Cardiac Emergencies Sharon Brown RN Numbers AHA states

Cardiac Emergencies Sharon Brown RN

Numbers • AHA states that every 26 seconds, an American will suffer from a cardiac event and every minute someone dies as a result of a cardiac event.

Risk factors for CHD • • Elevated cholesterol levels Untreated HTN Tobacco use Diabetes Obesity Lack of regular physical activity Poor dietary intake

CMS • Centers for Medicare and Medicaid (CMS) • Core measures that are identified to ensure that patients with ACS receive appropriate evidence based standards of care.

Anatomy and Physiology

ASSESSMENT • • PQRST Could be pain, discomfort, pressure, tightness R/O most threatening first Newer studies show that many young MI patients are positive for cocaine yet drug use is rarely questioned in MI
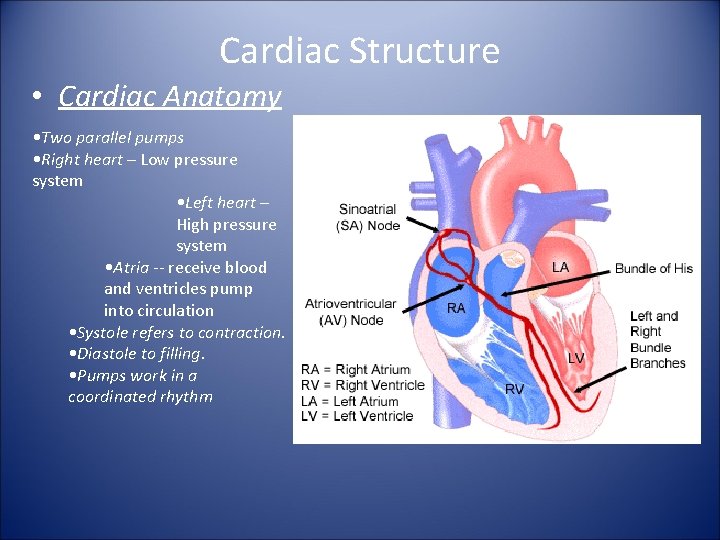
Cardiac Structure • Cardiac Anatomy • Two parallel pumps • Right heart – Low pressure system • Left heart – High pressure system • Atria -- receive blood and ventricles pump into circulation • Systole refers to contraction. • Diastole to filling. • Pumps work in a coordinated rhythm

