CARDIAC RHYTHM ABNORMALITIES Dr T A DIALLO Cardiologist

CARDIAC RHYTHM ABNORMALITIES Dr T A DIALLO Cardiologist EFSTH

Definition • Arrhythmias are cardiac rhythm abnormalities, that is, rhythms differing from the normal sinus rhythm, which is characterized by heart rates ranging from 60 to 100 beats per minute (bpm). When the rate falls below 60 bpm, the patient is said to have a bradyarrhythmia, whereas rates above 100 bpm are referred to as tachyarrhythmias. • Electrocardiographic analysis of an arrhythmia is not limited, however, to heart rate (increased versus decreased): it also includes the rhythm (which can be regular or irregular), the origin (supraventricular versus ventricular), and the morphology of the QRS complex (narrow versus wide)
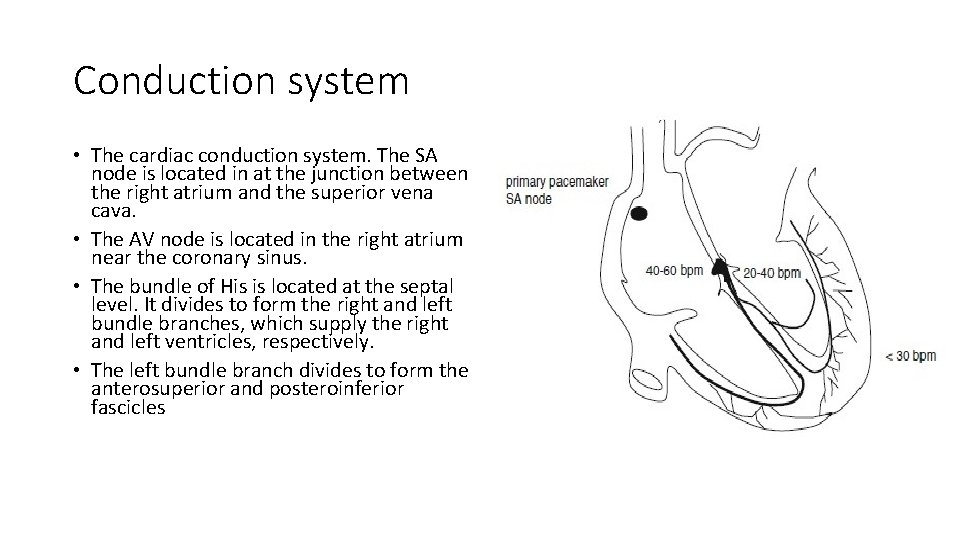
Conduction system • The cardiac conduction system. The SA node is located in at the junction between the right atrium and the superior vena cava. • The AV node is located in the right atrium near the coronary sinus. • The bundle of His is located at the septal level. It divides to form the right and left bundle branches, which supply the right and left ventricles, respectively. • The left bundle branch divides to form the anterosuperior and posteroinferior fascicles
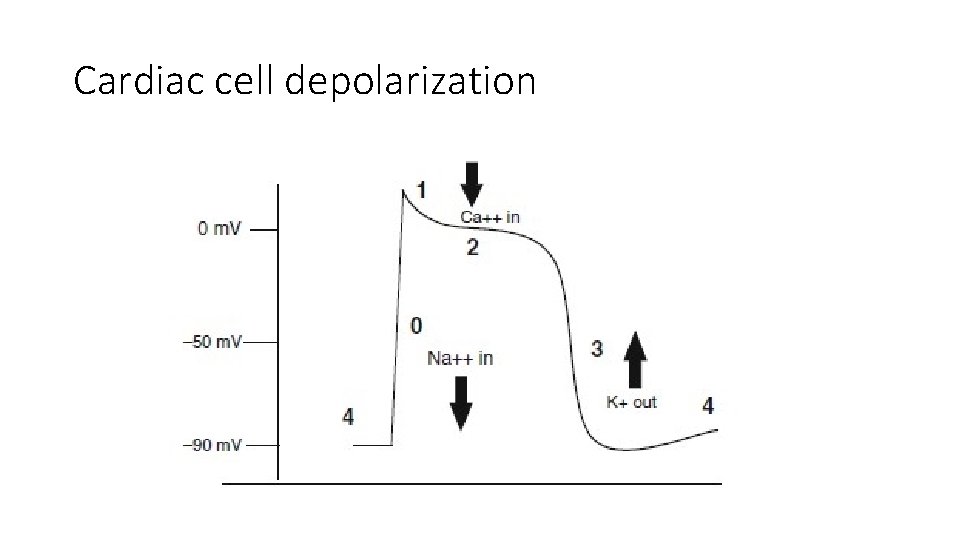
Cardiac cell depolarization
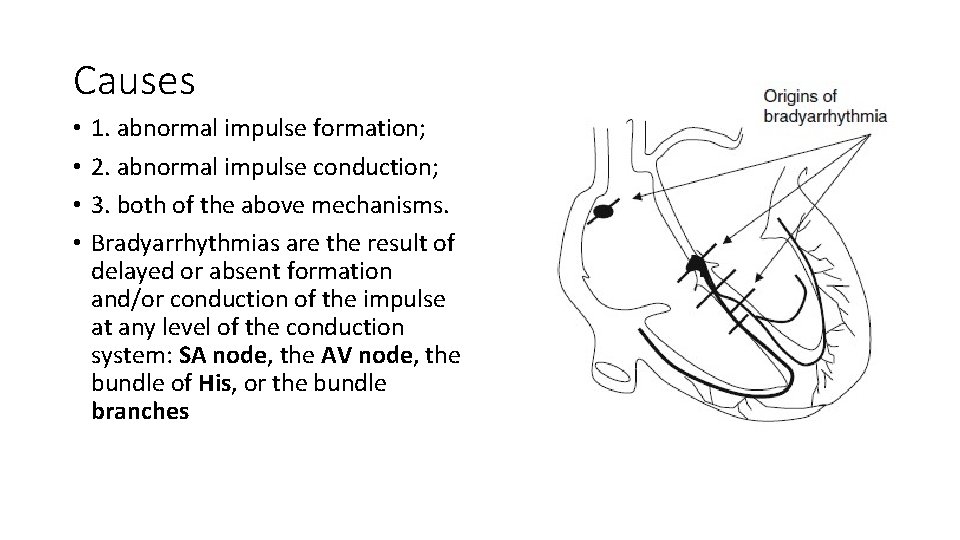
Causes • • 1. abnormal impulse formation; 2. abnormal impulse conduction; 3. both of the above mechanisms. Bradyarrhythmias are the result of delayed or absent formation and/or conduction of the impulse at any level of the conduction system: SA node, the AV node, the bundle of His, or the bundle branches

