CARDIAC II Katie Detrick RN BSN CCRN Abington

CARDIAC II Katie Detrick RN, BSN, CCRN Abington Jefferson Health Medical Intensive Care

DEFINITIONS OF HEART FAILURE • Inability of the heart to pump blood through the systemic circulation in an amount sufficient to meet the body’s needs • Causes include anatomical, physiological, and non-cardiac

DETERMINATION OF SEVERITY OF HEART FAILURE NY Heart Association Functional Classification System ◦ Class I – Minimal ◦ Class II – Mild ◦ Class III – Moderate ◦ Class IV - Severe

ACTIVATION OF THE NEUROHORMONAL SYSTEM ADRENERGIC ACTIVATION • Baroreceptors: • Low BP/CO = Activation of the sympathetic nervous system • Norepinephrine and epinephrine released • Increased heart rate and contractility • Alpha 1 stimulation = vasoconstriction • Beta blockers

ACTIVATION OF THE NEUROHORMONAL SYSTEM Renin-Angiotensin-Aldosterone • Low BP/CO causes • Decreased glomerular filtration rate • Renin released • Angiotensin I released • Converts to Angiotensin II • Vasoconstriction • Aldosterone released • Sodium and Water retained • ACE • ARB • Aldactone • Nesiritide

END RESULT • Increased heart rate • Increased contractility • Vasoconstriction • Sodium and Water Retention • Increased cardiac output and blood pressure

NEUROHORMONAL MECHANISMS IN HF Results in structural changes ◦ Chamber dilation ◦ Damaged myocytes ◦ Spherical shape Decreased functioning

HEART FAILURE SYMPTOMS • Dyspnea • Fatigue • Fluid retention, decreased urinary output • Decreased exercise tolerance • Cool skin

EFFECTS OF HF ON CO Heart rate Stroke volume ◦ Preload ◦ Afterload ◦ Contractility

RIGHT VS LEFT SIDED HEART FAILURE LEFT VENTRICLE • Orthopnea • Dyspnea on exertion • Crackles • Low oxygen saturation • S 3 and S 4 • Systolic murmur • Oliguria • PAWP> 20 mm Hg • SVR > 1200 • Cardiac output < 4 RIGHT VENTRICLE • Distended neck veins • Dependent edema • Hepatic engorgement • Hepatojugular reflux • Anorexia/nausea • Weight gain • CVP > 8 mm. Hg • PVR>300

SYSTOLIC VS DIASTOLIC DYSFUNCTION SYSTOLIC DIASTOLIC Decrease in muscle strength Inability of the ventricle to fully relax Forward blood flow falls Increased pressure and volume in the ventricle Systemic hypo perfusion occurs Stroke volume/ejection fraction falls Decreases forward blood flow Pulmonary congestion occurs Strength of heart is normal (EF is normal) Stroke volume is reduced

DIAGNOSTIC TESTING CXR ◦ Enlarged cardiac silhouette ◦ Kerley B lines ◦ Pleural effusion ECG ◦ Q waves ◦ IVCD ◦ AF ◦ Ventricular ectopy ◦ Atrial enlargement ◦ Ventricular hypertrophy

DIAGNOSTIC TESTING Both nonspecific Two-dimensional echocardiogram with Doppler flow studies ◦ Abnormal wall motion ◦ Chamber dilation ◦ Hypertrophy ◦ Valve dysfunction ◦ Decreased ejection fraction ◦ Most useful test

LABS • CBC • Electrolytes • BUN, creatinine • Liver enzymes • Thyroid testing B-type natriuretic peptide ◦ Elevated in proportion to severity of HF ◦ Correlate with NYHA

TREATMENT OF HEART FAILURE • Reverse the cause Surgery to repair anatomical problem Treat the physiological cause • Decrease the “bad” effects of the compensatory mechanisms Major treatments are pharmacologic

DIURETICS – REDUCE PRELOAD ◦ Loop Lasix (furosemide), Bumex (bumetanide) ◦ K+-sparing (Aldosterone antagonist) Aldactone (spironolactone) ◦ Thiazide Zaroxolyn (metolazone )
VASODILATORS – DECREASE PRELOAD, AFTERLOAD ACE inhibitors ◦ Capoten (captopril) Vasotec (enalapril) ARBs Beta-blockers ◦ Zebeta (bisoprolol) ◦ Coreg (carvedilol) ◦ Lopressor (metoprolol) ◦ Cozaar (losartan) Diovan (valsartan) Nitroglycerin Hydralazine (Apresoline) B-type natriuretic Peptide o. Nesiritide (Natrecor)

INOTROPES • Cardiac glycosides: Digoxin (Lanoxin) • Sympathomimetics: Dobutamine (Dobutrex) • Phosphodiesterase Inhibitors: Amrinone (Inocor) and Milrinone (Primacor) • All work to increase the force of myocardial contraction and increase stroke volume and cardiac output

NON-PHARMACOLOGICAL INTERVENTIONS– OXYGEN THERAPY CPAP or Bi. PAP ◦ Noninvasive - increase in intrathoracic positive pressure decreases preload ◦ Mechanical ventilation if NIPPV not effective and/or cardiogenic shock
ICD Atrium • AT/AF tachyarrhythmia detection • Antitachycardia pacing • Cardioversion Decreases incidence of sudden death Ventricle • Antitachycardia pacing • Cardioversion • VT/ VF detection • Defibrillation Atrium & Ventricle Bradycardia sensing & pacing
CARDIAC RESYNCHRONIZATION Asynchrony due to IVCD; worsens HF Synchronization improves NYHA classification, improves exercise tolerance & QOL

ULTRAFILTRATION • Removal of fluid only • Ultrafiltration mode of CRRT or specialized pump through central line • Does not require dialysis catheter • Maximum fluid removal 500 ml/hr • Well tolerated

NURSING INTERVENTIONS Pt assessment q 1 -20 ◦ VS, LOC ◦ Head-to-toe assessments Heart sounds ◦ S 3, gallop, murmur, distant Neuro ◦ Decreased mentation ◦ Indicates poor perfusion to brain Edema Peripheral pulses Skin ◦ Temp, color, moisture Nailbeds ◦ Color, cap refill
PULMONARY • Crackles • Wheezes • Tachypnea • Frothy sputum GI • Nausea • Vomiting • Decreased appetite • Diminished bowel sounds
RENAL Urine output ◦ Oliguria ◦ Anuria ◦ Concentrated ◦ Dilute • Daily weights • Electrolytes
CARDIOMYOPATHIES

