Cardiometabolic Risk Faculty of Medicine Universitas Brawijaya Malang

Cardiometabolic Risk Faculty of Medicine Universitas Brawijaya Malang

§ A comprehensive approach to patient care; Multiple disease pathways and risk factors are considered to facilitate earlier intervention § Early assessment and targeted intervention are needed to treat and prevent all risk factors associated with CVD and diabetes

§ Gives a comprehensive picture of a patient’s health and potential risk for future disease and complications § Is inclusive of all risks related to metabolic changes associated with CVD § Accommodates emerging risk factors as useful predictive tools § Focuses clinical attention to the value of systematic evaluation, education, disease prevention and treatment § Supports an integrated approach to care Kahn, et al. The Metabolic Syndrome: Time for a Critical Appraisal: Joint Statement From the American Diabetes Association and the European Association for the Study of Diabetes Care. 2005; 28 (9)2289 -2304.

§ 2 out of 3 Americans are overweight or obese § More than 70 million (nearly 1 in 4) Americans have varying degrees of insulin resistance § There an estimated 54 million (more than 1 in 6) Americans with prediabetes § Nearly 1 in 4 U. S. adults has high cholesterol § 1 in 3 American adults has high blood pressure
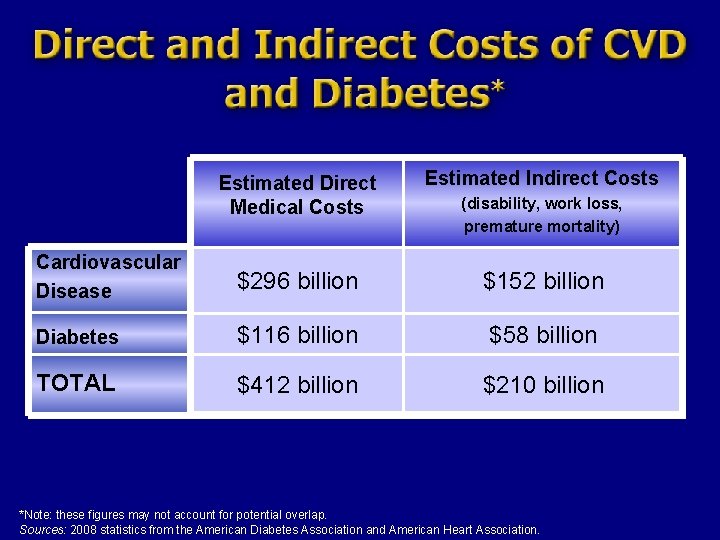
Direct and Indirect Cost of CVD and Diabetes Estimated Direct Medical Costs Estimated Indirect Costs Cardiovascular Disease $296 billion $152 billion Diabetes $116 billion $58 billion TOTAL $412 billion $210 billion (disability, work loss, premature mortality) *Note: these figures may not account for potential overlap. Sources: 2008 statistics from the American Diabetes Association and American Heart Association.
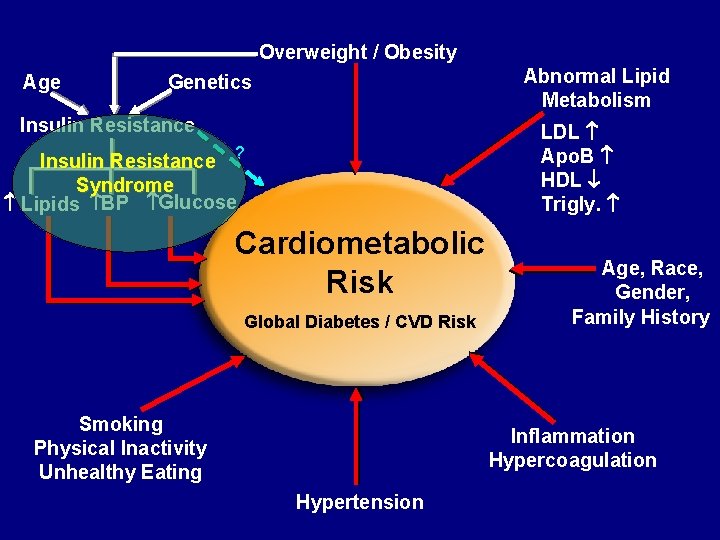
Overweight / Obesity Age Abnormal Lipid Metabolism Genetics Insulin Resistance LDL Apo. B HDL Trigly. Insulin Resistance ? Syndrome Lipids BP Glucose Cardiometabolic Risk Global Diabetes / CVD Risk Smoking Physical Inactivity Unhealthy Eating Age, Race, Gender, Family History Inflammation Hypercoagulation Hypertension

Non-modifiable § § Age Race/ethnicity Gender Family history Modifiable § § § § Overweight Abnormal lipid metabolism Inflammation, hypercoagulation Hypertension Smoking Physical inactivity Unhealthy diet Insulin resistance

§ 47 -year-old African American man, hasn’t seen doctor in years § Works as a truck driver, eats mostly fast food § Smokes 1 pack per day § At health fair found to have BP = 146/86, total cholesterol = 210 § Weight = 230 lbs; BMI = 29 kg/m² § Family history of HTN and diabetes

§ § Age Race/ethnicity Gender Family history 47 African American Male HTN and diabetes § § § Overweight/obesity Abnormal lipid metab Hypertension Smoking Physical Inactivity Unhealthy diet BMI = 29 TC = 210 BP = 146/86 1 pack per day Yes Fast food diet

