Carbohydrate Disposal This version is quite information dense

Carbohydrate Disposal This version is quite “information dense” to save paper.

Sources of Dietary Carbs • Starch – polymer of glucose – Amylose • linear, forms helices, difficult to digest, flatulence – Amylopectin • branched, easy to digest

Sources of Dietary Carbs • Disaccharides – Lactose • galactose and glucose • consequences of lactase deficiency = lactose intolerance – Sucrose • fructose and glucose – Maltose • glucose and glucose • Monosaccharides – Glucose – Fructose • especially these days with high fructose corn syrup
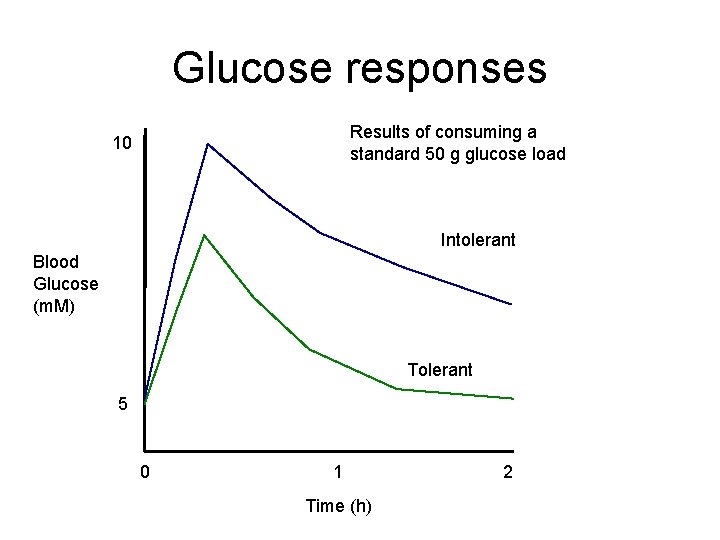
Glucose responses Results of consuming a standard 50 g glucose load 10 Intolerant Blood Glucose (m. M) Tolerant 5 0 1 Time (h) 2

Consequences of Intolerance • Post-prandial hyperglycemia is a problem – If occurs after each meal and persists for several hours then there will be problems • The person will rarely be euglycemic! • Leads to complications of hyperglycemia • Protein glycosylation – Root cause may be insulin resistance • Impaired ability of tissues to respond to insulin • Underlies Type II Diabetes • Control of glucose intolerance – Consumption of slowly absorbed starches
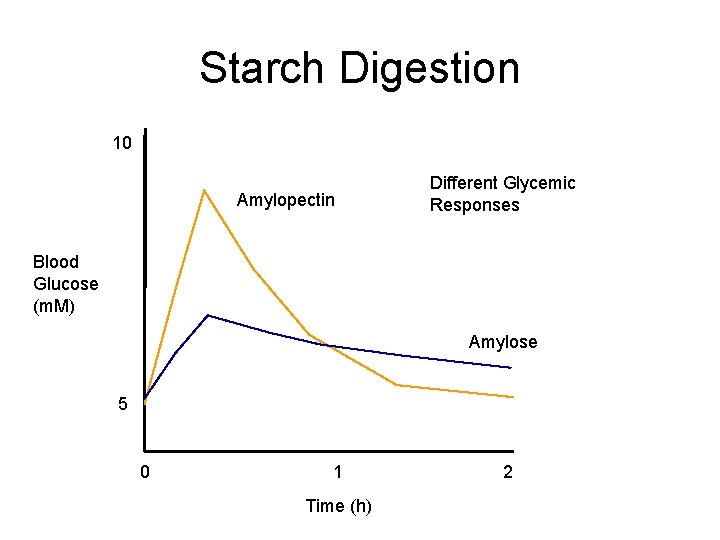
Starch Digestion 10 Amylopectin Different Glycemic Responses Blood Glucose (m. M) Amylose 5 0 1 Time (h) 2

