Calcium Channel Blocking Drugs Outline Introduction Pharmacokinetics CCB

Calcium Channel Blocking Drugs

Outline Ø Introduction Ø Pharmacokinetics Ø CCB binding sites Ø Adverse effects Ø Heterogeneity of action Ø Contraindications Ø Cardiac & hemodynamic Ø Summary differentiation
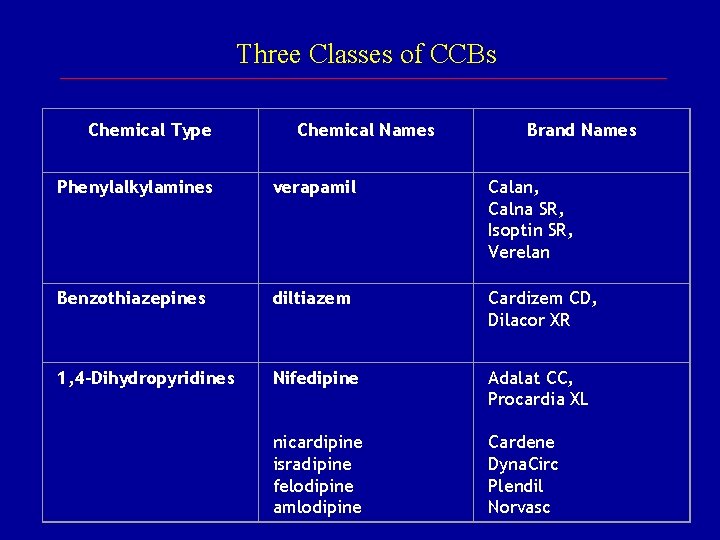
Three Classes of CCBs Chemical Type Chemical Names Brand Names Phenylalkylamines verapamil Calan, Calna SR, Isoptin SR, Verelan Benzothiazepines diltiazem Cardizem CD, Dilacor XR 1, 4 -Dihydropyridines Nifedipine nicardipine isradipine felodipine amlodipine Adalat CC, Procardia XL Cardene Dyna. Circ Plendil Norvasc

Widespread use of CCBs Ø Angina pectoris Ø Hypertension Ø Treatment of supraventricular arrhythmias - Atrial Flutter - Atrial Fibrillation - Paroxysmal SVT

Outline Ø Introduction Ø Pharmacokinetics Ø CCB binding sites Ø Adverse effects Ø Heterogeneity of action Ø Contraindications Ø Cardiac & hemodynamic Ø Summary differentiation
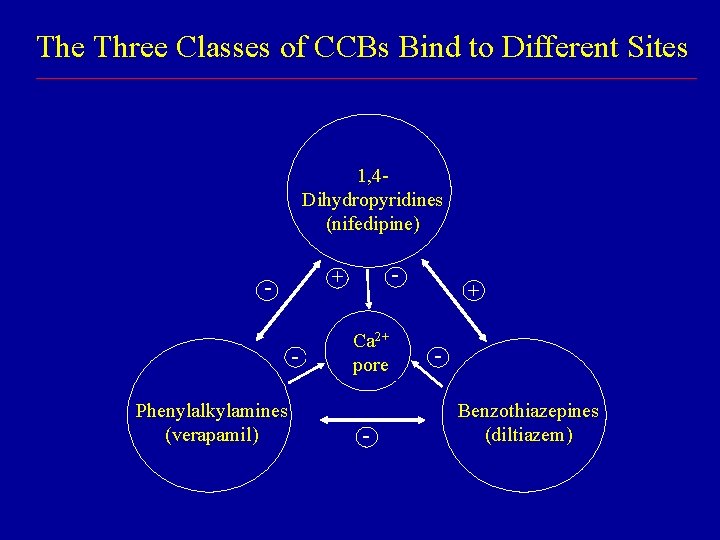
The Three Classes of CCBs Bind to Different Sites 1, 4 Dihydropyridines (nifedipine) Phenylalkylamines (verapamil) - + - Ca 2+ pore - + Benzothiazepines (diltiazem)

CCBs – Mechanisms of Action Ø Increase the time that Ca 2+ channels are closed Ø Relaxation of the arterial smooth muscle but not much effect on venous smooth muscle Ø Significant reduction in afterload but not preload

Outline Ø Introduction Ø Pharmacokinetics Ø CCB binding sites Ø Adverse effects Ø Heterogeneity of action Ø Contraindications Ø Cardiac & hemodynamic Ø Summary differentiation