Cardiac Structure • Cardiac Valves -Atrioventricular (Tricuspid and Mitral) – Leaflets attached to a valve annulus between the chambers – Chordae tendinea strong fibrous cords attached to valve leaflet on one end and papillary muscle on other – Papillary muscle projects into ventricular wall – Systole pulls the chordae tendinea using the papillary muscle to control valve operation – Valves form a parachute to prevent prolapse during contraction
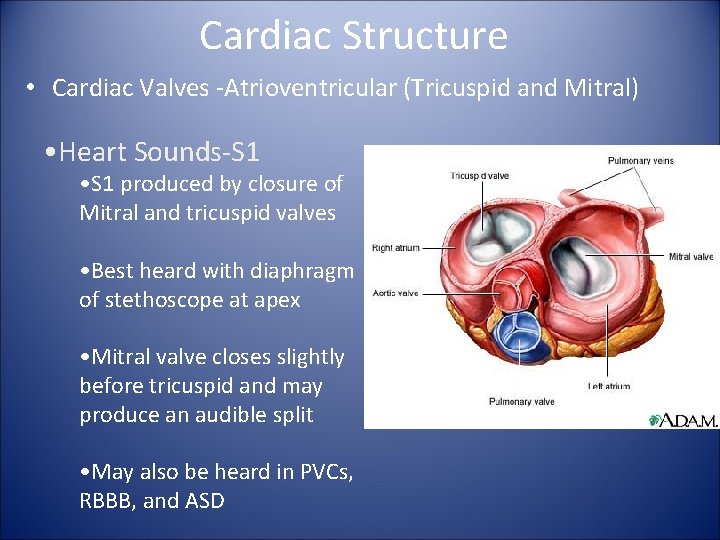
Cardiac Structure • Cardiac Valves -Atrioventricular (Tricuspid and Mitral) • Heart Sounds-S 1 • S 1 produced by closure of Mitral and tricuspid valves • Best heard with diaphragm of stethoscope at apex • Mitral valve closes slightly before tricuspid and may produce an audible split • May also be heard in PVCs, RBBB, and ASD
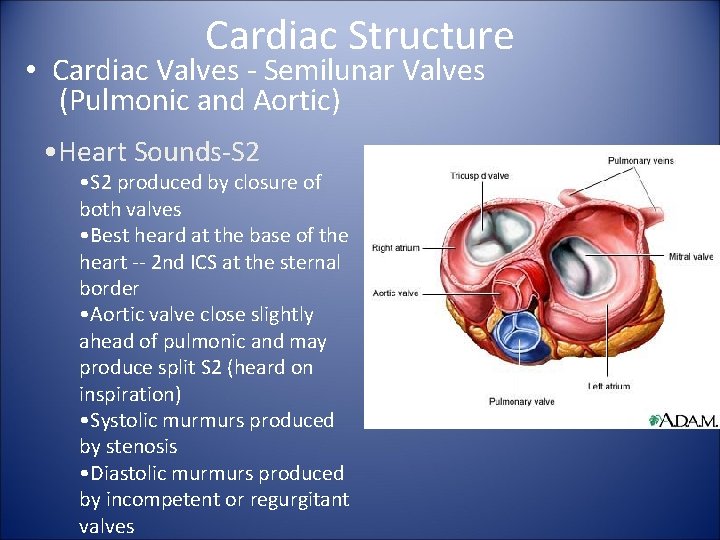
Cardiac Structure • Cardiac Valves - Semilunar Valves (Pulmonic and Aortic) • Heart Sounds-S 2 • S 2 produced by closure of both valves • Best heard at the base of the heart -- 2 nd ICS at the sternal border • Aortic valve close slightly ahead of pulmonic and may produce split S 2 (heard on inspiration) • Systolic murmurs produced by stenosis • Diastolic murmurs produced by incompetent or regurgitant valves
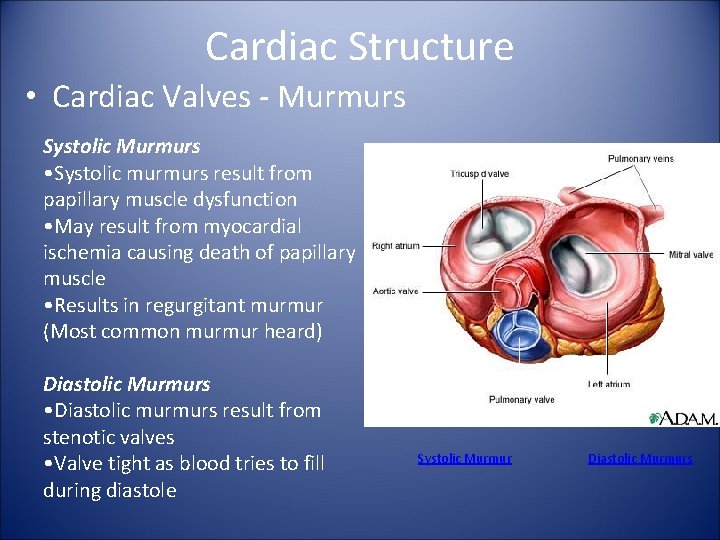
Cardiac Structure • Cardiac Valves - Murmurs Systolic Murmurs • Systolic murmurs result from papillary muscle dysfunction • May result from myocardial ischemia causing death of papillary muscle • Results in regurgitant murmur (Most common murmur heard) Diastolic Murmurs • Diastolic murmurs result from stenotic valves • Valve tight as blood tries to fill during diastole Systolic Murmur Diastolic Murmurs

