Cardiac Implantable Devices Nursing Care The Basics and

Cardiac Implantable Devices Nursing Care: The Basics and Beyond

Welcome! l Terri Rhodes, RN, BSN ¡Clinical Level III, CEP Lab Nurse l Laura Hess, RN, BSN ¡Clinical Level II, CEP Lab Nurse l Please feel free to ask questions during the presentation!

Objectives: l Examine device terminology l Examine the components, functions and indications for a pacemaker l Inventory the components, indications and functions of an internal cardiac defibrillator (ICD) l Compare the pacing modes using NBG pacing code system l Assess patient needs preoperatively l Manage patient postoperatively l Analyze rhythm strips for appropriate pacemaker and ICD functioning

Outline l 1. Welcome and general information l 2. Pacemakers l 3. ICD’s l 4. NBG codes l 5. Biventricular Pacing l 6. Nursing Considerations l 7. Pacemaker Practice Strips
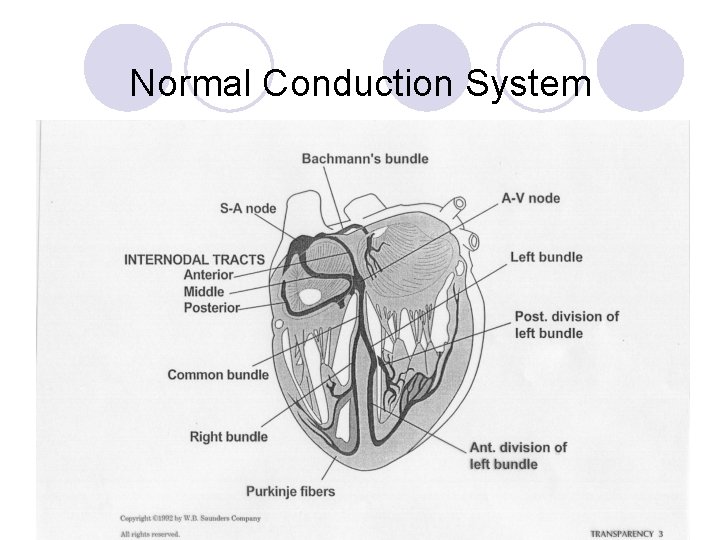
Normal Conduction System

A Brief History of Implantable Devices l 1958 - First human implant ¡ Dr. Senning in Stockholm, only lasted 3 hours l 1960 - First clinically successful human implant ¡ Dr’s Chardack and Gage in the US ¡ William Greatbatch, engineer l 1965 - First VVI implanted l 1972 - Partially programmable l 1977 -Multiprogrammable l 1981 - Dual chamber multi-programmable

Along Came ICD’s… l 1980 - First human implant l Thoracotomy ¡ Epicardial patch & lead ¡ Large device placed in abdomen ¡ Not programmable; i. e. only one setting l Second generation ICD ¡ Transvenous electrode ¡ Bradycardia & anti-tachycardia pacing l Fifth generation ¡ Dual-chamber rate responsive pacing ¡ Improved recognition of SVT l The Next Generation ¡ Remote interrogation ¡ CHF Management ¡ S-ICD- subcutaneous ICD

General “Device” Terms to Understand l Sense l Fire l Capture

Sense l Sense: the ability of the device to recognize the presence or absence of an innate “p” wave or “qrs” complex

Fire l Fire: the device has sensed a missed “p” wave or “qrs” complex, and has sent energy down the pacing wire to the tissue

Capture l Capture: the energy has contracted the myocardial tissue, and resulted in a “p” wave or “qrs” complex on skin leads

Device Terms Continued… l Failure to Capture: ¡ A spike is noted on strip, but is not followed by appropriate “p” or “qrs” wave form l Failure to Sense ¡ Spike (energy) is missing during absence of “p” or “qrs” ¡ Spike noted at inappropriate times l R on T ¡ Occurs when device fails to sense, and delivers energy during vulnerable T wave - or – if programmed at VOO/AOO, the pacemaker delivers the energy in spite of intrinsic activity and paces on the t-wave. l Failure to Fire ¡ Device does not send energy (pacer spike) when indicated ***If you notice any of these, check your patient, check pulse and notify physician***

What Do You Need To Have a Paced Beat? l Atrial Paced Beat: ¡“a” pacing spike ¡P wave immediately following pacer spike l Ventricular Paced Beat: ¡“v” pacing spike ¡QRS immediately follows pacing spike
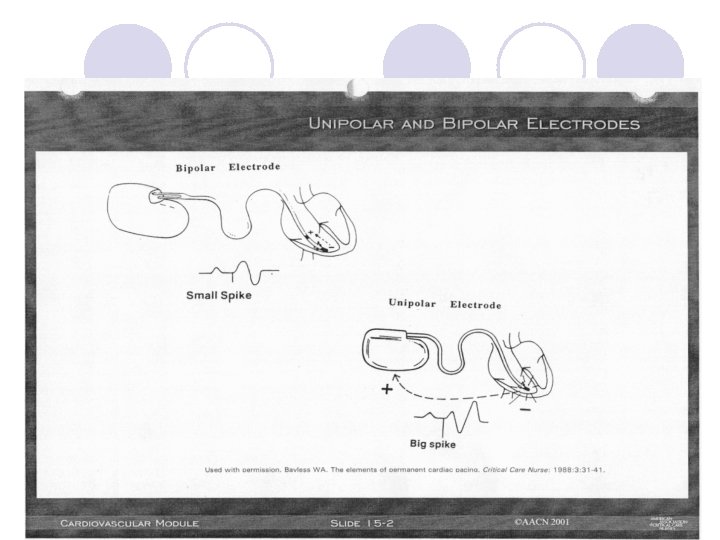
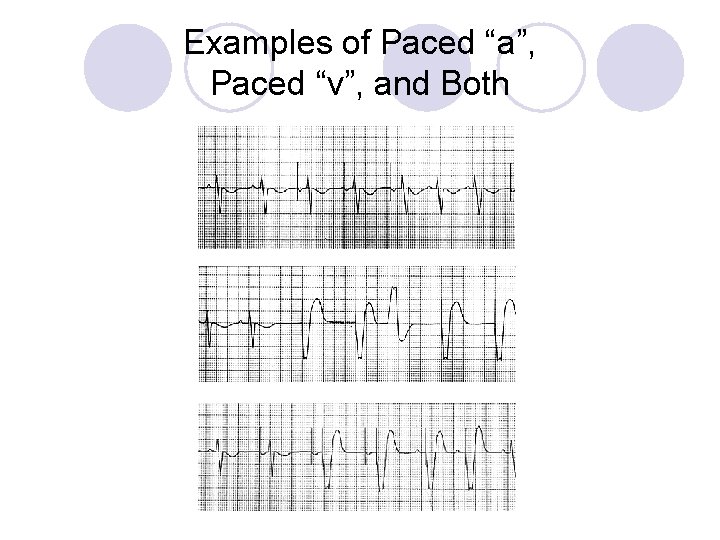
Examples of Paced “a”, Paced “v”, and Both

Pacemakers

What is a pacemaker? l A internal device that regulates electrical impulses through the heart. ¡ Sense ¡ Fire ¡ Capture Single Chamber, Dual Chamber and Bi-Ventricular

Pacemaker Components l Pulse generator- battery which provides the energy. Controls the rate, output, and sensitivity. ¡The “Can” l Leads- carries the impulse to the heart tissue ¡Atrial ¡Right Ventricle ¡Left Ventricle l. Coronary Sinus
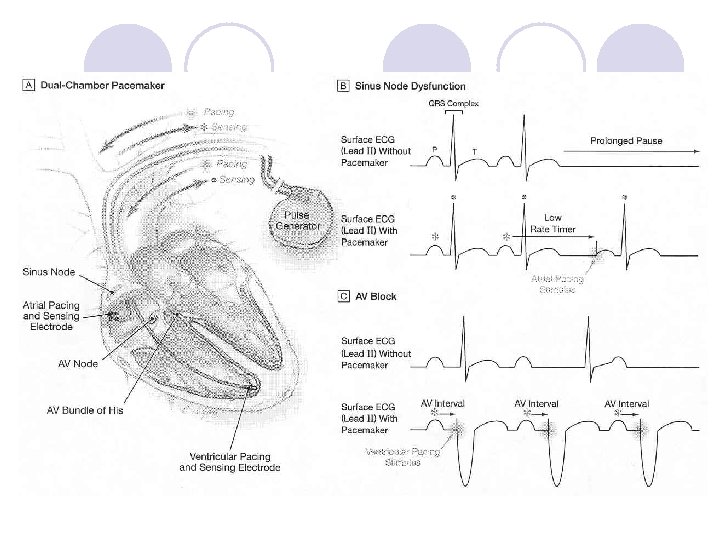

Indications for pacemakers l Symptomatic 2 nd degree, Mobitz Type II heart block l Complete heart block (3 rd degree) l Asystole l Symptomatic bradycardia l Sinus node dysfunction l Carotid sinus syndrome and hypersensitivity ¡ An exaggerated response to carotid sinus baroreceptor stimulation. Sometimes even mild stimulation in the neck region causes a marked decrease in heart rate, blood pressure, and causes syncope.

