Cardiorespiratory Diseases 4 Chambers Heart Chambers R atrium

Cardiorespiratory Diseases
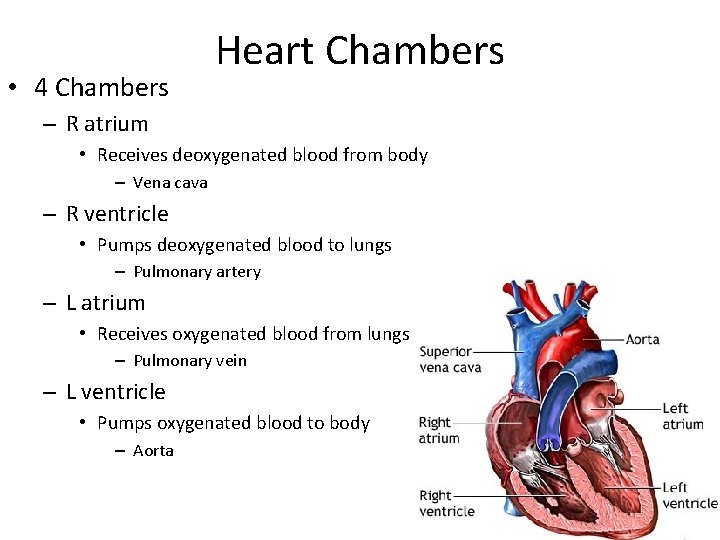
• 4 Chambers Heart Chambers – R atrium • Receives deoxygenated blood from body – Vena cava – R ventricle • Pumps deoxygenated blood to lungs – Pulmonary artery – L atrium • Receives oxygenated blood from lungs – Pulmonary vein – L ventricle • Pumps oxygenated blood to body – Aorta
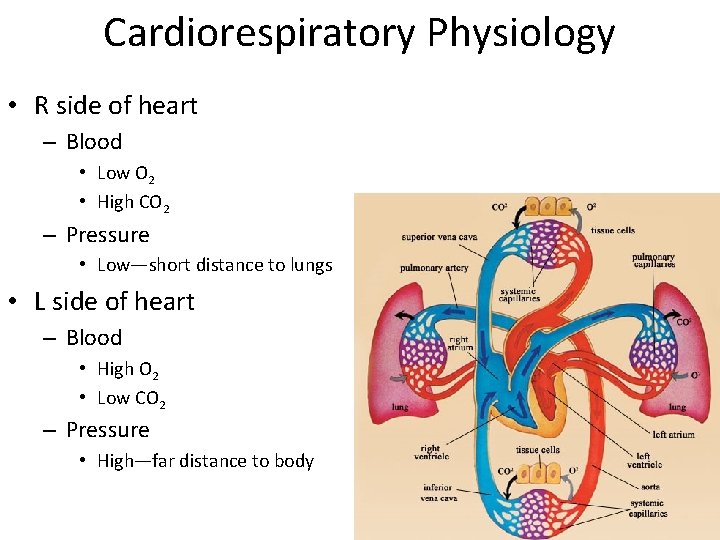
Cardiorespiratory Physiology • R side of heart – Blood • Low O 2 • High CO 2 – Pressure • Low—short distance to lungs • L side of heart – Blood • High O 2 • Low CO 2 – Pressure • High—far distance to body
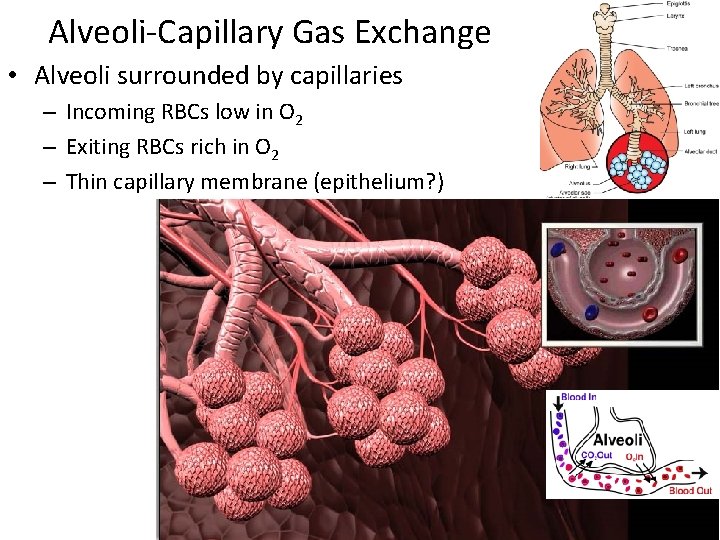
Alveoli-Capillary Gas Exchange • Alveoli surrounded by capillaries – Incoming RBCs low in O 2 – Exiting RBCs rich in O 2 – Thin capillary membrane (epithelium? )
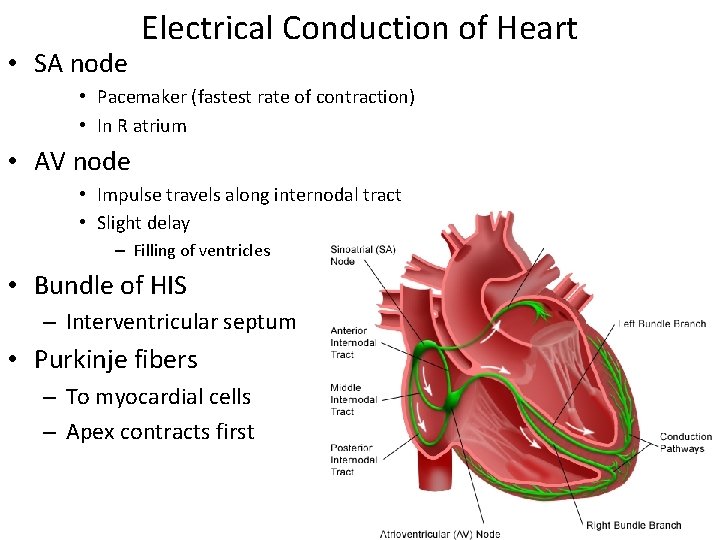
• SA node Electrical Conduction of Heart • Pacemaker (fastest rate of contraction) • In R atrium • AV node • Impulse travels along internodal tract • Slight delay – Filling of ventricles • Bundle of HIS – Interventricular septum • Purkinje fibers – To myocardial cells – Apex contracts first
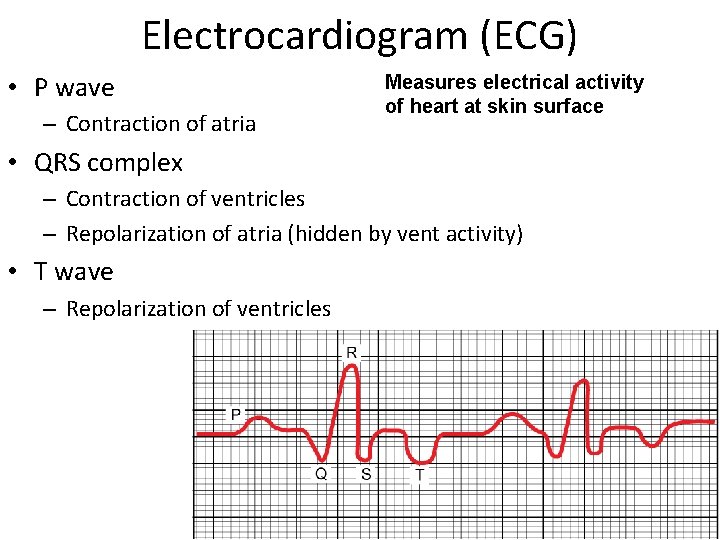
Electrocardiogram (ECG) • P wave – Contraction of atria Measures electrical activity of heart at skin surface • QRS complex – Contraction of ventricles – Repolarization of atria (hidden by vent activity) • T wave – Repolarization of ventricles

Cardiovascular Diseases • Heart Failure—returning blood is not pumped fast enough to meet body’s needs • Heart failure is not a heart attack – 2 causes • Myocardial (heart muscle) dysfunction – Cardiomyopathy – Myocarditis – Taurine (an amino acid) deficiency in cats • Circulatory failure – – Hypovolemia (shock, hemorrhage, dehydration) Anemia Valvular dysfunction Congenital shunts or defects • Congestive heart failure—when failing heart leads to fluid congestion a) in lungs (pulmonary edema), b) in body (edema) – Heart failure almost always progresses to congestive heart failure
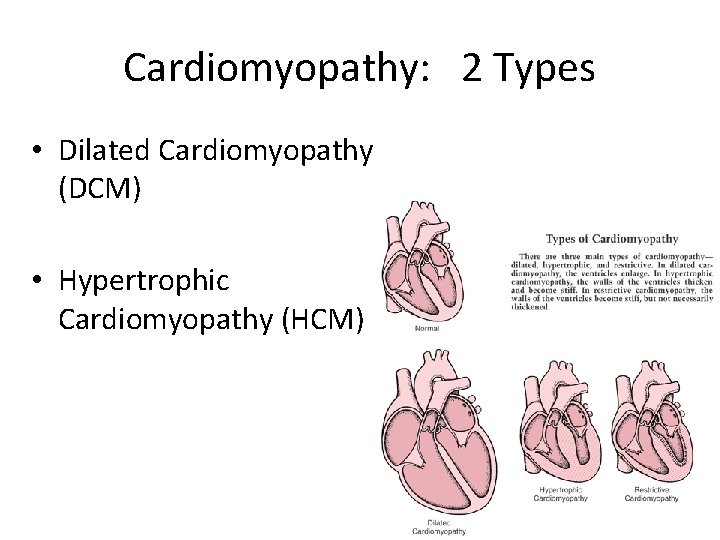
Cardiomyopathy: 2 Types • Dilated Cardiomyopathy (DCM) • Hypertrophic Cardiomyopathy (HCM)
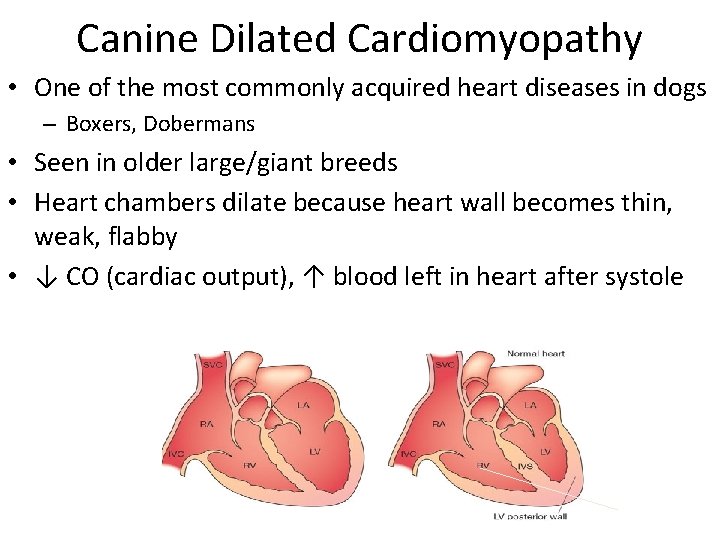
Canine Dilated Cardiomyopathy • One of the most commonly acquired heart diseases in dogs – Boxers, Dobermans • Seen in older large/giant breeds • Heart chambers dilate because heart wall becomes thin, weak, flabby • ↓ CO (cardiac output), ↑ blood left in heart after systole
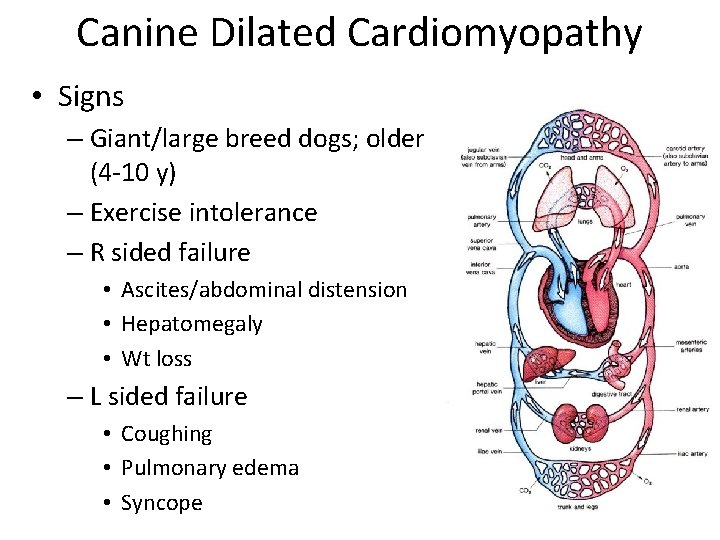
Canine Dilated Cardiomyopathy • Signs – Giant/large breed dogs; older (4 -10 y) – Exercise intolerance – R sided failure • Ascites/abdominal distension • Hepatomegaly • Wt loss – L sided failure • Coughing • Pulmonary edema • Syncope

