Calcium metabolism and its disorders Dr Amir Babiker

Calcium metabolism and its disorders Dr Amir Babiker MBBS, FRCPCH (UK), CCT (UK), Msc in Endocrinology and Diabetes - Queen Mary University, London (UK) Consultant Paediatric Endocrinologist (KKUH) Assistant Professor (KSU, KSA)
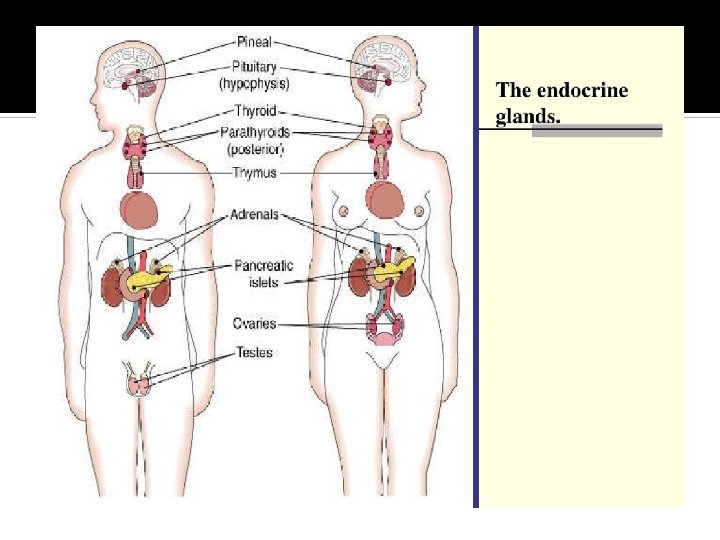
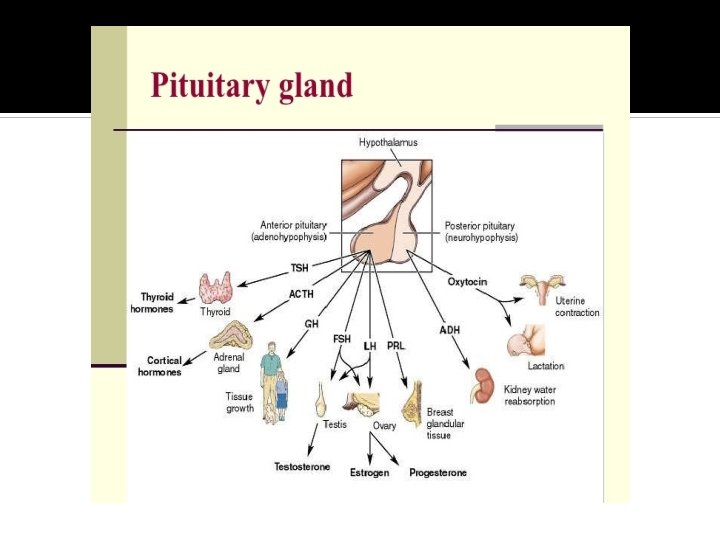
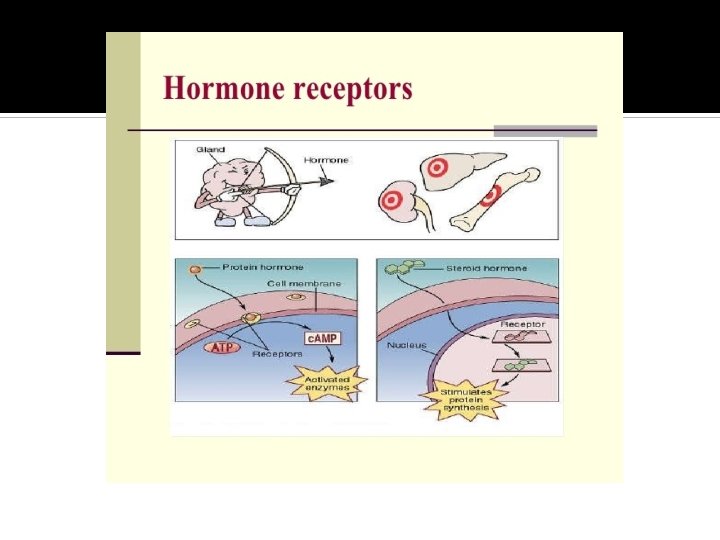