Other Indications l. Hypertrophic Obstructive Cardiomyopathy (HOCM) ¡S/P Alcohol Septal Ablation l. Congestive heart failure (CHF) Biventricular pacing

Magnet Placement for a Pacemaker l Temporarily changes the mode of pacing to asynchronous (VOO, DOO) while magnet is in place. l Paces regardless of rhythm l This is programmable feature of the device; NOT ONE SIZE FITS ALL

Break? ? ?

Intracardiac Cardioverter Defibrillators or ICD’s

What is an ICD? l An internal device that can regulate electrical impulses through the heart, but its main function is to detect and terminate tachy arrhythmias. ¡Defibrillation ¡Override pacing ¡Cardioversion ¡Pacemaker Functions (Single/Dual/Bi. V)

Components of an ICD l Pulse generator- battery which provides the energy. Detects tachy arrhythmias and delivers defibrillation energy when indicated. Controls the rate, output, and sensitivity of the pacemaker function. ¡The “Can” l Leads- carries the impulse to the heart tissue ¡Right Ventricle l Endo Coil – High output lead ¡Atrium l Pacemaker lead ¡Left Ventricle l Placed via the Coronary Sinus when placed in EP lab, and epicardial when placed in OR
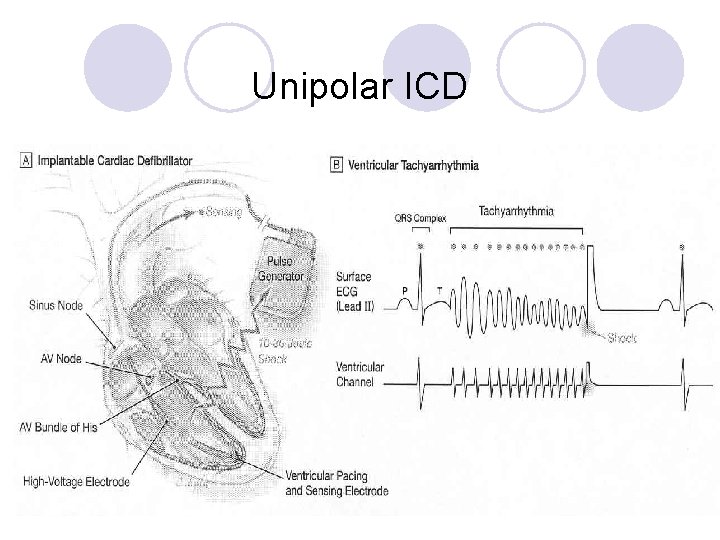
Unipolar ICD

Indications for ICDs Secondary prevention (already had event) l Sudden Cardiac Death; NSVT, Sustained VT, Vfib arrest l Inducible VT (EP testing) Primary prevention (trying to treat FIRST event) l Cardiomyopathy (SCD-He. FT) l At risk for sudden cardiac death ¡ Unknown etiology ¡ Long QT ¡ Brugada Syndrome (Na channel abnormality resulting in RBBB with J point elevation and concave ST elevation) l Cardiac Sarcoid

And the Latest… S-ICD The S-ICD System is intended to provide defibrillation therapy for the treatment of lifethreatening ventricular tachyarrhythmias in patients who do not have: *symptomatic bradycardia *incessant VT *spontaneous, frequently recurring VT that is reliably terminated with anti-tachycardia pacing
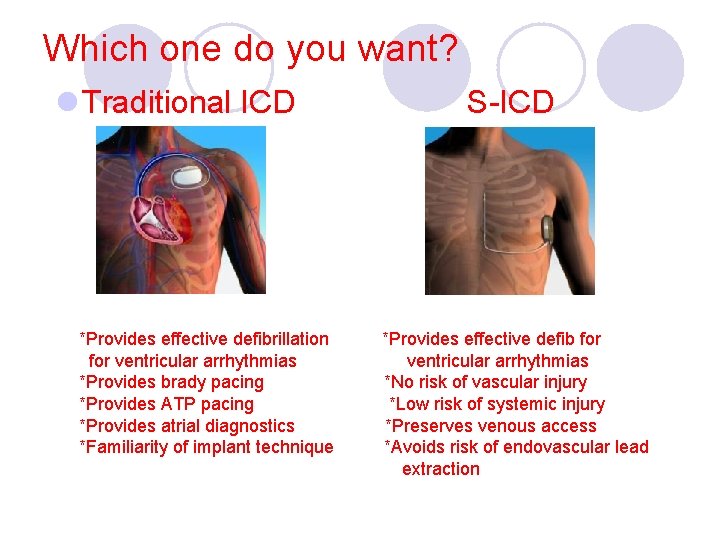
Which one do you want? l Traditional ICD *Provides effective defibrillation for ventricular arrhythmias *Provides brady pacing *Provides ATP pacing *Provides atrial diagnostics *Familiarity of implant technique S-ICD *Provides effective defib for ventricular arrhythmias *No risk of vascular injury *Low risk of systemic injury *Preserves venous access *Avoids risk of endovascular lead extraction

Magnet Placement for an ICD l Suspends tachycardia detection while the magnet is in place l Pacing parameters remain unchanged l This is a programmable feature of the ICD, and may be different

Caution! l Place magnet on device ONLY under guidance or supervision from a physician or Electrophysiology Department nurse. l Examples of when placing magnet is appropriate: ¡ICD “ shocking” at inappropriate times ¡During OR procedures requiring cautery. Stat pads must be placed on patient. ¡During a code situation when you want to take ‘control of the shocking’

Special Considerations for Pt’s with ICD’s l If ICD discharges? ¡ 1. Check your pt: Think BLS/ACLS! l ABC’s, is pt. responsive, what rhythm are they in? l Take appropriate action if pt. is not stable ¡ 2. If pt. is stable notify EP department l During a CODE? ¡ DO NOT place STAT pads directly over device ¡ UCH policy: Place external defibrillator pads 4 -6 inches away from the device laterally if possible. l Pt. is going for another OR procedure ¡ Notify Anesthesia that pt. has device, tell them the company and they will notify the EP department

Break?

NBG Codes l Generic code created for NASPE and BPEG. (NASPE is the North American Society of Pacing and Electrophysiology. BPEG is the British Pacing and Electrophysiology Group. ) l Pacemaker programming codes that identifies how the pacemaker is programmed to function.

