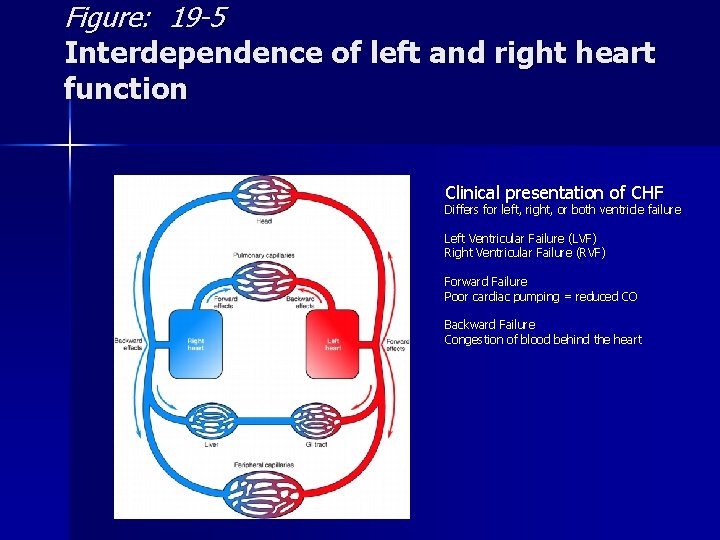
Figure: 19 -5 Interdependence of left and right heart function Clinical presentation of CHF Differs for left, right, or both ventricle failure Left Ventricular Failure (LVF) Right Ventricular Failure (RVF) Forward Failure Poor cardiac pumping = reduced CO Backward Failure Congestion of blood behind the heart
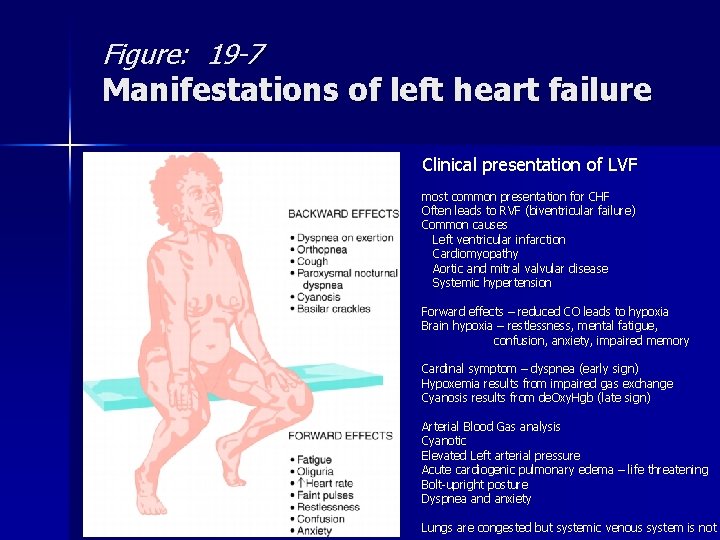
Figure: 19 -7 Manifestations of left heart failure Clinical presentation of LVF most common presentation for CHF Often leads to RVF (biventricular failure) Common causes Left ventricular infarction Cardiomyopathy Aortic and mitral valvular disease Systemic hypertension Forward effects – reduced CO leads to hypoxia Brain hypoxia – restlessness, mental fatigue, confusion, anxiety, impaired memory Cardinal symptom – dyspnea (early sign) Hypoxemia results from impaired gas exchange Cyanosis results from de. Oxy. Hgb (late sign) Arterial Blood Gas analysis Cyanotic Elevated Left arterial pressure Acute cardiogenic pulmonary edema – life threatening Bolt-upright posture Dyspnea and anxiety Lungs are congested but systemic venous system is not

Summary Anemia n Heart Failure n Valvular Defects n Cardiomyopathy n Congenital Defects n Vascular Insufficiency n

Valvular Disorders n Abnormalities of Valve function: – Stenosis & Regurgitation n Etiology – congenital – rheumatic – degenerative calcification – infective n Diagnostic Evaluation: Echo-doppler

Common Valve Disorders Mitral Stenosis n Mitral Regurgitation n Aortic Stenosis n Aortic Regurgitation n Mitral valve lies between the left atrium and left ventricle. Stenosis – obstruction to blood flow thru cardiac valves that are not opening completely Regurgitation – retrograde blood flow through a cardiac valve when the valve is closed

Differential Diagnosis of Murmur n Mitral Stenosis – Increased Left Arterial Pressure – Loud S 1 opening snap at apex – Murmur rare, if present, short diastolic – atrial fibrillation is common
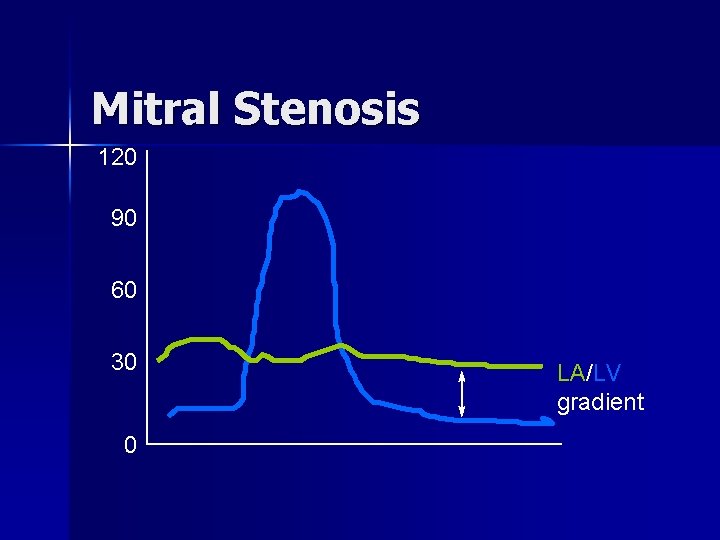
Mitral Stenosis 120 90 60 30 0 LA/LV gradient

Differential Diagnosis of Murmur n Mitral Regurgitation – Systolic Murmur – Radiates to left axilla – Pansystolic, blowing – Prominent S 3
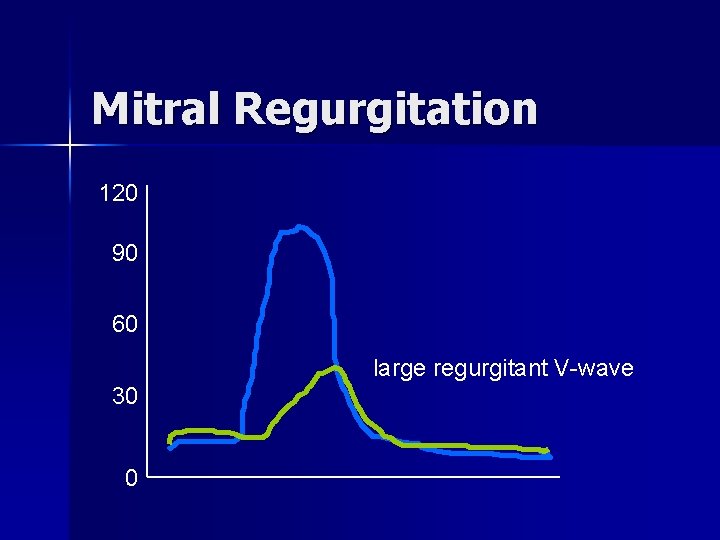
Mitral Regurgitation 120 90 60 large regurgitant V-wave 30 0

