Cardiology Review Part 3 Oct 2018 SVT Case






































- Slides: 47

Cardiology Review Part 3 Oct 2018

SVT

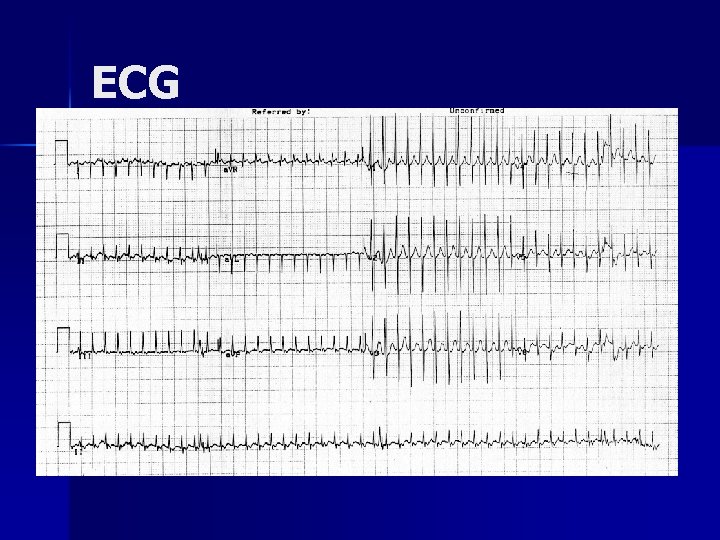
Case n A 10 day old male infant arrives in the emergency room with a heart rate of 270 bpm, narrow complex.

ECG

Supraventricular Tachycardia (SVT) 1. Atrial Ectopic Tachycardia (AET) 2. Accessory pathway mediated re-entry tachycardia (AVRT) 3. AV nodal re-entry tachycardia (AVNRT)

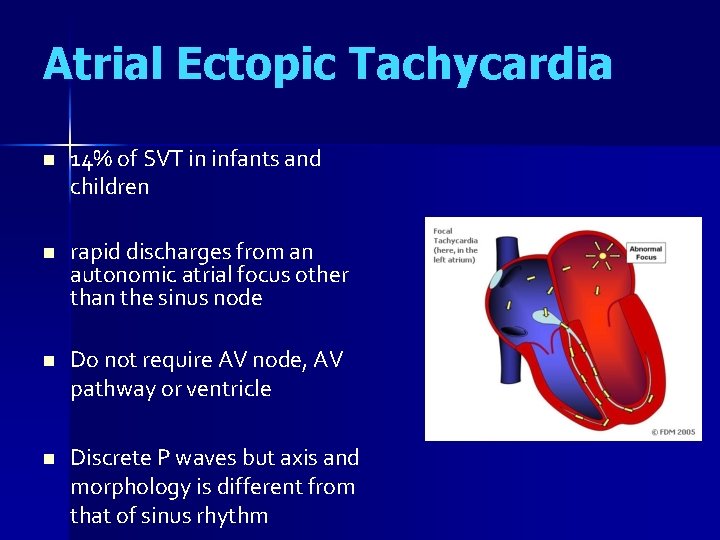
Atrial Ectopic Tachycardia n 14% of SVT in infants and children n rapid discharges from an autonomic atrial focus other than the sinus node n Do not require AV node, AV pathway or ventricle n Discrete P waves but axis and morphology is different from that of sinus rhythm

Atrial Ectopic Tachycardia n Clinical presentation – Tachycardia is usually chronic and often incessant – High association with tachycardia-induced cardiomyopathy – Infants/children may present with CHF symptoms – Most have structurally normal heart

Characteristics Wide variation in rate that correlates directly with sympathetic tone ▪ Increases during exertion, stress, fever Gradual “warm up and cool down” of heart rates Sometimes an incessant disorder ▪ Risk of tachycardia mediated cardiomyopathy Does not terminate with vagal maneuvers or cardioversion

Atrial Ectopic Tachycardia Infants (< 1 years) Likely to outgrow Children (> 1 years) & Adolescents Likely to require longterm therapy May require ablation

