Candidiasis A primary or secondary mycotic infection caused




- Slides: 28

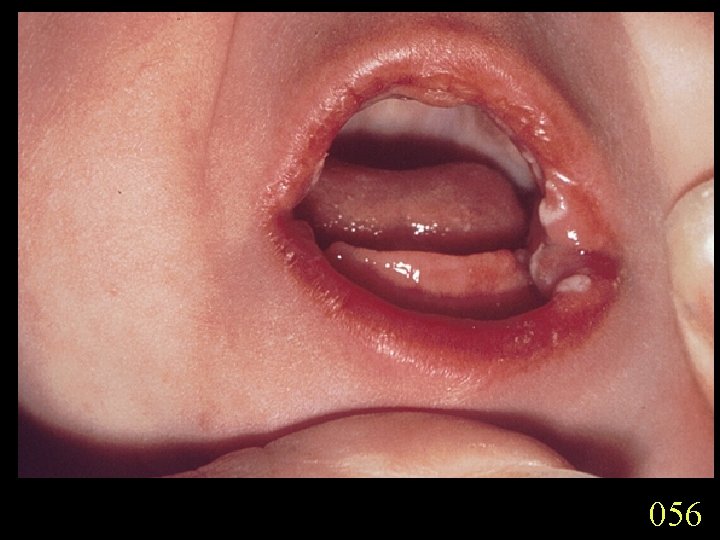
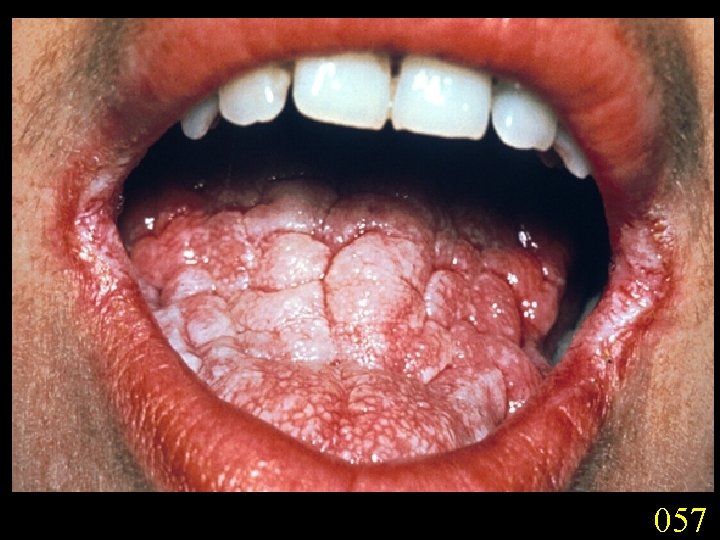
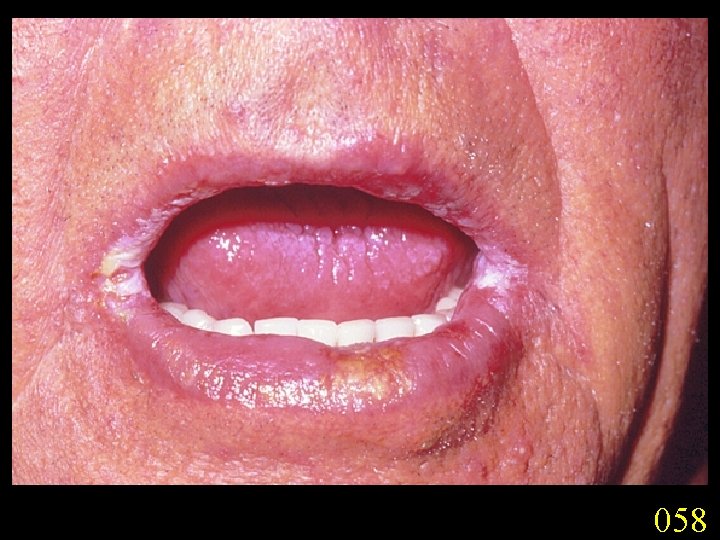
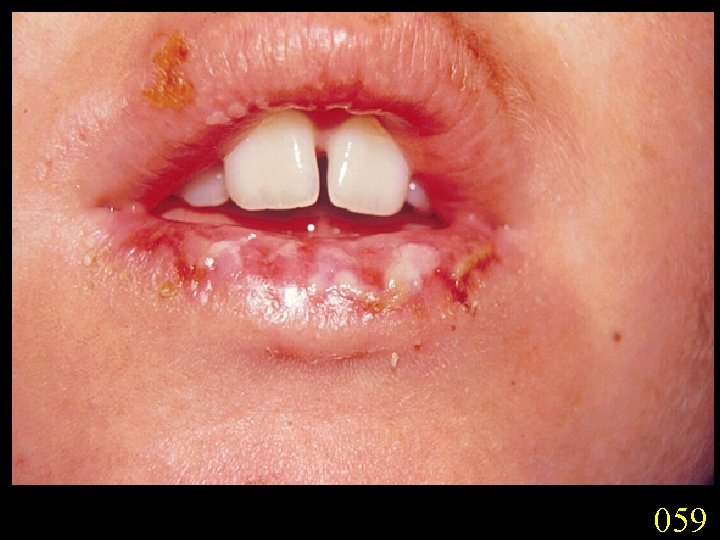