NBG Codes: Programming the pacemaker l I- What chamber do you want to pace? l II- What chamber do you want to sense? l III-What do you want to do with the sensed information? Inhibit pacing or trigger pacing? ¡Tracking the Atrial activity l IV-Do you want to increase the rate with the patient’s activity?
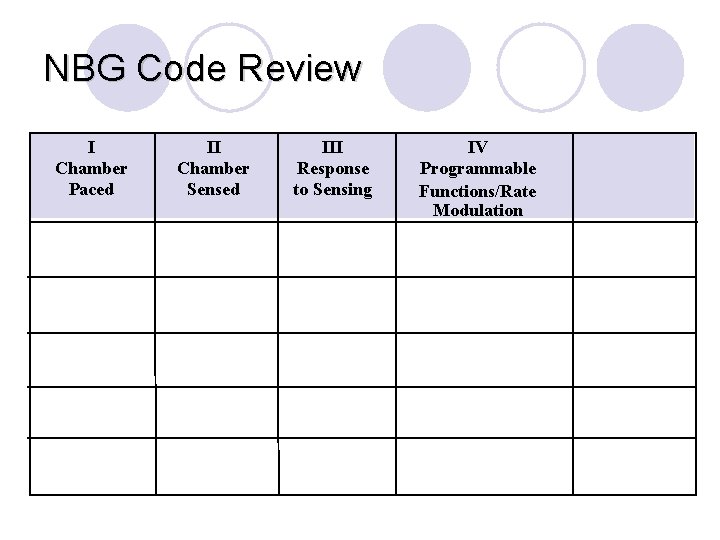
NBG Code Review I Chamber Paced II Chamber Sensed III Response to Sensing V: Ventricle T: Triggered P: Simple programmable A: Atrium I: Inhibited M: Multiprogrammable D: Dual (A+V) D: Dual (T+I) C: Communicating O: None R: Rate modulating S: Single (A or V) O: None IV Programmable Functions/Rate Modulation O: None
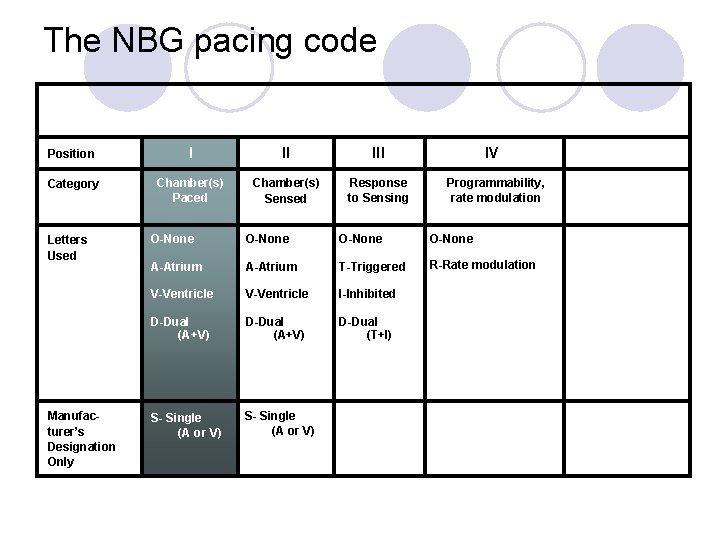
The NBG pacing code Position I II III Category Chamber(s) Paced Chamber(s) Sensed Response to Sensing Letters Used Manufacturer’s Designation Only IV Programmability, rate modulation O-None A-Atrium T-Triggered R-Rate modulation V-Ventricle I-Inhibited D-Dual (A+V) D-Dual (T+I) S- Single (A or V)
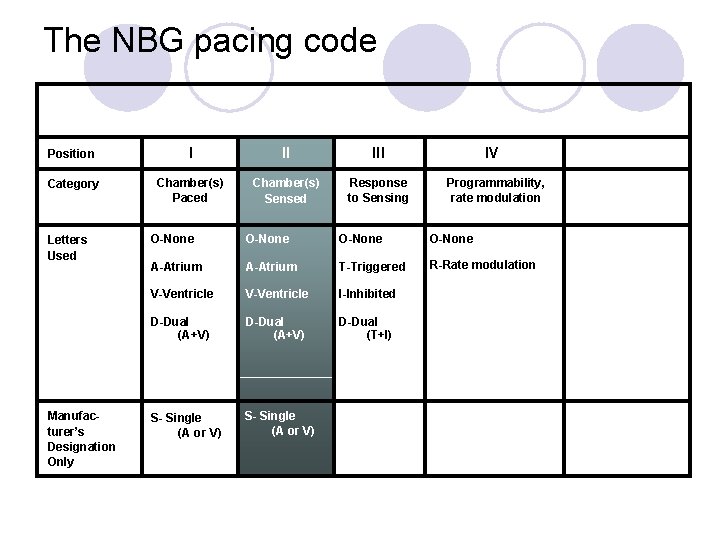
The NBG pacing code Position I II III Category Chamber(s) Paced Chamber(s) Sensed Response to Sensing Letters Used Manufacturer’s Designation Only IV Programmability, rate modulation O-None A-Atrium T-Triggered R-Rate modulation V-Ventricle I-Inhibited D-Dual (A+V) D-Dual (T+I) S- Single (A or V)
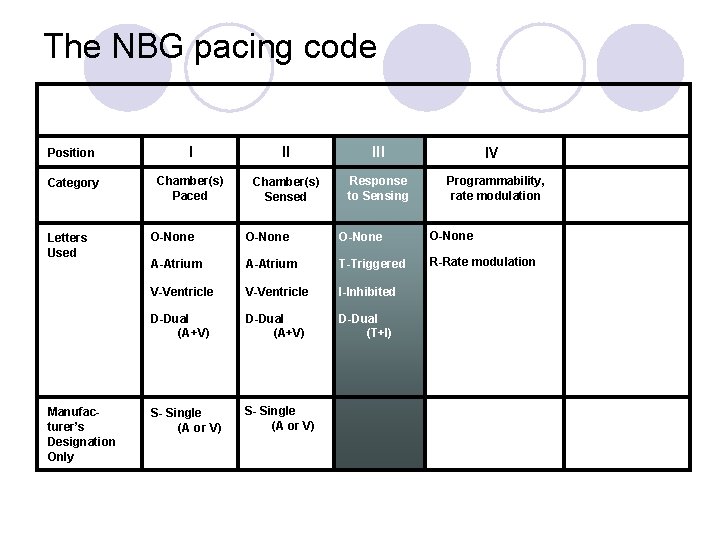

The NBG pacing code Position I II III Category Chamber(s) Paced Chamber(s) Sensed Response to Sensing Letters Used Manufacturer’s Designation Only IV Programmability, rate modulation O-None A-Atrium T-Triggered R-Rate modulation V-Ventricle I-Inhibited D-Dual (A+V) D-Dual (T+I) S- Single (A or V)
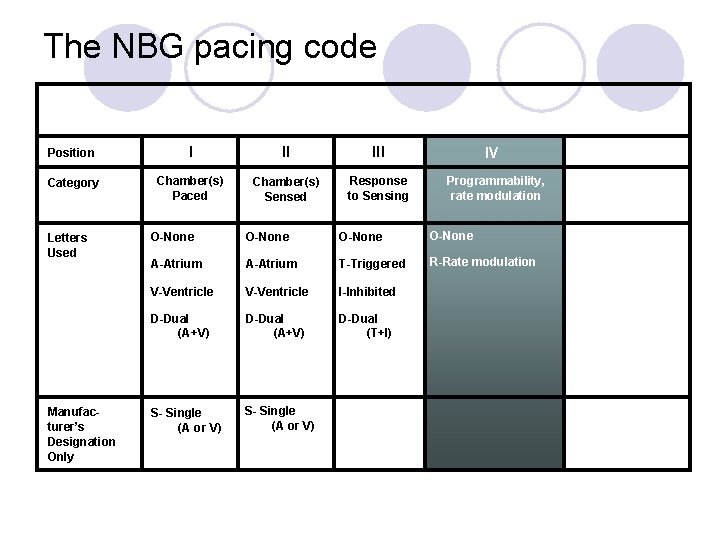

The NBG pacing code Position I II III Category Chamber(s) Paced Chamber(s) Sensed Response to Sensing Letters Used Manufacturer’s Designation Only IV Programmability, rate modulation O-None A-Atrium T-Triggered R-Rate modulation V-Ventricle I-Inhibited D-Dual (A+V) D-Dual (T+I) S- Single (A or V)