Re-Entry SVT The typical “SVT” of childhood > 80% of SVTs in childhood Re-Entry circuit: 2 pathways for conduction Electrical impulse cycles repetitively through circuit

Re-Entry SVT How do you know this is “SVT”? Sudden/paroxysmal onset of symptoms (palpitations) Typically occurs at rest Exercise may be a trigger for some Abrupt onset and termination ▪ Automaticity has “ warm-up/warm-down” periods Terminated with vagal maneuvers or cardioversion (medical or electrical) Rates typically > 220 infants, >180 children

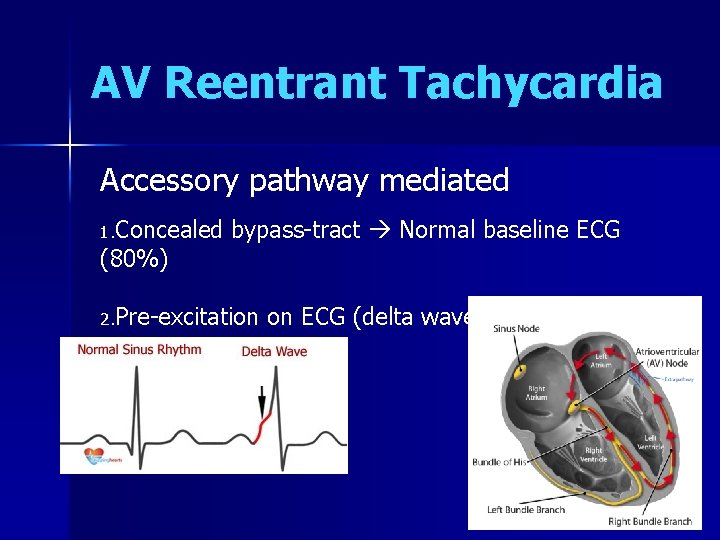
AV Reentrant Tachycardia Accessory pathway mediated 1. Concealed (80%) bypass-tract Normal baseline ECG 2. Pre-excitation on ECG (delta wave) (20%)

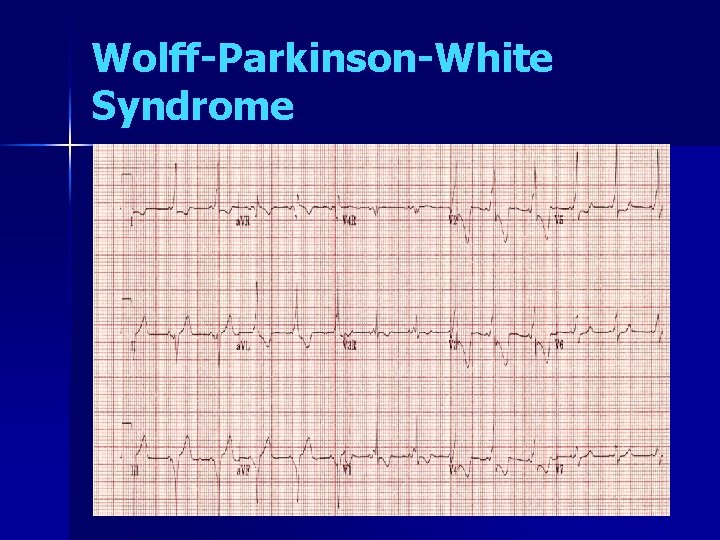
Wolff-Parkinson-White Syndrome

Wolff-Parkinson-White WPW pattern on ECG - 0. 13 -0. 25% in general population WPW “syndrome” associated symptoms (SVT) Sudden cardiac death in WPW syndrome is estimated to range from 0. 15% to 0. 39% over 3 - to 10 -year follow-up Rapid pre-excited A. Fib Requires risk stratification ▪ ▪ Non-invasive studies- Holter and Exercise testing Invasive EP studies ALL need referral to cardiology, even if asymptomatic

Natural History of SVT n AVRT – 70% of infant SVT will “outgrow” by 1 year – 30% may have recurrence later in childhood (average 8 years) n AVNRT – Rare in infants – Represents ~ 30% SVT in older children/adolescents

