CARDIAC CHANNELOPATHIES Dr Binjo J Vazhappilly SR Cardiology

CARDIAC CHANNELOPATHIES Dr Binjo J Vazhappilly SR Cardiology Calicut Medical College

• Cardiac channelopathies refers to genetic disorders characterized by altered cardiac excitability, in the absence of structural cardiac involvement. • Also known as inherited arrhythmogenic diseases (IADs). • Disorders due to genetic mutation affecting the genes that control the excitability of myocardial cells.

Major cardiac channelopathies include Long QT Syndrome Brugada syndrome CPVT Short QT syndrome
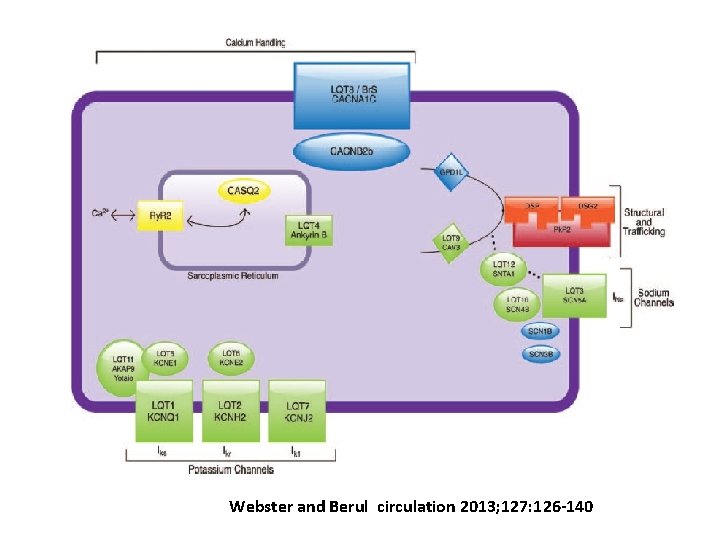
Webster and Berul circulation 2013; 127: 126 -140

Long QT Syndrome • LQTS is an IAD characterized by abnormally prolonged QT interval. • 13 genes are found to be linked to LQTS till now. • Mutations in 3 genes KCNQ 1 (LQT 1), KCNH 2 (LQT 2) and SCN 5 A (LQT 3) accounts for approximately 75% of cases with a strong clinical phenotype.
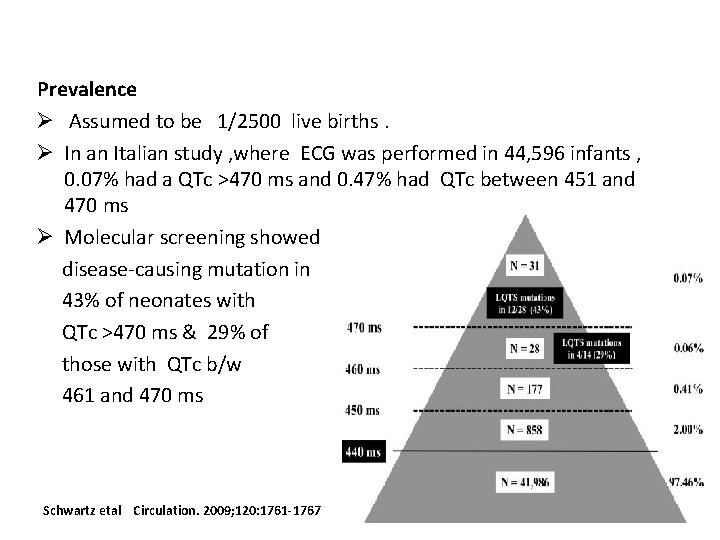
Prevalence Ø Assumed to be 1/2500 live births. Ø In an Italian study , where ECG was performed in 44, 596 infants , 0. 07% had a QTc >470 ms and 0. 47% had QTc between 451 and 470 ms Ø Molecular screening showed disease-causing mutation in 43% of neonates with QTc >470 ms & 29% of those with QTc b/w 461 and 470 ms Schwartz etal Circulation. 2009; 120: 1761 -1767
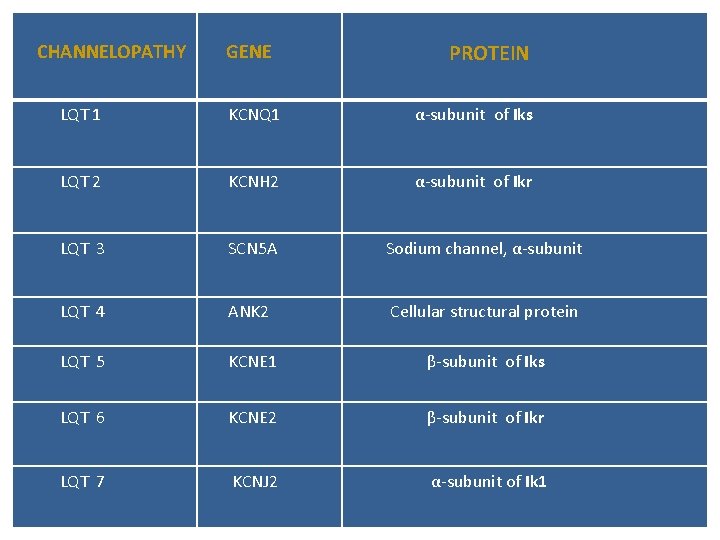
CHANNELOPATHY GENE PROTEIN LQT 1 KCNQ 1 α-subunit of Iks LQT 2 KCNH 2 α-subunit of Ikr LQT 3 SCN 5 A Sodium channel, α-subunit LQT 4 ANK 2 Cellular structural protein LQT 5 KCNE 1 β-subunit of Iks LQT 6 KCNE 2 β-subunit of Ikr LQT 7 KCNJ 2 α-subunit of Ik 1
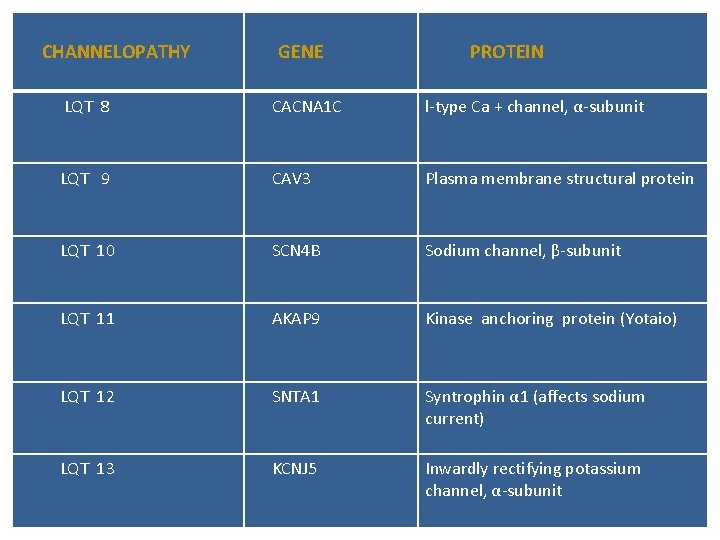
CHANNELOPATHY GENE PROTEIN LQT 8 CACNA 1 C l-type Ca + channel, α-subunit LQT 9 CAV 3 Plasma membrane structural protein LQT 10 SCN 4 B Sodium channel, β-subunit LQT 11 AKAP 9 Kinase anchoring protein (Yotaio) LQT 12 SNTA 1 Syntrophin α 1 (affects sodium current) LQT 13 KCNJ 5 Inwardly rectifying potassium channel, α-subunit