The Glycemic Index • Describes the post-prandial glucose response – Area under the ‘test’ food glucose curve divided by – Area under a ‘reference’ food glucose curve • Reference food is normally 50 g gluocse • Test food given in an amount that will give 50 g digestible carbohydrate – Expressed as a % – GI of modern, processed, amylopectin foods >80 – GI of legumes < 30

The Glycemic Index • Useful knowledge for controlling blood glucose – Especial relevance to diabetes – QUALITY of carbohydrate (GI) as important as total amount of carbohydrate

GI critics say. . • Area under slowly absorbed may be the same as quickly absorbed – Look closely at previous figure • The GI should not apply to foods other than starches – Sugary foods are low GI • Because half the carbohydrate is fructose • Similarly, fructose containing foods are low GI – Dairy foods are low GI • Because half the carbohydrate is galactose • And protein elicits insulin secretion lipogenesis

GI critics say. . • Some Low GI values – Due to inaccurate estimation of digestible carbohydrate portion • Claims of “slow burning energy” ? ? – What regulates energy expenditure and ‘supply’ of substrates? – Even if supply was important, the classic “persistently but subtly” raised post-prandial glucose response is hardly ever seen
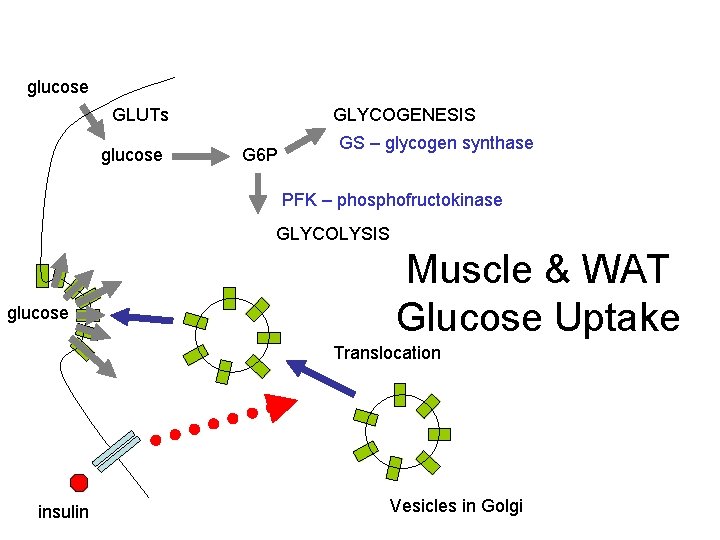
glucose GLUTs glucose GLYCOGENESIS G 6 P GS – glycogen synthase PFK – phosphofructokinase GLYCOLYSIS glucose Muscle & WAT Glucose Uptake Translocation insulin Vesicles in Golgi
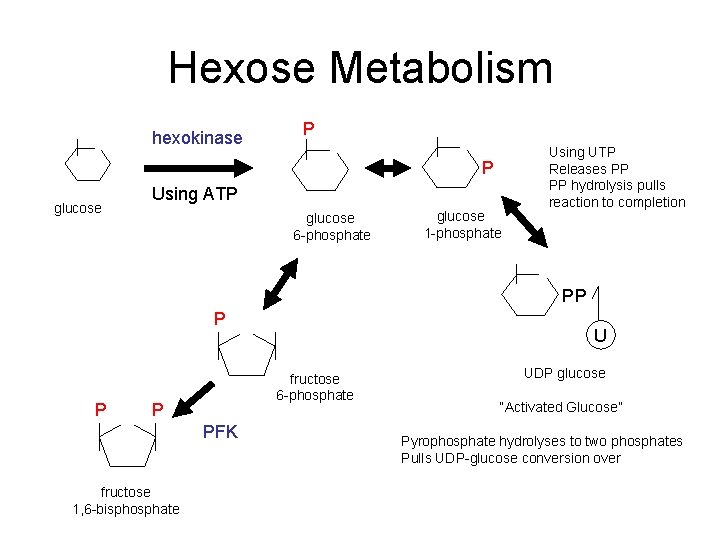
Hexose Metabolism hexokinase P P glucose Using ATP glucose 6 -phosphate glucose 1 -phosphate Using UTP Releases PP PP hydrolysis pulls reaction to completion PP P P fructose 6 -phosphate P PFK fructose 1, 6 -bisphosphate U UDP glucose “Activated Glucose” Pyrophosphate hydrolyses to two phosphates Pulls UDP-glucose conversion over
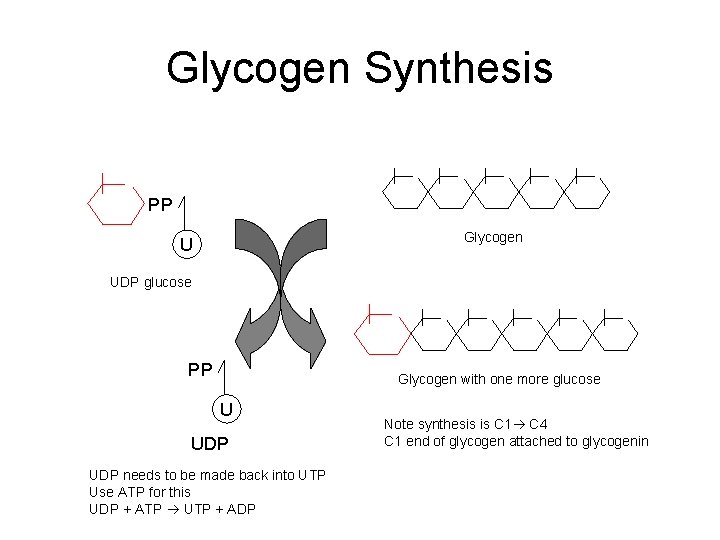
Glycogen Synthesis PP Glycogen U UDP glucose PP Glycogen with one more glucose U UDP needs to be made back into UTP Use ATP for this UDP + ATP UTP + ADP Note synthesis is C 1 C 4 C 1 end of glycogen attached to glycogenin