Cardiac Valves – Murmur Characteristics

Pericardial Friction Rub • Described as rough, scratching, squeaky sound • Caused by inflammation of pericardium – Occurs in 15% of MI, Not uncommon after cardiac surgery • Heard best with patient leaning forward, holding breath in full expiration Pericardial Friction Rub
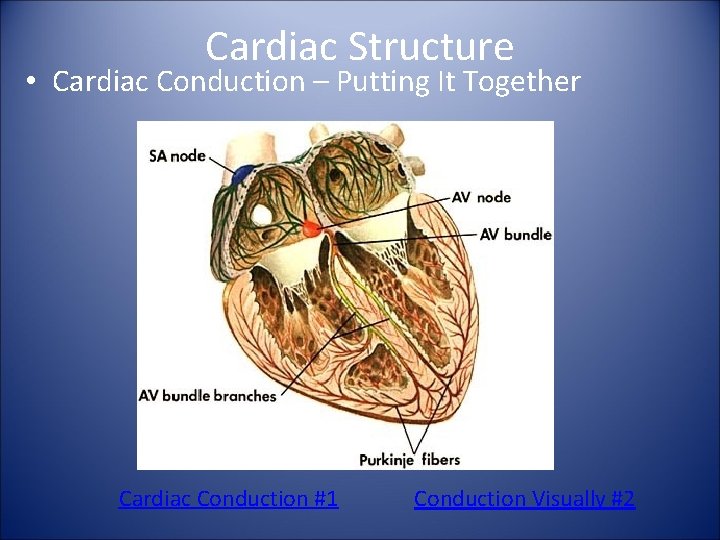
Cardiac Structure • Cardiac Conduction – Putting It Together Cardiac Conduction #1 Conduction Visually #2
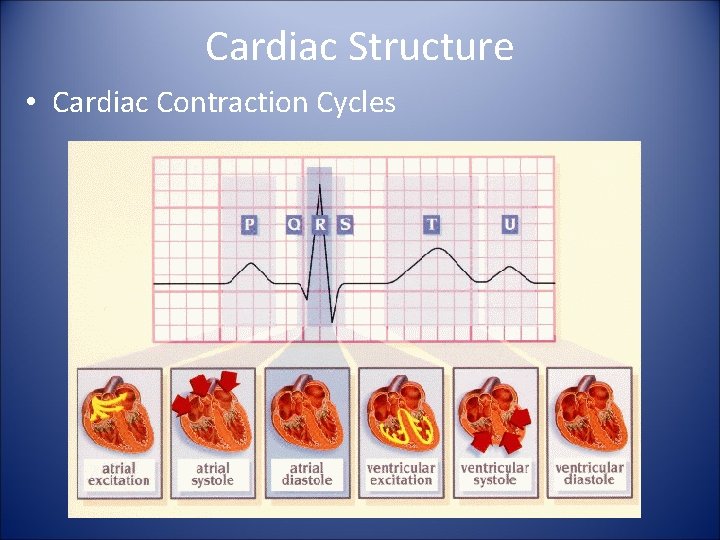
Cardiac Structure • Cardiac Contraction Cycles

Cardiac Contraction Cycles • Atrial Excitation – This occurs when the SA node sends out an electrical impulse through the right and left atria. – This action creates the “P” wave on an EKG Rhythm. • Atrial Systole – As the atria contract, the blood pressure in each atrium increases, forcing additional blood into the ventricles. – This action creates the “Q” wave on an EKG Rhythm. • Atrial diastole – As the signal passes through the AV node the atria and ventricles are both at rest • Ventricular Excitation – Occurs as the electrical impulse travels from the AV node through the bundle branches and Purkinje fibers. – This action creates the “RS” wave on an EKG Rhythm. • Ventricular Systole – Occurs as the right and left ventricles contract and push blood out. – This action creates the “T” wave on an EKG Rhythm. • Ventricular Diastole – During this phase the ventricles are at rest. – This action creates the “U” wave on an EKG Rhythm.
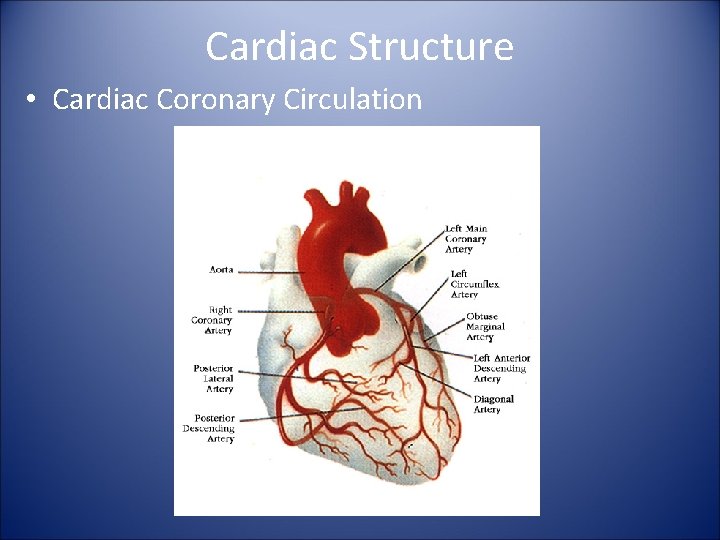
Cardiac Structure • Cardiac Coronary Circulation

