By Sindhu Priya E S Physiology Physis means
By Sindhu Priya E S

Ø Physiology - Physis means “nature/origin” - Logos means “Study” “Physiology is the study of normal functioning of the body” Ø Pathophysiology - Patho means “suffering” from a disease “Pathophysiology is the study of disordered physiological processes associated with disease or injury”

• Etiology is the origin of a disease including causes and modifying factors • Pathogenesis refers to the steps in the development of a disease

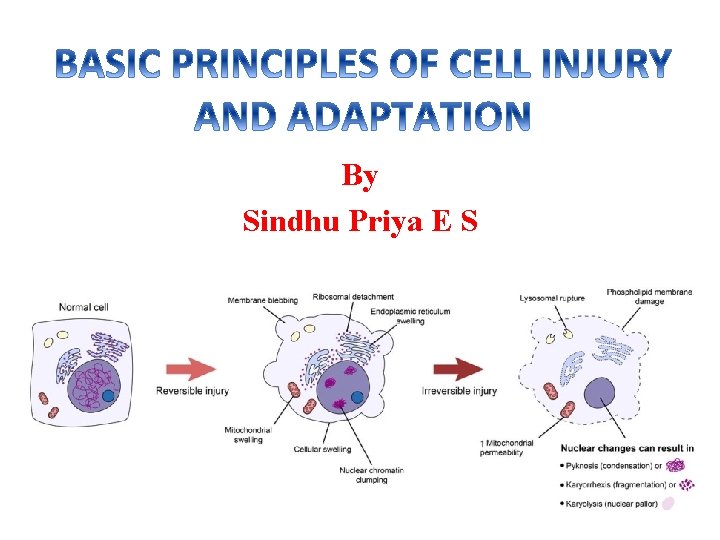
Ø Cell injury is the alteration of cell structure or biochemical functioning resulting from some stress that exceeds the ability of the cell to compensate through normal physiologic adaptive mechanisms. Ø Adaptation is the capability of the cells under stress to adapt to the changes in the physiologic and pathologic conditions by alteration of their morphology, pattern of growth or metabolic activity.
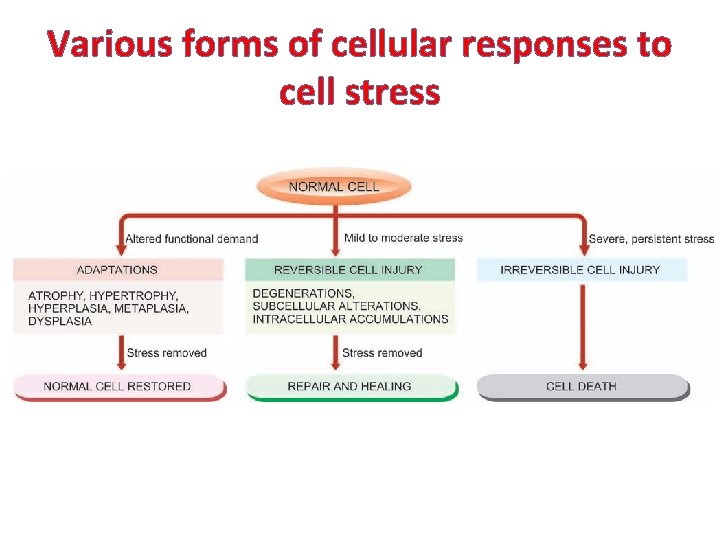
Various forms of cellular responses to cell stress


Homeostasis • Homeostasis refers to the stability, balance or equilibrium in the body’s internal environment due to constant interaction of body’s many regulatory processes • The adjustment of physiological systems within the body to maintain stability is called homeostatic regulation

Components • Homeostatic mechanism is maintained by control system or feedback system with 3 components 1. Receptors 2. Control center (integrator) 3. Effector

1. Receptor Ø It is a region of tissue, or a molecule in a cell membrane, which responds specifically to a particular neurotransmitter, hormone, antigen, or other substance. Ø It monitors changes in the controlled condition and seeds input to a control center in the form of nerve impulse or chemical signals

