Cardiodynamics and Blood Vessels Muse s 13 Bio
Cardiodynamics and Blood Vessels Muse s 13 Bio 238 Lecture #3 5/16/13

The Conducting System § The Role of Calcium Ions in Cardiac Contractions § Contraction of a cardiac muscle cell is produced by an increase in calcium ion concentration around myofibrils

The Conducting System § The Role of Calcium Ions in Cardiac Contractions § 20% of calcium ions required for a contraction § Calcium ions enter plasma membrane during plateau phase § Arrival of extracellular Ca 2+ § Triggers release of calcium ion reserves from sarcoplasmic reticulum

The Conducting System § The Role of Calcium Ions in Cardiac Contractions § As slow calcium channels close § Intracellular Ca 2+ is absorbed by the SR § Or pumped out of cell § Cardiac muscle tissue § Very sensitive to extracellular Ca 2+ concentrations

The Conducting System § The Energy for Cardiac Contractions § Aerobic energy of heart § From mitochondrial breakdown of fatty acids and glucose § Oxygen from circulating hemoglobin § Cardiac muscles store oxygen in myoglobin

The Cardiac Cycle § Phases of the Cardiac Cycle § Within any one chamber § Systole (contraction) § Diastole (relaxation)
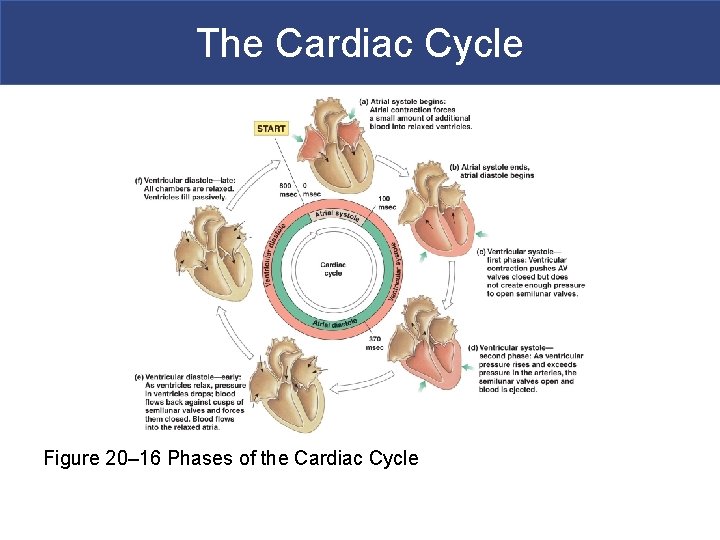
The Cardiac Cycle Figure 20– 16 Phases of the Cardiac Cycle
The Cardiac Cycle § Blood Pressure § In any chamber § Rises during systole (ventricular compression) 120 § Falls during diastole (vessel elasticity) 60 § Blood flows from high to low pressure § Controlled by timing of contractions § Directed by one-way valves - not perfect seals

The Cardiac Cycle § Cardiac Cycle and Heart Rate § At 75 beats per minute § Cardiac cycle lasts about 800 msecs § When heart rate increases § All phases of cardiac cycle shorten, particularly diastole
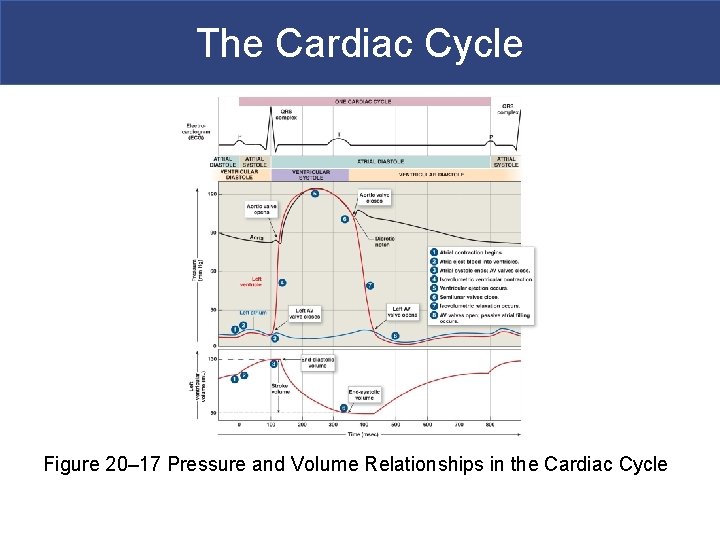
The Cardiac Cycle Figure 20– 17 Pressure and Volume Relationships in the Cardiac Cycle
The Cardiac Cycle § Heart Sounds § S 1 § Loud sounds § Produced by AV valves § S 2 § Loud sounds § Produced by semilunar valves § S 3, S 4 § Soft sounds § Blood flow into ventricles and atrial contraction

The Cardiac Cycle § Heart Murmur § Sounds produced by regurgitation through valves
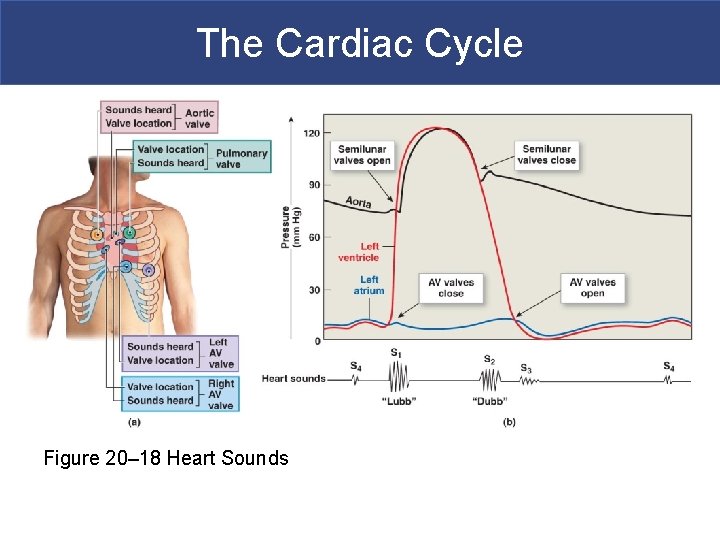
The Cardiac Cycle Figure 20– 18 Heart Sounds
Cardiodynamics § Cardiac Output § CO = HR X SV § CO = cardiac output (m. L/min) § HR = heart rate (beats/min) § SV = stroke volume (m. L/beat)

Cardiodynamics § Factors Affecting Cardiac Output § Cardiac output § Adjusted by changes in heart rate or stroke volume § Heart rate § Adjusted by autonomic nervous system or hormones § Stroke volume § Adjusted by changing EDV or ESV
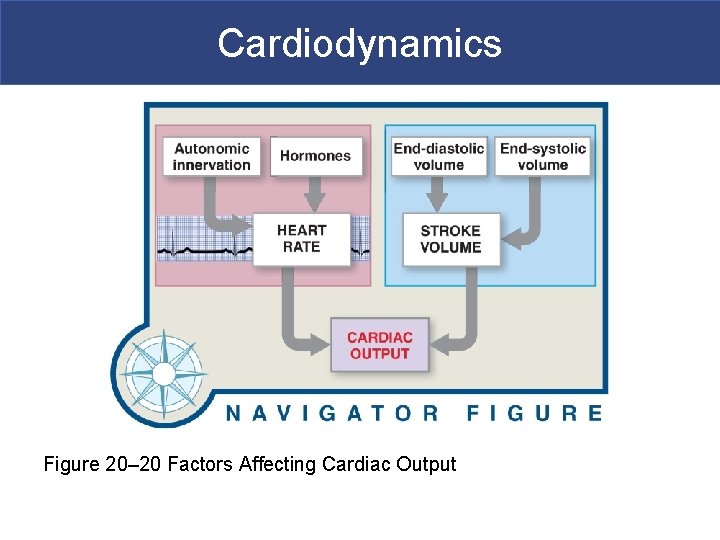
Cardiodynamics Figure 20– 20 Factors Affecting Cardiac Output