CARDIOMYOPATHY • Dilated • Most common type • Hypertrophic • Constrictive
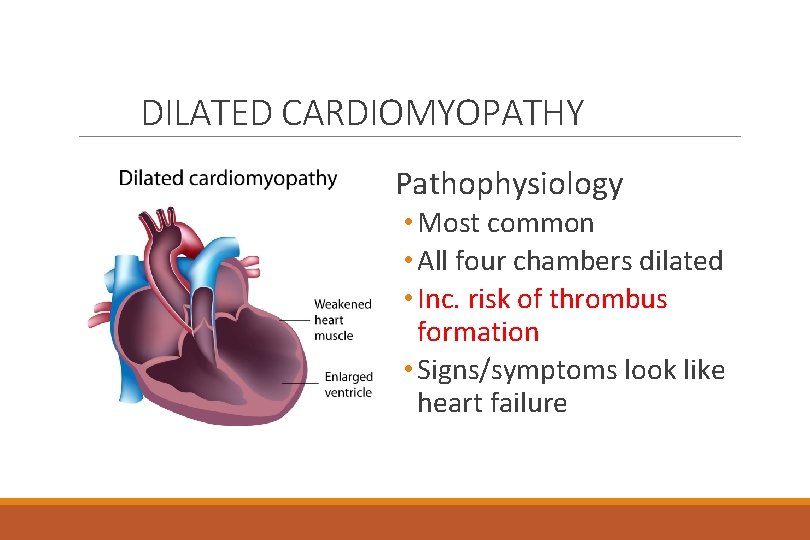
DILATED CARDIOMYOPATHY Pathophysiology • Most common • All four chambers dilated • Inc. risk of thrombus formation • Signs/symptoms look like heart failure

MEDICAL MANAGEMENT AND PHARMACOLOGY OF DILATED CM Medical Mgmt Pharmacology ◦ Treat as for heart failure ◦ Inotropes ◦ May be candidate for ◦ Diuretics heart transplant ◦ Vasodilators ◦ ACE inhibitors ◦ Antidysrhythmics ◦ Anticoagulants**
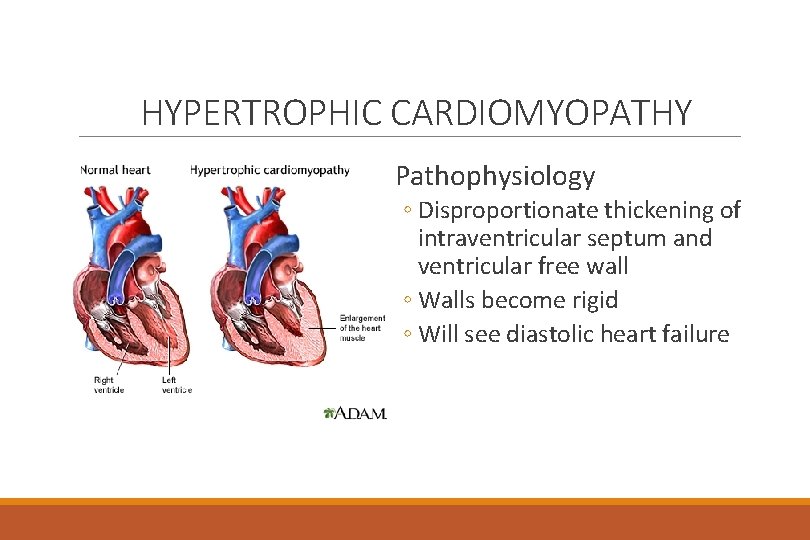
HYPERTROPHIC CARDIOMYOPATHY Pathophysiology ◦ Disproportionate thickening of intraventricular septum and ventricular free wall ◦ Walls become rigid ◦ Will see diastolic heart failure
CLINICAL MANIFESTATIONS OF HYPERTROPHIC CM • Dyspnea • Fatigue • Chest pain • Heart failure • Murmur of aortic stenosis and mitral regurgitation** • Syncope**

HEMODYNAMICS OF HYPERTROPHIC CM • CO normal at rest due to increased filling pressures that increase stroke volume** • CVP, PAWP, SVR increased

MEDICAL MANAGEMENT AND PHARMACOLOGY OF HYPERTROPHIC CM Medical Mgmt • Minimize obstruction of outflow tract • Maintain adequate filling pressures • IV fluids • Heart transplant Pharmacology • β-blockers • Ca++ channel blockers • NO inotropes • Caution with nitrates and diuretics
RESTRICTIVE CARDIOMYOPATHY Pathophysiology • Abnormal diastolic filling due to rigid ventricular walls • Contractility mostly unimpaired • Least common
CLINICAL MANIFESTATIONS OF RESTRICTIVE CM • Dyspnea • Fatigue • Chest pain • Heart failure • Edema
HEMODYNAMICS OF RESTRICTIVE CM • CO decreased • CVP, PAWP, SVR increased • Consistent with heart failure

MEDICAL MANAGEMENT AND PHARMACOLOGY OF RESTRICTIVE CM Medical Mgmt ◦ Treat as for heart failure ◦ Alcohol ablation of obstruction ◦ May be candidate for heart transplant Pharmacology ◦ Inotropes ◦ Diuretics ◦ Vasodilators ◦ ACE inhibitors ◦ Antidysrhythmics