Outlines Calcium metabolism Calcium disorders (↓Ca, ↑Ca) • Parathyroid disorders • Vitamin D disorders Rickets
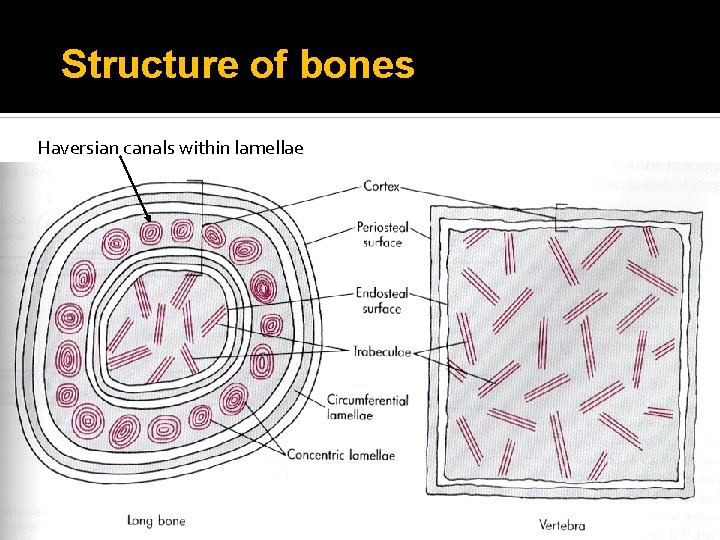
Structure of bones Haversian canals within lamellae
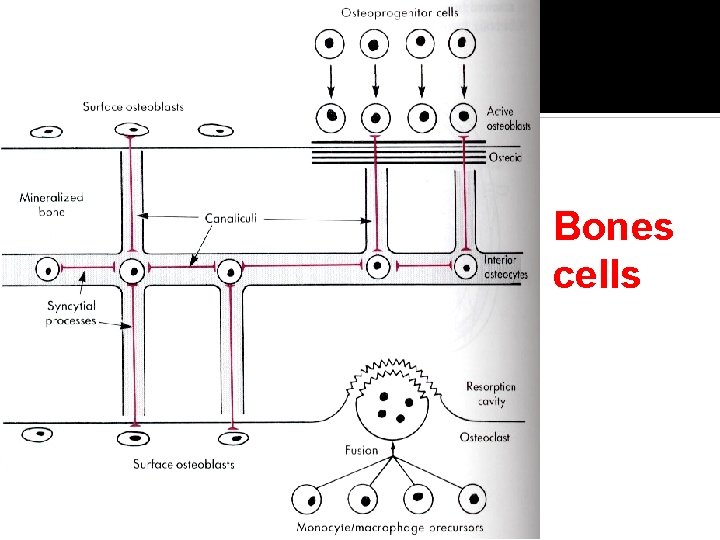
Bones cells

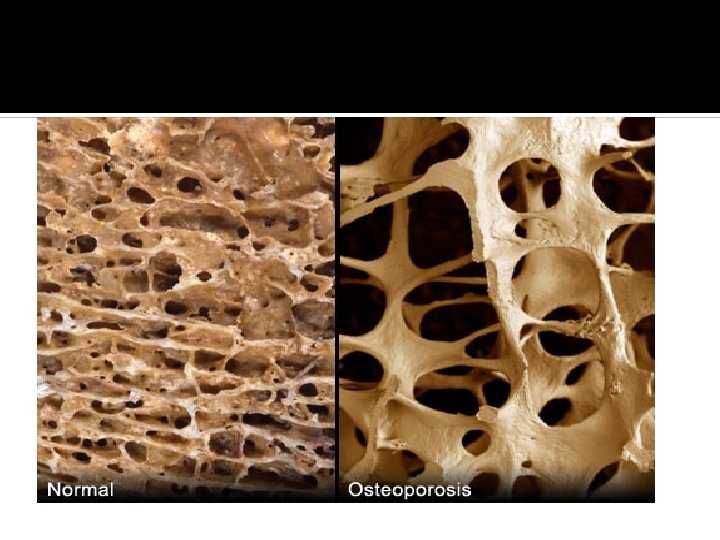
Physiological importance of Calcium salts in bone provide structural integrity of the skeleton Calcium ions in extracellular and cellular fluids is essential to normal function of a host of biochemical processes Neuoromuscular excitability Blood coagulation Hormonal secretion Enzymatic regulation

