Capnography in prehospital care Picture space central BASICS
Capnography in pre-hospital care Picture space central © BASICS Education October 2017

Capnography in pre-hospital care Aims • To review the role of capnography • To understand its application in pre-hospital care • To present some of the relevant evidence base

History • • • First used in Holland in the 1970’s Established in hospital medicine within anaesthesia and intensive care Standard of care within UK pre-hospital care: • • • Immediate Care Practitioners HEMS physicians Critical care paramedics

Capnography Provides information on: • • CO 2 exhalation Respiratory patterns Real time indicator of: • Respiratory rate • A sudden drop may indicate reduced cardiac output or pulmonary embolism Usually achievable in the self-ventilating or ventilated patient
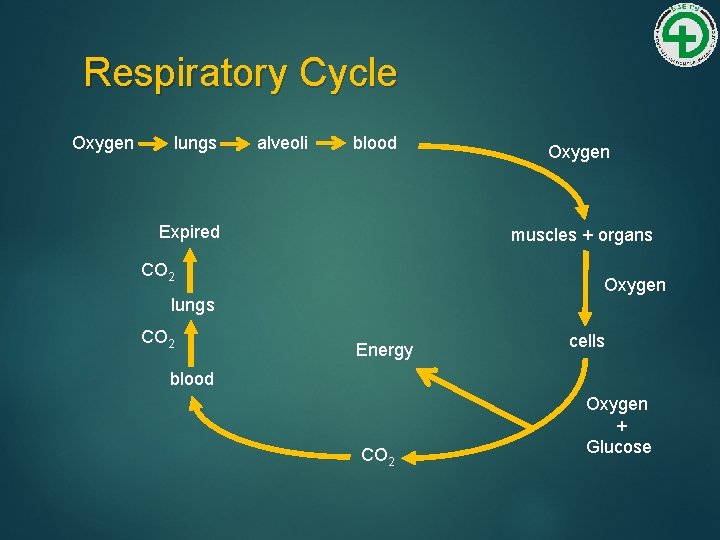
Respiratory Cycle Oxygen lungs alveoli blood Expired muscles + organs CO 2 Oxygen lungs CO 2 Oxygen Energy cells blood CO 2 Oxygen + Glucose

ETCO 2 versus Sp. O 2 Fundamentally different Sp. O 2 measures oxygenation • Cannot determine the metabolism of oxygen • Does not demonstrate the amount of oxygen being used by a patient. • De-saturation occurs minutes after hypoventilation / apnoea

Capnographic devices Colourimetric • Indicates presence of CO 2 in expired air • Requires indwelling airway adjunct i. e. ETT or LMA • Confirmation of endotracheal tube placement in non-cardiac arrest patients is not always reliable • The membrane can change colour when the device is contaminated with acidic substances such as fizzy drinks, gastric acid or adrenaline • The device will not provide a reading if it is clogged with secretions. …of limited value in prehospital care

Capnographic devices Capnometer • Digital readout only • Some can be used with patients ventilating through mouth and nose • Some limited to being placed in line with LMA / ETT
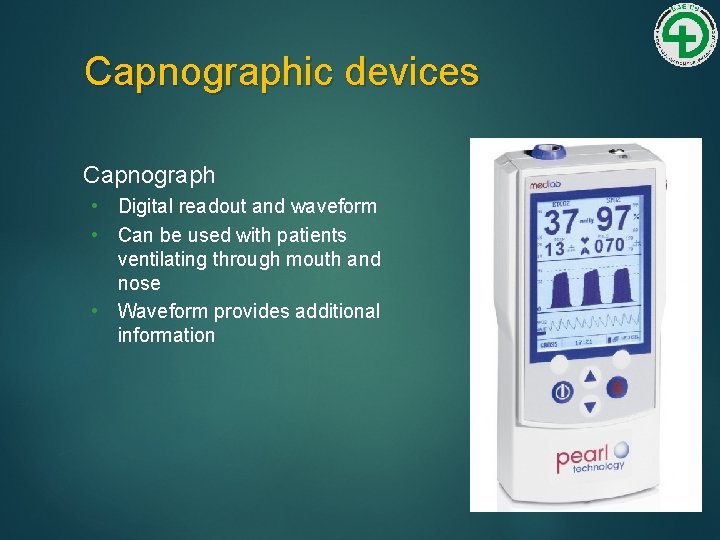
Capnographic devices Capnograph • Digital readout and waveform • Can be used with patients ventilating through mouth and nose • Waveform provides additional information