Number 800, 000 600, 000 400, 000 200, 000 0 20 -39 40 -59 Age Group 60+ Centers for Disease Control and Prevention. National diabetes fact sheet: general information and national estimates on diabetes in the United States, 2005. Atlanta, GA: U. S. Department of Health and Human Services, Centers for Disease Control and Prevention, 2005.
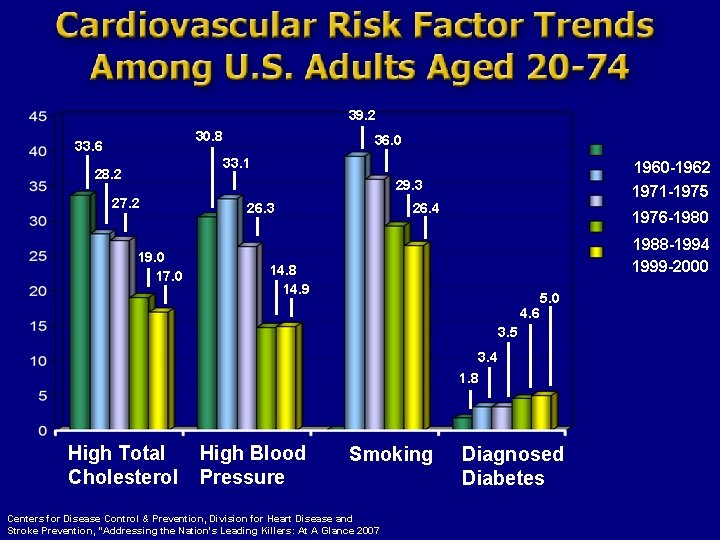
39. 2 30. 8 33. 6 36. 0 33. 1 28. 2 1960 -1962 29. 3 27. 2 19. 0 17. 0 26. 3 1971 -1975 26. 4 1976 -1980 1988 -1994 1999 -2000 14. 8 14. 9 4. 6 5. 0 3. 5 3. 4 1. 8 High Total Cholesterol High Blood Pressure Smoking Centers for Disease Control & Prevention, Division for Heart Disease and Stroke Prevention, "Addressing the Nation's Leading Killers: At A Glance 2007 Diagnosed Diabetes

American Indians/ Alaska Natives Non-Hispanic Blacks Hispanic/Latino Americans Non-Hispanic Whites 0 2 4 6 8 10 12 14 16 18 20 Centers for Disease Control and Prevention. National diabetes fact sheet: general information and national estimates on diabetes in the United States, 2005. Atlanta, GA: U. S. Department of Health and Human Services, Centers for Disease Control and Prevention, 2005.


• • Overweight/ fat distribution Age Genetic predisposition Activity level Medications Puberty Pregnancy

• Impaired Fasting Glucose (IFG): a condition in which the blood glucose level is between 100 mg/d. L to 125 mg/d. L after an 8 - to 12 -hour fast. • Impaired Glucose Tolerance (IGT): a condition in which the blood glucose level is between 140 and 199 mg/d. L at 2 hours during an oral glucose tolerance test (OGTT).
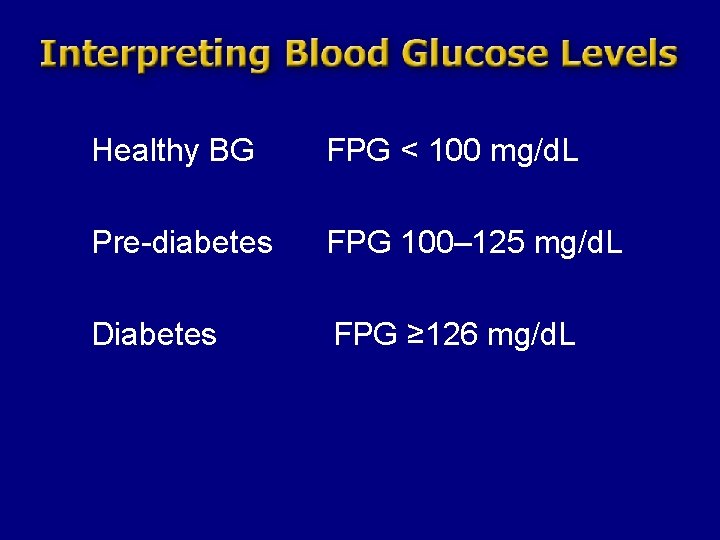

Healthy BG FPG < 100 mg/d. L Pre-diabetes FPG 100– 125 mg/d. L Diabetes FPG ≥ 126 mg/d. L

§ Overweight (BMI > 85 th percentile for age and sex, weight for height > 85 th percentile, or weight § >120 percent of ideal for height) Plus any two of the following: • Family history • Race/ethnicity • Signs of insulin resistance or conditions associated with insulin resistance • Maternal history of diabetes or GDM

1. Testing should be considered in all overweight adults (BMI ≥ 25 kg/m 2*) and have additional risk factors: § Physical inactivity § First-degree relative with diabetes § Members of a high-risk ethnic population § Women delivering baby weighing >9 lb or were diagnosed with GDM § Hypertension (≥ 140/90 mm. Hg) Continued

§ § § HDL cholesterol level <35 mg/dl (0. 90 mmol/l) and/or a triglyceride level >250 mg/dl (2. 82 mmol/l) Women with polycystic ovarian syndrome (PCOS) IGT or IFG on previous testing Other clinical conditions associated with insulin resistance (e. g. , severe obesity and acanthosis nigricans) History of CVD

