Cardio Monday Oct 2005 Approach to narrow QRS

































- Slides: 90


Cardio. Monday Oct. 2005 Approach to narrow QRS tachycardias EL-SAYED M. FARAG (Msc. Cardiology)

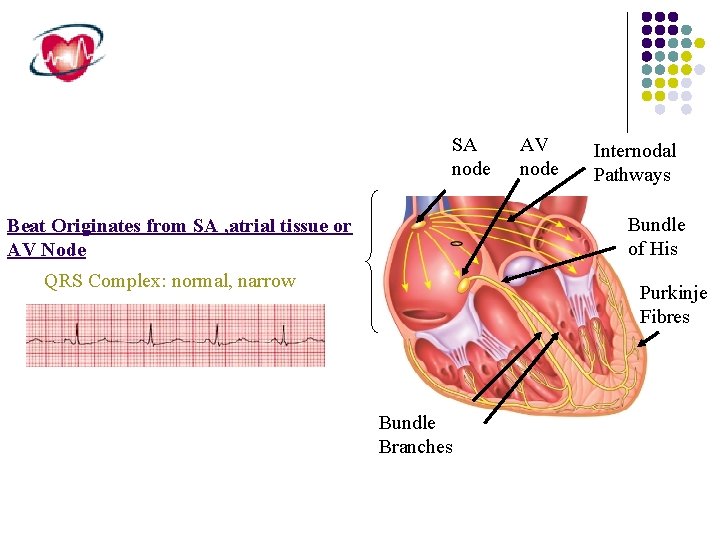
Definiton Narrow QRS complex tachycardias(NCT) are defined as tachyarrhythmias with a rate faster than 100 beats/minute and a QRS duration of 120 msec (0. 12 sec) or less, as demonstrated on the electrocardiogram (ECG) or cardiac The normal QRS duration reflects normally synchronous activation of both ventricles through the His bundle, bundle branches, and terminal Purkinje conduction system.

SA node AV node Internodal Pathways Bundle of His Beat Originates from SA , atrial tissue or AV Node QRS Complex: normal, narrow Purkinje Fibres Bundle Branches

The narrow QRS complex tachycardias include: § Sinus tachycardia (ST) § Inappropriate sinus tachycardia (IST) § Sinoatrial nodal reentrant tachycardia (SNRT) § Atrial tachycardia (AT) § Multifocal atrial tachycardia (MAT) § Atrial fibrillation (AF) § Atrial flutter (AFl) § Junctional ectopic tachycardia (JET) § Nonparoxysmal junctional tachycardia (NPJT) § Atrioventricular nodal reentrant tachycardia (AVNRT) § Atrioventricular reentrant tachycardia (AVRT)


Mechanisms Altered automaticity Triggered activity Reentry

1. Altered Automaticity Hypothermia decrease, hyperthermia increase phase 4 slope Hypoxia & hypercapnia both increase phase 4 slope Cardiac dilation increases phase 4 slope Local areas of ischemia or necrosis increases automaticity of neighboring cells Hypokalemia increases phase 4 slope, increases ectopics, prolongs repolarization Hyperkalemia decreases phase 4 slope; slow conduction, blocks

2. Triggered Activity Afterdepolarization reaches threshold § Early: interrupt repolarization § Delayed: after completion of AP.

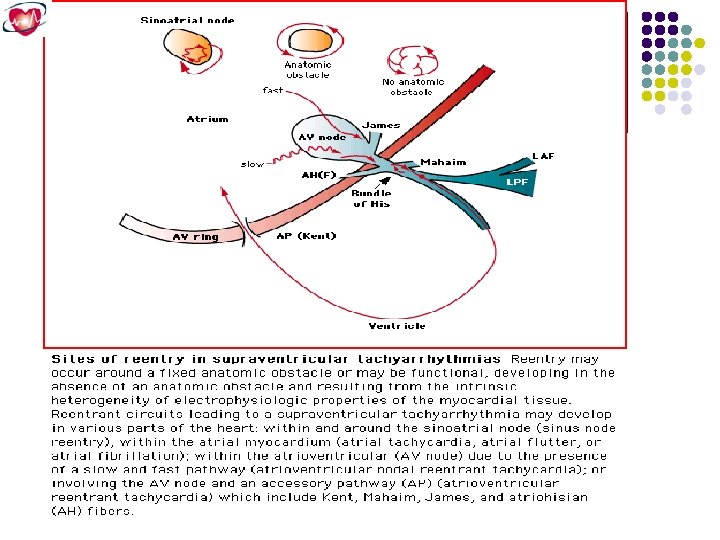
3. Reentry Requires: available circuit, unidirectional block, and different conduction speed in limbs of circuit Exp: WPW reciprocating tachycardia, AVnodal reentry, …. .


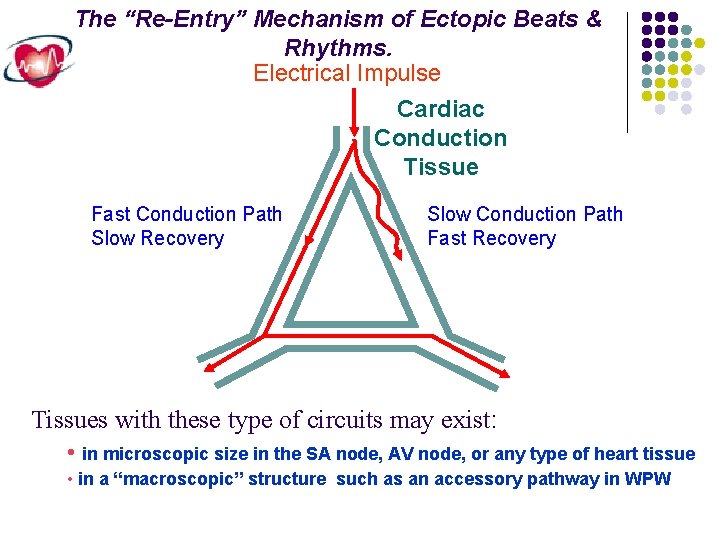
The “Re-Entry” Mechanism of Ectopic Beats & Rhythms. Electrical Impulse Cardiac Conduction Tissue Fast Conduction Path Slow Recovery Slow Conduction Path Fast Recovery Tissues with these type of circuits may exist: • in microscopic size in the SA node, AV node, or any type of heart tissue • in a “macroscopic” structure such as an accessory pathway in WPW

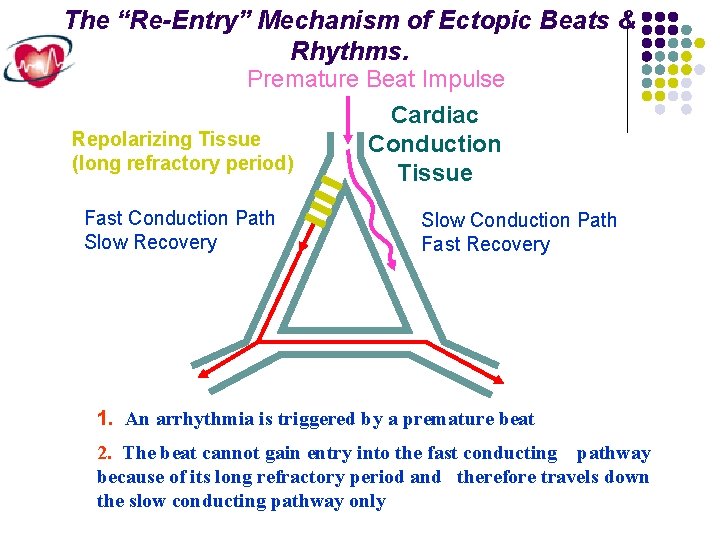
The “Re-Entry” Mechanism of Ectopic Beats & Rhythms. Premature Beat Impulse Cardiac Repolarizing Tissue Conduction (long refractory period) Tissue Fast Conduction Path Slow Recovery Slow Conduction Path Fast Recovery 1. An arrhythmia is triggered by a premature beat 2. The beat cannot gain entry into the fast conducting pathway because of its long refractory period and therefore travels down the slow conducting pathway only

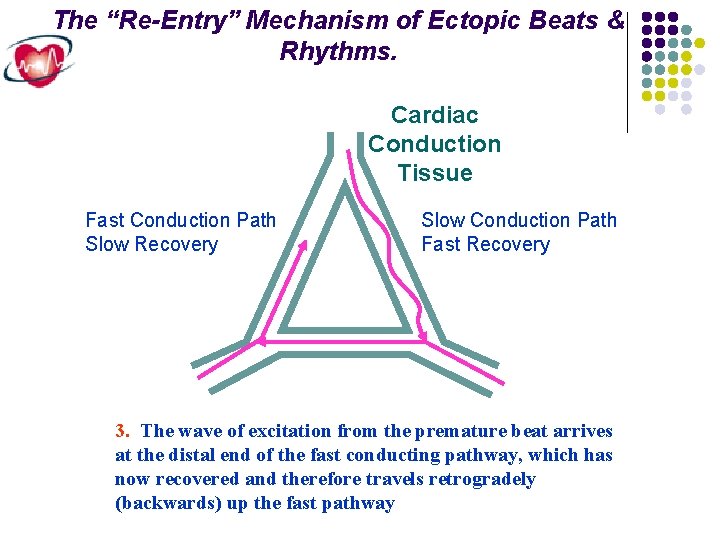
The “Re-Entry” Mechanism of Ectopic Beats & Rhythms. Cardiac Conduction Tissue Fast Conduction Path Slow Recovery Slow Conduction Path Fast Recovery 3. The wave of excitation from the premature beat arrives at the distal end of the fast conducting pathway, which has now recovered and therefore travels retrogradely (backwards) up the fast pathway