Potassium Channel LQTS • Potassium channel derangements account for majority of LQTS cases : Long QT 1, 2, 5, 6, 7 and 13. • IKs : slowly activating delayed rectifier cardiac potassium channel subunit is encoded by KCNQ 1 β subunit is encoded by KCNE 1 Loss of function mutation result in LQT 1 and LQT 5 • Ikr : rapid delayed rectifier potassium channel subunit encoded by KCNH 2 β subunit encoded by KCNE 2 Loss of function mutation result in LQT 2 and LQT 6.

• IKI : another inwardly rectifying K+ channel encoded by gene KCNJ 2 Loss of function mutation result in LQT 7 (Tawil-Anderson syn) • KCNJ 5 mutation which is a loss-of-function mutation in an inwardly rectifying potassium channel result in LQT 13

Sodium channel LQTS • subunit of sodium channel is encoded by SCN 5 A and β subunit encoded by SCN 4 B. • Gain of function mutations in SCN 5 A produce LQT 3. • Mutations in SCN 4 B produce LQT 10.
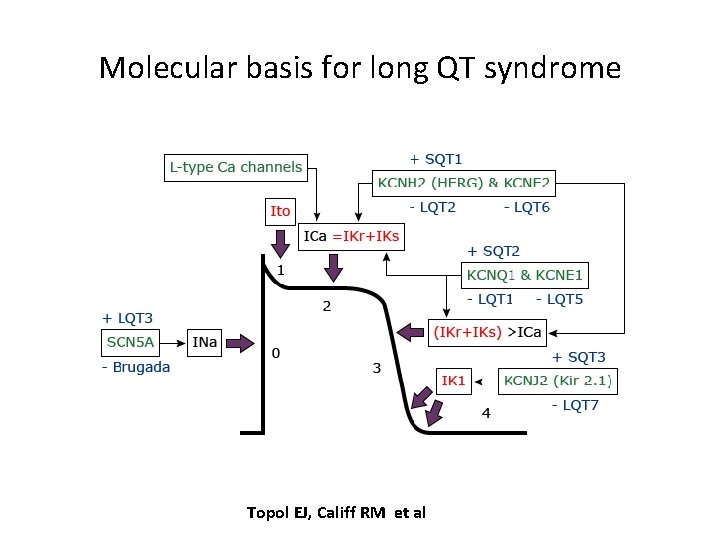
Molecular basis for long QT syndrome Topol EJ, Califf RM et al

Pathophysiology of LQTS • Prolonged repolarization results fm net reduction in outward current, due to ↑ in inward Na + or Ca + current, ↓ in outward K+ current or both resulting in long QT interval. Ø Fast heart rate preceding Td. P in LQT 1 postulate delayed afterdepolarizations (DADs) as its arrthymogenic mechanism. • Increased Ca+ loading in parallel with QT prolongation, facilitate DADs and DAD-dependent Td. P. Ø Pause-dependent Td. P is triggered by early afterdepolarizations (EADs). • Pause leads to enhanced Ca+ release from intracellular stores and activate Ca+ dependent transmembrane currents.
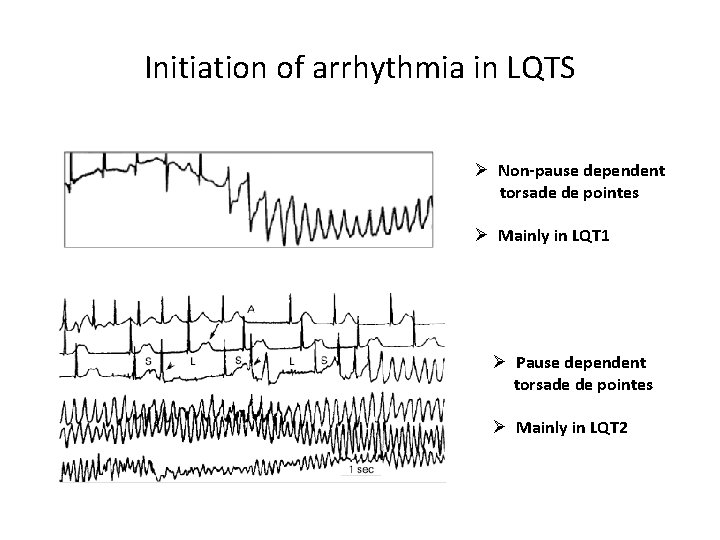
Initiation of arrhythmia in LQTS Ø Non-pause dependent torsade de pointes Ø Mainly in LQT 1 Ø Pause dependent torsade de pointes Ø Mainly in LQT 2