Cardiodynamics § Factors Affecting the Heart Rate § Autonomic innervation § Cardiac plexuses: innervate heart § Vagus nerves (X): carry parasympathetic preganglionic fibers to small ganglia in cardiac plexus § Cardiac centers of medulla oblongata: – cardioacceleratory center controls sympathetic neurons (increases heart rate) – cardioinhibitory center controls parasympathetic neurons (slows heart rate)

Cardiodynamics § Autonomic Innervation § Cardiac reflexes § Cardiac centers monitor: – blood pressure (baroreceptors) – arterial oxygen and carbon dioxide levels (chemoreceptors) § Cardiac centers adjust cardiac activity § Autonomic tone § Dual innervation maintains resting tone by releasing ACh and NE § Fine adjustments meet needs of other systems
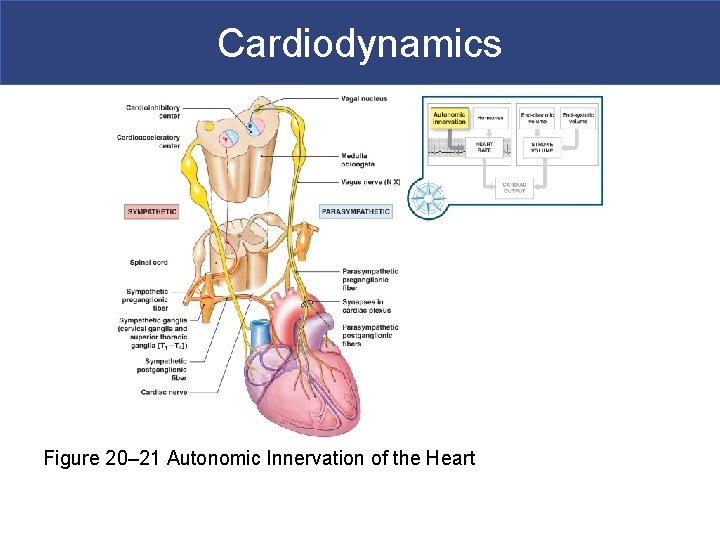
Cardiodynamics Figure 20– 21 Autonomic Innervation of the Heart

Cardiodynamics § Effects on the SA Node § Sympathetic and parasympathetic stimulation § Greatest at SA node (heart rate) § Membrane potential of pacemaker cells § Lower than other cardiac cells § Rate of spontaneous depolarization depends on § Resting membrane potential § Rate of depolarization § ACh (parasympathetic stimulation) § Slows the heart § NE (sympathetic stimulation) § Speeds the heart
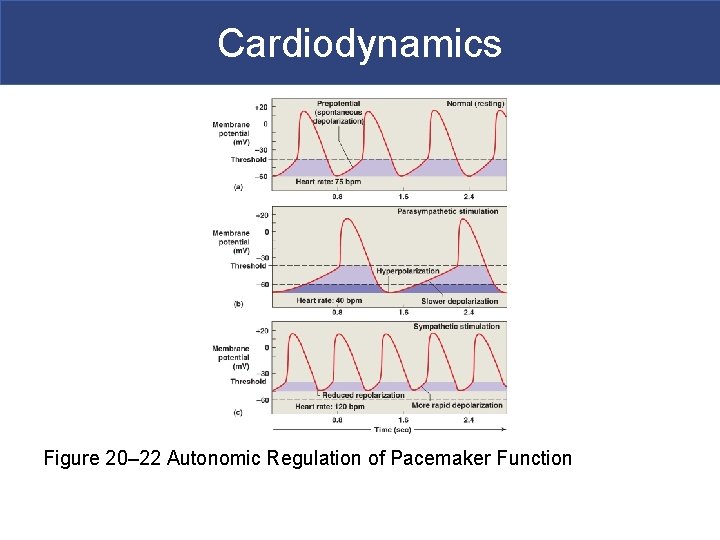
Cardiodynamics Figure 20– 22 Autonomic Regulation of Pacemaker Function

Cardiodynamics § Hormonal Effects on Heart Rate § Increase heart rate (by sympathetic stimulation of SA node) § Epinephrine (E) § Norepinephrine (NE) § Thyroid hormone

Cardiodynamics § Factors Affecting the Stroke Volume § The EDV: amount of blood a ventricle contains at the end of diastole § Filling time: – duration of ventricular diastole § Venous return: – rate of blood flow during ventricular diastole

Cardiodynamics § The Frank–Starling Principle § As EDV increases, stroke volume increases § Physical Limits § Ventricular expansion is limited by § Myocardial connective tissue § The cardiac (fibrous) skeleton § The pericardial sac

Cardiodynamics § End-Systolic Volume (ESV) § The amount of blood that remains in the ventricle at the end of ventricular systole is the ESV

Cardiodynamics § Effects of Autonomic Activity on Contractility § Sympathetic stimulation § NE released by postganglionic fibers of cardiac nerves § Epinephrine and NE released by suprarenal (adrenal) medullae § Causes ventricles to contract with more force § Increases ejection fraction and decreases ESV

Cardiodynamics § Effects of Autonomic Activity on Contractility § Parasympathetic activity § Acetylcholine released by vagus nerves § Reduces force of cardiac contractions

Cardiodynamics § Hormones § Many hormones affect heart contraction § Pharmaceutical drugs mimic hormone actions § Stimulate or block beta receptors § Affect calcium ions (e. g. , calcium channel blockers)

Cardiodynamics § Heart Rate Control Factors § Autonomic nervous system § Sympathetic and parasympathetic § Circulating hormones § Venous return and stretch receptors Cardiac Reserve The difference between resting and maximal cardiac output
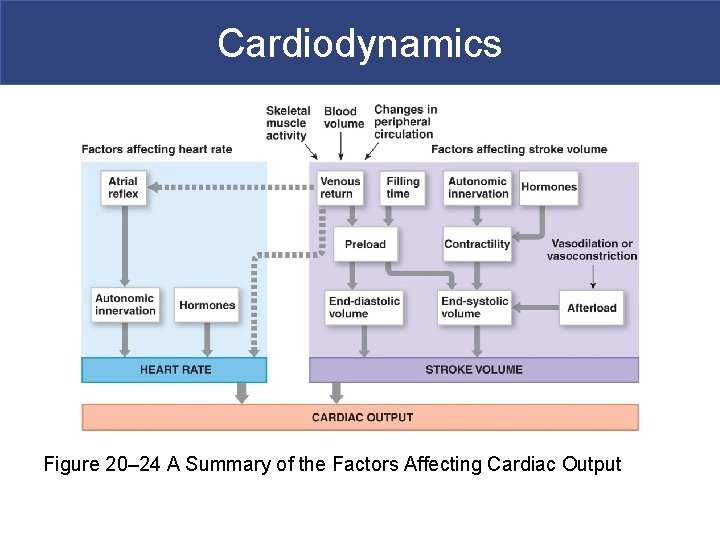
Cardiodynamics Figure 20– 24 A Summary of the Factors Affecting Cardiac Output
Classes of Blood Vessels § Arteries § Carry blood away from heart § Arterioles § Are smallest branches of arteries § Capillaries § Are smallest blood vessels § Location of exchange between blood and interstitial fluid § Venules § Collect blood from capillaries § Veins § Return blood to heart
Blood Vessels § The Largest Blood Vessels § Attach to heart § Pulmonary trunk § Carries blood from right ventricle § To pulmonary circulation § Aorta § Carries blood from left ventricle § To systemic circulation