Capnography waveform Phase III Alveolar Expiration Phase 0 Inspiration Phase II Expiration Anatomical Dead Space Phase I Expiration Anatomical Dead Space
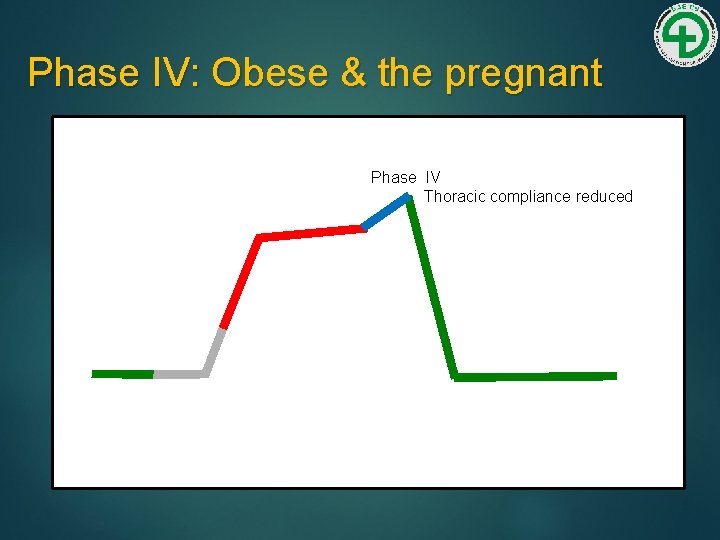
Phase IV: Obese & the pregnant Phase IV Thoracic compliance reduced
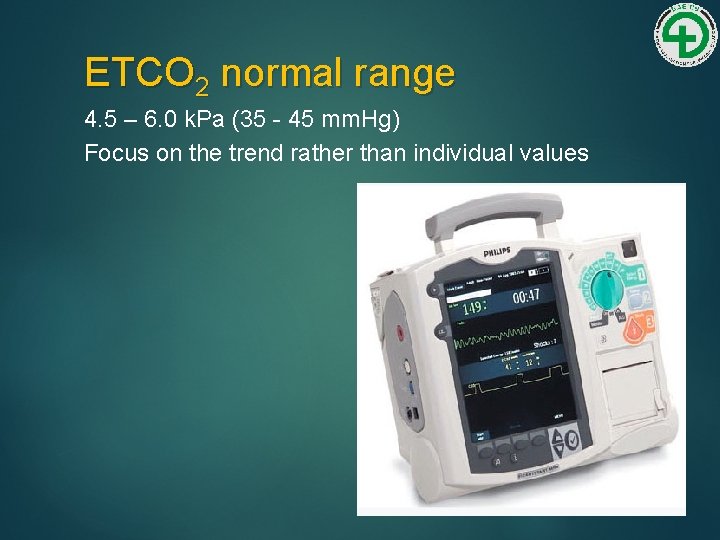
ETCO 2 normal range 4. 5 – 6. 0 k. Pa (35 - 45 mm. Hg) Focus on the trend rather than individual values
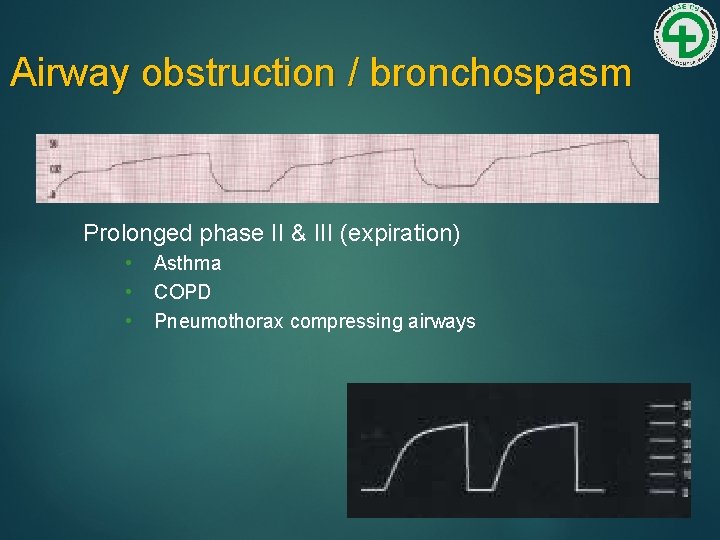
Airway obstruction / bronchospasm Prolonged phase II & III (expiration) • • • Asthma COPD Pneumothorax compressing airways