Diagnosis History Differential diagnosis of palpitations Neonates are high-risk group for CHF/tachycardia induced cardiomyopathy Baseline ECG Evaluate for pre-excitation Holter TTM- transtelephone monitor

1. Vagal stimulatory maneuvers: Ice bag to forehead, up to 5 -10 seconds in infants Bearing down Blowing through occluded straw/balloon Head stands 2. Adenosine Causes transient heart block in the AV node Extremely short half-life (seconds) Side Effects: ▪ ▪ ▪ “Impending Doom” Facial flushing Rash on chest Pro-arrhythmic effects (VT!!!!) 3. Electrical cardioversion 4. Anti-arrhythmics or trans-esophageal pacing Done in consultation with cardiology

SVT n n n If a child has hemodynamic compromise, hypotension or altered consciousness, immediate electrical cardioversion is indicated Vagal maneuvers if hemodynamically stable Adenosine is tx of choice if stable, and vagal maneuver has failed

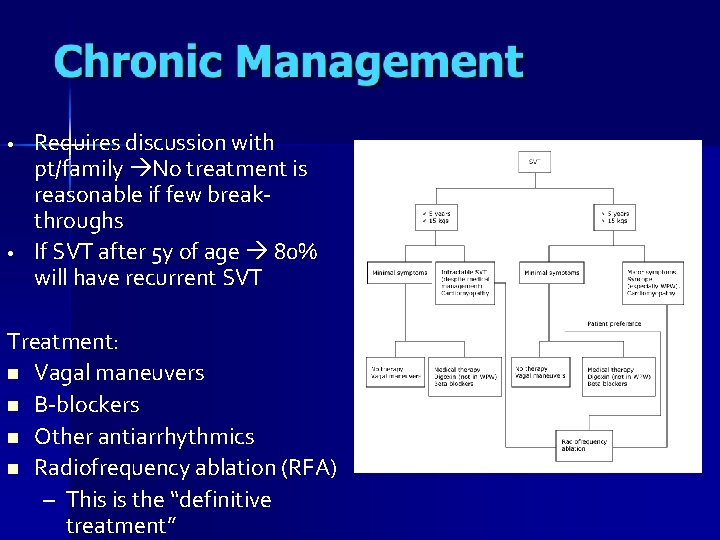
• • Requires discussion with pt/family No treatment is reasonable if few breakthroughs If SVT after 5 y of age 80% will have recurrent SVT Treatment: n Vagal maneuvers n B-blockers n Other antiarrhythmics n Radiofrequency ablation (RFA) – This is the “definitive treatment”

B-Blocker therapy Considerations: n n Cardio B 1 selective vs. non-cardio selective Dosing: once daily, BID, TID Side Effects: n n n Depression Fatigue Lipid metabolism + weight gain Hypoglycemia – Particularly infants Increased airways resistance – Consideration in asthmatics

LONG QT Congenital n Acquired n Electrolyte abnormality Medications/Drugs ▪ ▪ ▪ macrolide antibiotics antifungal agents antiretroviral agent Cytochrome p 450 system ▪ Drug-drug interactions

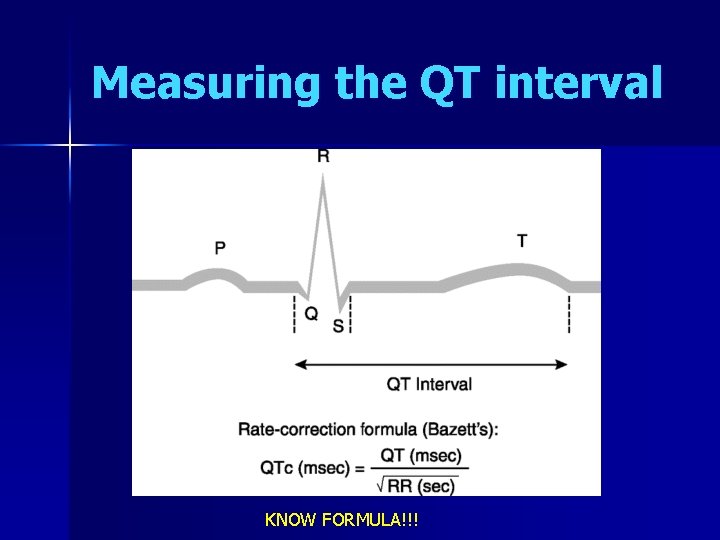
Measuring the QT interval KNOW FORMULA!!!

