CAP Community Acquired Pneumonia CAP by Dr R

CAP Community Acquired Pneumonia (CAP) by Dr. R V S N Sarma. , MD. , MSc. , (Canada) Consultant Physician & Chest Specialist

CAP Improving Outcomes Through Education The New Treatment Paradigm – Selecting Appropriate Empiric Antibiotics
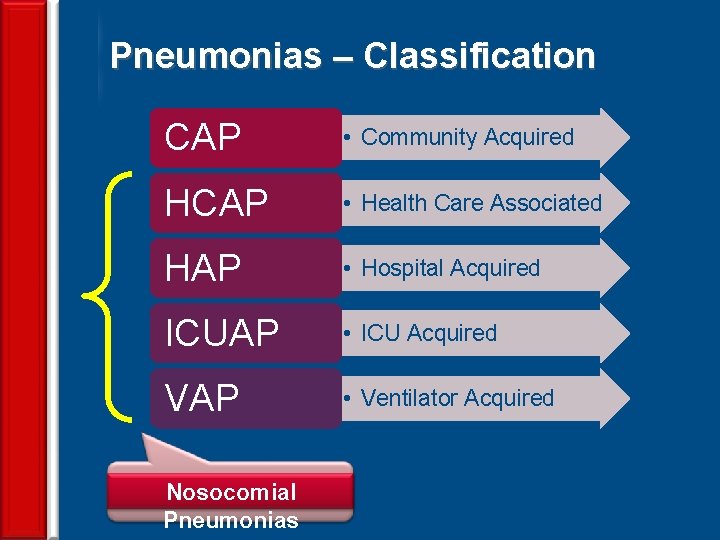
Pneumonias – Classification 3 CAP • Community Acquired HCAP • Health Care Associated HAP • Hospital Acquired ICUAP • ICU Acquired VAP • Ventilator Acquired Nosocomial Pneumonias

Community Acquired Pneumonia (CAP) § Definition … an acute infection of the pulmonary parenchyma that is associated with some symptoms of acute infection, accompanied by the presence of an acute infiltrate on a chest radiograph, or auscultatory findings consistent with pneumonia, in a patient not hospitalized or residing in a long term care facility for > 14 days before onset of Bartlett. Clin Infect Dis 2000; 31: 347 -82. 4 symptoms.

Guidelines for CAP § American Thoracic Society (ATS) § Guidelines - Management of Adults with CAP (2001) § Infectious Diseases Society of America (IDSA) § Update of Practice Guidelines Management of CAP in Immuno-competent adults (2003) § ATS and IDSA joint effort (we will follow this) § IDSA/ATS Consensus Guidelines on the Management of CAP in Adults (March 2007) 5

Why Guidelines? § Evidence-based practice § Best outcome for patients § Best use of resource § Restricts idiosyncratic behaviour § Legal protection § Identify research needs § A tool for education § Gain public confidence 6

CAP – The Two Types of Presentations • Sudden onset of CAP • High Classical fever, shaking chills • Pleuritic chest pain, SOB • Productive cough • Rusty sputum, blood tinge • Poor general condition • High mortality up to 20% in patients with bacteremia 7 Atypical • Gradual & insidious onset • Low grade fever • Dry cough, No blood tinge • Good GC – Walking CAP • Low mortality 1 -2%; except in cases of Legionellosis • Mycoplasma,

CAP – Pathogenesis Inhalation Aspiration Hematogenous 8

CAP – Risk Factors for Pneumonia § § § Age Obesity; Exercise is protective Smoking, PVD Asthma, COPD Immuno-suppression, HIV Institutionalization, Old age homes etc § Dementia 9 ID Clinics 1998; 12: 723. Am J Med 1994; 96: 313

Community Acquired Pneumonia (CAP) Epidemiology § 4 -5 million cases annually 10 § ~500, 000 hospitalizations – 20% require admission § ~45, 000 deaths § Fewest cases in 18 -24 yr group § Probably highest incidence in <5 and >65 yrs § Mortality disproportionately high in >65 yrs § Over all mortality is 2 -30%; Hospitalized Pt Bartlett. CID 1998; 26: 811 -38. mort
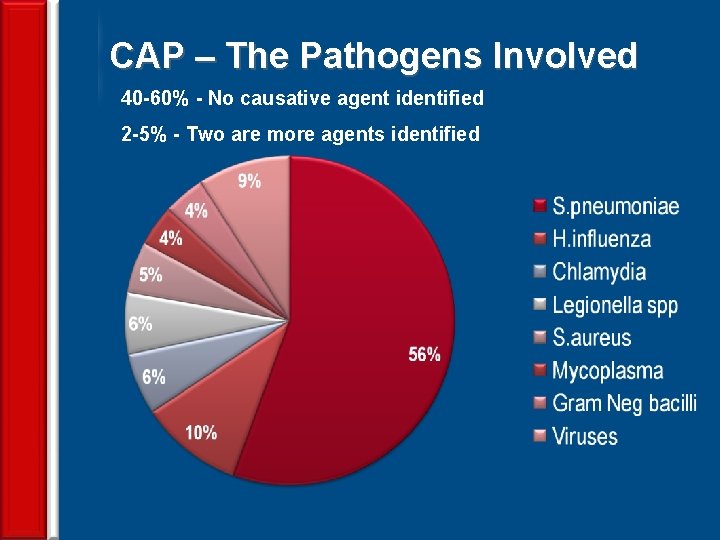
CAP – The Pathogens Involved 40 -60% - No causative agent identified 2 -5% - Two are more agents identified 11

Streptococcus pneumonia (Pneumococcus) § Most common cause of CAP § About 2/3 of CAP are due to S. pneumoniae § These are gram positive diplococci § Typical symptoms (e. g. malaise, shaking chills fever, rusty sputum, pleuritic chest pain, cough) § Lobar infiltrate on CXR § May be Immuno suppressed host 12 § 25% will have bacteremia – serious

CAP – Special Features – Pathogen wise Typical – S. pneumoniae, H. influenza, M. catarrhalis – Lungs Blood tinged sputum - Pneumococcal, Klebsiella, Legionella H. influenzae CAP has associated of pleural effusion S. Pneumoniae – commonest – penicillin resistance problem S. aureus, K. pneumoniae, P. aeruginosa – not in typical host S. aureus causes CAP in post-viral influenza; 13 Serious CAP