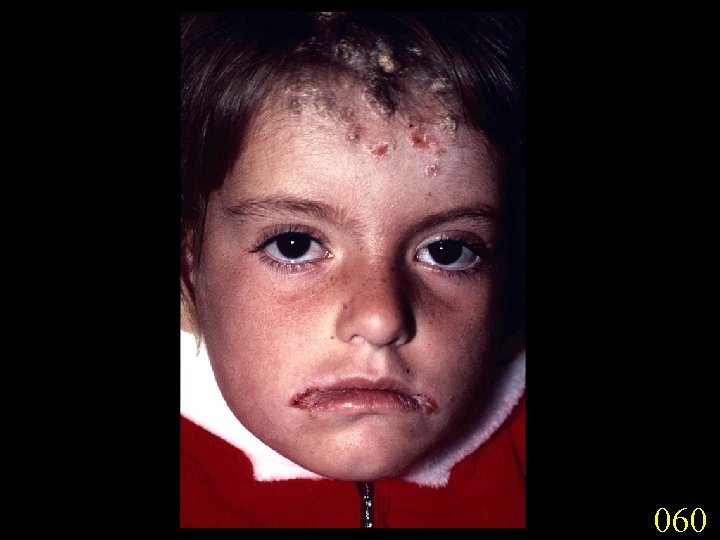
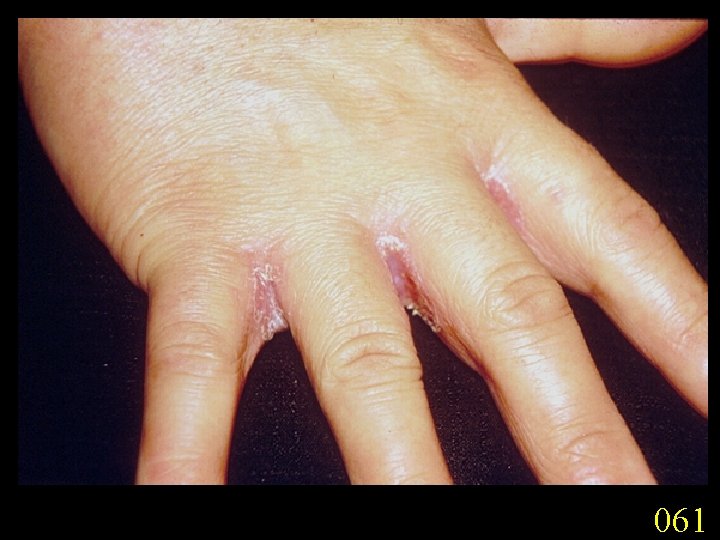
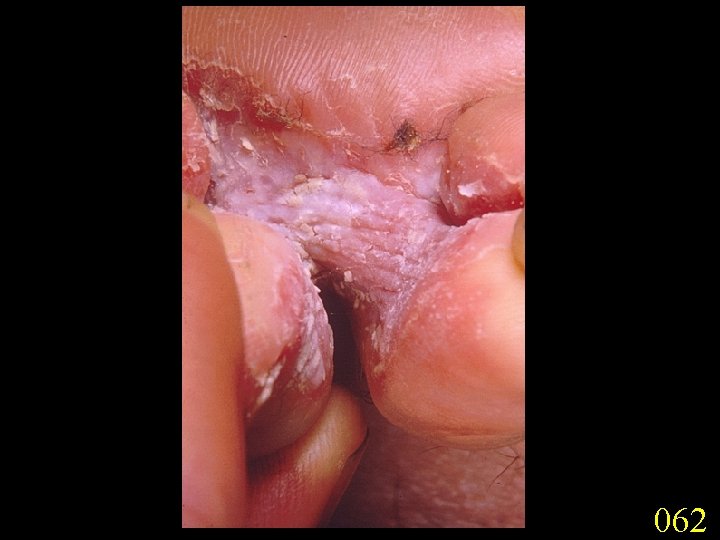
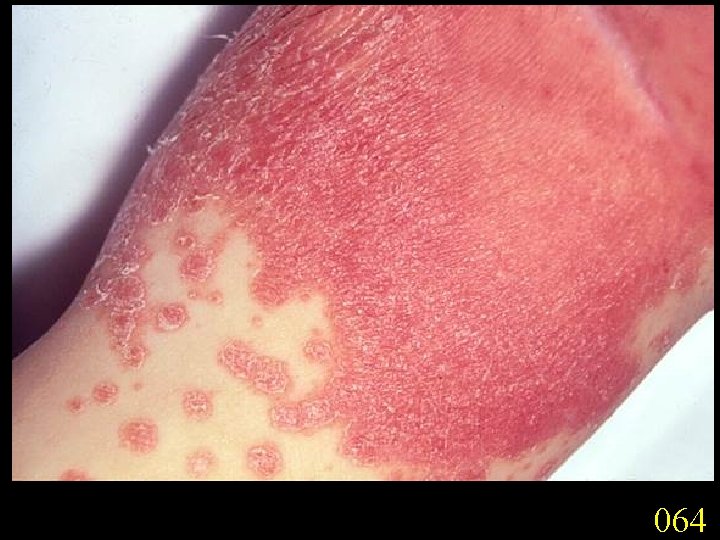
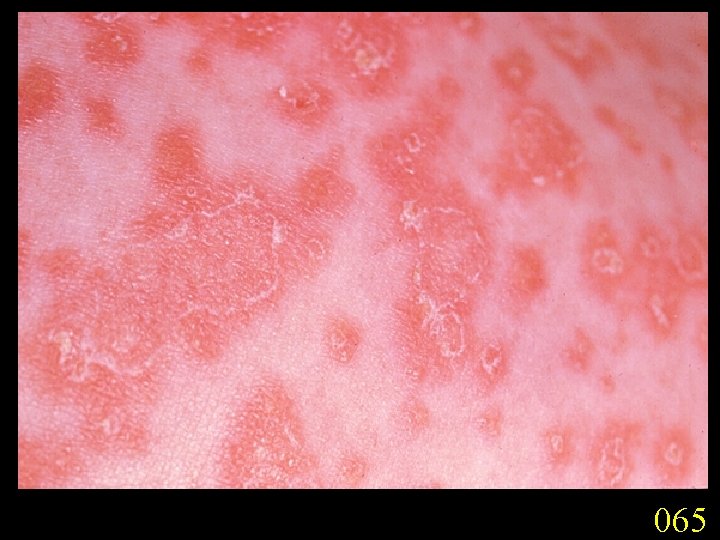