2. In the absence of the above criteria, testing for prediabetes and diabetes should begin at age 45 years 3. If results are normal, testing should be repeated at least at 3 -year intervals, with consideration of more frequent testing depending on initial results and risk status. *At-risk BMI may be lower in some ethnic groups.
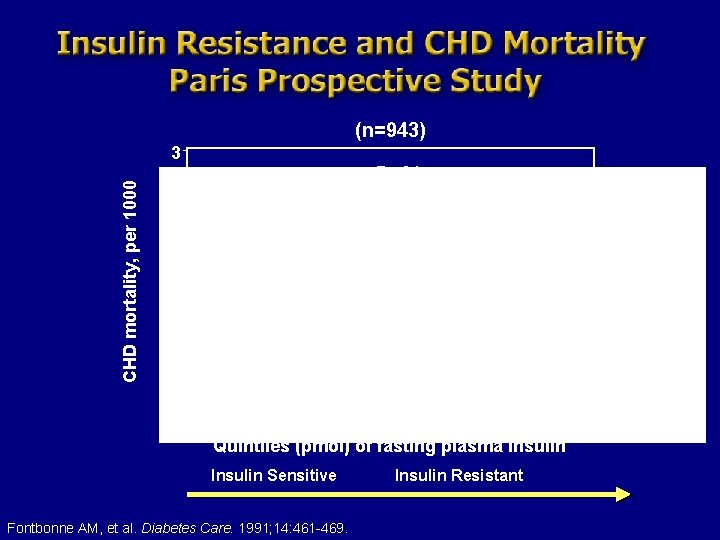
(n=943) CHD mortality, per 1000 3 P<. 01 2 1 0 29 30 -50 51 -72 73 -114 115 Quintiles (pmol) of fasting plasma insulin Insulin Sensitive Fontbonne AM, et al. Diabetes Care. 1991; 14: 461 -469. Insulin Resistant
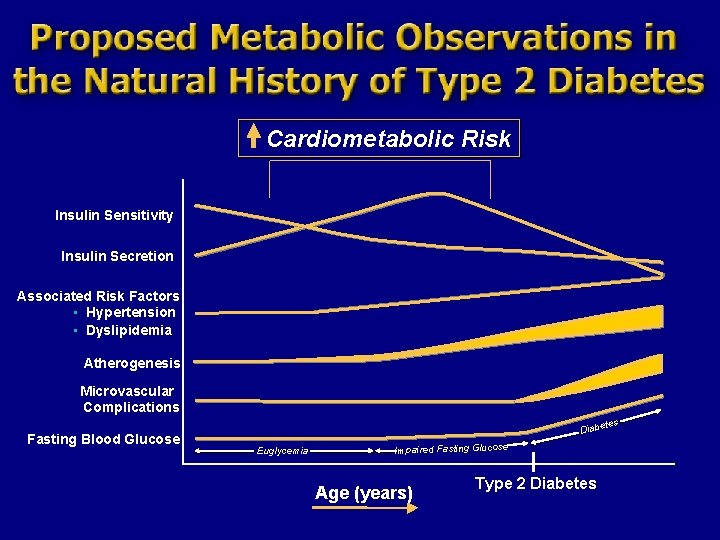
Cardiometabolic Risk Insulin Sensitivity Insulin Secretion Associated Risk Factors • Hypertension • Dyslipidemia Atherogenesis Microvascular Complications tes Fasting Blood Glucose Diabe Euglycemia Impaired Fasting Glucose Age (years) Type 2 Diabetes

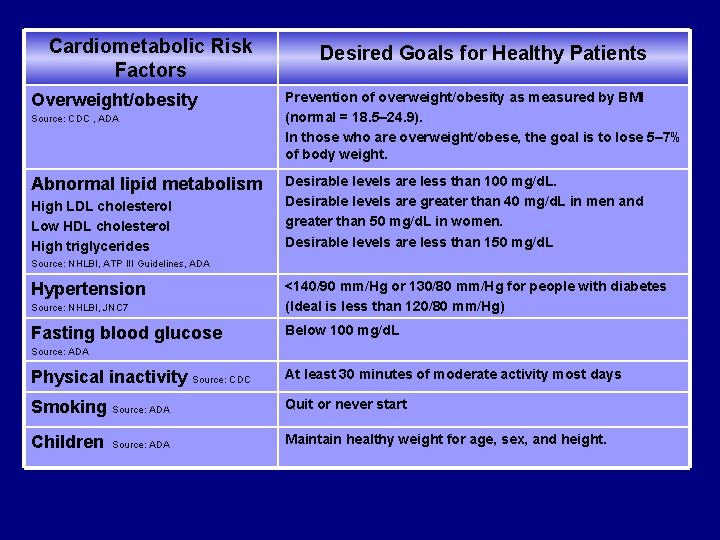
Cardiometabolic Risk Factors Overweight/obesity Source: CDC , ADA Abnormal lipid metabolism High LDL cholesterol Low HDL cholesterol High triglycerides Desired Goals for Healthy Patients Prevention of overweight/obesity as measured by BMI (normal = 18. 5– 24. 9). In those who are overweight/obese, the goal is to lose 5– 7% of body weight. Desirable levels are less than 100 mg/d. L. Desirable levels are greater than 40 mg/d. L in men and greater than 50 mg/d. L in women. Desirable levels are less than 150 mg/d. L Source: NHLBI, ATP III Guidelines, ADA Source: NHLBI, JNC 7 <140/90 mm/Hg or 130/80 mm/Hg for people with diabetes (Ideal is less than 120/80 mm/Hg) Fasting blood glucose Below 100 mg/d. L Hypertension Source: ADA Physical inactivity Source: CDC At least 30 minutes of moderate activity most days Smoking Source: ADA Quit or never start Children Source: ADA Maintain healthy weight for age, sex, and height.