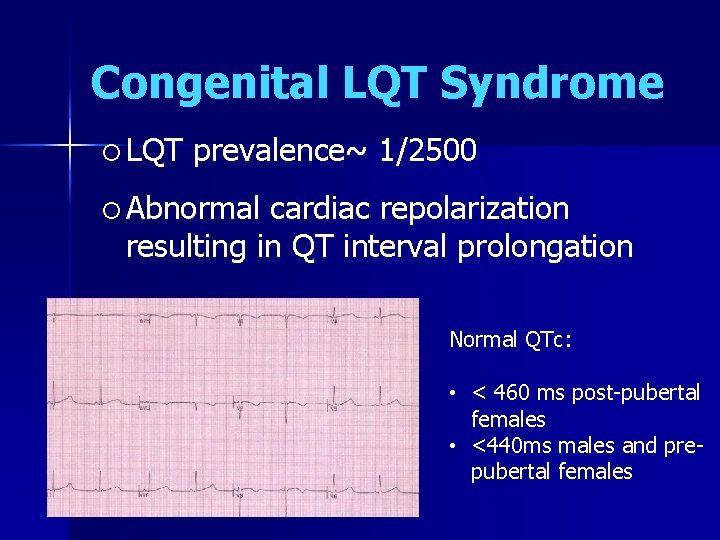
Congenital LQT Syndrome LQT prevalence~ 1/2500 Abnormal cardiac repolarization resulting in QT interval prolongation Normal QTc: • < 460 ms post-pubertal females • <440 ms males and prepubertal females

Congenital LQT Syndrome. Genetics n 13 types of congenital LQTS have been identified – LQT 1 - 30 to 35 % – LQT 2 - 25 to 40 % – LQT 3 - 5 to 10 % – Other types - <5 % n Romano-Ward syndrome Autosomal Dominant – More common form of long QT – Normal hearing! n Jarvell and Lange Nielsen Autosomal Recessive – Associated with Sensorineural hearing loss

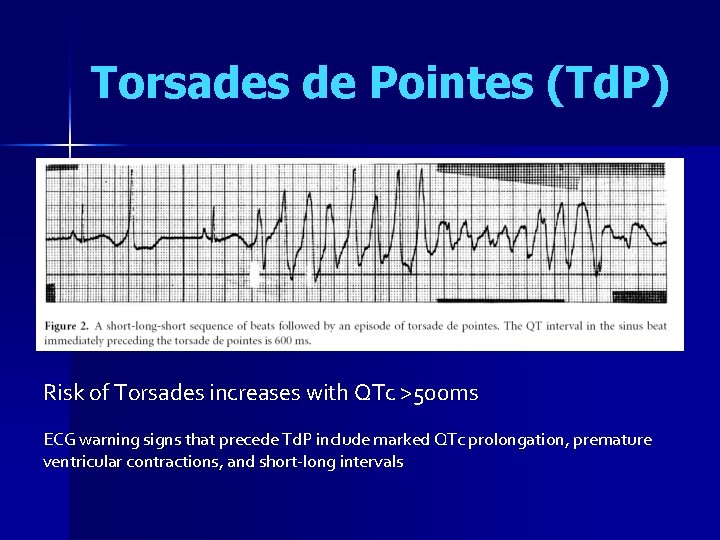
Torsades de Pointes (Td. P) Risk of Torsades increases with QTc >500 ms ECG warning signs that precede Td. P include marked QTc prolongation, premature ventricular contractions, and short-long intervals

LQT management n 1 st line B-blocker n. Exercise restrictions – No competitive sports – Avoid swimming n. Avoid QT prolonging meds – Long list – www. crediblemeds. org n. ICD +/- pacemaker

Congenital Long QT Syndrome www. crediblemeds. org

Syncope- Differential diagnosis Neurally mediated n Orthostatic n Primary arrhythmia n Primary Cardiac structural n