Single Chamber Pacing How Do We Use The NBG Language?
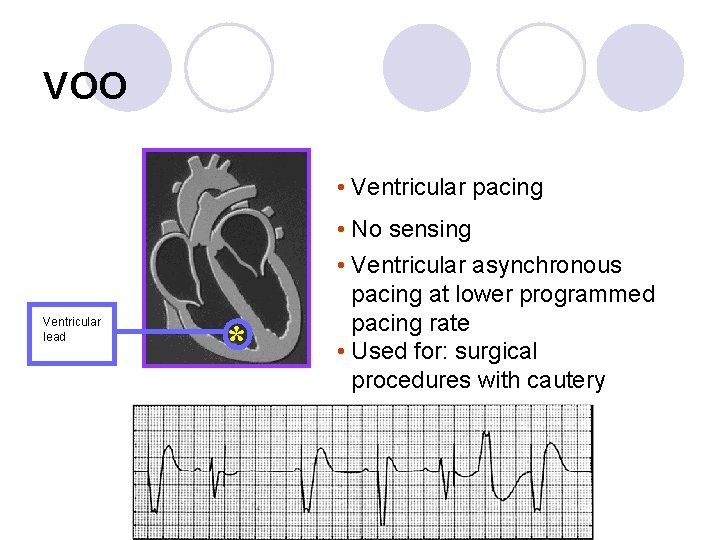
VOO • Ventricular pacing Ventricular lead * • No sensing • Ventricular asynchronous pacing at lower programmed pacing rate • Used for: surgical procedures with cautery
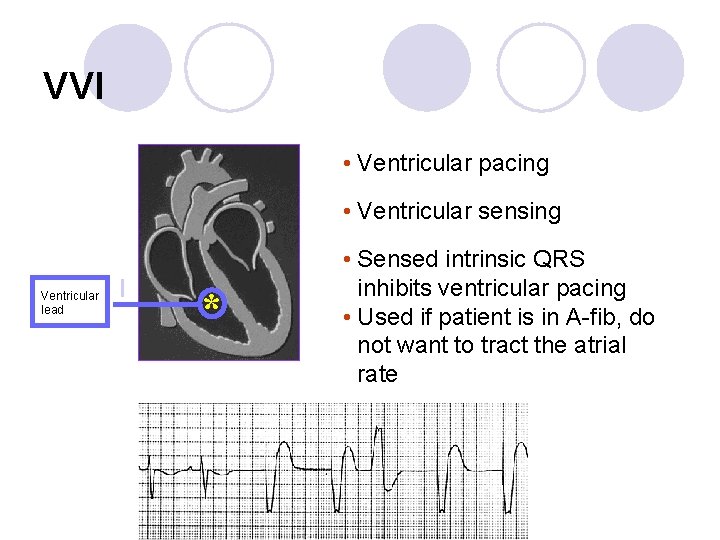
VVI • Ventricular pacing • Ventricular sensing Ventricular lead I * • Sensed intrinsic QRS inhibits ventricular pacing • Used if patient is in A-fib, do not want to tract the atrial rate
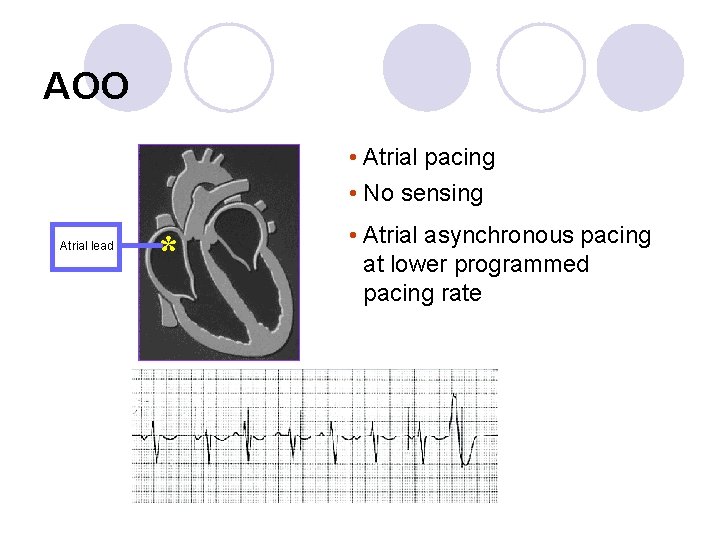
AOO • Atrial pacing • No sensing Atrial lead * • Atrial asynchronous pacing at lower programmed pacing rate
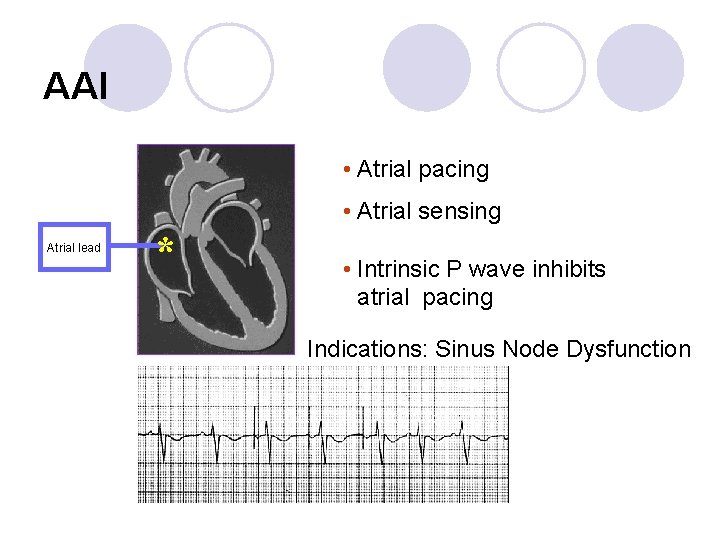
AAI • Atrial pacing • Atrial sensing Atrial lead * • Intrinsic P wave inhibits atrial pacing Indications: Sinus Node Dysfunction

Dual Chamber Pacing Tracking Mode: Both triggers and inhibits pacing

Benefits of Dual Chamber Pacing l Provides AV synchrony l Lower incidence of atrial fibrillation l Lower risk of systemic embolism and stroke l Lower incidence of new congestive heart failure l Lower mortality and higher survival rates
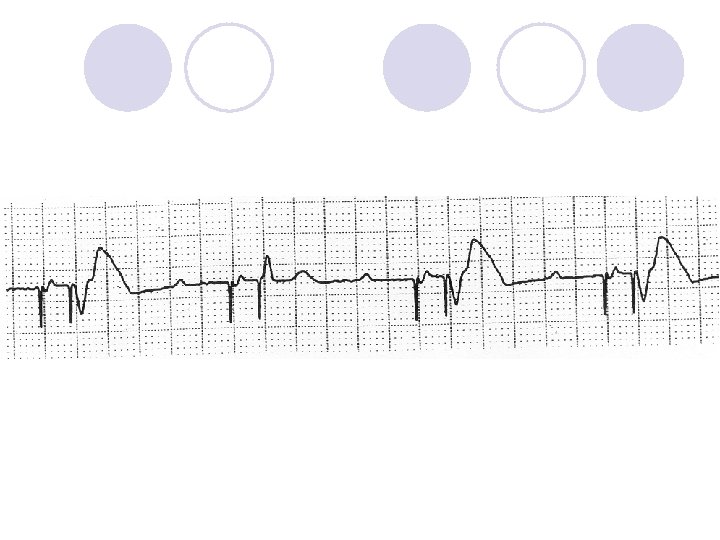
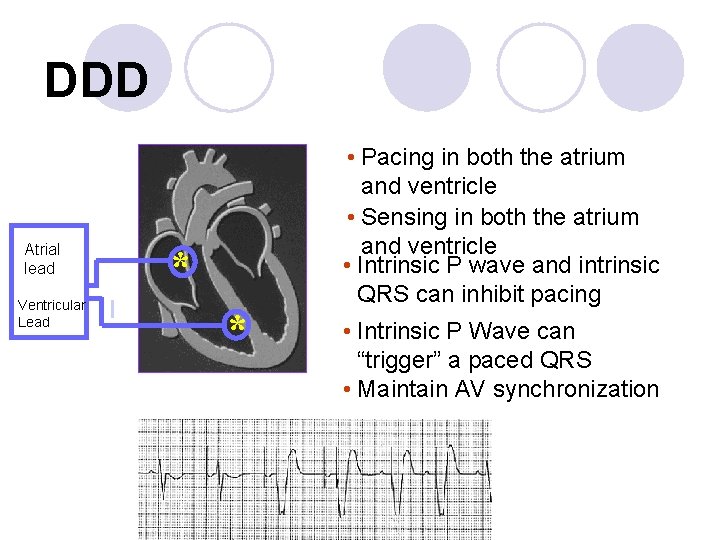
DDD Atrial lead Ventricular Lead * I * • Pacing in both the atrium and ventricle • Sensing in both the atrium and ventricle • Intrinsic P wave and intrinsic QRS can inhibit pacing • Intrinsic P Wave can “trigger” a paced QRS • Maintain AV synchronization