Canine DCM • PE – Weakness, depression – Hypokinetic femoral pulse from low CO – Pulse deficits – Jugular pulses – HR – fast 150 -200+
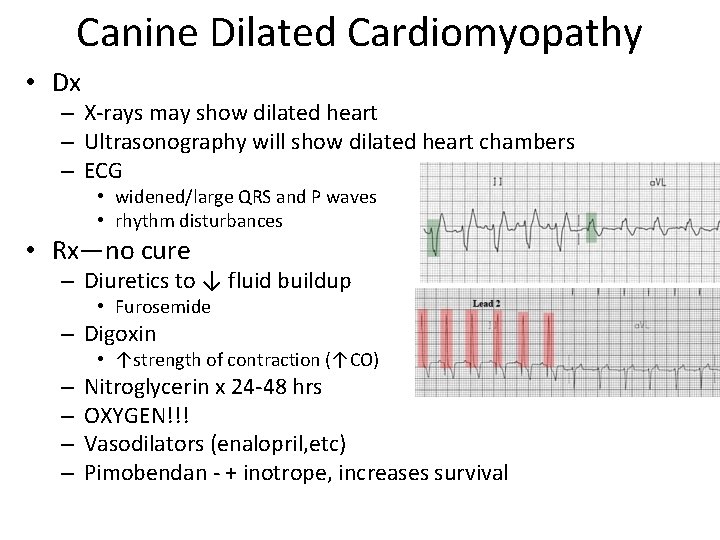
Canine Dilated Cardiomyopathy • Dx – X-rays may show dilated heart – Ultrasonography will show dilated heart chambers – ECG • widened/large QRS and P waves • rhythm disturbances • Rx—no cure – Diuretics to ↓ fluid buildup • Furosemide – Digoxin • ↑strength of contraction (↑CO) – – Nitroglycerin x 24 -48 hrs OXYGEN!!! Vasodilators (enalopril, etc) Pimobendan - + inotrope, increases survival

• Client info Canine DCM – Fatal disease (6 mo to 2 y) – SUDDEN DEATH – More prevalent in large breeds – Diet – decrease Na intake – Minimal exercise – let patient be guide http: //www. vetspecialistsofrochester. com/Cardiology/Canine_Conditions. aspx
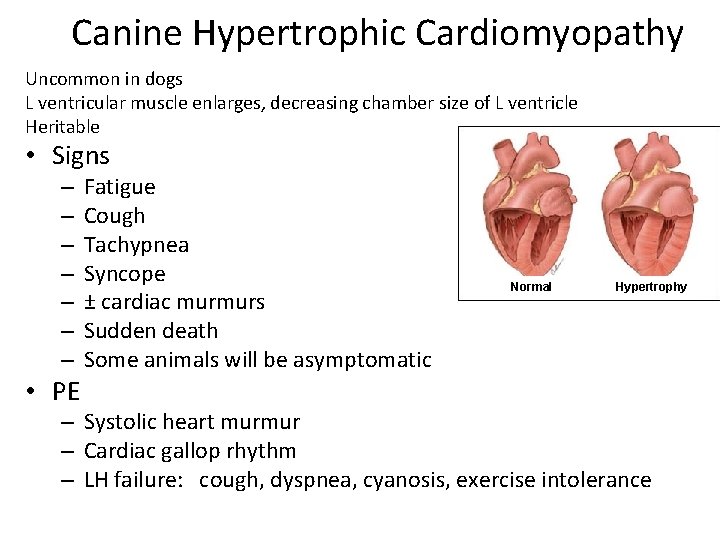
Canine Hypertrophic Cardiomyopathy Uncommon in dogs L ventricular muscle enlarges, decreasing chamber size of L ventricle Heritable • Signs – – – – • PE Fatigue Cough Tachypnea Syncope ± cardiac murmurs Sudden death Some animals will be asymptomatic Normal Hypertrophy – Systolic heart murmur – Cardiac gallop rhythm – LH failure: cough, dyspnea, cyanosis, exercise intolerance

Canine HCM • Dx – X-rays may be normal, have La or LV enlargement and/or pulmonary edema – Ultrasound shows thickened L vent wall – EKG: Normal or ST segment and T wave abn • Rx—none routinely used unless signs of HF • Client info – Sudden death and CHF may occur – Certain breeds more susceptible (G Shep, Rott, Dalm, C Span, Bostons, Shih Tzu)

Feline Dilated Cardiomyopathy Prior to late 1980’s, this was frequently seen in cats Associated with taurine deficiency; addition to cat feed has greatly reduced incidence Similar pathology to DCM in dogs • Signs – Older, mixed breed (Siamese, Burmese, Abyssinian) – Dyspnea, tachypnea – Inactivity – Anorexia – Acute lameness/paralysis (rear legs) – Pain/lack of circulation in affected limbs (no pulse due to thromboemboli)

Feline DCM • PE: – – – HR variable (fast, normal or slow) Systolic heart murmur Gallop rhythm +/- arrhythmia Hypothermia Increased CRT Tachypnea Quiet lung sound (if pleural effusion) Crackles if pulmonary edema Hypokinetic femoral pulses +/- posterior paresis/paralysis

Feline DCM • Dx – Clin signs; ECG; ultrasound – Taurine levels – X-rays

Feline Dilated Cardiomyopathy • Rx – – – Oral taurine supplement (250 -500 mg/d) Furosemide Oxygen Digoxin Aspirin or heparin – prevent thromboemboli Vasodilator; ↓vascular resistance • Hydralazine • Cutaneous nitroglycerin paste • Client info – Most dangerous time is first 2 wks of treatment – If cat responds to taurine treatment, good Px – Unresponsive to taurine treatment, poor long-term Px
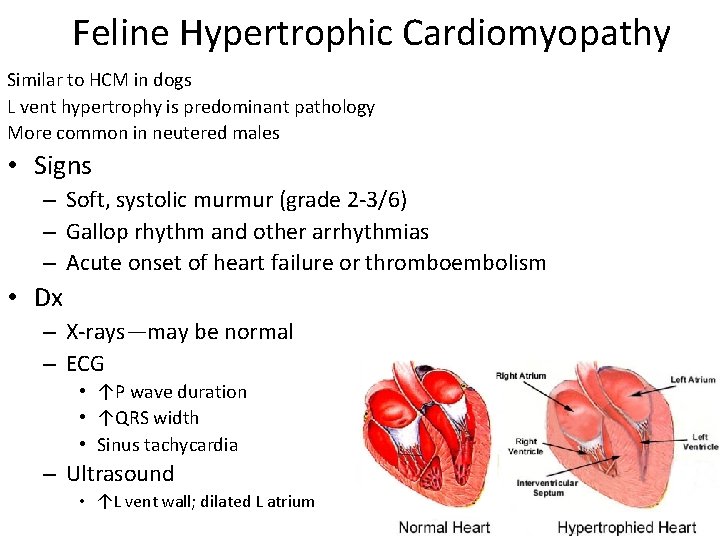
Feline Hypertrophic Cardiomyopathy Similar to HCM in dogs L vent hypertrophy is predominant pathology More common in neutered males • Signs – Soft, systolic murmur (grade 2 -3/6) – Gallop rhythm and other arrhythmias – Acute onset of heart failure or thromboembolism • Dx – X-rays—may be normal – ECG • ↑P wave duration • ↑QRS width • Sinus tachycardia – Ultrasound • ↑L vent wall; dilated L atrium