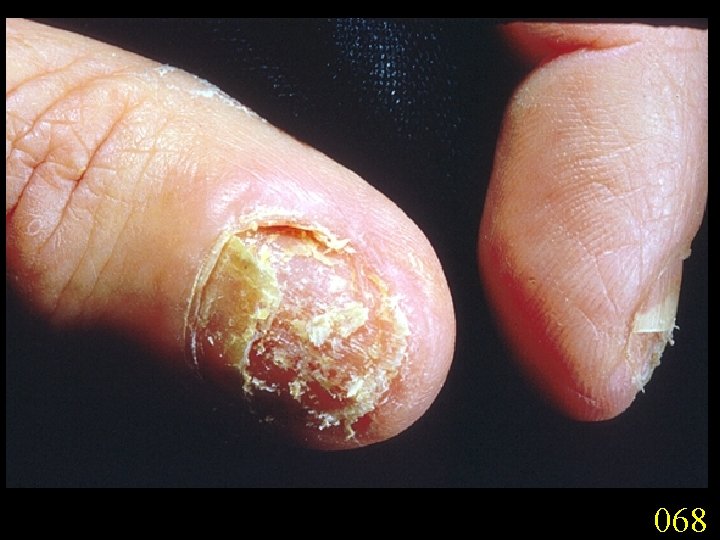
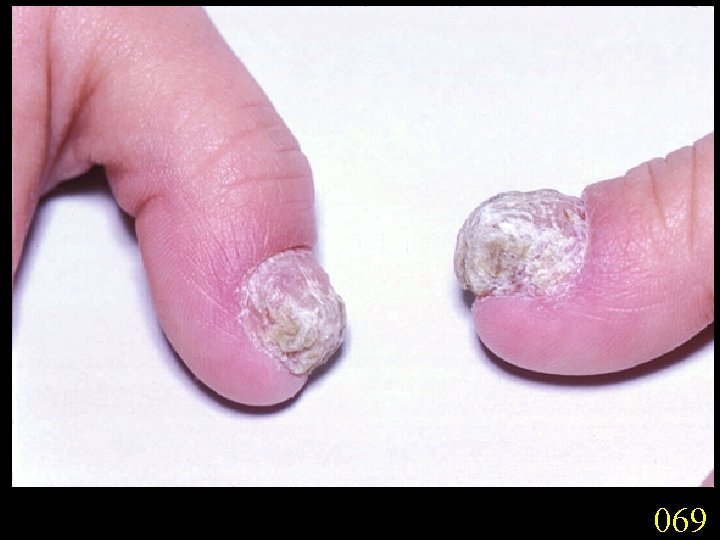
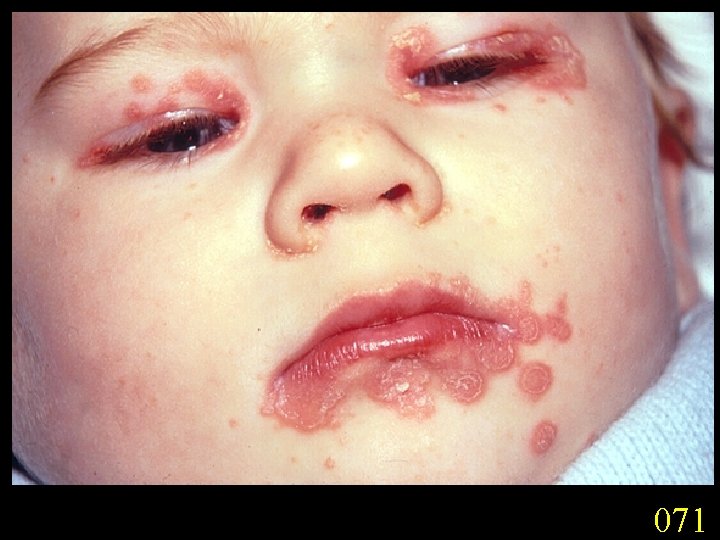
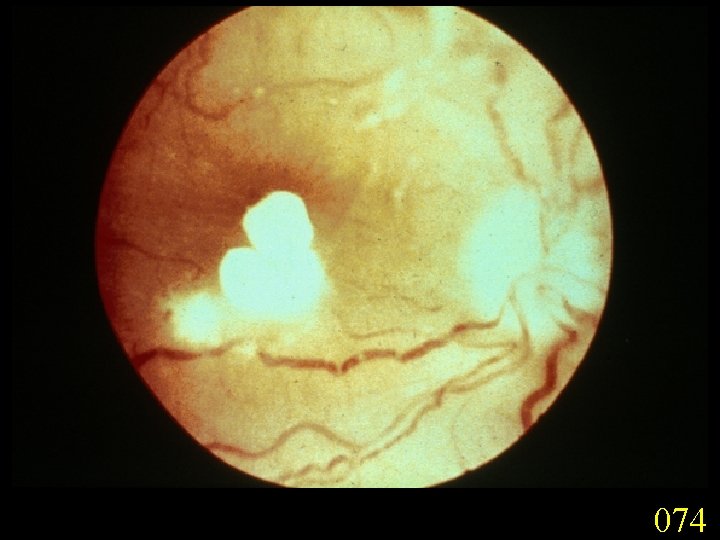
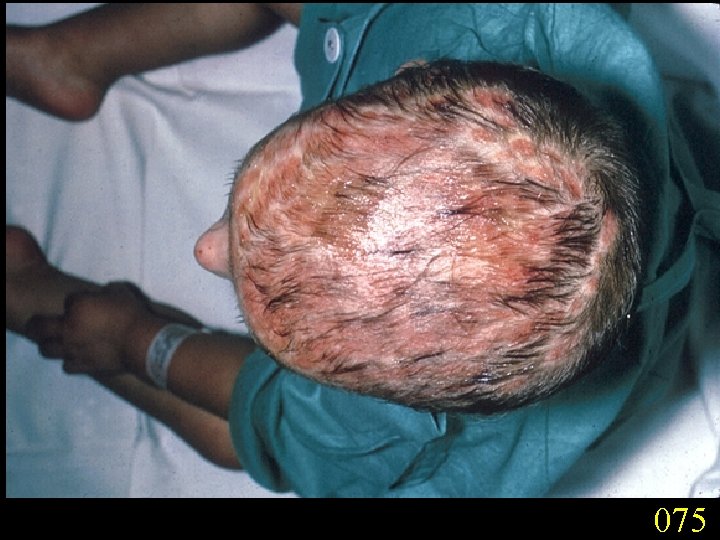
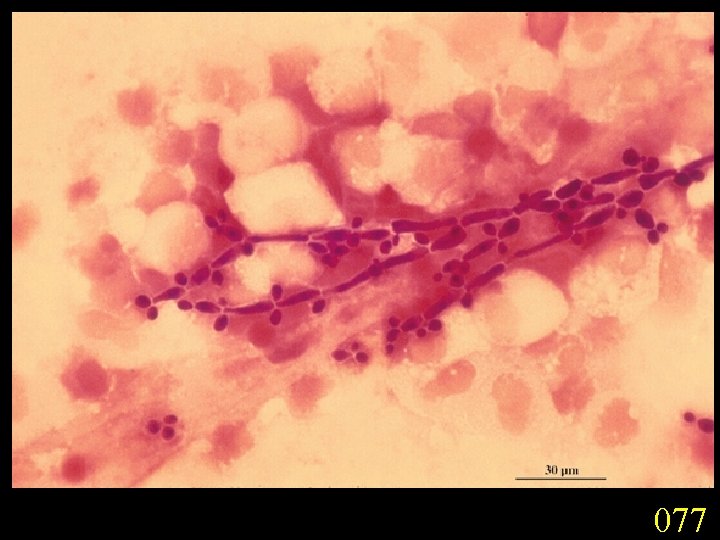