VALVULAR DISEASE Stenotic or Regurgitant ◦ Stenotic - Valve opening decreases in size; chamber hypertrophies ◦ Regurgitation – also known as insufficiency or incompetent; valve does not completely close; dilated chamber ◦ Ms. Ard and Mr. Ass ◦ “MS/AR Diastolic MR/AS Systolic”
ETIOLOGY • Rheumatic heart disease • Calcification • Congenital malformation • Endocarditis • Marfan’s syndrome • Hypertension • Connective tissue disease • Trauma • Aortic and mitral valves most commonly affected
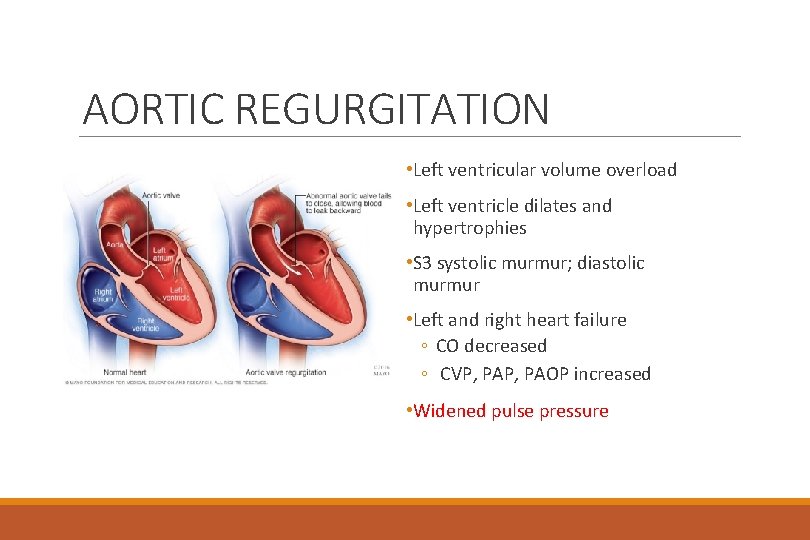
AORTIC REGURGITATION • Left ventricular volume overload • Left ventricle dilates and hypertrophies • S 3 systolic murmur; diastolic murmur • Left and right heart failure ◦ CO decreased ◦ CVP, PAOP increased • Widened pulse pressure
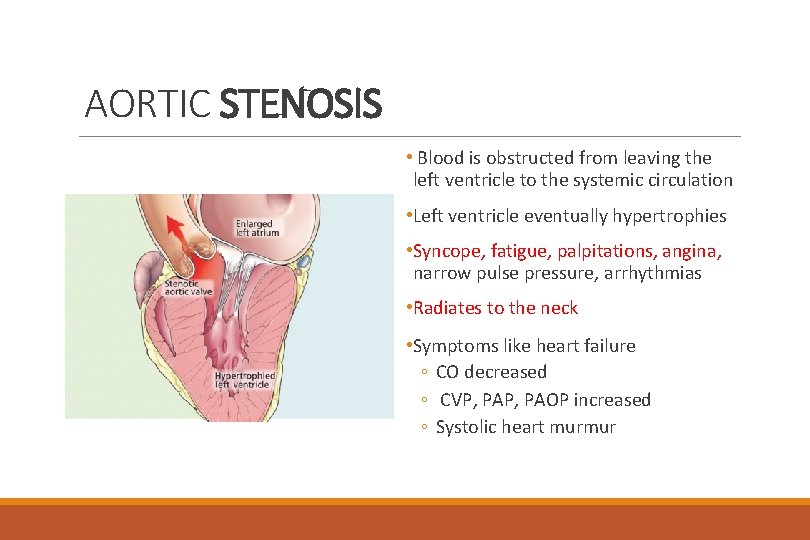
AORTIC STENOSIS • Blood is obstructed from leaving the left ventricle to the systemic circulation • Left ventricle eventually hypertrophies • Syncope, fatigue, palpitations, angina, narrow pulse pressure, arrhythmias • Radiates to the neck • Symptoms like heart failure ◦ CO decreased ◦ CVP, PAOP increased ◦ Systolic heart murmur
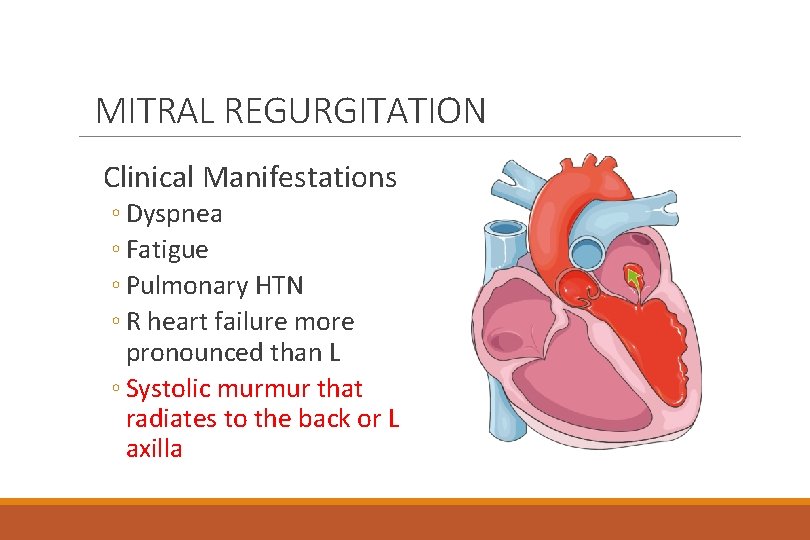
MITRAL REGURGITATION Clinical Manifestations ◦ Dyspnea ◦ Fatigue ◦ Pulmonary HTN ◦ R heart failure more pronounced than L ◦ Systolic murmur that radiates to the back or L axilla

MITRAL REGURGITATION ECG ◦ Atrial fibrillation Hemodynamics ◦ CO decreased ◦ CVP, PAOP increased ◦ As with heart failure
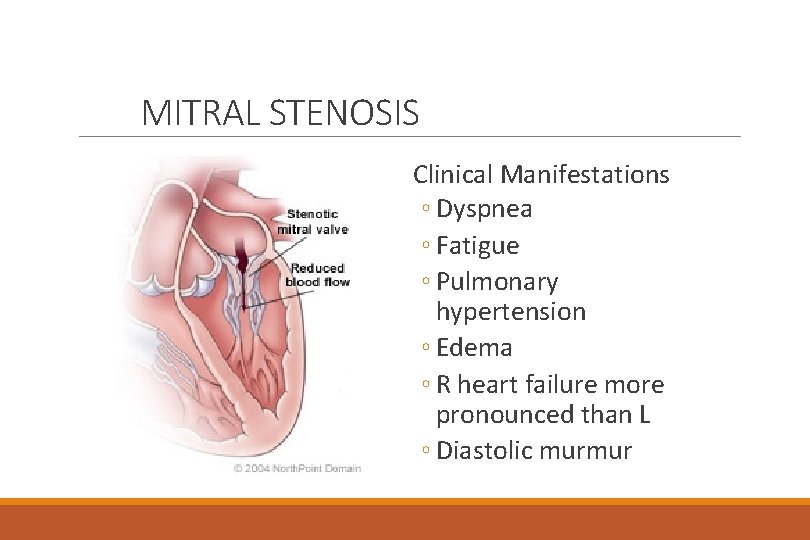
MITRAL STENOSIS Clinical Manifestations ◦ Dyspnea ◦ Fatigue ◦ Pulmonary hypertension ◦ Edema ◦ R heart failure more pronounced than L ◦ Diastolic murmur

MITRAL STENOSIS ECG ◦ Atrial fibrillation Hemodynamics ◦ CO decreased ◦ CVP, PAOP increased ◦ As with HF

MEDICAL MANAGEMENT Activity restriction Sodium and fluid restriction Oxygen Heart failure management Management of complications ◦ Dysrhythmias ◦ Emboli