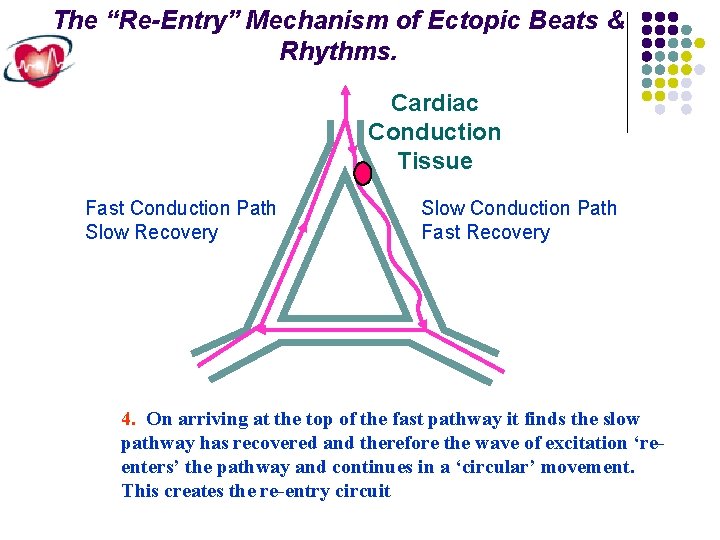
The “Re-Entry” Mechanism of Ectopic Beats & Rhythms. Cardiac Conduction Tissue Fast Conduction Path Slow Recovery Slow Conduction Path Fast Recovery 4. On arriving at the top of the fast pathway it finds the slow pathway has recovered and therefore the wave of excitation ‘reenters’ the pathway and continues in a ‘circular’ movement. This creates the re-entry circuit

NCT WORKUP ECG Lab. Workup ( CBC, TFT, s. electrolyte, 24 hour Holter monitor Continuous loop event recorder Echocardiogram Treadmill test ( with or after exercise)

ALL ARE NARROW BUT THE DIFFERENCE IS WIDE !!

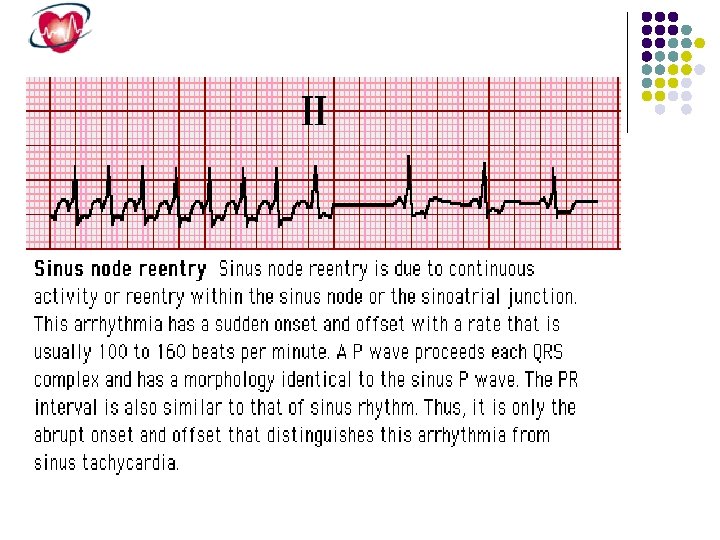
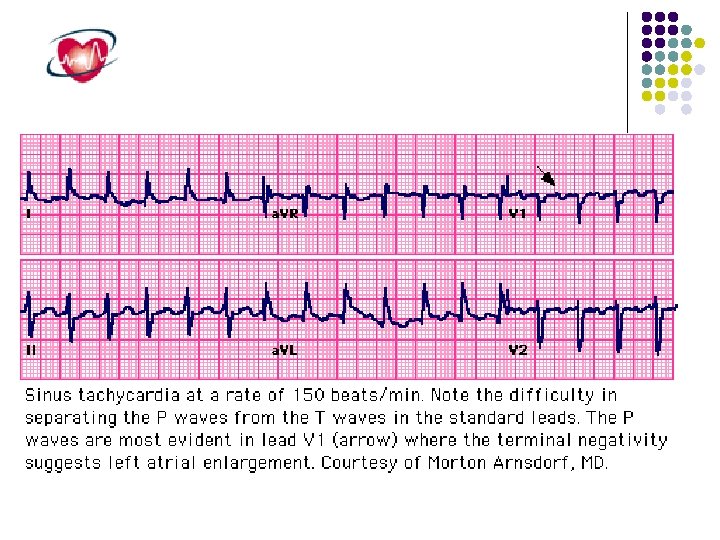
Tachycardias Arising From the Sinus Node Region Sinus tachycardia and Inappropriate sinus tachycardia Sinus node rentry tachycardia

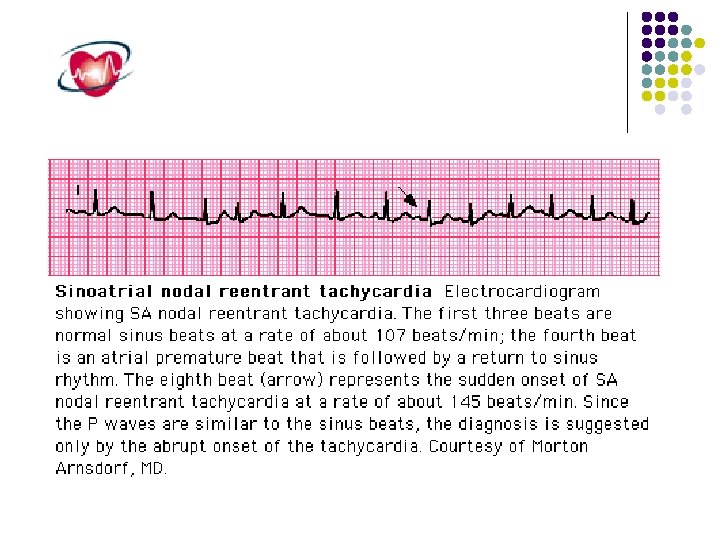
Sinus node reentry tachycardia arises from a reentrant circuit involving the sinus node, producing P waves that are fairly similar if not identical to those during sinus rhythm. sinus node reentry can be initiated and terminated abruptly by a premature atrial stimulus, which is consistent with its reentrant mechanism. It is usually nonsustained and associated with slower rates than inappropriate sinus tachycardia, making it clinically insignificant. Carotid sinus massage and other vagal maneuvers typically slow or terminate sinus node reentry.



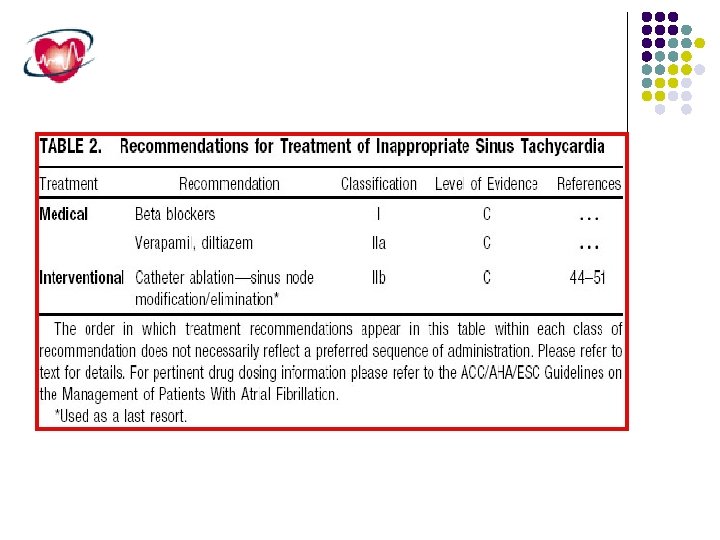
Inappropriate sinus tachycardia It is a clinical syndrome characterized by sinus tachycardia without an identifiable physiologic stimulus. Secondary causes for resting sinus tachycardia must be ruled out, such as anemia, hyperthyroidism, pheochromocytoma, and diabetes mellitus with autonomic dysfunction. At least two clinical variants have been described: (1) resting heart rate of 100 beats/min or greater and (2) increased heart rate response to minimal exertion. Sinus rates greater than 200 beats/min are not characteristic of inappropriate sinus tachycardia, and paroxysmal increases in heart rate are not seen. The mechanism of inappropriate sinus tachycardia is still speculative but is thought to be a primary abnormality of the sinus node complex characterized by a high intrinsic heart rate, beta-adrenergic hypersensitivity, and accentuation by a depressed cardiovagal reflex.


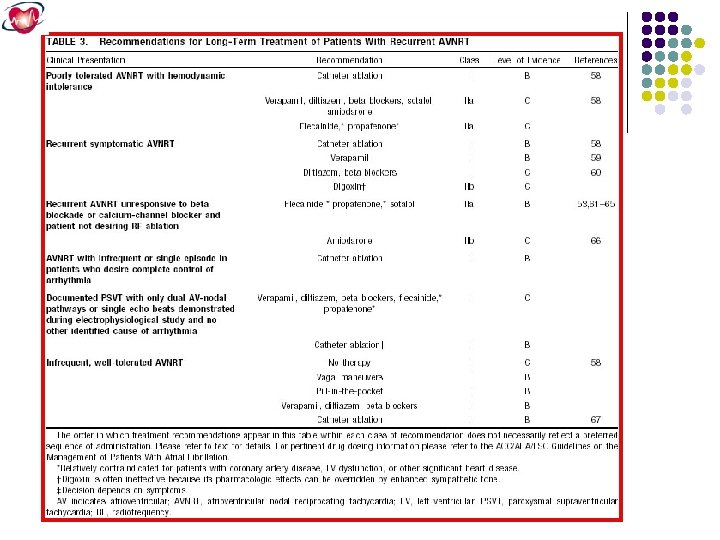
Atrioventricular Node Reentrant Tachycardia (AVNRT) The most common form of paroxysmal SVT is AV node reentrant tachycardia (AVNRT), which accounts for greater than 60% of cases referred to an electrophysiology laboratory. Patients typically present in their 30 s or 40 s, with greater than 70% being women. Although the mechanism for AVNRT is reentry involving the AV node, the precise location of the reentrant circuit is uncertain but includes atrial tissue surrounding the AV node. The reentrant circuit consists of an anterograde limb and a retrograde limb.