Differential Diagnosis of Murmur n Aortic Stenosis – Mid systolic – Crescendo-decrescendo – Radiates to neck – S 4 prominent – Angina, syncope common
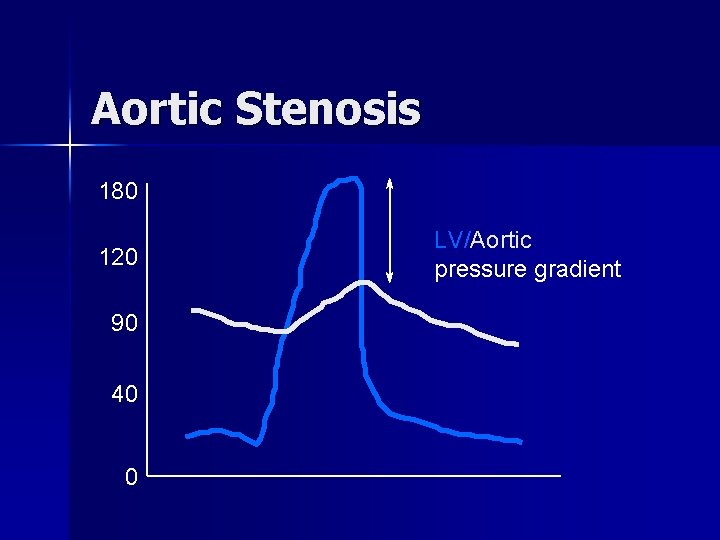
Aortic Stenosis 180 120 90 40 0 LV/Aortic pressure gradient

Differential Diagnosis of Murmur n Aortic Regurgitation – Diastolic murmur – Bounding Pulse “waterhammer” – Wide pulse pressure
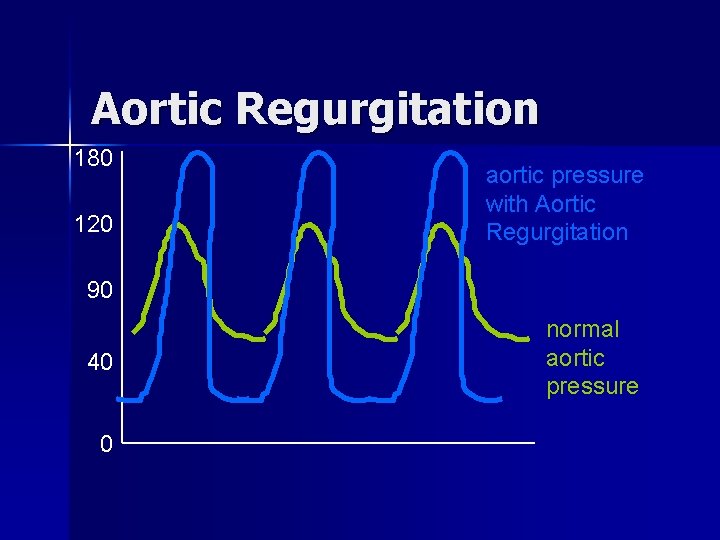
Aortic Regurgitation 180 120 aortic pressure with Aortic Regurgitation 90 40 0 normal aortic pressure

Cardiomyopathy n Dilated – enlarged heart chambers – poor contractility n Hypertrophic – outflow obstruction – ischemia n Restrictive – impaired diastolic filling

Congenital Heart Defects Acyanotic n L to R shunt – Atrial Septal Defect – Ventricular Septal Defect – Patent Ductus Arteriosus Cyanotic n R to L shunt – Transposition – Tetralogy of Fallot

Shock n n n Defining Characteristic: Oxygen Delivery to one or more tissues is below basal requirements leading to hypoxic and immunologic injury. Types of Shock: – Hypovolemic – Cardiogenic – Distributive (e. g. anaphylactic, septic, neurogenic) Manifestations: Signs and symptoms of tissue ischemia and death.

Diagnosis of Shock Tachycardia n Hypotension (orthostatic) n Peripheral hypoperfusion (slow capillary refill, cool, mottled) n Oliguria or anuria n Metabolic acidosis n In septic shock: fever, chills n

General Treatment Measures n n n n Supine position Oxygen Analgesics Labs: CBC, ABG, Renal panel, Type & X, UA Cardiac Monitoring CVP Monitoring (at least) Volume replacement (colloid vs crystalloid vs blood) Vasoactive Drugs

Septic Shock n n Usually caused by gram negative bacteria. Monoclonal antibody to endotoxin may be used. Don’t be fooled by high cardiac output, still have insufficient blood volume to fill the tank. Oxygen consumption is often low due to abnormal distribution and shunt. Look for increased consumption with treatment. Mortality is high: 40 -80%