Why Do CCBs Act Selectively on Cardiac and Vascular Muscle?
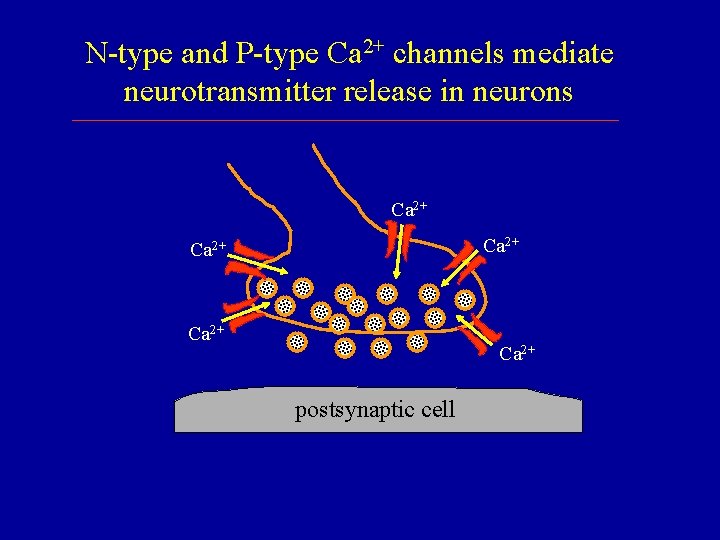
N-type and P-type Ca 2+ channels mediate neurotransmitter release in neurons Ca 2+ Ca 2+ postsynaptic cell
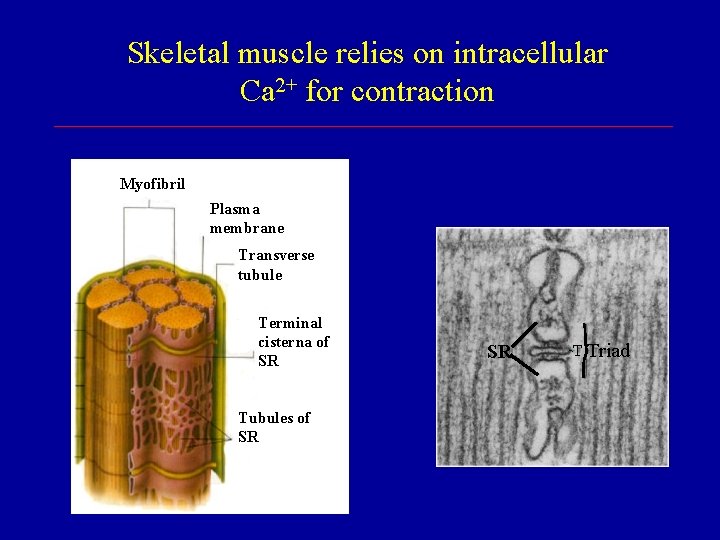
Skeletal muscle relies on intracellular Ca 2+ for contraction Myofibril Plasma membrane Transverse tubule Terminal cisterna of SR Tubules of SR SR T Triad

Cardiac cells rely on L-type Ca 2+ channels for contraction and for the upstroke of the AP in slow response cells Ca 2+ L-Type Ca 2+ Contractile Cells (atria, ventricle) Slow Response Cells (SA node, AV node)
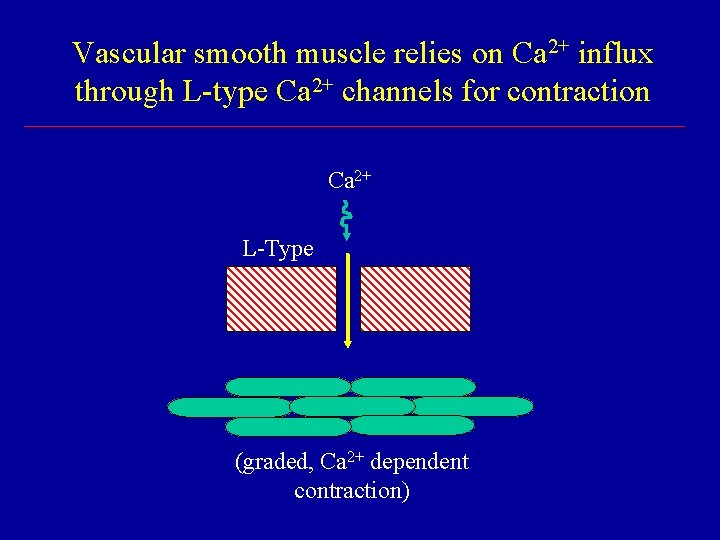
Vascular smooth muscle relies on Ca 2+ influx through L-type Ca 2+ channels for contraction Ca 2+ L-Type (graded, Ca 2+ dependent contraction)