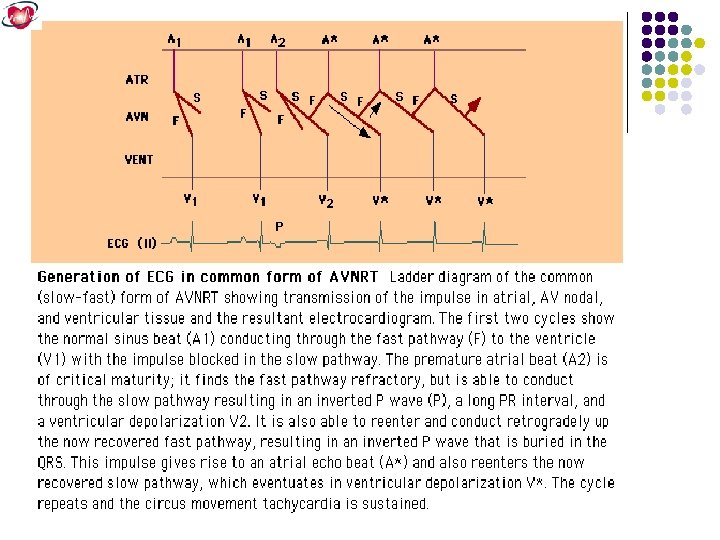
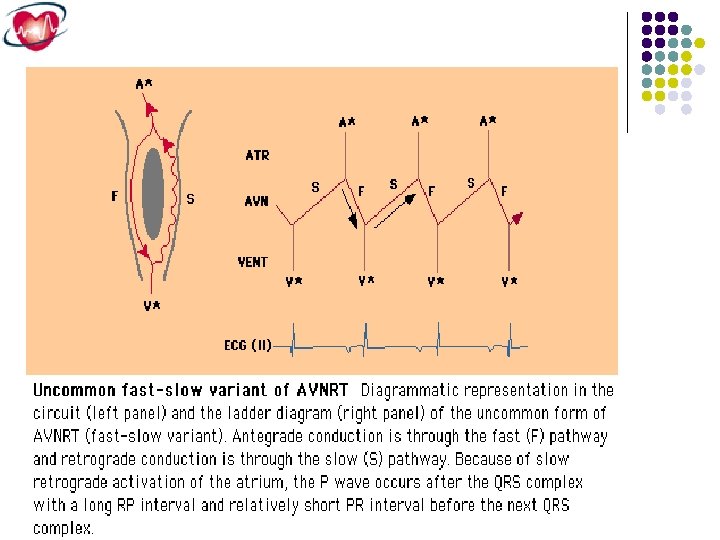
Types of AVNRT Common (Slow – Fast). Uncommon : *Fast-Slow *Slow-Slow



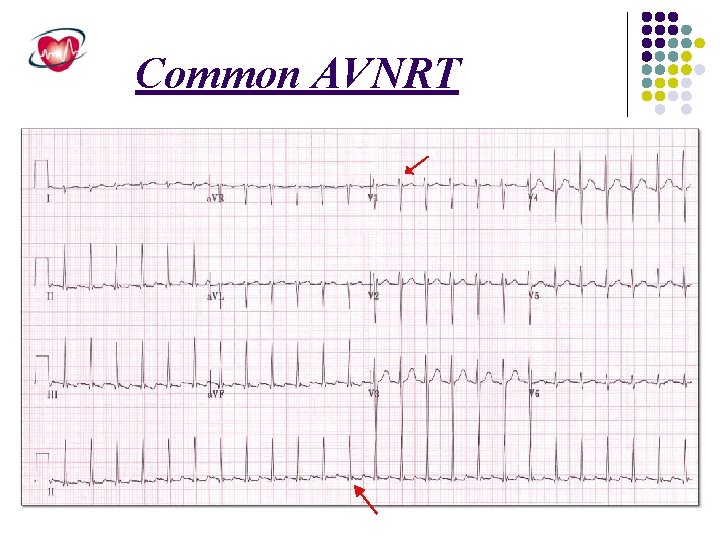
Common AVNRT

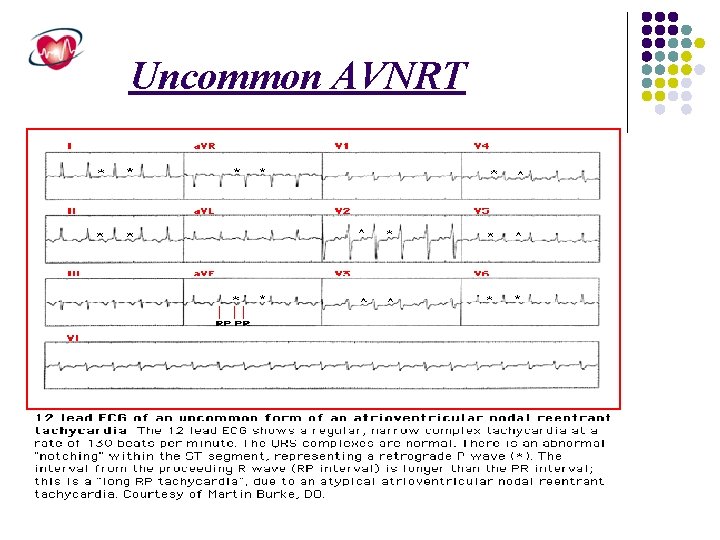
Uncommon AVNRT

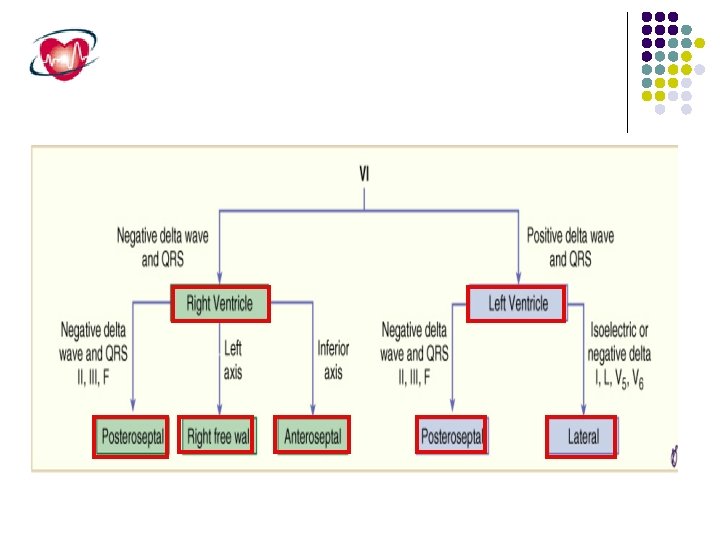
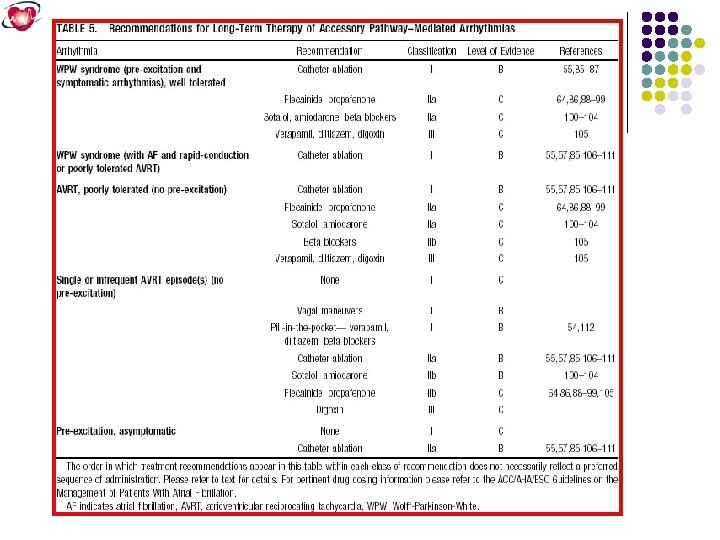
Atrioventricular Reentrant Tachycardia Mediated by Accessory Pathways. The second most common form of paroxysmal SVT is AV reentrant tachycardia (AVRT) using an accessory pathway Accessory pathways are discrete bundles of myocardial tissue bridging the atrium and ventricle along the tricuspid or mitral valve annulus. More than half of accessory pathways are situated in the left free wall, 20% to 30% occur in the posteroseptal location, 10% to 20% occur in the right free wall, and 5% to 10% occur in the anteroseptal location near the AV node.

Because the accessory pathway conducts more rapidly than the normal conduction system, the ventricle is producing a short P-R interval and a delta wave on the surface ECG. In contrast, about 25% of accessory pathways conduct only retrogradely and are not manifest on the ECG during sinus rhythm (Concealed accessory pathway).