Clinical features • May be asymptomatic • Symptomatic pts present with palpitations, presyncope, syncope or cardiac arrest. • Neuronal deafness is associated with Jervell and Lange-Nielsen syndrome • In a study on 287 pts , 61% were symptomatic : 9% presented with a cardiac arrest, 26% with syncope , 10% with seizures , 6% had presyncore or palpitation • 67% had symptoms related to exercise, 18% had symptoms during exercise and with emotion, 7% with emotion alone, 3% with loud noise and exercise and 2% with anesthesia. A Garson, M Dick et al Circulation. 1993; 87: 1866 -1872
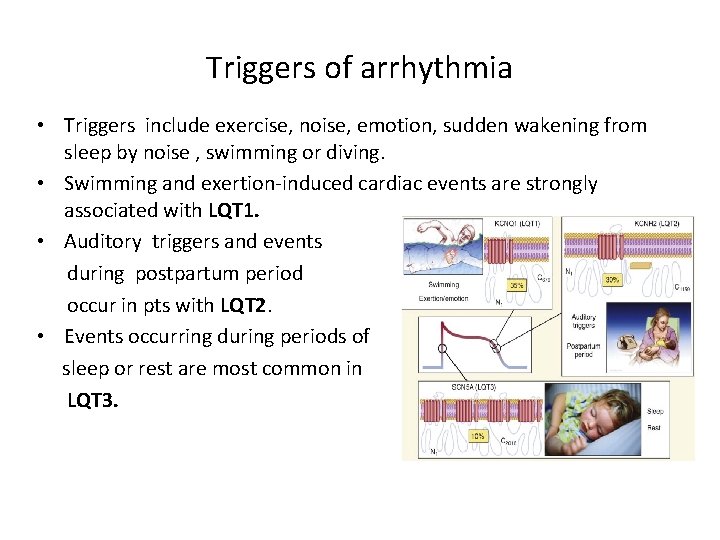
Triggers of arrhythmia • Triggers include exercise, noise, emotion, sudden wakening from sleep by noise , swimming or diving. • Swimming and exertion-induced cardiac events are strongly associated with LQT 1. • Auditory triggers and events during postpartum period occur in pts with LQT 2. • Events occurring during periods of sleep or rest are most common in LQT 3.
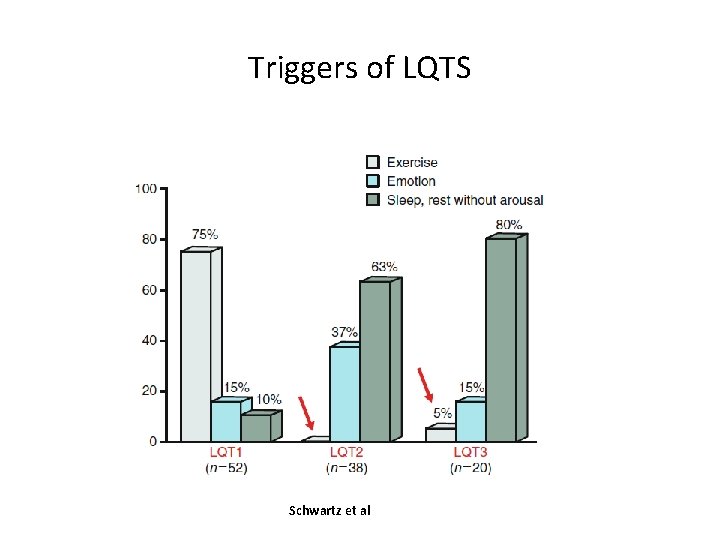
Triggers of LQTS Schwartz et al

Jervell and Lange-Nielsen syndrome • Autosomal recessive variant of long QT syndrome. • Due to homozygous or compound heterozygous mutations on either the KCNQ 1 or KCNE 1 genes. • Pts also suffer from congenital deafness. • Most severe of major variants of LQTS. • 90% have cardiac events, 50% become symptomatic by age of 3 yrs and their average QTc is markedly prolonged (557± 65 ms)
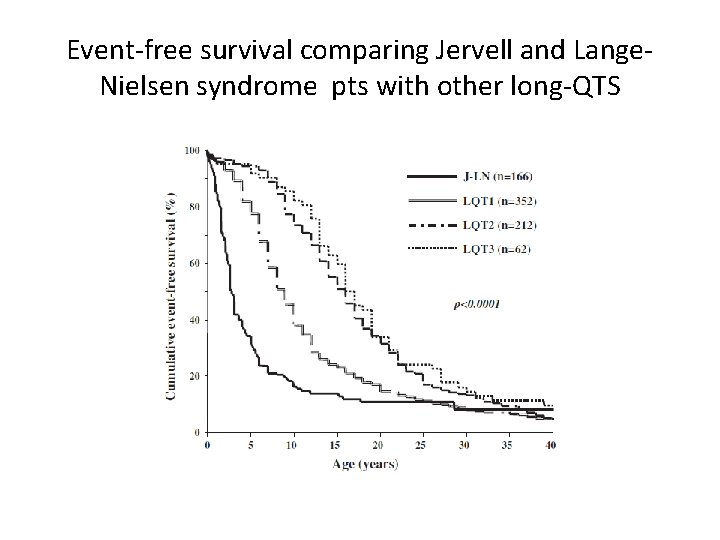
Event-free survival comparing Jervell and Lange. Nielsen syndrome pts with other long-QTS