Glycogen Synthase • Catalyses the addition of ‘activated’ glucose onto an existing glycogen molecule – UDP-glucose + glycogenn UDP + glycogenn+1 • Regulated by reversible phosphorylation (covalent modification) – Active when dephosphorylated, inactive when phosphorylated • Phosphorylation happens on a serine residue – Dephosphorylation catalysed by phosphatases (specifically protein phosphatase I, PPI) – Phosphorylation catalysed by kinases (specifically glycogen synthase kinase) • Insulin stimulates PPI – And so causes GS to be dephosphorylated and active – So insulin effectively stimulates GS

Phosphofructokinase • Catalyses the second ‘energy investment’ stage of glycolysis – F 6 P + ATP fructose 1, 6 bisphosphate + ADP • Regulated allosterically – Simulated by low energy charge • Energy charge is balance of ATP, ADP & AMP • An increase in ADP/AMP and a decrease in ATP • These molecules bind at a site away from the active site – the allosteric binding sites. • Small change in ATP/ADP causes large change in AMP via adenylate kinase reaction – Many other molecules affect PFK allosterically but all are effectively indicators of ‘energy charge’

Coupling (again!) • The stimulation of glycogen synthesis by insulin creates an ‘energy demand’ – Glycogenesis is anabolic – The activation of glucose requires ATP – This drops the cellular [ATP] and increases the [ADP] & [AMP] • Drop in ‘energy charge’ is stimulates PFK – Anabolic pathway requires catabolic pathway – Insulin has ‘indirectly’ stimulated PFK and glucose oxidation – So signals to store fuels also cause fuels to be burnt