§ § Measure BMI routinely at each regular check-up. Classifications: • BMI 18. 5 -24. 9 = normal • BMI 25 -29. 9 = overweight • BMI 30 -39. 9 = obesity • BMI ≥ 40 = extreme obesity Clinical Guidelines on the Identification, Evaluation, and Treatment of Overweight and Obesity in Adults: The Evidence Report. NIH Publication # 98 -4083, September 1998, National Institutes of Health.

§ Large waist circumference (WC) can identify some at increased risk over BMI alone § If BMI and other cardiometabolic risk factors are assessed, currently there is insufficient evidence to: – Substitute WC for BMI – Measure WC in addition to BMI Klein, et al. Waist Circumference and Cardiometabolic Risk. Diabetes Care. 2007 0: dc 07 -9921 v 1 -0.

Primary Metabolic Disturbance Intermediate Vascular Disease Risk Factor Intravascular Pathology Clinical Event Insulin Resistance Hypertension Dyslipidemia Hyperglycemia Overnutrition Hyperinsulinemia Inflammation Atherosclerosis • • • Coronary arteries Carotid arteries Cerebral arteries Aorta Peripheral arteries CVD Hypercoagulability Impaired Fibrinolysis Endothelial Dysfunction Despres JP, et al. Abdominal obesity and metabolic syndrome. Nature. 2006; 444: 881 -887. CVD: Cardiovascular disease
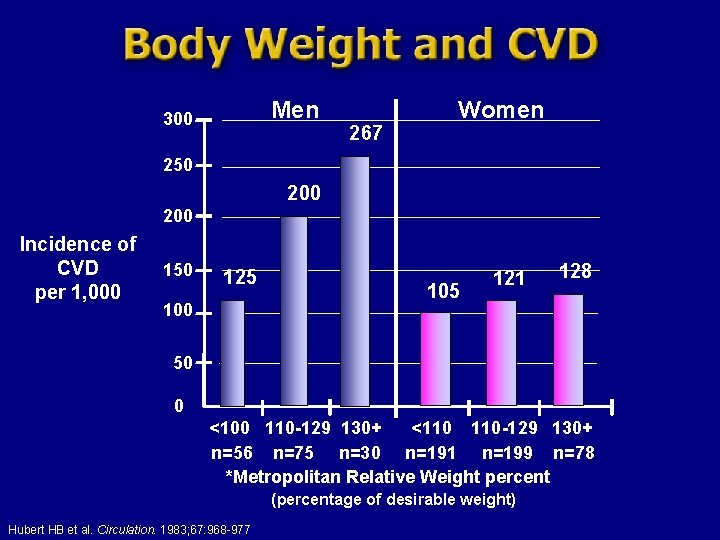
Men 300 267 Women 250 200 Incidence of CVD per 1, 000 150 125 100 105 121 128 50 0 <100 110 -129 130+ <110 110 -129 130+ n=56 n=75 n=30 n=191 n=199 n=78 *Metropolitan Relative Weight percent (percentage of desirable weight) Hubert HB et al. Circulation. 1983; 67: 968 -977

§ Lifestyle modification • Reduce caloric intake by 500 -1000 kcal/day (depending on starting weight) • Target 1 -2 pound/week weight loss • Increase physical activity • Healthy diet • Diabetes Prevention Program • DASH diet Clinical Guidelines on the Identification, Evaluation, and Treatment of Overweight and Obesity in Adults: The Evidence Report. NIH Publication # 98 -4083, September 1998, National Institutes of Health. Diabetes Prevention Program (DPP) Diabetes Care 25: 2165– 2171, 2002. The Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure, NIH Publication No. 04 -5230, August 2004

§ § Consider pharmacologic treatment • BMI 30 with no related risk factors or diseases, or • BMI 27 with related risk factors or diseases • As part of a comprehensive weight loss program incl. diet & physical activity Consider surgery • BMI 40 or • BMI 35 with comorbid conditions Clinical Guidelines on the Identification, Evaluation, and Treatment of Overweight and Obesity in Adults: The Evidence Report. NIH Publication # 98 -4083, September 1998, National Institutes of Health. Diabetes Prevention Program (DPP) Diabetes Care 25: 2165– 2171, 2002


• Desirable — Less than 200 mg/d. L • Borderline high risk — 200– 239 mg/d. L • High risk — 240 mg/d. L and over American Diabetes Association. Understanding Cardiometabolic Risk: Broadening Risk Assessment and Management, Dyslipidemia Richard M Bergenstal, MD International Diabetes Center

Increased: Decreased: é Triglycerides é VLDL é LDL and small dense LDL é Apo. B ê HDL ê Apo A-I American Diabetes Association. Diabetes Care. 2007; 30: S 4 -41.

• Cigarette smoking • Hypertension (≥ 140/90 mm Hg or on antihypertensive medication) • Low HDL-C (<40 mg/d. L) • Family history of early heart disease • Age (men ≥ 45 years; women ≥ 55 years)

§ Statins (also called HMG-Co. A reductase inhibitors) work by increasing hepatic LDL-C removal from the blood. § Resins (also called bile acid sequestrants) bind to bile acids in the intestines and prevent their reabsorption, leading to increased hepatic LDL-C removal from the blood. § Cholesterol absorption inhibitors help lower LDL-C by reducing the amount of cholesterol absorbed in the intestines; increases LDL receptor activity.

