Cardiopulmonary History and Exam Wendy Blount DVM Housekeeping
Cardiopulmonary History and Exam Wendy Blount, DVM

Housekeeping • Dylan is our “concierge” • Let her know if you need another note pad • Or anything else! • Course materials are also downloadable at • • • http: //wendyblount. com Direct link: http: //wendyblount. com/cardiology. php Click on Presentation Notes
Housekeeping • Dylan is our “concierge” • Let her know if you need another note pad • Or anything else! • Course materials are also downloadable at • • • http: //wendyblount. com Direct link: http: //wendyblount. com/cardiology. php Click on Presentation Notes

Housekeeping • Click on this presentation at the top
Housekeeping • Click on this presentation at the top

Housekeeping Seminar Packet: • • • Flash Drive Agenda Evaluation CE Certificate pen and notepad List of Abbreviations Hank and Eli Fund, Dark Horse Lodge info Cardiology Form, Global. FAST® Forms & Handouts Instructions for screen sharing Info on hands-on ultrasound training

Housekeeping Flash Drive: • • • All Power. Points with embedded videos. pdfs of Power. Points – 1 and 6 slides per page Forms – in clinic and lab submission Scientific articles Diagnostic and treatment aid handouts Agenda, abbreviations, instructions for following along • Hank and Eli Fund, Dark Horse Lodge info

Housekeeping • We will take a 5 minute break each hour and a half, but take your own breaks as you wish PLEASE PARTICIPATE!!! • But take private conversations outside or, in the classroom or store • Get your CE certificate signed at the end of each day • If you leave early, the time will be added to the form • Pretty Please fill out the Course Evaluation form • Leave with Dylan

Our Host • Smoking outside the entrance, in the designated area • Restrooms through the door at the back of the room, and to the left of the classroom • Lunch will be served there • There is no cell service in the building – enable Wi. Fi Calling • Wi. Fi: Meadow. Ridge Password: safety 01

Social Distancing • IR (non-contact) temperature at morning sign in • Anyone with a fever will not be admitted • Tables & chairs disinfected with Rescue daily • Rescue wipes and spray at the sanitation table • Treat it like a surgery table • Use hand sanitizer each time you access the table • Masks are encouraged but not required • If you come within 6 feet of another person, please wear your mask – especially during breaks, meals and the dry lab, and especially for people >65 yrs
Social Distancing • Those who are already significantly exposed to each other prior to the seminar may share a table • No more than 2 people at a table • The seat you have chosen is yours for the weekend • Place OCCUPIED table marker in your packet on your table, so others know it is reserved for you. • Wear the HIGH RISK nametag in your packet if you wish • Hand sanitizer at your table – use it often • Wash your hands as often as is possible • No touching anyone else’s table or chair or ANYTHING YOU CAN AVOID TOUCHING!

Social Distancing • When lining up for food or dry lab, please stay 6 feet behind the next person • MASKS ARE REQUIRED FOR THE DRY LAB • Food will be served to you, and single use condiments are available on request • Sanitize hands before (and after if you can) • touching any doorknobs or other shared items • Touching the sign-in table – Dylan will sign you in and I will sign you out • Touching anything but your stuff on your table

Following Along 1. Screen at the front of the room 2. Flash Drive –. pdfs of Power. Points - 1 & 6 slides/page –. pptx of Power. Points – Filed in section folders 3. Website – updated Power. Points – http: //wendyblount. com/cardiogy. php 4. Screen Sharing: www. startmeeting. com – Click on the “join” button at the top right
Following Along 1. Screen at the front of the room 2. Flash Drive –. pdfs of Power. Points - 1 & 6 slides/page –. pptx of Power. Points – Filed in section folders 3. Website – updated Power. Points – http: //wendyblount. com/cardiogy. php 4. Screen Sharing: www. startmeeting. com – Click on the “join” button at the top right