2. Control center (integrator) • It integrates data from sensors and commands the effector to produce a physiological response restoring the initial changes 3. Effector • It is the mechanism that has a body structure that receives output from the control center to produce physiological response
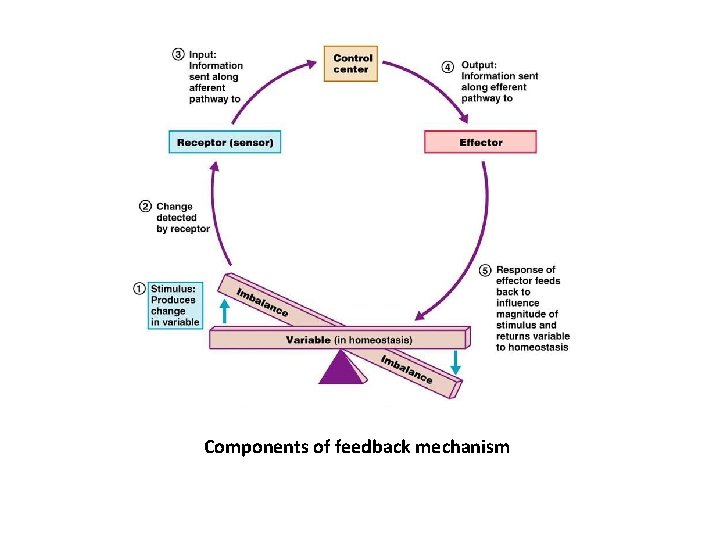
Components of feedback mechanism

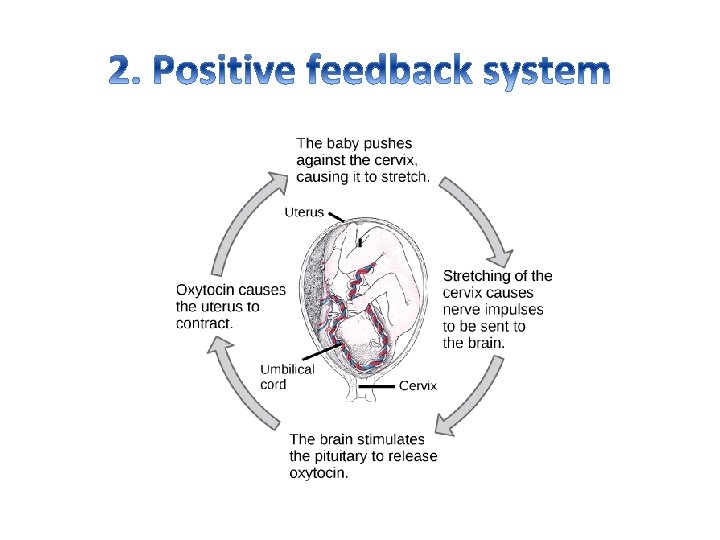
Feedback system • It consists of cycle of events information about a change is fed back into the system so that regulator can control the process. There are two types of feedback system 1. Negative feedback system 2. Positive feedback system




Causes of cell injury 1. Hypoxia and Hyperoxia (Ischemia) 2. Physical agents / stress (Trauma, shock etc. . ) 3. Chemical agents and drugs (Cyanide, mercury, cytotoxic agents) 4. Microbial agents (Bacteria, fungi, virus) 5. Immunologic factors (autoimmune disease, allergy)

Causes of cell injury 6. Nutritional derangements (deficiencies, excess) 7. Aging (senescense) 8. Psychogenic diseases (Drug addiction, alcoholism, smoking) 9. Iatrogenic factors (Drugs, radiation) 10. Idiopathic diseases (unknown cause)


Different mechanisms involved in the pathogenesis of cell injury are: 1. Reversible hypoxic injury 2. Irreversible hypoxic injury 3. Free radical mediated cell injury 4. Chemical injury