S. aereus CAP – Dangerous § This CAP is not common; Multi lobar Involvement § Post Influenza complication, Class IV or V § Compromised host, Co-morbidities, Elderly § CA MRSA – A Problem; CA MSSA also occurs § Empyema and Necrosis of lung with cavitations § Multiple Pyemic abscesses, Septic 14
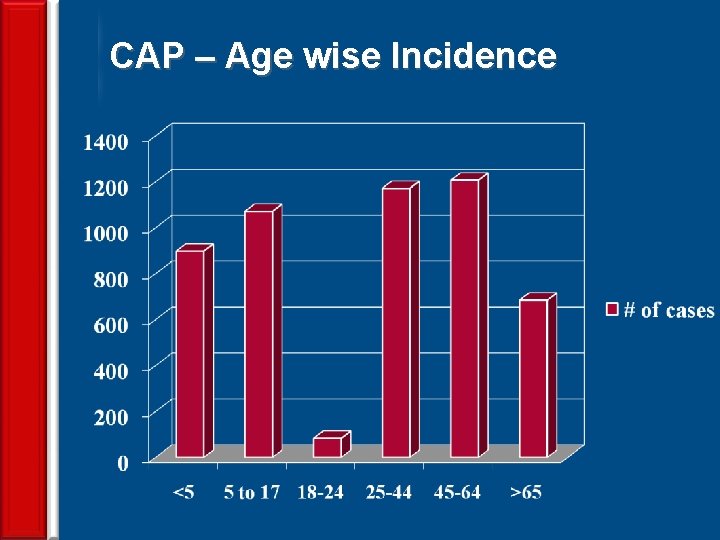
CAP – Age wise Incidence 15
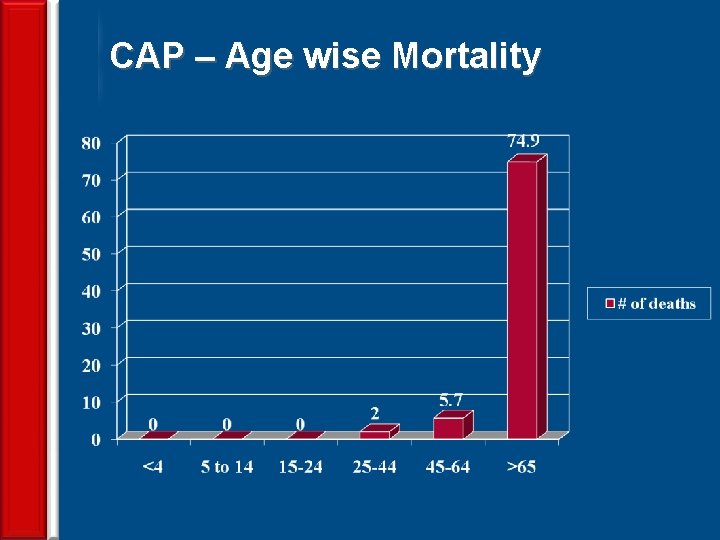
CAP – Age wise Mortality 16

CAP – Risk Factors for Hospitalization § Older, Unemployed, Unmarried § Recurrent common cold § Asthma, COPD; Steroid or bronchodilator use § Chronic diseases, Diabetes, CHF, Neoplasia § Amount of smoking § Alcohol is NOT related to increased ID Clinics 1998; 12: 723. Am J Med 1994; 96: 313 risk for hospitalization 17

CAP – Risk Factors for Mortality 18 § Age > 65 § Bacteremia (for S. pneumoniae) § S. aureus, MRSA , Pseudomonas § Extent of radiographic changes § Degree of immuno. ID Clinics 1998; 12: 723. Am J Med 1994; 96: 313
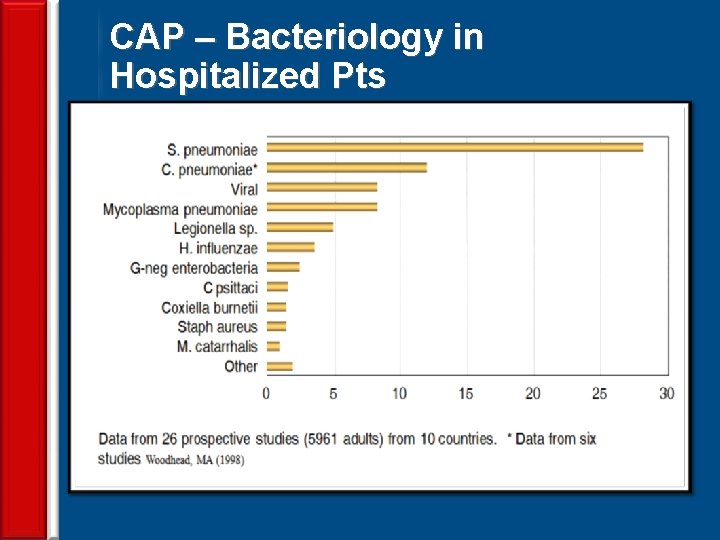
CAP – Bacteriology in Hospitalized Pts 19
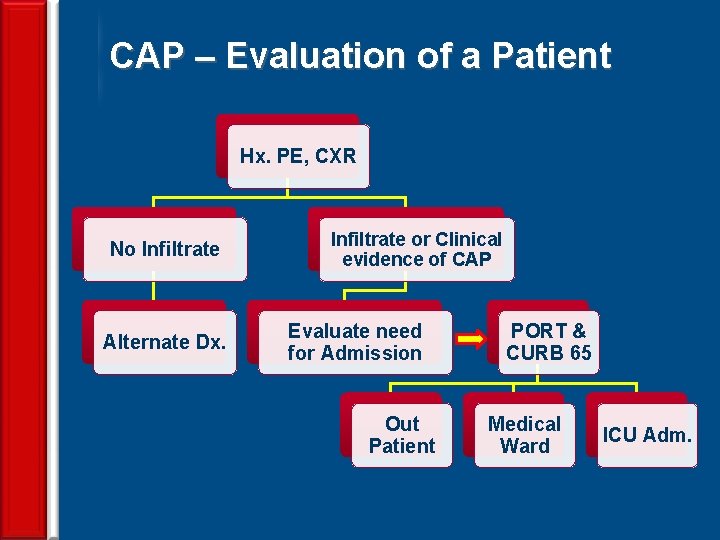
CAP – Evaluation of a Patient Hx. PE, CXR No Infiltrate Alternate Dx. Infiltrate or Clinical evidence of CAP Evaluate need for Admission Out Patient 20 PORT & CURB 65 Medical Ward ICU Adm.

CAP – Management Guidelines § Rational use of microbiology laboratory § Pathogen directed antimicrobial therapy whenever possible § Prompt initiation of Antibiotic therapy 21 § Decision to hospitalize based on prognostic criteria - PORT or CURB 65
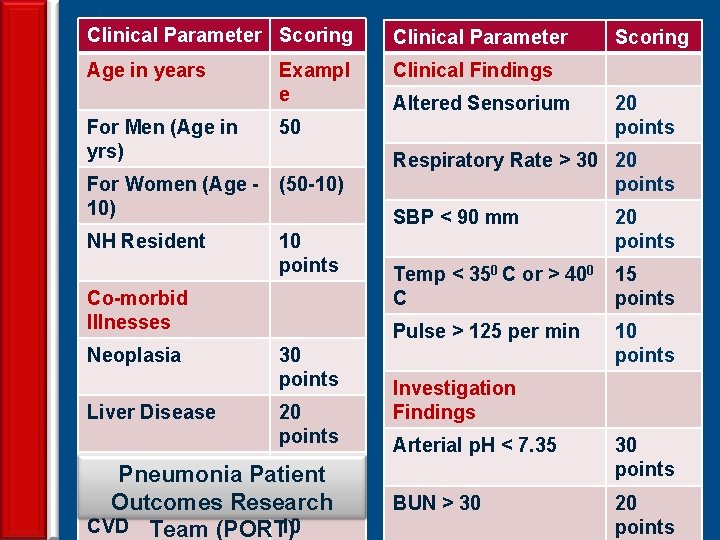
Clinical Parameter Scoring Clinical Parameter Age in years Clinical Findings For Men (Age in yrs) Exampl e 50 For Women (Age - (50 -10) NH Resident 10 points Co-morbid Illnesses Neoplasia 30 points 20 – PORT Scoring points PSI Liver Disease CHFPneumonia Patient 10 points Outcomes Research 22 CVD Altered Sensorium 10 Team (PORT) Scoring 20 points Respiratory Rate > 30 20 points SBP < 90 mm 20 points Temp < 350 C or > 400 C 15 points Pulse > 125 per min 10 points Investigation Findings Arterial p. H < 7. 35 30 points BUN > 30 20 points