Following Along 1. Screen at the front of the room 2. Flash Drive –. pdfs of Power. Points - 1 & 6 slides/page –. pptx of Power. Points – Filed in section folders 3. Website – updated Power. Points – http: //wendyblount. com/cardiogy. php 4. Screen Sharing: www. startmeeting. com – Click on the “join” button at the top right
Following Along 1. Screen at the front of the room 2. Flash Drive –. pdfs of Power. Points - 1 & 6 slides/page –. pptx of Power. Points – Filed in section folders 3. Website – updated Power. Points – http: //wendyblount. com/cardiogy. php 4. Screen Sharing: www. startmeeting. com – Click on the “join” button at the top right
Following Along 1. Screen at the front of the room 2. Flash Drive –. pdfs of Power. Points - 1 & 6 slides/page –. pptx of Power. Points – Filed in section folders & Power. Point folder 3. Website – updated Power. Points – http: //wendyblount. com/neurology. php 4. Screen Sharing: www. startmeeting. com – Click on the “join” button at the top right

Practical Vet. Med Philosophy • As referral medicine becomes more advanced, it by default becomes more expensive • There is a growing gap between general practice and specialty practices • These seminars intend to fill that gap • Everything we talk about this weekend can be done in a rural mixed animal practice with no emergency clinic or specialists within a few hours • DISCLAIMER – I AM NOT A SPECIALIST

Practical Vet. Med Philosophy Our Goal for the Weekend: • Review common things in detail • Cover uncommon things in less detail – Recognize them and refer to the proceedings • Increase level of care at your clinic – And/or be better referring vets • Build relationships with your colleagues – Texas. Vets list – Rosemary Lindsey, moderator – rosemarylindsey@sbcglobal. net

Hank & Eli’s Fund – Dark Horse Lodge $3302 so far… • Hank & Eli’s Fund is a source of financial support for active duty service men and women, retired veterans’ service animals, and retired military animals with veterinary medical bills • There is a one page flyer in your packet • Letter from Colton’s mother on flash drive • Donation box on Dylan’s desk • give online: http: //www. hankandeli. com • Mail donations to address on flyer Free Power. Point Templates

Hank & Eli’s Fund Free Power. Point Templates

Hank & Eli’s Fund Southside Animal Hospital 6940 S Padre Island Dr Corpus Christi TX 78412 (361) 993 -7388 mmooremailforme@yahoo. com If you want a collection box for your clinic, contact Dr. Mike Moore Free Power. Point Templates


Signalment Age • Congenital disease – young • Myxomatous Valvular Disease – old • Exceptions – Cavalier King Charles Spaniels – mild PDA, PS, SAS – Reverse PDA – HCM in purebred cats

History - Collapse How can you tell the difference between seizure and syncope? – Urination/defecation/vocalization/paddling – Stiff/opisthotonus or flaccid • Narcolepsy, exercise induced collapse – Twitching and muscle fasciculations – Cyanosis, pallor – Abnormal behavior before and after – Duration of stiffness/opisthotonus Many times, you can’t (especially when short)

History - Collapse What causes syncope? 1. 2. 3. 4. 5. Bradyarrhythmia Period of asystole Tachyarrhythmia Obstruction of blood flow to or from the heart Inability to deliver oxygen to the brain, especially when there is increased demand • Decreased CO - Heart Failure** • Lung/airway disease • Anemia or other RBC/Hb problem

History - Collapse What causes syncope? – Bradyarrhythmia • 3 rd degree heart block • Sick sinus syndrome (define) – Period of asystole • Sick sinus syndrome (SSS) • Vagal surge (examples) – Abdominal dz & retching – Intubation (brachycephalic)
History - Collapse What causes syncope? – Tachyarrhythmia burst • Vtach (define, causes) – Boxer Cardio. Myopathy – Myocarditis (Chagas, Parvovirus) – Myocardial hypoxia – Abdominal pathology (spleen) • Supraventricular tachycardia (SVT) (define) • Re-entry pathway (define) • Atrial fibrillation (Afib) • SSS

History - Collapse What causes syncope? – Obstruction of a great vessel or heart chamber • Thrombus (clot or HWDz) • Neoplasia • Extramural mass – Increased oxygen demand can not be met due to severe cardiovascular or pulmonary disease • AKA Exercise intolerance