Timothy syndrome / LQT 8 • Mutations in CACNA 1 C, encoding voltage-gated calcium channel results in Timothy syndrome or LQT 8. • Rare and extremely malignant variant. • Pts had marked QT prolongation and associated syndactyly. • Presents with 2: 1 atrioventricular block and macroscopic T-wave alternans. • Among 17 children reported by Splawski et al, 10 (59%) died at a mean age of 2. 5 yrs.
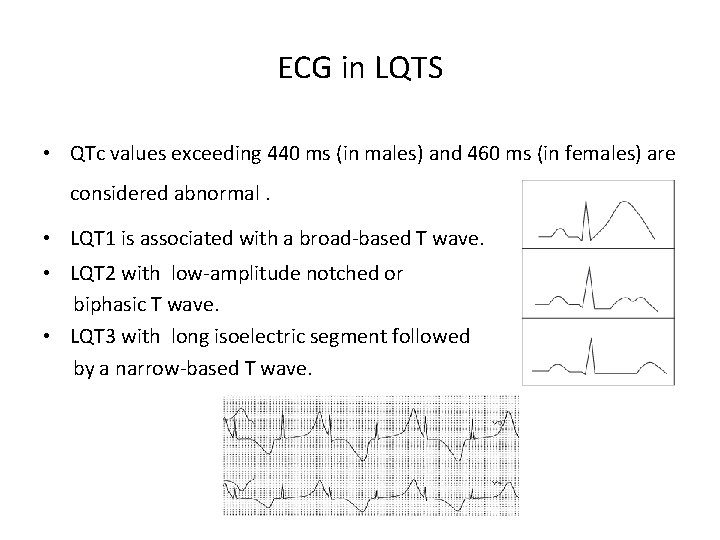
ECG in LQTS • QTc values exceeding 440 ms (in males) and 460 ms (in females) are considered abnormal. • LQT 1 is associated with a broad-based T wave. • LQT 2 with low-amplitude notched or biphasic T wave. • LQT 3 with long isoelectric segment followed by a narrow-based T wave.

LQTS : Diagnostic Criteria Score ≤ 1 point: low probability 1. 5– 3 points: intermediate probability ≥ 3. 5 points: high probability. Schwartz et al Circ Arrhythm Electrophysiol. 2012;
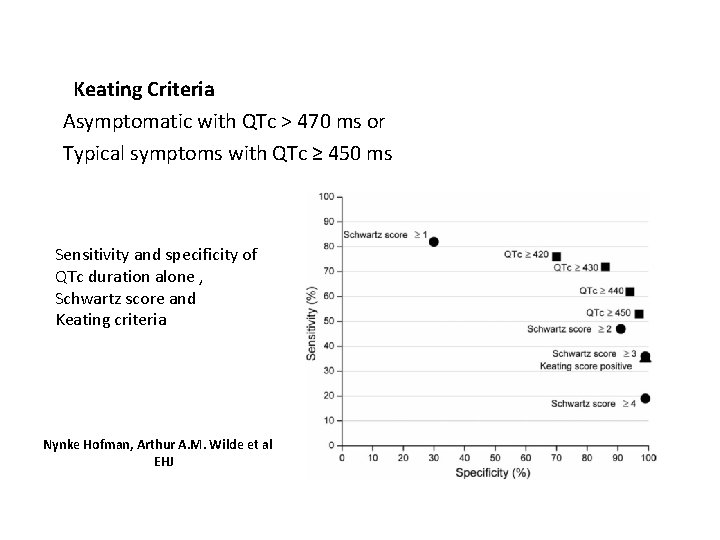
Keating Criteria Asymptomatic with QTc > 470 ms or Typical symptoms with QTc ≥ 450 ms Sensitivity and specificity of QTc duration alone , Schwartz score and Keating criteria Nynke Hofman, Arthur A. M. Wilde et al EHJ

Risk stratification Risk of a 1 st cardiac event in pts younger than 40 years of age in the absence of any LQTS active treatment

Treatment • All LQTS pts with h/o syncope and asymptomatic individuals with definite QT prolongation should be treated withβ-blockers • Drugs used are Propranolol ( 2 -4 mg/kg/d), Nadolol (1 -2. 5 mg/kg/d) Metoprolol (2 -4 mg/kg/d) • Dose titration done with a target of 25% to 35% reduction of maximal heart rate attained on therapy. • Left Cardiac Sympathetic Denervation may be considered in symptomatic patients even after betablocker therapy.

Treatment • ICD implantation along with β -blockers is recommended for LQTS patients with previous cardiac arrest or who are experiencing syncope and/or VT while receiving beta blockers. • Permanent pacing is indicated for sustained pause-dependent VT, with or without QT prolongation. • Avoid competitive sports, QT-prolonging drugs and lowered K+ levels.

β-blocker therapy in LQTS • β-blocker therapy results in 42% to 78% reduction of aborted cardiac arrest or sudden cardiac death. • Pts on β-blockers still have risk of sudden death. • In a study , no. of cardiac events before initiation of β-blocker therapy was 0. 97 events /pt/yr which decreased to 0. 31 after initiation of therapy. • β-blocker is most efficacious in LQT 1 and less effective in LQT 3. • In LQT 3, combination of mexiletine with a noncardioselective βblocker (propranolol ) is used.