Tachyarrhythmia • Three electrophysiological mechanisms give rise to tachyarrhythmias: 1 abnormal automaticity, 2 the reentry phenomenon, 3 triggered activity. • The first involves increased spontaneous firing by pacemaker cells or common cardiomyocytes. It can be caused by various factors: -increased sympathetic activity, -ischemia, -acidosis, -hypokalemia • These conditions are characterized by increases in the slope of phase 4 of the action potential and in the firing rate of the cardiac cells
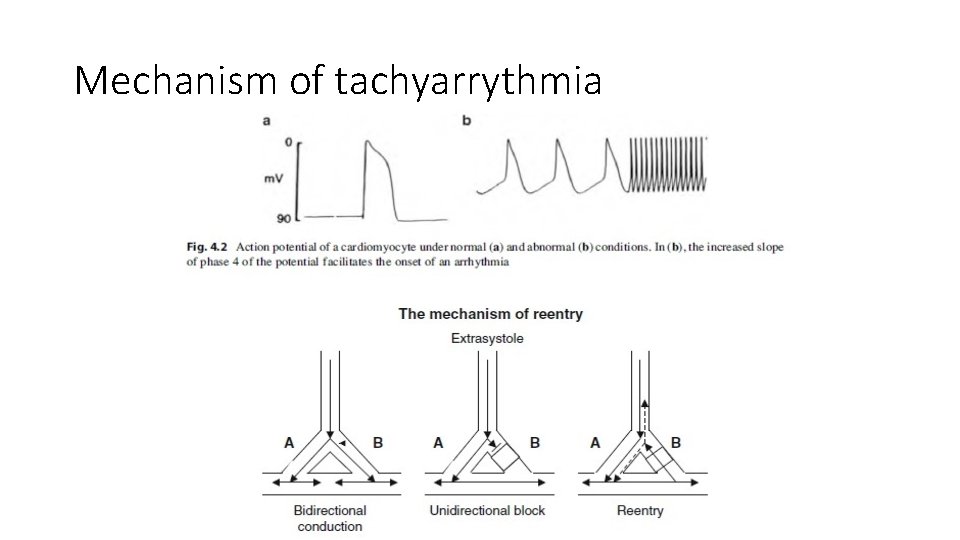
Mechanism of tachyarrythmia

Afterdepolarizations • Oscillating currents present during the repolarization phase that are sometimes large enough in amplitude to generate repetitive firing. Under normal conditions, cardiac muscle fibers generate rhythmical electrical impulses as a manifestation of their spontaneous automaticity. • In “triggered" activity, the action potential may be generated before phase 4 of the previous potential reaches the threshold level: afterdepolarizations therefore appear in relation to one or more of the previous electrical stimuli (which explains the term “triggered. ”) There are two types of afterdepolarizations : those occurring before repolarization has been completed, during phase 2 or 3 of the action potential (early afterpotentials), and those that occur after repolarization has been completed, that is, in phase 4
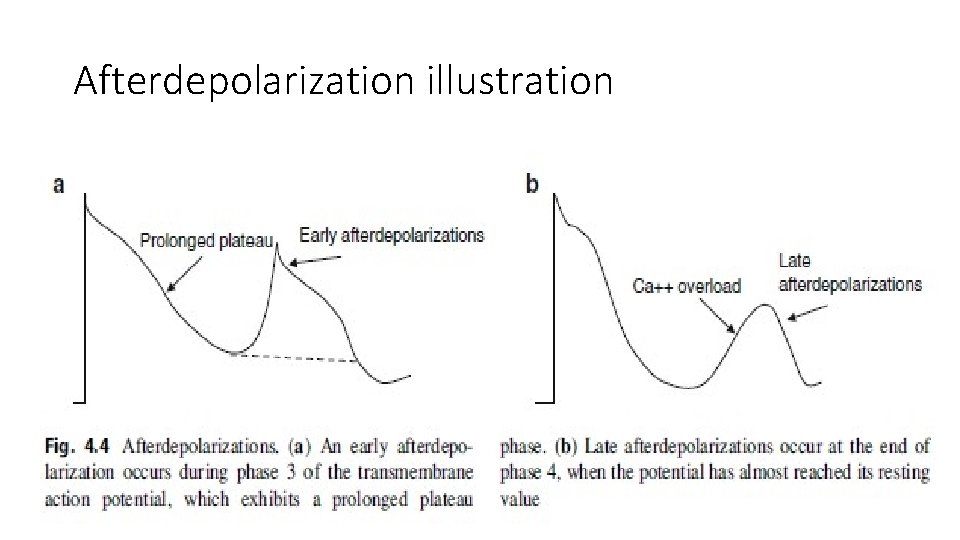
Afterdepolarization illustration