History - Cough How can you tell the difference between cardiac and respiratory cough/dyspnea? – Honking cough, soft moist cough, dry hacking cough – Coughing/gagging up white foamy fluid, acting like something caught in the throat – Coughing up blood tinged fluid – Cough when drinking water, on tracheal palpation, or exercise induced cough – Presence of a murmur (big dog, little dog, cat) Many times, you can’t without PE/diagnostics

History - Cough on tracheal palpation – Any dog or cat will cough a few times on vigorous tracheal palpation – Prolonged coughing after tracheal palpation often indicates pathology (cardio or resp? ) • equally likely with airway disease and cardiovascular disease

History - Cough Dogs vs Cats – Coughing cats • much more likely to have respiratory disease than heart failure • Cats with heart failure more often present with acute and severe dyspnea, with no cough • Some cat owners can find it difficult to distinguish vomiting, gagging and coughing – Coughing dogs can have either or both

Exam – Stethoscopes • • Ear pieces fit snugly in the ears Angle fits your ear canals Poor fit, and you’ll miss low intensity murmurs Tubing longer than 18 inches will dampen sounds Electronic stethoscopes (microphone based) • Difficult to distinguish heart from lung sounds • Difficult to distinguish patient from background noise • Meditron sensor based scope eliminates problems – Connect to computer & record for PCG consult

Exam – Stethoscopes Pediatric stethoscope (infant & pediatric sizes) • For cats and small dogs • Will distort and decrease sound intensity if used on a medium or large dog Adult stethoscope • For medium to large dogs • Won’t localize murmurs properly in cats and small dogs

Exam – Stethoscopes Cardiology Stethoscope - Diaphragm • Filters out low frequency sounds to hear high frequency sounds better • Press firmly against the chest Bell • For low frequency sounds (S 3 S 4 in dogs) • Press gently against the chest

Auscultation Minimizing patient noise • Panting, whining – close mouth, occlude nostrils • Purring ( audio ) – – Aversives – turn water on, show another animal Gentle pressure on the larynx Cotton ball with alcohol to the nose Jiggle the doorknob • Sometimes sedation is needed (chart) – Acepromazine 0. 0125 -0. 025 mg/lb, maximum 1 mg per dog – Butorphanol 0. 1 mg/lb or buprenorphine 0. 01 -0. 02 mg/kg – IV the fastest and most profound (30 -45 minutes)
Auscultation • Patient is standing in a quiet place – R Lateral recumbency and listen from bottom if muffled • Firm pressure with the diaphragm to avoid hair noises • get comfortable ausculting heart and palpating pulses at the same time • Listen at least 5 min for cardiac patients – Heart - R and L apex, L bases – L armpit (30 sec+ each) – Lungs – RCr, RMid, RDCd, LCr, LMid, LDCd (20 sec+ each)

Auscultation • Is the murmur hemodynamically significant? – Prolonged and loud - yes – Pansystolic - yes – Diastolic - yes – Low intensity - maybe – Early systolic - maybe – Musical – maybe not so much Loudness is not necessarily correlated to presence of heart failure