Calcium homeostasis Parathyroid Hormone (PTH), Vitamin D 3 (25 OH Vit D 3) and

Three Forms of Circulating Ca 2+

Regulation of Calcium Metabolism Minerals; serum concentration Calcium (Ca 2+); 2. 2 -2. 6 mmol/l (total) Phosphate (HPO 42 -); 0. 7 -1. 4 mmol/l Magnesium (Mg 2+); 0. 8 -1. 2 mmol/l Organ systems that play an import role in Ca 2+ metabolism Skeleton GI tract Kidney Calcitropic Hormones Parathyroid hormone (PTH) Calcitonin (CT) Vitamin D (1, 25 dihydroxycholecalciferol) Parathyroid hormone related protein (PTHr. P)

Calcium homeostasis While PTH and vitamin D act to increase plasma Ca++-- Calcitonin causes a decrease in plasma Ca++.
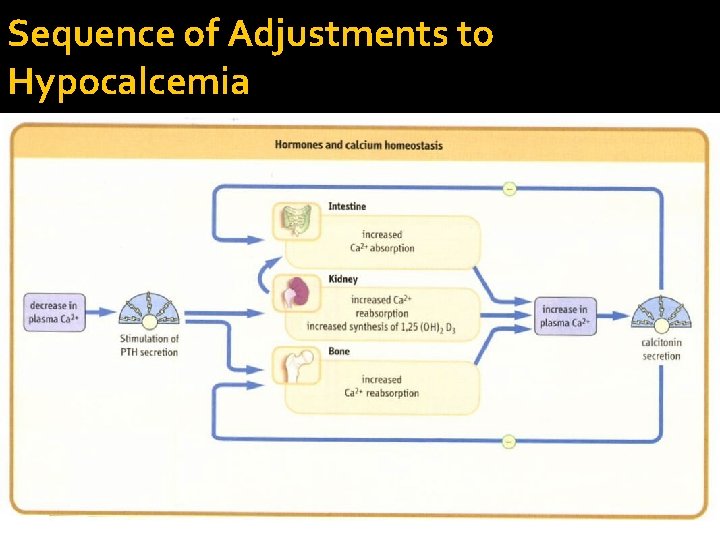
Sequence of Adjustments to Hypocalcemia

Parathyroid Hormone PTH is synthesized and secreted by the parathyroid gland which lie posterior to the thyroid glands. The blood supply to the parathyroid glands is from the thyroid arteries. The dominant regulator of PTH is plasma Ca 2+. Secretion of PTH is inversely related to [Ca 2+].

Vitamin D Vitamin D, after its activation to the hormone 1, 25 -dihydroxy Vitamin D 3 is a principal regulator of Ca++. Vitamin D increases Ca++ absorption from the intestine and Ca++ resorption from the bone.

