Campylobacter C fetus veneralis C fetus C jejuni

Campylobacter C. fetus veneralis C. fetus C. jejuni / coli 1 קמפילובקטר




: גורמי אלימות • Motility and chemotaxis – Chemoattraction towards bile and mucin allows colonization of the intestine and gall bladder • adherence to epithelial cells – Adherence with proteins, flagella and lipopolysaccharide. – Campylobacter are adherent to cell membrane and are internalized into cytoplasmic vacuoles. – flagellin and adhesion both are required for irreversible binding of bacteria to cells 6

: גורמי אלימות • Intracellular : – C. fetus is capable of adhering, entering, and surviving within the nonphagocytic epithelial cells • Proteins and enzymes – cytolethal distending toxin (CDT) causes cellular distention and eventually death of the cell lines – hemolysin. – Catalase is required for Campylobacter hydrogen peroxide resistance as well as persistence in macrophages 7

Cell Wall • typical of gram-negative cells. • three layers, – an outer lipoprotein layer, – a middle lipopolysaccharide layer – inner mucopeptide layer. • The LPS consisted of three distinct regions – lipid A anchored in the outer membrane and is the endotoxic part of the LPS molecule. – the core, which is attached to the lipid – the O antigen attached to the outer core. • The LPS molecules of Campylobacter are involved in adherence and play a role in antigenic variations, as Campylobacter has the ability to shift the LPS antigenic composition. • Surprisingly N-acetyl neuraminic acid (sialic acid) is present in the core oligosaccharide, not frequently found in prokaryotes. These sialic acid residues appeared like gangliosides in structure, when attached to –D galactosidase. • This molecular mimicry is involved in the neuropathological autoimmune diseases like Guillains Barre' Syndrome and Reiter 8 syndrome.


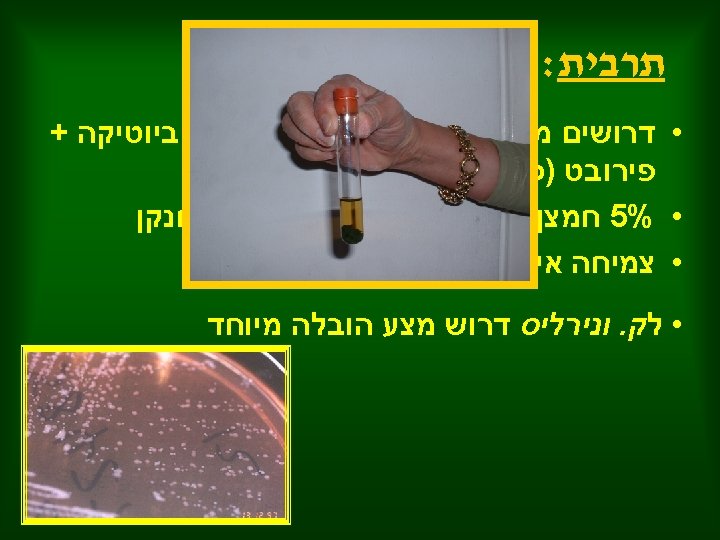
Survival in the Environment • Survival of C. jejuni outside the gut is poor, and replication does not occur readily. • C. jejuni grows best at 37°C to 42°C, the approximate body temperature of the chicken (41°C to 42°C). • C. jejuni grows best in a low oxygen or microaerophilic environment, such as an atmosphere of 5% O 2, 10% CO 2, and 85% N 2. • The organism is sensitive to freezing, drying, acidic conditions (p. H < 5. 0), and salinity. 10





Disease Prevalence • In the United States, an estimated 2. 1 to 2. 4 million cases of human campylobacteriosis (illnesses ranging from loose stools to dysentery) occur each year. • Commonly reported symptoms of patients with laboratory-confirmed infections (a small subset of all cases) include diarrhea, fever, and abdominal cramping. • In one study, approximately half of the patients with laboratory-confirmed campylobacteriosis reported a history of bloody diarrhea. • Less frequently, C. jejuni infections produce bacteremia, septic arthritis, and other extraintestinal symptoms. • Centers for Disease Control and Prevention/U. S. Department of Agriculture/Food and Drug Administration Collaborating Sites Foodborne Disease Active Surveillance Network, 1996 16