Auscultation – Lung Sounds • Snaps crackles and wheezes (cardio or resp? ) – More likely respiratory in dogs (audio) – Not very sensitive for pulmonary edema – Beware similar hair rubbing noises • Pleural/pericardial Rubs (pleural rubs) (pericardial rubs) • Dull/absent lung sounds (dog vs cat) (causes) – Lung consolidation – Pneumothorax, pleural effusion (TFAST®) • Harsh lung sounds with no murmur in cat – think asthma or heartworm disease (audio)
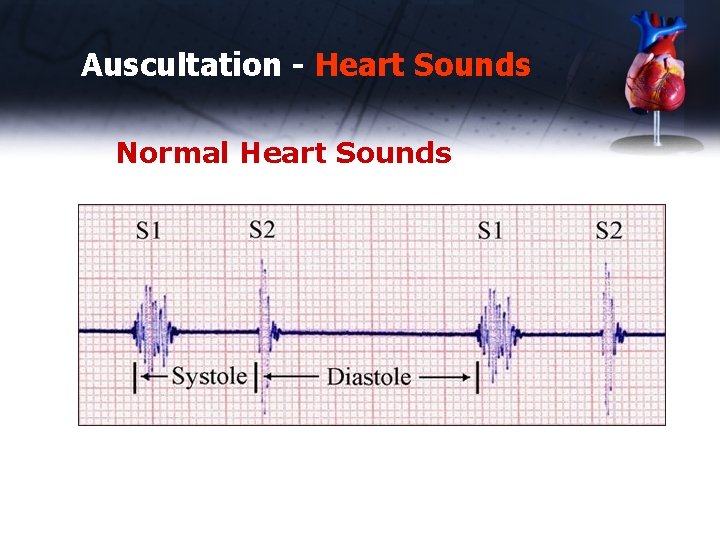
Auscultation - Heart Sounds Normal Heart Sounds
Auscultation - Heart Sounds Normal Heart Sounds • S 1 – AV Valves close – Beginning of systole/End of diastole • S 2 – Semilunar valves close – beginning of diastole/End of systole • Tachycardia – which is which? – S 2 shorter and higher frequency • Pulse is during systole (audio)
Auscultation - Heart Sounds • Variable intensity S 1 – Arrhythmia (variable FS) • Louder S 1 (AV slamming) – Young, narrow chested dogs (Doberman) – Increased sympathetic tone – Anemia (decreased blood viscosity) – Fever – Hypertension – Advanced mitral valve disease
Auscultation - Heart Sounds • Louder S 2 (SL slamming) – Hyperthyroidism – Fever, anemia – Heartworm Disease – Cor pulmonale (define) • Quieter S 1 -S 2 (SL softly closing) – Myocardial failure (DCM, severe MR) – Obesity, barrel chested
Auscultation - Heart Sounds Third Heart Sound (Gallop) S 3 (S 1 -S 2 -S 3) S 4 (S 4 -S 1 -S 2) Split S 2 Systolic Click Summation Gallop (S 4 -S 1 -S 2 -S 3)
Auscultation - Heart Sounds Third Heart Sound • Split S 2 – PMI right heart base (left side) – Ao. V PV don’t close at same time (PV later) – Reverse PDA – Pulmonary hypertension (HWDz, COPD) – Severe RBBB – relative PS of right to left shunts (ASD) – normal variation in large dogs (audio)
Auscultation - Heart Sounds Third Heart Sound Systolic Click – Very sharp, high frequency click of Mitral valve prolapse, in early MVD • Snapping of the chordae tendinae as they go taught – PMI left apex – Mid-Systolic (audio) – May be accompanied by a systolic murmur • Early, late, or holosystolic (audio) – Often years until CHF develops, if at all
3 Heart Sounds How Can you tell the difference? Does it Matter? – Systolic less likely pathogenic (S 1 -S 2 -S 3) – Systolic Click sounds sharper – Diastolic more likely pathogenic (PMI L base) (S 4 -S 3 -S 1) How Can you tell if S 3 or S 4? – Can’t tell if heart rate is > 160 -180 (summation) – just do a cardio work-up
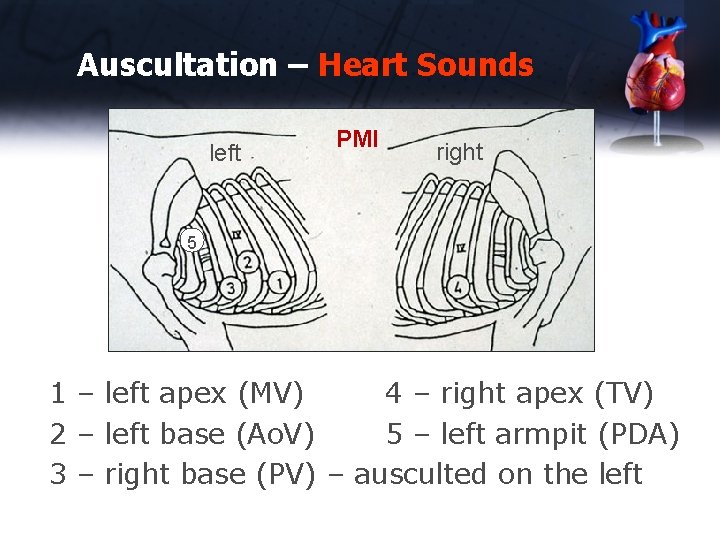
Auscultation – Heart Sounds left PMI right 5 1 – left apex (MV) 4 – right apex (TV) 2 – left base (Ao. V) 5 – left armpit (PDA) 3 – right base (PV) – ausculted on the left
Auscultation – Heart Sounds PMI (Point of Maximal Intensity) Left Apex – at palpable apical beat – S 1 - MR (mild MR) (severe MR) Left Base – slide cranially & a little dorsally – S 2 - SAS (audio) – S 1, S 2 - Ao endocarditis (audio) Right Base (left side) – S 2 - PS (mild PS) (severe PS) Left Axilla – continuous - PDA (PDA) (severe PDA) Right Apex – S 1 – TR – like MR but often quieter (audio)
Auscultation – Heart Sounds Muffled Heart Sounds (causes) effusion (*difference*) • Pleural, Pericardial • Diaphragmatic hernia, thoracic masses • Obesity What besides cardiac disease can cause a pathologic murmur? • Anemia • hypoproteinemia