SURGICAL MANAGEMENT Valvuloplasty ◦ Repair of valve Commissurotomy ◦ Surgical separation of valve leaflets Valve Replacement ◦ ◦ ◦ Homograft - From human cadaver Heterograft - From animal Artificial – Manufactured Post-op care similar to CABG
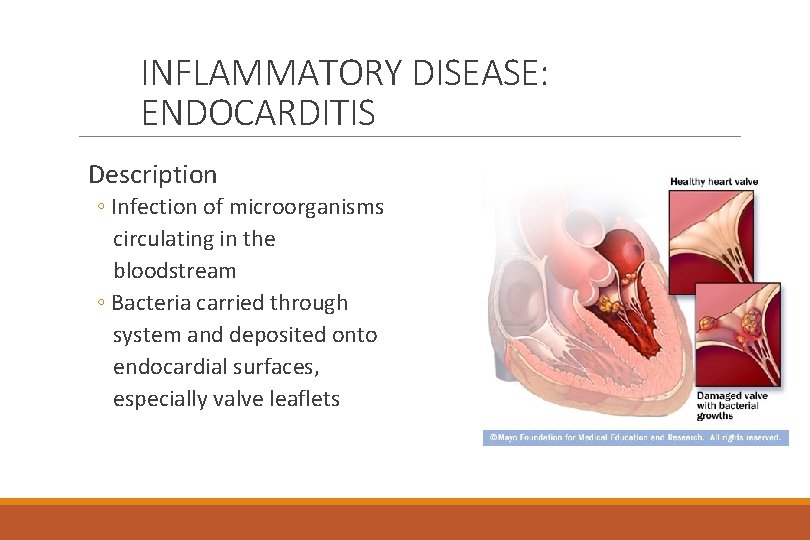
INFLAMMATORY DISEASE: ENDOCARDITIS Description ◦ Infection of microorganisms circulating in the bloodstream ◦ Bacteria carried through system and deposited onto endocardial surfaces, especially valve leaflets

INFECTIOUS PROCESS Bacteria grow on leaflets –Vegetation Lesions or vegetations form on valves Valves have irregular or “cauliflower” appearance Leaflets damaged and dysfunctional

INFECTIOUS PROCESS Life-threatening May require valve surgery Can grow to involve the: ◦ Chordae tendinea ◦ Papillary muscles ◦ Conduction system

ORGANISMS & VALVES Organisms ◦ Streptococcus ◦ Most common ◦ Staphylococcus ◦ Gram negative bacilli ◦ E. coli ◦ Klebsiella ◦ Fungi ◦ Candida ◦ Histoplasma Valves ◦ Mitral most commonly affected ◦ Aortic second most affected

POPULATIONS AT RISK Rarely occurs in people with normal hearts IV drug abuse Risk increased with preexisting cardiac conditions • Prosthetic valves • History of previous endocarditis • Damaged or abnormal heart valves due to: • Rheumatic fever • Congenital heart disease • Congenital valve defects

PRESENTING SYMPTOMS Dependent on: • Valve involved • Organism • Duration of time • Extent of vegetative growth

PRESENTING SYMPTOMS • Fever • Fatigue • Chills • Headache • Night sweats • Musculoskeletal complaints • Cough • New murmur • Weight loss • Heart failure • General malaise • Positive blood cultures • Weakness • Anemia

TREATMENT • Blood cultures to identify organism • Administration of antibiotics or antifungals • Oxygen if indicated • HF treatment if present • May require valve replacement surgery

EXAM QUESTIONS A patient with heart failure is receiving diuretics, beta-blockers, and ACE inhibitors. The patient has a weight gain of 2 kg and severe shortness of breath. BP is 100/76 mm Hg, HR 70/min, RR 26/min. The nurse anticipates administering 40 mg IV furosemide (Lasix) and:

EXAM QUESTIONS A. Discontinuing beta-blocking medications B. Decreasing beta-blocker dosage C. Administering an additional dose of beta-blocker D. Administering an additional dose of ACE inhibitor

EXAM QUESTIONS A patient is admitted with complaints of chest pain accompanied by nausea and vomiting. The skin is cool and clammy. The following are noted: VS: BP 140/90; HR 120; RR 26 CO 3. 5 L/min; CI 2. 1 L/min/M 3 CVP 10 mm. Hg; PAOP 20 mm. Hg Presence of S 3 12 lead ECG shows acute changes in V 3 -V 4

EXAM QUESTIONS For this patient, the goals of therapy would be to: A. B. C. D. Decrease preload and afterload Increase contractility and preload Decrease contractility and afterload

EXAM QUESTIONS A patient with acute decompensated heart failure is receiving a continuous infusion of nesiritide (Natrecor) at 0. 01 mcg/kg/min. Currently, the patient has the following vital signs: HR 116 bpm, sinus tachycardia with premature atrial contractions, BP 78/48 mm. Hg, RR 28/min, and Sp. O 2 90% on 40% Bi. PAP mask. Immediate interventions by the nurse would include which of the following?

EXAM QUESTIONS A. Discontinue the nesiritide (Natrecor) infusion B. Place the patient in a supine position C. Administer a 250 ml normal saline fluid bolus D. Continue the nesiritide (Natrecor) infusion and administer 40 mg furosemide (Lasix) intravenously

EXAM QUESTIONS Which of the following medications is administered to prevent sudden death associated with dilated cardiomyopathy? . A. Warfarin (Coumadin) to prevent clot formation B. Calcium channel blockers to control tachycardia C. Nitrates to improve coronary artery perfusion D. Digoxin to reduce atrial dysrhythmias and improve contractility

EXAM QUESTIONS Which of the following medications may worsen symptoms of heart failure associated with hypertrophic cardiomyopathy? A. Calcium channel blockers B. Beta-blockers C. Nitroglycerin D. Amiodarone

EXAM QUESTIONS Chest pain associated with aortic stenosis can be caused by: A. Decreased stroke volume B. Disproportionate oxygen supply versus demand C. Prolapsed valve leaflets D. Decreased contractility

EXAM QUESTIONS Which of the following medication regimens would be most appropriate to relieve chest pain in a patient with a diagnosis of myocarditis? A. Nitroglycerin 1/150 grains sublingual B. Furosemide 40 mg IV C. Ibuprofen 800 mg PO D. Morphine sulfate 2 mg IV

DYSRHYTHMIAS Any cardiac rhythm other than sinus rhythm Too fast, too slow Will see S/S of decreased CO D/T MI, ischemia, hypoxemia

