California Department of Public Health Hospital Preparedness Program

California Department of Public Health Hospital Preparedness Program Update Barbara Taylor Deputy Director for Public Health Emergency Preparedness California Department of Public Health May 2018
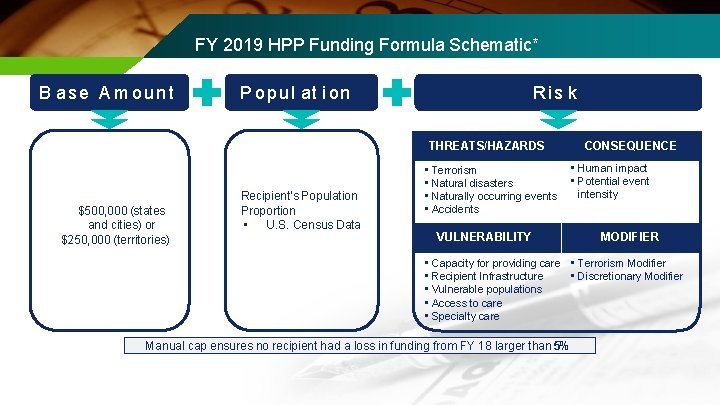
FY 2019 HPP Funding Formula Schematic* B ase A mount P o p u l at i on Ris k THREATS/HAZARDS $500, 000 (states and cities) or $250, 000 (territories) Recipient’s Population Proportion • U. S. Census Data • Terrorism • Natural disasters • Naturally occurring events • Accidents VULNERABILITY CONSEQUENCE • Human impact • Potential event intensity MODIFIER • Capacity for providing care • Terrorism Modifier • Recipient Infrastructure • Discretionary Modifier • Vulnerable populations • Access to care • Specialty care Manual cap ensures no recipient had a loss in funding from FY 18 larger than 5%
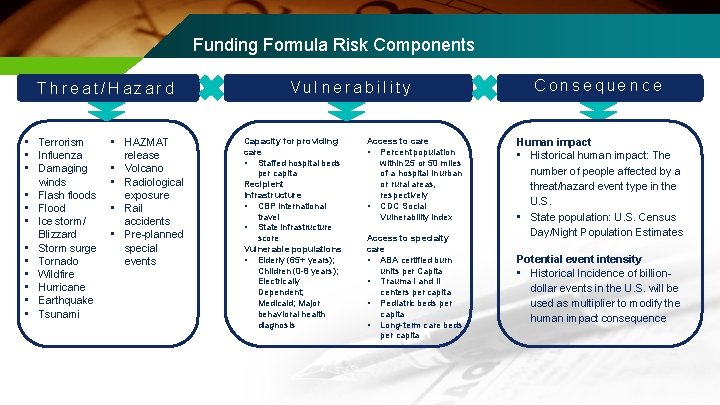
Funding Formula Risk Components T h r e a t / H a z ar d • Terrorism • Influenza • Damaging winds • Flash floods • Flood • Ice storm/ Blizzard • Storm surge • Tornado • Wildfire • Hurricane • Earthquake • Tsunami • HAZMAT release • Volcano • Radiological exposure • Rail accidents • Pre-planned special events V ul n e r a b i l i t y Capacity for providing care • Staffed hospital beds per capita Recipient Infrastructure • CBP international travel • State infrastructure score Vulnerable populations • Elderly (65+ years); Children (0 -8 years); Electrically Dependent; Medicaid; Major behavioral health diagnosis Access to care • Percent population within 25 or 50 miles of a hospital in urban or rural areas, respectively • CDC Social Vulnerability Index Access to specialty care • ABA certified burn units per Capita • Trauma I and II centers per capita • Pediatric beds per capita • Long-term care beds per capita C o n s e q ue n c e Human impact • Historical human impact: The number of people affected by a threat/hazard event type in the U. S. • State population: U. S. Census Day/Night Population Estimates Potential event intensity • Historical Incidence of billiondollar events in the U. S. will be used as multiplier to modify the human impact consequence
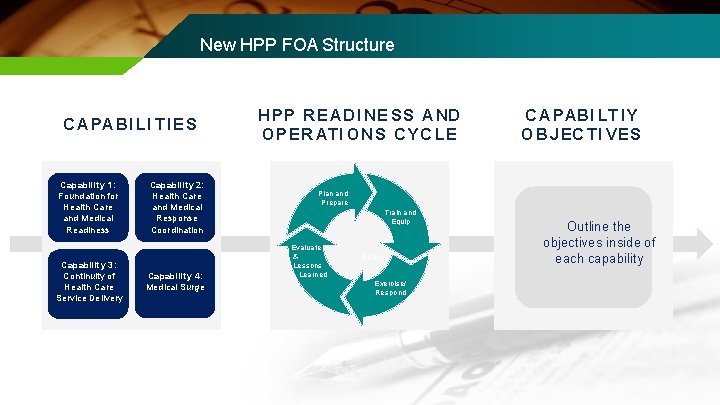
New HPP FOA Structure C A PA B I LI T I E S Capability 1: Foundation for Health Care and Medical Readiness Capability 3: Continuity of Health Care Service Delivery Capability 2: Health Care and Medical Response Coordination Capability 4: Medical Surge H P P R E AD I NE S S A ND O P ER ATI O N S C YC LE C A PABI LT I Y O B J EC TI VES Plan and Prepare Train and Equip Evaluate & Lessons Learned Share Exercise/ Respond Outline the objectives inside of each capability