Auscultation – Heart Sounds Why do puppies have innocent murmurs? • Musical, grade 1 -2, short (audio) (mild MR) • Larger SV relative to great vessel size • Lower PCV and plasma proteins • Artifact – high frequency breath sounds • They tend to be musical and relatively quiet

Auscultation – Heart Sounds Why do cats have innocent murmurs? • Short systolic murmur at the sternum (audio) • Not pansystolic and usually not holosystolic • Sympathetic tone episodic hypertension, increased SV • Can come and go during a vet visit

Auscultation – Murmur Grade 1 • Heard in a very quiet room, concentrating Grade 2 • easily heard on the PMI - focal Grade 3 • Moderately loud Grade 4 • Very loud over much of the chest Grade 5 • Heard with edge of stethoscope on chest, palpable thrill Grade 6 • Heard with stethoscope off chest, palpable thrill

Auscultation – Murmur Grade High grade murmurs are more likely to be associated with severe disease Severe disease can also be present with low grade murmur • Occasionally no auscultable murmur in the cat (dog? ) • DCM • ASD • VSD • Reverse PDA (right to left shunting) Dogs almost never have CHF without a murmur Cats can have CHF without a murmur
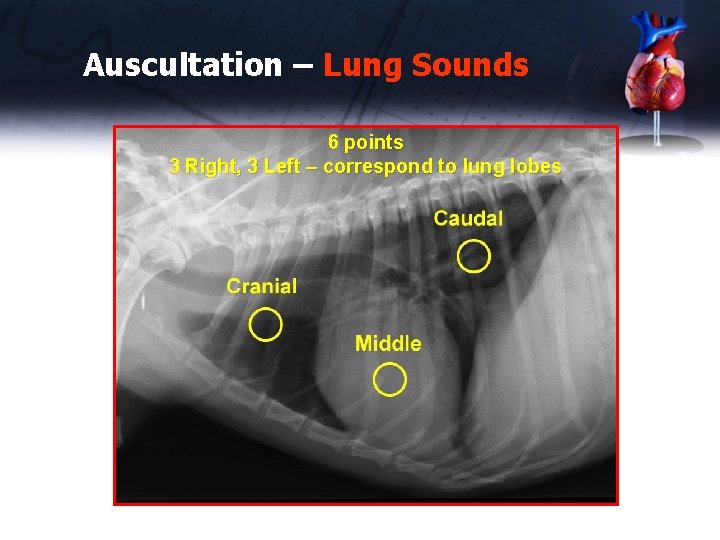
Auscultation – Lung Sounds 6 points 3 Right, 3 Left – correspond to lung lobes
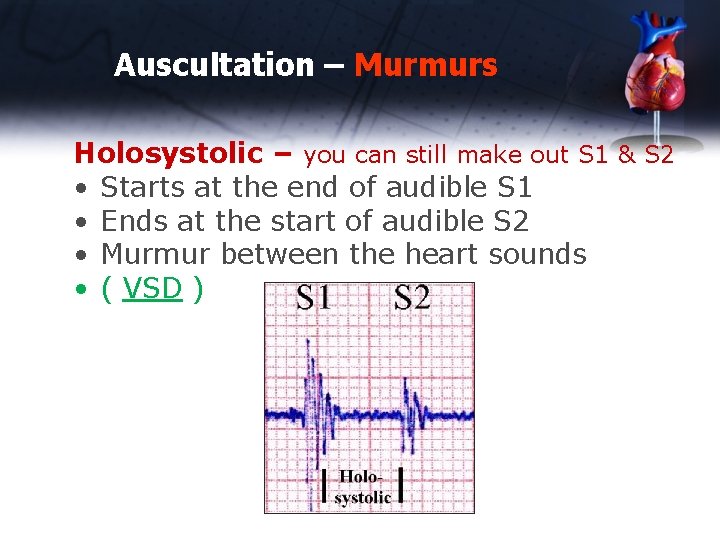
Auscultation – Murmurs Holosystolic – you can still make out S 1 & S 2 • Starts at the end of audible S 1 • Ends at the start of audible S 2 • Murmur between the heart sounds • ( VSD )
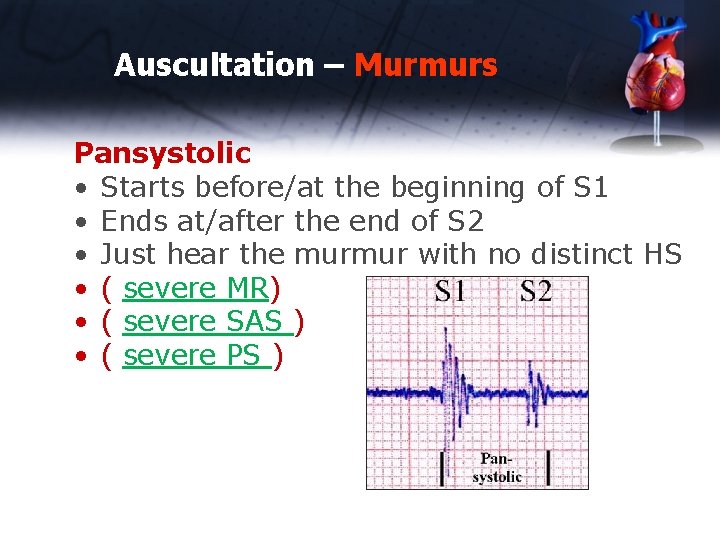