DDD pacing l. Dual-chamber pacing capable of pacing and sensing in both the atrial and ventricular chambers of the heart l 4 distinct patterns can be observed with DDD pacing
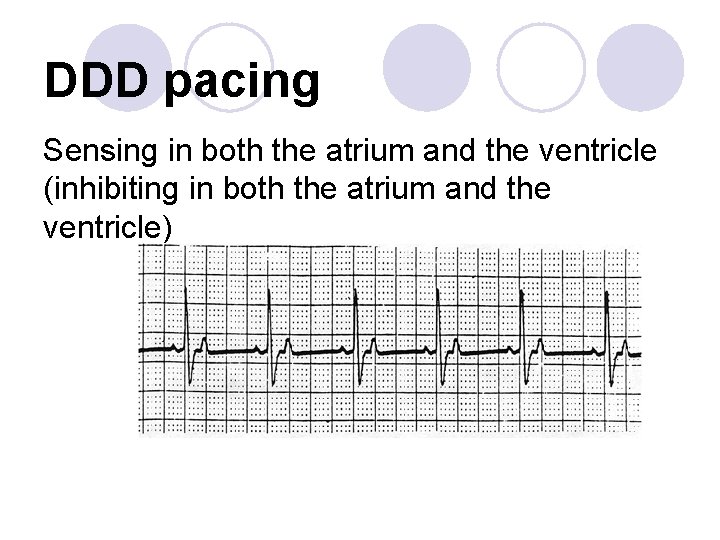
DDD pacing Sensing in both the atrium and the ventricle (inhibiting in both the atrium and the ventricle)
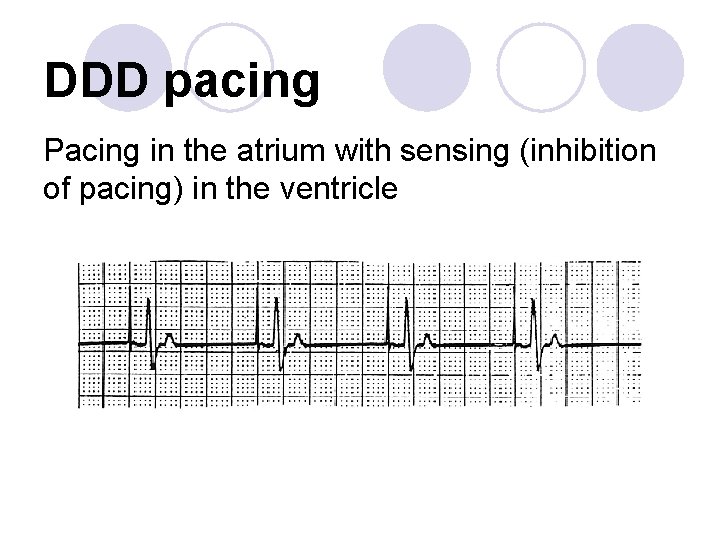
DDD pacing Pacing in the atrium with sensing (inhibition of pacing) in the ventricle
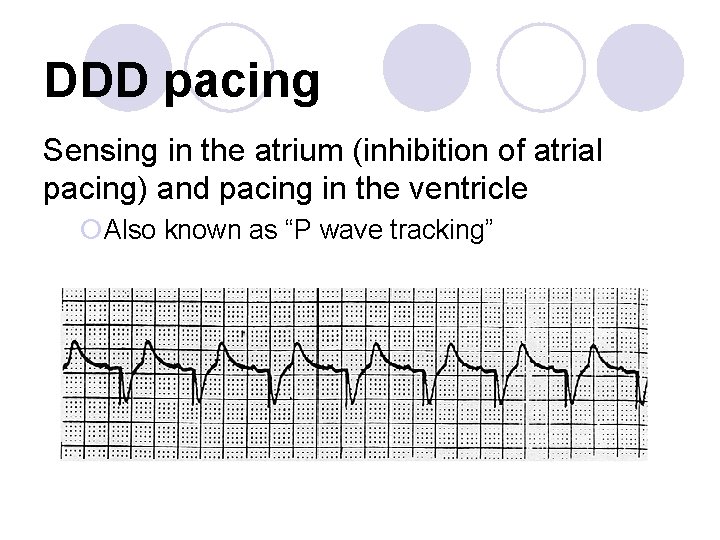
DDD pacing Sensing in the atrium (inhibition of atrial pacing) and pacing in the ventricle ¡Also known as “P wave tracking”
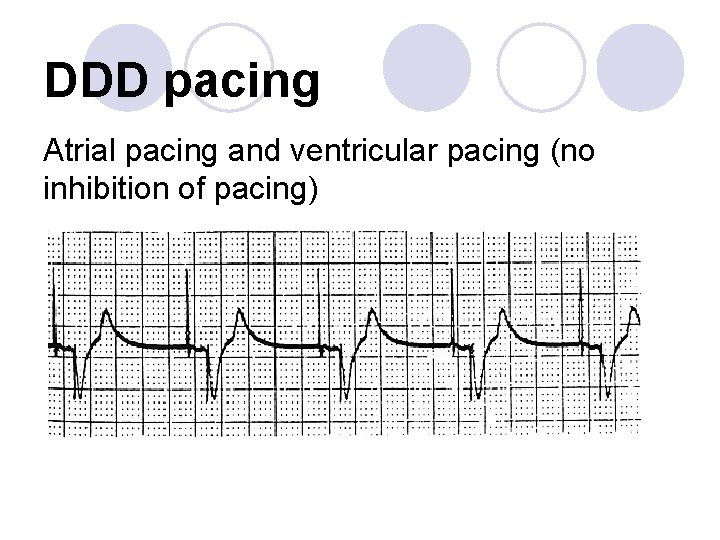
DDD pacing Atrial pacing and ventricular pacing (no inhibition of pacing)

DDD mode l May resemble other modes of pacing l Will strive to maintain AV synchrony with variable atrial rates and AV conduction

Dual Chamber Timing Parameters l Lower rate l Upper rate intervals
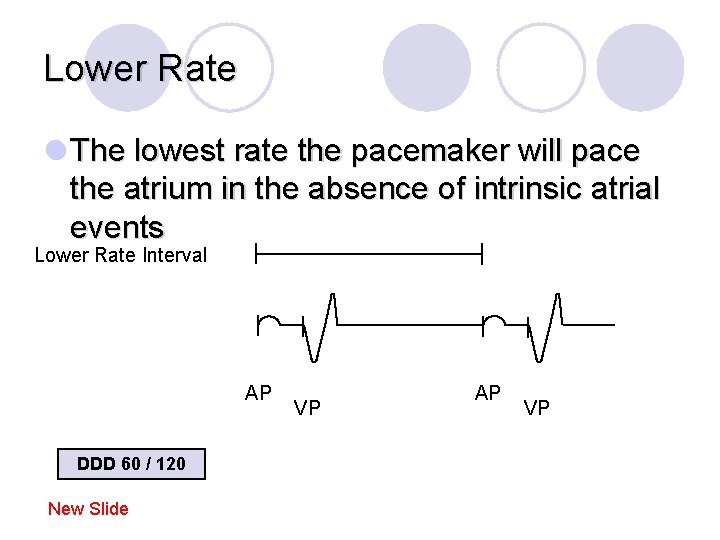
Lower Rate l The lowest rate the pacemaker will pace the atrium in the absence of intrinsic atrial events Lower Rate Interval AP DDD 60 / 120 New Slide VP AP VP
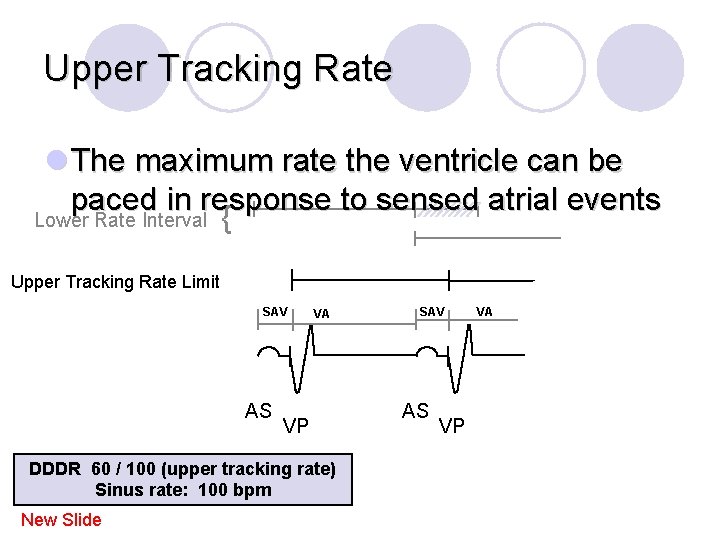
Upper Tracking Rate l The maximum rate the ventricle can be paced in response to sensed atrial events Lower Rate Interval { Upper Tracking Rate Limit SAV AS VA VP DDDR 60 / 100 (upper tracking rate) Sinus rate: 100 bpm New Slide SAV AS VP VA

Rate responsiveness/ adaptive-rate pacing The 4 th Letter in the NBG Code

Rate responsiveness/adaptive-rate pacing Rate response attempts to mimic the sinus node by increasing heart rate in response to increasing metabolic demand

Rate responsiveness/adaptive-rate pacing Sensor(s) detect changes in physiologic needs and increase the pacing rate accordingly

Rate responsiveness/adaptive-rate pacing The sensor detects changes by: ¡Sensing motion (crystal or accelerometer) ¡Sensing changes in intrathoracic impedance, e. g. , minute ventilation