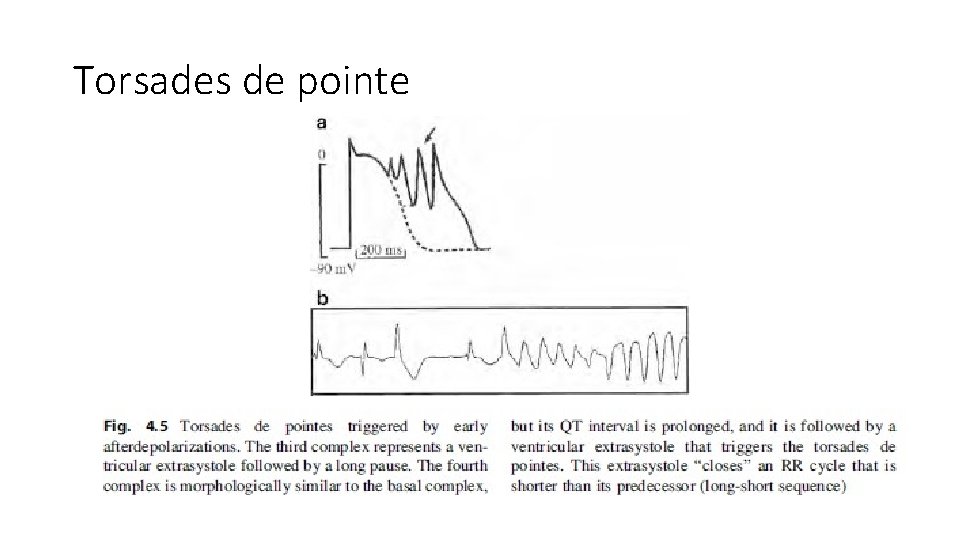
Torsades de pointe

Bradyarrythmia mechanism Useful insight into the bradyarrhythmias can be obtained with intracardiac ECG, which is performed with a catheter electrode placed inside the cardiac chambers. The tracing obtained with this technique (Fig. 5. 2) includes three main polyphasic elements: • – the A deflection, which represents activation of the atria; • – the H deflection, which corresponds to activation of the common trunk of the His bundle and has a normal duration of approximately 20– 25 ms; • – the V deflection, which reflects activation of the ventricular myocardium. If the surface and intracardiac ECGs are recorded simultaneously, three important intervalscan be measured: • – The PA interval, which is measured from the onset of the P wave on the surface ECG to the first rapid A deflection. It represents the time required for the stimulus to travel from the SA node to the AV node (normally 15– 25 ms). • – The AH interval, which is measured from the onset of the A deflection to the onset of the H deflection. It reflects the conduction time through the AV node (normally 60– 120 ms). • – The HV interval, from the onset of the H deflection to the first rapid component of the V deflection, represents the time needed for depolarization of the His bundle, the bundle branches, and the Purkinje network (normally 35– 55 ms). • These elements are necessary for subsequent understanding of the locations of atrioventricular blocks (AVBs) and their clinical significance and prognostic implications.