Feline Hypertrophic Cardiomyopathy • Rx – Diuretics to decrease fluid load on heart • Furosemide – Beta blocker to decrease sinus heart rate • Propanolol – Calcium channel blocker to reduce blood pressure • Diltiazem • Client info – Affected cats may experience heart failure, arterial embolism, sudden death – Cats with HR <200 bpm have better Px than >200 bpm – Median survival time ~2 y
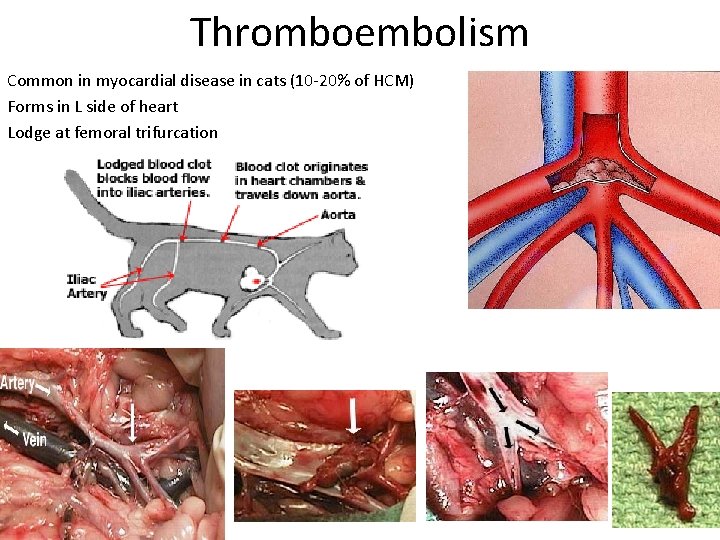
Thromboembolism Common in myocardial disease in cats (10 -20% of HCM) Forms in L side of heart Lodge at femoral trifurcation

Thromboembolism • Signs – – • Dx Acute onset of rear leg pain/paresis Cold, bluish foot pads Lack of femoral pulse Hx of myocardial disease – Clinical signs – Angiography (if available) • Rx – Dissolve clot • TPA (Activase [Genentech]) • Heparin – Aspirin for prophylaxis • Aspirin is slowly metabolized in cats; must be monitored • Client info – Painful, cold, or paralyzed rear legs in cats is an emergency – Px is guarded to poor – Surgical removal of thrombus is difficult/expensive
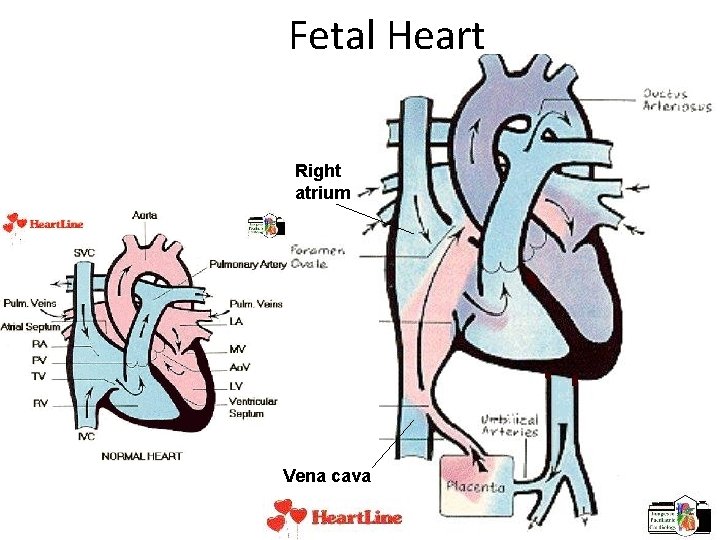
Fetal Heart Right atrium Vena cava
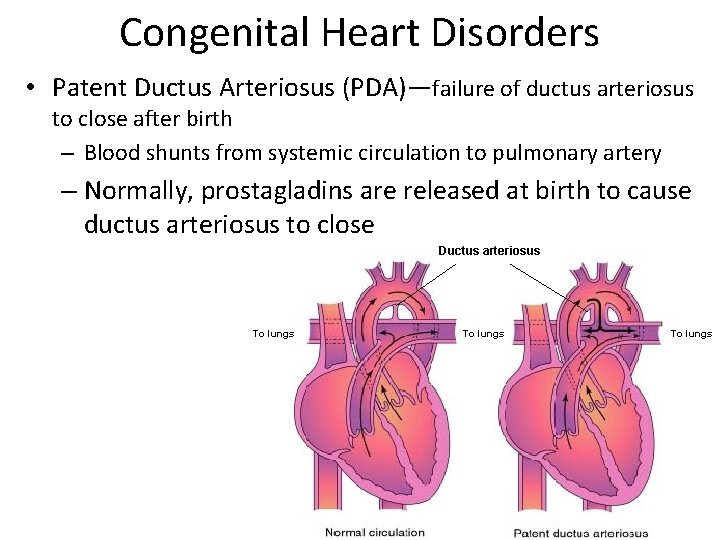
Congenital Heart Disorders • Patent Ductus Arteriosus (PDA)—failure of ductus arteriosus to close after birth – Blood shunts from systemic circulation to pulmonary artery – Normally, prostagladins are released at birth to cause ductus arteriosus to close Ductus arteriosus To lungs

PDA • Clinical signs – Usually female – Predisposed breeds: chi, collie, maltese, poodle, poms, E Spring, kees, bichons frises, Shetlands – Presence of a loud heart murmur over L thorax – Some puppies are asymptomatic • Dx – ECG • L vent dilation – X-ray • L atrial and L vent enlargement • Rx—surgical correction • Client info – Px is excellent following surgery – 64% of PDA will die within 1 y without surgery – Dog should not be used for breeding
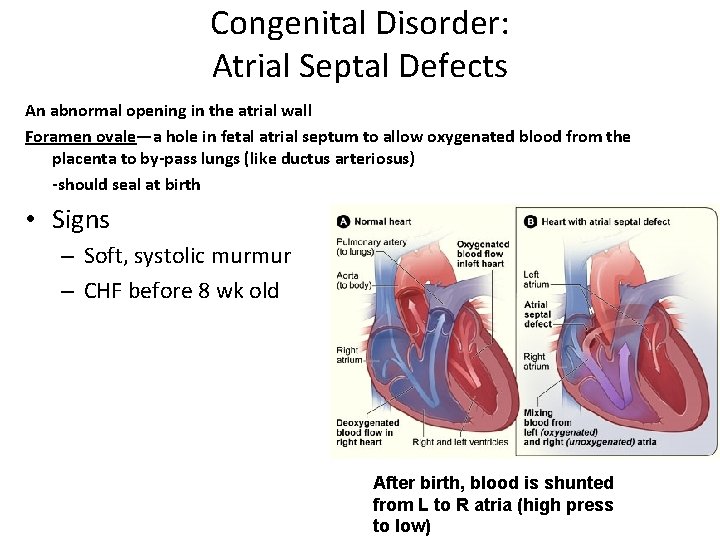
Congenital Disorder: Atrial Septal Defects An abnormal opening in the atrial wall Foramen ovale—a hole in fetal atrial septum to allow oxygenated blood from the placenta to by-pass lungs (like ductus arteriosus) -should seal at birth • Signs – Soft, systolic murmur – CHF before 8 wk old C After birth, blood is shunted from L to R atria (high press to low)
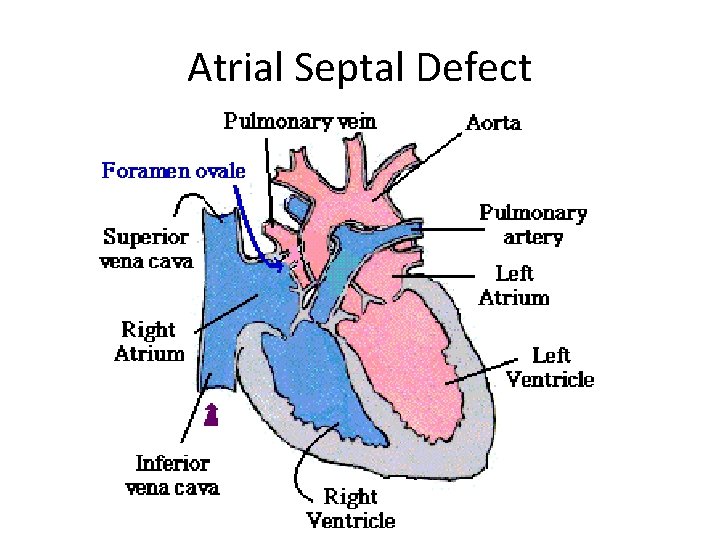
Atrial Septal Defect
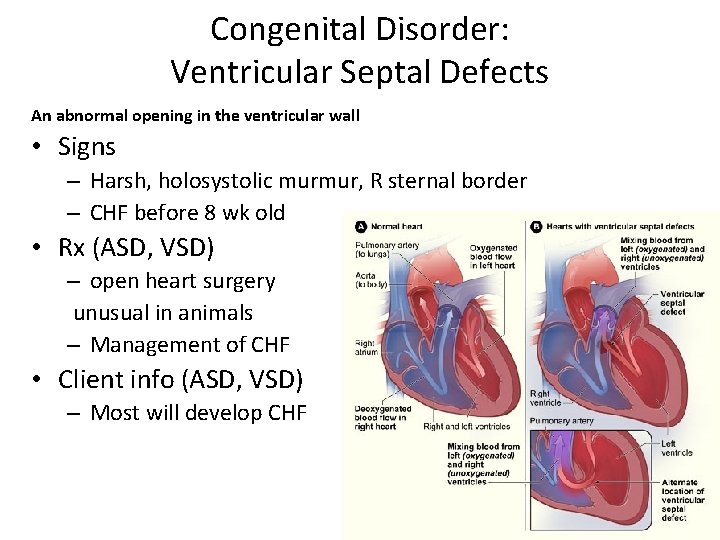
Congenital Disorder: Ventricular Septal Defects An abnormal opening in the ventricular wall • Signs – Harsh, holosystolic murmur, R sternal border – CHF before 8 wk old • Rx (ASD, VSD) – open heart surgery unusual in animals – Management of CHF • Client info (ASD, VSD) – Most will develop CHF C
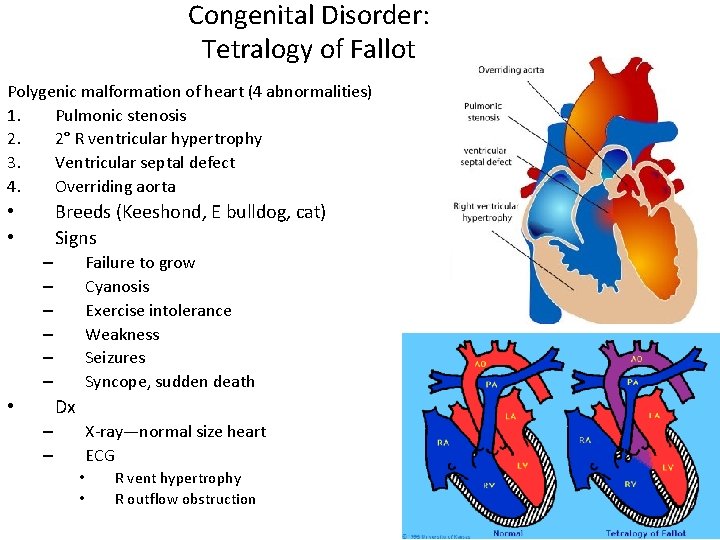
Congenital Disorder: Tetralogy of Fallot Polygenic malformation of heart (4 abnormalities) 1. Pulmonic stenosis 2. 2° R ventricular hypertrophy 3. Ventricular septal defect 4. Overriding aorta Breeds (Keeshond, E bulldog, cat) Signs • • Failure to grow Cyanosis Exercise intolerance Weakness Seizures Syncope, sudden death – – – Dx • X-ray—normal size heart ECG – – • • R vent hypertrophy R outflow obstruction

