Calcium homeostasis Bone remodeling and repair Continuous remodeling

Calcium homeostasis

Bone remodeling and repair • Continuous remodeling – 5 to 7 % of total bone mass per week – Critical for maintenance of proper structure • Removal of calcium

Bone remodeling • Location – Periosteum – Endosteum • Remodeling units – Osteoblasts – Osteoclasts • Does not occur uniformly – Different bones/different rates

Bone remodeling • Deposit – Site of injury – Strength re-enforcement – Nutrients • Proteins • Vitamins (A and D) • Minerals

Bone remodeling • Deposit – Osteroid seam • New matrix deposit – Unmineralized bone • Calcification front • Rate of calcification – Local concentrations of mineral products – Matrix proteins – Alkaline phosphatase

Bone remodeling • Resorption – Break down of bone matrix • Formation of resorption bay – Osteoclasts • • Lysosomal enzymes HCL Phagocytosis of dead osteocytes Activation triggered by T-lymphocytes
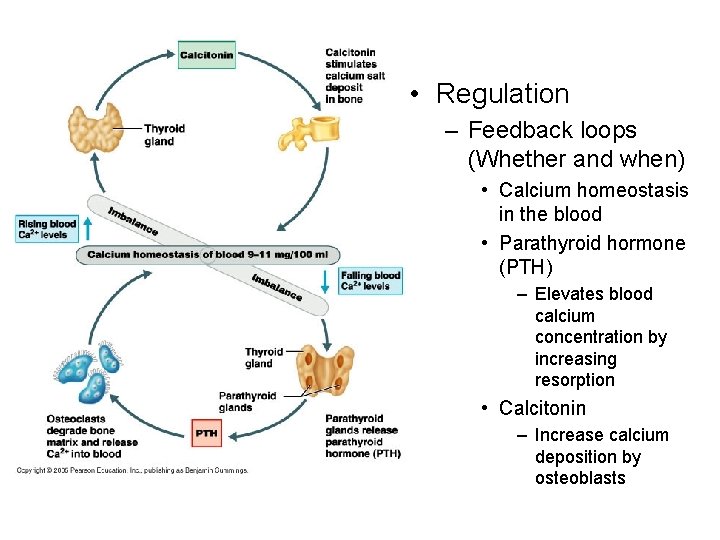
• Regulation – Feedback loops (Whether and when) • Calcium homeostasis in the blood • Parathyroid hormone (PTH) – Elevates blood calcium concentration by increasing resorption • Calcitonin – Increase calcium deposition by osteoblasts
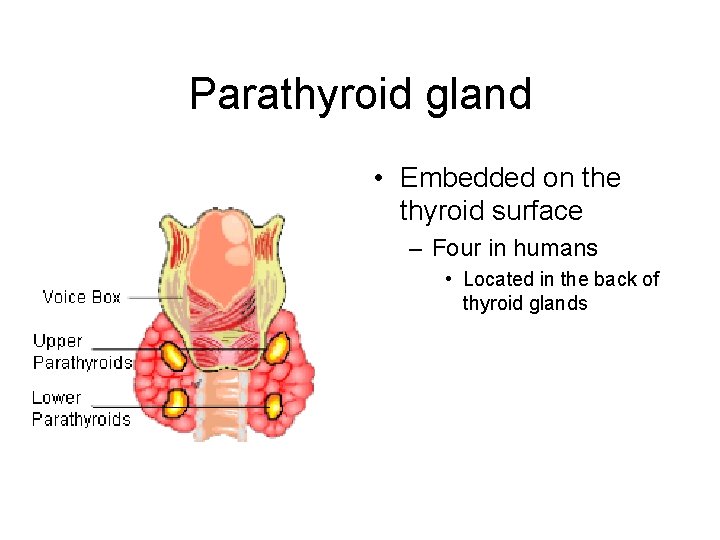
Parathyroid gland • Embedded on the thyroid surface – Four in humans • Located in the back of thyroid glands
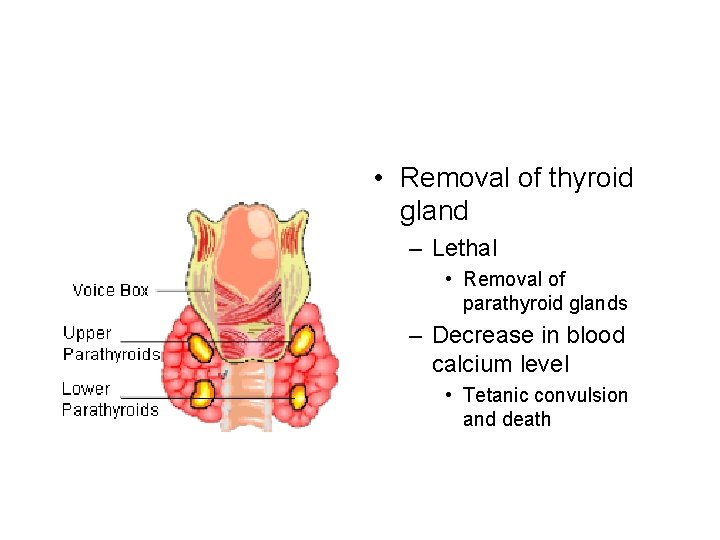
• Removal of thyroid gland – Lethal • Removal of parathyroid glands – Decrease in blood calcium level • Tetanic convulsion and death
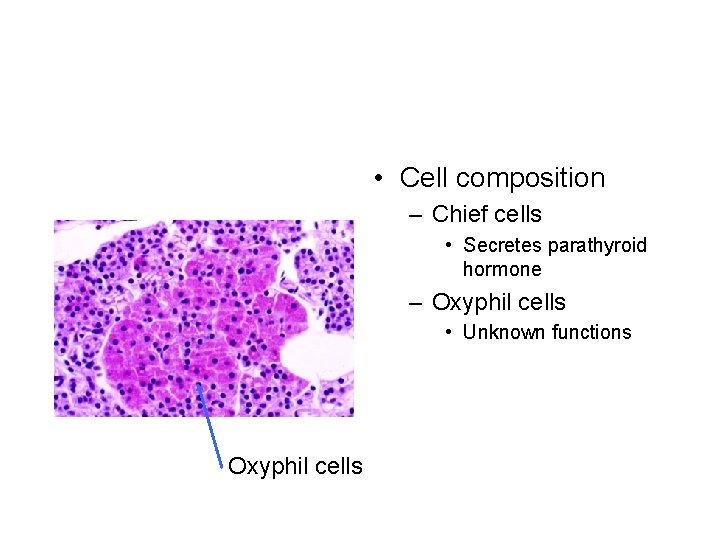
• Cell composition – Chief cells • Secretes parathyroid hormone – Oxyphil cells • Unknown functions Oxyphil cells