Differential Diagnosis n Syncope Mimics: – Conversion – Pseudo-syncope – Cataplexy – Transient ischemic attacks

Differential Diagnosis Neurally Mediated: n. Neurocardiogenic n. Orthostatic n. Hypotension n *MOST COMMON! n. Vagal – Vasovagal – Micturition – Cough n. Carotid sinus hypersensitivity n. Breath-holding Spell (younger child) Neuropsychiatric n. Hyperventilation n. Atypical migraine n. Seizure n. Hypoglycemia n n CARDIAC Primary cardiac arrhythmia Primary cardiac structural disease

Structural Problems n n n n Hypertrophic Cardiomyopathy (HCM) Arrythmogenic right ventricular dysplasia (ARVD) Dilated cardiomyopathy Aortic Stenosis Coronary artery anomalies Acute myocarditis Marfan Syndrome – aortic root rupture Pulmonary Hypertension

Electrical Problems Long QT n AV block/ Brady-arrhythmia n Pre-excitation (WPW) n Brugada syndrome rare n Catecholamine polymorphic ventricular tachycardia (CPVT) rare n Congenital short QT very rare n

“Reg Flags” on Hx n n n Sudden syncope (no preceding lightheadedness/dizziness) With exertion – Particularly peak exercise – Early recovery phase Associated with palpitations With sudden increase in sympathetic tone (eg: emotion, fright) Young age Positive family history

Syncope Work-up n Orthostatic/Vagal: n n ECG only 2017 AHA guidelines: if clear vasovagal syncope, Ecg not required Exercise or non-prodromal Syncope: – ECG – Holter – Echo – Treadmill

What is Rheumatic Fever? n n n Acute inflammatory illness Follows GAS pharyngitis (strep throat) Involves 4 main organ systems – – Heart Joints Brain Skin

Pathogenesis of ARF M protein

Acute Rheumatic Fever overcrowding strain 5 -15 y virulence genetic factors 0. 3 - 5% develop ARF after untreated GAS pharyngiti

Jones Criteria for Diagnosis of ARF ***Evidence of GAS pharyngeal infection*** Major Criteria n n n Carditis Chorea Polyarthritis Erythema marginatum Subcutaneous nodules Minor Criteria n n n Fever Arthralgia Elevated acute-phase reactants – ESR, CRP n Prolonged PR interval Primary RF episode = 2 major or 1 major + 2 minor (Exception is Chorea if present only criteria needed

Non-Cardiac Manifestations of ARF n n Appear 10 d - 5 wks after GAS pharyngitis Migratory polyarthritis (40 -70%) – – migratory large joints (knees, ankles, elbows and wrists) affected joints are red, swollen and ++ tender rapid response to ASA n Erythema marginatum (<5%) n Subcutaneous nodules (0 -10%) n Sydenham chorea (10 -30% of cases) – Macular, nonpruritic rash with serpiginous erythematous border – Rash comes and goes – Painless, movable nodules on extensor surfaces of joints – presents 1 -6 months post-GAS infection

2015 AHA guidelines

2015 AHA guidelines

Carditis in ARF 30 -70% of cases n Presents within 2 weeks of GAS infection n Valvulitis (inflammation of valves) n – mitral regurgitation (95%) – aortic regurgitation (20 -25%) n Variable severity – murmur – critical heart failure

For cases of suspected ARF Throat culture n ASOT (anti-streptolysin O titre) n WBC n ESR n CRP n ECG n Echocardiogram n

Treatment of ARF n Antibiotic treatment – PO Penicillin V x 10 days n clindamycin, cephalosporin, azithromycin if allergic – IM Penicillin G x 1 dose n n Restricted activity Anti-inflammatory therapy – ASA for mild-moderate carditis – Steroids for severe carditis – optimal duration ? Heart failure treatment if necessary Secondary prophylaxis – – Penicillin G IM every 3 -4 weeks Penicillin V PO BID

ARF

Rheumatic Heart Disease Consequence of ARF n Chronic mitral regurgitation n – mitral stenosis in older adults Chronic aortic regurgitation n More severe disease with recurrent episodes of ARF n

Questions?