HPP and PHEP Alignment • ASPR’s Hospital Preparedness Program (HPP) and CDC’s Public Health Emergency Preparedness (PHEP) grants remain programmatically aligned Separate grants management: ASPR Grants Management Continued coordination of private health care sector and state and local public health sector Continued joint HPP and PHEP activities

Joint HPP and PHEP Activities Plan and Prepare: • Administrative preparedness activities and • • Jurisdictional Risk Assessment ( JRA) Inclusive planning for whole community, including Health Care Coalitions (HCCs) and SME groups (formerly described as planning for at-risk and vulnerable populations) All-hazards response planning, including MCM, infectious diseases, provision of medical care in shelters, and HCC coordination and communication Train and Equip: • Provide PIO and PPE training and education Exercises and Response: • Joint statewide exercise including surge of • • patients into healthcare system Federal health care situational awareness initiatives Common operating picture, information sharing platforms Management of volunteers Ensure the ability to surge to meet the demands during a highly infectious disease response Evaluate and Share Lessons Learned • Submit AAR/IPs Saving Lives. Protecting Americans. 6

HCC Annual Requirements BE N C H M A RK S Subject to withholding Uploaded in CAT • HCC Response Plan Annexes • HCC Annual Budget • HCC Annual Work Plan • Pre-Event EEIs • Coalition Surge Test • Performance Measures (must also be submitted to recipient) S E L E CT A D D I T I O N A L RE Q UI RE ME NT S Uploaded in CAT • HCC Governance • HCC HVA • HCC Preparedness Plan • HCC Training Plan • HCC Response Plan • Inventory Management Protocol (if applicable) • NDMS FCC Exercise (if applicable) – AAR/IP Verified During Site visit • Clinical Advisor engagement • Readiness & Response Coordinator engagement • NIMS Implementation • HCC Information System Training • Communication Coordination • Staff / Volunteer Management • Resource Inventory Assessment Verified with HCC Budget, Work Plan or Response Plan • HCC Staffing x 2 (1 FTE) • Projects tied to Hazards/Risks • HCC EEI Integration

HCC Fiscal Year Requirements 2019 • Surge Estimator • Pediatric Surge Annex • Pediatric Annex TTX 2021 2022 2023 PIO Training HCC COOP Plan Supply Chain Assessment Infectious Disease Annex CSC Integration Infectious Disease TTX CSC Exercise (if applicable) • Surge Estimator • Radiation Surge Annex • Radiation Annex TTX • Chemical Surge Annex • Chemical Annex TTX • Surge Estimator 2020 • Burn Surge Annex • Clinical Info Sharing SOP • Burn Annex TTX • • A l l Year s • NDMS FCC Exercise (if applicable)