Tetralogy of Fallot • Rx – Surgical procedures can improve condition (cardiology specialty practice) – Medical treatment includes phlebotomy to keep PCV between 62 -68% • Client info – – – Genetic disease; don’t breed Sudden death is common; may live for years CHF is rare Limit stress/exercise Tranquilizers/sedatives may have adverse effects Regular phlebotomies will be required
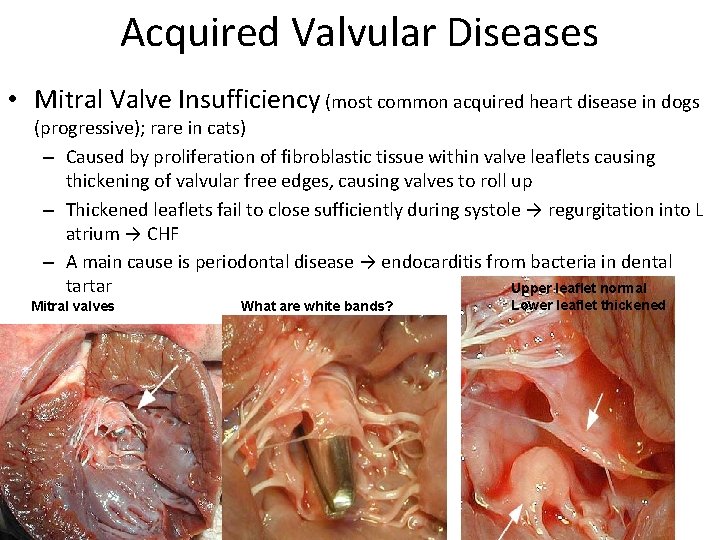
Acquired Valvular Diseases • Mitral Valve Insufficiency (most common acquired heart disease in dogs (progressive); rare in cats) – Caused by proliferation of fibroblastic tissue within valve leaflets causing thickening of valvular free edges, causing valves to roll up – Thickened leaflets fail to close sufficiently during systole → regurgitation into L atrium → CHF – A main cause is periodontal disease → endocarditis from bacteria in dental tartar Upper leaflet normal Mitral valves What are white bands? Lower leaflet thickened
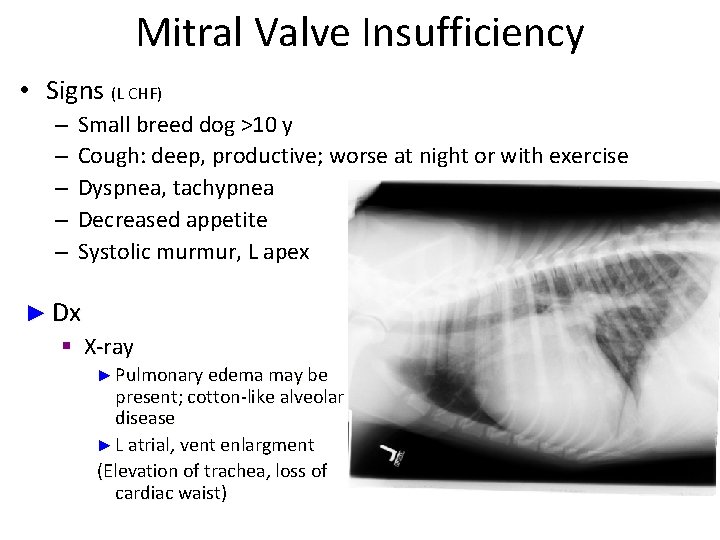
Mitral Valve Insufficiency • Signs (L CHF) – – – Small breed dog >10 y Cough: deep, productive; worse at night or with exercise Dyspnea, tachypnea Decreased appetite Systolic murmur, L apex ► Dx § X-ray ► Pulmonary edema may be present; cotton-like alveolar disease ► L atrial, vent enlargment (Elevation of trachea, loss of cardiac waist)

Mitral Valve Insufficiency • Rx—there is no cure; goal is to improve quality of life – Diuretics—furosemide to reduce fluid volume of heart – Digoxin—to increase efficiency of heart and ↓HR • Client info – MVI is a progressive disease; periodic evaluation/readjustment of Rx – No cure – Low salt diet helps prevent fluid accumulation – Eventually medication will not control the condition Mitral valve (L A-V)

Tricuspid Insufficiency • Same disease as Mitral Valve Insufficiency except R sided heart failure results instead of L sided failure • Signs (R CHF) – Pleural effusion (fluid in pleural cavity not lung tissue) – Abdominal distension – Hepatomegaly • Rx—same as MVI Tricuspid valve (R A-V) – Abdominocentesis may be required periodically
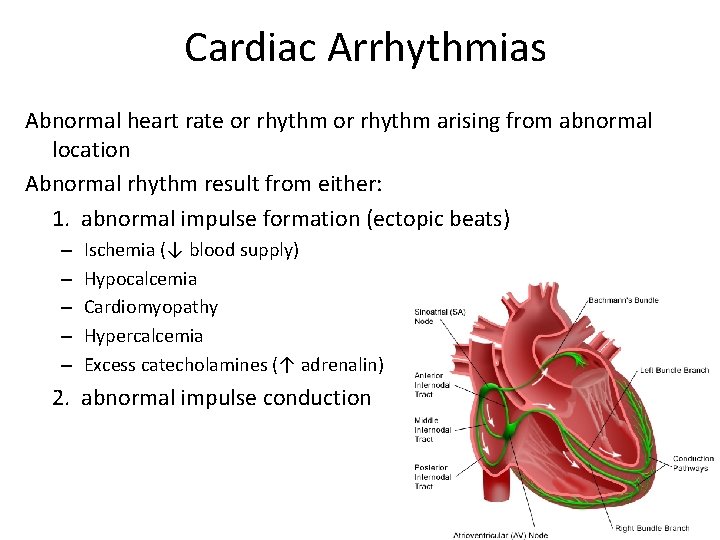
Cardiac Arrhythmias Abnormal heart rate or rhythm arising from abnormal location Abnormal rhythm result from either: 1. abnormal impulse formation (ectopic beats) – – – Ischemia (↓ blood supply) Hypocalcemia Cardiomyopathy Hypercalcemia Excess catecholamines (↑ adrenalin) 2. abnormal impulse conduction
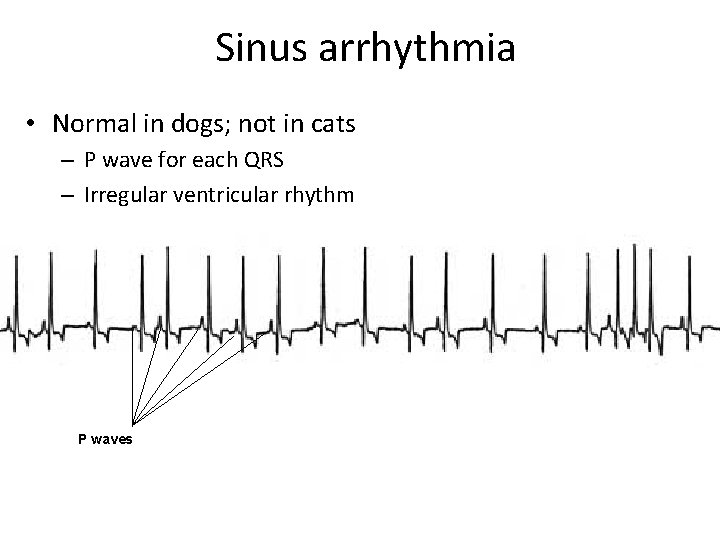
Sinus arrhythmia • Normal in dogs; not in cats – P wave for each QRS – Irregular ventricular rhythm P waves
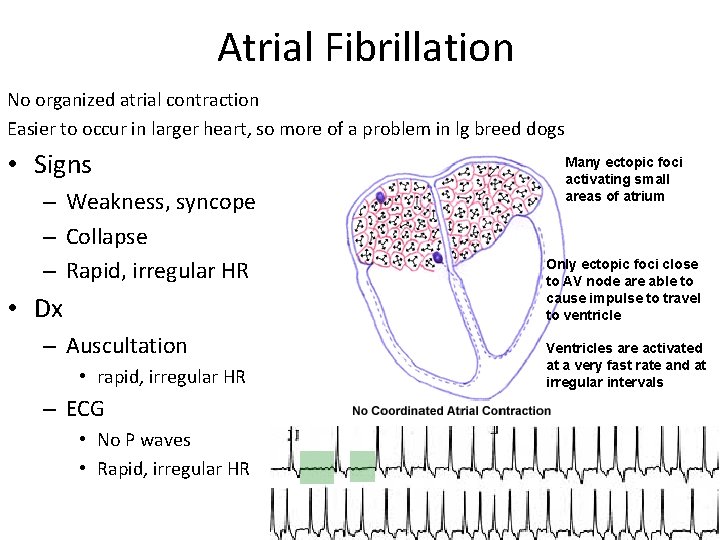
Atrial Fibrillation No organized atrial contraction Easier to occur in larger heart, so more of a problem in lg breed dogs • Signs – Weakness, syncope – Collapse – Rapid, irregular HR • Dx – Auscultation • rapid, irregular HR – ECG • No P waves • Rapid, irregular HR Many ectopic foci activating small areas of atrium Only ectopic foci close to AV node are able to cause impulse to travel to ventricle Ventricles are activated at a very fast rate and at irregular intervals