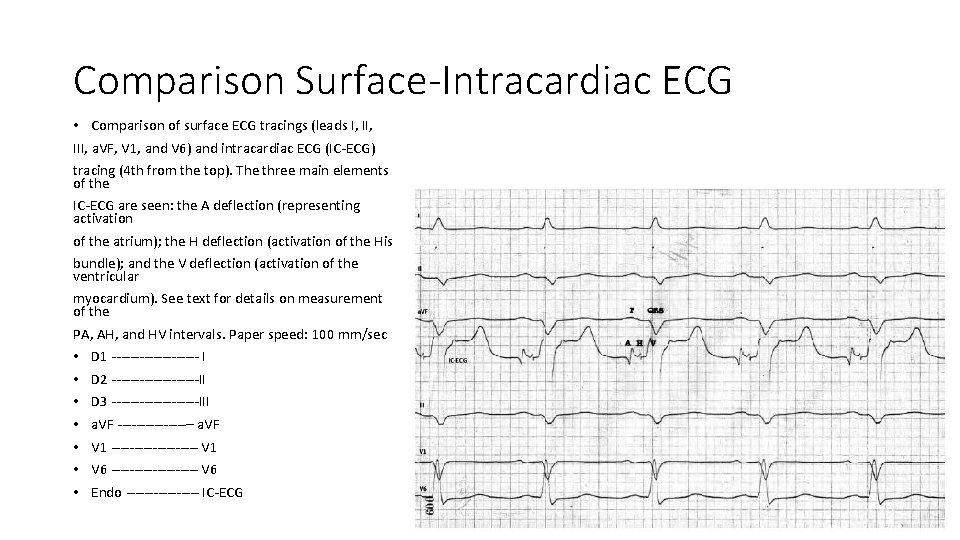
Comparison Surface-Intracardiac ECG • Comparison of surface ECG tracings (leads I, III, a. VF, V 1, and V 6) and intracardiac ECG (IC-ECG) tracing (4 th from the top). The three main elements of the IC-ECG are seen: the A deflection (representing activation of the atrium); the H deflection (activation of the His bundle); and the V deflection (activation of the ventricular myocardium). See text for details on measurement of the PA, AH, and HV intervals. Paper speed: 100 mm/sec • D 1 ---------- I • D 2 ----------II • D 3 ----------III • a. VF --------– a. VF • V 1 ---------- V 1 • V 6 ---------- V 6 • Endo -------- IC-ECG
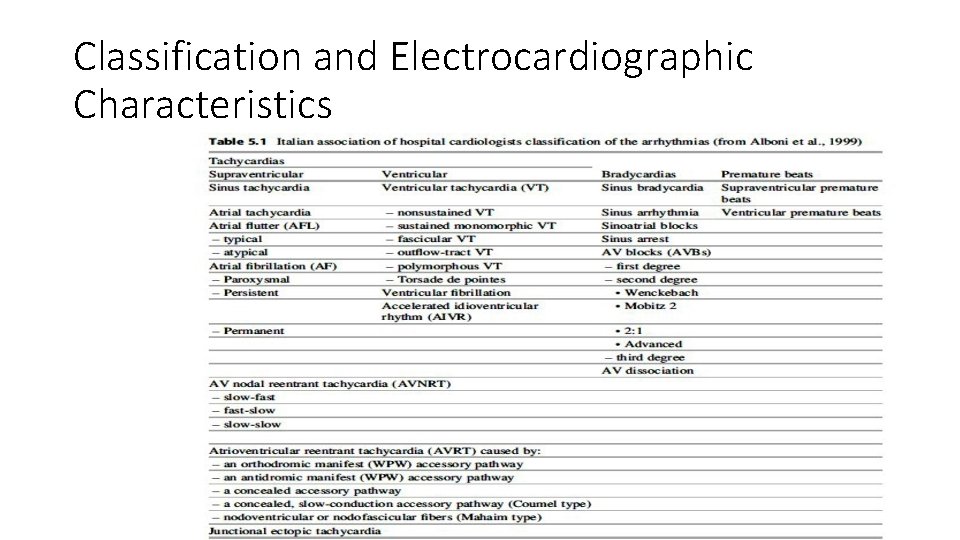
Classification and Electrocardiographic Characteristics
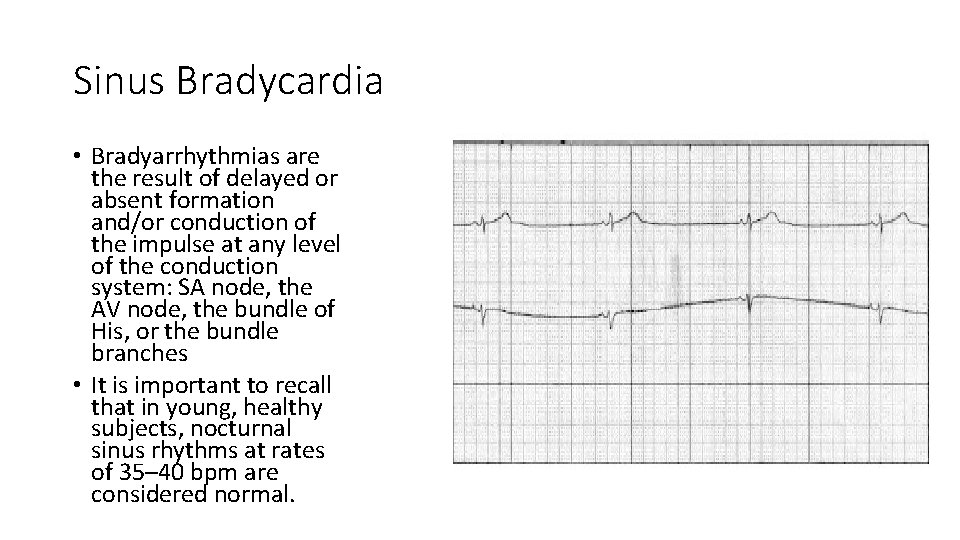
Sinus Bradycardia • Bradyarrhythmias are the result of delayed or absent formation and/or conduction of the impulse at any level of the conduction system: SA node, the AV node, the bundle of His, or the bundle branches • It is important to recall that in young, healthy subjects, nocturnal sinus rhythms at rates of 35– 40 bpm are considered normal.