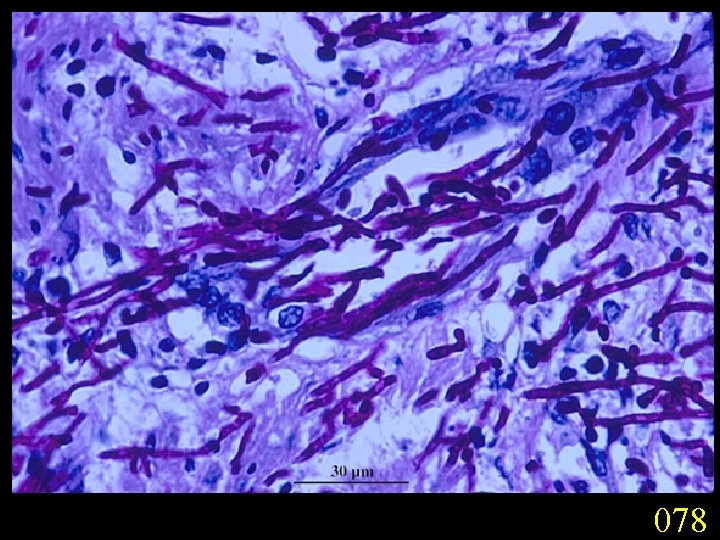
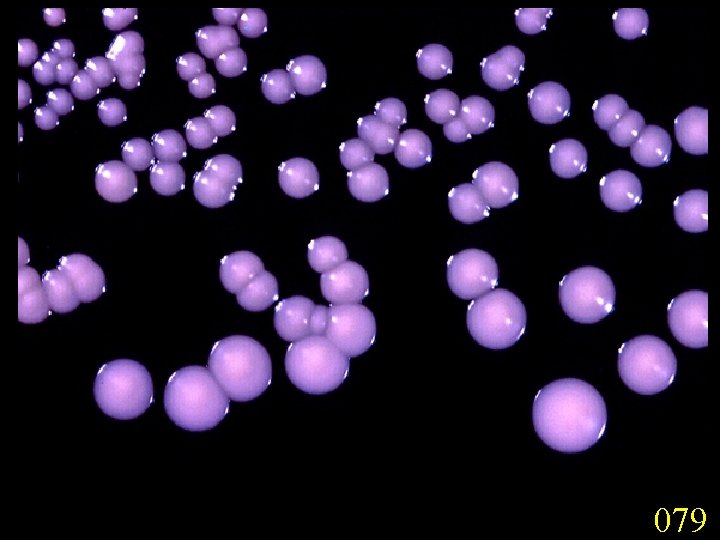
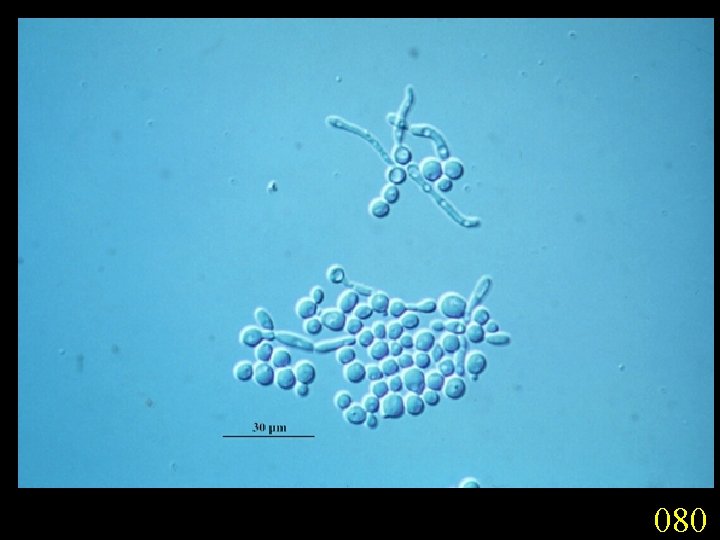
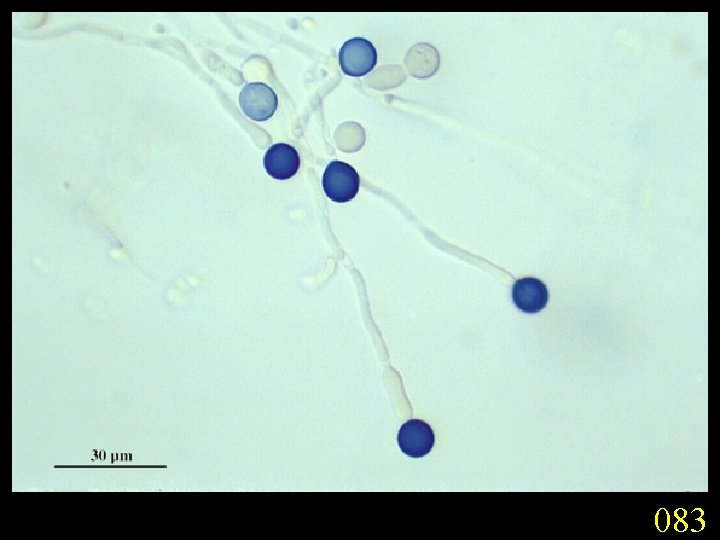
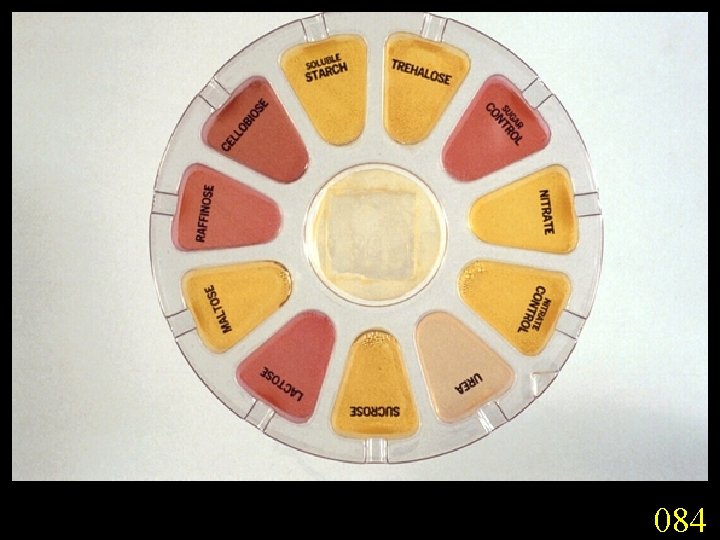