Vascular System Arterial Insufficiency Venous Insufficiency

Risks for Vascular Insufficiency n Arterial – – – – smoking atherosclerosis inflammatory: Buerger s trauma DIC emboli from LV vasospasm diabetes mellitus n Venous – stasis of bloodflow n n n immobility R heart failure prolonged standing obesity pregnancy – trauma – hypercoagulable n n high platelets high hematocrit
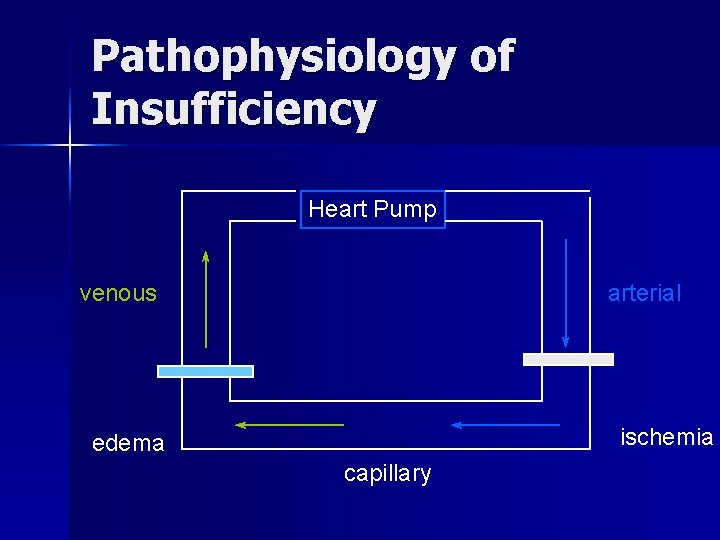
Pathophysiology of Insufficiency Heart Pump venous arterial ischemia edema capillary
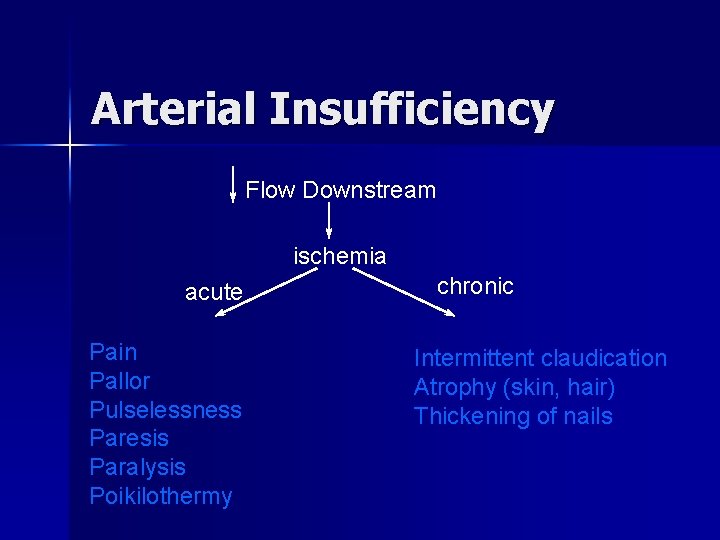
Arterial Insufficiency Flow Downstream ischemia acute Pain Pallor Pulselessness Paresis Paralysis Poikilothermy chronic Intermittent claudication Atrophy (skin, hair) Thickening of nails

Venous Insufficiency Obstruction of Venous Drainage capillary hydrostatic pressure edema, stasis pain risk of pulmonary embolus stasis ulcers and skin changes

Thrombophlebitis n Deep Vein (DVT) – – – n n n – local Inflammation Extremity Edema General leg pain Fever n n n High Risk of PE Treatment – – – immobilize anticoagulate treat risk factors Superficial n warm tender red swollen – Collateral veins minimize edema n Low Risk of PE

Assessment of Cardiac Function Electrical Function Contractile Function

Is Electrical Conduction Normal? R P T Q S

ECG Assessment Rate? n Conduction Abnormality? n – Dysrhythmias – Conduction blocks Ischemia/Infarction? n LVH? n

Cardiovascular Pathophysiology Afterload – The resistance that must be overcome to eject blood from a cardiac chamber. Left ventricular afterload is correlative with the resistance in the systemic vasculature. Preload – The volume of blood that remains in the cardiac chamber prior to systole.
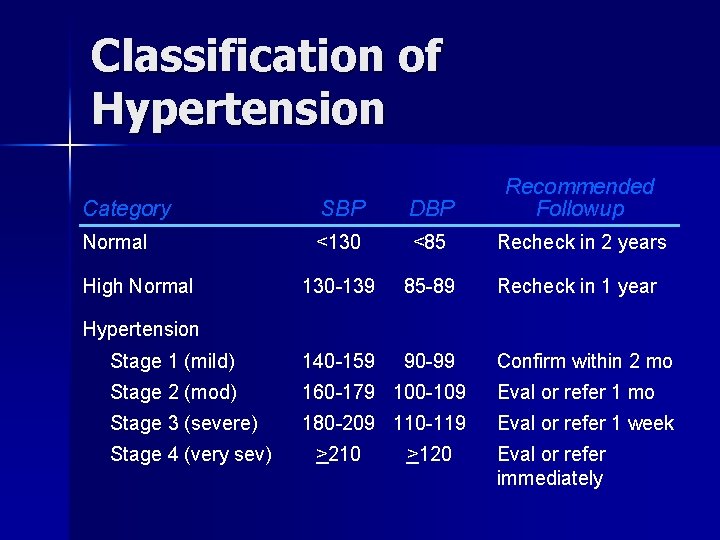
Classification of Hypertension Category SBP DBP Recommended Followup Normal <130 <85 Recheck in 2 years 130 -139 85 -89 Recheck in 1 year Stage 1 (mild) 140 -159 90 -99 Confirm within 2 mo Stage 2 (mod) 160 -179 100 -109 Eval or refer 1 mo Stage 3 (severe) 180 -209 110 -119 Eval or refer 1 week High Normal Hypertension Stage 4 (very sev) >210 >120 Eval or refer immediately

Differential Diagnosis of Hypertension Primary Hypertension (95%) n Secondary Hypertension n – Contraceptive use – Renal disease – Renal artery stenosis – Cushing’s syndrome – Pheochromocytoma – Pregnancy induced hypertension

Treatment? Diuretics, beta blockers, ACE inhibitors, calcium channel blockers, alpha blockers n Consider age, ethnicity, coexisting disorders, cost, lipid profile n
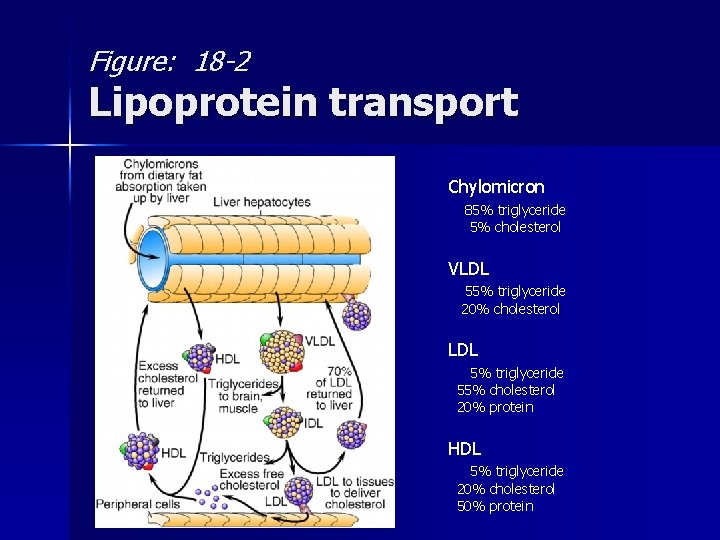
Figure: 18 -2 Lipoprotein transport Chylomicron 85% triglyceride 5% cholesterol VLDL 55% triglyceride 20% cholesterol LDL 5% triglyceride 55% cholesterol 20% protein HDL 5% triglyceride 20% cholesterol 50% protein

Figure: 18 -3 Type I - IV atherosclerotic plaques Types I-III Asymptomatic Arterial wall narrowing Types IV-VI Predispose to ischemic episodes

Ischemic Heart Disease n Etiology: – Coronary Atherosclerosis Risks: n Clinical Syndromes: n – angina pectoris – myocardial infarction – chronic ischemic heart disease – sudden cardiac death