Blood Vessels § The Smallest Blood Vessels § Capillaries § Have small diameter and thin walls § Chemicals and gases diffuse across walls

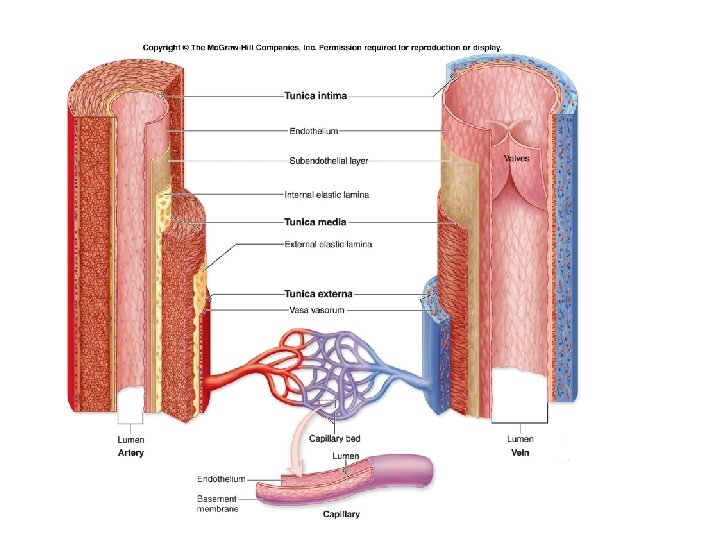
Blood Vessels § The Structure of Vessel Walls § Walls have three layers: § Tunica intima § Tunica media § Tunica externa

Blood Vessels § The Tunica Intima § Is the innermost layer § Includes § The endothelial lining § Connective tissue layer § Internal elastic membrane: – in arteries, is a layer of elastic fibers in outer margin of tunica intima
Blood Vessels § The Tunica Media § Is the middle layer § Contains concentric sheets of smooth muscle in loose connective tissue § Binds to inner and outer layers § External elastic membrane of the tunica media § Separates tunica media from tunica externa

Blood Vessels § The Tunica Externa § Is outer layer § Contains connective tissue sheath § Anchors vessel to adjacent tissues in arteries § Contain collagen § Elastic fibers § In veins § Contains elastic fibers § Smooth muscle cells § Vasa vasorum (“vessels of vessels”) § Small arteries and veins § In walls of large arteries and veins § Supply cells of tunica media and tunica externa
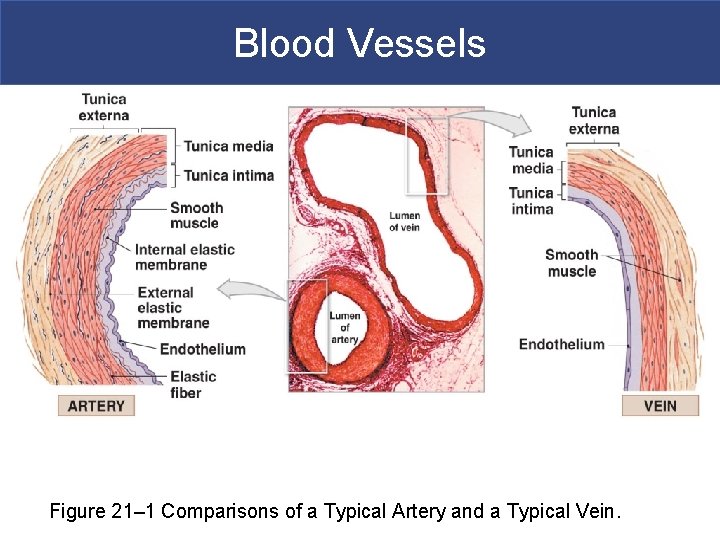
Blood Vessels Figure 21– 1 Comparisons of a Typical Artery and a Typical Vein.
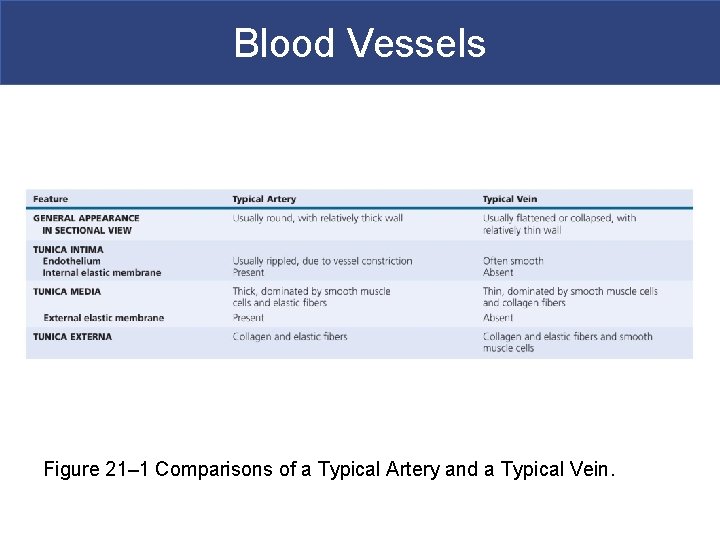
Blood Vessels Figure 21– 1 Comparisons of a Typical Artery and a Typical Vein.
Blood Vessels § Differences between Arteries and Veins § Arteries and veins run side by side § Arteries have thicker walls and higher blood pressure § Collapsed artery has small, round lumen (internal space) § Vein has a large, flat lumen § Vein lining contracts, artery lining does not § Artery lining folds § Arteries more elastic § Veins have valves
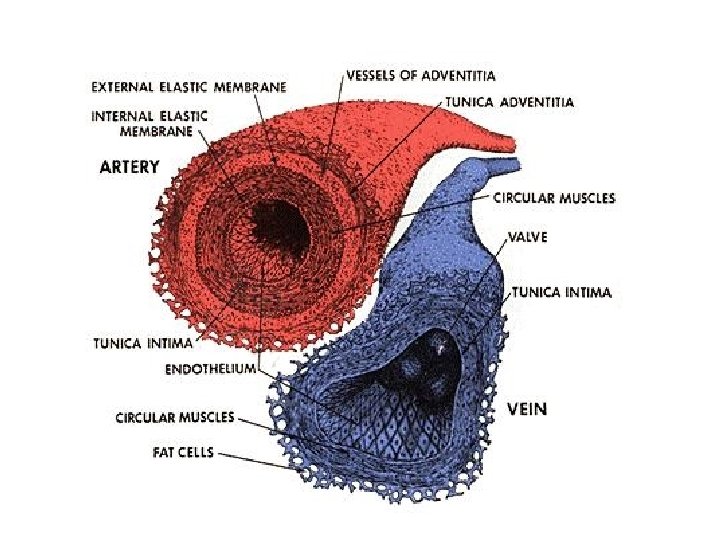