Liver Glucose Uptake • GLUT-2 used to take up glucose from bloodstream – Very high activity and very abundant – [Glucose] blood = [Glucose] liver • Glucokinase – Rapidly converts G G 6 P – Not inhibited by build up of G 6 P – High Km (10 m. M) for glucose – not saturated by high levels of liver glucose – So [G 6 P] rapidly increases as blood [glucose] rises • G 6 P can stimulate inactive GS – Even phosphorylated GS – Glucose itself also stimulates the dephosphorylation of GS • Via a slightly complex process that involves other kinases and phosphatases which we needn’t go into right now

Glycogenesis • In liver – The “push” mechanism • Glycogenesis responds to blood glucose without the need of insulin • Although insulin WILL stimulate glycogenesis further • In muscle – [G 6 P] never gets high enough to stimulate GS • “Push” method doesn’t happen in muscle • More of a “pull’ as insulin stimulates GS

Glycogenesis • In both liver and muscle – 2 ATPs required for the incorporation of a glucose into glycogen chain • G G 6 P and UDP UTP – Branching enzyme needed to introduce a 1 6 branch points – Transfers a segment from one chain to another – Limit to the size of glycogen molecule • Branches become too crowded, even if they become progressively shorter • Glycogen synthase may need to interact with glycogenin to be fully active

Hexokinases • Glucokinase (GK) – – – Only works on glucose High Km for glucose (~10 m. M) Not inhibited by G 6 P Only presents in liver, beta-cells Responsive to changes in [glucose] blood • Hexokinase (HK) – – – Works on any 6 C sugar Km for glucose ~0. 1 m. M Strongly inhibited by its product G 6 P Present in all other tissues If G 6 P is not used immediately, its build up and inhibits hexokinase – Easily saturated with glucose
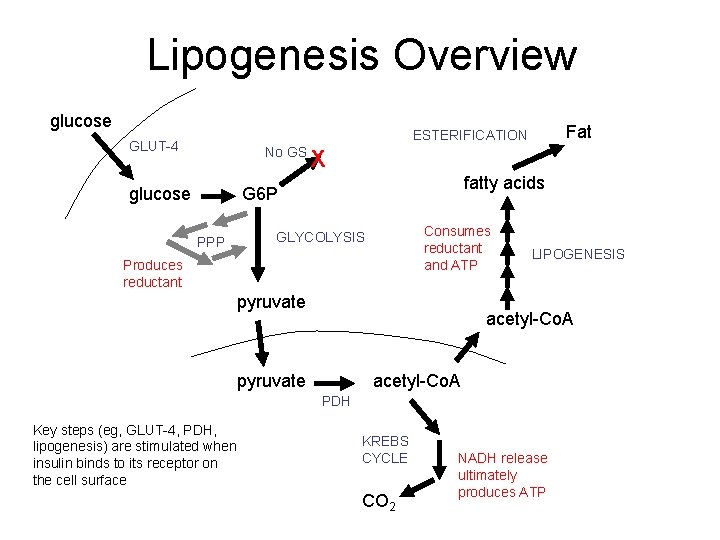
Lipogenesis Overview glucose Fat ESTERIFICATION GLUT-4 No GS glucose X fatty acids G 6 P PPP Consumes reductant and ATP GLYCOLYSIS Produces reductant pyruvate LIPOGENESIS acetyl-Co. A pyruvate acetyl-Co. A PDH Key steps (eg, GLUT-4, PDH, lipogenesis) are stimulated when insulin binds to its receptor on the cell surface KREBS CYCLE CO 2 NADH release ultimately produces ATP

Pyruvate Dehydrogenase Pyruvate + Co. A + NAD acetyl-Co. A + NADH + CO 2 • Irreversible in vivo • No pathways in humans to make acetate into ‘gluconeogenic’ precursors – Can’t make glucose from acetyl-Co. A – No way of going back once the PDH reaction has happened – Key watershed between carbohydrate and fat metabolism