DDDR pacing Example of Dual-Chamber Rate. Responsive pacing

Biventricular PPM or ICD A Brief Overview of What It Means To Bi. V Pace
Biventricular pacing Three lead system: l. Right atrial l. Right ventricular l. Left ventricular
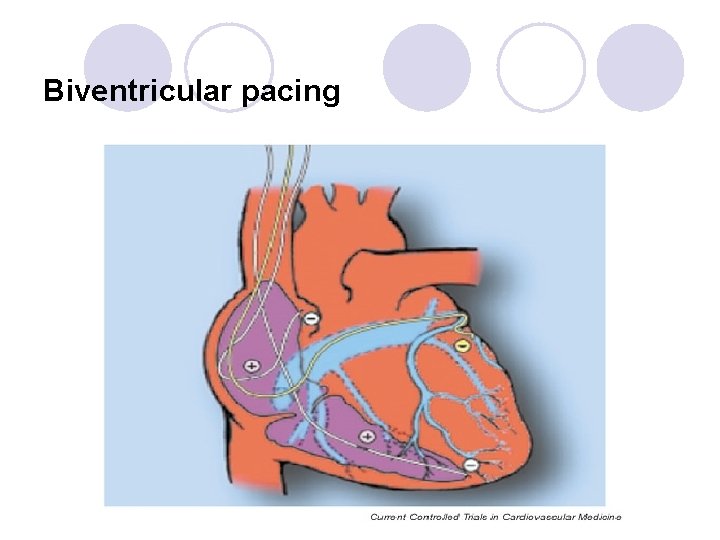
Biventricular pacing
Cardiac Resynchronization Therapy (CRT) Patient Indications l Bi-Ventricular ICD ¡Moderate to severe HF (NYHA Class III/IV) patients ¡Symptomatic despite optimal, medical therapy ¡QRS 130 msec ¡LVEF 35%

Biventricular pacing l Also known as cardiac resynchronization therapy, keeps the right and left ventricles pumping together by sending small electrical impulses to the heart muscle coordinating their contractions. l The heart is able to fill and pump blood more effectively. This along with medical therapy, helps to improve heart failure symptoms. l Improves quality of life in many.

Biventricular pacing Achieved by: l Inhibiting intrinsic ventricular rhythm l Ensure pacing in RV and LV l Short A-V delays to promote pacing in the ventricle

Break?

When Devices Go Bad!!!!
Complications of Device Implantation: q Pocket hematoma q Pocket infection q Pneumothorax q Cardiac perforation q Cardiac tamponade q Vascular damage l Lead dislodgement l Lead fracture l Lead infection l Inappropriate shocks

Laser Lead Extraction Program q. Implemented at UCH in 2008 by Chancey Weaver RN and Dr. Michelle Khoo M. D. q. First laser lead extraction in January 2009 q~30 leads extracted/year Reasons for a lead extraction: l l Fractured Leads Infected Lead(s) Non-functional leads/too many leads Regaining venous access
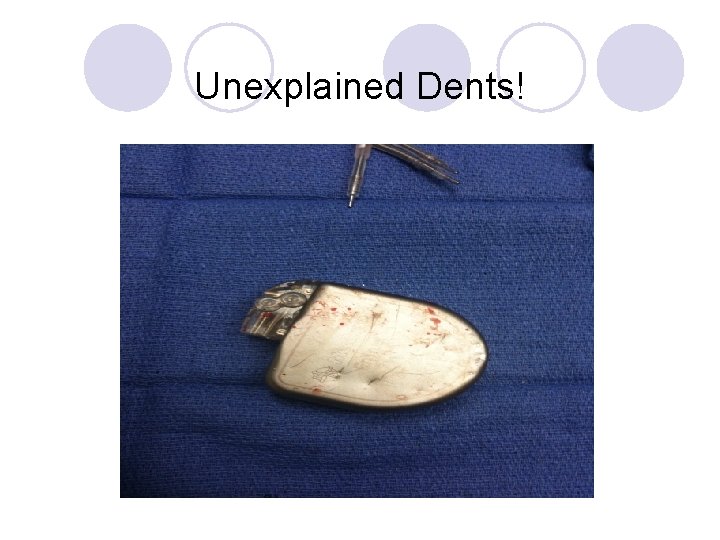
Unexplained Dents!
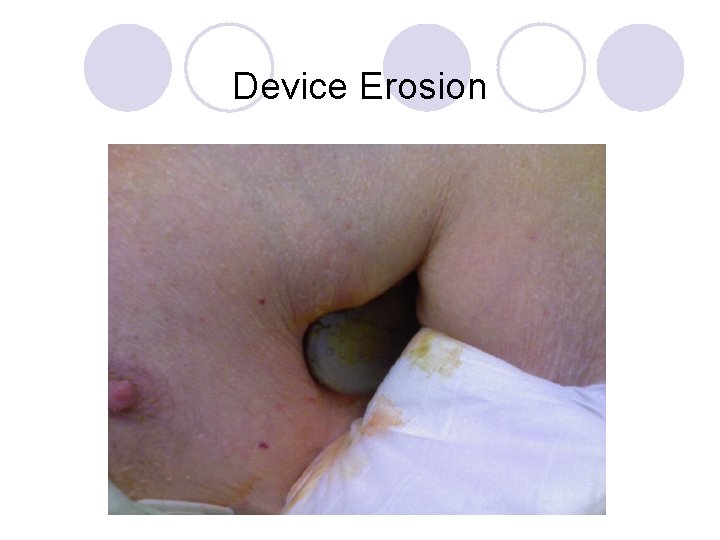
Device Erosion
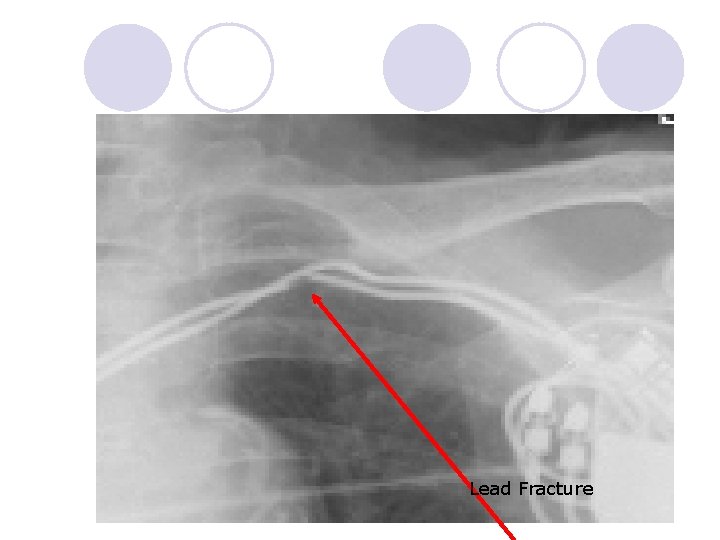
Lead Fracture
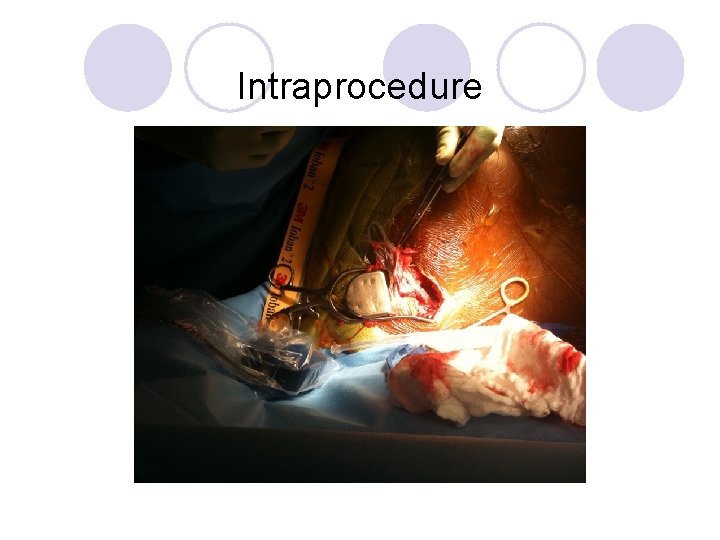
Intraprocedure

Extracted Lead

Extracted Generator and Lead

Nursing Considerations Preoperative ICD Placement and Postoperative Care

Preoperative l Left/right arm IV l Reinforce patient and family education ¡ EP department performs education prior to and after procedure, any further questions, please call the EP lab l NPO l Surgical site l Pre-op medications ¡ Antibiotics l Blood work (WBC, Platelets, INR, Basic) l Anesthesia in the procedure l Restrictions after procedure

Postoperative l Vital signs ¡ Changes may indicate pericardial effusion or pneumothorax l Type of device and settings l ECG interpretation and documentation, as per unit guidelines l Activity l HOB <30 degrees for the first 4 hours l Antibiotics l Incision site l X-ray within 1 hour of arriving back in room and X-ray in AM as well **Pt. placed in sling for 24 hours to allow leads to adhere to tissue**

Documentation l According to hospital policy: ¡ University of Colorado Hospital l Call report to telemetry: Include device manufacturer and model number, mode (VVI, DDD, etc. ), and lower and upper programmed rates (should be given in report). l Place in computerized documentation: Device manufacturer, mode, rate cut off, therapies, and date of implant. l If the device fires, document any therapies of the device including the precipitating dysrhythmia and outcome in your charting. Include ECG strips, if available, documenting the dysrhythmia, the delivery of therapy via the ICD and the resultant rhythm and the patient response.