Calcitonin acts to decrease plasma Ca++ levels. Calcitonin is synthesized and secreted by the parafollicular cells of the thyroid gland. The major stimulus of calcitonin secretion is a rise in plasma Ca++ levels Calcitonin is a physiological antagonist to PTH with regard to Ca++ homeostasis
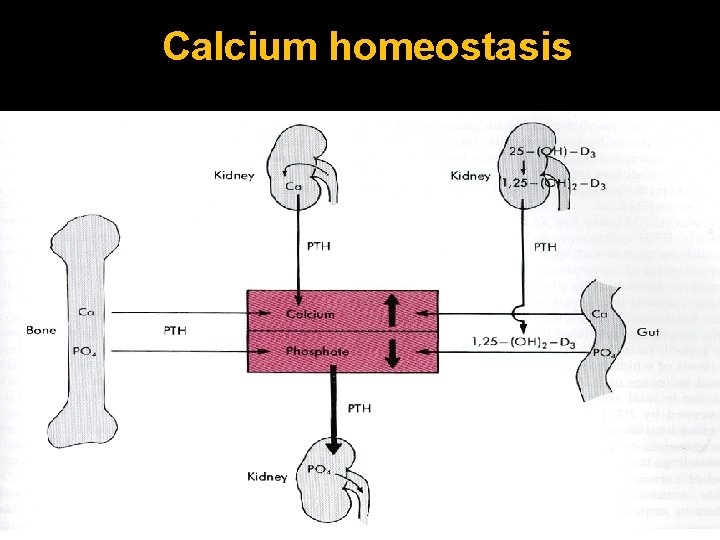
Calcium homeostasis
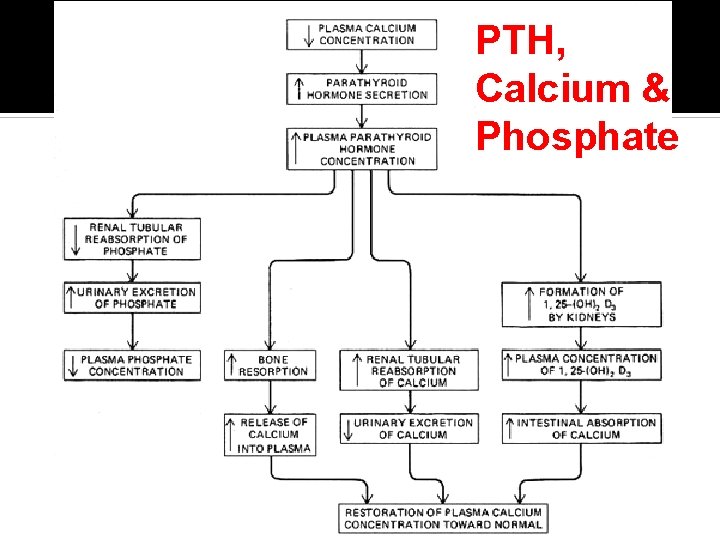
PTH, Calcium & Phosphate
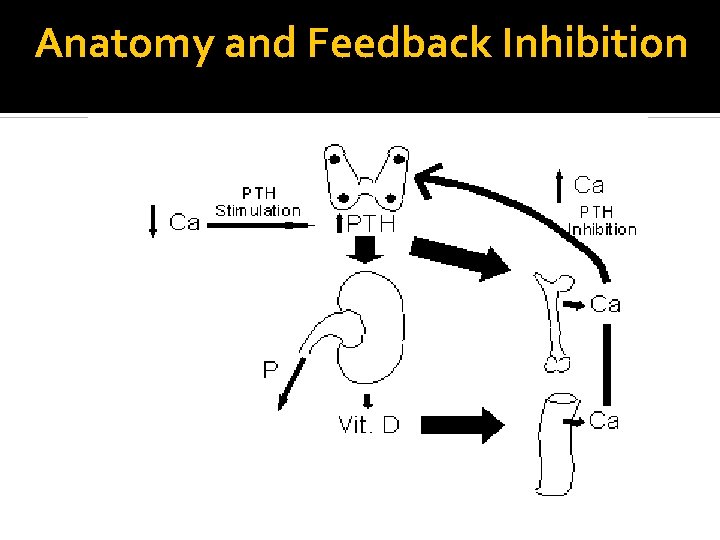
Anatomy and Feedback Inhibition
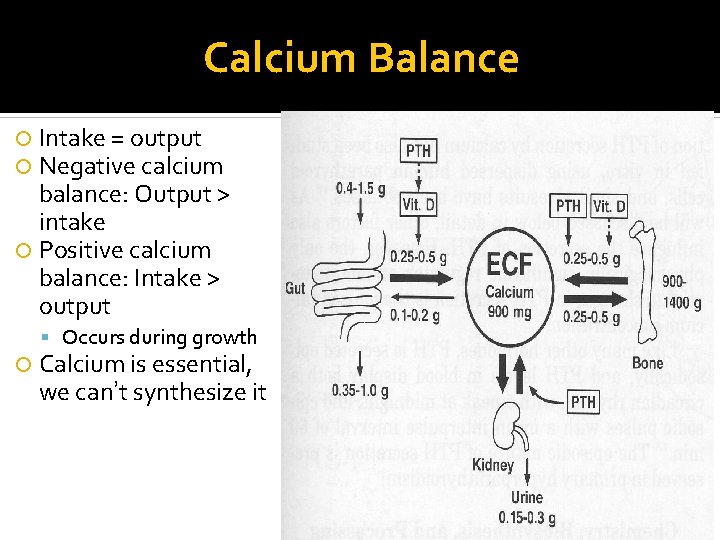
Calcium Balance Intake = output Negative calcium balance: Output > intake Positive calcium balance: Intake > output Occurs during growth Calcium is essential, we can’t synthesize it
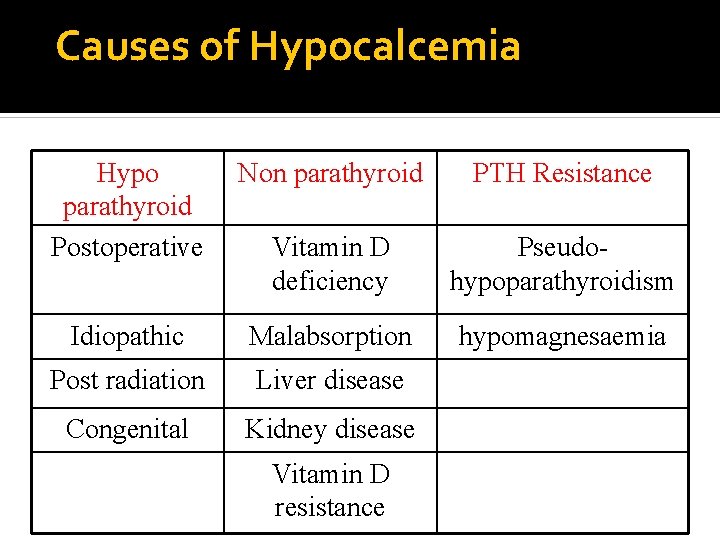
Causes of Hypocalcemia Hypo parathyroid Postoperative Non parathyroid PTH Resistance Vitamin D deficiency Pseudohypoparathyroidism Idiopathic Malabsorption hypomagnesaemia Post radiation Liver disease Congenital Kidney disease Vitamin D resistance