§ Fibrates (also called fibric acid derivatives) activate an enzyme that speeds the breakdown of triglyceriderich lipoproteins while also increasing HDL-C. § Niacin (also called nicotinic acid) reduces the liver’s ability to produce VLDL. When given at high doses, it can also increase HDL-C. American Diabetes Association. Understanding Cardiometabolic risk: Broadening risk Assessment and Management, Dyslipidemia Richard M Bergenstal, MD International Diabetes Center

§ For patients >20 years of age, cholesterol should be checked every 5 years § Ordering a fasting lipid panel is preferred to gauge the patient’s total cholesterol, LDL-C, HDL-C and triglycerides § Treatment priorities

LDL-C-lowering Category of risk LDL-C Goal 0 -1 risk factor* < 160 mg/d. L or lower Multiple (2+) risk factors* < 130 mg/d. L or lower People with coronary heart < 100 mg/d. L or lower disease or risk equivalent (e. g. , diabetes) < 70 mg/d. L or lower Known CAD and DM may be ideal

§ § § Improve glucose control if diabetes is present Weight loss if overweight Daily exercise Smoking cessation Dietary modifications including low saturated fat (fat intake less than 30% of total calories and saturated fat less than 7% of total calories), low cholesterol (no more than 200 mg daily) diet § Pharmacologic treatment frequently necessary § Risk factors include hypertension; HDL < 40; family history of MI before age 55; male > 45 years old; female > 55 years old; smoking.
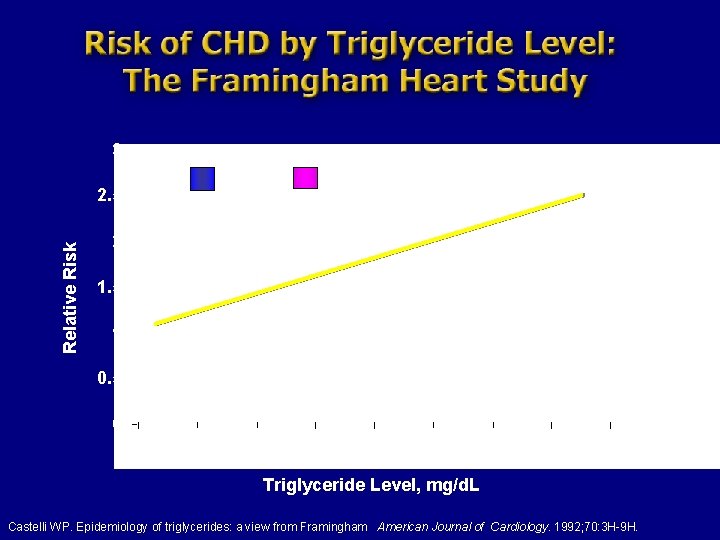
3 2. 5 Relative Risk Women Men n=5, 127 2 1. 5 1 0. 5 0 50 100 150 200 250 300 350 400 Triglyceride Level, mg/d. L Castelli WP. Epidemiology of triglycerides: a view from Framingham American Journal of Cardiology. 1992; 70: 3 H-9 H.
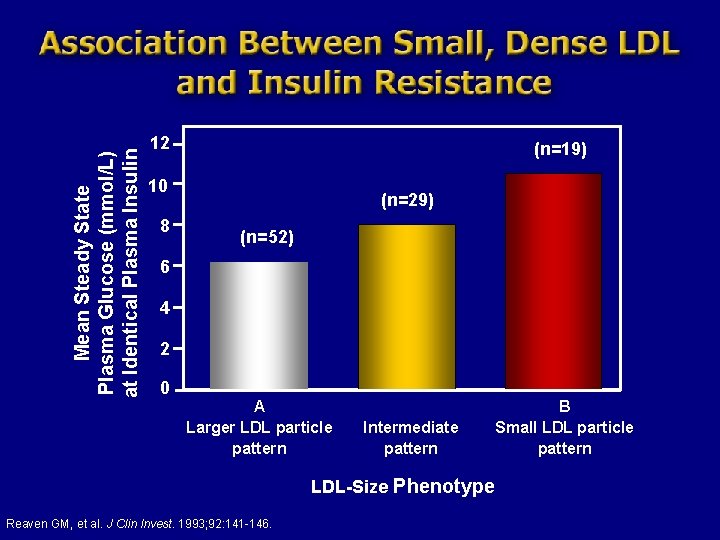
Mean Steady State Plasma Glucose (mmol/L) at Identical Plasma Insulin 12 (n=19) 10 8 (n=29) (n=52) 6 4 2 0 A Larger LDL particle pattern Intermediate pattern B Small LDL particle pattern LDL-Size Phenotype Reaven GM, et al. J Clin Invest. 1993; 92: 141 -146.

Risk of CHD ) g L /d C LD H (m LDL-C (mg/d. L) Gordon T, Castelli WP, Hjortland MC, Kannel WB, Dawber TR. High density lipoprotein as a protective factor against coronary heart disease. The Framingham Study. American Journal of Medicine. 1977; 62: 707 -14.