Auscultation – Murmurs Pansystolic • Starts before/at the beginning of S 1 • Ends at/after the end of S 2 • Just hear the murmur with no distinct HS • ( severe MR) • ( severe SAS ) • ( severe PS )

Respiratory Sinus Arrhythmia • Heart rate increases during respiration Due to increased vagal tone • Normal variation in dogs (not cats) • No pulse deficits • If present, heart failure is not likely – Increased sympathetic tone overrides • Pronounced in disease processes of increased vagal tone – Increased CSF pressure – Chronic respiratory disease – Thoracic or abdominal disease – After sedation

Respiratory Sinus Arrhythmia • DDx – Afib with a normal ventricular rate – Frequent APCs or VPCs (maybe pulse deficits) – Intermittent SSS None of these vary consistently with the respiratory cycle • RSA is regularly irregular • Others are usually irregular (RSA) (PS with RSA)

Physical Exam – Ascites • most common cause of cardiogenic ascites in cats – TVD > VSD • Tap and do fluid analysis to distinguish between transudate, modified transudate and exudate (handout) • Usually accumulates slowly, though owners often don’t notice until huge • If truly does develop over days, think pericardial tamponade or caval syndrome

Exam – Mucous Membranes Cyanosis • > 4 g/d. L of deoxygenated Hb in the blood – Severely anemic animals don’t turn blue – Even with life threatening hypoxia • Differential cyanosis (define) – Front of body pink, back of body blue – Reverse PDA, FATE (why r. PDA) – Compare pulse oximetry or blood gases from front of body with rear of body – Weak or no femoral pulses, pain, paresis with FATE • USE YOUR COLOR DOPPLER!!!