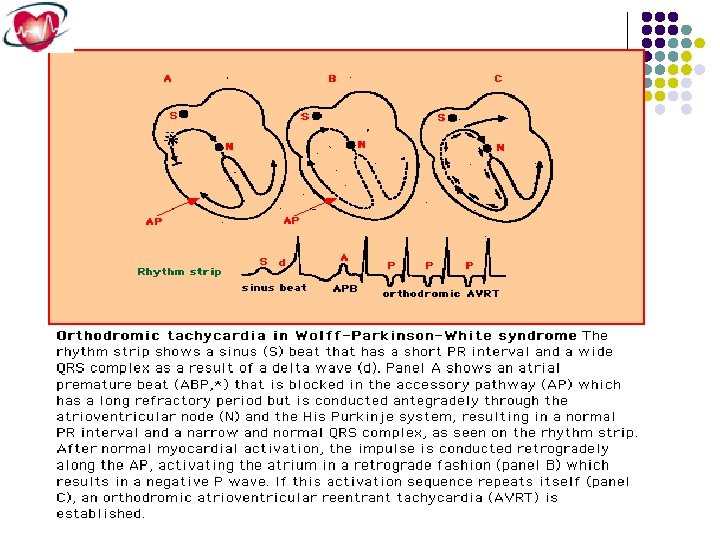
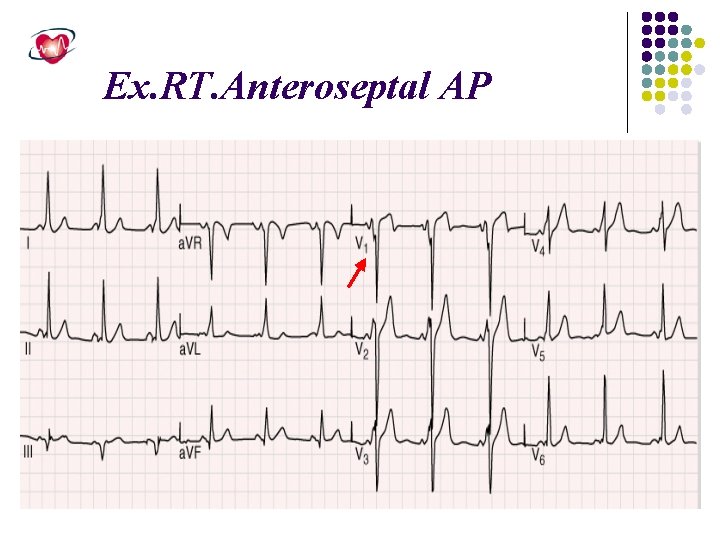
Orthodromic atrioventricular reentrant tachycardia involving an accessory pathway, the tachycardia is narrow complex because of anterograde conduction down the AV node and His-Purkinje system. Retrograde atrial activation over the accessory pathway results in a P wave within the early ST segment.



Ex. RT. Anteroseptal AP

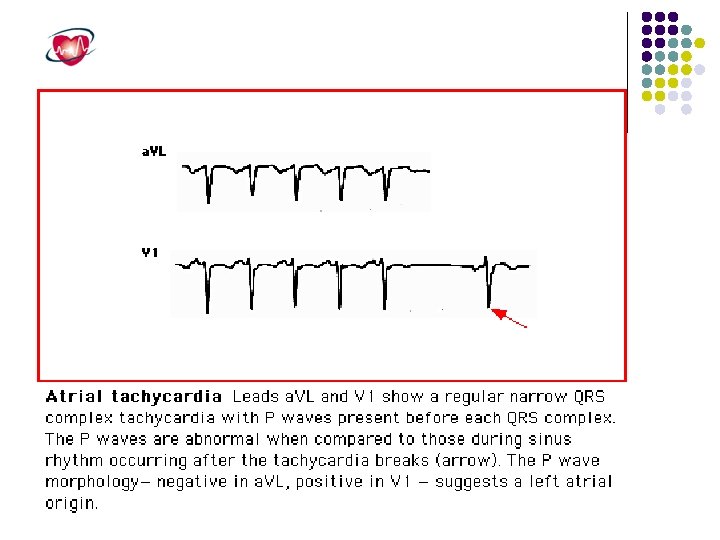
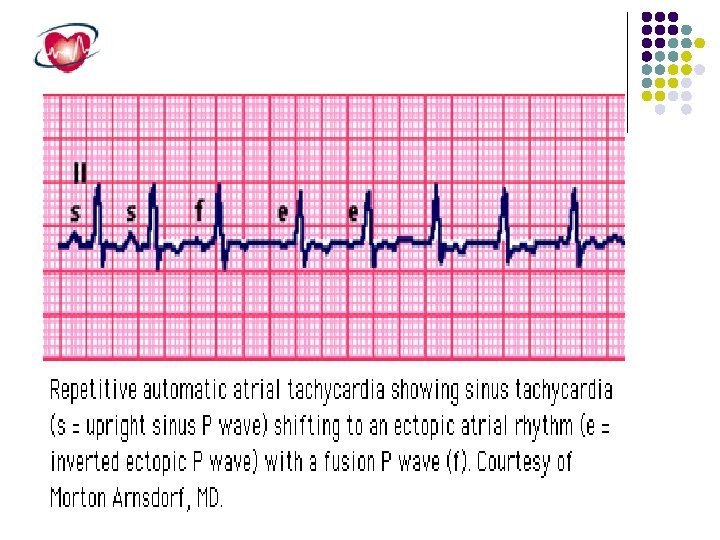
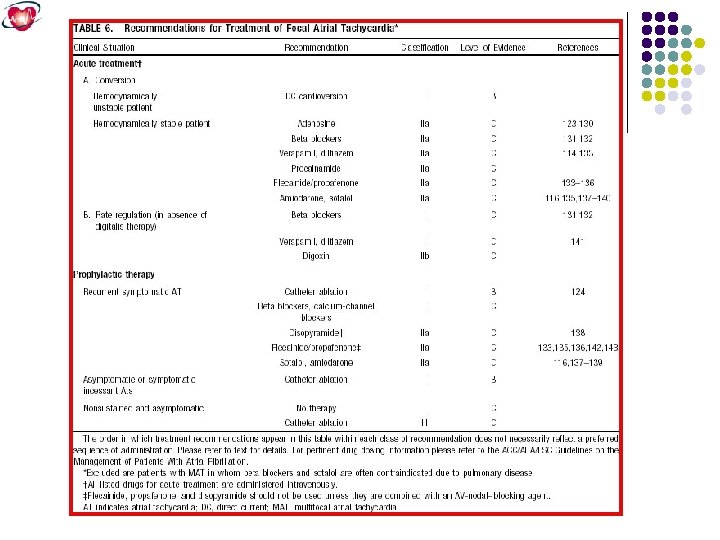
Atrial Tachycardia Atrial tachycardia is less common than AVNRT or AVRT, accounting for fewer than 15% of patients referred for electrophysiology study. It can occur in the pediatric population, especially in children with surgically corrected congenital heart disease. Atrial tachycardia usually arises from a single localized atrial focus.



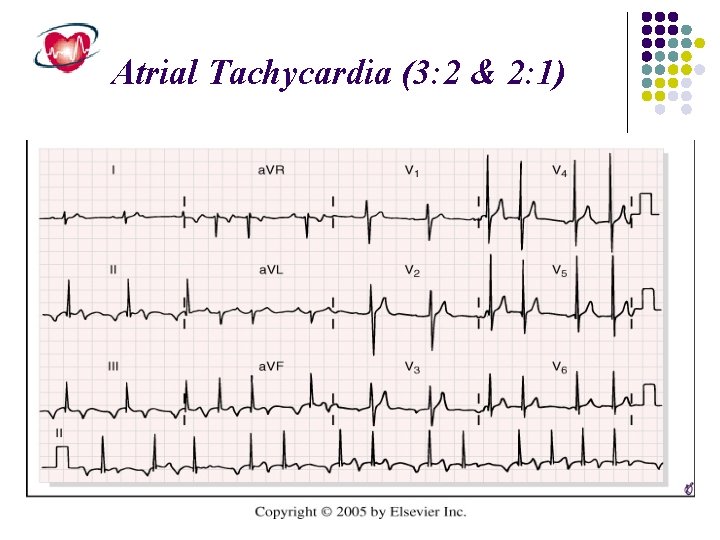
Atrial Tachycardia (3: 2 & 2: 1)

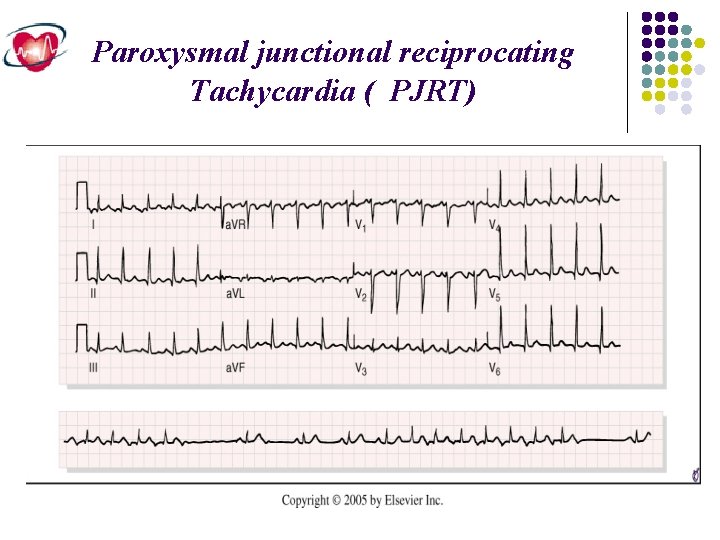
Paroxysmal junctional reciprocating Tachycardia ( PJRT)

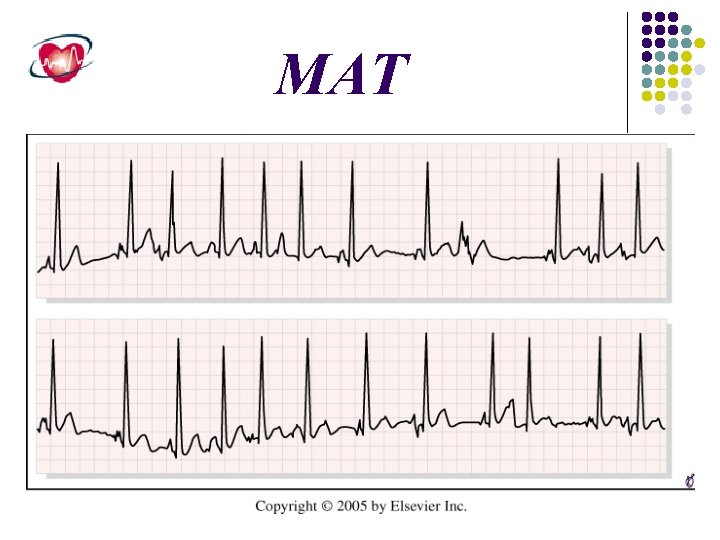
Multifocal atrial tachycardia (MAT) Multifocal atrial tachycardia is a rare SVT. It involves more than one atrial focus and requires at least three distinct P wave morphologies to be diagnosed on the surface ECG. Because the foci fire independently of one another, the atrial rate is irregular and typically averages 100 beats/min. The P-R interval also may vary depending on the location of the foci relative to the AV node The mechanism for multifocal atrial tachycardia has not been defined clearly but may be due to enhanced automaticity or triggered activity. Most patients with this arrhythmia have exacerbations of severe underlying pulmonary disease with hypoxia.