Classification of Severity - PORT Class I Predictors Class II Absent Class IV 23 91 - 130 70 Class V Class III > 130 71 – 90
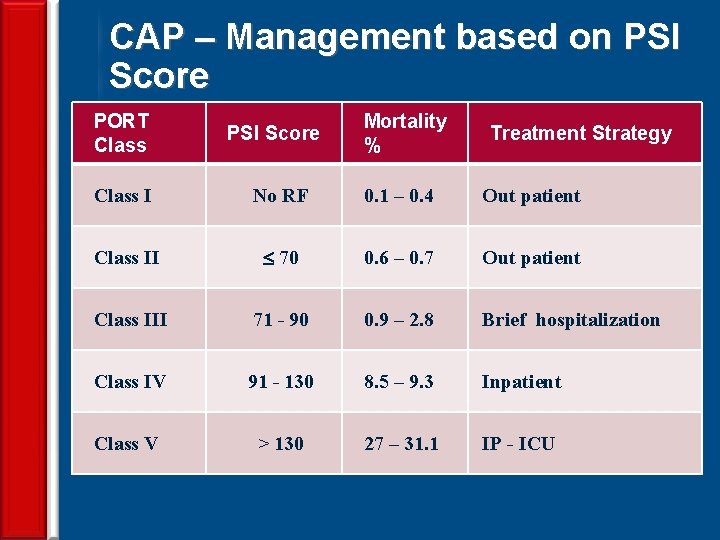
CAP – Management based on PSI Score PORT Class PSI Score Mortality % Treatment Strategy Class I No RF 0. 1 – 0. 4 Out patient Class II 70 0. 6 – 0. 7 Out patient Class III 71 - 90 0. 9 – 2. 8 Brief hospitalization Class IV 91 - 130 8. 5 – 9. 3 Inpatient Class V > 130 27 – 31. 1 IP - ICU 24
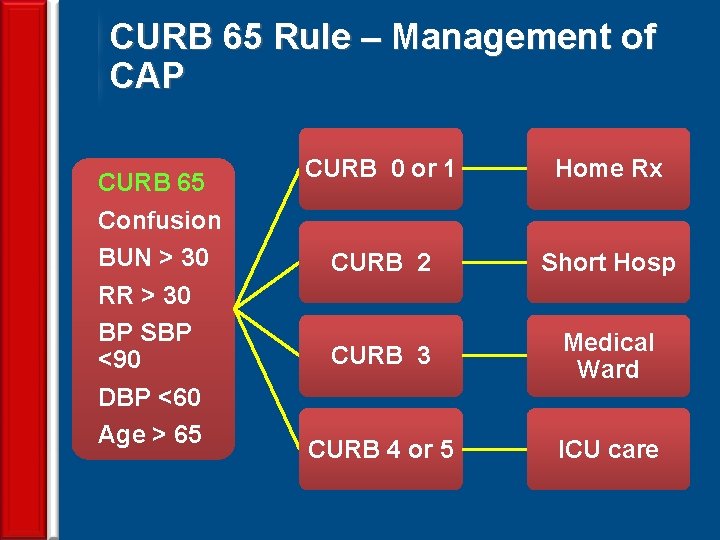
CURB 65 Rule – Management of CAP CURB 65 Confusion BUN > 30 RR > 30 BP SBP <90 DBP <60 Age > 65 25 CURB 0 or 1 Home Rx CURB 2 Short Hosp CURB 3 Medical Ward CURB 4 or 5 ICU care
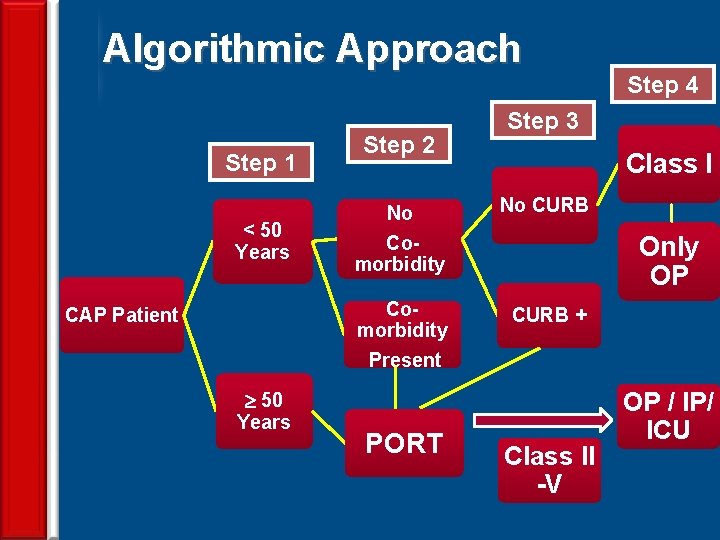
Algorithmic Approach Step 1 < 50 Years CAP Patient 50 Years 26 Step 2 Step 3 Class I No Comorbidity No CURB Comorbidity Present CURB + PORT Step 4 Only OP Class II -V OP / IP/ ICU

Who Should be Hospitalized? Class I and II hospitalization Usually do not require Class III May require brief hospitalization Class IV and V Usually do require Severity of CAP with poor prognosis hospitalization RR > 30; Pa. O 2/Fi. O 2 < 250, or PO 2 < 60 on room air Need for mechanical ventilation; Multi lobar involvement Hypotension; Need for vasopressors Oliguria; Altered mental status 27

CAP – Criteria for ICU Admission Major criteria § Invasive mechanical ventilation required § Septic shock with the need of vasopressors Minor criteria (least 3) § Confusion/disorientation § Blood urea nitrogen ≥ 20 mg% § Respiratory rate ≥ 30 / min; Core temperature < 36ºC § Severe hypotension; Pa. O 2/Fi. O 2 ratio ≤ 250 § Multi-lobar infiltrates 28§ WBC < 4000 cells; Platelets <100, 000

CAP – Laboratory Tests • CXR – PA & lateral • CBC with Differential • BUN and Creatinine • Serum electrolytes • FBG, PPBG • Gram stain of sputum • Liver enzymes • Culture of sputum 29 • Pre Rx. blood cultures

CAP – Value of Chest Radiograph • Usually needed to establish diagnosis • It is a prognostic indicator • To rule out other disorders • May help in etiological diagnosis J Chr Dis 1984; 37: 215 -25 30