Cardiac Arrest • The H’s include: • • • H’s and T’s • • ACLS/AHA Guidelines • • Hypovolemia, Hypoxia, Hydrogen ion (acidosis), Hyper-/hypokalemia, Hypoglycemia, Hypothermia. • The T’s include: • • • Toxins, Tamponade(cardiac), Tension pneumothorax, Thrombosis (coronary and pulmonary), Trauma.

Therapeutic Electrical Interventions • • Defibrillation Cardioversion Pacemakers Implantable cardioverter-Defibrillator

Resuscitation Interventions • Fluids • Pharmacologic Therapy • Post-Cardiac Arrest Therapeutic Hypothermia

Adenosine • Re-Entry SVT • Dose: 6 mg IV/IO push followed by 20 ml saline • 1 -2 min later 12 mg IV/IO Then move on to otherapy(ie Cardioversion)

Amiodarone • : Shock Resistant Ventricular Fibrillation Dose: 300 mg IV/IO, • Second does of 150 mg if VF recurs • 24 hr maximum is 2. 2 gm • Half-life lasts up to 40 days? • Remember … 300 without a pulse, 150 with a pulse.

Atropine • Indication: Sympomatic Bradycardia • Dose: . 5 mg IV, can be given up to 3 ms • Sequence for Bradycardia is: Atropine, TCP, Epinephrine, Dopamine. If no IV access go straight to TCP. • Can be given for organophosphate poisoing (extremely large dose needed: 2 -4 mg)

Calcium Chloride • Indication: Magnesium Toxicity or Calcium Channel blocker Over Dose 500 -100 mg IV • Be careful with patients on Digitalis

Diltiazem • Indication: Slow Rapid Ventricular Response associated with A. Fib/A. Fluter Dose: 0. 25 mg/kg • After 15 min 0. 35 mg/kg, • Infusion: 5 -15 mg/hr titrated to heart rate • Avoid in patients with WPW

Dopamine • Function: Cardio Genic Shock(Increases Cardiac Output and BP) • • Dose: • 1 -5 mcg/kg/min(Renal and Splanchnic Dilation) • 5 -10 mcg/kg/min(Beta Effects(inotropy)) • 10 -20 mcg/kg/min(Alpha Effects(vasoconstriction))

Epinephrine • ↑Myocardial and CNS blood Flow d/t α effects • Dose: 1 mg IV push Q 3 -5 min • 2 -2. 5 mg down the ET tube • May need higher doses with ß blockers or Calcium channel blockers • Given in anaphylaxis (0. 3 mg 1: 1000, SQ)

Lidocaine • Alternative therapy for refractory VF/pulseless VT • Dose: • 1 -1. 5 mg/ KG IV followed by • 1 -4 mg/min infusion

Magnesium • Torsade De Pointe VT • Hypomagnesmia hinders the cellular movement of K+ and thereby makes the heart proarrhythmic. • Dose: 1 -2 gm IV push over 1 -2 minutes. • Torsade with pulse = 1 -26 mg in 100 ml D 5 W over • 5 -60 minutes

Morphine • Analgesic of Choice for ischemic pain w/ ACS that is not relieved by Nitroglycerin. • Also good for treating pulmonary edema as it decreases venous return to the heart and has a mild bronchodilatory effect. • 2 -4 mg IV push