Structure and Function of Arteries § Arteries and Pressure § Elasticity allows arteries to absorb pressure waves that come with each heartbeat § Contractility § Arteries change diameter § Controlled by sympathetic division of ANS § Vasoconstriction: – the contraction of arterial smooth muscle by the ANS § Vasodilatation: – the relaxation of arterial smooth muscle – enlarging the lumen

Structure and Function of Arteries § Vasoconstriction and Vasodilation § Affect § Afterload on heart § Peripheral blood pressure § Capillary blood flow

Structure and Function of Arteries § From heart to capillaries, arteries change § From elastic arteries § To muscular arteries § To arterioles

Structure and Function of Arteries § Elastic Arteries § Also called conducting arteries § Large vessels (e. g. , pulmonary trunk and aorta) § Tunica media has many elastic fibers and few muscle cells § Elasticity evens out pulse force

Structure and Function of Arteries § Muscular Arteries § Also called distribution arteries § Are medium sized (most arteries) § Tunica media has many muscle cells

Structure and Function of Arteries § Arterioles § Are small § Have little or no tunica externa § Have thin or incomplete tunica media § Artery Diameter § Small muscular arteries and arterioles § Change with sympathetic or endocrine stimulation § Constricted arteries oppose blood flow – resistance (R): » resistance vessels: arterioles
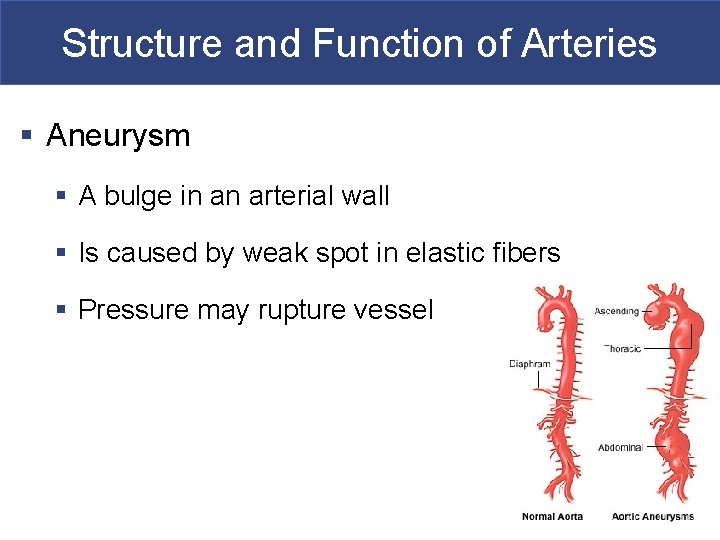
Structure and Function of Arteries § Aneurysm § A bulge in an arterial wall § Is caused by weak spot in elastic fibers § Pressure may rupture vessel
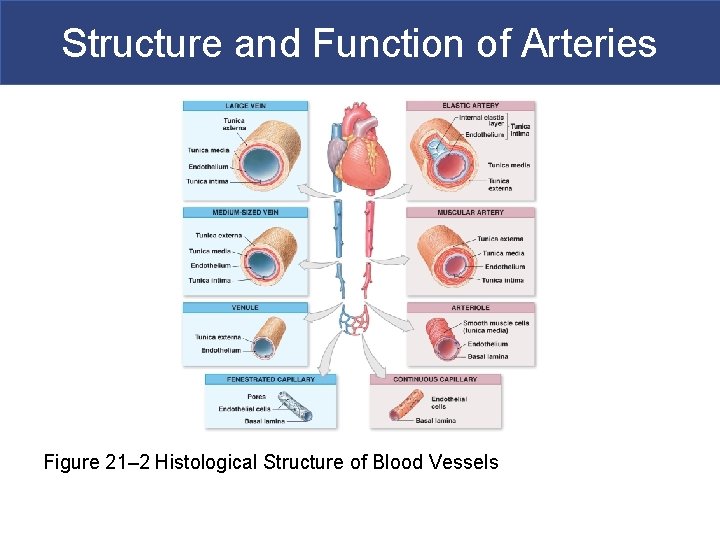
Structure and Function of Arteries Figure 21– 2 Histological Structure of Blood Vessels
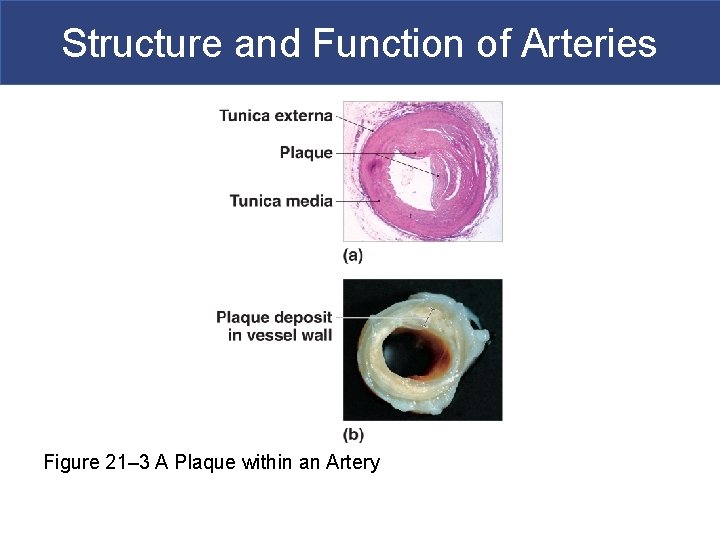
Structure and Function of Arteries Figure 21– 3 A Plaque within an Artery

Atherosclerosis § Hardening of the arteries. -Cholesterol rich fatty plaques stick to side walls of artery and fill with calcium. § When they burst can lead to inflammation which occludes the artery. § White blood cells can build up here and contribute to inflammatory response
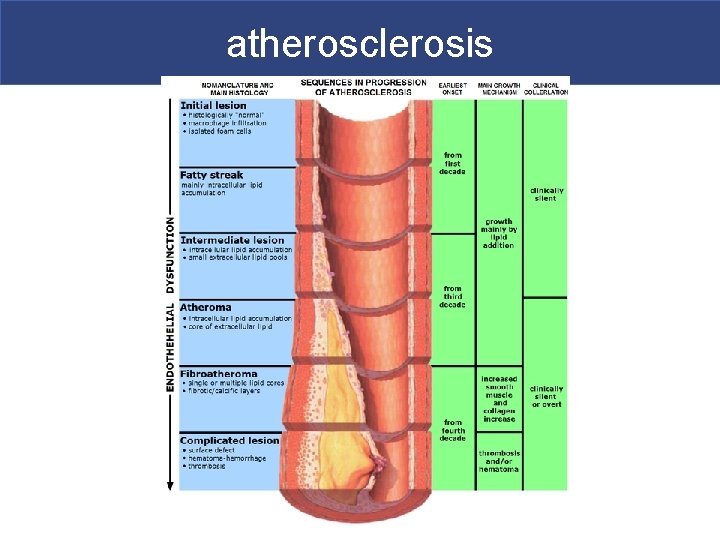
atherosclerosis