Persons without Diabetes § Test at least every 5 years, starting at age 20, including adults with low-risk values Persons with Diabetes § § In adults, test at least annually Lipoproteins: measure at after initial blood glucose control is achieved as hyperglycemia may alter results Preventing Cancer, Cardiovascular Disease, and Diabetes: A Common Agenda for The American Cancer Society, the American Diabetes Association, and the American Heart Association. Circulation. 2004; 109: 3244 -3255. American Diabetes Association. Standards of Medical Care in Diabetes 2007. Available at: http: //care. diabetesjournals. org/cgi/reprint/30/suppl_1/S 4
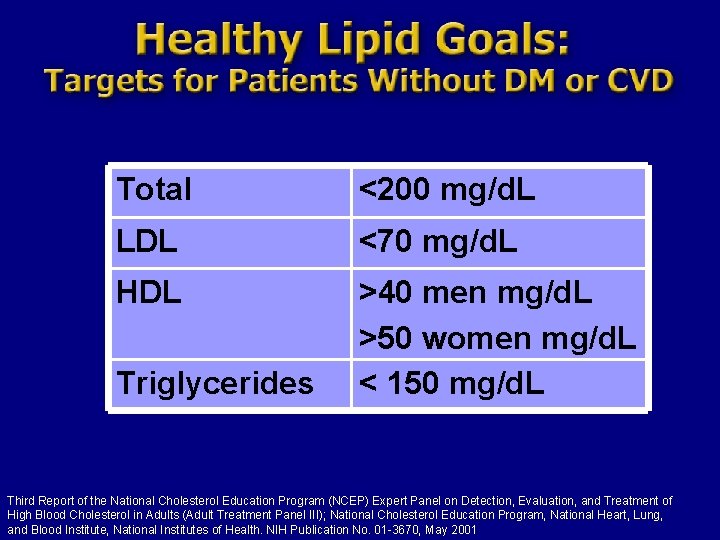

Total <200 mg/d. L LDL <70 mg/d. L HDL >40 men mg/d. L >50 women mg/d. L < 150 mg/d. L Triglycerides Third Report of the National Cholesterol Education Program (NCEP) Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults (Adult Treatment Panel III); National Cholesterol Education Program, National Heart, Lung, and Blood Institute, National Institutes of Health. NIH Publication No. 01 -3670, May 2001

§ Lifestyle modification • Increased physical activity • Diet: reduced saturated fat, trans fat, • and cholesterol Weight loss, if indicated American Diabetes Association. Diabetes Care. 2007; 30: S 4 -41.

§ Pharmacologic treatment: primary goal is LDL lowering • Without overt CVD: If over 40, statin therapy recommended to achieve 30 -40% LDL reduction • With overt CVD: All patients should receive statin therapy to achieve 30 -40% LDL reduction • Lowering triglycerides and raising HDL with a fibrate is associated with fewer cardiovascular events in patients with clinical CVD, low HDL, and near-normal LDL American Diabetes Association. Diabetes Care. 2007; 30: S 4 -41.


Persons without Diabetes § BP should be measured at each regular visit or at least once every 2 years if BP <120/80 mm. Hg § BP measured seated after 5 min rest in office Persons with Diabetes § BP should be measured at each regular visit § BP measured seated after 5 min rest in office § Patients with ≥ 130 or ≥ 80 mm. Hg should have BP confirmed on a separate day Preventing Cancer, Cardiovascular Disease, and Diabetes A Common Agenda for the American Cancer Society, the American Diabetes Association, and the American Heart Association. Circulation. 2004; 109: 3244 -3255. American Diabetes Association. Diabetes Care. 2007; 30: S 4 -41.

Non-pharmacologic § DASH diet • Dietary Approaches to Stop Hypertension • High in whole grains, fruits, vegetables, and low-fat dairy • Low in saturated and trans fat, cholesterol § Physical Activity § Weight loss, if applicable The Dash Diet. http: //dashdiet. org. American Diabetes Association. Diabetes Care. 2007; 30: S 4 -41.

Pharmacologic § Drug therapy indicated if BP ≥ 140/ ≥ 90 mm Hg § Combination therapy often necessary § Treatment should include ACE or ARB § Thiazide diuretic may be added to reach goals § Monitor renal function and serum potassium The Dash Diet. http: //dashdiet. org. American Diabetes Association. Diabetes Care. 2007; 30: S 4 -41.

Microvascular § Renal disease § Autonomic neuropathy § Eye disease (glaucoma, retinopathy with potential blindness) Macrovascular § Cardiac disease § Cerebrovascular disease § Reduced survival and recovery rates from stroke § Peripheral vascular disease American Diabetes Association. Diabetes Care. 2007; 30: S 4 -41. .


§ 35% of coronary heart disease deaths in the US can be attributed to an inactive lifestyle* § Consistent exercise can reduce CVD risk* § Exercise, combined with healthy diet and weight loss, is proven to prevent/delay onset of type 2 diabetes * American Diabetes Association. Diabetes Care. 2007; 30: S 4 -41. Diabetes Prevention Program Diabetes Care 25: 2165– 2171, 2002.

Guidelines § Fit into daily routine § Aim for at least 150 minutes/week of moderate aerobic exercise § Start slowly and gradually build intensity § Wear a pedometer (10, 000 steps) § Encourage patients to take stairs, park further away or walk to another bus stop, etc. American Diabetes Association. Diabetes Care. 2007; 30: S 4 -41.

Benefits of Exercise § Increased insulin sensitivity § Improved lipid levels § Lower blood pressure § Weight control § Improved blood glucose control § Reduced risk of CVD § Prevent/delay onset of type 2 diabetes American Diabetes Association. Diabetes Care. 2007; 30: S 4 -41.

§ Peripheral neuropathy can cause loss of sensation in feet; educate about preventive care measures for foot protection § Pre-existing CVD can cause arrhythmias, myocardial ischemia, or infarction during exercise § In presence of PDR or severe NPDR, vigorous exercise or resistance training may be contraindicated because of risk of vitreous hemorrhage or retinal detachment American Diabetes Association. Diabetes Care. 2007; 30: S 4 -41.