CLINICAL MANIFESTATIONS Anxiety, dizziness, syncope Restlessness, confusion Cool, clammy skin Chest pain, dyspnea Hypotension, oliguria Pulmonary edema
ANTIDYSRHYTHMIC THERAPY Asystole, PEA › Epinephrine Pulseless VT, VF » Shock » Epinephrine » Amiodarone Tachydysrhythmias » Adenosine » Amiodarone Bradydysrhythmias » Atropine » TCP

PACEMAKER THERAPY Indications Types of temporary pacing ◦ 2 nd degree AVB type II ◦ Transcutaneous ◦ 3 rd degree AVB ◦ Transvenous ◦ AF with slow ◦ Epicardial ventricular response Pacing codes (not TCP) ◦ Symptomatic ◦ First letter = chamber paced bradycardia ◦ Second letter = chamber sensed ◦ Third letter = response to sensing
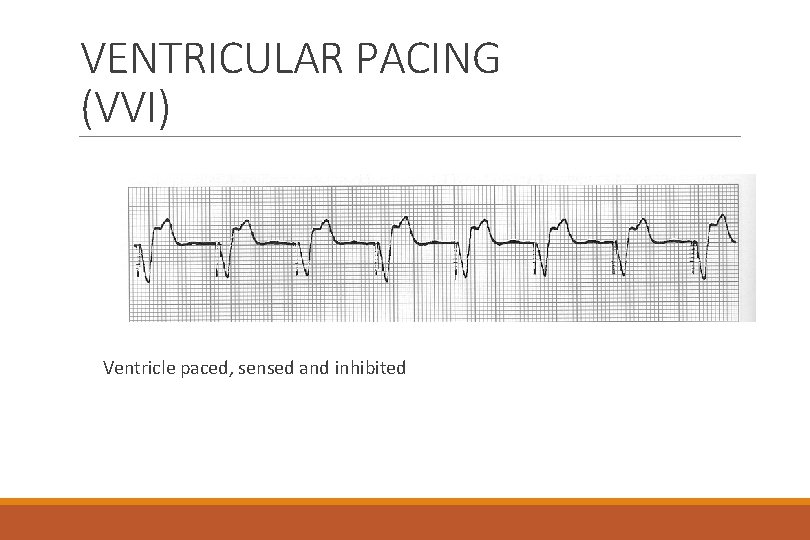
VENTRICULAR PACING (VVI) Ventricle paced, sensed and inhibited
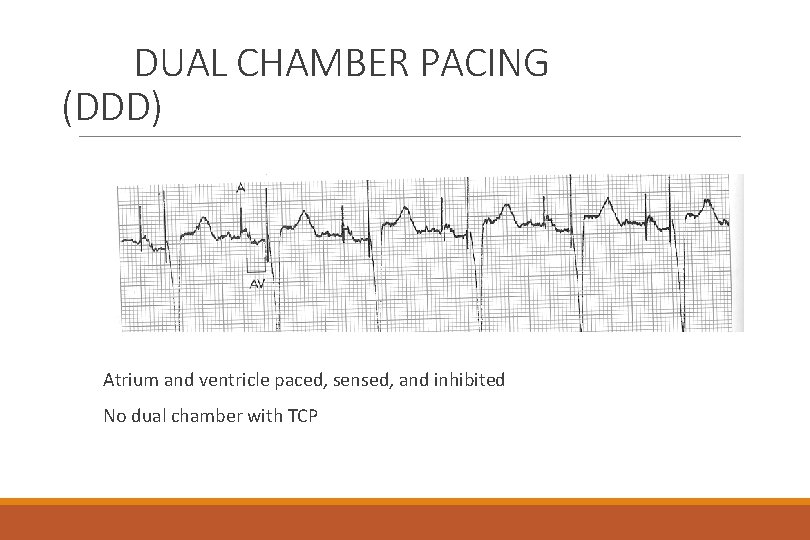
DUAL CHAMBER PACING (DDD) Atrium and ventricle paced, sensed, and inhibited No dual chamber with TCP

TRANSCUTANEOUS PACING Does not use letter system; only two types of settings Demand (Synchronous) ◦ Paces only when patient’s HR falls below set rate ◦ Appearance similar to VVI Fixed (Asynchronous) ◦ Unable to obtain capture ◦ Pacer unable to sense intrinsic activity ◦ Artifact prevents sensing ◦ Danger of pacemaker spike falling on T wave and causing ventricular tachycardia or ventricular fibrillation

PACEMAKER SETTINGS • Rate • Output (m. A) • Threshold • Sensitivity

INITIATING PACING Set heart rate and AV control per physician order Determine threshold ◦ Set m. A 2 -3 times higher than threshold to ensure capture ◦ TCP may increase m. A by 10% after capture obtained

INITIATING PACING Set sensitivity control so that pacemaker senses the heart’s intrinsic electrical activity (R wave) ◦ Ensure that sensitivity not so low that it also senses lower amplitude electrical signals such as the T wave ◦ Will consider it to be an R wave and double-count rate ◦ Will not pace when HR is below set rate ◦ No sensitivity on TCP

TCP PREPARATION Explain to patient and family ◦ TCP will be uncomfortable ◦ May require analgesia Thoroughly wash and dry skin ◦ Use skin preparation Pad placement ◦ Anterior-posterior preferred ◦ Anterior-anterior may need to be used

NURSING CARE All ◦ Report settings as part of shift change ◦ Check connections Transvenous and epicardial: ◦ Wear gloves when handling pacing wires ◦ Cover when not in use; secure to patient ◦ Secure pacemaker box ◦ Patient’s waist ◦ Telemetry pouch ◦ Hang from IV pole

NURSING CARE Transvenous and epicardial: ◦ Extra batteries ◦ Site care TCP ◦ Assess integrity of TCP pads ◦ Assess skin integrity ◦ Be sure TCP is plugged in