CCBs Act Selectively on Cardiovascular Tissues Ø Neurons rely on N-and P-type Ca 2+ channels Ø Skeletal muscle relies primarily on [Ca]i Ø Cardiac muscle requires Ca 2+ influx through L-type Ca 2+ channels - contraction (fast response cells) - upstroke of AP (slow response cells) Ø Vascular smooth muscle requires Ca 2+ influx through L-type Ca 2+ channels for contraction

Outline Ø Introduction Ø Pharmacokinetics Ø CCB binding sites Ø Adverse effects Ø Heterogeneity of action Ø Contraindications Ø Cardiac & hemodynamic Ø Summary differentiation

Differential effects of different CCBs on CV cells Dihydropyridines: Selective vasodilators Peripheral vasodilation Non -dihydropyridines: equipotent for cardiac tissue and vasculature Heart rate moderating SN AV Potential reflex increase in HR, myocardial contractility and O 2 demand SN AV Coronary VD Reduced inotropism Peripheral and coronary vasodilation
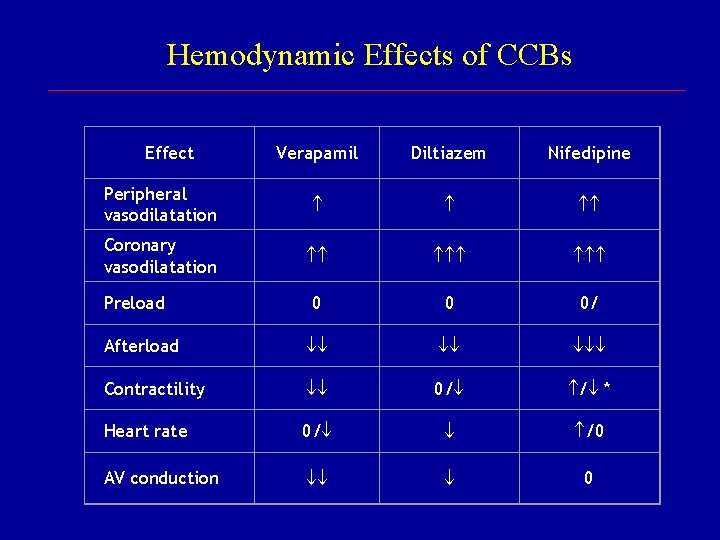
Hemodynamic Effects of CCBs Effect Verapamil Diltiazem Nifedipine Peripheral vasodilatation Coronary vasodilatation 0 0 0/ Afterload Contractility 0/ / * Heart rate 0/ /0 AV conduction 0 Preload

Outline Ø Introduction Ø Pharmacokinetics Ø CCB binding sites Ø Adverse effects Ø Heterogeneity of action Ø Contraindications Ø Cardiac & hemodynamic Ø Summary differentiation
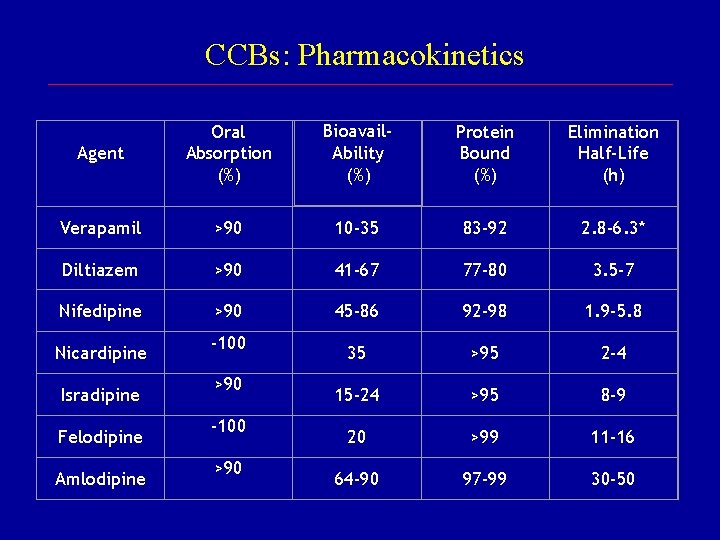
CCBs: Pharmacokinetics Agent Oral Absorption (%) Bioavail. Ability (%) Protein Bound (%) Elimination Half-Life (h) Verapamil >90 10 -35 83 -92 2. 8 -6. 3* Diltiazem >90 41 -67 77 -80 3. 5 -7 Nifedipine >90 45 -86 92 -98 1. 9 -5. 8 35 >95 2 -4 15 -24 >95 8 -9 20 >99 11 -16 64 -90 97 -99 30 -50 Nicardipine Isradipine Felodipine Amlodipine -100 >90