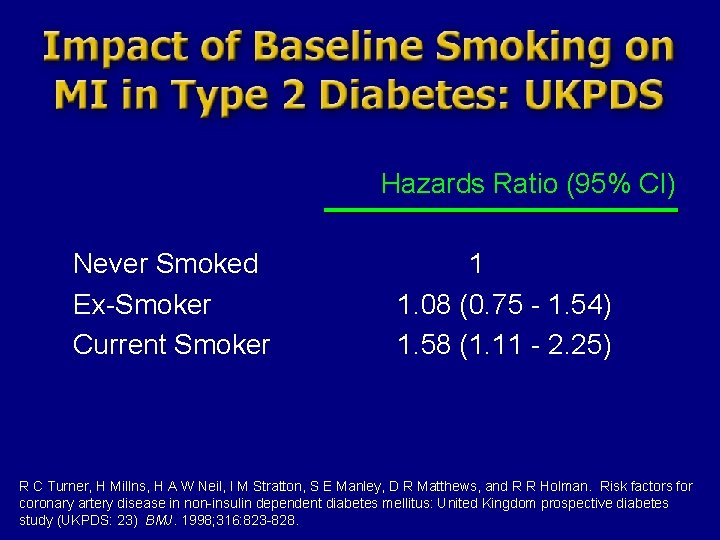
Hazards Ratio (95% CI) Never Smoked Ex-Smoker Current Smoker 1 1. 08 (0. 75 - 1. 54) 1. 58 (1. 11 - 2. 25) R C Turner, H Millns, H A W Neil, I M Stratton, S E Manley, D R Matthews, and R R Holman. Risk factors for coronary artery disease in non-insulin dependent diabetes mellitus: United Kingdom prospective diabetes study (UKPDS: 23) BMJ. 1998; 316: 823 -828.

§ § Obtain documentation of history of tobacco use Ask whether smoker is willing to quit – If no, initiate brief, motivational discussion regarding: • the need to stop using tobacco • risks of continued use • encouragement to quit, as well as support when ready – If yes, assess preference for and initiate either minimal, brief, or intensive cessation counseling. American Diabetes Association. Diabetes Care. 2004; 27: S 74 -S 75 .

§ § Set a Plan Offer counseling and referrals Offer medication assistance Offer combined pharmacologic and behavioral intervention American Diabetes Association. Diabetes Care. 2004; 27: S 74 -S 75 .


§ Proinflammatory/prothrombotic factors underlie cardiometabolic risk § Inflammation is a major component of atherogenesis and other cardiometabolic problems § Obesity is associated with inflammation Ross R. Atherosclerosis: an inflammatory disease. N Engl J Med. 1999; 340: 115 -126. Ballantyne CH, Nambi V. Markers of inflammation and their clinical significance. Atherosclerosis suppl 2005; 6: 21 -9. Mc. Laughlin T et al. Differentiation between obesity and insulin resistance in the association with C-reactive protein. Circulation.

§ High-sensitivity CRP tests may be used to further evaluate underlying risk Relative risk categories • Low risk <1 mg/L • Average risk 1 -3 mg/L • High risk >3 mg/L § § § Aspirin and statins reduce CRP levels Unclear whether CRP should be a treatment target Reduce weight Ross R. Atherosclerosis: an inflammatory disease. N Engl J Med. 1999; 340: 115 - 126. Ballantyne CH.


§ Pre-diabetes is an important risk factor future diabetes and cardiovascular disease § Recent studies have shown that lifestyle modification can reduce the rate of progression from pre-diabetes to diabetes American Diabetes Association, Diabetes Care. 2007: 30: S 4 -41. .
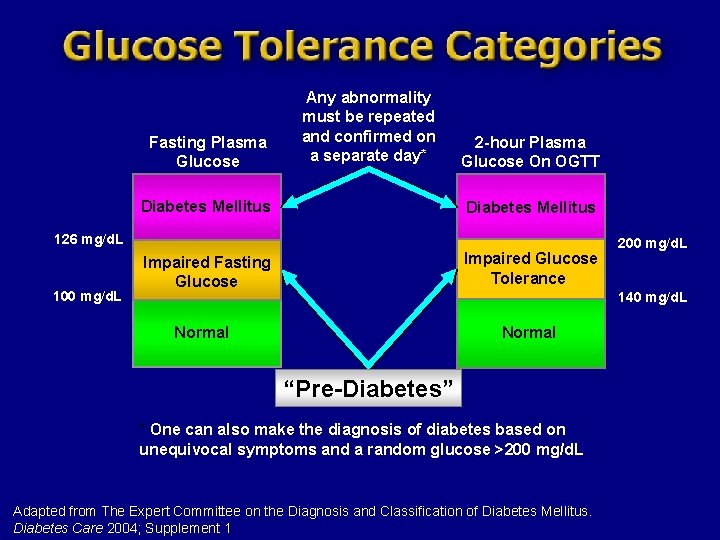
Fasting Plasma Glucose Any abnormality must be repeated and confirmed on a separate day* Diabetes Mellitus 2 -hour Plasma Glucose On OGTT Diabetes Mellitus 126 mg/d. L 100 mg/d. L Impaired Glucose Tolerance Impaired Fasting Glucose 200 mg/d. L 140 mg/d. L Normal “Pre-Diabetes” * One can also make the diagnosis of diabetes based on unequivocal symptoms and a random glucose >200 mg/d. L Adapted from The Expert Committee on the Diagnosis and Classification of Diabetes Mellitus. Diabetes Care 2004; Supplement 1