Nitroglycerin • Indication: Chest Pain • relaxes vascular smooth mucscle. • Can be given topical, spray, sublingually, IV • Contraindicated in patients taking some medications for erectile dysfunction

Sodium Bicarb • Indication: Acidosis reversal. • Initial dose without a blood gas: 1 meq/kg IV push • w/ half dose administered q 10 min • Mainly used for TCA OD, Hyperkalemia, preexisting metabolic acidosis

Vasopressin • Shock refractory VF or pulesless VT & Asystole in place of initial or second dose of epinephrine. Has powerful vasoconstrictive effects. • Dose: 40 u IV one time then return to epinephrine

Therapeutic Hypothermia
Improving Post Cardiac Arrest Outcomes Facts: After cardiac arrest, brain injury is a major source of morbidity and mortality!

Current Cardiac Arrest Outcomes Pre-hospital ROSC (Response of Spontaneous Circulation) 45% of v-fib arrests 37% of all cardiac arrests Discharge 12% make it to discharge Post Resuscitation Deaths 10% die due to recurrent dysrhythmias 30% die to due to cardiovascular collapse 40% die due to PRE (Post Resuscitation Encephalopathy)

Post Resuscitation Encephalopathy Initial insult from cardiac arrest Period of intense hyperperfusion Cell injury Oxygen free radical formation Inflammatory cascade Glutamate mediated cell death Loss of autoregulation Sludging and hypoperfusion Perfusion/demand mismatch

Beneficial Effects of Hypothermia • Decrease in cerebral metabolism • Maintains integrity of membranes • Preserves ion homeostasis • Decrease Ca influx • Decrease free radical formation • Decrease vascular damage

Hypothermia Induction Orders HYPOTHERMIA INDUCTION ORDERS Decrease Patient Temperature to ≤ 34 C Goal: Achieve patient temperature of 32 – 34◦C within 1 -2 hours of resuscitation.

Complications of Hypothermia No difference in complication rates in normothermic and hypothermic cohorts • Potassium shifts Intracellular shift with induction Extracellular shift with warming • Fluid status Cooling causes diuresis Warming causes hypovolemia • • Respiratory Alkalosis Temperature corrected ABG allows changes in minute ventilation to support normal Pa. CO 2 Hyperglycemia

Complications of Hypothermia (Con’t) • Neutropenia and increased incidence of pneumonia seen in patients exposed to prolonged hypothermia (>24 hrs) in other applications • Coagulopathy May alter clotting cascade, platelet function • Cardiac dysrhythmias Little risk for clinically significant dysrhythmias if temperatures are maintained >30°C

Shifting of Potassium Hypothermia Serum Potassium “Hypokalemia is expected with hypothermia as potassium moves into the cell, as the patient is re-warmed there will be a rebound effect, therefore aggressive supplement of K + is not recommended. ” Do not provide supplement unless K+ < 3. 0 mmol/l or cardiac instability Target K+ 3. 5/cardiac stability

Acute Coronary Syndrome • General term used to describe a group of coronary artery diseases and their symptoms. – Unsable Angina – STEMI – Non-STEMI • Assessment is key • Differential diagnosis

Assessment • PQRST-What are the elements? • 12 lead EKG • Cardiac Markers
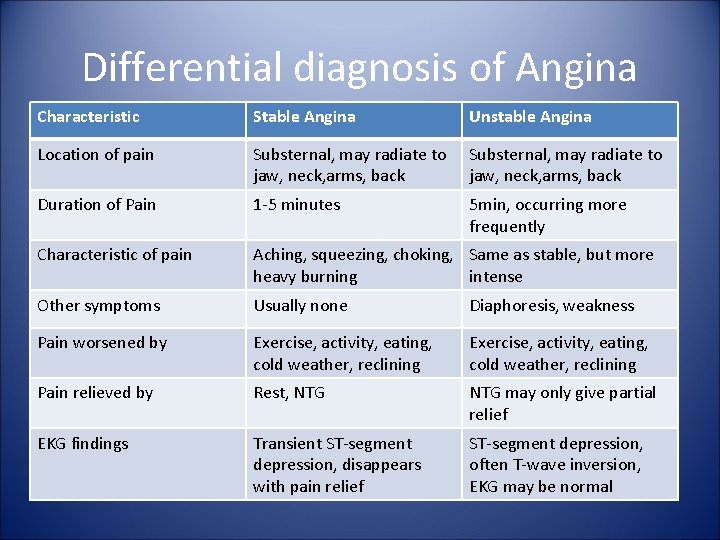
Differential diagnosis of Angina Characteristic Stable Angina Unstable Angina Location of pain Substernal, may radiate to jaw, neck, arms, back Duration of Pain 1 -5 minutes 5 min, occurring more frequently Characteristic of pain Aching, squeezing, choking, Same as stable, but more heavy burning intense Other symptoms Usually none Diaphoresis, weakness Pain worsened by Exercise, activity, eating, cold weather, reclining Pain relieved by Rest, NTG may only give partial relief EKG findings Transient ST-segment depression, disappears with pain relief ST-segment depression, often T-wave inversion, EKG may be normal