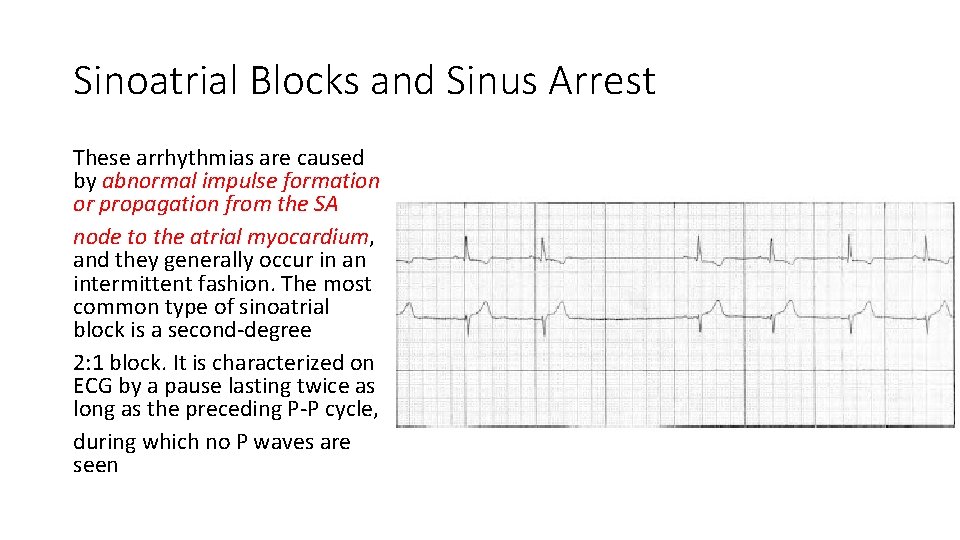
Sinoatrial Blocks and Sinus Arrest These arrhythmias are caused by abnormal impulse formation or propagation from the SA node to the atrial myocardium, and they generally occur in an intermittent fashion. The most common type of sinoatrial block is a second-degree 2: 1 block. It is characterized on ECG by a pause lasting twice as long as the preceding P-P cycle, during which no P waves are seen
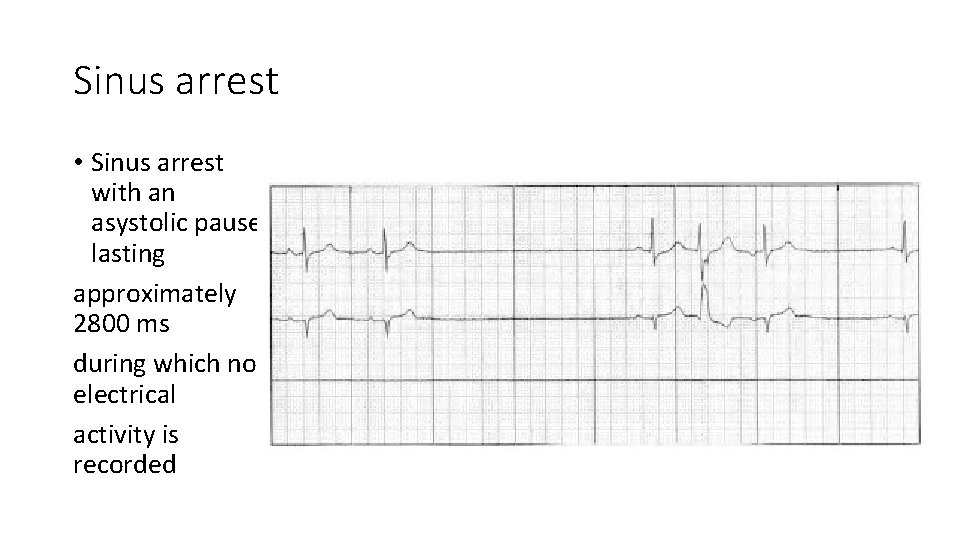
Sinus arrest • Sinus arrest with an asystolic pause lasting approximately 2800 ms during which no electrical activity is recorded
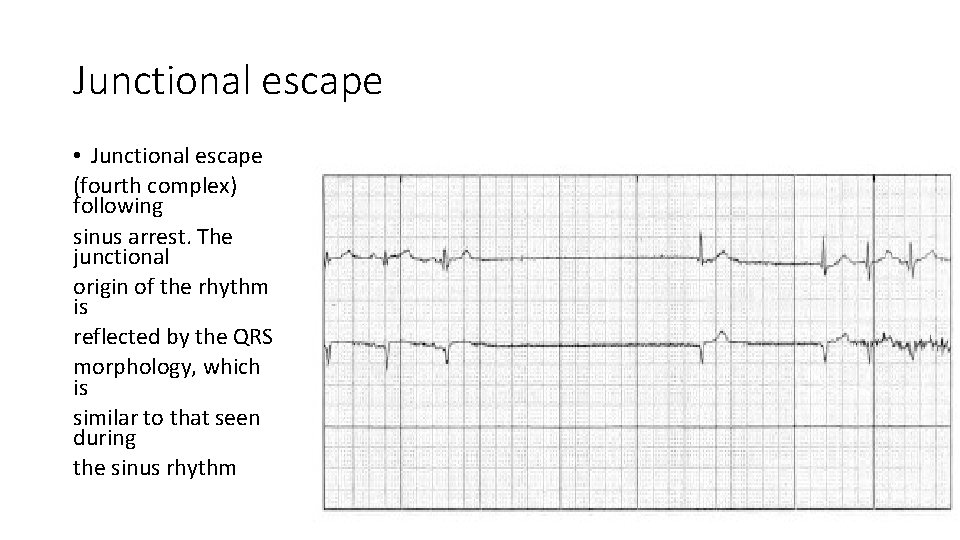
Junctional escape • Junctional escape (fourth complex) following sinus arrest. The junctional origin of the rhythm is reflected by the QRS morphology, which is similar to that seen during the sinus rhythm
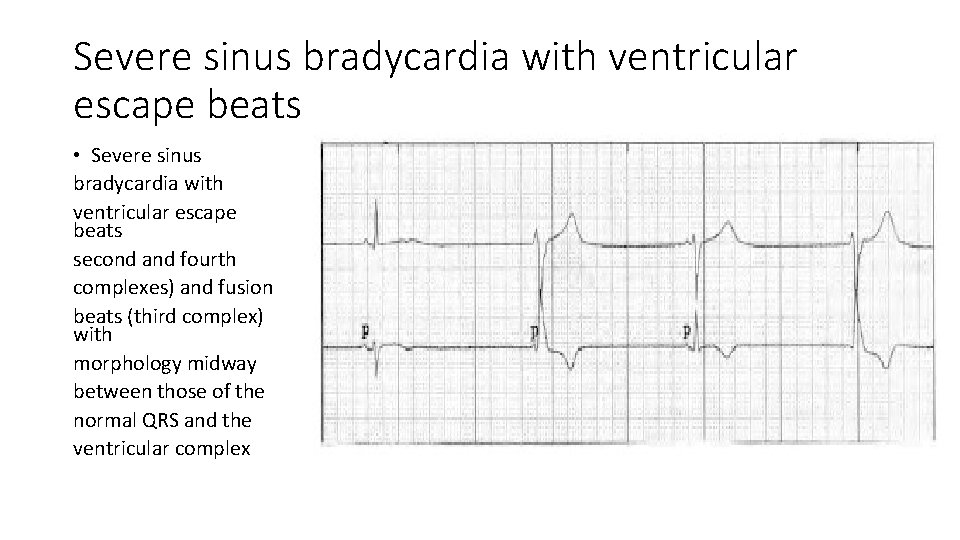