Brugada Syndrome • Characterized by peculiar ECG pattern of ST-segment elevation in leads V 1 to V 3 and incomplete or complete RBBB in the absence of signs of acute MI. • Autosomal dominant disorder with variable expression • More common in men than in women. • Usually diagnosed in adulthood ( Avg age at diagnosis is 41 yrs).
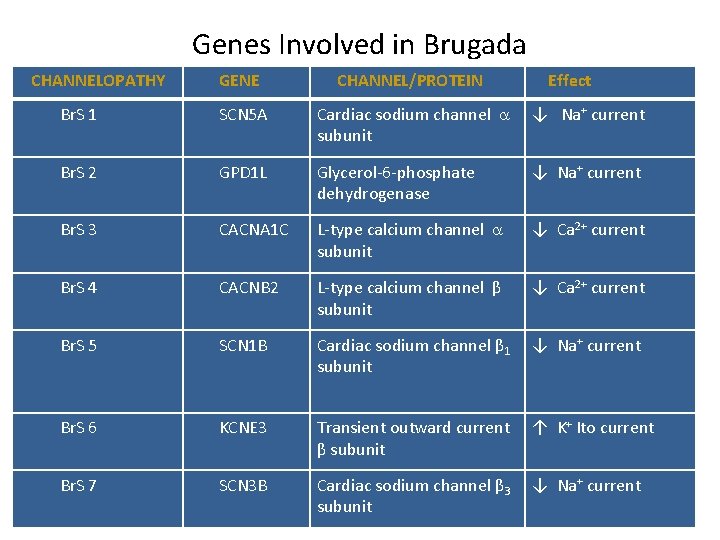
Genes Involved in Brugada CHANNELOPATHY GENE CHANNEL/PROTEIN Effect Br. S 1 SCN 5 A Cardiac sodium channel subunit ↓ Na+ current Br. S 2 GPD 1 L Glycerol-6 -phosphate dehydrogenase ↓ Na+ current Br. S 3 CACNA 1 C L-type calcium channel subunit ↓ Ca 2+ current Br. S 4 CACNB 2 L-type calcium channel β subunit ↓ Ca 2+ current Br. S 5 SCN 1 B Cardiac sodium channel β 1 subunit ↓ Na+ current Br. S 6 KCNE 3 Transient outward current β subunit ↑ K+ Ito current Br. S 7 SCN 3 B Cardiac sodium channel β 3 subunit ↓ Na+ current
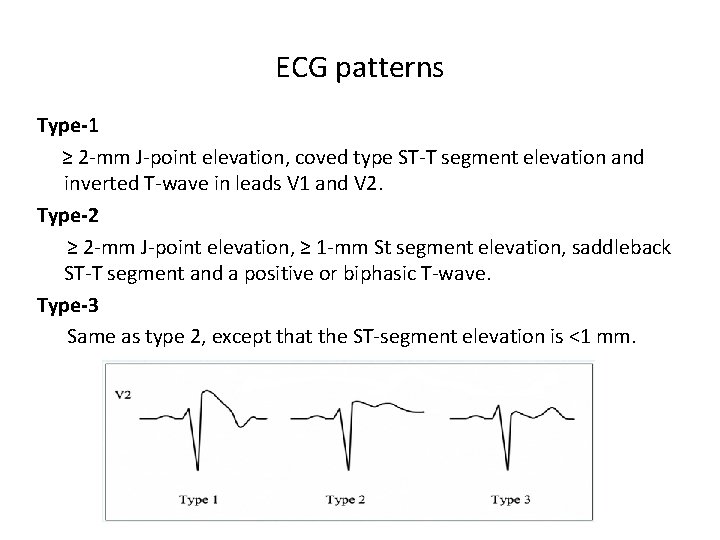
ECG patterns Type-1 ≥ 2 -mm J-point elevation, coved type ST-T segment elevation and inverted T-wave in leads V 1 and V 2. Type-2 ≥ 2 -mm J-point elevation, ≥ 1 -mm St segment elevation, saddleback ST-T segment and a positive or biphasic T-wave. Type-3 Same as type 2, except that the ST-segment elevation is <1 mm.
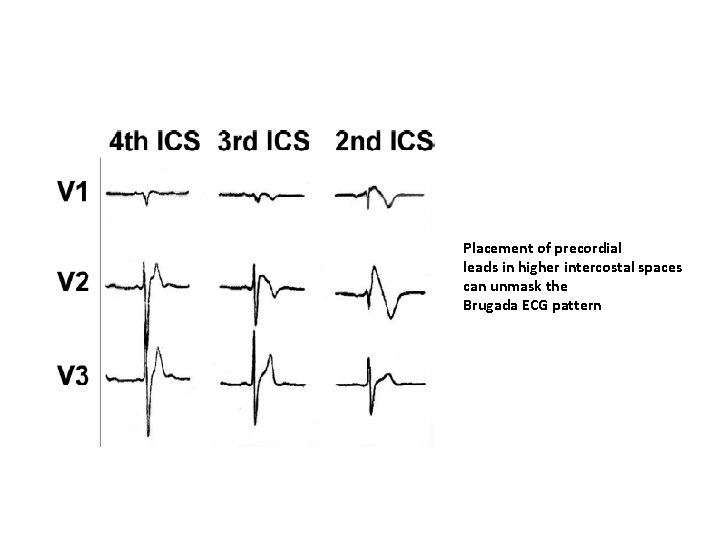
Placement of precordial leads in higher intercostal spaces can unmask the Brugada ECG pattern