Increased ETCO 2 Output Fever Tourniquet release Pulmonary Perfusion Alveolar Ventilation Increased BP Hypoventilation Increased cardiac output Partial airway obstruction

Decreased ETCO 2 Output Hypothermia Pulmonary Perfusion Alveolar Ventilation Reduced cardiac output Hyperventilation Hypotension Apnoea Hypovolaemia Total airway obstruction Increasing pneumothorax Partial airway obstruction Tension pneumothorax Pulmonary embolism Cardiac arrest

Hyperventilation Kills

CPR ETCO 2 1. 5 – 2. 0 k. Pa (possibly higher) indicates adequate CPR • Change Rescuers if ETCO 2 falls below 1. 5 k. Pa
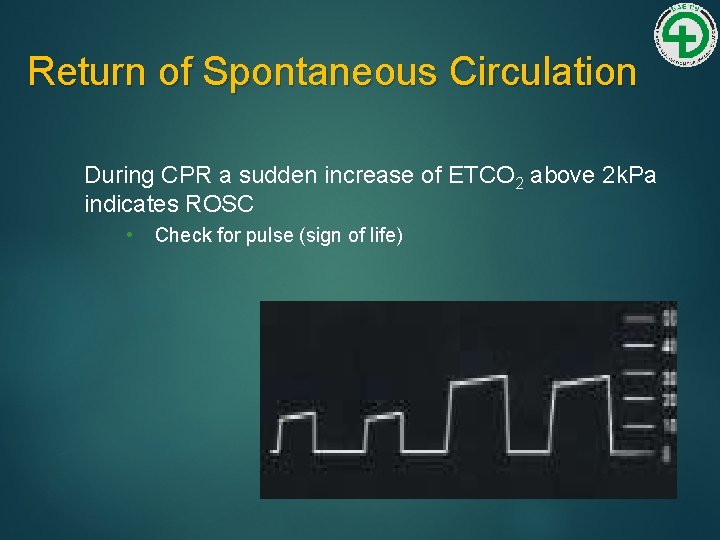
Return of Spontaneous Circulation During CPR a sudden increase of ETCO 2 above 2 k. Pa indicates ROSC • Check for pulse (sign of life)

Head injured patients Several studies have shown that inadvertent hyperventilation of head-injured patients in the pre-hospital phase has been linked to poor outcomes Deakin CD, Sado DM, Coats TJ, Davies G. Prehospital end-tidal carbon dioxide concentration and outcome in major trauma. J Trauma 2004; 57(1): 65 -68.

Head injury and abnormal ETCO 2 Aim to maintain at 4 k. Pa (30 mm. Hg) ETCO 2 raised: Increase minute volume or rate to blow off CO 2 ETCO 2 lowered Decrease minute volume or rate 4 k. Pa

Capnography Questions ?

Summary Capnography • Provides a breath by breath measurement of a patient's ventilation • Can quickly reveal a worsening trend in a patient's conditi • Allows pre-hospital clinicians to optimise their care throug careful ventilatory management

REFRESHER COURSE www. basics. org. uk
- Slides: 23