Patient Management • • • History OMI/MONA Frequent monitoring Percutaneous Coronary Intervention (PCI) Fibrinolytic Therapy – Activase, Retavase, TNKase Table 31 -13 • Heparin, NTG, ACE, B-Blocker

Bradycardia • • HR less than 60 Inferior wall MI Can be vagal response Treat the underlying cause
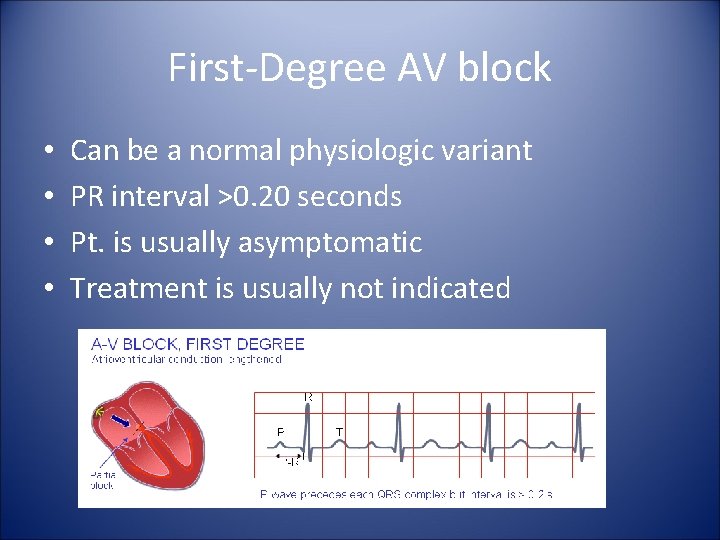
First-Degree AV block • • Can be a normal physiologic variant PR interval >0. 20 seconds Pt. is usually asymptomatic Treatment is usually not indicated
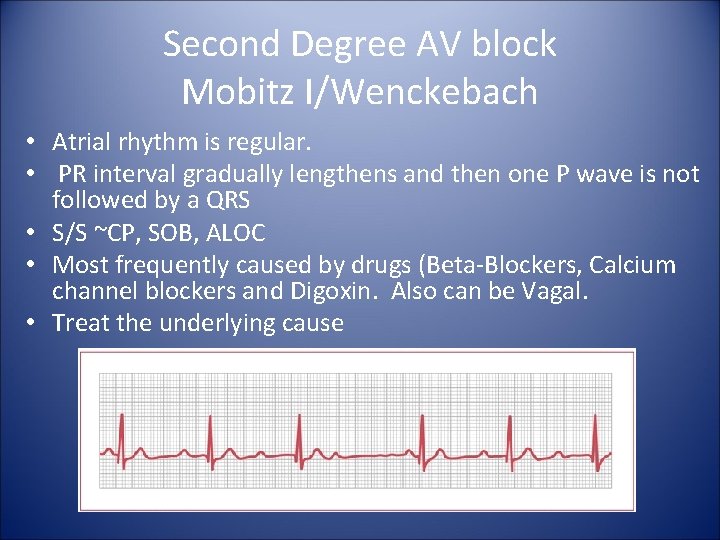
Second Degree AV block Mobitz I/Wenckebach • Atrial rhythm is regular. • PR interval gradually lengthens and then one P wave is not followed by a QRS • S/S ~CP, SOB, ALOC • Most frequently caused by drugs (Beta-Blockers, Calcium channel blockers and Digoxin. Also can be Vagal. • Treat the underlying cause
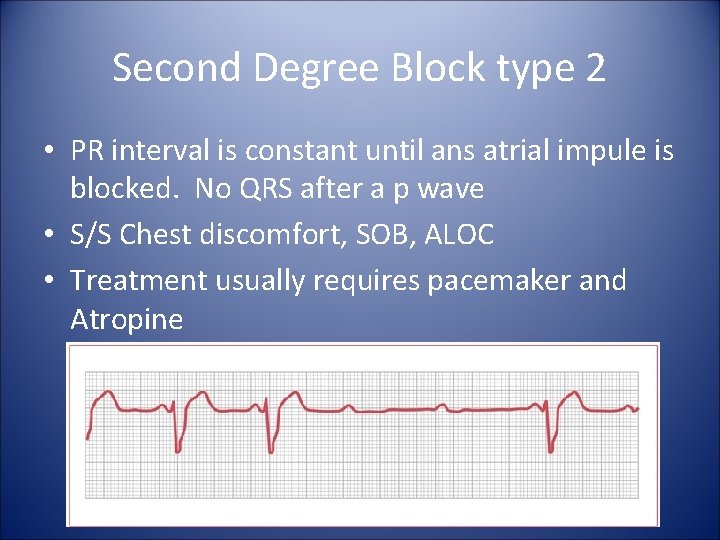
Second Degree Block type 2 • PR interval is constant until ans atrial impule is blocked. No QRS after a p wave • S/S Chest discomfort, SOB, ALOC • Treatment usually requires pacemaker and Atropine