Pathogenesis of Atherosclerosis Lipid accumulates in vascular wall Macrophages infiltrate the wall and oxidize the lipids Cell injury and release of local growth factors (Angiotensin II) Plaque formation on intimal wall
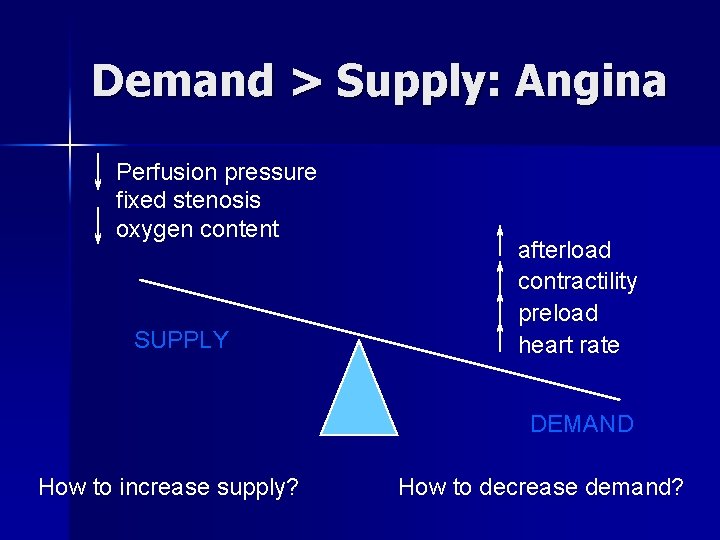
Demand > Supply: Angina Perfusion pressure fixed stenosis oxygen content SUPPLY afterload contractility preload heart rate DEMAND How to increase supply? How to decrease demand?

Pathogenesis of Ischemia Plaque Disruption or Breakdown Tissue Thromboplastin Exposed Platelet Aggregation and Clotting Cascade Activated Thrombus Formation Acute Ischemia

Ischemic Syndromes Stable Angina Unstable Angina MI Patho: Fixed stenosis Thrombus >75% + lysis Thrombus with occlusion Pain: predictable relieved by rest (3 -5 min) unpredictable not relieved rest (>15 -30) not elevated Serum Enz: not elevated

ECG Changes with Ischemia n n Indicative Leads show: Ischemia: ST elevation or depression T-wave peaking, flattening, inversion Bigger than normal Q-waves ST elevation Q

Sequela of Myocardial Infarction Decreased Myocardial Perfusion Partially ischemic cells Totally ischemic cells Anaerobic metabolism and lack of ATP No ATP Ion leak across cell membrane ST changes Dysrhythmias Cell rupture and death Q-waves Elevated Enzymes
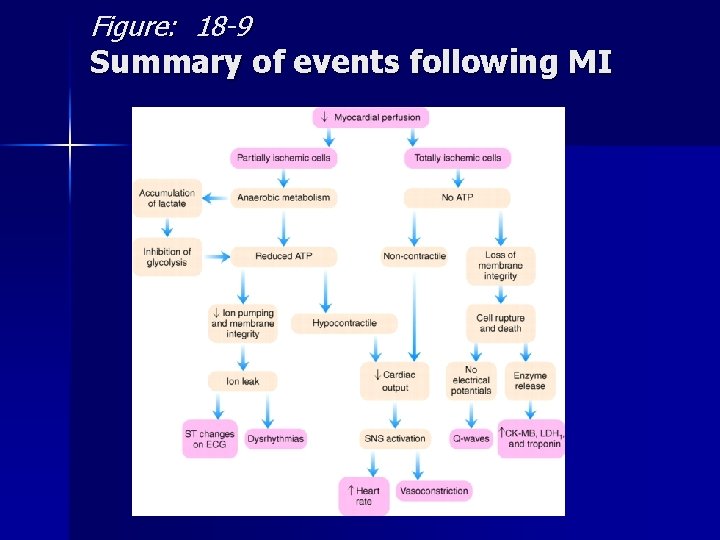
Figure: 18 -9 Summary of events following MI
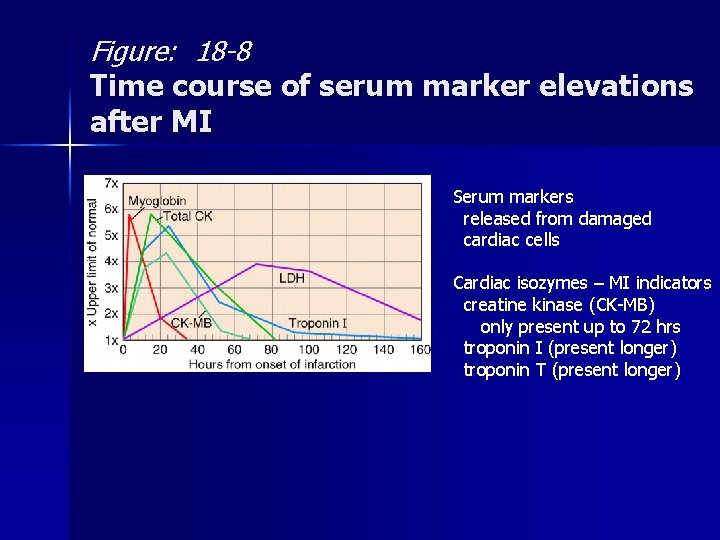
Figure: 18 -8 Time course of serum marker elevations after MI Serum markers released from damaged cardiac cells Cardiac isozymes – MI indicators creatine kinase (CK-MB) only present up to 72 hrs troponin I (present longer) troponin T (present longer)
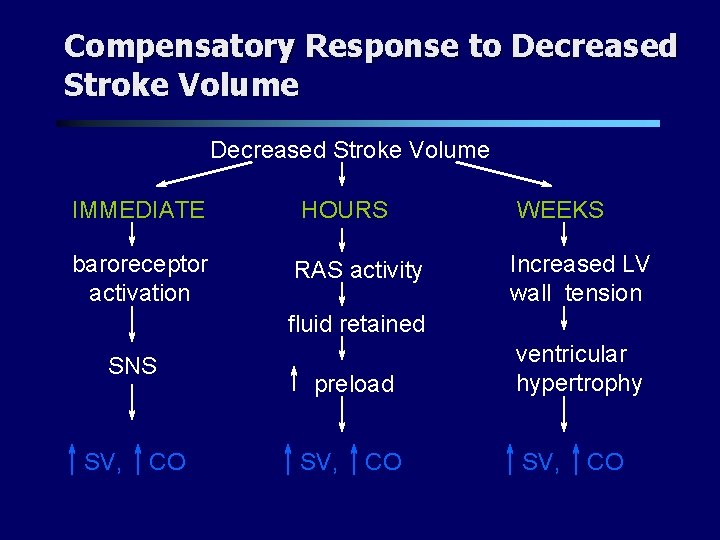
Compensatory Response to Decreased Stroke Volume IMMEDIATE baroreceptor activation HOURS RAS activity WEEKS Increased LV wall tension fluid retained SNS SV, CO preload SV, CO ventricular hypertrophy SV, CO