Structure and Function of Capillaries § Are smallest vessels with thin walls § Microscopic capillary networks permeate all active tissues § Capillary function § Location of all exchange functions of cardiovascular system § Materials diffuse between blood and interstitial fluid

Structure and Function of Capillaries § Capillary Structure § Endothelial tube, inside thin basal lamina § No tunica media § No tunica externa § Diameter is similar to red blood cell

Structure and Function of Capillaries § Fenestrated Capillaries § Have pores in endothelial lining § Permit rapid exchange of water and larger solutes between plasma and interstitial fluid § Are found in § Choroid plexus § Endocrine organs § Kidneys § Intestinal tract
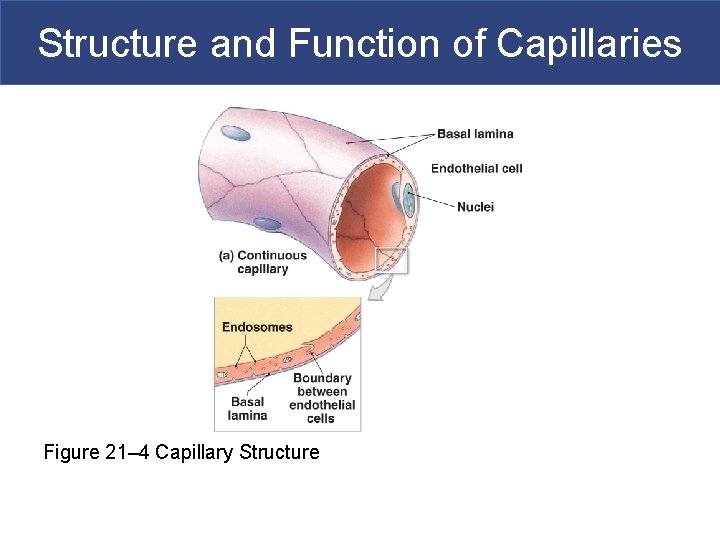
Structure and Function of Capillaries Figure 21– 4 Capillary Structure
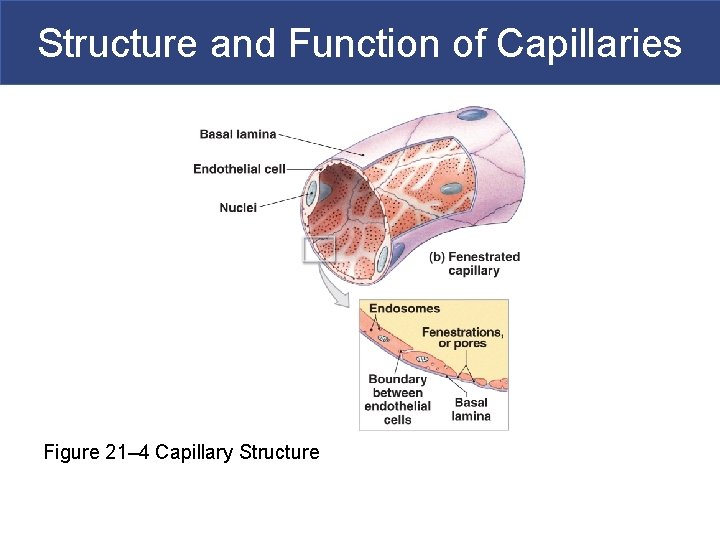
Structure and Function of Capillaries Figure 21– 4 Capillary Structure

Structure and Function of Capillaries § Capillary Sphincter § Guards entrance to each capillary § Opens and closes, causing capillary blood to flow in pulses

Structure and Function of Capillaries § Vasomotion § Contraction and relaxation cycle of capillary sphincters § Causes blood flow in capillary beds to constantly change routes
Structure and Function of Veins § Collect blood from capillaries in tissues and organs § Return blood to heart § Are larger in diameter than arteries § Have thinner walls than arteries § Have lower blood pressure

Structure and Function of Veins § Vein Categories § Venules § Very small veins § Collect blood from capillaries § Medium-sized veins § Thin tunica media and few smooth muscle cells § Tunica externa with longitudinal bundles of elastic fibers § Large veins § Have all three tunica layers § Thick tunica externa § Thin tunica media
Structure and Function of Veins § Venous Valves § Folds of tunica intima § Prevent blood from flowing backward § Compression pushes blood toward heart
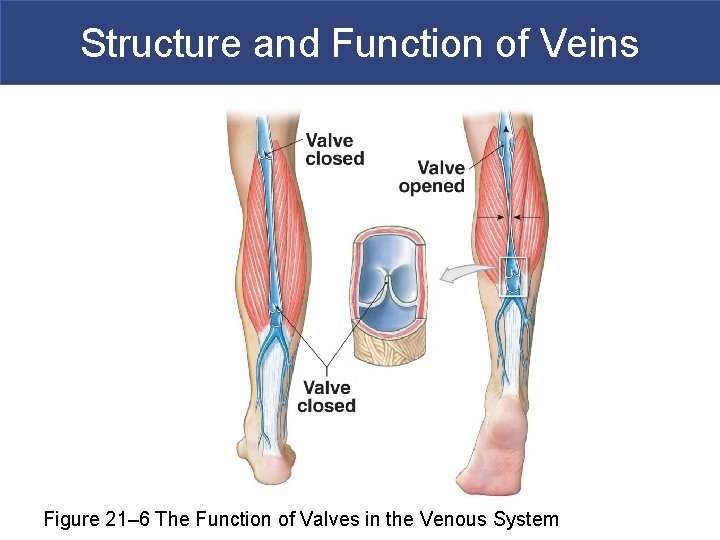
Structure and Function of Veins Figure 21– 6 The Function of Valves in the Venous System
Blood Vessels § The Distribution of Blood § Heart, arteries, and capillaries § 30– 35% of blood volume § Venous system § 60– 65%: – 1/3 of venous blood is in the large venous networks of the liver, bone marrow, and skin
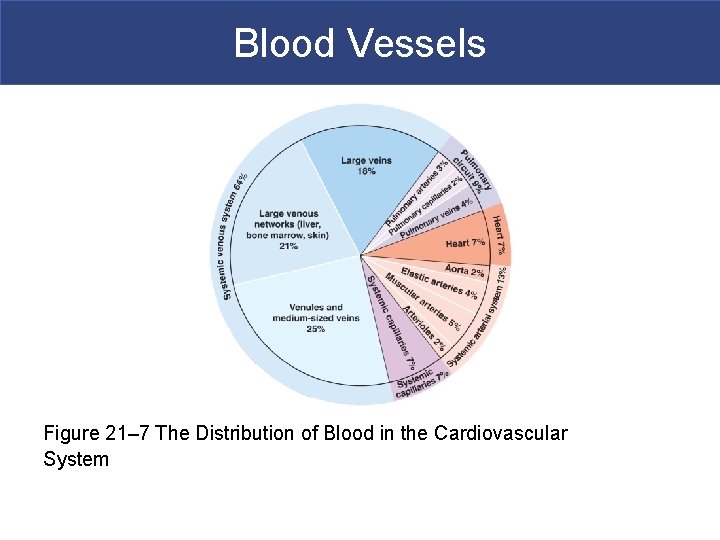
Blood Vessels Figure 21– 7 The Distribution of Blood in the Cardiovascular System