Pathophysiology • Debate is still going on whether pathophysiology is due to repolarization or depolarization disorder. Repolarization hypothesis by Yan and Antzelevitch Ø Transmembrane voltage gradient b/w RV epicardium and endocardium due to heterogenous loss of AP dome in epicardium and not in endocardium. Ø Heterogeneity of transmembrane voltage potentials result in phase 2 reentry and triggered VF.
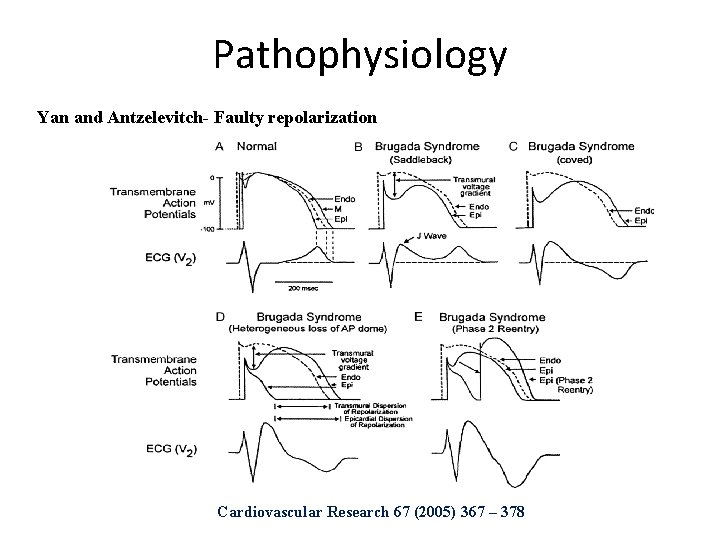
Pathophysiology Yan and Antzelevitch- Faulty repolarization Cardiovascular Research 67 (2005) 367 – 378

Depolarization hypothesis • In BS pts RVOT endocardium shows activation slowing and is the last to depolarize. • Delay in AP of RVOT causes an electrical gradient from more positive RV to RVOT, leading to ST-elevation in right precordial leads. • When RVOT depolarizes later (during repolarization of RV), this gradient is reversed and net current flows towards RV, resulting in a negative T-wave in right precordial leads.

Depolarization Hypothesis conduction delay in RVOT Cardiovascular Research 67 (2005) 367 – 378

Clinical Presentation • Clinical spectrum ranges from asymptomatic to SCD. • Patients may present with late onset of VF, despite having abnormal ECG pattern for decades. • Syncope or seizures may occur due to self-terminating VF episodes. • Agonal respiration and difficulty in arousal at night also may be due to self-terminating VF episodes. • Majority of BS pts are young, b/w 20 and 40 yrs of age at presentation.

Brugada : Diagnostic criteria Appearance of type 1 ST segment elevation (coved type) in > 1 rt precordial lead (V 1 - V 3) in the presence or absence of a sodium channel blocker, plus at least one of the following: Ø Documented ventricular fibrillation. Ø Polymorphic ventricular tachycardia (VT). Ø Family h/o sudden cardiac death at less than 45 years of age. Ø Family h/o of type 1 Brugada pattern ECG changes. Ø Inducible VT during electrophysiology study. Ø Unexplained syncope. Ø Nocturnal agonal respiration. Type 2 and type 3 ECG are not diagnostic of Brugada syndrome Second Consensus Conference : Europeon Heart Rhythm Society

• Brugada pattern : Pts with typical ECG features who are asymptomatic and not having other clinical criteria. • Brugada syndrome : Pts with typical ECG features and clinical criteria (who have experienced sudden cardiac death or a sustained ventricular tachyarrhythmia or who have one or more of the other associated clinical criteria )

Drug challenge • Done in pts with resting ECG type 2 or 3 Brugada pattern and having family h/o sudden cardiac death at < 45 yrs and/or a family h/o type 1 Brugada pattern ECG • Drugs used Flecainide : 2 mg/kg over 10 min iv or 400 mg PO Procainamide : 10 mg/kg over 10 min iv Ajmaline : 1 mg/kg over five minutes iv Pilsicainide : 1 mg/kg over 10 minutes iv

Drug challenge Indications for termination of the drug challenge include: Ø Development of a diagnostic type 1 Brugada pattern Ø ≥ 2 mm increase in ST segment elevation in pts with type 2 Brugada ECG pattern Ø Development of ventricular premature beats or other arrhythmias Ø Widening of the QRS ≥ 30 percent above baseline
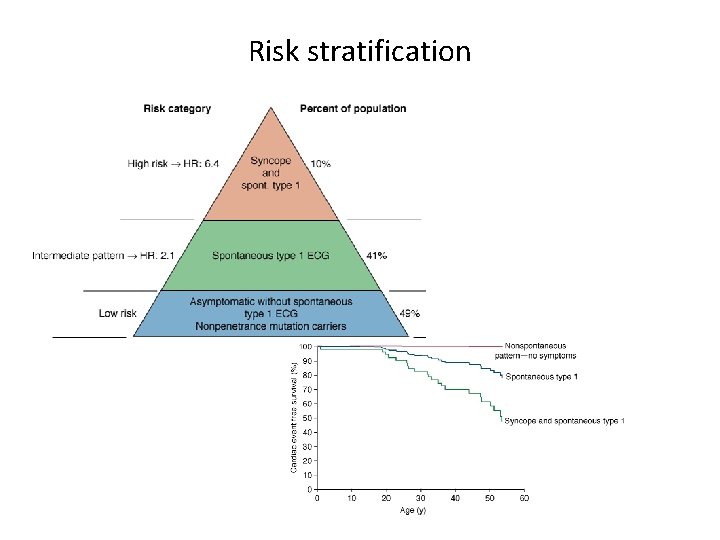
Risk stratification

Treatment • ICD is the only effective treatment to reduce mortality in Br. S • ICD indication Class 1 Br. S pts with previous cardiac arrest. Class IIa Br. S pts with spontaneous pattern with h/o syncope. Br. S pts with documented VT that has not resulted in cardiac arrest. Drugs : Quinidine or amiodarone may be used for pts not willing for ICD / reduced life expectancy. Electrical storm: Isoprotenol or Quinidine may be used.