Third Degree AV block • Atrial and Ventricle disassociation • Both rates are usually regular, but do not correlate • S/S CP, SOB, ALOC, syncope • Tx includes pacemaker • Do not use lidocaine/amiodarone

Pericarditis • Inflammation of pericardial sac • S/S~ fever, chills, severe chest pain, friction rub • Pain increases when patient lies down and decreases when sitting up

Cardiac Tamponade • Fluid accumulation in pericardial sac • Beck’s Triad~JVD, hypotension, distant heart sounds • Pericardiocentesis
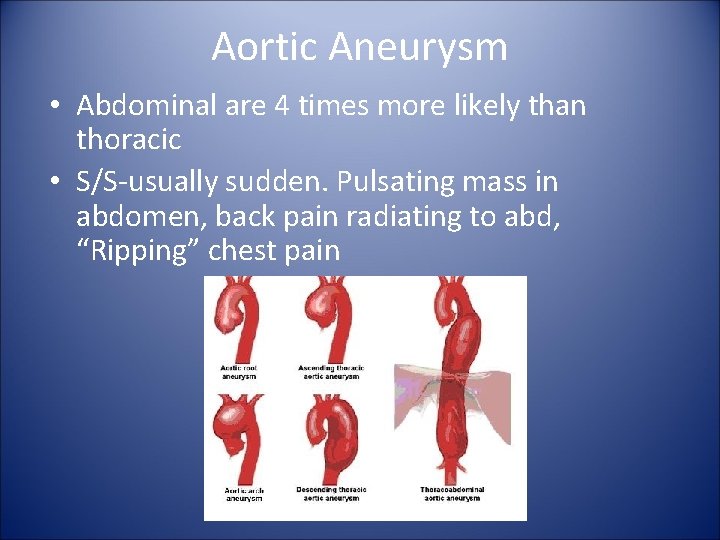
Aortic Aneurysm • Abdominal are 4 times more likely than thoracic • S/S-usually sudden. Pulsating mass in abdomen, back pain radiating to abd, “Ripping” chest pain

IMPLANTED CARDIOVERTER DEFIBRILLATOR ICDs are becoming more common ER visits related to miss-firing are common. Treat CP in these patients are you would normally. Patient will usually have a card describing what type of device is being used. • Placing a magnet over device will disable shocking, but not pacing. • If override defibrillation is necessary, make sure pads are at least 10 cm away. • •
- Slides: 55