Atrial Fibrillation • Rx (aim is to slow HR; it will not correct fibrillation) – Digitalis (digoxin) to slow HR – Ca++ channel blockers (diltiazem HCl) to slow AV node conduction • Client info – Rx will not cure atrial fibrillation – Concurrent heart disease will progress even with treatment – CHF will occur eventually

Ventricular Tachycardia Rapid HR reduces vent filling time, and, therefore decreases CO If untreated, may lead to vent fibrillation (cardiac arrest), a life-threatening situation • Causes: – Cardiomyopathy, CHF, endocarditis, neoplasia – Electrolyte or acid/base imbalance • Signs – Weakness, collapse, syncope with rapid HR – Sudden death not uncommon – CHF
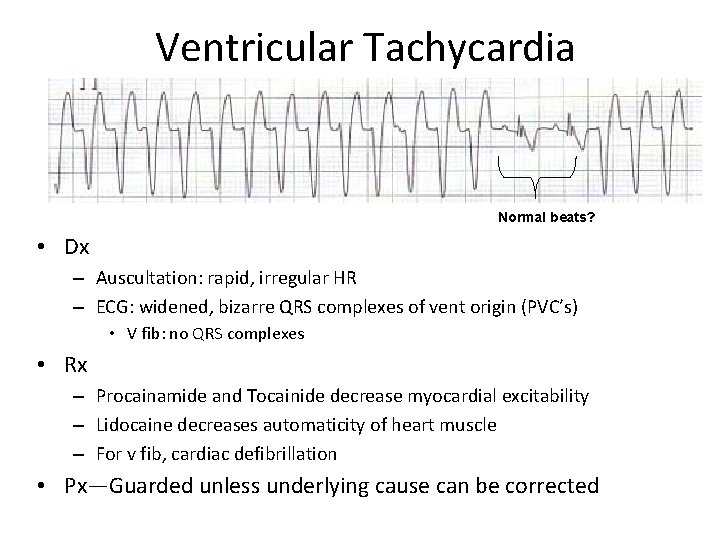
Ventricular Tachycardia Normal beats? • Dx – Auscultation: rapid, irregular HR – ECG: widened, bizarre QRS complexes of vent origin (PVC’s) • V fib: no QRS complexes • Rx – Procainamide and Tocainide decrease myocardial excitability – Lidocaine decreases automaticity of heart muscle – For v fib, cardiac defibrillation • Px—Guarded unless underlying cause can be corrected
Sinus bradycardia Def: normal P, QRS complexes; HR <70 bpm May be symptom of disease: • – – – • ↑ Intracranial pressure Hypothyroidism Hypothermia Hyperkalemia Hypoglycemia Also seen in athletic, well-conditioned dogs

Sinus bradycardia • Signs – Episodic weakness, syncope, collapse • Dx – Auscultation: slow HR – ECG: slow HR; normal P, QRS complexes • Rx – Treat underlying disease – Atropine increases HR – Placement of artificial pacemaker • Client info – May be normal in athletic dog – Correction of underlying problem may correct bradycardia – Most dogs can live normal life with this condition
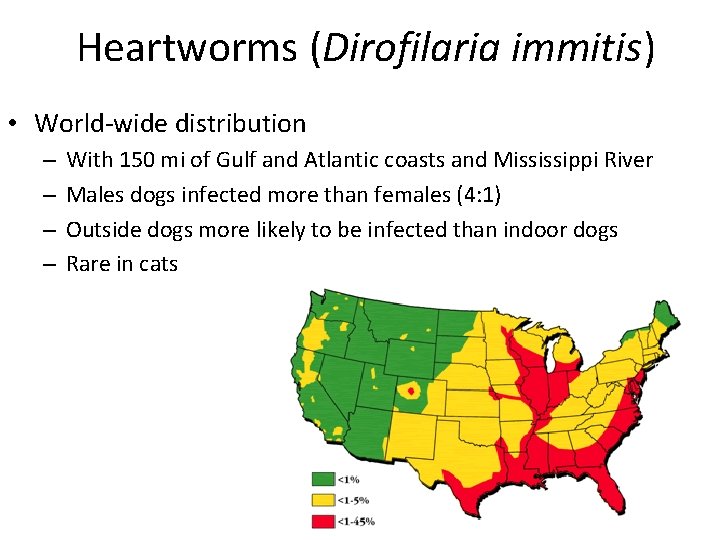
Heartworms (Dirofilaria immitis) • World-wide distribution – – With 150 mi of Gulf and Atlantic coasts and Mississippi River Males dogs infected more than females (4: 1) Outside dogs more likely to be infected than indoor dogs Rare in cats
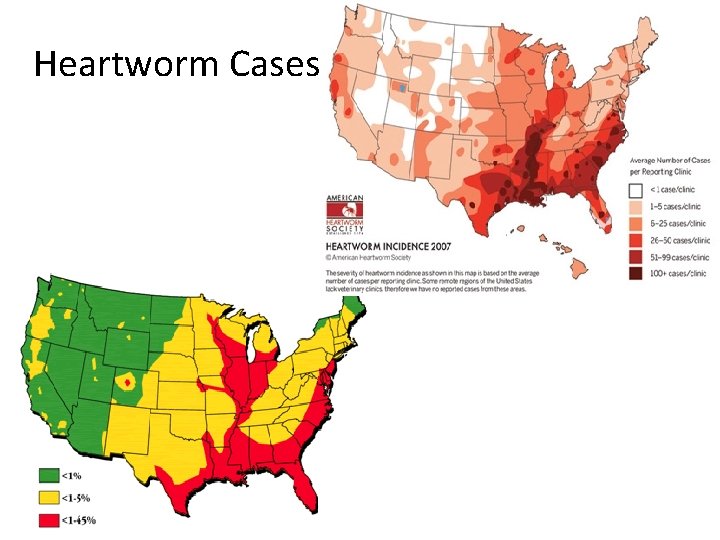
Heartworm Cases
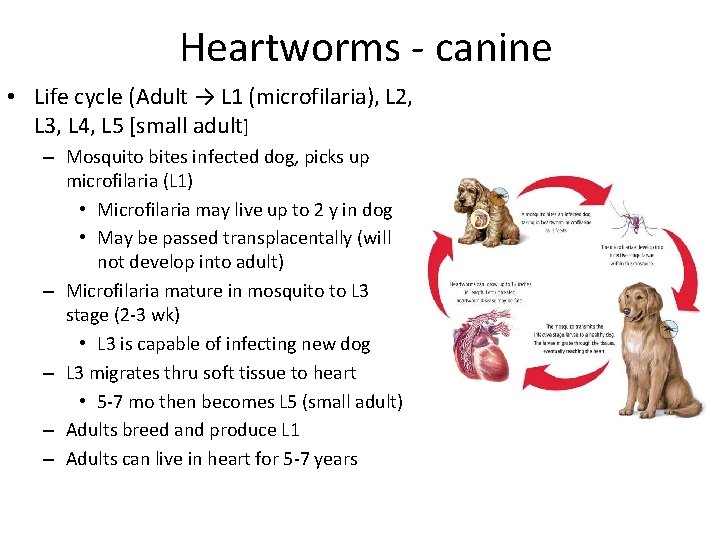
Heartworms - canine • Life cycle (Adult → L 1 (microfilaria), L 2, L 3, L 4, L 5 [small adult] – Mosquito bites infected dog, picks up microfilaria (L 1) • Microfilaria may live up to 2 y in dog • May be passed transplacentally (will not develop into adult) – Microfilaria mature in mosquito to L 3 stage (2 -3 wk) • L 3 is capable of infecting new dog – L 3 migrates thru soft tissue to heart • 5 -7 mo then becomes L 5 (small adult) – Adults breed and produce L 1 – Adults can live in heart for 5 -7 years
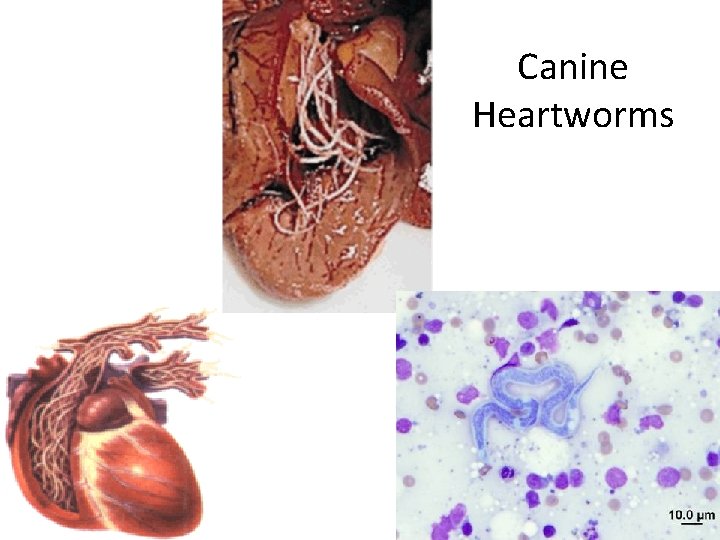
Canine Heartworms
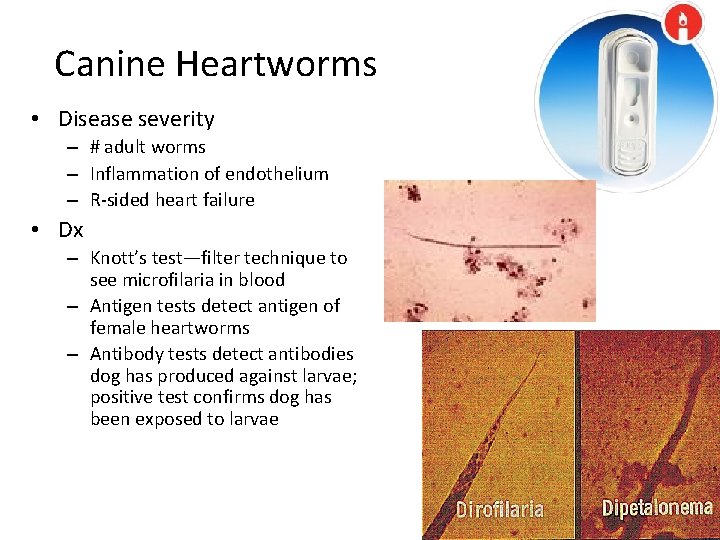
Canine Heartworms • Disease severity – # adult worms – Inflammation of endothelium – R-sided heart failure • Dx – Knott’s test—filter technique to see microfilaria in blood – Antigen tests detect antigen of female heartworms – Antibody tests detect antibodies dog has produced against larvae; positive test confirms dog has been exposed to larvae
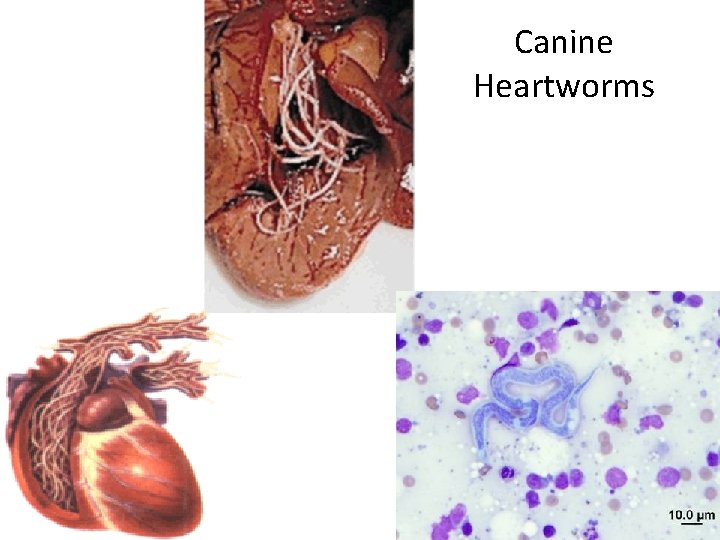
Canine Heartworms
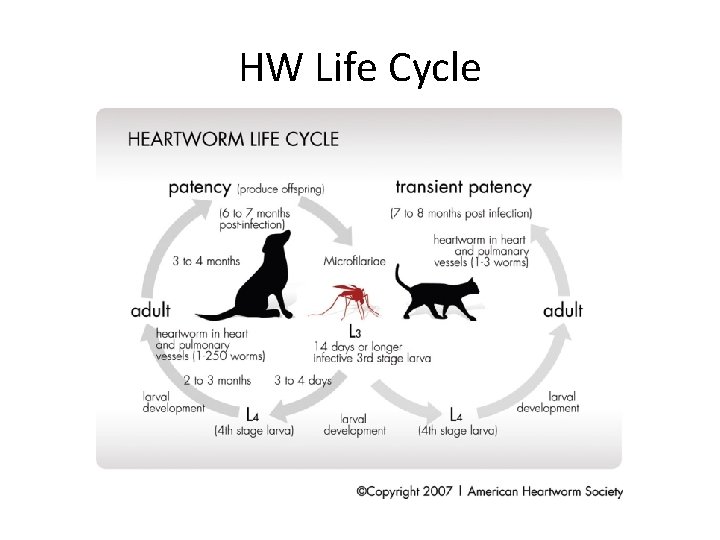
HW Life Cycle