Short QT Syndrome • Rare condition with short-QT interval (<320 ms). • Presents symptomatically with recurrent syncope, sudden cardiac death and atrial fibrillation. • Mutations in 6 different genes (3 gain of function and 3 loss of function) are identified.
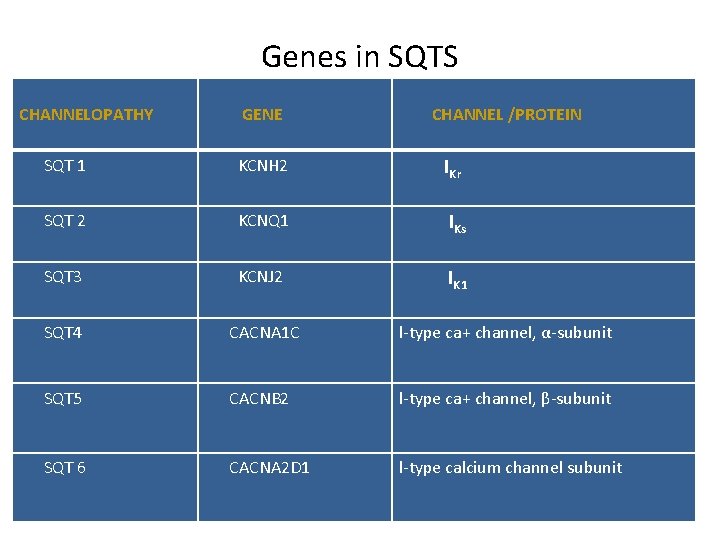

Genes in SQTS CHANNELOPATHY GENE CHANNEL /PROTEIN SQT 1 KCNH 2 IKr SQT 2 KCNQ 1 IKs SQT 3 KCNJ 2 IK 1 SQT 4 CACNA 1 C l-type ca+ channel, α-subunit SQT 5 CACNB 2 l-type ca+ channel, β-subunit SQT 6 CACNA 2 D 1 l-type calcium channel subunit

Basis of Arrhythmogenesis • Abbreviation of action potential in SQTS is heterogeneous with preferential abbreviation of either epicardial or endocardial cells as compared with sub-endocardial M cells, resulting in dispersion of repolarization. • Dispersion of repolarization serves as substrate for initiation and maintenance of reentry.

• In a case series 1 of 29 pts 62 % (18 out of 29) were symptomatic Cardiac arrest – 34 %(initial symptom in 28%) Palpitations – 31 % Syncope – 24 % Atrial fibrillation – 17 % • Electrocardiographic findings Abnormally short QT interval Absence of ST segment Tall and peaked T waves Prolonged Tpeak-Tend interval and Tpeak-Tend/QT ratio. 1. Carla Giustetto, Fernando Di Monte etal EHJ(2006) 27, 2440– 2447
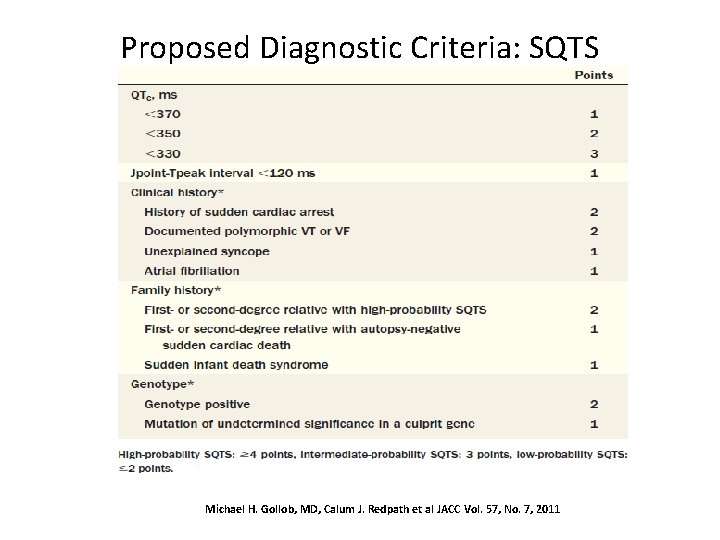
Proposed Diagnostic Criteria: SQTS Michael H. Gollob, MD, Calum J. Redpath et al JACC Vol. 57, No. 7, 2011

Management • ICD implantation recommended for both primary and secondary prevention of SCD in pts with SQTS. • Pharmacological therapy with QT prolonging drugs. • Quinidine is recommended in SQT 1 syndrome. • Disopyramide and amiodarone are also shown to prolong QT in SQTS pts.

Catecholaminergic polymorphic ventricular tachycardia (CPVT) • CPVT is a disorder of intracellular calcium handling causing adrenergic-dependent arrhythmias and sudden death. • Pts have normal resting ECG and develop ventricular ectopy progressing to bidirectional or polymorphic VT during exercise or catecholamine infusion. • Pts present with life-threatening VT or VF occurring during emotional or physical stress. • Affected patients may have a family h/o juvenile sudden death or stress-induced syncope. • CPVT can also present sporadically following a de novo mutation.