Hypoparathyroidism PTH-deficiency: reduced or absent synthesis of PTH Congenital (Di. George syndrome) or Acquired (Autoimmune or surgery) Hypocalcaemia occurs when there is inadequate response of the Vitamin D-PTH axis to hypocalcaemic stimuli Hypocalcemia is often bihormonal—concomitant decrease in 1, 25 -(OH)2 -D

Pseudohypoparathyroidism PTH-resistant hypoparathyroidism Due to defect in PTH receptor-adenylate cyclase complex Mutation in Gas subunit High or normal PTH, low Ca, high phosphate, normal Vit D 3 Clinical features: Hereditary Albright osteodystrophy, obesity, SS, subcutaneous nodules, short fourth metacarpal +/- intracranial calcification
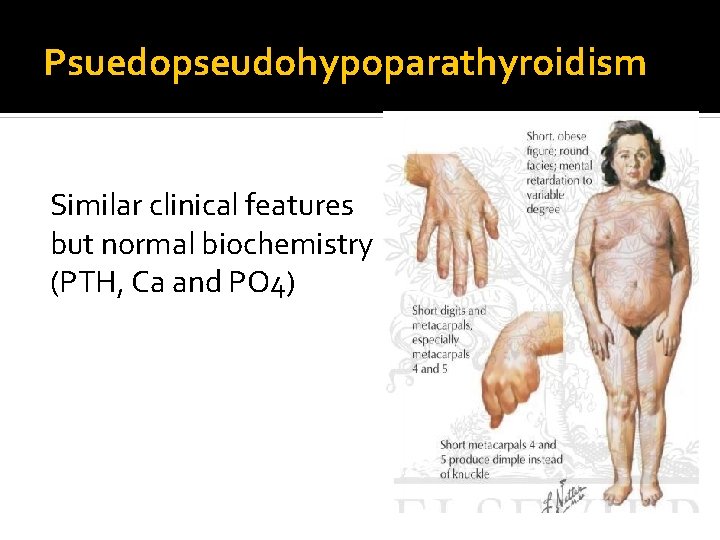
Psuedopseudohypoparathyroidism Similar clinical features but normal biochemistry (PTH, Ca and PO 4)