Hemorrhage! When large amounts of blood is lost in a short time Class II haemorrhage (15– 30% total blood volume)
Blood Vessels § Capacitance of a Blood Vessel § The ability to stretch § Relationship between blood volume and blood pressure § Veins (capacitance vessels) stretch more than arteries

Blood Vessels § Venous Response to Blood Loss § Vasomotor centers stimulate sympathetic nerves § Systemic veins constrict (venoconstriction) § Veins in liver, skin, and lungs redistribute venous reserve
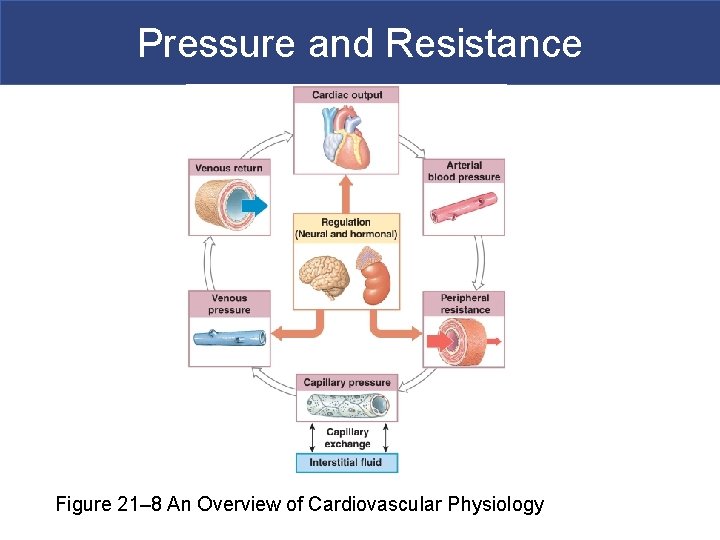
Pressure and Resistance Figure 21– 8 An Overview of Cardiovascular Physiology

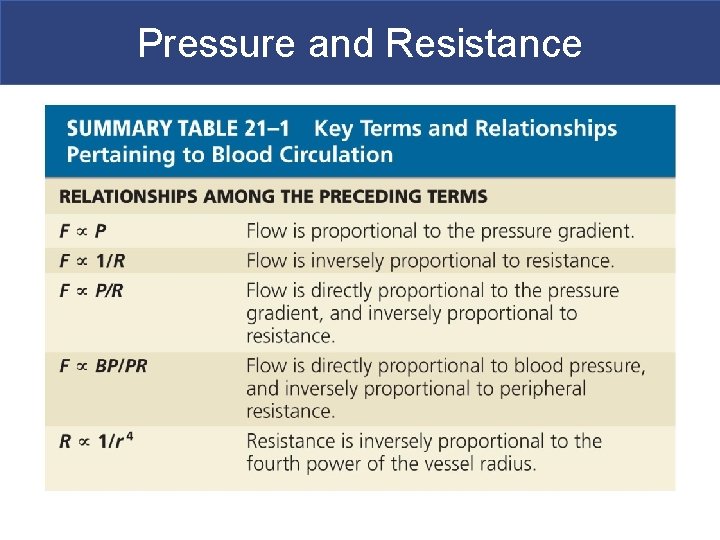
Pressure and Resistance § Pressure (P) § The heart generates P to overcome resistance § Absolute pressure is less important than pressure gradient § The Pressure Gradient ( P) § Circulatory pressure = pressure gradient § The difference between § Pressure at the heart § And pressure at peripheral capillary beds

Pressure and Resistance § Force (F) § Is proportional to the pressure difference ( P) § Divided by R
Pressure and Resistance § Measuring Pressure § Blood pressure (BP) § Arterial pressure (mm Hg) § Capillary hydrostatic pressure (CHP) § Pressure within the capillary beds § Venous pressure § Pressure in the venous system

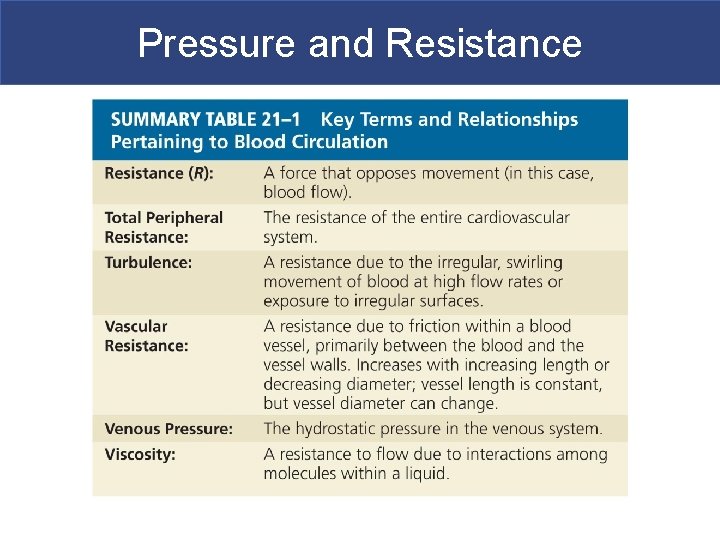
Pressure and Resistance § Viscosity § R caused by molecules and suspended materials in a liquid § Whole blood viscosity is about four times that of water

Pressure and Resistance § Turbulence § Swirling action that disturbs smooth flow of liquid § Occurs in heart chambers and great vessels § Atherosclerotic plaques cause abnormal turbulence

Pressure and Resistance

Pressure and Resistance
Pressure and Resistance
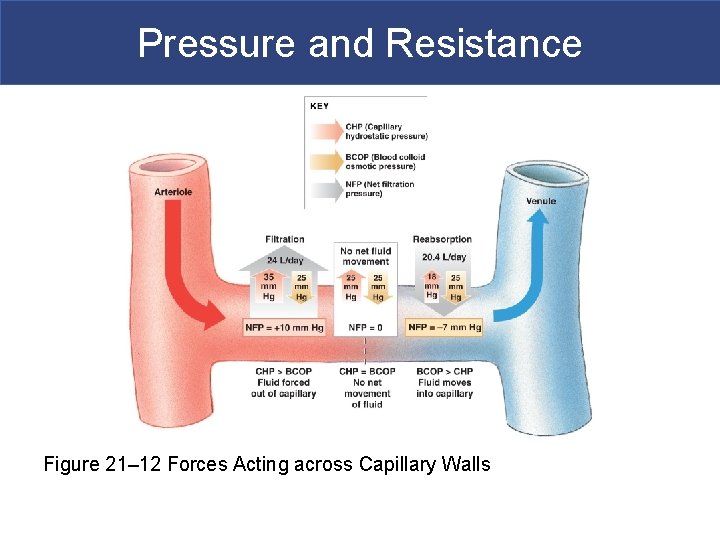
Pressure and Resistance Figure 21– 12 Forces Acting across Capillary Walls
Cardiovascular Regulation § Tissue Perfusion § Blood flow through the tissues § Carries O 2 and nutrients to tissues and organs § Carries CO 2 and wastes away § Is affected by § Cardiac output § Peripheral resistance § Blood pressure