Heartworms • Signs – – Usually asymptomatic; diagnoses on routine screening Exercise intolerance Coughing, dyspnea R-sided heart failure • Rx—pretreatment lab workup (CBC, Chem Panel) – Melarsomine (Immiticide; Merial)—kills adult worms – Ivermectin—kills microfilaria and migrating worms (L 3, L 4) – +/- Doxycycline – Prevention—many products – Diethylcarbamazine (daily) – Ivermectin (monthly) – Milbemycin (monthly)

Feline Heartworms • Prevalence – 1997 necropsy survey in SE Texas – 10% of shelter cats had adult HW – Greater infection rate than Fe. LV or FIV

Feline Heartworms • Epidemiology – – – Female mosquito feeds on infected dog; picks up mf Become L 1 to L 3 in mosquito Deposited on skin of cat or dog in saliva L 3 enter thru bite, molt to L 4, migrate through tissues for 2 months Final molt to immature adult (previously L 5); enter peripheral vein Immature worms carried to heart – 75 -90 days PI By day 100 – worms 2 inches long Matures to adult over 2 -3 months Most juvenile worms die shortly after arriving in pulmonary arteries Initiates an inflammatory reaction A few worms live 2 -4 years in small percentage of cats

Feline Heartworms- Heartworm Asocciated Respiratory Disease (HARD) • 3 stages – 1 st • Acute inflammatory reaction to presence and death of worms • Coughing, dyspnea • Intermittent vomiting • 28% asymptomatic • X-rays – inflammatory infiltrates around R caudal lobar artery • Similar to allergic bronchitis or asthma • Responds to steroids

Feline HARD • 2 nd stage – Adult HW (if survives) suppresses immune system => decreased signs – Worm dies – no more immune suppression – Intense inflammatory reaction occurs – Thromboembolism => acute lung injury and sudden death • 3 rd stage – If cat lives => permanent injury and chronic resp disease

Feline Heartworms • Diagnosis – Filtration for mf useless – usually single sex infections (1 -2 worms only) – X-rays as above – 55% have radiographic signs – US – 70 -100% accurate – Serology • Ag tests – do not detect early or male only infections – Negative result does not r/o HW dz • Ab test – confirms recent infection with L 4 or older but not disease • Ag test in process of being added to Fe. LV/FIV test.
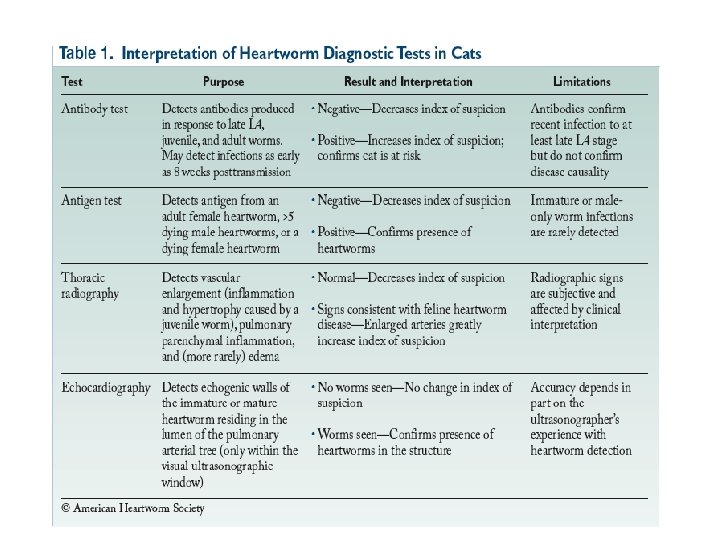

Feline Heartworm Testing
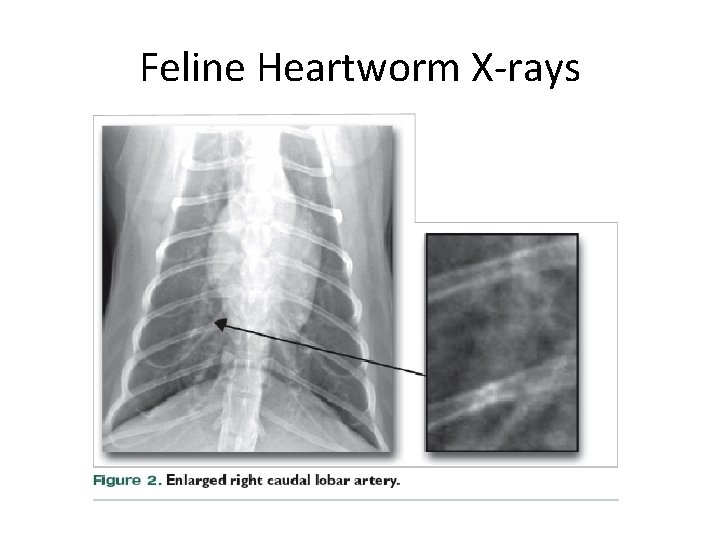
Feline Heartworm X-rays

Feline Heartworms • Rx— – Acute respiratory distress • Steroids (Dex SP 1 -2 mg/kg IM/IV, Pred. SS 50 -100 mg/kg/cat IV • Bronchodilator • Supportive – IV fluids, etc – If not demonstrating clinical signs, supportive care until heartworm dies • Prednisolone to reduce pulmonary effects – +/- doxycycline

Feline Heartworms • Prevention – – – Safe for all cats because mf infection rare or minimal Heartgard® for Cats (Ivermectin, orally) from Merial Interceptor® (Milbemycin oxime, orally) from Novartis Revolution® (Selemectin, topically) from Pfizer Advantage Multi™ for Cats (Moxidectin / imidacloprid, topically) from Bayer
Respiratory Diseases