Rickets Reduced mineralization of bone matrix due to calcium deficiency. Commonest cause is Vit D 3 deficiency: Dietary lack of the vitamin Insufficient ultraviolet skin exposure Malabsorption of fats and fat-soluble vitamins- A, D, E, & K. Abnormal metabolism of vitamin D Chronic renal failure.
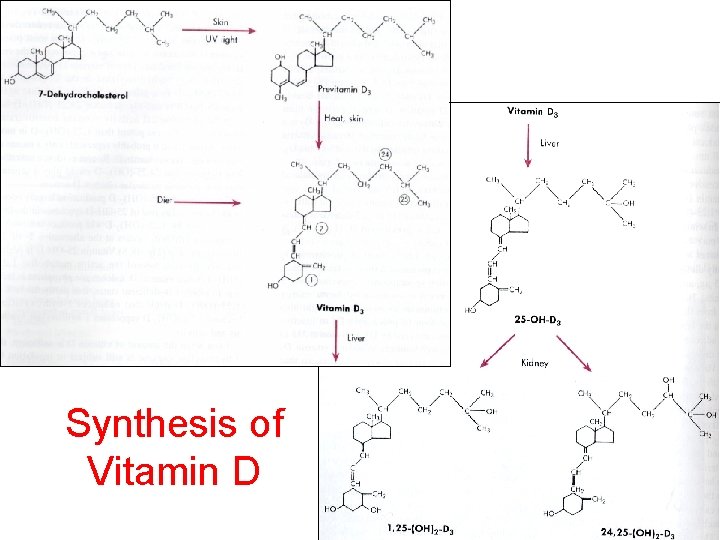
Synthesis of Vitamin D
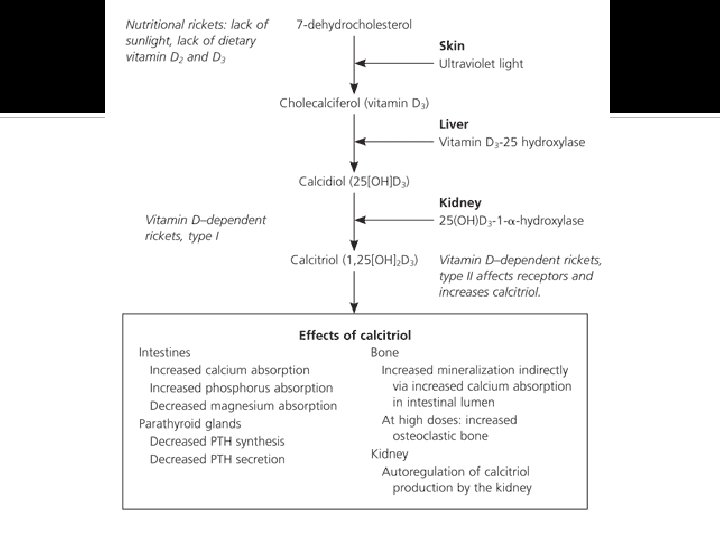

Types of rickets Nutritional Vitamin D deficient Vitamin D dependant type II (Vit D resistant) Hypophosphataemic

Other conditions that can cause rickets Medications Antacids Anticonvulsants Corticosteroids Loop diuretics Malignancy Prematurity

Clinical features Skeletal deformities Features of hypocalcaemia ( eg. Apathatic, poor feeding, tetany and seizures) Hypotonia and delayed motor development
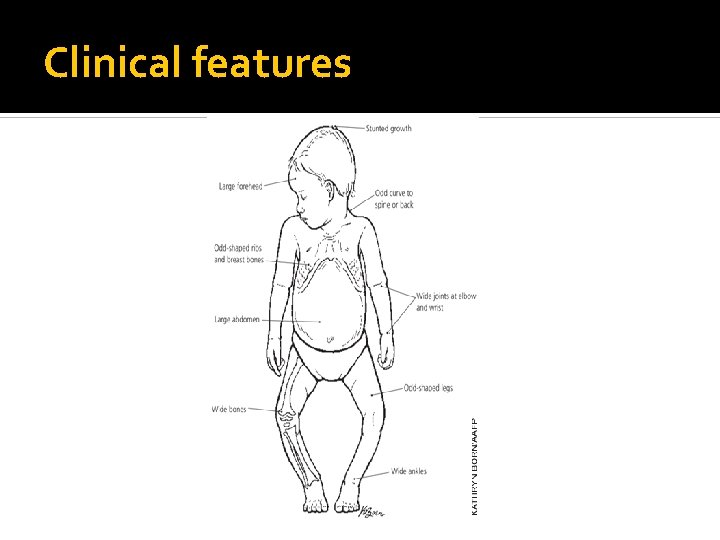
Clinical features