Differential Diagnosis of Chest Pain Cardiac ischemia n Chest wall trauma, costochondritis n Pleural pain - pneumonias n Pneumothorax n Gastrointestinal (GERD) n

Treatment of Cardiac Ischemia n Stable angina – SL nitroglycerin – Platelet inhibitor (e. g. ASA 325 mg qod) – beta blocker – add long acting nitrate (remove at night) – add calcium channel blocker (not verapamil)

Treatment of Cardiac Ischemia n If ECG shows signs of current ischemia – Continuous ECG monitoring, Labs – Oxygen – Give ASA – Relieve pain with SL nitro, morphine – Evaluate for thrombolytic therapy – Decrease MVO 2: bedrest, pain relief, etc – Manage dysrhythmias, hemodynamics

Heart Failure Pathophysiological state Abnormality of cardiac function to supply blood to meet demand Pumps only from abnormally elevated diastolic filling pressure Etiology Myocardial failure High demand on heart with near normal cardiac function Inadequate adaptation of cardiac myocytes to increased wall stress Causes circulatory failure but converse is not always true Adaptations Frank-Starling mechanism – increased preload sustains cardiac performance Myocardial hypertrophy – mass of contractile tissue increases Neurohumoral Activation – Adrenergic cardiac nerves causes release of NE Positive inotropy Activation of RAA system – salt and water retention (increased preload, increased energy expense) Release vasoconstrictive agents which increase afterload Increased c. AMP causes increased calcium entry Positive inotropy, negative lusitropy Increased energy expenditure and reduced CO which further stimulates RAA system Calcium overload may cause arrythmia and sudden death Cardiac Ang. II may cause negative lusitropy, positive inotropy, positive afterload, increased myocardial energy expense

Congestive Heart Failure Can result from most cardiac disorders. Most common causes of CHF is myocardial ischemia from coronary artery disease, hypertension and dilated cardiomyopathy Systolic dysfunction Reduced myocardial contractility Congestion is result of fluid backup in heart Common cause is myocardial cell death – MI (neg inotropy) EF less than 50% Chronic overexcitation of b receptor SNS may be exacerbate condition B receptor blockers – treatment Heart failure – Signs, symptoms CHF Reduced stroke volume Reduced cardiac output Reduced EF (typically < 40%; severe if EF<20%)

Congestive Heart Failure Diastolic dysfunction Reduced myocardial relaxation Ventricle is not compliant and does not fill effectively Ventricle filling dependent on Ca 2+ uptake (active phase of diastolic relaxation) Passive phase (myocardial stretch) impaired Common cause is myocardial cell death – MI (neg inotropy) Heart failure – Signs, symptoms CHF (congestion; edema) Reduced stroke volume Reduced cardiac output Near normal EF > 50%

Factors Affecting Cardiac Output Heart Rate (chronotropy) n Contractility (inotropy) n Preload n Afterload n

How is Heart Rate Regulated? n n Intrinsic pacemaker rate = 100 bpm Autonomic Influences – SNS------> B 1 receptor-------> Increased HR – PSNS-> Muscarinic (Ach)--> Decreased HR Stretch Reflex (Bainbridge): Increased filling------> Increased HR Drugs: ANS drugs, digitalis

What Factors Affect Contractility? n n n Anything that increases Ca++ availability in the heart muscle cell will increase Contractility. Anything that decreases Ca++ availability in the heart muscle cell will decrease Contractility. What would be the effect of: – SNS – PSNS – Digoxin – Ca++ channel blocker – B 1 blocker
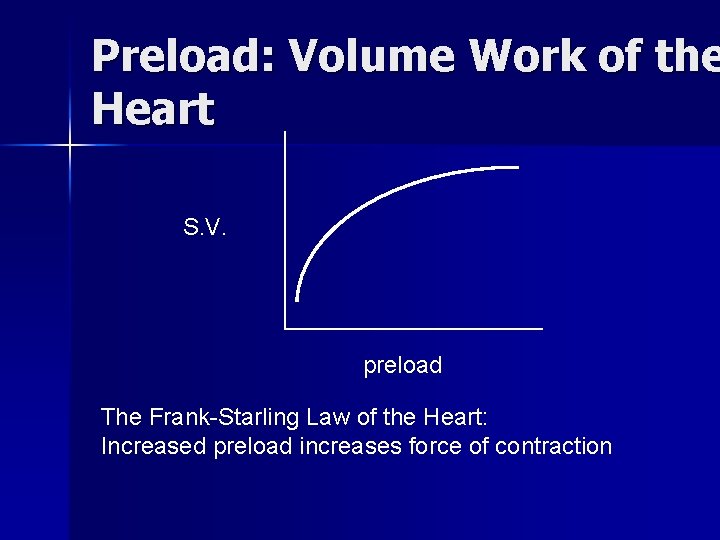
Preload: Volume Work of the Heart S. V. preload The Frank-Starling Law of the Heart: Increased preload increases force of contraction

Afterload: Pressure work of the Heart n Increased Afterload occurs with increased resistance to ejection of blood from the ventricle – Increased Systemic Vascular Resistance – Increased Diastolic Blood Pressure – Aortic Stenosis n Increased Afterload: Decreased stroke volume
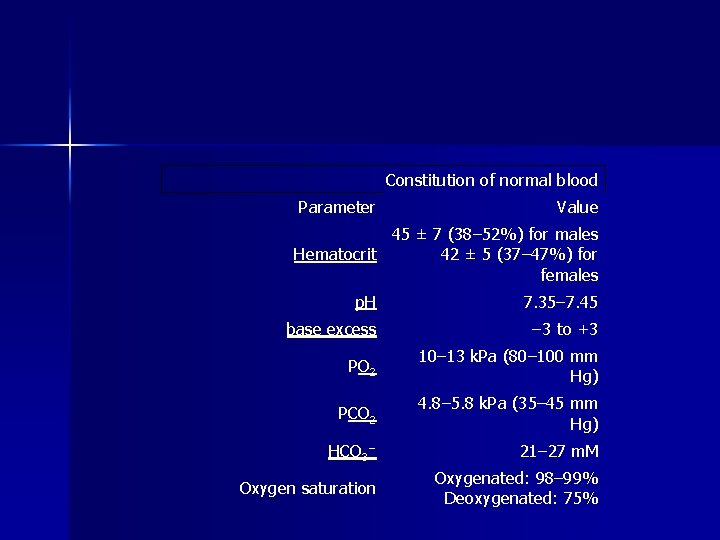