Infiltrate Patterns and Pathogens CXR Pattern Possible Pathogens Lobar S. pneumo, Kleb, H. influ, Gram Neg Patchy Atypicals, Viral, Legionella Interstitial Viral, PCP, Legionella Cavitatory Anerobes, Kleb, TB, S. aureus, Fungi Large effusion Staph, Anaerobes, Klebsiella 31
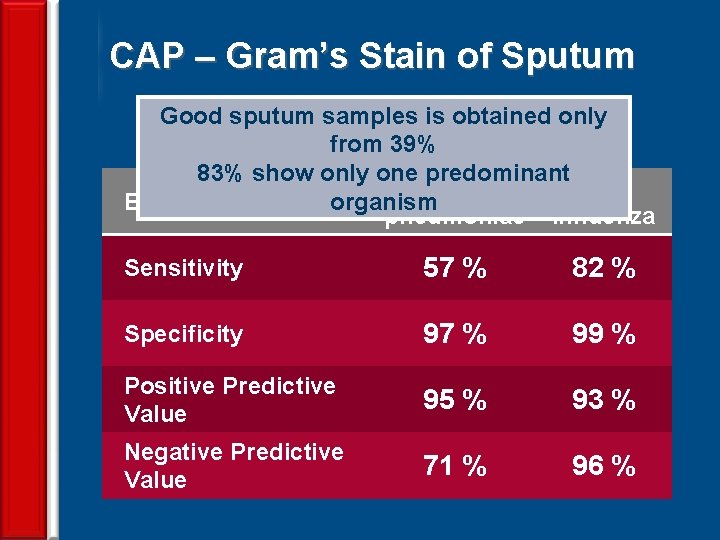
CAP – Gram’s Stain of Sputum Good sputum samples is obtained only from 39% 83% show only one predominant S. H. Efficiency of test organism pneumoniae influenza 32 Sensitivity 57 % 82 % Specificity 97 % 99 % Positive Predictive Value 95 % 93 % Negative Predictive Value 71 % 96 %
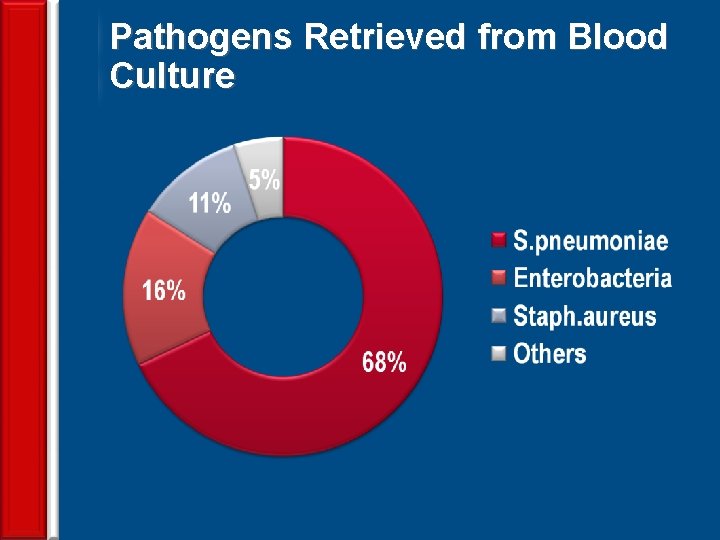
Pathogens Retrieved from Blood Culture 33

Mortality of CAP – Based on Pathogen § P. aeruginosa 61. 0 % § K. pneumoniae - 35. 7 % § S. aureus 31. 8 % § Legionella 14. 7 % § S. pneumoniae - 12. 0 % § C. pneumoniae - 9. 8 % § H. influenza 7. 4 % 34

Traditional Treatment Paradigm Conservative start with ‘workhorse’ antibiotics Reserve more potent drugs for non-responders 35

New Treatment Paradigm Hit hard and early with appropriate antibiotic(s) Short Rx. Duration; De-escalate where possible 36
The Therapy Conundrum Avoid emergence of multidrug resistant microorganisms Objective 1 37 Immediate Rx. of patients with serious sepsis Objective 2
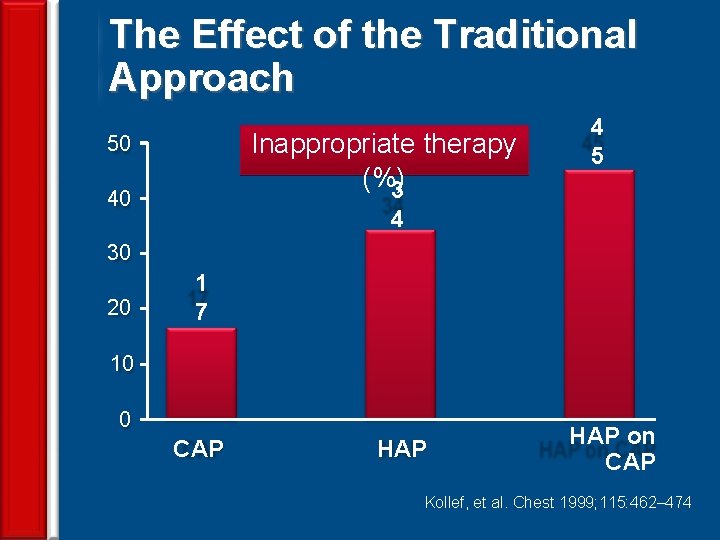
The Effect of the Traditional Approach Inappropriate therapy (%) 3 50 40 4 5 4 30 20 1 7 10 0 CAP 38 HAP on CAP Kollef, et al. Chest 1999; 115: 462– 474
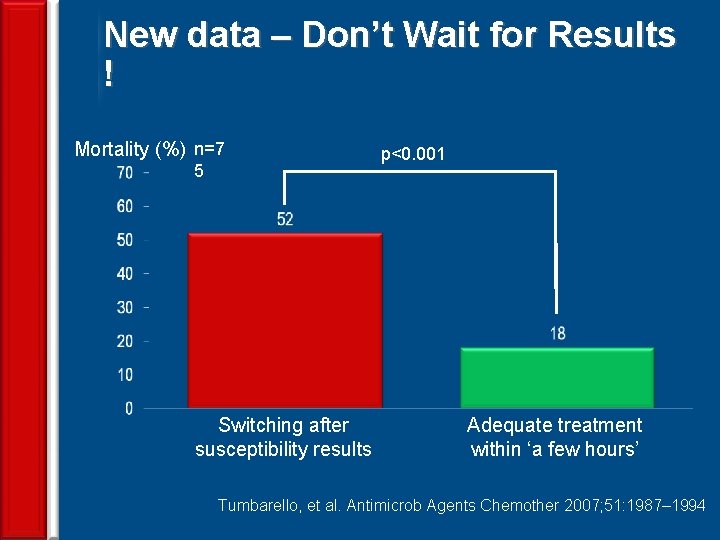
New data – Don’t Wait for Results ! Mortality (%) n=7 5 Switching after susceptibility results 39 p<0. 001 Adequate treatment within ‘a few hours’ Tumbarello, et al. Antimicrob Agents Chemother 2007; 51: 1987– 1994

CAP Treatment Consensus § Risk assessment approach § Early Antibiotic selection § Change treatment driven by local surveillance § Hit hard and hit early § As short a duration as possible § De-escalate when and where possible 40

OPAT – OP Parenteral Antimicrobial Therapy 41

Antibiotics of choice for CAP Antibiotics Macrolide -M • Azithromyci n • Clarithromy cin • Erythromyci n • Telithromycin 42 • Doxycycline Fluroquinolone. FQ • Levofloxacin • Moxifloxacin • Gatifloxacin • Trovafloxacin Betalactum B • Ceftriaoxon e • Cefotaxime • B Inhibitor BI • Sulbactam • Tazobacta
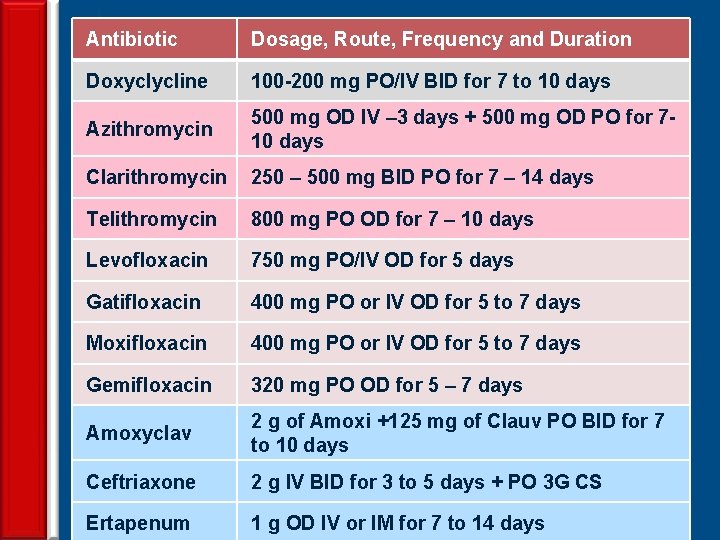
Antibiotic Dosage, Route, Frequency and Duration Doxyclycline 100 -200 mg PO/IV BID for 7 to 10 days Azithromycin 500 mg OD IV – 3 days + 500 mg OD PO for 710 days Clarithromycin 250 – 500 mg BID PO for 7 – 14 days Telithromycin 800 mg PO OD for 7 – 10 days Levofloxacin 750 mg PO/IV OD for 5 days Gatifloxacin 400 mg PO or IV OD for 5 to 7 days Moxifloxacin 400 mg PO or IV OD for 5 to 7 days Gemifloxacin 320 mg PO OD for 5 – 7 days Amoxyclav 2 g of Amoxi +125 mg of Clauv PO BID for 7 to 10 days Ceftriaxone 2 g IV BID for 3 to 5 days + PO 3 G CS 43 Ertapenum 1 g OD IV or IM for 7 to 14 days