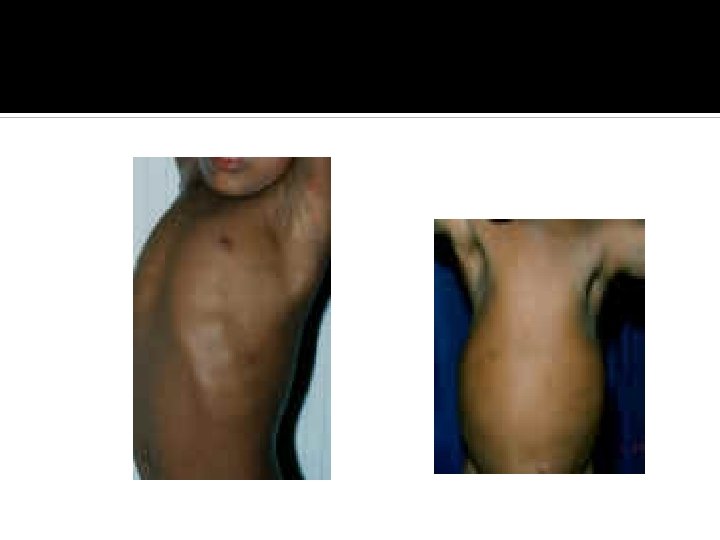
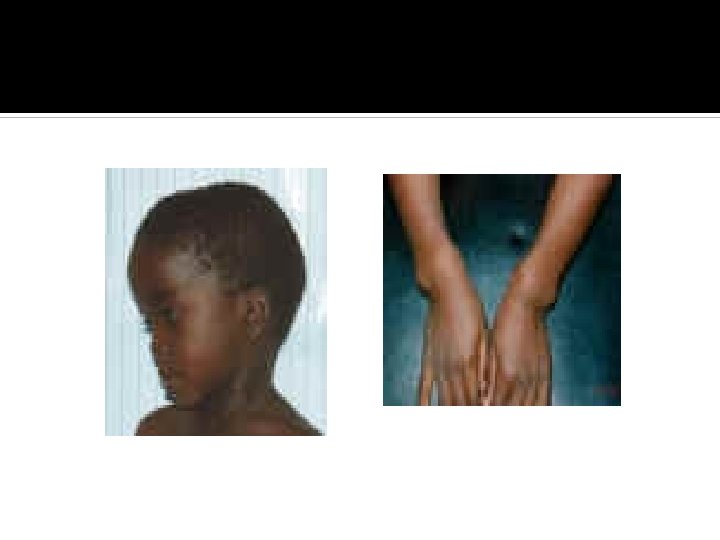

Investigations Bone profile calcium Phosphate Alkaline phosphatase Parathyroid hormone Vitamin D (25 OH Vit. D +/- 1, 25 (OH)2 Vit D) Urinary calcium and phospherus X- rays

Rickets confirmed if: Low or normal serum Ca Low phosphorus High alkaline phosphatase X rays of ends of long bones at knees or wrists: Widening, fraying, cupping of the distal ends of the shaft. Vit D level low Parathyroid hormone high