1. Reversible hypoxic injury § If ischemia or hypoxia is for short period of time, the cell can be reverting back to its normal condition which is known as Reversible cell injury § Steps involved in Reversible cell injury are 1. Decreased generation of cellular ATP 2. Intracellular lactic acidosis 3. Damage to plasma membrane pumps: Cell swelling and other membrane changes causing cell swelling 4. Reduced protein synthesis: dettachment of ribosomes from ER

2. Irreversible hypoxic injury • Persistence of ischaemia or hypoxia results in irreversible damage to the structure and function of the cell (cell death). This stage is called point of no return or irreversibility • Steps involved in Reversible cell injury are 1. 2. 3. 4. Calcium influx: Mitochondrial damage Activated phospholipases: Membrane damage Intracellular proteases: Cytoskeletal damage Activated endonucleases: Nuclear damage


3. Free radical mediated cell injury 1. Calcium overload 2. Generation of reactive oxygen radicals (superoxide, H 2 O 2, hydroxyl radicals) 3. Subsequent inflammatory reaction
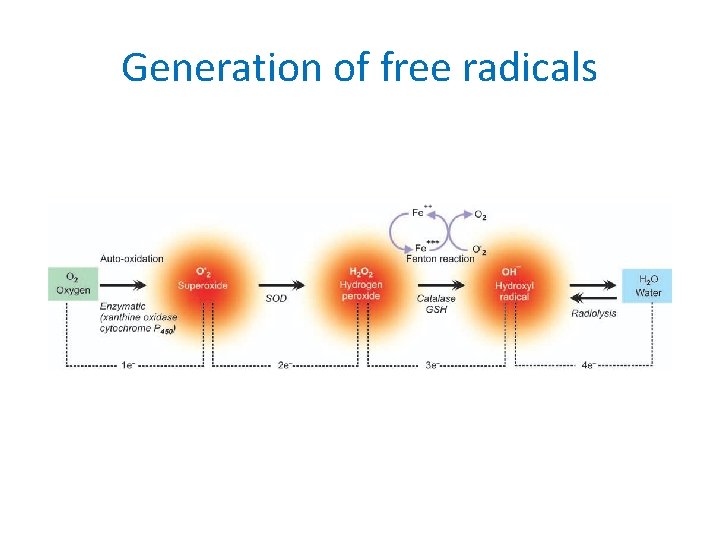
Generation of free radicals
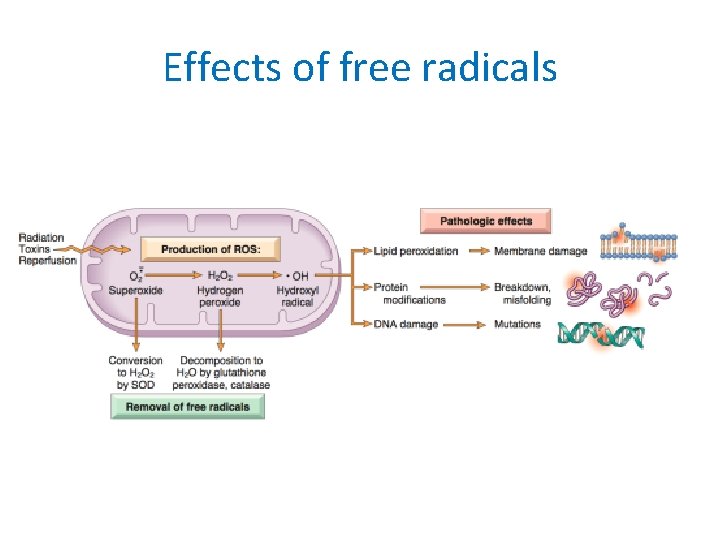
Effects of free radicals


4. Chemical induced cell injury • Chemicals induce cell injury by one of the following mechanism a. Direct cytotoxicity (Mercury, lead, Iron, anticancer drugs) b. Conversion of chemical into reactive metabolite (CCl 4, acetaminophen, bromobenzene)


1. Mitochondrial changes • Mitochondrial integrity is crucial for cell survival as it is the power house of the cell Causes: ü Increase Cytosolic calcium, free radicals Effects: ü No ATP generation ü Release of cytochrome into cytoplasm