Empiric Treatment – Outpatient Healthy and no risk factors for DR S. pneumoniae 1. Macrolide or Doxycycline Presence of co-morbidities, use of antimicrobials within the previous 3 months, and regions with a high rate (>25%) of infection with Macrolide resistant S. pneumoniae 1. Respiratory FQ – Levoflox, Gemiflox or 44

Empiric Treatment – Inpatient – Non ICU 1. A Respiratory Fluoroquinolone (FQ) Levo or 2. A Beta-lactam plus a Macrolide (or Doxycycline) (Here Beta-lactam agents are 3 Generation Cefotaxime, Ceftriaxone, Amoxiclav) 3. If Penicillin-allergic Respiratory FQ or 45 Ertapenem is another option

Empiric Treatment: Inpatient in ICU 1. A Beta-lactam (Cefotaxime, Ceftriaxone, or Ampicillin-Sulbactam) plus either Azithromycin or Fluoroquinolone 2. For penicillin-allergic patients, a respiratory 46 Fluoroquinolone and Aztreonam

Empiric Rx. – Suspected Pseudomonas 1. Piperacillin-Tazobactam, Cefepime, Carbapenums (Imipenem, or Meropenem) plus either Cipro or Levo 2. Above Beta-lactam + Aminoglycoside + Azithromycin 3. Above Beta-lactam + Aminoglycoside + an 47 antipseudomonal and antipneumococcal FQ

Empiric Rx. – CA MRSA For Community Acquired Methicillin-Resistant Staphylococcus aureus (CA-MRSA) § Vancomycin or Linezolid Neither is an optimal drug for MSSA § For Methicillin Sensitive S. aureus (MSSA) B-lactam and sometimes a respiratory Fluoroquinolone, (until susceptibility results). § Specific therapy with a penicillinase-resistant semisynthetic penicillin or Cephalosporin 48

Duration of Therapy • Minimum of 5 days • Afebrile for at least 48 to 72 h • No > 1 CAP-associated sign of clinical instability • Longer duration of therapy If initial therapy was not active against the identified pathogen or complicated by extra pulmonary infection 49
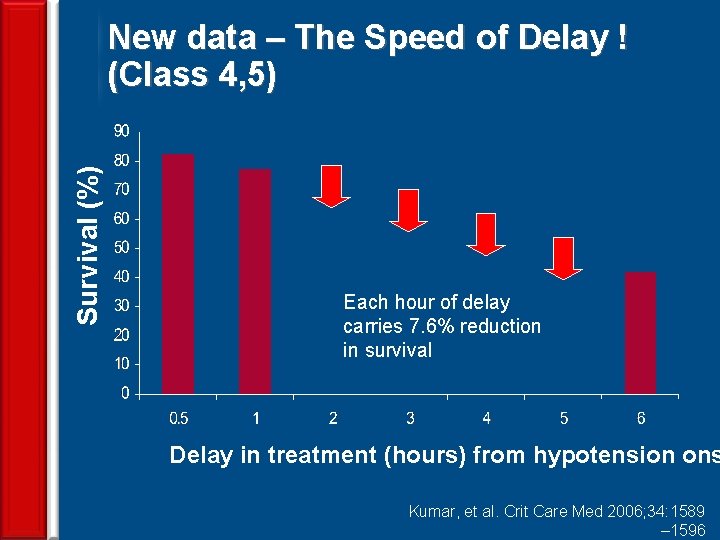
Survival (%) New data – The Speed of Delay ! (Class 4, 5) Each hour of delay carries 7. 6% reduction in survival Delay in treatment (hours) from hypotension ons 50 Kumar, et al. Crit Care Med 2006; 34: 1589 – 1596

CAP – Summary of Empiric Treatment Outpatient Rx – any one of the three • Macrolide or Doxycycline or Fluoroquinolone Patients in General Medical Ward • 3 rd Generation Cephalosporin + Macrolide • Betalactum / B-I + Macrolide or B / BI + FQ • Fluroquinolone alone Patients in ICU 51 • 3 GC + Macrolide 3 GC Clin + FQ IDSAor guidelines: Infect Dis 2000; 31: 347 -82
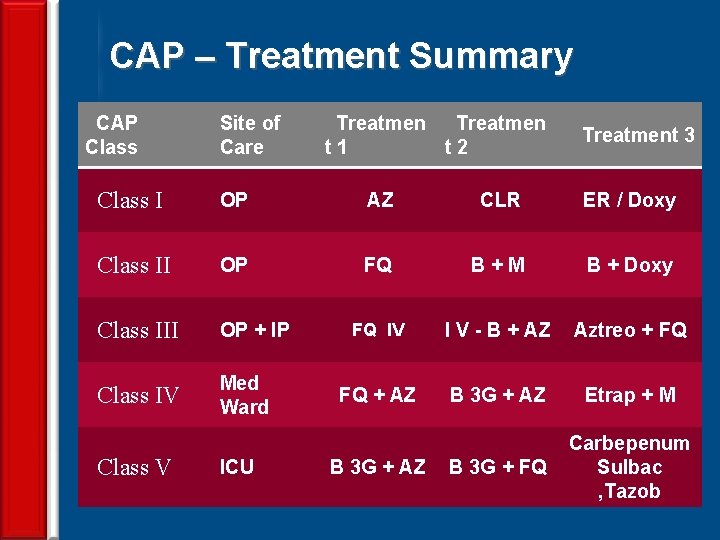
CAP – Treatment Summary CAP Class Site of Care Treatmen t 1 t 2 Treatment 3 Class I OP AZ CLR ER / Doxy Class II OP FQ B+M B + Doxy Class III OP + IP FQ IV I V - B + AZ Aztreo + FQ Class IV Med Ward FQ + AZ B 3 G + AZ Etrap + M B 3 G + FQ Carbepenum Sulbac , Tazob Class V 52 ICU B 3 G + AZ

Strategies for Prevention of CAP • Cessation smoking • Influenza Vaccine (Flu shot – Oct through Feb) It offers 90% protection and reduces mortality by 80% • Pneumococcal Vaccine (Pneumonia shot) It protects against 23 types of Pneumococci 70% of us have Pneumococci in our RT It is not 100% protective but reduces mortality 53 Age 19 -64 with co morbidity of high for

Switch to Oral Therapy § Four criteria § Improvement in cough, dyspnea & clinical signs § Afebrile on two occasions 8 h apart § WBC decreasing towards normal § Functioning GI tract with adequate oral intake § If overall clinical picture is otherwise favorable, hemodynamically stable; can 54

Management of Poor Responders § Consider non-infectious illnesses § Consider less common pathogens § Consider serologic testing § Broaden antibiotic therapy § Consider bronchoscopy 55

CAP – Complications § Hypotension and septic shock § 3 -5% Pleural effusion; Clear fluid + pus cells § 1% Empyema thoracis pus in the pleural space § Lung abscess – destruction of lung - CSLD § Single (aspiration) anaerobes, Pseudomonas § Multiple (metastatic) Staphylococcus aureus § Septicemia – Brain abscess, Liver Abscess § Multiple Pyemic Abscesses 56

Pneumocystis carinii (PCP) § Important cause of pneumonia in the severely immuno-compromised, i. e. not a “primary atypical pneumonia”. § Classically PCP pneumonia presents with slight fever, dyspnea and non-productive cough § Diagnosis – usually histological (silver staining). 57§ Treatment – Co-trimoxazole or Pentamidine.