Severe sinus bradycardia with ventricular escape beats • Severe sinus bradycardia with ventricular escape beats second and fourth complexes) and fusion beats (third complex) with morphology midway between those of the normal QRS and the ventricular complex

The Tachyarrhythmias • The tachyarrhythmias comprise a variety of disorders ranging from isolated ectopic beats to repetitive arrhythmias arising in the atria or ventricles. • Ectopic Beats (Extrasystoles) are abnormal impulses originating at points in the myocardium other than the physiological pacemaker • Depending on the actual location, they are described as supraventricular or ventricular
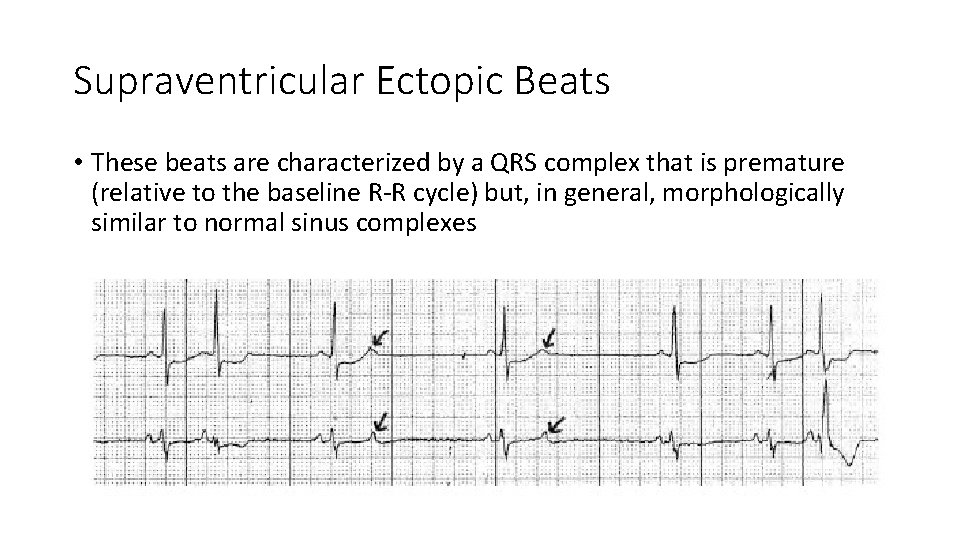
Supraventricular Ectopic Beats • These beats are characterized by a QRS complex that is premature (relative to the baseline R-R cycle) but, in general, morphologically similar to normal sinus complexes