MAT

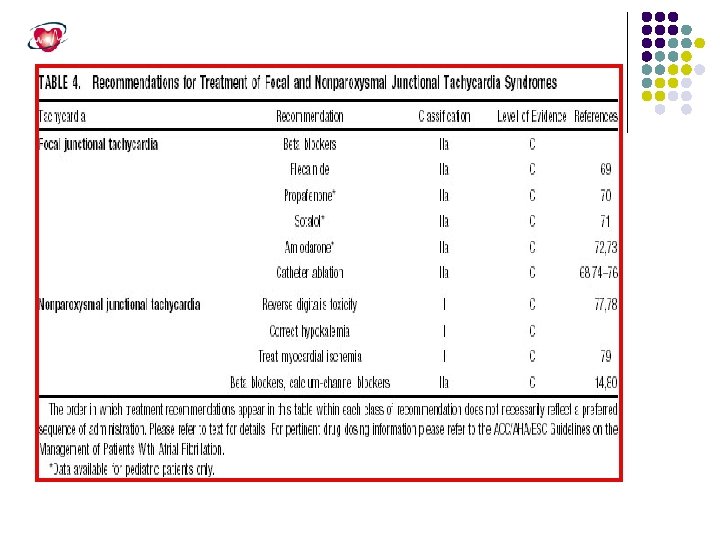
Jnctional Tachycardia Junctional tachycardias arise from a discrete focus within the AV node or the His bundle. In the pediatric population, junctional tachycardia also is known as junctional ectopic tachycardia. Junctional ectopic tachycardia presenting before 6 months of age usually is associated with underlying heart disease that carries a high mortality. In contrast, adult junctional tachycardia has a more benign prognosis and typically develops after the acute phase of myocardial infarction, digitalis intoxication, and acute myocarditis. Although the precise mechanism for junctional tachycardia has not been defined, it is likely due to enhanced impulse initiation in the region of the AV node by automaticity or triggered activity rather than reentry

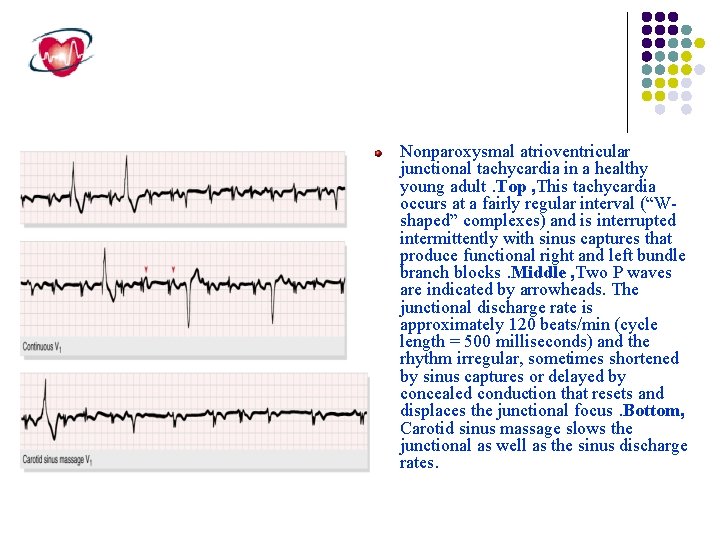
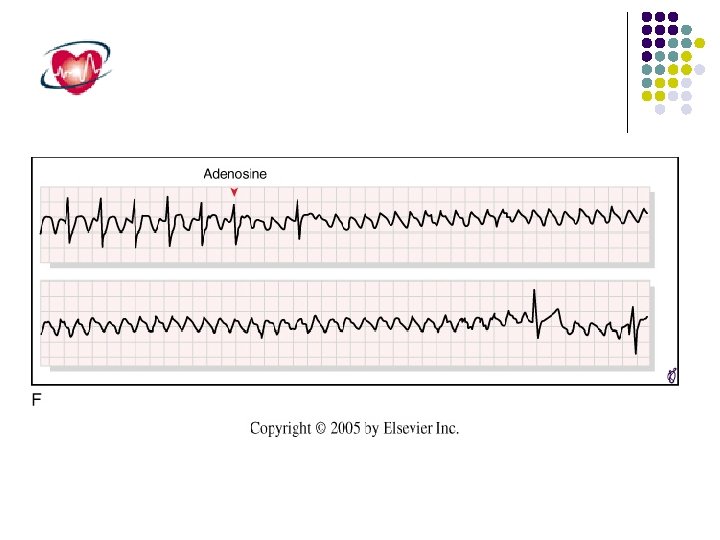
Nonparoxysmal atrioventricular junctional tachycardia in a healthy young adult. Top , This tachycardia occurs at a fairly regular interval (“Wshaped” complexes) and is interrupted intermittently with sinus captures that produce functional right and left bundle branch blocks. Middle , Two P waves are indicated by arrowheads. The junctional discharge rate is approximately 120 beats/min (cycle length = 500 milliseconds) and the rhythm irregular, sometimes shortened by sinus captures or delayed by concealed conduction that resets and displaces the junctional focus. Bottom, Carotid sinus massage slows the junctional as well as the sinus discharge rates.

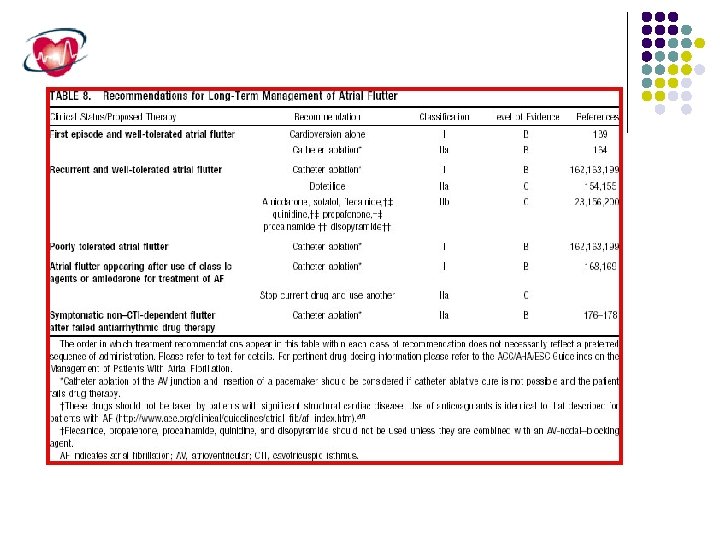
Atrial Flutter Atrial flutter is an atrial arrhythmia characterized by a regular rate, a uniform morphology, and a rate greater than 240 beats/min. Atrial flutter is usually accompanied by a fixed 2: 1 ventricular response, and it is this rapid ventricular response that results in most symptoms. Atrial flutter may be observed transiently after cardiac surgery or may persist for months to years. Many different forms of atrial flutter exist, which has led to multiple classification schemes.

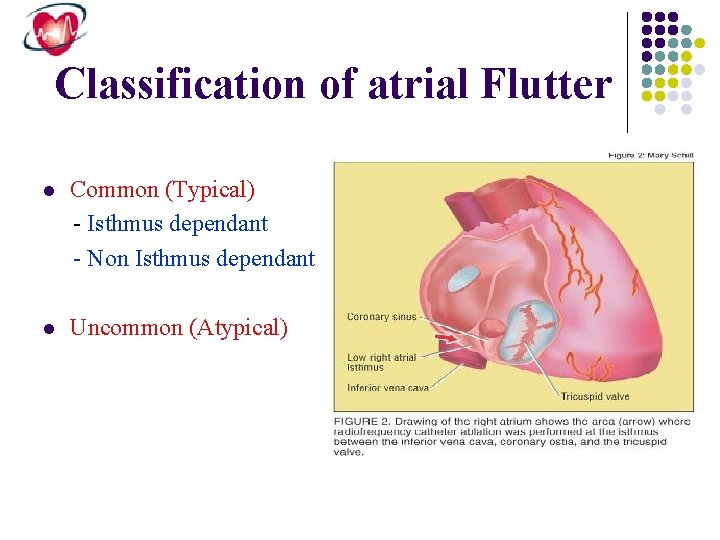
Classification of atrial Flutter l Common (Typical) - Isthmus dependant - Non Isthmus dependant l Uncommon (Atypical)