Constitution of normal blood Parameter Value 45 ± 7 (38– 52%) for males Hematocrit 42 ± 5 (37– 47%) for females p. H 7. 35– 7. 45 base excess − 3 to +3 PO 2 10– 13 k. Pa (80– 100 mm Hg) PCO 2 4. 8– 5. 8 k. Pa (35– 45 mm Hg) HCO 3− 21– 27 m. M Oxygen saturation Oxygenated: 98– 99% Deoxygenated: 75%
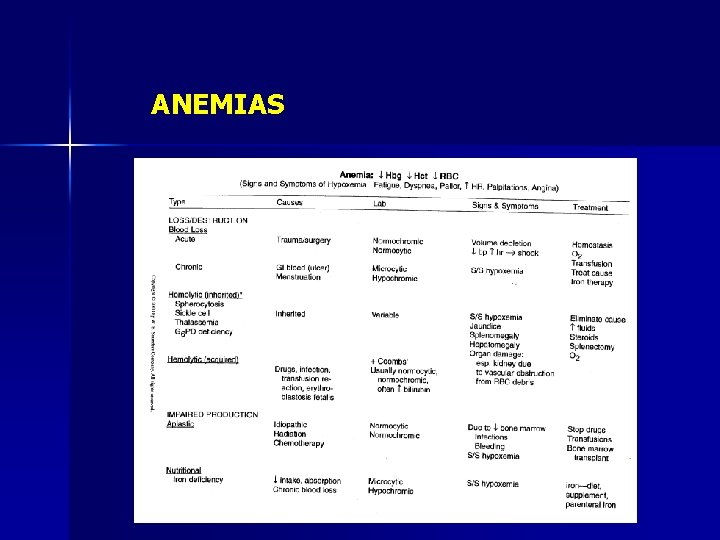
ANEMIAS

ANEMIAS

How can the different types of anemia be differentiated? n Laboratory Diagnosis of Anemia – Low Hematocrit – Low Hemoglobin – Low RBC count n Red Cell Indices – MCV (size) microcytic, normocytic macrocytic – MCHC (color) hypochromic, normochromic

MCV low Microcytic n n iron deficiency hemoglobinopathy chronic disease lead poisoning high normal Normocytic n n n acute bleeding aplastic hemolytic low erythropoietin malignancy Macrocytic n n low Vit B 12 low folate
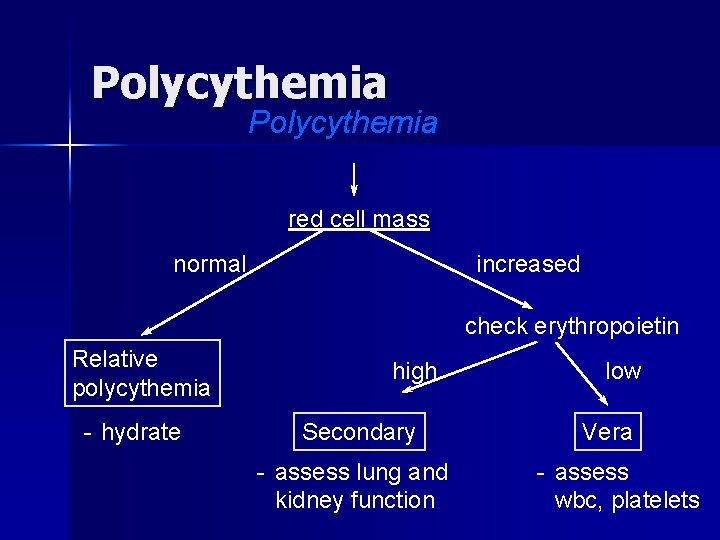
Polycythemia red cell mass normal increased check erythropoietin Relative polycythemia - hydrate high Secondary - assess lung and kidney function low Vera - assess wbc, platelets

Cardiovascular System Physiology

Figure: 19 -2 Compensatory mechanisms in heart failure These mechanisms attempt to improve cardiac output SNS activation – early response to reduced CO Increased heart rate Increased contractility Increased arterial vasoconstriction Increased renin release Chronic SNS activation Increased afterload Increased workload = Reduced CO Decreased CO reduces kidney perfusion Activates RAA system ultimately leading to increased fluid retention Decreased EF = Increased Preload = Reduced CO = Reduced GFR = Increased Fluid Retention = Increased RAS activation = Increased Blood volume= Increased Chamber volume = Increased Contraction (myocardial stretching) Higher Preload = Increased Contractility = Increased CO
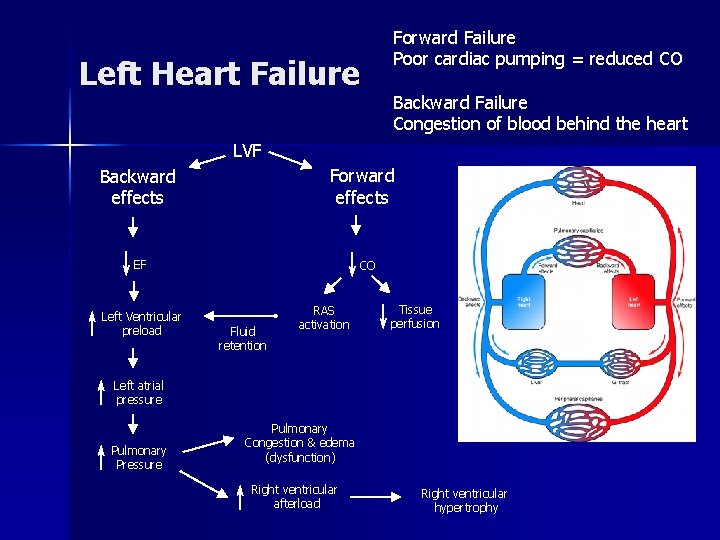
Left Heart Failure Forward Failure Poor cardiac pumping = reduced CO Backward Failure Congestion of blood behind the heart LVF Forward effects Backward effects EF Left Ventricular preload CO Fluid retention RAS activation Tissue perfusion Left atrial pressure Pulmonary Pressure Pulmonary Congestion & edema (dysfunction) Right ventricular afterload Right ventricular hypertrophy
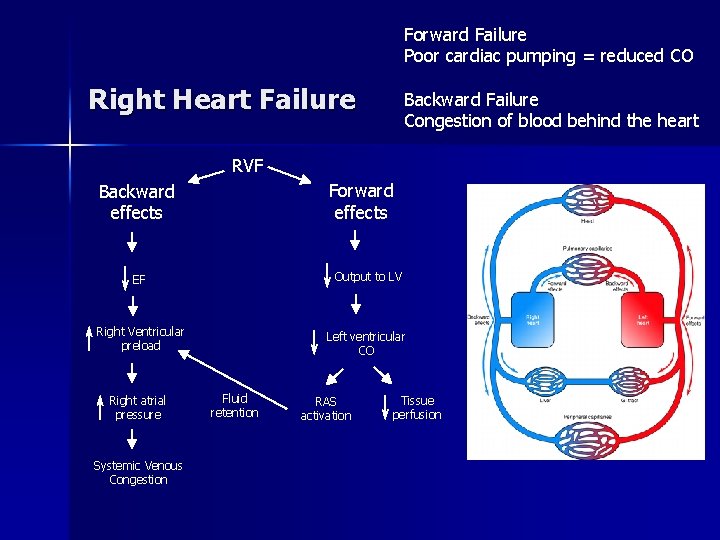
Forward Failure Poor cardiac pumping = reduced CO Right Heart Failure Backward Failure Congestion of blood behind the heart RVF Forward effects Backward effects EF Output to LV Right Ventricular preload Left ventricular CO Right atrial pressure Systemic Venous Congestion Fluid retention RAS activation Tissue perfusion
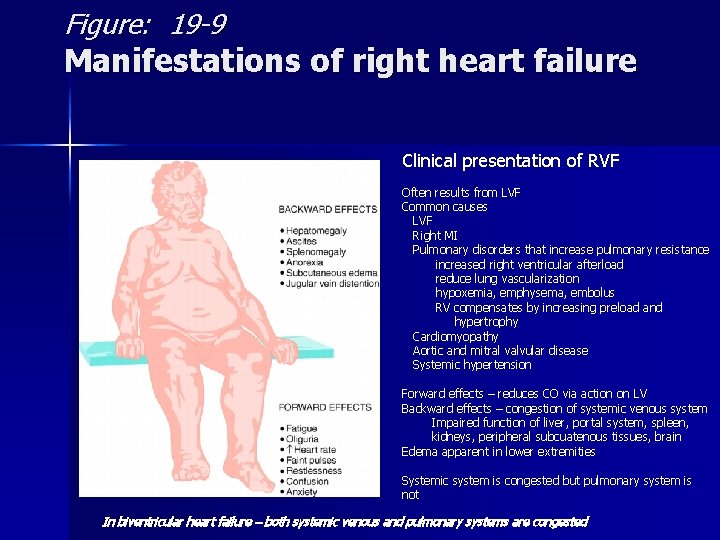
Figure: 19 -9 Manifestations of right heart failure Clinical presentation of RVF Often results from LVF Common causes LVF Right MI Pulmonary disorders that increase pulmonary resistance increased right ventricular afterload reduce lung vascularization hypoxemia, emphysema, embolus RV compensates by increasing preload and hypertrophy Cardiomyopathy Aortic and mitral valvular disease Systemic hypertension Forward effects – reduces CO via action on LV Backward effects – congestion of systemic venous system Impaired function of liver, portal system, spleen, kidneys, peripheral subcuatenous tissues, brain Edema apparent in lower extremities Systemic system is congested but pulmonary system is not In biventricular heart failure – both systemic venous and pulmonary systems are congested

