Californias Coordinated Care Initiative July 2014 Roadmap About

California’s Coordinated Care Initiative July 2014
Roadmap • About the Coordinated Care Initiative • Cal Medi. Connect • Medi-Cal Managed Long Term Services and Supports • Timeline and Enrollment • Participating in Cal Medi. Connect • Additional Resources 2
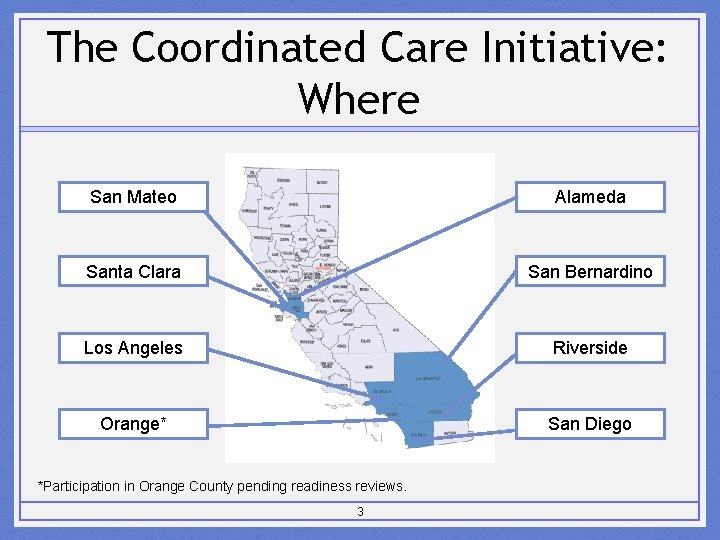
The Coordinated Care Initiative: Where San Mateo Alameda Santa Clara San Bernardino Los Angeles Riverside Orange* San Diego *Participation in Orange County pending readiness reviews. 3

Medicare and Medi-Cal Today Medicare Medi-Cal Who: 65+, under 65 with certain disabilities Who: low-income Californians • • Doctors Long-term services and supports • MSSP: Multipurpose Senior Services Program • IHSS: In-Home Supportive Services • CBAS: Community-Based Adult Services • Nursing facilities • Hospitals • Prescription drugs 4 • Durable medical equipment • Medicare cost sharing

The Coordinated Care Initiative: Two Parts Medi-Cal Medi. Connect Managed Long-Term Services and Supports (MLTSS) Who: many full dual eligible beneficiaries Who: Medi-Cal only beneficiaries, full dual eligibles who opt out of Cal Medi. Connect, other identified groups eligible for Medi-Cal • Optional • Combines Medicare and Medi-Cal benefits into one managed care health plan • Additional services, including care coordination 5 • Mandatory • Beneficiaries will now receive Medi-Cal benefits through a managed care health plan, including LTSS and Medicare wrap-around.

Cal Medi. Connect • Who: Medi-Medi beneficiaries • Original Medicare and Medi. Cal services • One number for all your health care needs • Vision benefit: one routine eye exam annually and a $100 co-pay for eye glasses/contacts every two years • Optional • Transportation benefit: 30 1 way trips per year in addition to the existing transportation benefit • Care Coordination 6

Cal Medi. Connect Care Coordination • Cal Medi. Connect plans will give providers information and resources to support care coordination. • Health Risk Assessments (HRAs) • Primary, acute, LTSS, behavioral health and functional needs • Interdisciplinary Care Teams • Beneficiary, plan care coordinator, key providers • Individualized Care Plans • Care teams will develop and implement ICPs • Plan Care Coordinators • Facilitates communication between plans, providers, beneficiary 7

Care Coordination: Example Patient X recently had a stroke and is back living at home. Under Cal Medi. Connect, a plan care coordinator will ensure the patient has: • Transportation to appointments • Coverage for prescriptions • Meals on Wheels • Other support for activities of daily living Before Cal Medi. Connect, the patient would have to navigate Medicare, Medi. Cal and county agencies to get needed social services – often relying on their doctor’s office staff for help. 8

If you have Medicare and Medi-Cal Option 1: Choose Cal Medi. Connect You can combine your Medicare A, B & D with your Medi-Cal benefits into a Cal Medi. Connect plan Select one of the participating Cal Medi. Connect plans in your county 9