MONITOR FOR MALFUNCTION: FAILURE TO CAPTURE Pacemaker spikes not followed by complex ◦ Low battery; m. A too low; transvenous lead: fibrin at tip, movement from wall
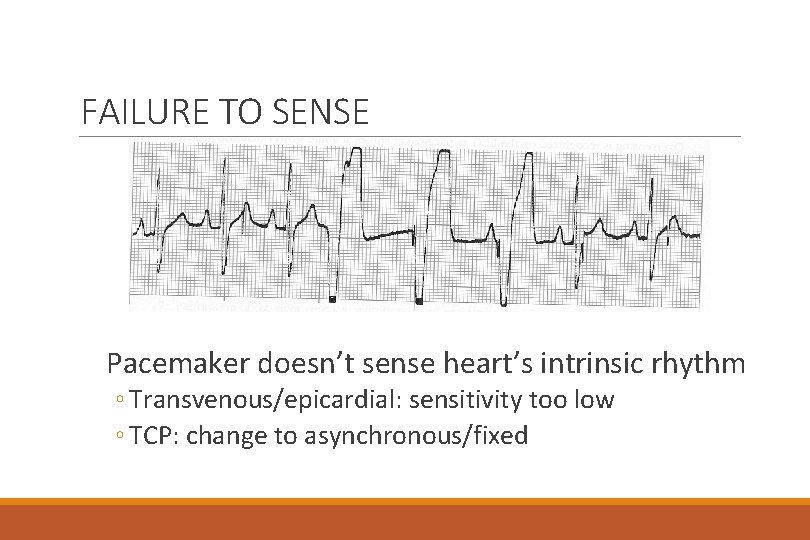
FAILURE TO SENSE Pacemaker doesn’t sense heart’s intrinsic rhythm ◦ Transvenous/epicardial: sensitivity too low ◦ TCP: change to asynchronous/fixed

EXAM QUESTIONS The nurse should perform which of the following interventions for a patient with chest pain, hypotension and tachycardia at a rate of 180 bpm? A. Administer amiodarone 150 mg IV over 10 minutes B. Administer adenosine 6 mg rapid IV push C. Perform synchronized cardioversion D. Defibrillate with 300 joules

EXAM QUESTIONS In a coronary care unit in which medications are not permitted to be left at the bedside and the crash cart with monitor/ transcutaneous pacemaker/ defibrillator is outside the central nurses’ station, a patient develops 3 rd degree AV block at a rate of 35 beats/minute with signs of poor tissue perfusion.

EXAM QUESTIONS The most appropriate initial intervention for the nurse assigned to this patient would be to: A. Initiate transcutaneous pacing B. Administer Atropine 0. 5 mg IV C. Initiate an infusion of Epinephrine at 5 mcg/min D. Initiate an infusion of Dopamine at 5 mcg/kg/min
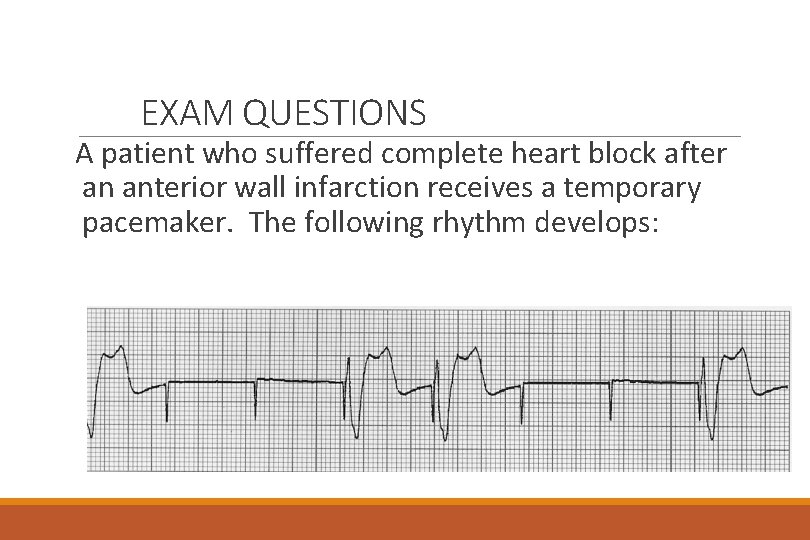
EXAM QUESTIONS A patient who suffered complete heart block after an anterior wall infarction receives a temporary pacemaker. The following rhythm develops:

EXAM QUESTIONS The nurse would respond by initiating which pacemaker action: A. Changing the pacing mode from paced to fixed (asynchronous). B. Increasing the output (m. A) C. Decreasing the output (m. A) D. Increasing the paced rate
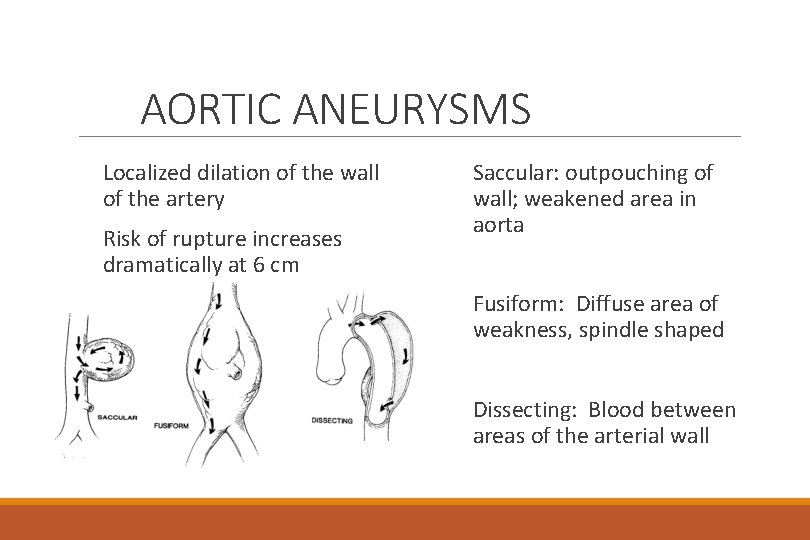
AORTIC ANEURYSMS Localized dilation of the wall of the artery Risk of rupture increases dramatically at 6 cm Saccular: outpouching of wall; weakened area in aorta Fusiform: Diffuse area of weakness, spindle shaped Dissecting: Blood between areas of the arterial wall
TYPES OF ANEURYSM Rupture Artery wall ruptures Blood leaks into mediastinum or abdomen

ETIOLOGY • 90% have h/o hypertension • Atherosclerosis • Blunt trauma • Marfan’s syndrome • Pregnancy
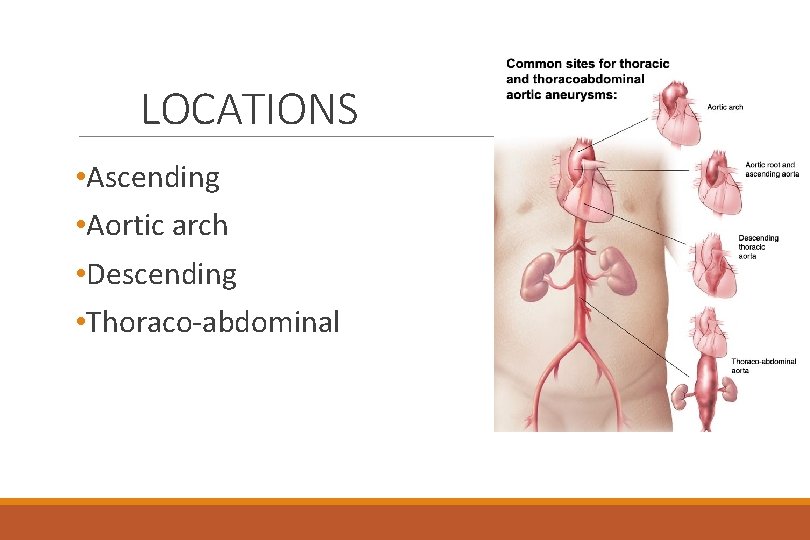
LOCATIONS • Ascending • Aortic arch • Descending • Thoraco-abdominal