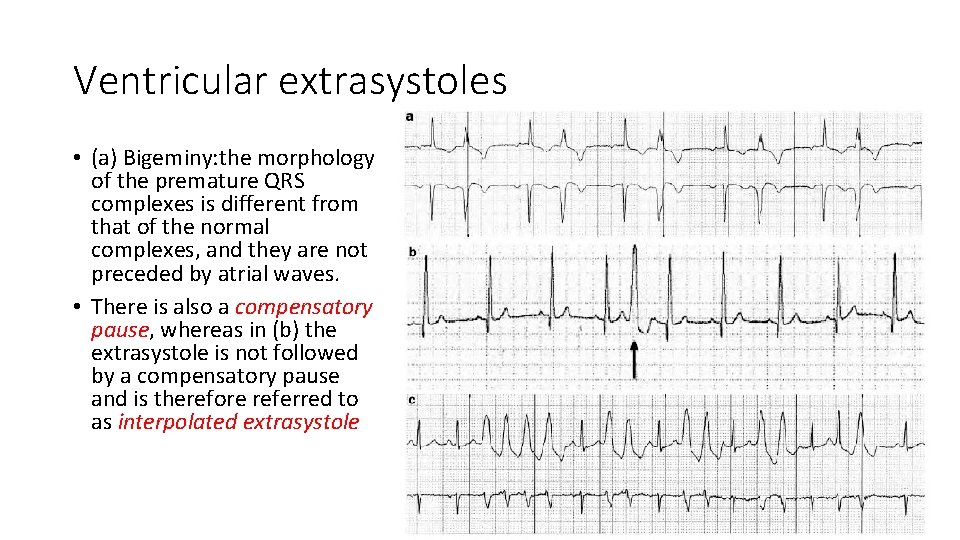
Ventricular extrasystoles • (a) Bigeminy: the morphology of the premature QRS complexes is different from that of the normal complexes, and they are not preceded by atrial waves. • There is also a compensatory pause, whereas in (b) the extrasystole is not followed by a compensatory pause and is therefore referred to as interpolated extrasystole
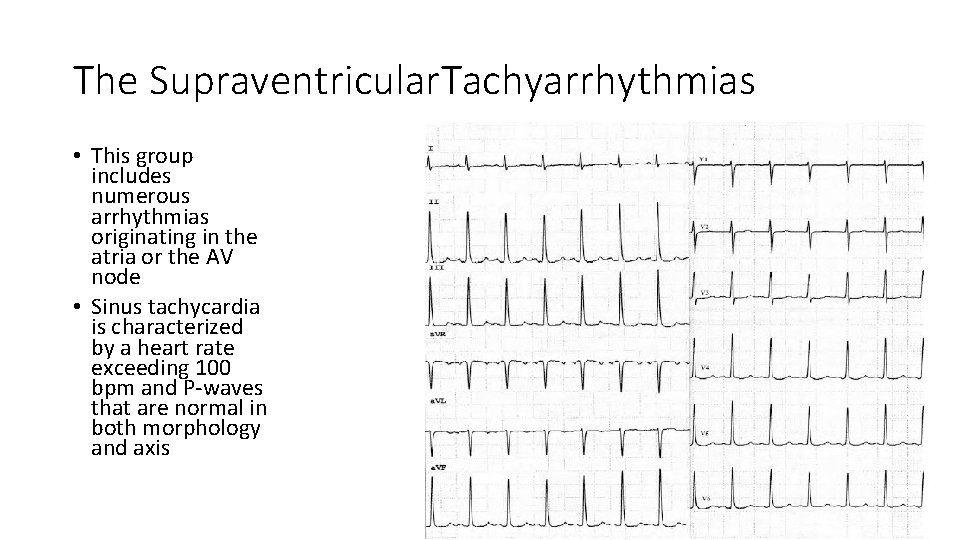
The Supraventricular. Tachyarrhythmias • This group includes numerous arrhythmias originating in the atria or the AV node • Sinus tachycardia is characterized by a heart rate exceeding 100 bpm and P-waves that are normal in both morphology and axis
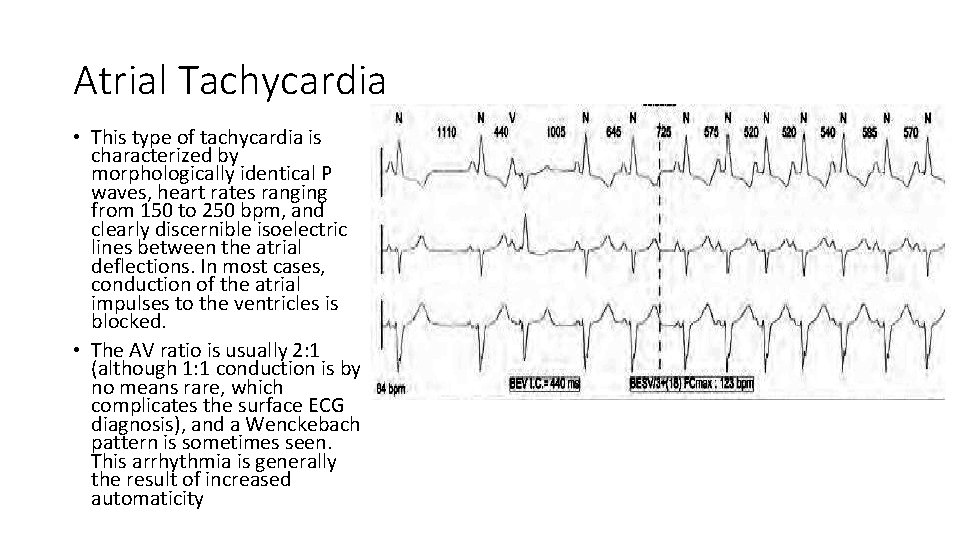
Atrial Tachycardia • This type of tachycardia is characterized by morphologically identical P waves, heart rates ranging from 150 to 250 bpm, and