PDH Control • Regulated by reversible phosphorylation – Active when dephosphorylated • Inactivated by PDH kinase • Activated by PDH phosphatase – Insulin stimulates PDH phosphatase • Insulin thus stimulates dephosphorylation and activation of PDH

Fate of Acetyl-Co. A • Burnt in the Krebs Cycle – Carbon atoms fully oxidised to CO 2 – Lots of NADH produced to generate ATP • Lipogenesis – Moved out into the cytoplasm – Activated for fat synthesis • In both cases the first step is citrate formation – Condensation of acetyl-Co. A with oxaloacetate • Regenerates Coenzyme A – Transport or Oxidation • The ‘fate’ will depend on the need for energy (ATP/energy charge) and the stimulus driving lipogenesis

ATP-Citrate Lyase • Once in the cytoplasm, the citrate is cleaved – By ATP-Citrate Lyase (ACL) – Using Co. A to generate acetyl-Co. A and oxaloacetate • Reaction requires ATP ADP + phosphate • ACL is inhibited by hydroxy-citrate (OHCit) – OHCit is found in the Brindleberry • Sold as a fat synthesis inhibitor – Would we expect it to prevent the formation of fatty acids • And, if so, would that actually help us lose weight?

The Carrier • Oxaloacetate produced by ACL needs to return to the matrix – Otherwise the mitochondrial oxaloacetate pool becomes depleted – Remember, oxaloacetate is really just a ‘carrier’ of acetates • Both in the Krebs's cycle and in the transport of acetyl-Co. As into the cytoplasm – Oxaloacetate cannot cross the inner mitochondrial membrane • Some interesting inter-conversions occur to get it back in!

Acetyl-Co. A Carboxylase • Activates acetyl-Co. A and ‘primes’ it for lipogenesis • Unusual in that it ‘fixes’ carbon dioxide – In the form of bicarbonate – A carboxylation reaction Acetyl-Co. A + CO 2 malonyl-Co. A – Reaction requires ATP ADP + phosphate – Participation of the cofactor, biotin • Biotin is involved in other carboxylation reactions

ACC Control • ACC is stimulated by insulin – Malonyl-Co. A is committed to lipogenesis • Reversible Phosphorlyation • Stimulated allosterically by citrate (polymerisation) • Inhibited allosterically by long-chain fatty acyl-Co. As

Malonyl-Co. A • Activated acetyl-Co. A – – Tagged and primed for lipogenesis But also a key regulator of fatty acid oxidation ACC is not only present in lipogenic tissues Also present in tissues that need to produce malonyl. Co. A in ‘regulatory’ amounts • Malonyl-Co. A inhibits carnitine acyl transferase I – An essential step in fatty acid oxidation – Only way of getting long chain fatty acyl-Co. As into the mitochondria

Malonyl-Co. A • So when ACC is active in, say, muscle – Malonyl-Co. A concentration rises – CPT-1 is inhibited – Fatty acid oxidation stops – Cell must use carbohydrate instead – Therefore insulin, by stimulating acetyl-Co. A carboxylase, encourages carbohydrate oxidation and inhibits fatty acid oxidation

Fatty Acyl Synthase

FAS - simplified

FAS • Fatty acyl synthase (FAS) is multi-functional – Lots of different enzyme activities in the complex – Can you count them all? • Bringing in acetyl and malonyl groups, catalysing the reaction between the decarboxylated malonyl and the growing fatty acid chain, the reduction/dehydration/reduction steps, moving the fatty acid to the right site and finally releasing it as FA-Co. A • Two free -SH groups on an ‘acyl-carring protein’ – Keeps the intermediates in exactly the right position for interaction with the right active sites – Each new 2 C unit is added onto the carboxy-end