Cal Medi. Connect Plan Options Los Angeles Alameda • Care 1 st, Care. More, Health Net, LA Care and Molina Health • Alameda Alliance and Anthem Blue Cross Orange* Santa Clara • Cal. Optima • Anthem Blue Cross and Santa Clara Family Health Plan San Diego San Bernardino • Care 1 st, Community Health Group, Health Net and Molina Health • Inland Empire Health Plan and Molina Health Riverside San Mateo • Inland Empire Health Plan and Molina Health • Health Plan of San Mateo *Participation in Orange County pending readiness reviews. 10

People not eligible for Cal Medi. Connect You can’t join Cal Medi. Connect if you: • Are younger than 21. • Receive developmental disability waiver services from a Regional Center. • Do not meet your Medi-Cal share of cost, if you have one. • Have End-Stage Renal Disease (ESRD), except in San Mateo County. • Have other health coverage, such as retirement, veterans or private coverage. • Live in a veterans home. • Receive services through one of the following waiver programs; Nursing Facility/Acute Hospital, HIV/AIDS, Assisted Living, or In Home Operations (you must disenroll from these programs to enroll in Cal Medi. Connect, you will not be passively enrolled). • Are enrolled in PACE (you must disenroll to be eligible for the Cal Medi. Connect; will not be passively enrolled). • Live in some rural zip codes in Los Angeles, Riverside and San Bernardino Counties. 11

Medi-Cal Managed Long-Term Services and Supports • Who: Medi-Cal only beneficiaries, full dual eligibles who opt out of Cal Medi. Connect, other identified groups eligible for Medi-Cal • Mandatory • Same Medi-Cal services beneficiaries currently receive • Hearing aids • Bathrooms aids (grab bars, shower chairs) • Non-emergency medical transportation (wheelchair vans and litter vans) • Incontinence supplies • Medi-Cal long-term services and supports (MLTSS) will now be coordinated by a managed care plan • MSSP: Multipurpose Senior Services Program • IHSS: In-Home Supportive Services • CBAS: Community-Based Adult Services • Nursing facilities 12

If you have Medicare and Medi-Cal Option 2: Keep your Medicare as it is and join a Medi-Cal health plan • Enroll in only a Medi-Cal Plan Your Medicare including your Part D plan, will stay the same • You will continue to use the same Medicare providers • Your Medi-Cal benefits are now assigned to the Medi-Cal health plan Select one of the participating Medi-Cal plans in your county 13

If you have only Medi-Cal You must choose a Medi-Cal plan for your Medi-Cal benefits Enroll in a Medi-Cal Plan Select one of the participating Medi-Cal plans in your county 14

MLTSS Plan Options Los Angeles Alameda • Health Net (Molina), LA Care (Anthem, Care 1 st, Kaiser) • Alameda Alliance and Anthem Blue Cross Orange* Santa Clara • Cal. Optima • Anthem Blue Cross and Santa Clara Family Health Plan San Diego San Bernardino • Care Community Health Group, Health Net, Molina, and Kaiser 1 st, • Inland Empire Health Plan (Kaiser) and Molina (Health Net) San Mateo Riverside • Health Plan of San Mateo • Inland Empire Health Plan (Kaiser) and Molina (Health Net) *Participation in Orange County pending readiness reviews. 15

PACE Program of All-inclusive Care for the Elderly • Who: Medi-Medi beneficiaries and Medi-Cal beneficiaries • Option available to those who are determined eligible You may be eligible to enroll in a PACE program If you: • Are 55 or older • Live in your home or community setting safely • Need a high level of care for a disability or chronic condition • Live in a ZIP code served by a PACE health plan 16

PACE Plans Alameda Los Angeles • Center for Elders’ Independence and On Lok Lifeways • Altamed Senior Buena. Care and Brandman Centers for Senior Care Santa Clara Orange* • On Lok Lifeways • Cal. Optima PACE San Bernardino San Diego • Innov. Age PACE Riverside • St. Paul’s PACE • Innov. Age PACE 17