Parathyroid hormone • Essential for life • Chemistry – 84 AA • Preprohormone (115 AA) – Synthesized and converted within the Golgi zone of the chief cells – Proteolytic cleavage yields 90 AA prohormone • prohormone – Removal of 6 AA to yield mature peptide • Released into the bloodstream via exocytosis

• Highly conserved hormone • Short half-life – 3 -4 min – Cleaved into two fragments

Regulation of secretion • Blood calcium level – Ca receptors on the parathyroid cells • Seven-transmembrane domain receptor – Coupled with G-protein complex • Highly conserved – 93 % AA homology between human and bovine receptors • Interaction of receptor with Ca – Concentration- dependent conformation alteration – Decreased c. AMP production when high Ca concentrations – Increased c. AMP production when low Ca concentrations

• Vitamin D – Inhibition of PTH secretion • Genomic level • Slow effects – No changes in release of PTH immediately after vitamin D treatment

Function of PTH • Elevation of blood calcium level – Decreased phosphate ion concentrations – Acts on kidneys, intestines, and bones • Effects on mineral metabolism – Increased osteoclast activity • Secretion of cytokines by stromal osteoblast in response to PTH • Demineralization of bones

• Renal excretion and reabsorption – Increased calcium reabsporption • Renal tubular reabsorption – Increased phosphate excretion (phosphaturia) • Increased ionization of calcium – Prevention of Ca. PO 4 formation – Increased Mg reabsorption – Inhibition of Na-H exchange • Decreased blood p. H – Inhibition of Ca binding to plasma proteins

• Absorption of calcium – Intestine • Increased uptake (direct) • Effects on vitamin D metabolism (indirect) • Control of vitamin D synthesis – Increased 1, 25 -dihydrovitamin D synthesis from vitamin D • Kidney

• Other actions – Increased reticulocyte and lymphocyte mitosis – Vasodilation • Direct action involving specific receptor

Mechanism of action • Interaction between PTH and its receptor – Increased c. AMP production • Gs – Activation of phospholipase C • Production of IP 3 and DG – Activated by Gq – Vitamin D-dependent • Mobilization of Ca from bones

• Role of vitamin D on PTH action – Not on c. AMP production • Normal c. AMP production by the bones from vitamin D deficient mice – Later parts of biochemical reactions
Calcitonin • Maintenance of blood Ca level – Critical – Acute elevation • Meal – Return to normal shortly after elevation • Role of thyroid gland – Secretion of calcitonin • C (clear) cells
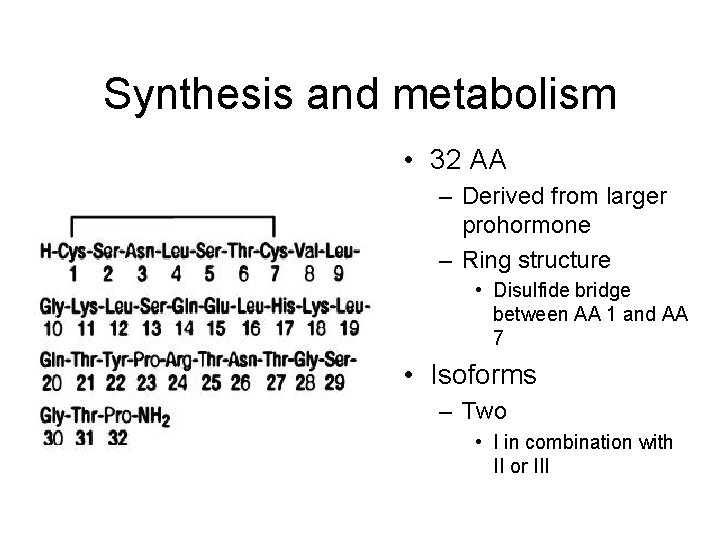
Synthesis and metabolism • 32 AA – Derived from larger prohormone – Ring structure • Disulfide bridge between AA 1 and AA 7 • Isoforms – Two • I in combination with II or III

• High structural similarity – Low AA homology – Fish calcitonin is more potent in humans • Resists proteolytic digestion • Higher receptor affinity
- Slides: 23