Infections Campylobacter jejuni Outbreak of Associated with Drinking Unpasteurized Milk Procured Through a Cow-Leasing Program ― Wisconsin, 2001 During November and December 2001, seventy-five persons from enteritis. This Campylobacter jejuni Northwestern Wisconsin became ill with outbreak was associated with drinking unpasteurized milk obtained through a cow-leasing program that was used to circumvent regulations prohibiting the sale of unpasteurized milk in Wisconsin. Consumers paid an initial fee to lease part of a cow. Farm operators then milked the cows and stored the milk from all leased cows together in a bulk tank. Customers either picked up milk at the farm or farm operators had it delivered. To ensure that unpasteurized milk will not be distributed to the public in Wisconsin, state officials are enforcing existing regulations and prohibiting cow-leasing. visit this CDC website Campylobacter systems. For more information on 17

Telegraph UK More than 160 mountain bikers made sick by sheep droppings 02 Dec 2008 Public health inspectors were called in after the cyclists fell ill with food poisoning after an event in the Welsh countryside. The cyclists tested positive for the bacterium campylobacter – usually caused by uncooked meat and poultry. But following an investigation by health experts, the muddy mountain cycle course was found to be heavily contaminated with sheep droppings. The cyclists are believed to have been affected by eating meals and snacks during the event – without washing their hands first. "At that point we launched an internet based questionnaire to investigate the outbreak ". More than 660 mountain bikers from all over Britain took part in the Builth Wells Mountain Biking Marathon in Powys in July this year. A total of 355 responses were received with 161 cyclists reporting symptoms such as diarrhoea and vomiting. The report, by the NPHSW, concluded the outbreak was caused by campylobacter spread to the cyclists by mud which was contaminated with sheep faeces. Heavy overnight rain is likely to have contributed to the outbreak by increasing the amount of liquid mud on the course. The report recommended cyclists to eat out of protective wrappers at 18 future events.

Sequelae to Infection • Guillain-Barré syndrome (GBS), a demyelating disorder resulting in acute neuromuscular paralysis, is a serious sequela of Campylobacter infection. An estimated one case of GBS occurs for every 1, 000 cases of campylobacteriosis. • Up to 40% of patients with the syndrome have evidence of recent Campylobacter infection. • Approximately 20% of patients with GBS are left with some disability, and approximately 5% die despite advances in respiratory care. Allos BM. Association between Campylobacter infection and Guillain. Barré syndrome. J Infect Dis 1997; 176: S 125 -8. 19

GBS Pathogenesis • precise mechanism of GBS is unclear. • certainly has an immunological basis; • most likely an autoimmunity triggered by an exogenous antigen. • It has been linked epidemiologically to Campylobacter jejuni as well as other infectious agents. • The preceding infection creates an immunological response to proteins epitopically similar to myelin. 20

Sequelae to Infection Reiter syndrome • Campylobacteriosis is also associated with Reiter syndrome, a reactive arthropathy. In approximately 1% of patients with campylobacteriosis, the sterile postinfection process occurs 7 to 10 days after onset of diarrhea. • Multiple joints can be affected, particularly the knee joint. Pain and incapacitation can last for months or become chronic. • Both GBS and Reiter syndrome are thought to be autoimmune responses stimulated by infection. • The pathogenesis of GBS and Reiter syndrome is not completely understood. Peterson MC. Rheumatic manifestations of Campylobacter jejuni and C. 21 fetus infections in adults. Scand J Rheumatol 1994; 23: 167 -70.

A survey of Campylobacter in animals. Manser PA, Dalziel RW. , Hyg (Lond). 1985 Aug; 95(1): 15 -21 • A survey of Campylobacter species in the faeces or rectal contents of domestic animals was carried out using direct and enrichment culture methods. • Campylobacters were isolated from 259 (31%) of 846 faecal specimens. • The highest isolation rate was found in pigs (66%); cattle (24%) and sheep (22%). In pigs all the isolates were C. coli, in sheep and cattle about 75% were C. jejuni. • Only five isolations of C. fetus subsp. fetus were made, all from cattle. More pigs with diarrhoea had C. coli in their faeces than healthy pigs (77% vs 47%), but such a clear difference in isolation rate between sick and healthy animals was not seen in cattle or sheep. • The results show that cattle, sheep and pigs constitute a large potential source of campylobacter infection for man. 22