Viruses and Pneumonia in the normal host • Adults or Children • Influenza A and B, RSV, Adenovirus Para Influenza Pneumonia in the immuno-compromised • Measles, HSV, CMV, HHV-6, Influenza viruses • Can cause a primary viral pneumonia. Cause partial paralysis of “mucociliary escalator” increased risk of secondary bacterial LRTI. 58 S. aureus pneumonia is a known

CAP – So How Best to Win the War? § Early antibiotic administration within 4 -6 hours § Empiric antibiotic Rx. as per guidelines (IDSA / ATS) § PORT – PSI scoring and Classification of cases § Early hospitalization in Class IV and V § Change Abx. as per pathogen & sensitivity pattern § Decrease smoking cessation - advice / counseling 59
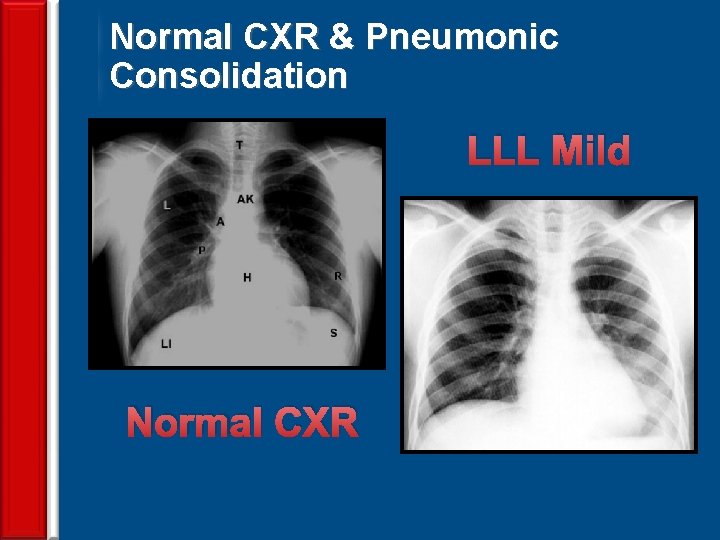
Normal CXR & Pneumonic Consolidation LLL Mild Normal CXR 60
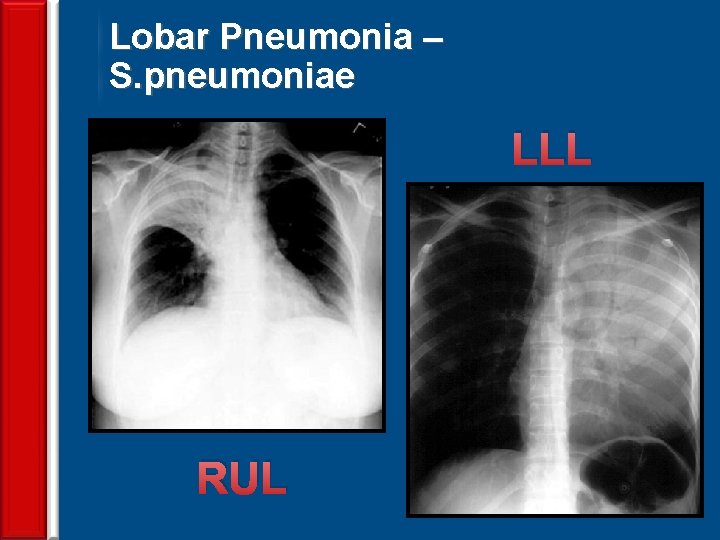
Lobar Pneumonia – S. pneumoniae LLL 61 RUL
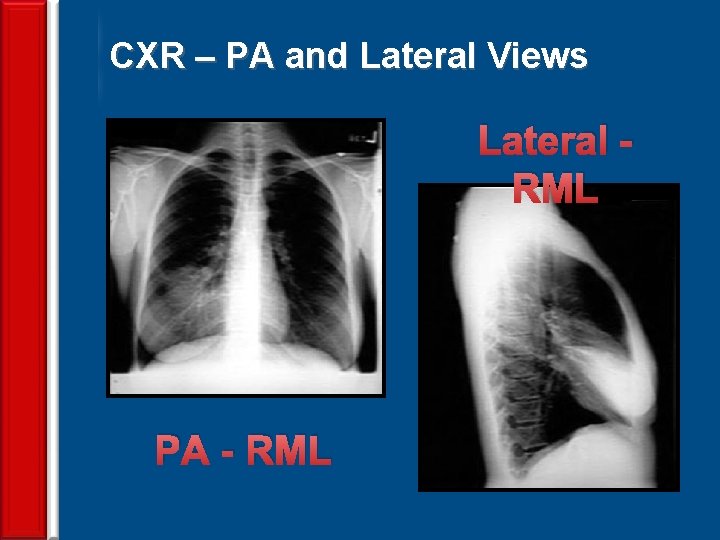