Strip Documentation l According to hospital policy, and individual unit guidelines. ¡Minimal information includes “running” a strip every 12 hours or with a change in rhythm ¡Documentation: date, time, patient's name, medical record #, heart rate, PR, QRS, and QT intervals, and rhythm analysis
Patient and Family Education l Wound care ¡ S/S of infection ¡ No submersion under water for 3 weeks ¡ No direct water spray (shower spray) for 1 week l Coughing and deep breathing l Activity ¡ All information in Post Op packet ¡ NO lifting arm above shoulder for 6 weeks l Follow-up appointment l Remote interrogations l Electromagnetic interference l Identification card

Patients Admitted With a PPM or an ICD

Patients admitted with a PPM/ICD l Ask patient for device information, i. e. registration card l EP does not need to be consulted if a patient is admitted for a non-device related problem and the device appears to be working appropriately. l MRI not recommended (except new Medtronic PPM) l Pre-op/Post-op patients may require device programming changes ¡ ICD- tachy therapies off, or may fire during cautery ¡ PPM- reprogram to VOO, or may fail to pace appropriately

Pacemaker Practice Strips

What You Need to Document l Underlying rhythm? l Is it “a” paced, “v” paced or both Is the device doing what it is programmed to do?

Troubleshooting l Failure to: ¡Sense ¡Fire ¡Capture