Upper Respiratory Diseases Upper Respiratory Tract is any resp structure above the trachea • Rhinitis—inflammation/infection of nasal passages Usually occurs with other resp diseases – Signs • Nasal discharge; crusty nares • Pawing at nose • Staphylococcus spp – Rx • Clean nares • Antibiotics if necessary
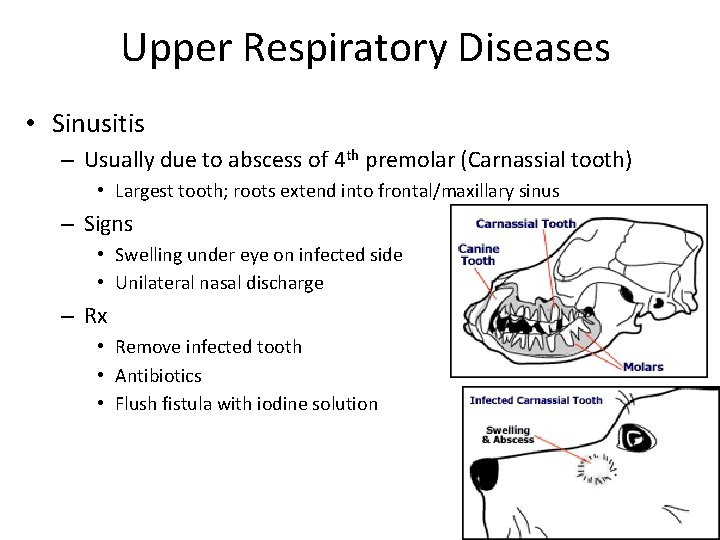
Upper Respiratory Diseases • Sinusitis – Usually due to abscess of 4 th premolar (Carnassial tooth) • Largest tooth; roots extend into frontal/maxillary sinus – Signs • Swelling under eye on infected side • Unilateral nasal discharge – Rx • Remove infected tooth • Antibiotics • Flush fistula with iodine solution
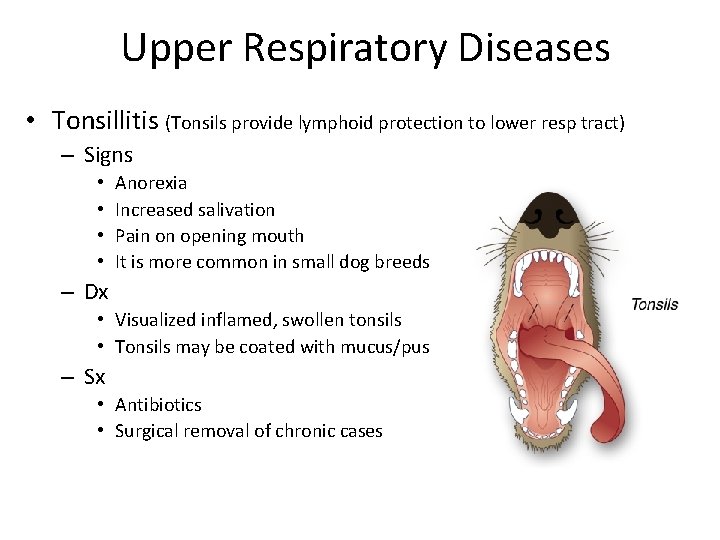
Upper Respiratory Diseases • Tonsillitis (Tonsils provide lymphoid protection to lower resp tract) – Signs • • Anorexia Increased salivation Pain on opening mouth It is more common in small dog breeds – Dx • Visualized inflamed, swollen tonsils • Tonsils may be coated with mucus/pus – Sx • Antibiotics • Surgical removal of chronic cases
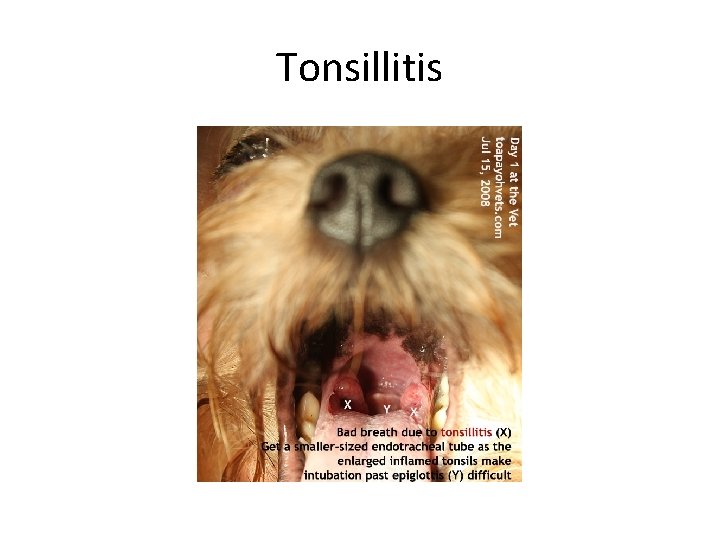
Tonsillitis

Upper Respiratory Diseases • Laryngitis Most common cause is excessive barking **Rabies can also change vocal quality • Signs – Loss of voice or alteration of voice – Increased mucus production in back of throat • Rx – Restrict barking – Anti-inflammatory medication (glucocorticoids) • Client info – Most Upper Respiratory Infections are self-limiting

Lower Respiratory Diseases Lower Respiratory Tract includes trachea, bronchi, lungs, pleural cavity • Infectious Canine Tracheobronchitis (Kennel Cough) – Causes (a collection of several causative agents including viruses, bacteria, mycoplasmas, fungi, parasites • • • Canine parainfluenza virus Canine adenovirus Canine herpesvirus Reovirus Bordetella bronchiseptica mycoplasma – Signs • Hx of exposure to animals at a kennel, hospital, groomer, show • Dry hacking cough in an otherwise healthy animal – Rx—antibiotics, glucocorticoids, antitussives – Client info • Self-limiting (2 -3 wks); Rx is to make animal/owner more comfortable • Vaccinate 2 -3 wk before chance of exposure
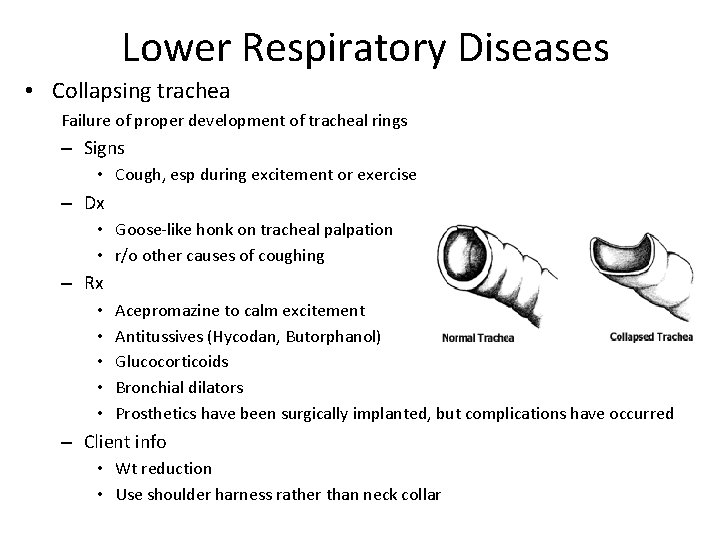
Lower Respiratory Diseases • Collapsing trachea Failure of proper development of tracheal rings – Signs • Cough, esp during excitement or exercise – Dx • Goose-like honk on tracheal palpation • r/o other causes of coughing – Rx • • • Acepromazine to calm excitement Antitussives (Hycodan, Butorphanol) Glucocorticoids Bronchial dilators Prosthetics have been surgically implanted, but complications have occurred – Client info • Wt reduction • Use shoulder harness rather than neck collar

Lower Respiratory Diseases • Feline Bordetella Infection Bordetella bronchiseptica grow in ciliated respiratory mucosa; release toxins – Signs (look like respiratory viral infections) • Fever • Sneezing, nasal discharge, coughing, rales • Submandibular lymphadenopathy – Rx (usually self-limiting) • Antibiotics (oral tetracycline or doxycycline) – Prevention • Eliminate stress • Good hygiene, good nutrition • Vaccination – Client info • Looks like resp infections caused by feline herpes and calicivirus • Usually self-limiting • Vaccination effective

Lower Respiratory Diseases • Feline asthma (bronchoconstriction, inflamed/hyperreactive airways) – Signs • Coughing, wheezing • Labored breathing – Dx • Clinical signs • X-rays show “doughnuts” typical of airway inflammation – Rx • Long-term corticosteroids (prednisone, Depo. Medrol) • Bronchodilators (terbutaline [Brethine], cyproheptadine) – Client info • Prognosis is variable – If allergens can be determined and exposure limited, most cats do well – A cure is not usually possible

Feline Asthma • Same cat – Top—normal – Bottom—asthma Airways more prominent because of inflammation and mucus buildup Doughnuts (end-on view) and tramways (lateral view) of airways

Feline Viral Resp Infections • 2 viruses responsible for most feline resp diseases – Feline Viral Rhinotracheitis (FVR; Feline Herpesvirus) – Feline Calicivirus (FCV) Caliciviridae family • • Highly contagious High mobidity Low mortality Most severe in kittens

Feline Viral Rhinotracheitis • Signs – – – Acute onset of sneezing Conjunctivitis, severe rhinitis Fever, depression, anorexia Ulcerated hard palate, excess salivation Corneal ulcers • Rx – Supportive Rx • IV fluids, broad spectrum antibiotics, decongestants • Nursing care: clean nose, eyes; force feed food; decrease stress • Antiviral therapy • Prevention – Vaccination • Client info – – FVR highly contagious; can transmit via clothing, hands, etc; only cats Warming food may improve palatability Vaccinated cats may show mild symptoms Disinfectants kill herpesvirus type I virus

Feline Calicivirus • Signs – – – • Rx Fever Serous ocular/nasal discharge; mild conjunctivitis Oral ulcers, salivation Pneumonia Diarrhea – Supportive care – Antibiotics – Force feed disinfect using bleach • Prevention – Vaccination • Client info – Highly contagious – Signs last 5 -7 d – Force-feeding may be necessary (if cats can’t smell, they won’t eat)
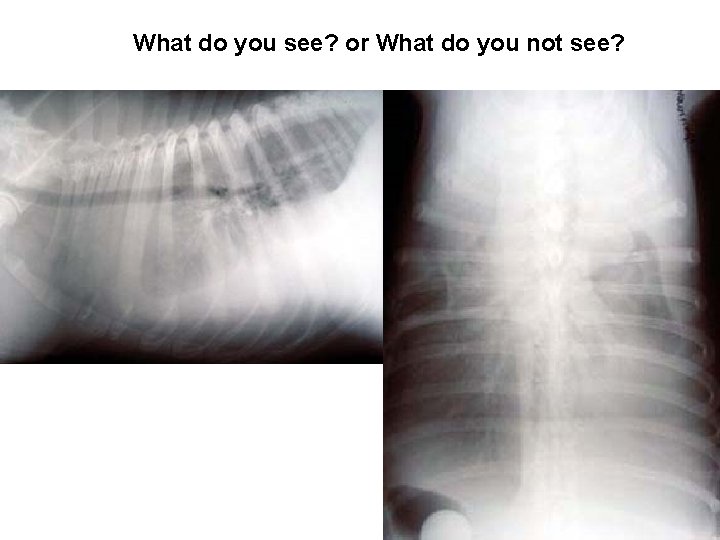
What do you see? or What do you not see?
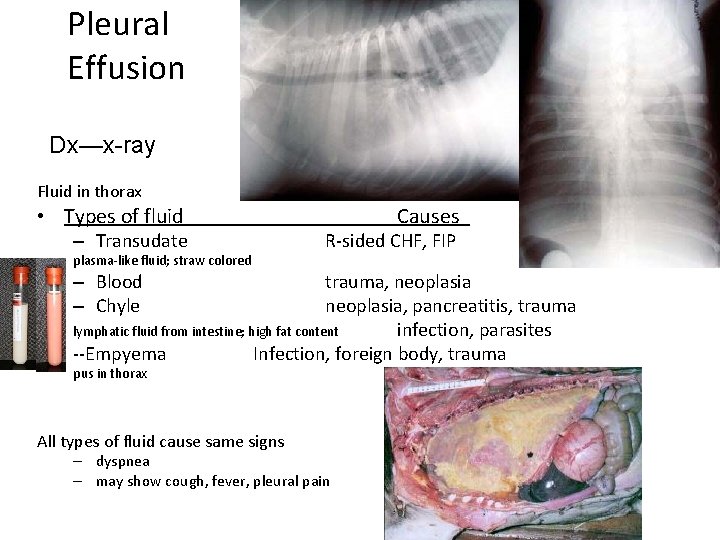
Pleural Effusion Dx—x-ray Fluid in thorax • Types of fluid – Transudate plasma-like fluid; straw colored Causes R-sided CHF, FIP – Blood – Chyle trauma, neoplasia, pancreatitis, trauma lymphatic fluid from intestine; high fat content infection, parasites --Empyema Infection, foreign body, trauma pus in thorax All types of fluid cause same signs – dyspnea – may show cough, fever, pleural pain