Results: § Treat IFG and IGT with aggressive lifestyle modification § For certain patients with both IFG and IGT consider metformin Nathan D, et al. Impaired Fasting Glucose and Impaired Glucose Tolerance: Implications for Care. Diabetes Care. 2007 30: 753 -759.
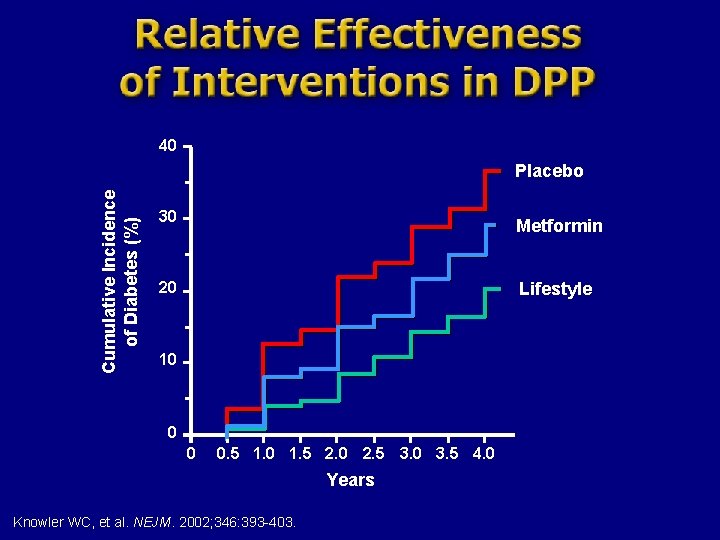
40 Cumulative Incidence of Diabetes (%) Placebo 30 Metformin 20 Lifestyle 10 0 0 0. 5 1. 0 1. 5 2. 0 2. 5 3. 0 3. 5 4. 0 Years Knowler WC, et al. NEJM. 2002; 346: 393 -403.
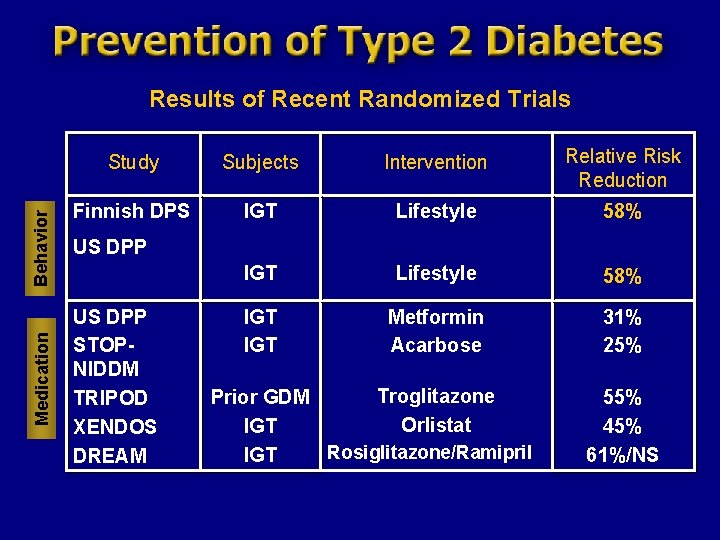
Medication Behavior Results of Recent Randomized Trials Study Subjects Intervention Relative Risk Reduction Finnish DPS IGT Lifestyle 58% IGT Metformin Acarbose 31% 25% US DPP STOPNIDDM TRIPOD XENDOS DREAM Troglitazone Prior GDM Orlistat IGT Rosiglitazone/Ramipril IGT 55% 45% 61%/NS

A 1 C*† <7. 0% Preprandial glucose 90 -130 mg/d. L Postprandial plasma glucose <180 mg/d. L * For non-pregnant individuals † As close to normal (<6%) as possible without significant hypoglycemia American Diabetes Association. Diabetes Care. 2007: 30: S 4 -41. .

§ § Fasting plasma glucose at least every 3 yrs starting at age 45 Consider at younger age, or more frequently, if patient is overweight and has one or more of the following risk factors (or two if not overweight): • Family history of diabetes • Overweight (BMI 25 kg/m 2) • Habitual physical inactivity (continued) American Diabetes Association. Diabetes Care. 2007: 30: S 4 -41. .

Additional risk factors: • Race/ethnicity (e. g. , African-Americans, Hispanic. Americans, Native Americans, Asian-Americans, and Pacific Islanders) • Previously identified IFG or IGT • Hypertension (140/90 mm. Hg in adults) • HDL cholesterol (35 mg/dl [0. 90 mmol/l] and/or a triglyceride level 250 mg/dl [2. 82 mmol/l]) • History of GDM or delivering baby weighing >9 lbs • Polycystic ovary syndrome (PCOS) American Diabetes Association. Diabetes Care. 2007: 30: S 4 -41. .

§ § § § § Age Race/ethnicity Gender Family history Overweight/obesity Abnormal lipid metab Hypertension Smoking Physical Inactivity Unhealthy diet 47 African American Male HTN and diabetes BMI = 29 TC = 210 BP = 146/86 1 pack per day Sedentary Fast food diet

§ Identify at-risk patients by evaluating a spectrum of predisposing risk factors § The existence of any one risk factor is an alert to evaluate patient for others § Integrate evidence-based risk management strategies to target modifiable risk factors Kahn, et al. The Metabolic Syndrome: Time for a Critical Appraisal: Joint Statement From the American Diabetes Association and the European Association for the Study of Diabetes Care. 2005; 28 (9)2289 -2304.


THANK YOU
- Slides: 77