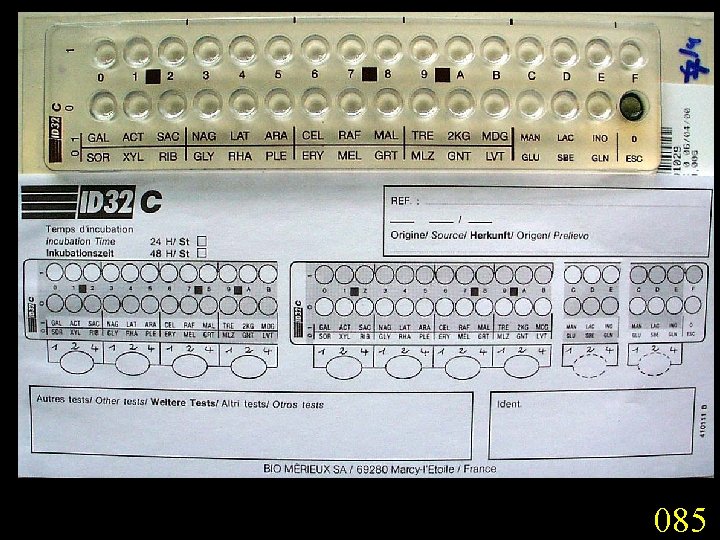
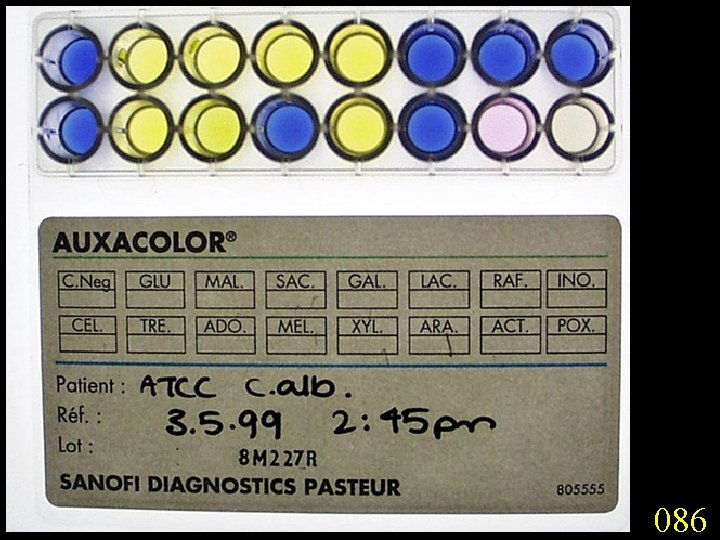
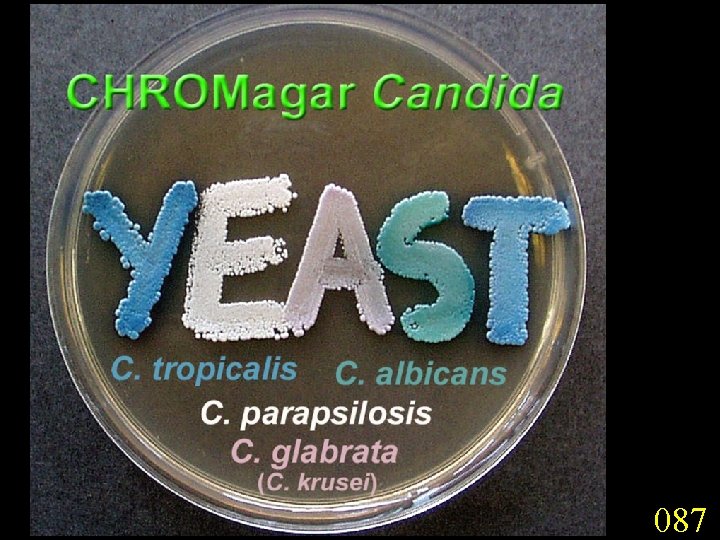
Candidiasis A primary or secondary mycotic infection caused by members of the genus Candida. The clinical manifestations may be acute, subacute or chronic to episodic. Involvement may be localized to the mouth, throat, skin, scalp, vagina, fingers, nails, bronchi, lungs, or the gastrointestinal tract, or become systemic as in septicaemia, endocarditis and meningitis. Distribution: World-wide. Aetiological Agents: Candida albicans, C. glabrata, C. tropicalis, C. krusei. C. parapsilosis, C. guilliermondii and C. pseudotropicalis. All are ubiquitous and occur naturally on humans.