Pleural Effusion • Thoracentesis – Clip hair, scrub skin, block with local anesthetic • Most dependent space (7 th-8 th intercostal space) – Aspirate using 3 way valve – Remove as much fluid as possible • Do not create pheumothorax – Analyze aspirate • Rx—depends on pathology causing effusion • Client info – Owner may need to continue pleural drainage – Unless 1° is treated, effusion will return – Rx can be long and expensive
Fungi
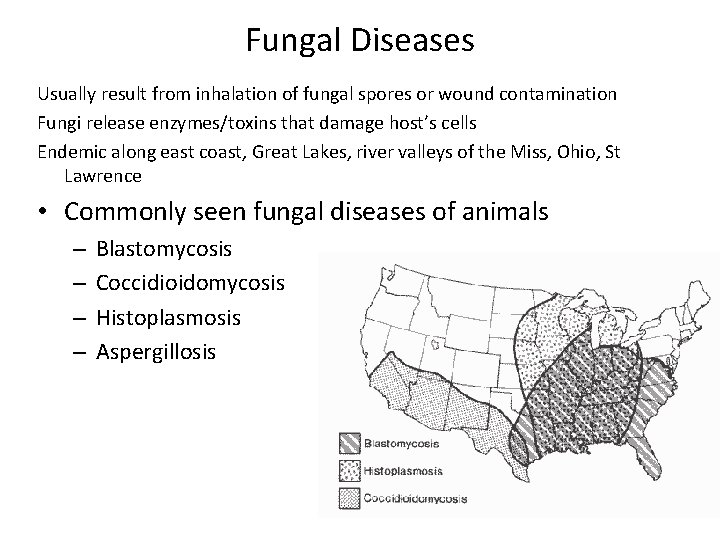
Fungal Diseases Usually result from inhalation of fungal spores or wound contamination Fungi release enzymes/toxins that damage host’s cells Endemic along east coast, Great Lakes, river valleys of the Miss, Ohio, St Lawrence • Commonly seen fungal diseases of animals – – Blastomycosis Coccidioidomycosis Histoplasmosis Aspergillosis

Blastomycosis (Blastomyces dermatitides) • Signs (non specific) – Anorexia, depression, wt loss – Fever, cough, dyspnea – Enlarged LN • Dx – X-rays—diffuse, nodular interstitial lung pattern (x-ray) – Serology testing is available – Most cases are diagnosed in the fall. • Rx – Amphotericin B • Client info – Blastomycosis usually not zoonotic disease, however, use caution with animals with draining wounds – Owners share same environment and are likely to be exposed – Relapses are common – Rx is expensive
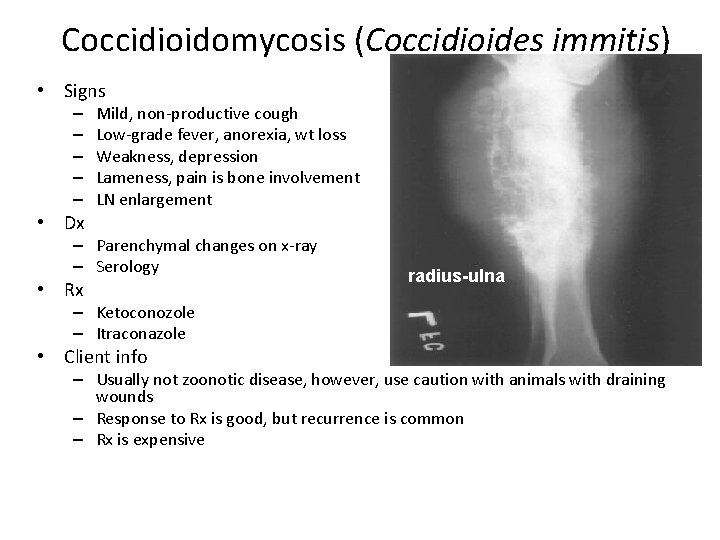
Coccidioidomycosis (Coccidioides immitis) • Signs – – – • Dx Mild, non-productive cough Low-grade fever, anorexia, wt loss Weakness, depression Lameness, pain is bone involvement LN enlargement – Parenchymal changes on x-ray – Serology • Rx radius-ulna – Ketoconozole – Itraconazole • Client info – Usually not zoonotic disease, however, use caution with animals with draining wounds – Response to Rx is good, but recurrence is common – Rx is expensive
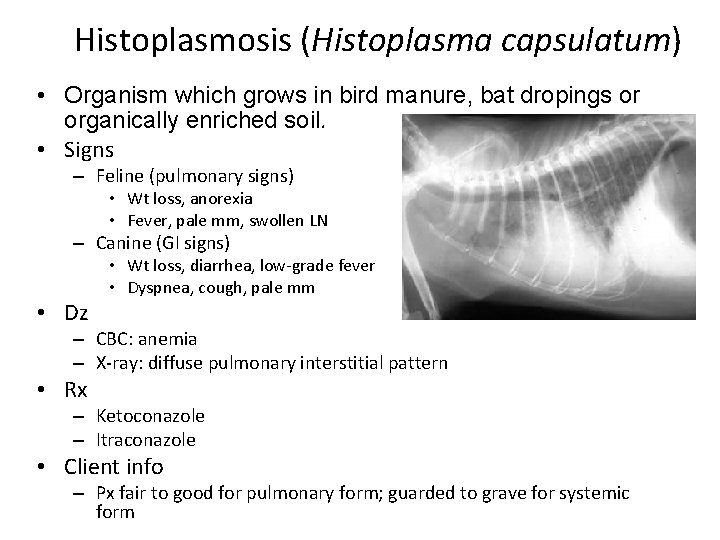
Histoplasmosis (Histoplasma capsulatum) • Organism which grows in bird manure, bat dropings or organically enriched soil. • Signs – Feline (pulmonary signs) • Wt loss, anorexia • Fever, pale mm, swollen LN – Canine (GI signs) • Dz • Wt loss, diarrhea, low-grade fever • Dyspnea, cough, pale mm – CBC: anemia – X-ray: diffuse pulmonary interstitial pattern • Rx – Ketoconazole – Itraconazole • Client info – Px fair to good for pulmonary form; guarded to grave for systemic form

Cryptococcosis (Cryptococcus neoformans) A yeast-like fungus found in soil contaminated with pigeon and other bird droppings. Inhalation major route of infection. Immunocompromised animal more susceptible than normal animal • Signs – Feline • Lesions in nasal and sinus cavities; chronic nasal discharge • enlarged LN, wt loss, anorexia, lwo-grade fever – Canine • Dx • Usually CNS lesions (vestibular dysfunction) – Cytology of aspirates, impression smears – Antigen test available • Rx – Amphotericin B – Ketoconozole – Itraconazole • Px – Fair to good unless CNS involvement – No known health hazard to humans

Aspergillosis (Aspergillus fumigatus) Inhalation major route of infection; nasal cavity is main location of lesions • Signs – Feline (uncommon) • May be immunocompromised (Fe. LV) • Lethargy, fever, wt loss, anorexia – Canine (localized) • Young to middle age • Chronic nasal discharge, sneezing, loud breathing (like snoring) – Canine (generalized infection) • Primarily seen in G Shep • Wt loss, anorexia • fever, lameness, paresis/paralysis • Dx – X-ray—loss of nasal turbinates – endoscopy: --yellow-green to black fungal plaques on nasal mucosa Rx—topical clotrimazole • • Client info – Localized dis—poor Px; Generalized dis—grave Px; not zoonotic

Pulmonary Neoplasms Tumors in lungs are usually metastatic, although primary lung tumors do occur • Signs – Primary neoplasia • Cough, exercise intolerance • Wt loss, poor condition • Dysphagia, vomiting, anorexia – Metastatic neoplasia • Evidence of primary tumor at other location • Same signs as above for Primary neoplasia
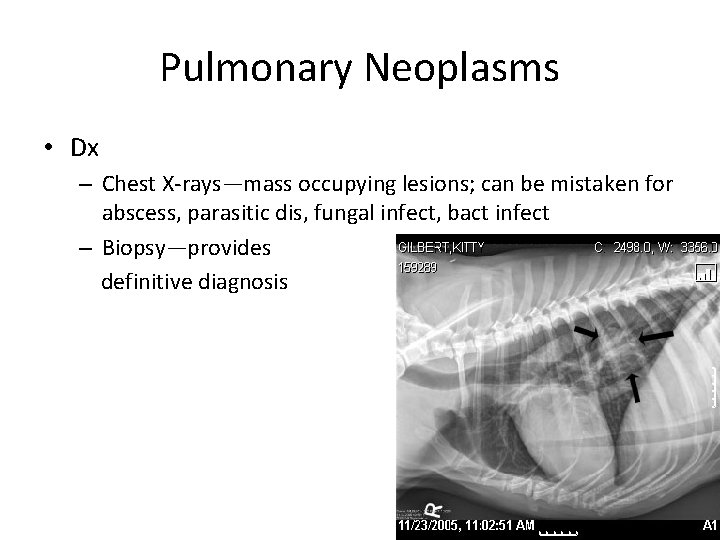
Pulmonary Neoplasms • Dx – Chest X-rays—mass occupying lesions; can be mistaken for abscess, parasitic dis, fungal infect, bact infect – Biopsy—provides definitive diagnosis

Pulmonary Neoplasms Same dog as x-ray • Rx—surgical removal is TOC – Lobectomy for solitary tumor • Chemotherapy (may reduce tumor size, may not increasse survival time • Client Info – Px is guarded to grave – By the time these tumors are diagnosed, they are usually in advanced stages – Chemotherapy may reduce clinical symptoms
- Slides: 88