Principles of Heart Failure Treatment n GOAL: Optimize Cardiac Output and Minimize Cardiac Workload – Management of Preload – Management of Afterload – Management of Contractility Drugs used in the management of Heart Failure (table 19 -3)
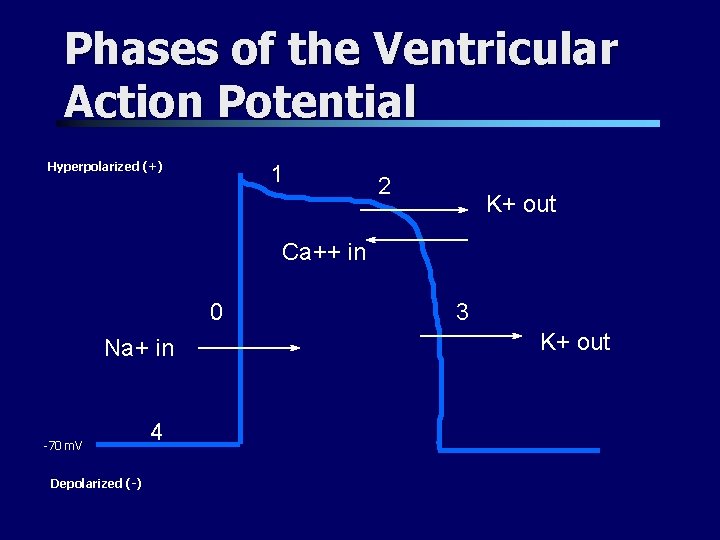
Phases of the Ventricular Action Potential Hyperpolarized (+) 1 2 K+ out Ca++ in 0 Na+ in -70 m. V Depolarized (-) 4 3 K+ out
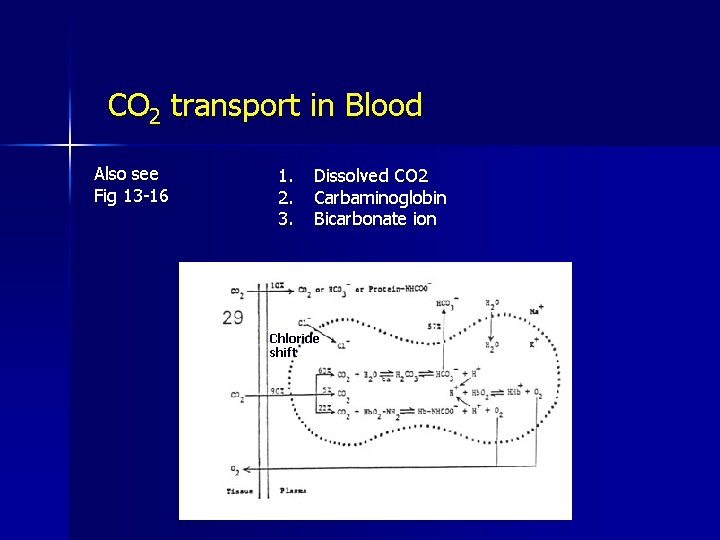
CO 2 transport in Blood Also see Fig 13 -16 1. 2. 3. Dissolved CO 2 Carbaminoglobin Bicarbonate ion Chloride shift
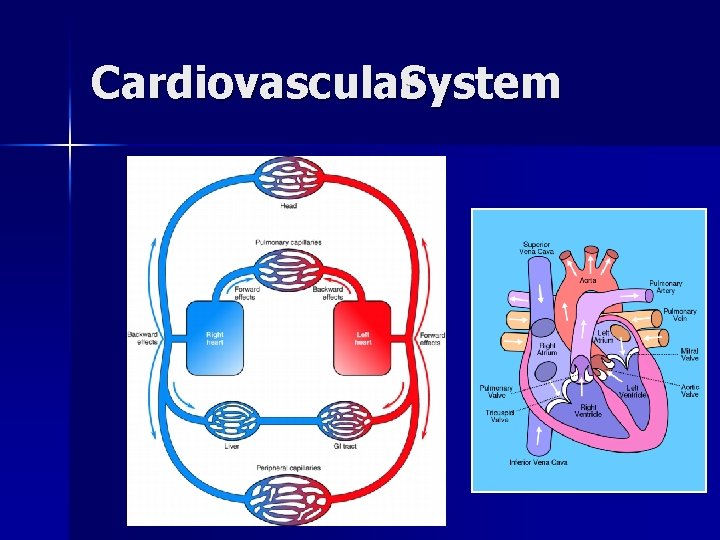
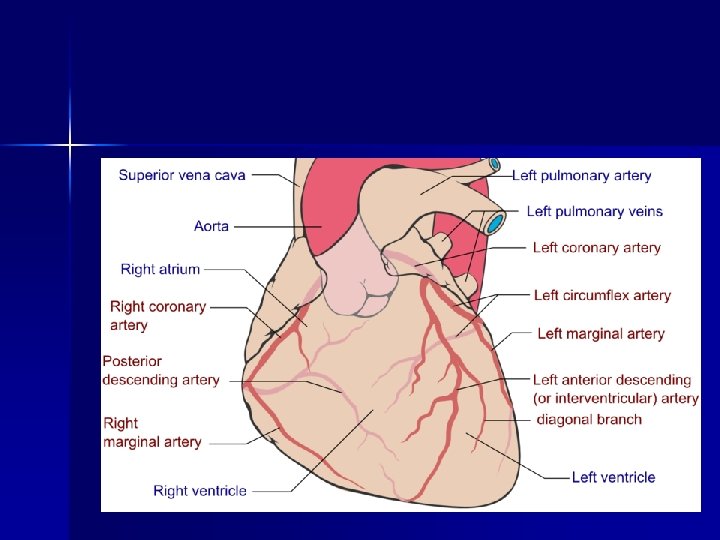
Cardiovascular. System
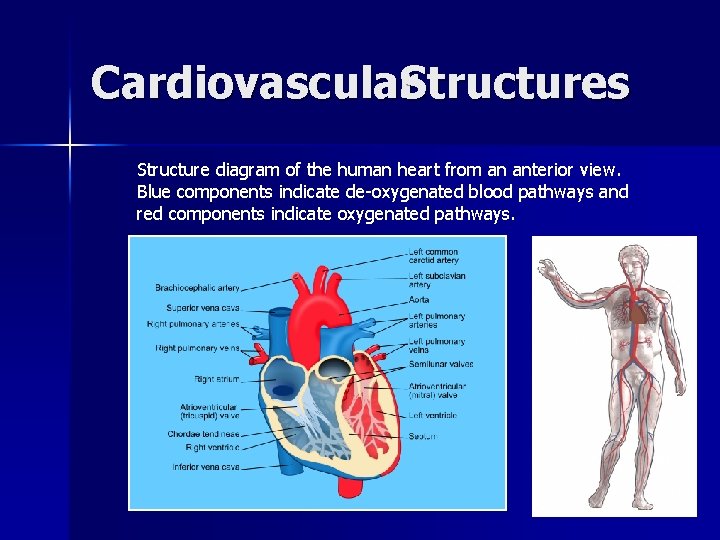
Cardiovascular. Structures Structure diagram of the human heart from an anterior view. Blue components indicate de-oxygenated blood pathways and red components indicate oxygenated pathways.