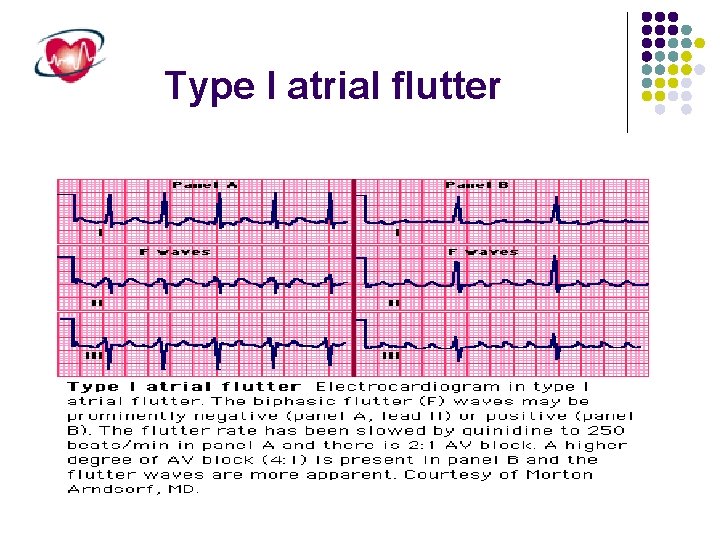
Type I atrial flutter

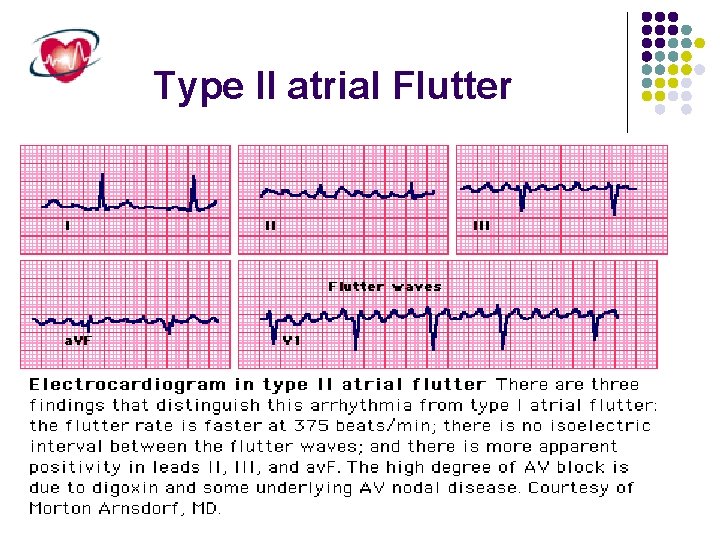
Type II atrial Flutter

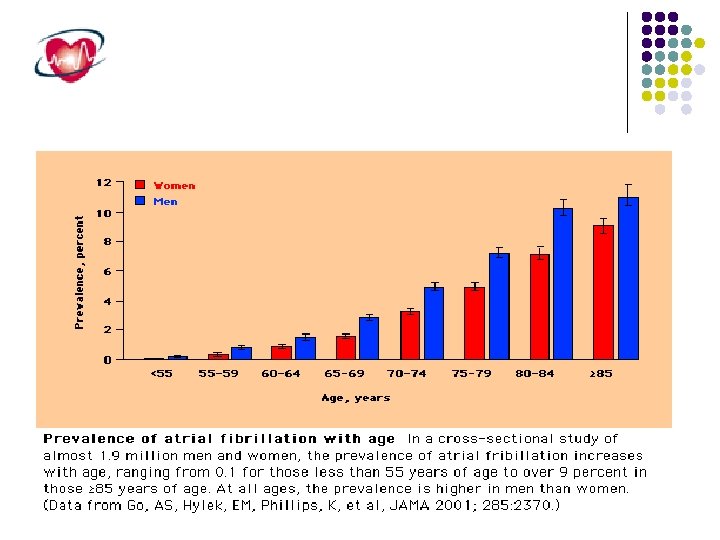
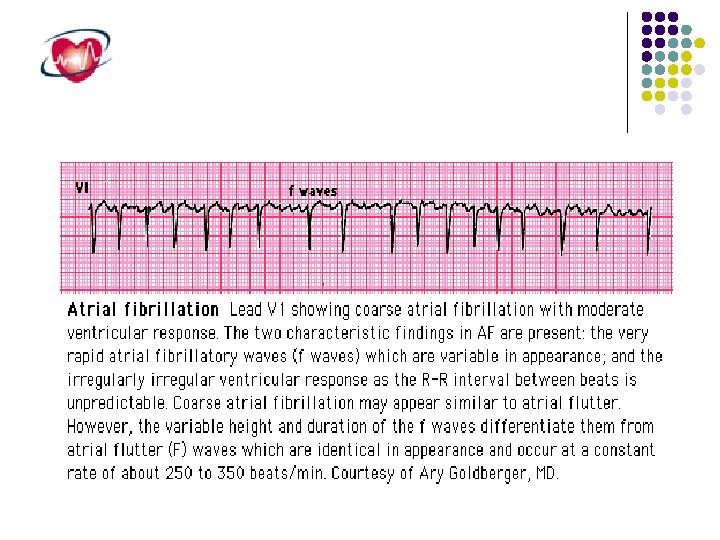
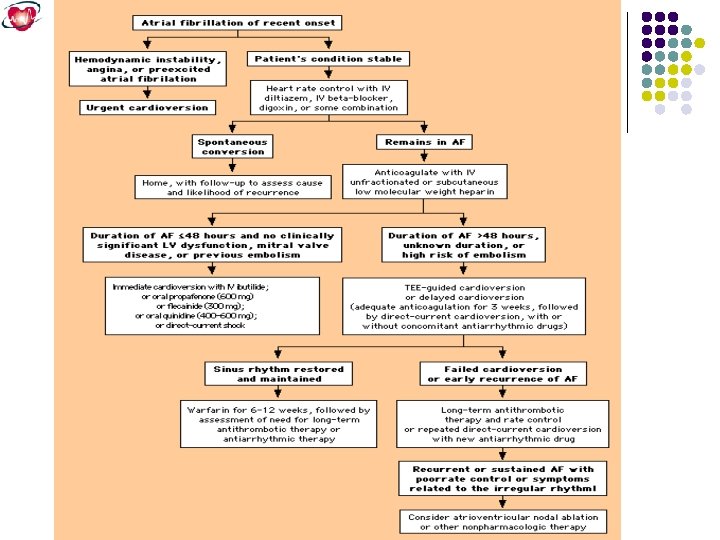
Atrial Fibrillation Atrial fibrillation )AF) is the most common sustained cardiac rhythm disturbance occuring in approximately 0. 4 to 1% of general population with increasing prevelance with age (10% over 80 years( AF may be : Primary, no underlying disease Secondary to: HPT, IHD, MVD Increased Morbidity Embolic complications )stroke( Reduced cardiac function; hemodynamic changes Complaints and symptoms Increased mortality . . . …


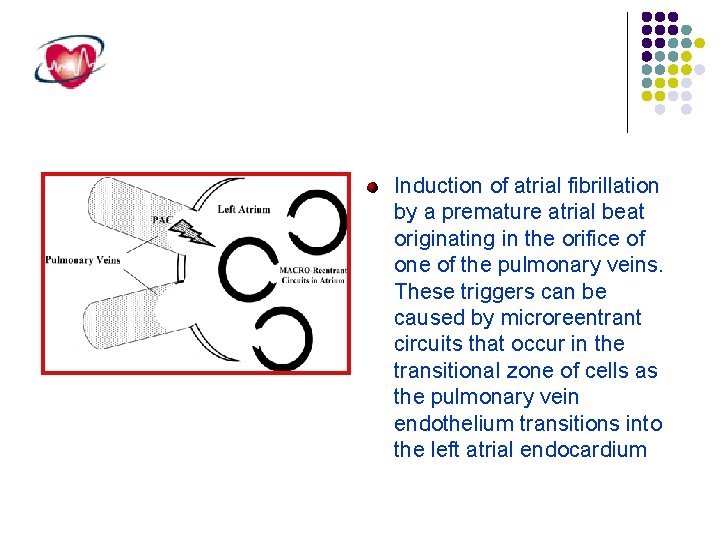
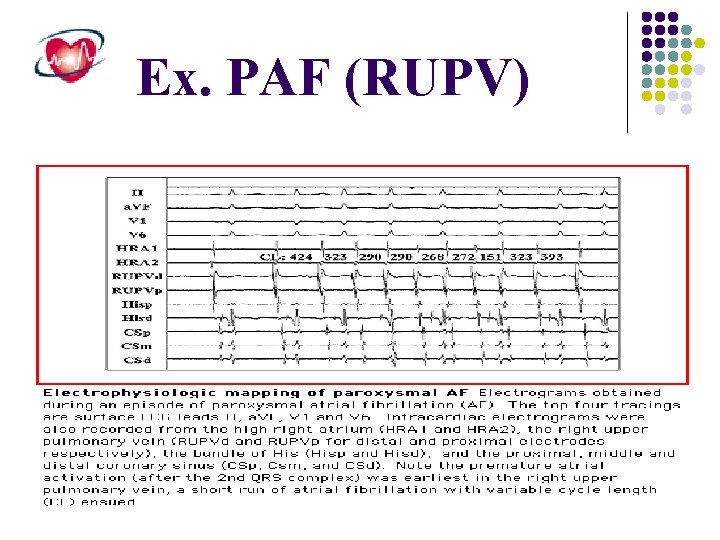
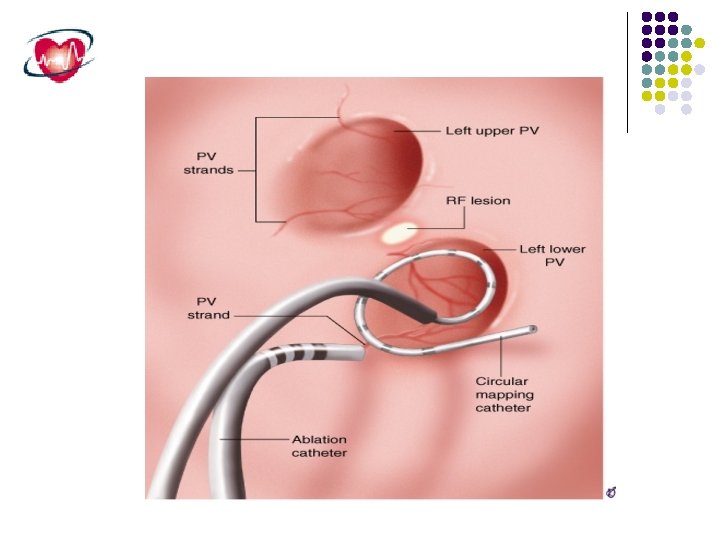
Induction of atrial fibrillation by a premature atrial beat originating in the orifice of one of the pulmonary veins. These triggers can be caused by microreentrant circuits that occur in the transitional zone of cells as the pulmonary vein endothelium transitions into the left atrial endocardium