Exam – Pulses Technique • Occlude the pulse • Then slowly release pressure until maximum pulse is detected Pulse Pressure = Systolic – Diastolic • Femoral pulse usually not palpable when MAP <50 mm. Hg • Dorsal pedal pulse not palpable when SAP <80 mm. Hg
Exam – Pulses Bounding Pulses (water hammer) • Increased systolic pressure (increased SV) – – – (causes) Aortic regurgitation Severe bradycardia Thyrotoxicosis (define EF, FS) Fever Anemia/hypoproteinemia • decreased diastolic pressure (diastolic runoff) – PDA – AV fistula – Aortic regurgitation (most common cause) • Aortic endocarditis > SAS
Exam – Pulses Weak Pulses • Severely decreased SV – severe forward LHF • Acutely decreased SV – hypovolemia • Decreased peripheral vascular resistance (shock) • Decreased arterial compliance (hypertension) Pulse peaks slowly and late in systole (feel the squirt) • Pulsus parvus et tardus (cause) • Severe SAS

Exam – Pulses Short, Brisk Pulses (snappy) • Short, fast systole • Compensated MR (what happens to FS with MR) Pulse weak or absent during inspiration • Pulsus paradoxus • Systolic pressure falls during inspiration • With pronounced respiratory sinus arrhythmia • Exaggerated by pericardial effusion
Exam – Pulses Alternating Weak and Normal Pulses • Pulsus alternans • Severe myocardial failure (define MF vs CHF) (causes) – DCM – RCM, UCM (define) – End stage valvular disease – Prolonged tachyarrhythmia or tachycardia
Exam – Pulses Pulse Deficits (heart beat generates no pulse) • VPCs • Atrial fibrillation with VPCs • Tachyarrhythmia (inadequate filling) • Every other heart beat has a pulse deficit – Pulsus bigeminis – Caused by ventricular bigeminy (define) Totally chaotic heart sounds and pulses (audio) • Lots of multiform VPCs, Atrial fibrillation • Delirium cordis – like tennis shoes in a dryer

Exam – Jugular Veins • Clip or wet the fur over the jugular veins • Evaluate sitting or standing (not sternal) • Jugular Distension (causes) – suggests increased RA pressure (normal dogs cats? ) • 2 -3 cm H 20 in cats, 5 -8 cm H 20 in dogs – Or less often jugular or caval occlusion • Jugular Pulse (normal dogs cats) – 5 -8 cm dorsal to RA in dogs, 2 -3 cm in cats (1/3 way up) – Too high indicates increased right heart pressure • If abnormalities above noted, occlude at thoracic inlet, and release • Hepatojugular reflux

Exam – Jugular Veins Jugular distension, high pulse, +HJR • Jugular/caval occlusion (causes) – Heartworm disease – External mass (cyst, abscess, granuloma, neoplasia) – Thrombus (causes) • Decreased RV compliance – RV hypertrophy • PS, TOF, pulmonary hypertension – Restrictive CM – RVOT obstruction • Heartworm disease, neoplasia, thrombus

Exam – Jugular Veins Jugular distension, high pulse, +HJR • RV volume overload – TR with RHF – VSD – HWDz • Compression on the RV, so it can’t fill – Pericardial effusion – constrictive pericarditis – Pericardial mass Evaluation of Cd. VC, hepatic & splenic veins on US are more sensitive for increased RV pressure than jugular vein exam

Exam – Extremities Peripheral edema • rare • Often accompanied by diarrhea • Due to RHF, including end stage biventricular failure Cold extremities • Due to RHF and venous stasis • Or saddle thrombus – Acutely painful, followed by lack of pain ( Cardiovascular Exam form )

Summary Power. Points -. pptx, . pdfs – 1 or 6 slides per page Form – Cardiovascular Exam. docx, . pdf Vet Handouts • Sedation Doses and Echo Values by Weight • Fluid Analysis Diagnostic Chart Audio Files (29) – thoracic auscultation

Summary Hidden Slides • List of common cardiovascular diseases by breed • More Details on gallop murmurs • Quiet heart sounds

Acknowledgements Smith FWK, Keene BW, Tilley LP • Rapid Interpretation of Heart and Lung Sounds, 2 nd ed, 2006 Kvart C & Haggstrom J • Cardiac Auscultation and Phonocardiography, Veterinary Information Network Kittleson M • Small Animal cardiovascular Medicine, Veterinary Information Network. Chapter 3 – Signalment, History and Physical Examination
- Slides: 74