Cardiovascular Regulation § Cardiovascular regulation changes blood flow to a specific area § At an appropriate time § In the right area § Without changing blood pressure and blood flow to vital organs
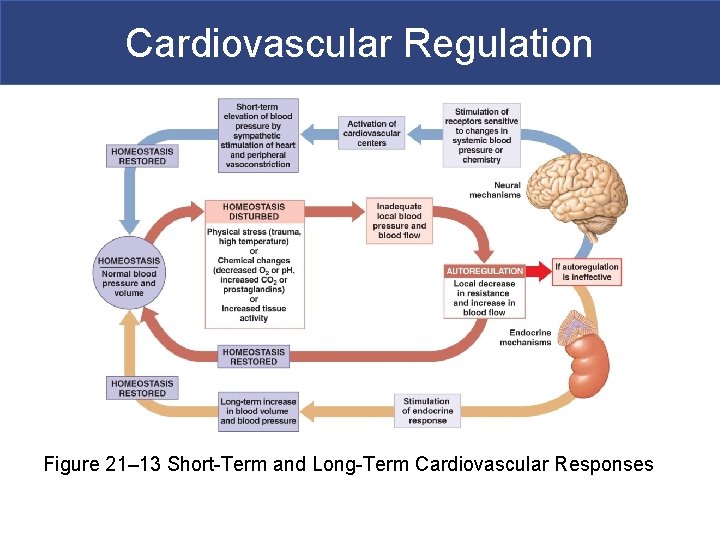
Cardiovascular Regulation Figure 21– 13 Short-Term and Long-Term Cardiovascular Responses

Cardiovascular Regulation § Controlling Cardiac Output and Blood Pressure § Autoregulation § Causes immediate, localized homeostatic adjustments § Neural mechanisms § Respond quickly to changes at specific sites § Endocrine mechanisms § Direct long-term changes
Cardiovascular Regulation § Autoregulation of Blood Flow within Tissues § Adjusted by peripheral resistance while cardiac output stays the same § Local vasodilators: – accelerate blood flow at tissue level » low O 2 or high CO 2 levels » low p. H (acids) » nitric oxide (NO) » high K+ or H+ concentrations » chemicals released by inflammation (histamine) » elevated local temperature

Cardiovascular Regulation § Vasomotor Tone § Produced by constant action of sympathetic vasoconstrictor nerves

Cardiovascular Regulation § Reflex Control of Cardiovascular Function § Cardiovascular centers monitor arterial blood § Baroreceptor reflexes: – respond to changes in blood pressure § Chemoreceptor reflexes: – respond to changes in chemical composition, particularly p. H and dissolved gases
Cardiovascular Regulation § Baroreceptor Reflexes § Stretch receptors in walls of § Carotid sinuses: maintain blood flow to brain § Aortic sinuses: monitor start of systemic circuit § Right atrium: monitors end of systemic circuit § When blood pressure rises, CV centers § Decrease cardiac output § Cause peripheral vasodilation § When blood pressure falls, CV centers § Increase cardiac output § Cause peripheral vasoconstriction
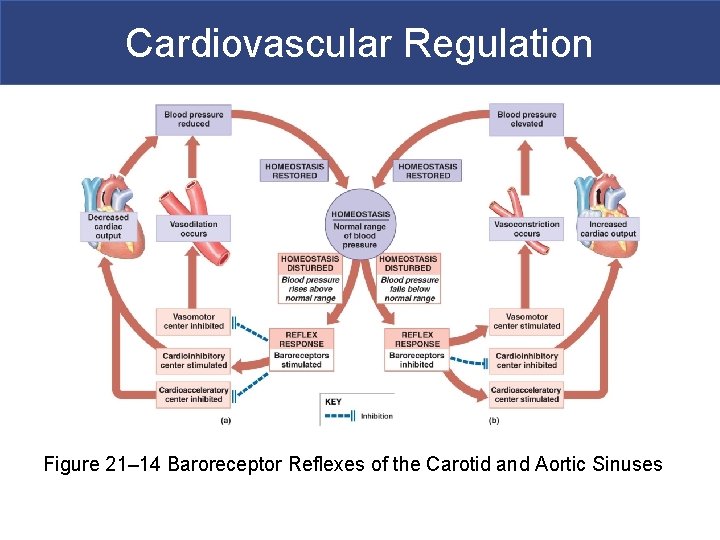
Cardiovascular Regulation Figure 21– 14 Baroreceptor Reflexes of the Carotid and Aortic Sinuses

Cardiovascular Regulation § Hormones and Cardiovascular Regulation § Hormones have short-term and long-term effects on cardiovascular regulation § For example, E and NE from suprarenal medullae stimulate cardiac output and peripheral vasoconstriction

Cardiovascular Regulation § Antidiuretic Hormone (ADH) § Released by neurohypophysis (posterior lobe of pituitary) § Elevates blood pressure § Reduces water loss at kidneys § ADH responds to § Low blood volume § High plasma osmotic concentration § Circulating angiotensin II