Genetic basis • Mutations in 2 genes are identified : ryanodine receptor gene (Ry. R 2) and calsequestrin 2 gene (CASQ 2). • Ry. R 2 mediates release of Ca+ from SR which is is required for myocardial contraction. • Ry. R 2 mutation result in Autosomal Dominant form of CPVT • Calsequestrin 2 protein is a protein in sarcoplasmic reticulum which binds large amounts of calcium. • CASQ 2 mutation result in Autosomal Recessive form of CPVT.

Mechanism for Arrhythmogenesis • Delayed after depolarization (DAD) dependent triggered activity. • Mutant ryanodine receptor is leaky and it releases excess of calcium during diastole. • This activates sodium-calcium exchanger that extrudes calcium ions out from the cell. • This generates a net inward current results in DAD. • When large enough, DADs trigger extrasystolic action potential.
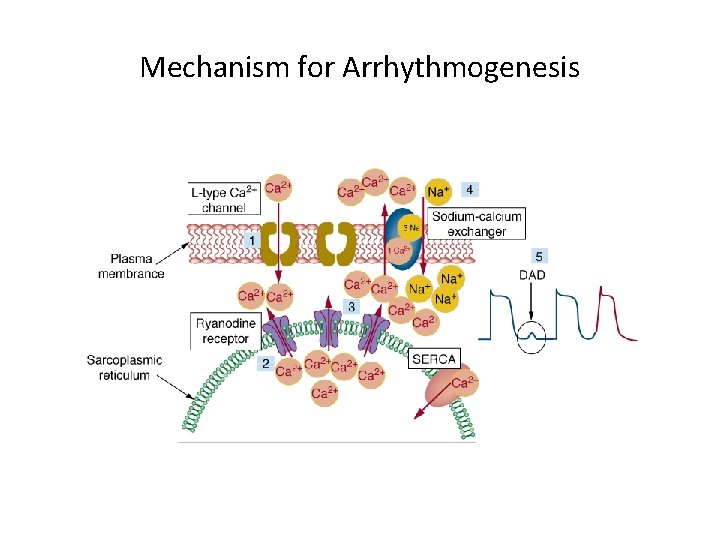
Mechanism for Arrhythmogenesis

Treatment • Avoiding competitive sports • Beta blockers for all pts with spontaneous or documented stressinduced ventricular arrhythmias. • For survivors of cardiac arrest or pts with syncope or sustained VT or VF despite therapy with beta blockers, ICD is recommend. • Flecainide or verapamil may be given for pts who are symptomatic with ICD and beta blockers. • Left sympathetic denervation for pts who remain symptomatic after maximal medical therapy.

Other Channelopathies Arrhythmogenic Right Ventricular Cardiomyopathy ( ARVC ) Ø Subset of ARVC is caused by defects in cardiac ryanodine receptor (Ry. R 2) Ø May represent a variant of CPVT rather than a subset of CPVT. Ø Majority are caused by defects in desmosomal proteins PKP 2 encoding plakophilin 2 : most common DSP encodes desmoplakin DSG 2 encodes desmoglein 2 Ø Hallmark of ARVC is fibrofatty replacement of the myocardium Ø Arrhythmias may precede histological evidence of disease
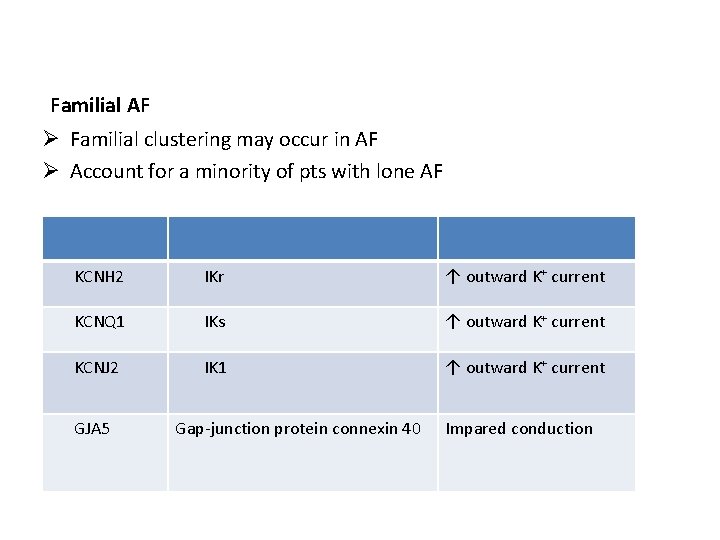
Familial AF Ø Familial clustering may occur in AF Ø Account for a minority of pts with lone AF KCNH 2 IKr ↑ outward K+ current KCNQ 1 IKs ↑ outward K+ current KCNJ 2 IK 1 ↑ outward K+ current GJA 5 Gap-junction protein connexin 40 Impared conduction

Sinus Node Dysfunction and Conduction Defects Ø Mutations of HCN 4 gene which codes for cardiac pacemaker current (If) results in sinus node dysfunction. Ø Other mutation which are associated with conduction defects are SCN 5 A , NKX 2. 5 and GATA 5

Summary • Cardiac channelopathies represent a group of disorders with inherited arrhythmogenic potential and structurally normal heart. • Majority are due to mutations in genes encoding Na+ , K+ , Ca + channels of heart. • In LQTS arrhythmia is triggered by exercise , emotion or noice. • Brugada syndrome is diagnosed by type 1 Ecg and documented event. • Beta blockers are useful in LQT 1 and CPVT. • ICD is indicated in survived cardiac arrest pts and in high risk patients.

THANK YOU
- Slides: 58