Pacemaker Cells SA node, AV node, Purkinje fibers n Spontaneously generate action potentials n Vary rate in response to ANS n Action potentials are associated with opening of slow calcium ion channels n Almost no contractile elements n
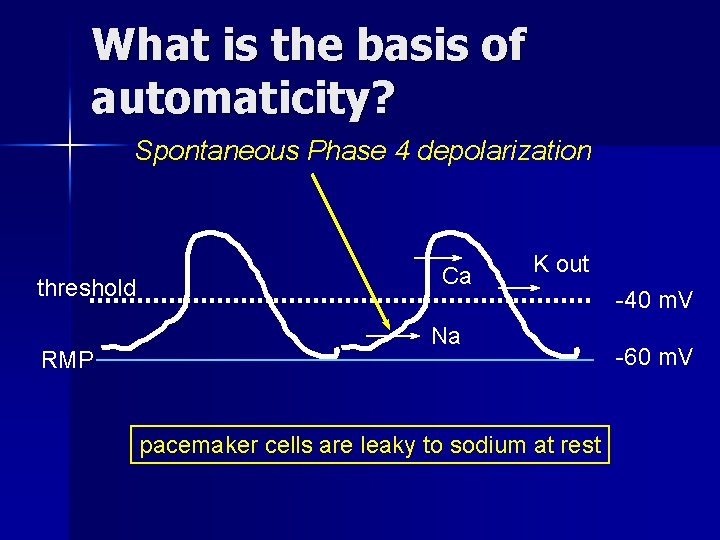
What is the basis of automaticity? Spontaneous Phase 4 depolarization threshold RMP Ca K out Na pacemaker cells are leaky to sodium at rest -40 m. V -60 m. V

ANS Influences on Ion Flux n Sympathetic: NE, E stimulates Beta receptors leading to opening of Na/Ca channels. The cell depolarizes faster. n Parasympathetic: acetylcholine stimulates muscarinic receptors leading to opening of K channels. Potassium leak out offsets sodium influx. The cell depolarizes slower.
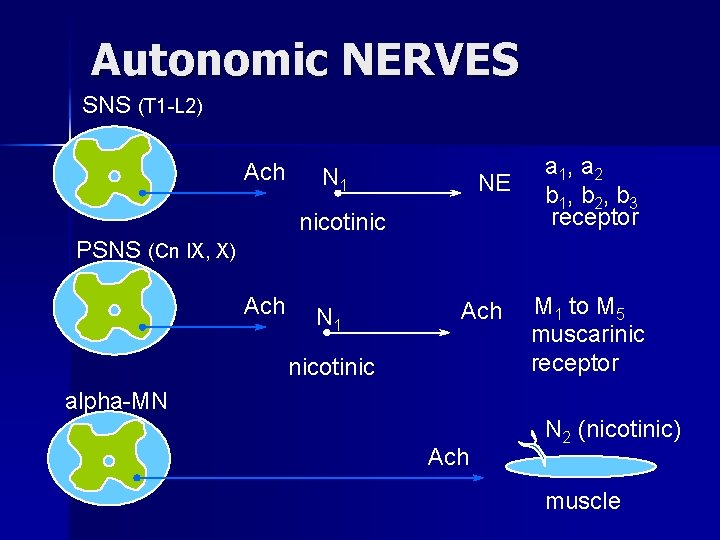
Autonomic NERVES SNS (T 1 -L 2) Ach N 1 NE nicotinic a 1, a 2 b 1, b 2, b 3 receptor PSNS (Cn IX, X) Ach N 1 Ach nicotinic M 1 to M 5 muscarinic receptor alpha-MN Ach N 2 (nicotinic) muscle
- Slides: 98