Rickets: Effects on growth plate Inadequate growth plate mineralization. Defective calcification in the interstitial regions Increase in thickness of growth plate. The columns of cartilage cells are disorganized.
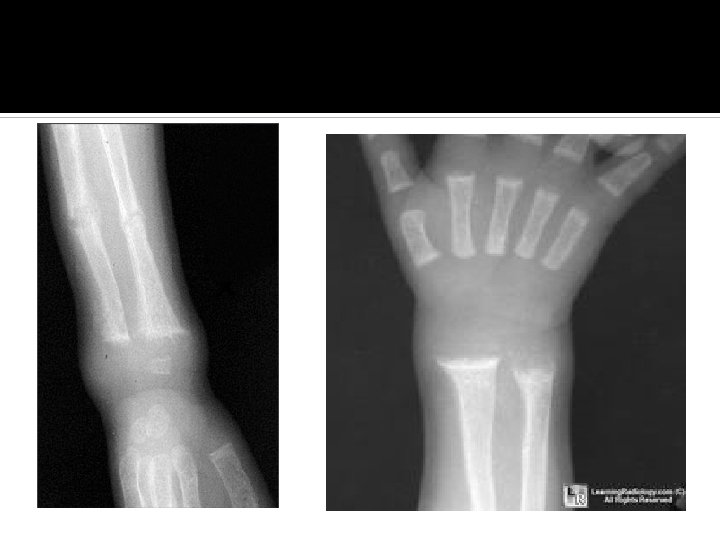
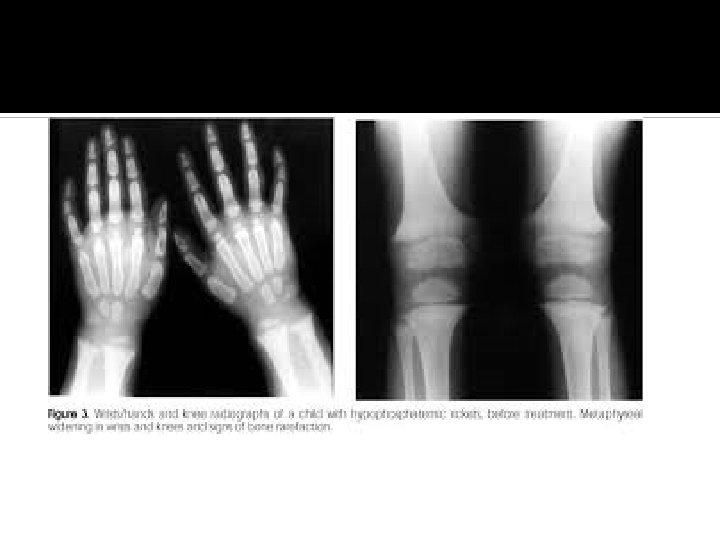

Skeletal and Radiographic Findings Associated with Rickets Bowing or widening of physis Costochondral beading (rachitic rosary) Craniotabes Delayed closure of anterior fontanel Dental abnormalities Flaring of ribs at diaphragm level (Harrison’s groove) Flaring of wrists Fraying and cupping

Treatment Vitamin D supplement or Vitamin D analogues (one alpha, calcitriol) Dose and type depends on the underline cause of Rickets Calcium Phosphate
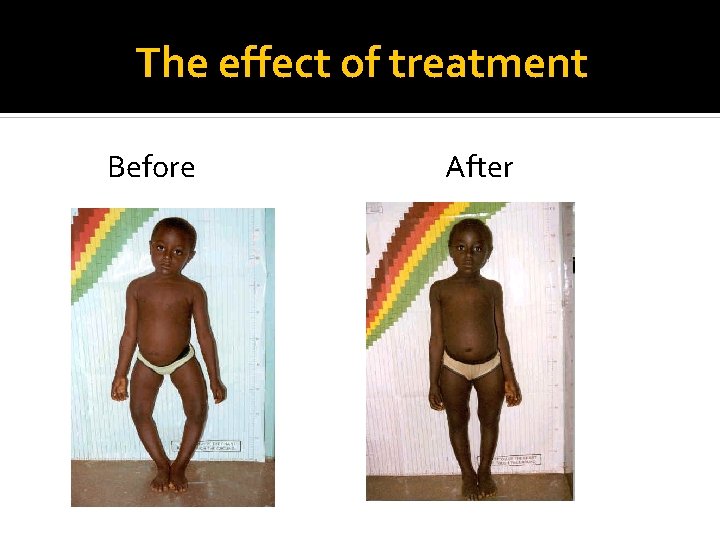
The effect of treatment Before After

Causes of Hypercalcemia Hyperparathyroidism Vitamin D toxicity (excessive intake) William syndrome Familial hypocalcuric hypercalcemia Malignant disease

Summary Calcium metabolism Calcium disorders (↓Ca, ↑Ca) • Parathyroid disorders • Vitamin D disorders Rickets

THANK YOU
- Slides: 48