CXR – PA and Lateral Views Lateral RML PA - RML 62
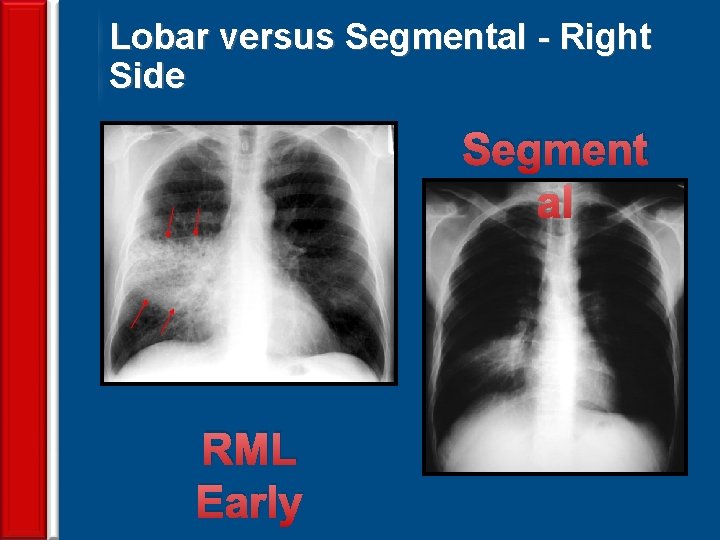
Lobar versus Segmental - Right Side Segment al 63 RML Early
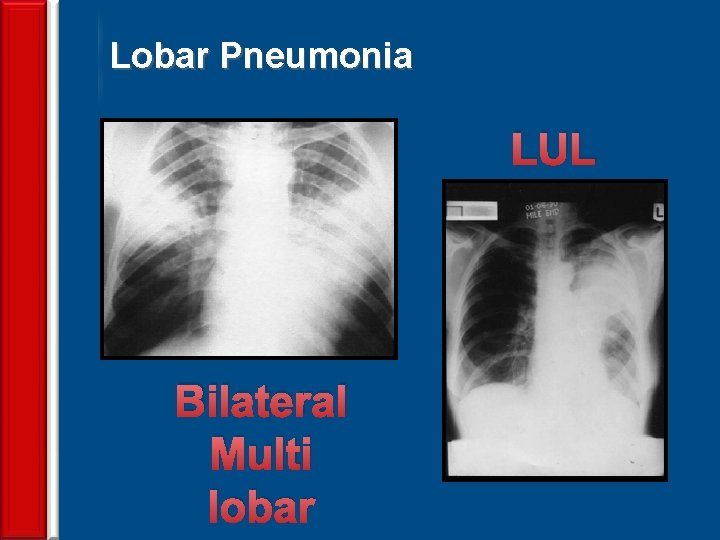
Lobar Pneumonia LUL 64 Bilateral Multi lobar
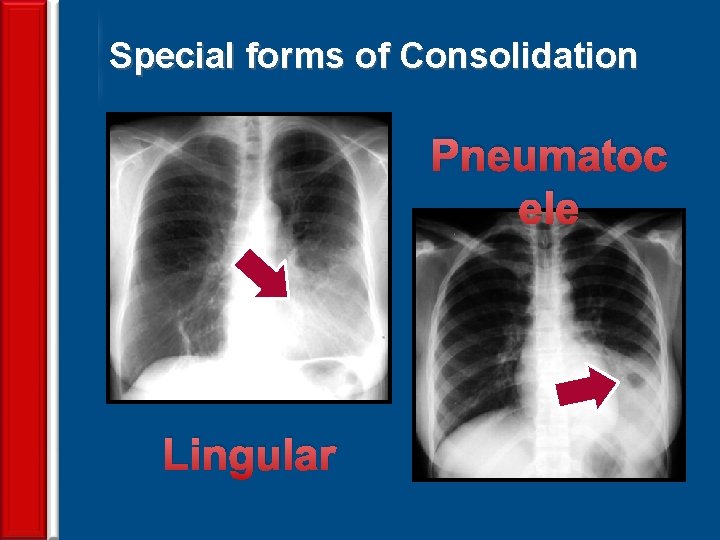
Special forms of Consolidation Pneumatoc ele Lingular 65
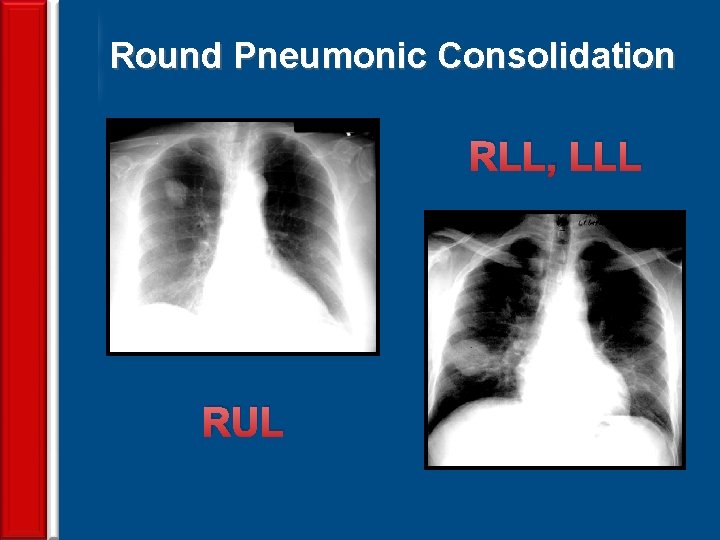
Round Pneumonic Consolidation RLL, LLL RUL 66
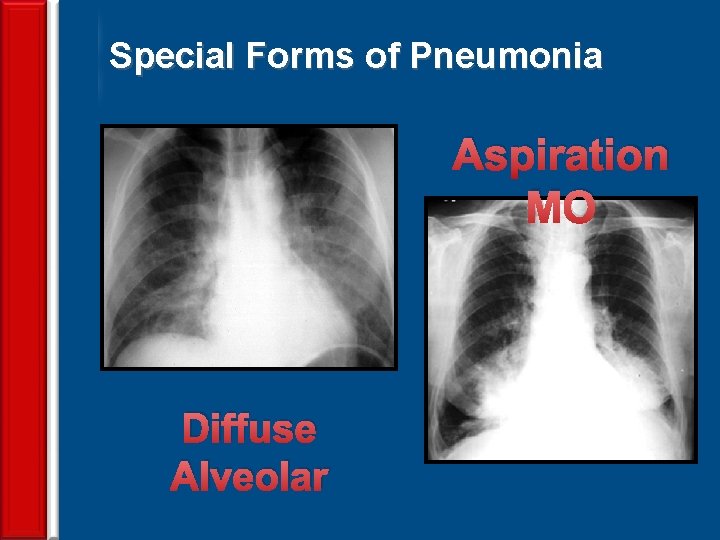
Special Forms of Pneumonia Aspiration MO Diffuse Alveolar 67
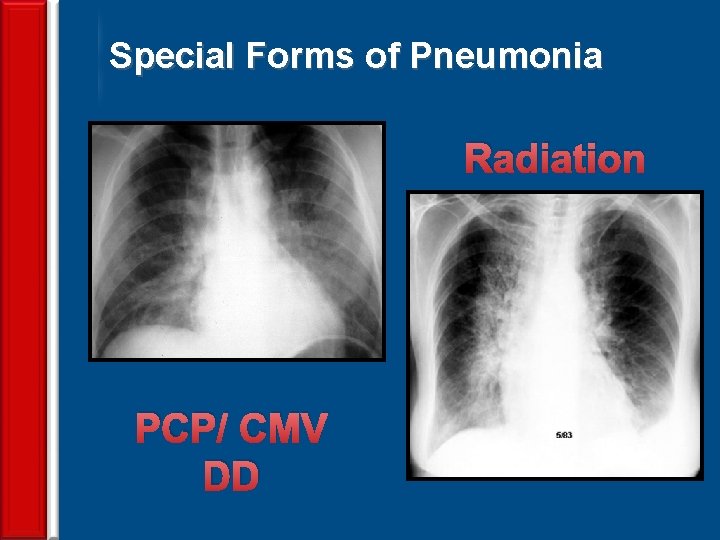
Special Forms of Pneumonia Radiation PCP/ CMV DD 68
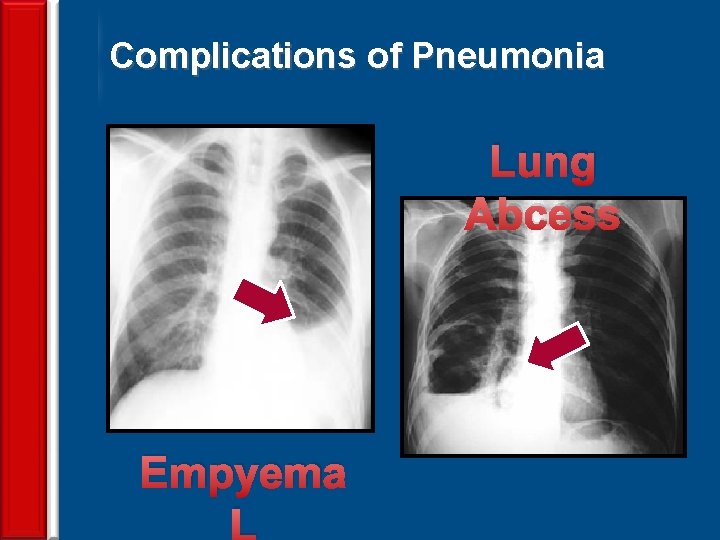
Complications of Pneumonia Lung Abcess 69 Empyema L
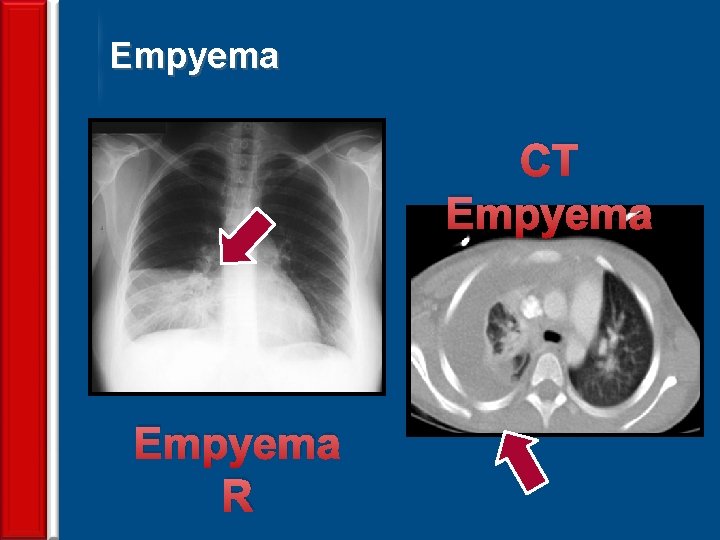
Empyema CT Empyema 70 Empyema R
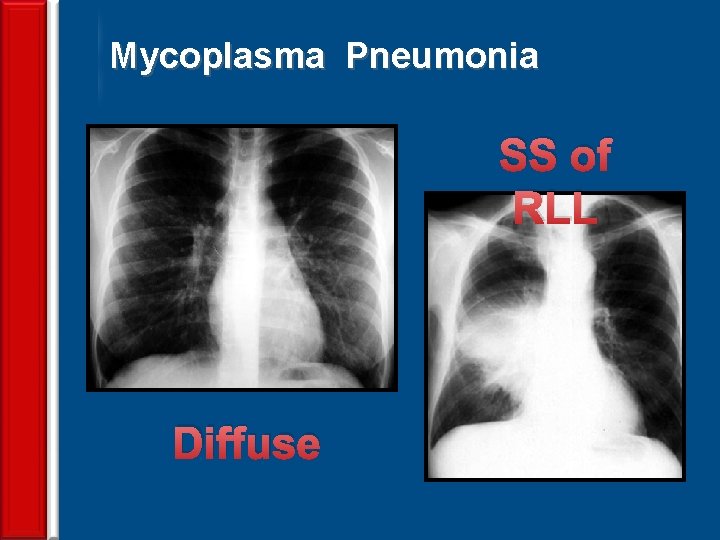
Mycoplasma Pneumonia SS of RLL Diffuse 71
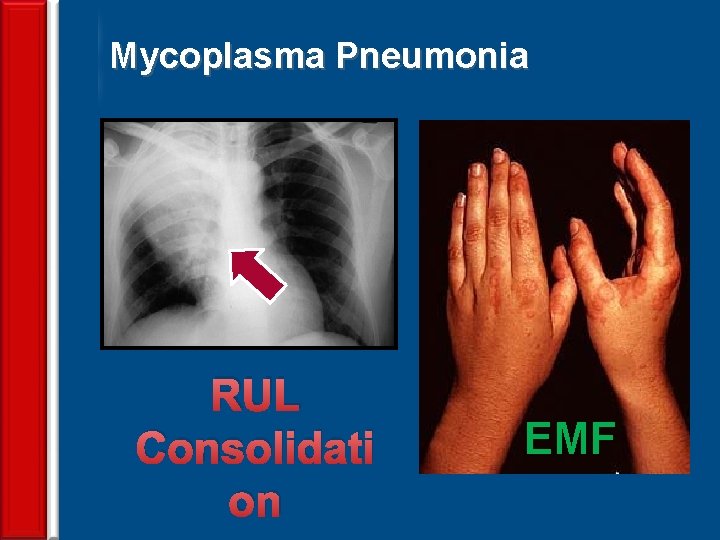