How to interpret a “paced” strip: One method of many… 1. 2. 3. 4. Is intrinsic activity present? Are pacing spikes present: “A”, “V”, or both? Is 1: 1 capture present? Is intrinsic activity sensed appropriately? Over sensing- sensing of an inappropriate single Leads to underpacing Under sensing- failure to sense intrinsic cardiac signal Results in overpacing 5. What is the heart rate? 6. What is the programmed pacing rate? Compliments of Northwestern Memorial Hospital, October 2002
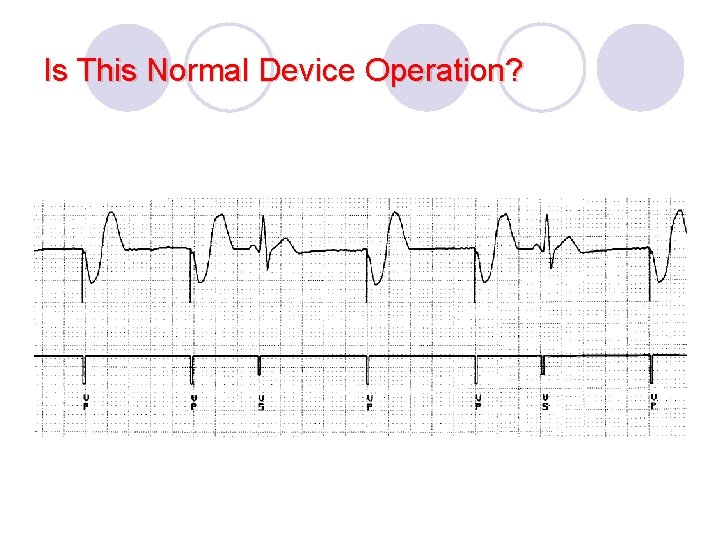
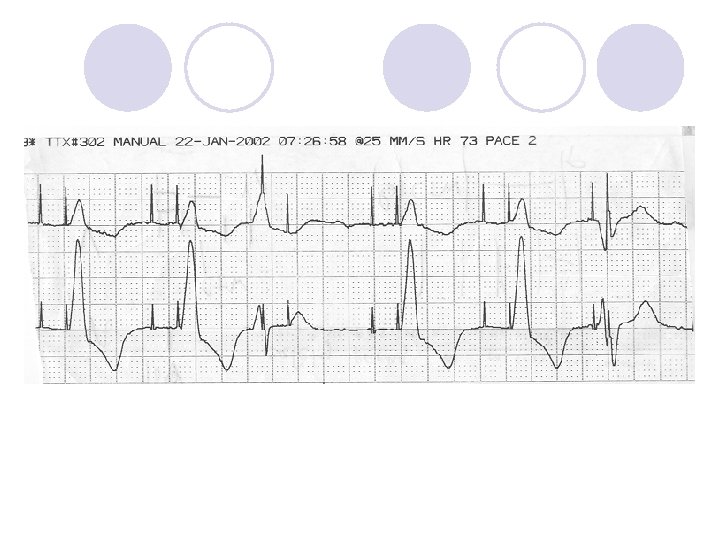
Is This Normal Device Operation?
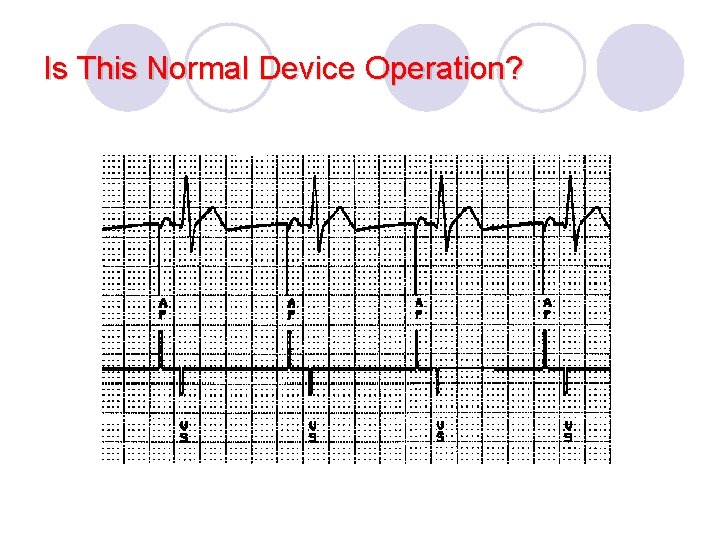
Is This Normal Device Operation?
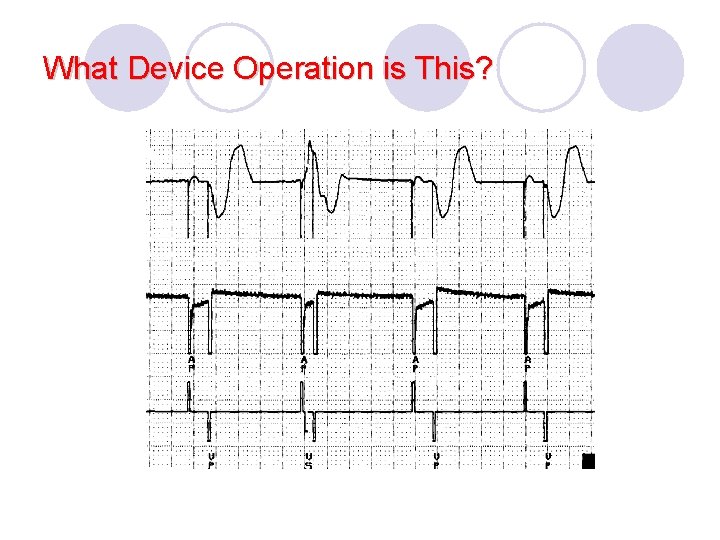
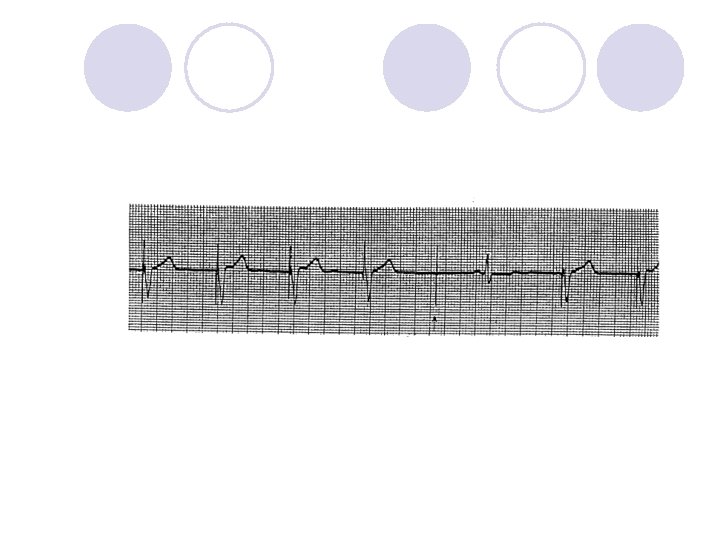
What Device Operation is This?
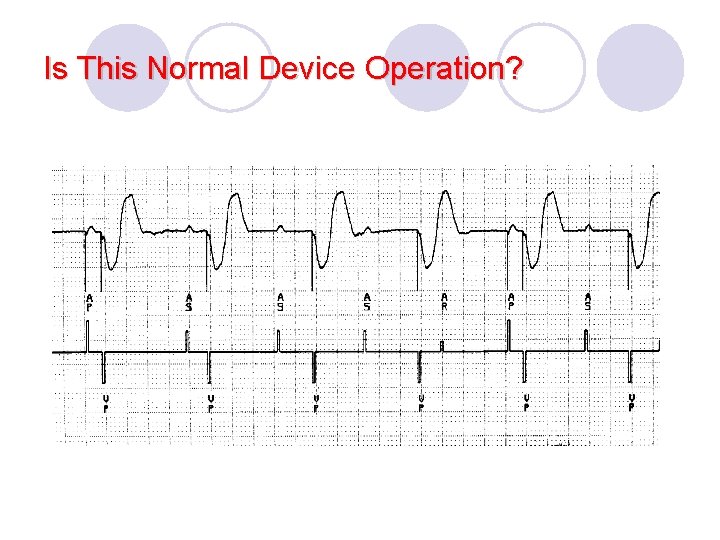
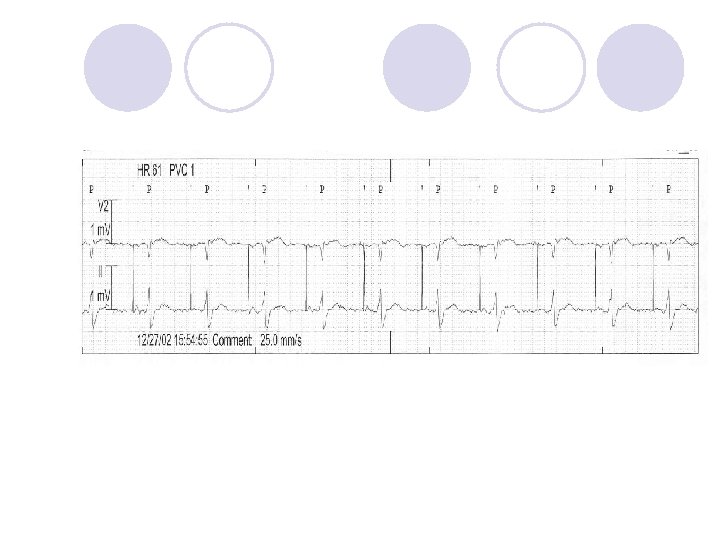
Is This Normal Device Operation?
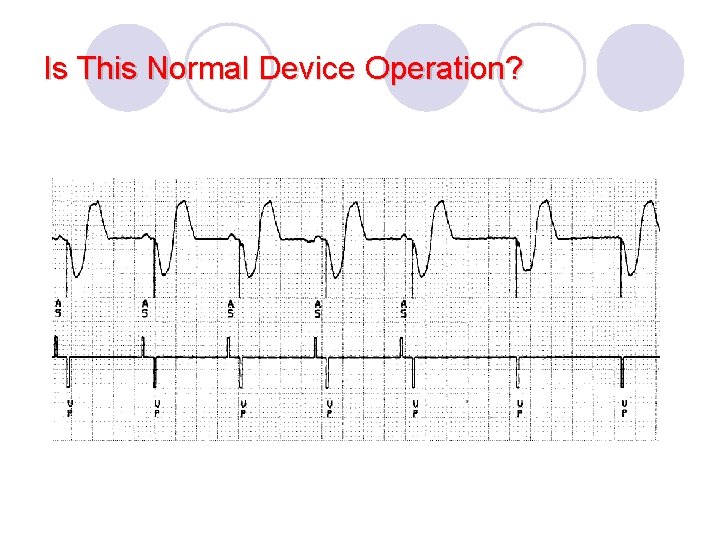
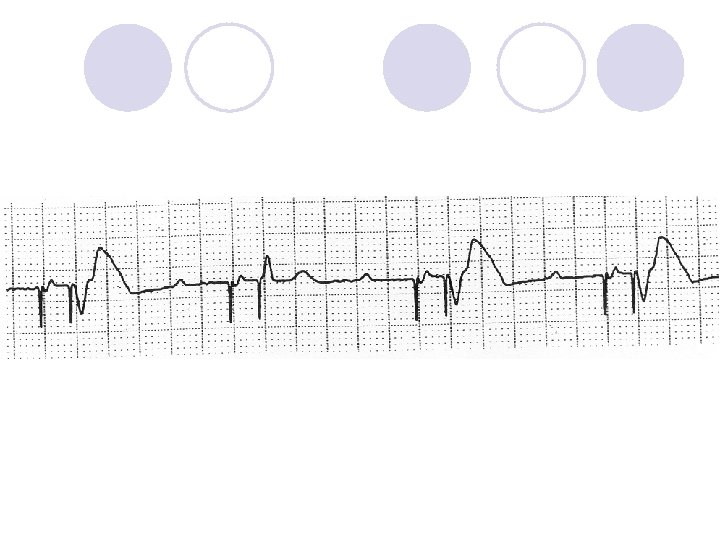
Is This Normal Device Operation?
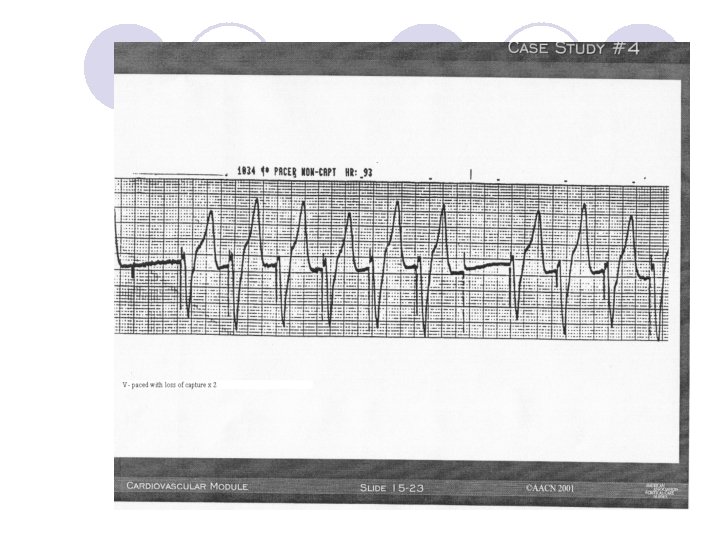
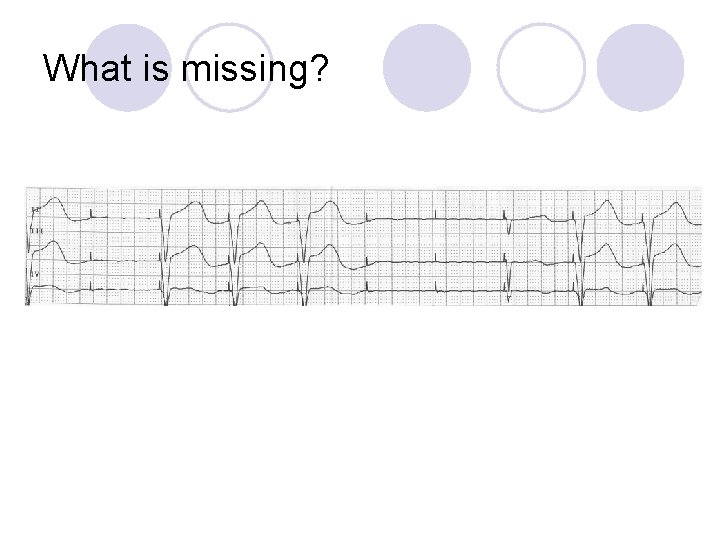
What is missing?


Thank You l Cardiac Electrophysiology ¡ ¡ ¡ Dena Keilman, RN Kari Jackson, RN Noelle Hernandez, RN Amanda Lange, RN Heidi Huber, RN Terri Rhodes, RN Dan Sullivan, RN Claire Rutherford, RN Matt Upton, RN Laura Hess, RN Diane Ridgway, RN Ann Czyz. RN ¡ William H. Sauer, MD ¡ Duy Nguyen, MD ¡ Paul Varosy, MD ¡ Ryan Aleong, MD ¡ Joe Schulller, MD ¡ Wendy Tzou, MD ¡ Christine Tompkins, MD ¡ David Katz, MD ¡ Cathy Kenny, ANP

References l l Burke M, et al. Safety and Efficacy of a Subcutaneous Implantable. Defibrillator (S-ICD System US IDE Study). Late-Breaking Abstract Session. HRS 2012.
- Slides: 109