When to Expect Notices • Beneficiaries will receive notices 90, 60, and 30 days prior to your coverage date. • For most people their coverage date is the first day of their birth month. • Cal Medi. Connect official information from the state will only arrive in blue envelopes. 18

General Timeline • April 2014 Enrollment in San Mateo • May 2014 Enrollment in San Diego, Riverside, and San Bernardino begins • July 2014 Enrollment in Los Angeles begins* • January 2015 Enrollment in Alameda, Santa Clara, and Orange begins* *Enrollment in Orange County and select Los Angeles plans pending readiness reviews. 19
20

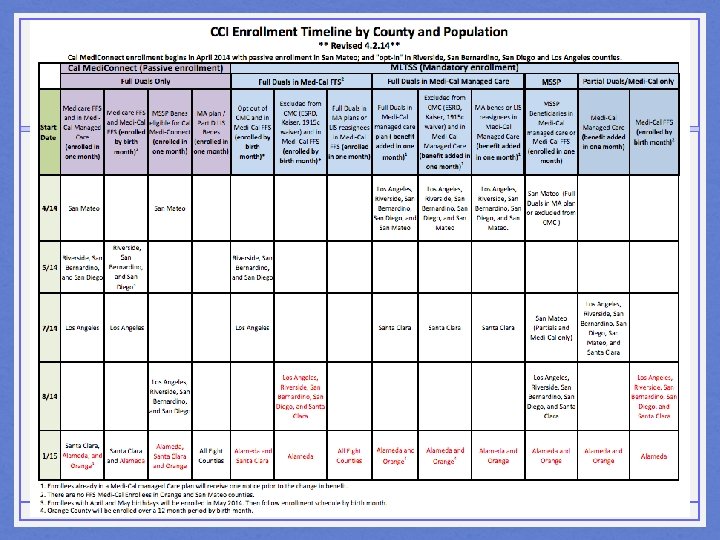
Timeline Specifics Individuals who receive passive enrollment notices: • Already in Managed Medi-Cal – enroll/benefit added in 1 month • Not in Managed Medi-Cal – enroll by birth month • In CCI-health plan DSNPs – enroll in one month in January 21

Timeline Specifics Individuals who are eligible for Cal Medi. Connect but WILL NOT receive passive enrollment notices: • Enrolled in non-CCI plan DSNP • Enrolled in Medicare Advantage • Enrolled in VA, waiver system, etc. These populations will be asked to selected a Managed Medi-Cal (MLTSS) plan. 22

Blue Envelope 23

Cal Medi. Connect Notices 90 Day Notice 60 Day Notice 24 30 Day Notice

MLTSS 90 Day Notice 60 Day Notice 25 30 Day Notice

Choice Form Section 3: Cal Medi. Connect Plan To select a Cal Medi. Connect plan, complete section 3 ONLY. Section 5: Medi-Cal Plan To “Opt-Out” of Cal Medi. Connect, fill out section 5 ONLY. Choose the Medi-Cal plan you are already in or select the Medi-Cal plan you want to join. Section 7: PACE Plans To select a PACE plan complete section 7 AND also complete section 3 OR 5 as back-up options. 26

Use the Choice Form to Choose the Plan you Want • If you have both Medicare and Medi-Cal and you do nothing: • You will be assigned to a Cal Medi. Connect plan that is the best match for you. • If you have only Medi-cal and you do nothing: • You will be assigned to a Medi-Cal plan that is the best match for you. • This way you will not lose your Medicare or Medi -Cal benefits or services. 27

Enrollment: Health Care Options Call Health Care Options to: • Enroll in a Cal Medi. Connect plan, or • Enroll in a Medi-Cal plan (and keep your Medicare as it is today), or • Enroll in a PACE plan 1 -844 -580 -7272 28

Enrollment • The use of independent agents/brokers will not be permitted and all MMP enrollment transactions must be processed by the State enrollment broker (Health Care Options). • If an individual is cross walked into a Cal Medi. Connect plan in some cases the broker may still receive payment from the health plan. 29

www. calduals. org 30

Additional Resources • Health Insurance Counseling and Advocacy Program (HICAP) • Call HICAP for free unbiased counseling • Email info@calduals. org • Twitter @Cal. Duals 31
- Slides: 31