CLINICAL MANIFESTATIONS • Ascending • Dyspnea, chest pain, widened pulse pressure, bounding pulse, aortic murmur • Aortic arch • Dyspnea, stridor, cough, chest pain, JVD, crackles, S 3 • Descending thoracic • Dull pain between shoulders, lower back • Abdominal • Dull and constant back pain, abdominal pain
DISSECTION PRESENTATION • Sudden intense, severe, tearing pain in the chest or abdomen • Severe hypertension • Acute neurologic deficits • Thoracic: BP or pulse difference between arms, new aortic regurgitation murmur

MEDICAL MANAGEMENT • Control risk factors • Check size every 6 months • Elective surgery when aneurysm is 6 cm

MEDICAL/SURGICAL • Dissection: • Vasodilators • Goal: MAP 80 -90 mm. Hg • IV fluids • Oxygen • Monitor UO, mental status, VS • Hypotension can indicate rupture • Surgery • Interventional

SURGICAL MANAGEMENT • Cross clamping of aorta • Placement of Dacron graft inside aneurysm • Sutured to proximal and distal aorta • Aneurysm wall closed over graft ◦

INTERVENTIONAL MANAGEMENT • Endovascular stent grafting • Descending thoracic and abdominal aneurysms • Graft fabric over metal mesh inserted through femoral artery • Placed at area of dissection

COMPLICATIONS OF SURGERY • Monitor for signs/symptoms of an MI • Bleeding • D/T hemorrhage or coagulopathy • Most common complication • Monitor S/S hypovolemia

COMPLICATIONS OF SURGERY • Renal failure • D/T cross clamping time, emboli • Monitor I&O, BUN, creatinine • Limb ischemia • D/T aeroembolism, cross clamp time • Assess distal pulses, skin temp, color, sensation, pain

COMPLICATIONS OF SURGERY • Colon ischemia • D/T emboli, cross clamp time • Assess bowel sounds, abdominal pain, melena • High mortality

COMPLICATIONS OF INTERVENTIONAL • Renal failure • Bowel infarction • Lower extremity embolism • Paraplegia/paraparesis
PERIPHERAL VASCULAR DISEASE • Peripheral arterial disease (PAD) • Can occur in any peripheral artery • More painful in lower extremity arteries • Common sites • Femoral artery • Popliteal artery • Distal aorta and iliac arteries

CAUSES AND RISK FACTORS • Atherosclerosis most common • Risk factors same as for CAD • Diabetes • Smoking • Hypertension • Hyperlipidemia • Male gender

DIAGNOSIS • Ankle-brachial index (ABI) • Noninvasive • Compares SBP of arm and leg, just above ankle • Arm SBP divided into ankle SBP • Lower the value, greater the symptoms • <0. 4 is severe PAD Typically asymptomatic until well advanced

CLINICAL MANIFESTATIONS • Thickened nails • Hair loss on lower leg, feet, and toes • Coolness • Intermittent claudication • Rest pain • Requires catheter or surgical intervention • Acute occlusion • Sudden onset of severe pain, loss of pulses, coldness • Requires immediate intervention

INTERVENTIONS • Pharmacologic management • • • Anticoagulants Vasodilators Antiplatelet agents • Interventional and surgical treatment • • • Angioplasty with stent placement Bypass surgery if diffuse disease Amputation • Acute occlusion may also be treated with thrombolytics
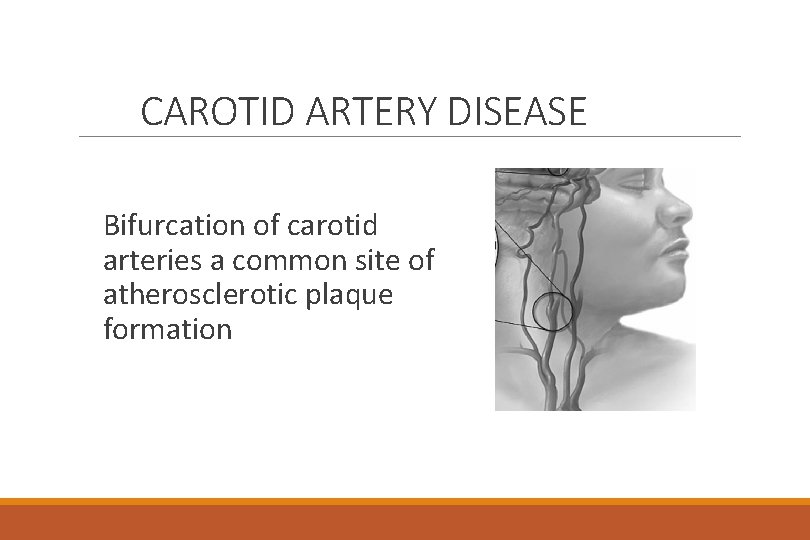
CAROTID ARTERY DISEASE Bifurcation of carotid arteries a common site of atherosclerotic plaque formation

ETIOLOGY • Atherosclerosis • Most common • Irradiation, arteritis • Risk factors as with CAD and PAD • Stenotic vessels • Modifiable risk factors • Uncontrolled hypertension • Afib • Smoking • Uncontrolled DM

MEDICAL MANAGEMENT • Doppler studies • Emergency CT scan with stroke • Treatment of stroke - discussed in Neuro • Control risk factors • Carotid endarterectomy • Carotid stenosis greater than 70% • Symptomatic • Carotid stenting if surgery contraindicated

CARDIAC TAMPONADE • Buildup of fluid in pericardial space • Impedes pumping • Decreased CO
ETIOLOGY • MI • CABG • Cardiac infection • Dissecting aortic aneurysm • Renal failure • Neoplasm • Penetrating and nonpenetrating trauma