HPP – What’s New? 1 Encourage additional HCC membership 4 Develop HCC specialty surge annexes 2 Designate lead or colead hospital and 1 FTE 5 Complete HCC Surge Estimator Tool 3 Encourage hospital partnerships with NDMS 6 Flexibility for geographically isolated areas (FAR 4 + 60 miles between hospitals)

Encourage Additional HCC Membership The four core members of HCCs will remain the same. However, HPP encourages additional representation from these functional entities that are required to support acute health care service delivery. These are not limited to the following: • • Medical supply chain organizations Pharmacies Blood banks Long term care organizations • Clinical labs • Federal health care organizations • Outpatient care centers In addition, all HCC inpatient facilities, must demonstrate existing transfer agreements specifically to the following specialty care centers: • • Pediatric centers Trauma and burn centers

Designate Lead or Co-Lead Hospital and 1 FTE 1. All HCCs should designate a lead or co-lead hospital or health care organization. 2. All HCCs must fund at least 1. 0 FTE (combined and may include in-kind support of dedicated time) to support the following role requirements. The breakdown is at the discretion of the HCC and recipient. CLINICAL ADVISOR Provide clinical guidance and coordination pertaining to acute medical surge readiness and response for CBRNE, trauma, burn, and pediatric emergencies. Individual must be clinically active – HCC READINESS AND RESPONSE COORDINATOR Oversee planning, training, exercising, operational readiness, financial sustainability, and evaluation of the HCC.

Encourage Hospital Partnerships with NDMS Hospitals should enter into formal agreements with the National Disaster Medical System (NDMS) to serve as receiving facilities if they: 1 Meet the eligibility criteria for participation in the NDMS 2 Are members of HPP-funded HCCs This is intended to improve the recipient and HCC's surge capacity and enhance hospital preparedness in response to a medical surge event.
National Disaster Medical Center (NDMS) At least once during the project period, HCCs with an FCC must participate in the NDMS patient movement exercise.

Develop HCC-Level Specialty Surge Annexes • • HCCs will develop complementary coalition-level annexes to their base surge capacity/trauma mass casualty response plan to manage a large number of casualties with specific needs. Five annexes will be developed and tested through tabletop exercises over the course of five years in this order: Pediatric FY 2019 Burn FY 2020 Infectious Disease FY 2021 Radiation FY 2022 Chemical FY 2023

Complete HCC Surge Estimator Tool HCCs must complete the HCC Surge Estimator Tool to support coalitions in determining surge capacity. Three distinct variables drive rapid development of surge capacity and vary significantly between hospitals: 1 Use of all available “staffed” beds, including closed units that could be rapidly reopened with appropriate staff but are otherwise equipped and appropriate for inpatient care 2 Use of pre-induction, post-anesthesia, and procedural area beds that can be used for temporary inpatient care, usually at an intermediate care (telemetry) or higher level 3 Ability to generate space or reduce the numbers of patients requiring evacuation by early discharge of appropriate current inpatients to support surge discharge

Flexibility for Geographically Isolated Areas ASPR is providing flexibility by adding additional locations to existing territory/FAS guidance Hospitals located in geographic regions that are classified by both criteria below are eligible for classification as an "isolated frontier hospital“ and will be offered modified objectives, activities, and funding requirements • Geographic US Region classified as Frontier and Remote (FAR) 4 • Greater than 60 miles from nearest hospital / inpatient facility

Health Care Essential Elements of Information (EEI) HCC requirement: • Within the first 90 days of each budget period, all HCCs must provide ASPR an updated preevent specific EEI template. ASPR will provide recipients with a list of all required post-event and special-event EEIs for incorporation into state, local, and HCC reporting systems. HCC Requirement: • The HCC and its members must, at a minimum, define and integrate into their response plans procedures for sharing essential elements of information (EEIs). This includes but is not limited to: The current operational status of facilities Elements of electronic systems (HCC-level requirement) Resource needs and availability. • Upload in to the CAT a list of all required post-event and special-event elements will be provided for incorporation into state, local, and HCC reporting templates. *Content of presentation provided by ASPR Web. Ex meetings - April 2019
- Slides: 17