Outline Ø Introduction Ø Pharmacokinetics Ø CCB binding sites Ø Adverse effects Ø Heterogeneity of action Ø Contraindications Ø Cardiac & hemodynamic Ø Summary differentiation
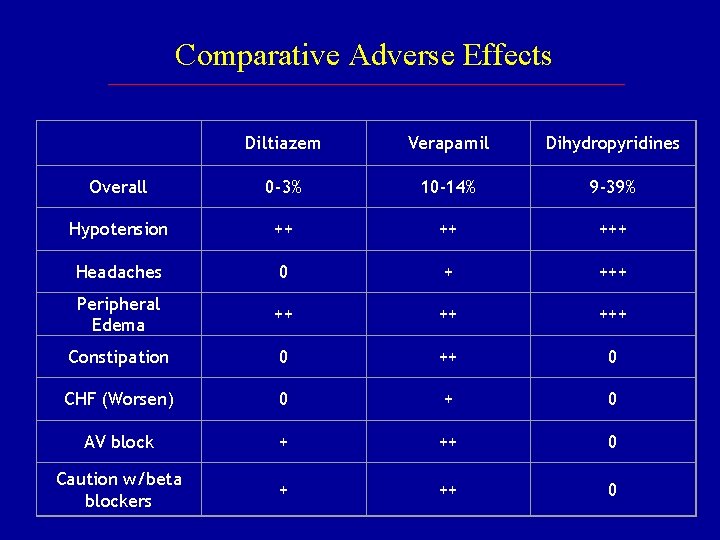
Comparative Adverse Effects Diltiazem Verapamil Dihydropyridines Overall 0 -3% 10 -14% 9 -39% Hypotension ++ ++ +++ Headaches 0 + +++ Peripheral Edema ++ ++ +++ Constipation 0 ++ 0 CHF (Worsen) 0 + 0 AV block + ++ 0 Caution w/beta blockers + ++ 0

CCBs - Monitoring Ø heart rate Ø blood pressure Ø anginal symptoms Ø signs of CHF Ø adverse effects

Outline Ø Introduction Ø Pharmacokinetics Ø CCB binding sites Ø Adverse effects Ø Heterogeneity of action Ø Contraindications Ø Cardiac & hemodynamic Ø Summary differentiation
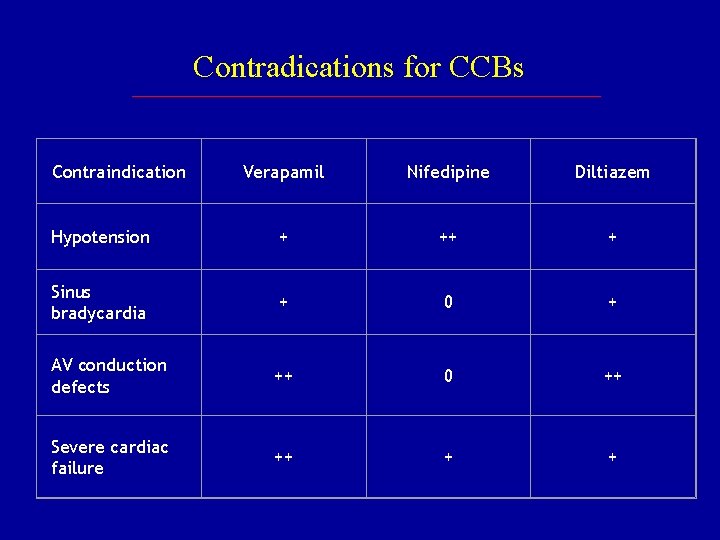

Contradications for CCBs Contraindication Verapamil Nifedipine Diltiazem Hypotension + ++ + Sinus bradycardia + 0 + AV conduction defects ++ 0 ++ Severe cardiac failure ++ + +

Outline Ø Introduction Ø Pharmacokinetics Ø CCB binding sites Ø Adverse effects Ø Heterogeneity of action Ø Contraindications Ø Cardiac & hemodynamic Ø Summary differentiation

Which CCB is most likely to cause hypotension and reflex tachycardia? A. Diltiazem B. Nifedipine C. Verapamil

Contraindications for CCBs include (choose all appropriate): A. Supraventricular tachycardias B. Hypotension C. AV heart block D. Hypertension E. Congestive heart failure

CCBs may improve cardiac function by: A. Reducing cardiac afterload B. Increasing O 2 supply C. Decreasing cardiac preload D. Normalizing heart rate in patients with E. supraventricular tachycardias

Thank you!
- Slides: 29