Cardiovascular Regulation § Angiotensin II § Responds to fall in renal blood pressure § Stimulates § Aldosterone production § ADH production § Thirst § Cardiac output § Peripheral vasoconstriction
Cardiovascular Regulation § Erythropoietin (EPO) § Released at kidneys § Responds to low blood pressure, low O 2 content in blood § Stimulates red blood cell production
Cardiovascular Regulation § Natriuretic Peptides § Atrial natriuretic peptide (ANP) § Produced by cells in right atrium § Brain natriuretic peptide (BNP) § Produced by ventricular muscle cells § Respond to excessive diastolic stretching § Lower blood volume and blood pressure § Reduce stress on heart
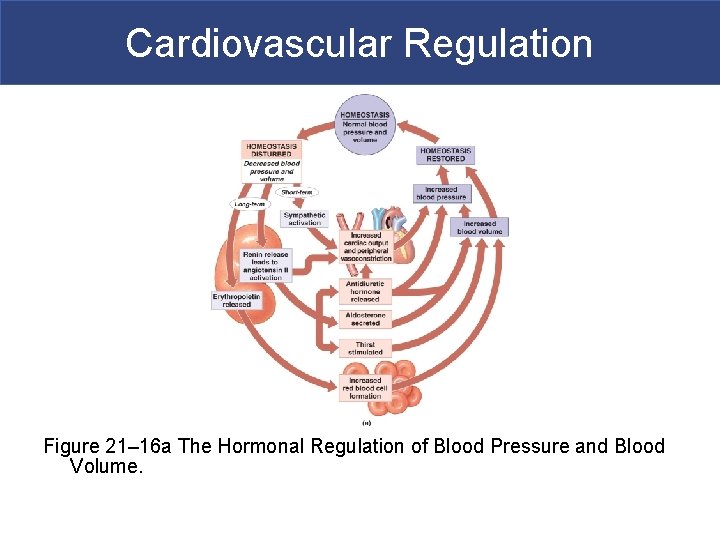
Cardiovascular Regulation Figure 21– 16 a The Hormonal Regulation of Blood Pressure and Blood Volume.
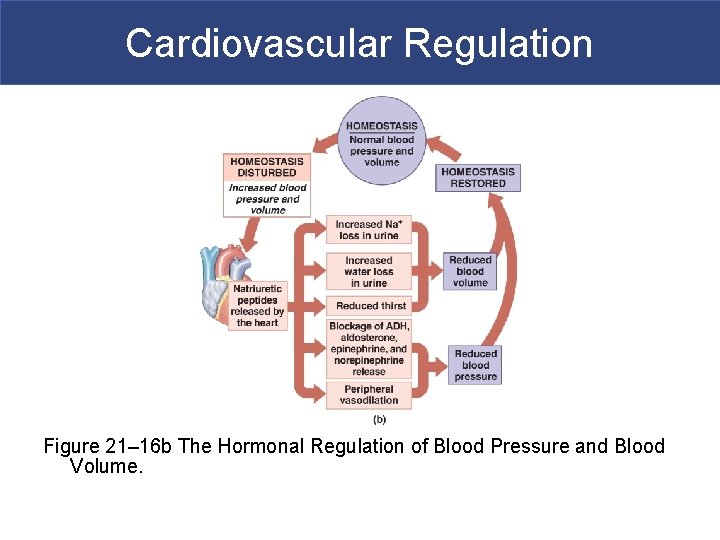
Cardiovascular Regulation Figure 21– 16 b The Hormonal Regulation of Blood Pressure and Blood Volume.
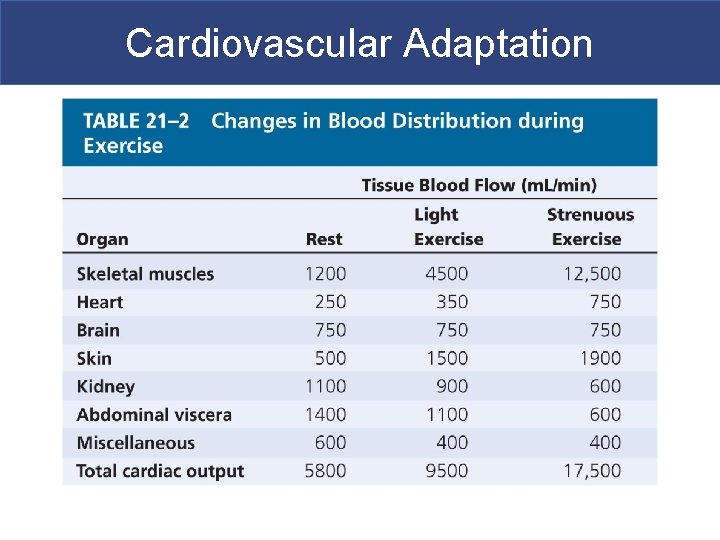
Cardiovascular Adaptation
Cardiovascular Adaptation § Short-Term Elevation of Blood Pressure § Carotid and aortic reflexes § Increase cardiac output (increasing heart rate) § Cause peripheral vasoconstriction § Sympathetic nervous system § Triggers hypothalamus § Further constricts arterioles § Venoconstriction improves venous return
Cardiovascular Adaptation § Short-Term Elevation of Blood Pressure § Hormonal effects § Increase cardiac output § Increase peripheral vasoconstriction (E, NE, ADH, angiotensin II)
Cardiovascular Adaptation § Long-Term Restoration of Blood Volume § Recall of fluids from interstitial spaces § Aldosterone and ADH promote fluid retention and reabsorption § Thirst increases § Erythropoietin stimulates red blood cell production
Cardiovascular Adaptation § Blood Flow to the Brain § Is top priority § Brain has high oxygen demand § When peripheral vessels constrict, cerebral vessels dilate, normalizing blood flow
Cardiovascular Adaptation § Stroke § Also called cerebrovascular accident (CVA) § Blockage or rupture in a cerebral artery § Stops blood flow
Cardiovascular Adaptation § Heart Attack § A blockage of coronary blood flow § Can cause § Angina (chest pain) § Tissue damage § Heart failure § Death
Cardiovascular Adaptation § Blood Flow to the Lungs § Regulated by O 2 levels in alveoli § High O 2 content § Vessels dilate § Low O 2 content § Vessels constrict
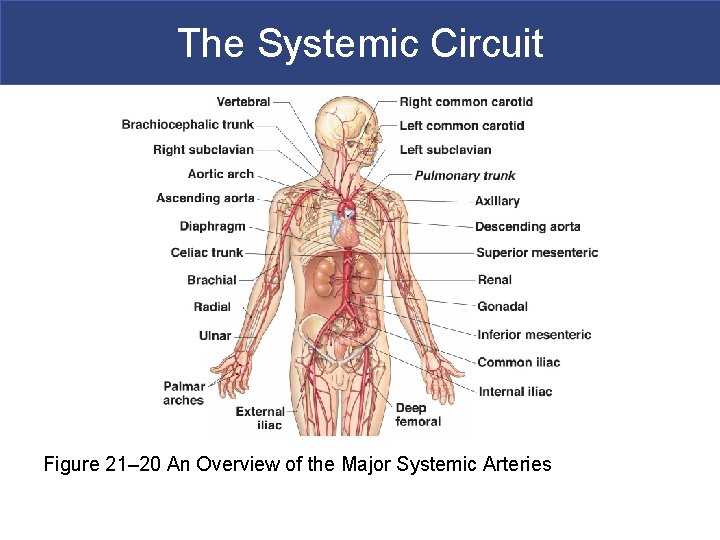
The Systemic Circuit Figure 21– 20 An Overview of the Major Systemic Arteries
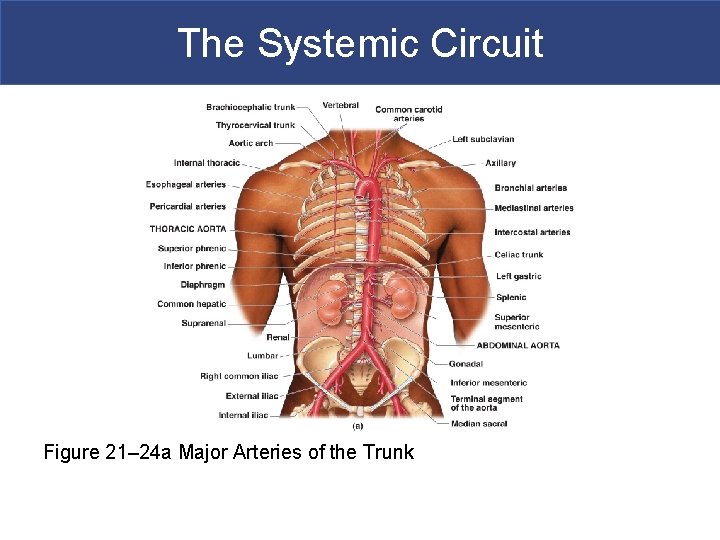
The Systemic Circuit Figure 21– 24 a Major Arteries of the Trunk
Aging and the Cardiovascular System § Three Age-Related Changes in Blood § Decreased hematocrit § Peripheral blockage by blood clot (thrombus) § Pooling of blood in legs § Due to venous valve deterioration
Aging and the Cardiovascular System § Five Age-Related Changes in the Heart § Reduced maximum cardiac output § Changes in nodal and conducting cells § Reduced elasticity of cardiac (fibrous) skeleton § Progressive atherosclerosis § Replacement of damaged cardiac muscle cells by scar tissue
Aging and the Cardiovascular System § Three Age-Related Changes in Blood Vessels § Arteries become less elastic § Pressure change can cause aneurysm § Calcium deposits on vessel walls § Can cause stroke or infarction § Thrombi can form § At atherosclerotic plaques
- Slides: 108