Addition Sequence • Each round of 2 C addition requires – 2 molecules of NADPH … but No ATP (!!) – The release of the carbon dioxide that went on during the production of malonyl-Co. A • Thus the carboxylation of acetyl-Co. A does not result in ‘fixing’ CO 2 • FAs start getting ‘released’ as FA-Co. A when chain length is C 14 – Desaturation is done AFTER FAS

Pentose Phosphate Pathway • Provides NADPH for lipogenesis – NADPH - A form of NADH involved in anabolic reactions – Rate of NADPH production by PPP is proportional to demand for NADPH • Key regulatory enzyme is G 6 PDH – Glucose 6 -phosphate dehydrogenase G 6 P + NADP 6 -phosphogluconolactone + NADPH – The gluconolactone is further oxidised to give more NADPH • Decarboxylation to give a 5 -carbon sugar phosphate (ribulose 5 -phosphate)

Pentose Phosphate Pathway • Need to put the 5 -C sugar back into glycolysis – Accomplished by rearranging and exchanging carbon atoms between 5 C molecules – Catalysed by enzymes called transaldolases and transketolases • So, 5 C + 5 C C 7 + C 3 by a transketolase (2 C unit transferred) • Then C 7 + C 3 C 6 + C 4 by a transaldolase (3 C unit transferred) • Then C 4 + C 5 C 6 + C 3 by a transketolase (2 C unit transferred) – The C 6 and C 3 sugars can go back into glycolysis • Alternatively, PPP used to make ribose 5 -phosphate – Important in nucleotide pathways • Or generate NADPH as an anti-oxidant – Red blood cells - deficiency in G 6 PDH can cause anemia

Esterification • Formation of Fat • Glycerol needs to be glycerol 3 -phosphate – From reduction of glycolytic glyceraldehyde 3 -phosphate – Glycolysis important both for production of acetyl-Co. A and glycerol! • Esterification enzyme uses FA-Co. A – Not just FAs – FAs added one at a time • Both esterification enzyme and FAS are unregulated by insulin – Gene expression and protein synthesis • FAS is downregulated when lots of fat around – As in a Western diet!!
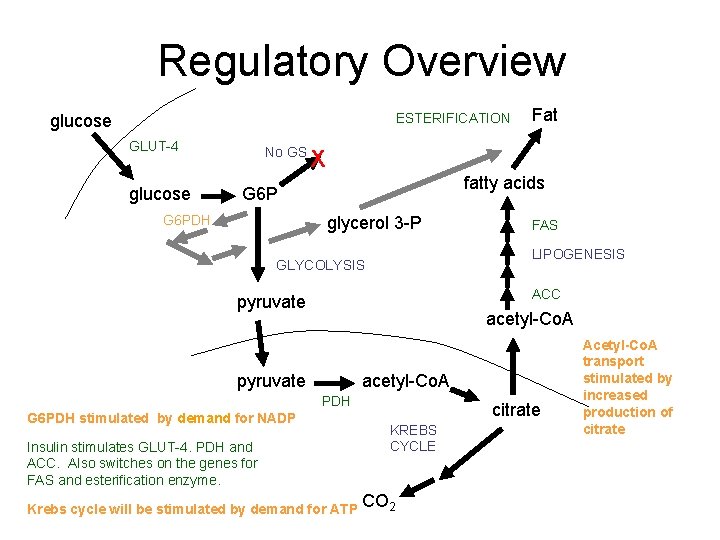
Regulatory Overview ESTERIFICATION glucose GLUT-4 glucose No GS X fatty acids G 6 PDH Fat glycerol 3 -P FAS LIPOGENESIS GLYCOLYSIS ACC pyruvate acetyl-Co. A PDH G 6 PDH stimulated by demand for NADP Insulin stimulates GLUT-4. PDH and ACC. Also switches on the genes for FAS and esterification enzyme. Krebs cycle will be stimulated by demand for ATP citrate KREBS CYCLE CO 2 Acetyl-Co. A transport stimulated by increased production of citrate
- Slides: 38