Mycoplasma Pneumonia 72 RUL Consolidati on EMF
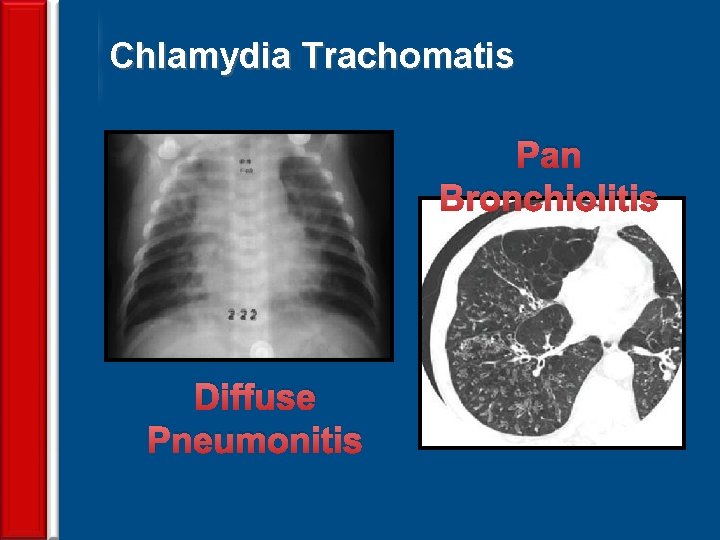
Chlamydia Trachomatis Pan Bronchiolitis Diffuse Pneumonitis 73
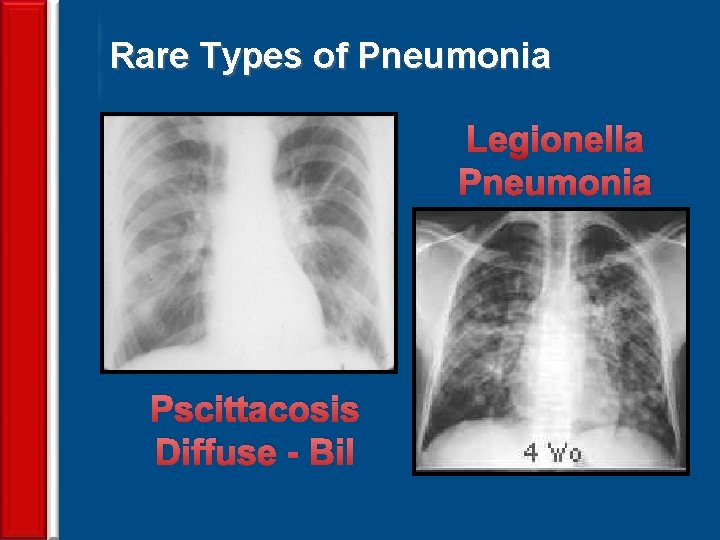
Rare Types of Pneumonia Legionella Pneumonia Pscittacosis Diffuse - Bil 74

��������� �������� shrothram shruthae naiva na ������ kundalaena ������ dhaanaena paanir na thu kankanaena ����� � vibhaathi kaayah karunaa ������� BHARTHRU HARI paraanaam paropakaaraena na chandanaena

Hearing science glorifies the ears, nay diamond ear-rings Giving to the needy enriches the hand, nay golden bangles To be kind shrothram and sympathetic and helping shruthae naiva na in all possible ways kundalaena Enriches the beauty ofpaanir our body, nay perfume or dhaanaena na thu sandal paste kankanaena vibhaathi kaayah karunaa paraanaam paropakaaraena na chandanaena Visit our website: www. drsarma. in our blog: http: //drsarma. blogspot. com
- Slides: 76