clearly discernible isoelectric lines between the atrial deflections. In most cases, conduction of the atrial impulses to the ventricles is blocked. • The AV ratio is usually 2: 1 (although 1: 1 conduction is by no means rare, which complicates the surface ECG diagnosis), and a Wenckebach pattern is sometimes seen. This arrhythmia is generally the result of increased automaticity
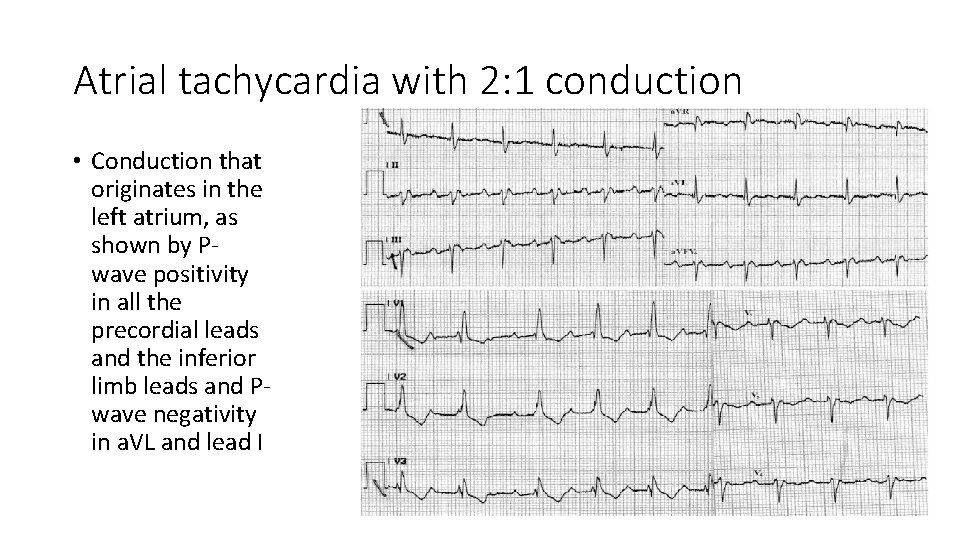
Atrial tachycardia with 2: 1 conduction • Conduction that originates in the left atrium, as shown by Pwave positivity in all the precordial leads and the inferior limb leads and Pwave negativity in a. VL and lead I

Conclusion • There is lot to see on this chapter. This lecture should only be seen as an introduction to the vast subject of cardiac arrhythmia. • Later we’ll come for further details on AV conduction abnormalities. • Thank You all.

- Slides: 26