056

057

058

059

060

061

062

064

065

068

069

071

074

075

077

078

079

080

083

084

085

086

087

088

090

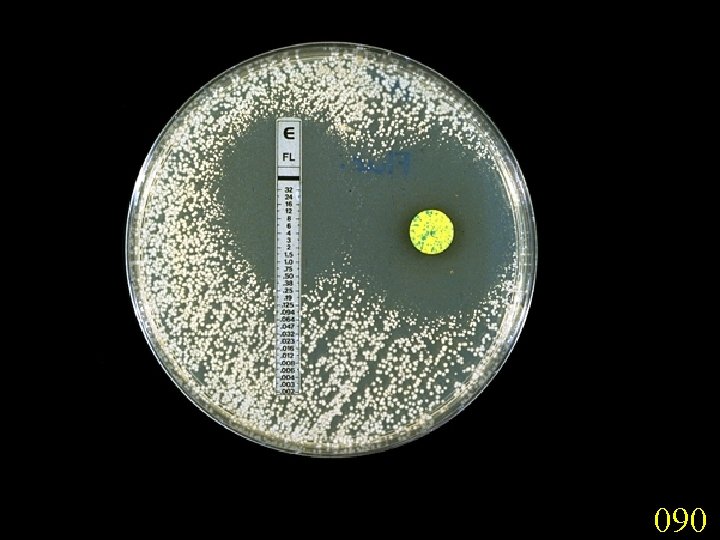
Treatment The treatments used to manage Candida infections vary substantially and are based on • anatomic location of the infection, • patients' underlying disease and immune status, • patients' risk factors for infection, • specific of Candida responsible for infection, • and in some cases, the susceptibility of the Candida species to specific antifungal drugs. • Fluconazole is the first-line agent in nonneutropenic patients with candidemia or suspected invasive candidiasis. • Cutaneous candidiasis infections may be treated with any number of topical antifungal agents (eg, clotrimazole, econazole, miconazole, ketoconazole, nystatin). • In cases of extensive cutaneous infections, infections in immunocompromised patients, folliculitis, or onychomycosis, systemic antifungal therapy is recommended. • Oropharyngeal candidiasis OPC can be treated with either topical antifungal agents (eg, nystatin, clotrimazole, amphotericin B oral suspension) or systemic oral azoles (fluconazole, itraconazole, or posaconazole). • Vulvovaginal candidiasis (VVC) can be managed with either topical antifungal agents or a single dose of oral fluconazole.

• Infections in HIV-positive patients tend to respond more slowly and, in approximately 60% of patients, recur within 6 months of the initial episode. • Approximately 3%-5% of patients with advanced HIV infection (CD 4 cell counts < 50/µL) may develop refractory OPC. • In these situations, in addition to attempting correction of the immune dysfunction, higher doses of fluconazole (up to 800 mg/d) or itraconazole (up to 600 mg/d) can be attempted. • Posaconazole suspension at 400 mg orally twice per day has also yielded excellent results in such patients. • Additionally, caspofungin 50 mg/d IV and anidulafungin 100 mg/d IV have also yielded excellent efficacy in such patents. • Amphotericin B is rarely necessary to treat such cases, but, when used, low doses of amphotericin B can be used (0. 3 -0. 7 mg/kg) and have been shown to be effective.