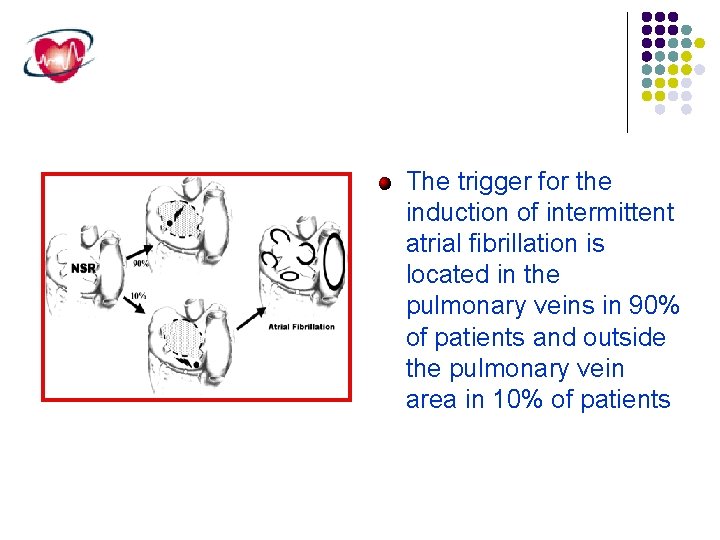
The trigger for the induction of intermittent atrial fibrillation is located in the pulmonary veins in 90% of patients and outside the pulmonary vein area in 10% of patients


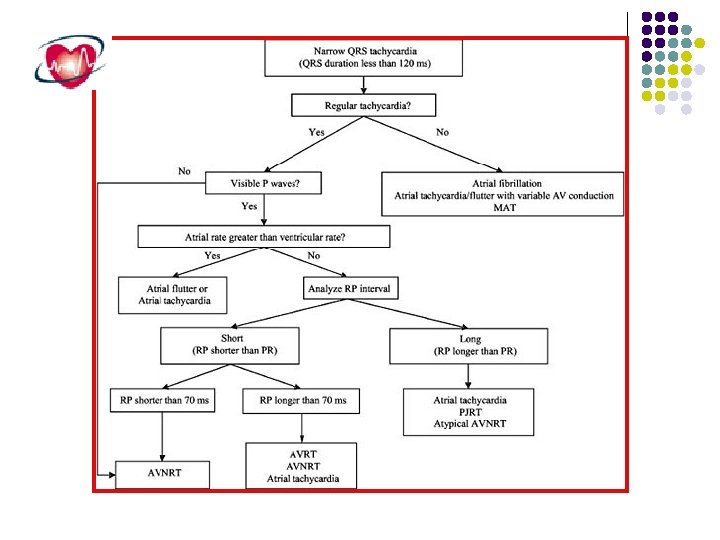
IT IS TOO WIDE HOW TO NARROW? ?





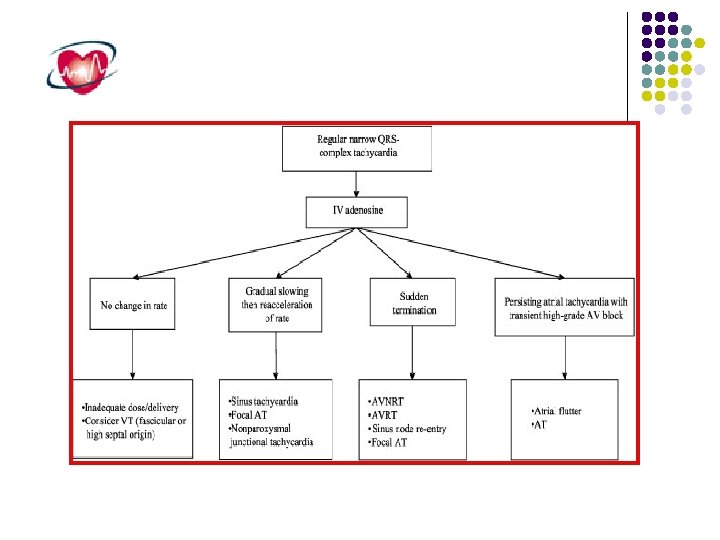
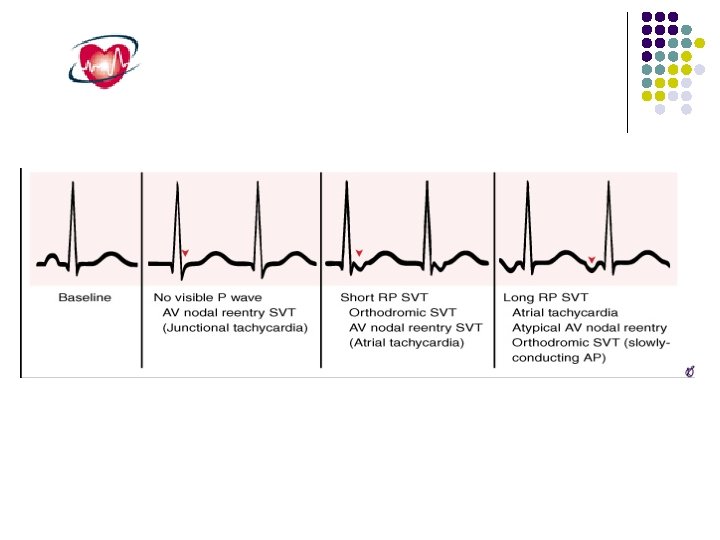
Take home messege l Observe either the onest or the termination. l Note the P , PR and RP. l Do vagal maneuver and adenosine.

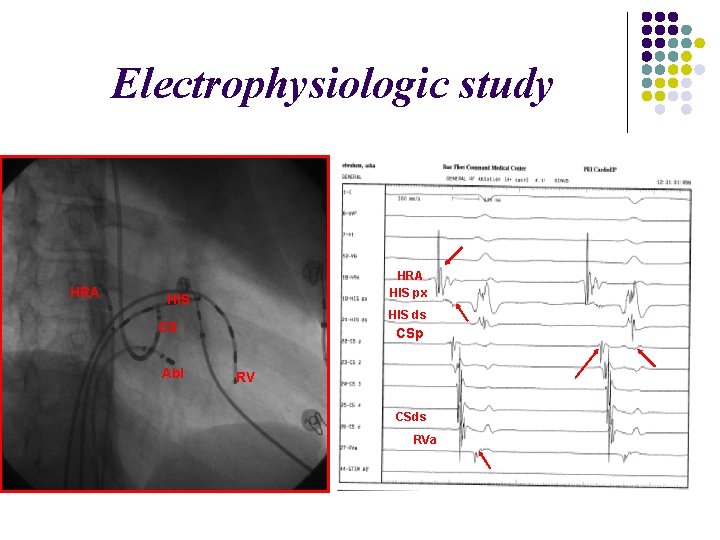
STILL VAGUE? EPS


Electrophysiologic study HRA HIS px HIS ds CS Abl CSp RV CSds RVa

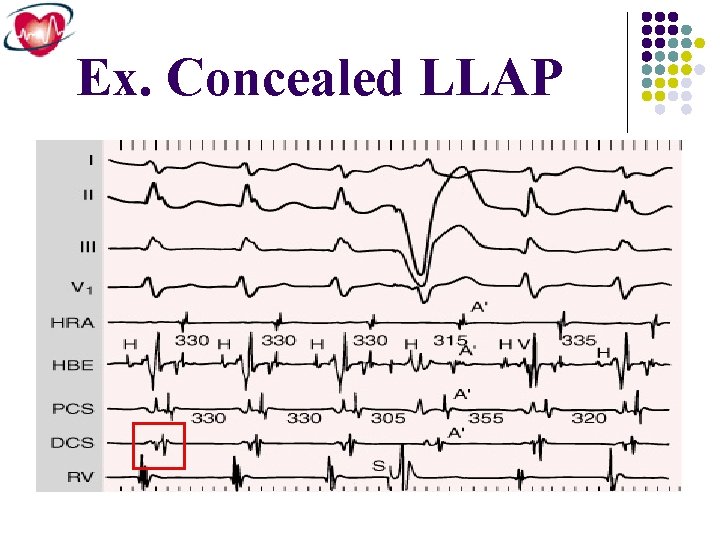
Ex. Concealed LLAP

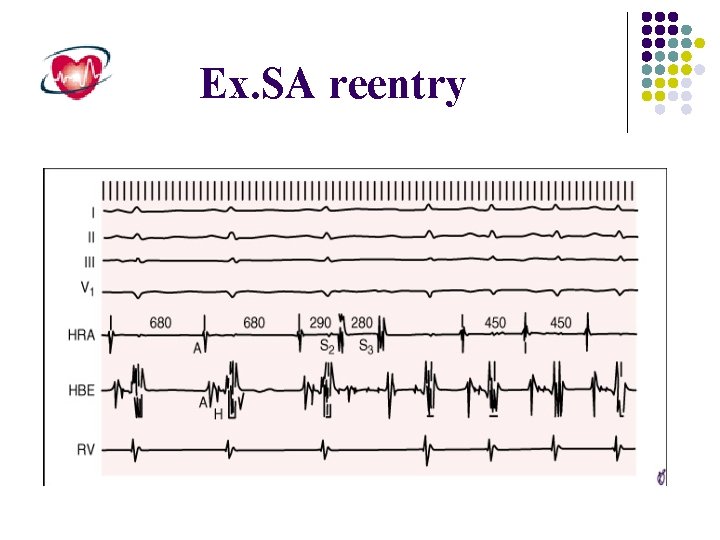
Ex. SA reentry

Ex. PAF (RUPV)