24

Antimicrobial Resistance • The increasing rate of human infections caused by antimicrobial-resistant strains of C. jejuni makes clinical management of cases of campylobacter more difficult. • Antimicrobial resistance can prolong illness and compromise treatment of patients with bacteremia. • The rate of antimicrobial-resistant enteric infections is highest in the developing world, where the use of antimicrobial drugs in humans and animals is relatively unrestricted. • Piddock LJV. Quinolone resistance and Campylobacter spp. Antimicrob Agents Chemother 1995; 36: 891 -8. • Jacobs-Reitsma WF, Kan CA, Bolder NM. The induction of quinolone resistance in Campylobacteria in broilers by quinolone treatment. In: Campylobacters, helicobacters, and related organisms. Newell DG, Ketley JM, Feldman RA, editors. 25 New York: Plenum Press; 1996. p. 307 -11.

Antimicrobial Resistance • Experimental evidence demonstrates that fluoroquinolonesusceptible C. jejuni readily become drug-resistant in chickens when these drugs are administered. • After flouroquinolone use in poultry was approved in Europe, resistant C. jejuni strains emerged rapidly in humans during the early 1990 s. • Similarly, within 2 years of the 1995 approval of fluoroquinolone use for poultry in the United States, the number of domestically acquired human cases of ciprofloxacin-resistant campylobacteriosis doubled in Minnesota. Smith KE, Besser JM, Leano F, Bender J, Wicklund J, Johnson B, et al. Fluoroquinoloneresistant Campylobacter isolated from humans and poultry in Minnesota [abstract]. 26 Program of the 1 st International Conference on Emerging Infectious Diseases; Atlanta, Georgia; 1998 Mar 7 -10. Atlanta: Centers for Disease Control and Prevention; 1998.
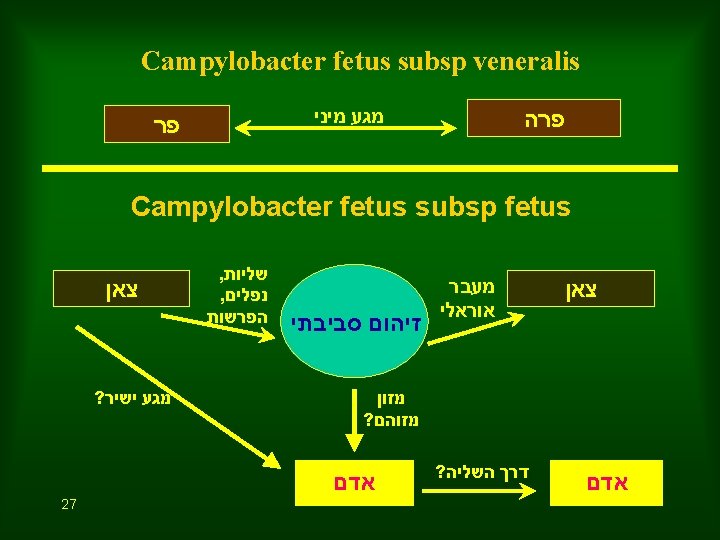





Campylobacter fetus in man Campylobacter fetus subsp veneralis • – Few cases documented in man – Debilitating factors (pregnancy, alcoholism, neoplasia, cardiac dis. • Campylobacter fetus subsp fetus – Septicemia – 17% - 43% die – Abortion, premature birth, full term birth which up to 50% may die of meningoencephalitis 32





Control of Campylobacter Infection On the Farm • Control of Campylobacter contamination on the farm may reduce contamination of carcasses, poultry, and red meat products at the retail level. • Epidemiologic studies indicate that strict hygiene reduces intestinal carriage in food-producing animals. • In field studies, poultry flocks that drank chlorinated water had lower intestinal colonization rates than poultry that drank unchlorinated water. • Experimentally, treatment of chicks with commensal bacteria and immunization of older birds reduced C. jejuni colonization. • Because intestinal colonization with campylobacters readily occurs in poultry flocks, even strict measures may not eliminate intestinal carriage by food-producing animals. Stern NJ. Mucosal competitive exclusion to diminish colonization of chickens by Campylobacter jejuni. Poult Sci 1994; 73: 402 -7. 37 Widders PR, Perry R, Muir WI, Husband AJ, Long KA. Immunization of chickens to reduce intestinal colonization with Campylobacter jejuni. Br Poult Sci 1996; 37: 765 -8.

Important Tip! Protect yourself against getting Campylobacter from animals. Simply wash your hands with running water and soap after any contact with animals and animal feces (stool). 38
- Slides: 37