CLINICAL MANIFESTATIONS • Dyspnea and tachycardia • PEA • Beck’s triad • Narrowed pulse pressure • Pulsus paradoxus • CVP, PAD, PAWP ALL Elevated • Pericardial friction rub • CO And SVO 2 • Echo – RA Collapse • Progresses to air hunger • JVD • Hypotension • Muffled heart sounds • Equalized pressures > 20 mm. Hg
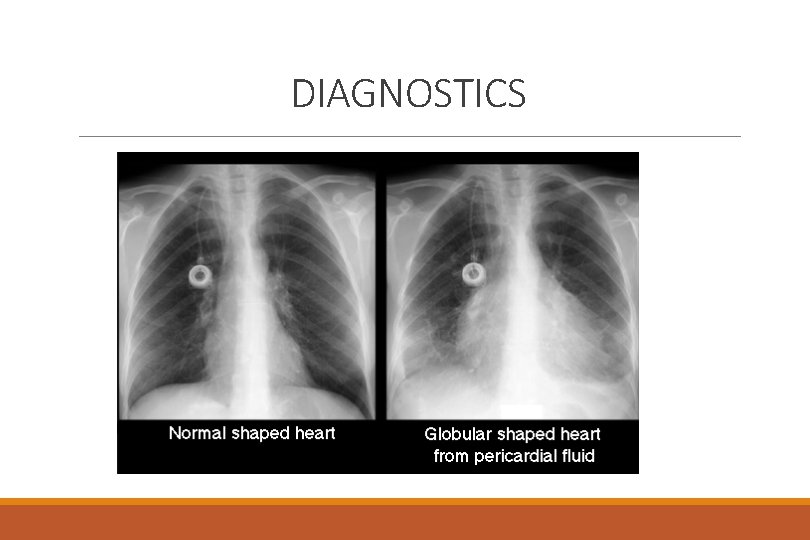
DIAGNOSTICS
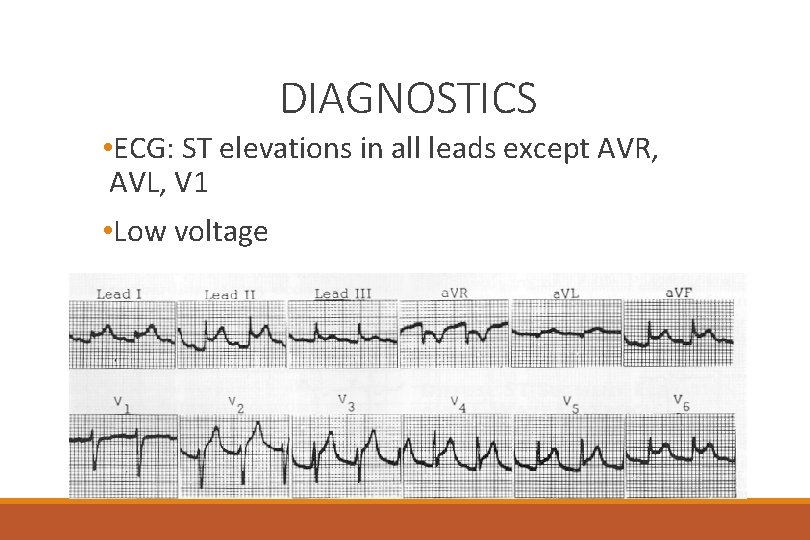
DIAGNOSTICS • ECG: ST elevations in all leads except AVR, AVL, V 1 • Low voltage
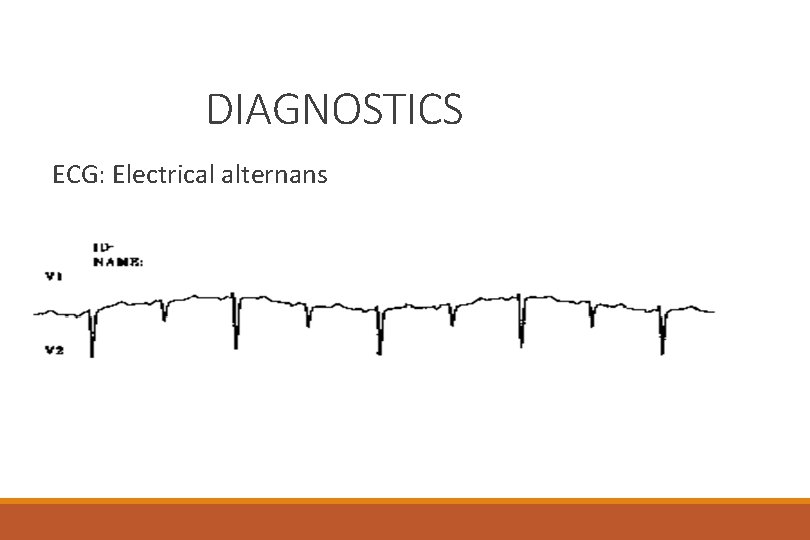
DIAGNOSTICS ECG: Electrical alternans

DIAGNOSTICS Doppler echocardiography ◦ Visualizes pericardial fluid and compressed chambers ◦ Usually right atrium and ventricle ◦ Left atrial collapse highly specific for tamponade
MEDICAL MANAGEMENT • Fluid resuscitation • Treat cause • Pericardiocentesis • Dialysis if uremic • Pericardial window • Pericardiectomy

NURSING MANAGEMENT • VS, cardiac & hemodynamic monitoring • Monitor output from chest tube • Fluids as needed • Monitor labs • H&H, Electrolytes, BUN, creatinine, CK-MB, Troponins

EXAM QUESTIONS A patient is 8 hours post repair of a dissecting abdominal aortic aneurysm. Assessment reveals: BP: 140/90 HR: 105 BUN: 46 mg/dl UO: <20 cc/hr Creatinine: 2. 8 Serum Electrolytes: Normal WBCs: 12, 000/mm 3 Urinalysis: Gross RBCs

EXAM QUESTIONS The patient’s urinary status is most likely associated with: A. B. C. D. A urinary tract infection An intraoperative MI Renal ischemia Hypovolemia

EXAM QUESTIONS A patient receiving thrombolytics via continuous infusion for acute limb ischemia suddenly complains of pain in the affected limb. The most appropriate nursing intervention for this patient is to: A. Administer narcotic pain medication to relieve pain B. Elevate the affected extremity above the level of the heart C. Notify the MD that the patient may have compartment syndrome D. Discontinue thrombolytic infusion and notify the MD

EXAM QUESTIONS The nurse in the ICU is admitting a patient with a stab wound of the chest. Cardiac tamponade is suspected. The physician orders an ECG. Which of the following would be consistent with cardiac tamponade? A. Third degree heart block B. ST elevations in leads II, III, and AVF C. Tall R waves D. Alternating voltage

Good Luck Katie Det@aol. com
- Slides: 121