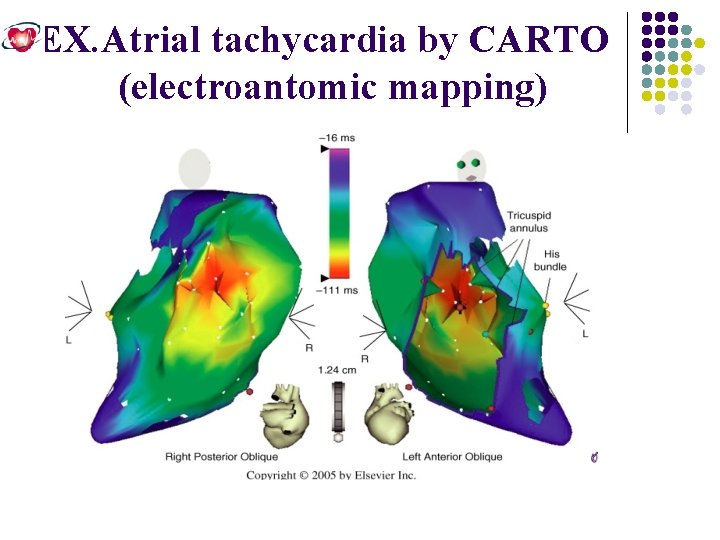
EX. Atrial tachycardia by CARTO (electroantomic mapping)

HOW TO TREAT?

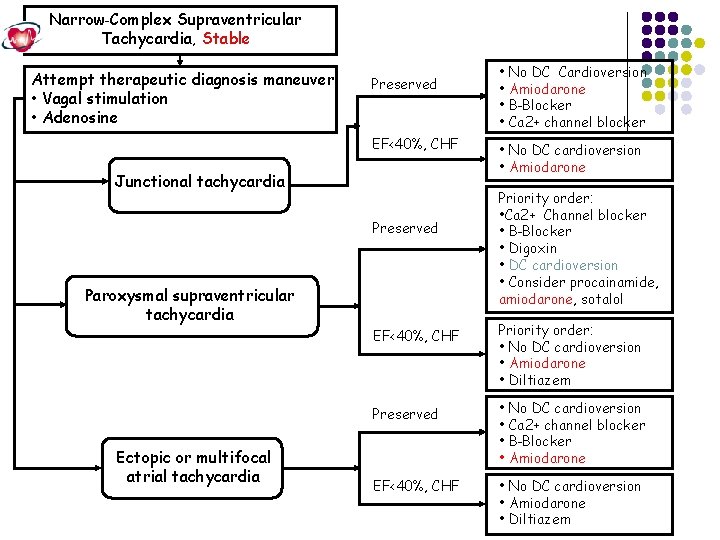
Narrow-Complex Supraventricular Tachycardia, Stable Attempt therapeutic diagnosis maneuver • Vagal stimulation • Adenosine Preserved EF<40%, CHF Junctional tachycardia Preserved Paroxysmal supraventricular tachycardia Ectopic or multifocal atrial tachycardia • No DC Cardioversion • Amiodarone • B-Blocker • Ca 2+ channel blocker • No DC cardioversion • Amiodarone Priority order: • Ca 2+ Channel blocker • B-Blocker • Digoxin • DC cardioversion • Consider procainamide, amiodarone, sotalol EF<40%, CHF Priority order: • No DC cardioversion • Amiodarone • Diltiazem Preserved • No DC cardioversion • Ca 2+ channel blocker • B-Blocker • Amiodarone EF<40%, CHF • No DC cardioversion • Amiodarone • Diltiazem












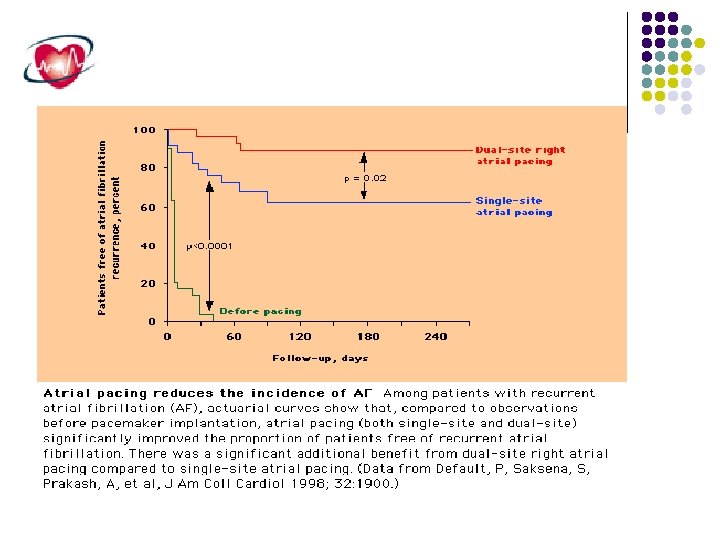
Non Pharmacologic AF therapy Catheter ablation. Atrial pacing (single or dual site pacing). Intraatrial ICD.



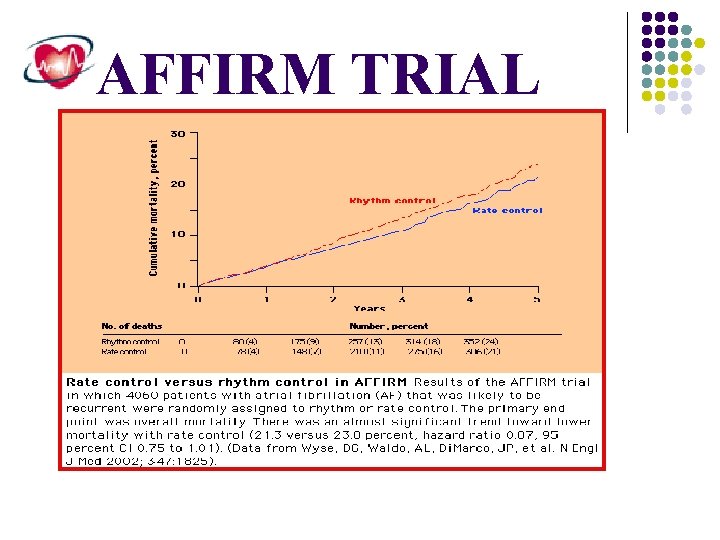
AFFIRM TRIAL

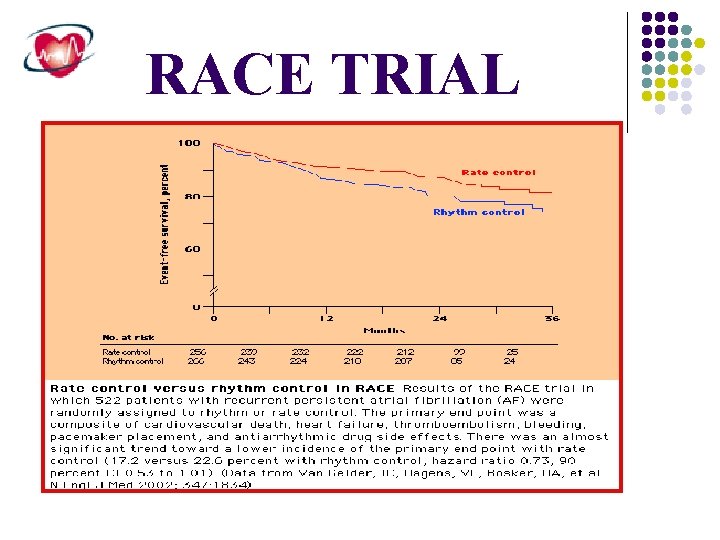
RACE TRIAL

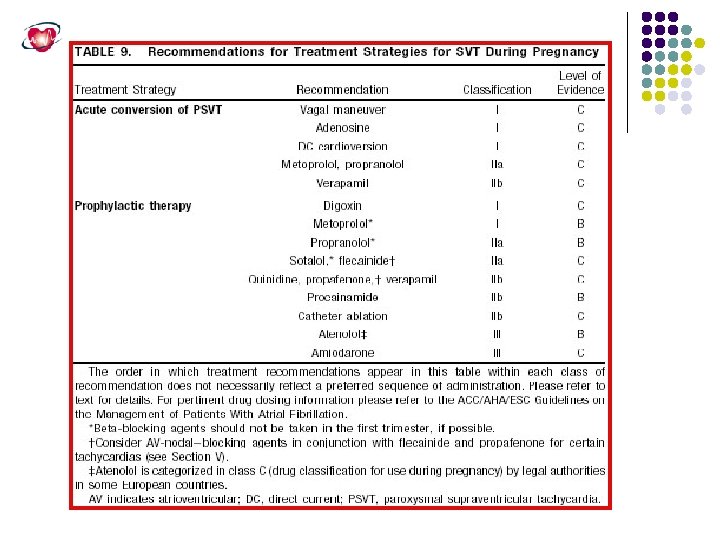
SPECIAL GROUP NEEDS SPECIAL TREATMENT



WHAT IS COLOUR OF THIS TISSUE? ? ? !!

Thank You