2. Cell membrane damage § Cell membrane controls the movement of substances in and out of the cell and protects the cell from its surroundings § It consists of phospholipid molecules embedded with protein molecules. v. Causes üDirect damage by toxins (bacteria, viruses, physical or chemical injury) üCalcium- mediated phospholipase and protease activation üFree radical induced lipid peroxidation v. Effects üLoss of Membrane barriers thus loss of cellular contents. Eg. Loss of mitochondria which results in decreased ATP production. üLoss of cell integrity


3) Ribosome damage Ribosomes are the protein (DNA & RNA) making factories of the cell v Causes ü Oxidative damage through Reactive oxygen species (ROS) eg. Ethyl alcohol, hydrogen peroxide ü RNA oxidation is more common than DNA oxidation v Effects Dysfunctioning in protein synthesis and eventually cell death


Cellular adaptations • Adaptation is the phenomenon wherein a cell adjusts to changes in its environment in an attempt to escape injury and sustain viability and function • Physiological adaptation (changes in their environment) • Pathological adaptation pathologic injury) (due to non-lethal

Adaptive changes in cell growth 1. 2. 3. 4. 5. Atrophy Hyperplasia Metaplasia Dysplasia
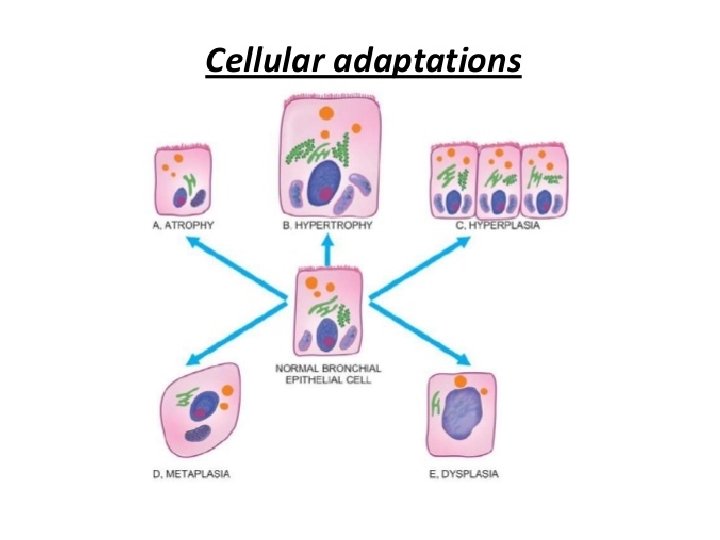

1. Atrophy • Atrophy is decrease in cell size due to loss of cell substance • Causes: – Physiological: normal process of aging – Pathological: starvation atrophy, ischemic atrophy, disuse atrophy, neuropathic atrophy


Morphological features Irrespective of the underlying cause for atrophy, the pathologic changes are similar. • The organ is small, often shrunken • The cells become smaller in size but are not dead cells. • Shrinkage in cell size is due to reduction in cell organelles, chiefly mitochondria, myofilaments and endoplasmic reticulum. • There is often increase in the number of autophagic vacuoles containing cell debris • These autophagic vacuoles may persist to form ‘residual bodies’ in the cell cytoplasm e. g. lipofuscin pigment granules in brown atrophy

2. Hypertrophy • Hypertrophy is increase in cell size resulting from increased functional capacity & thus cells are bigger than normal • 2 types of Hypertrophy: Physiologic hypertrophy and Pathologic hypertrophy. • Example of Physiologic hypertrophy: – – Reproductive organs get bigger when there is demand like mammary glands after pregnancy Muscles get bigger after heavy exerscise • Example of Pathologic hypertrophy: – If there is blockage of heart then the heart muscles face unnatural load leading to hypertrohy and then eventually heart failure

Morphological features • The affected organ is enlarged and heavy • At ultrastructural level, there is increased synthesis of DNA and RNA, increased protein synthesis • Increased number of organelles like mitochondria, endoplasmic reticulum and myofibrils


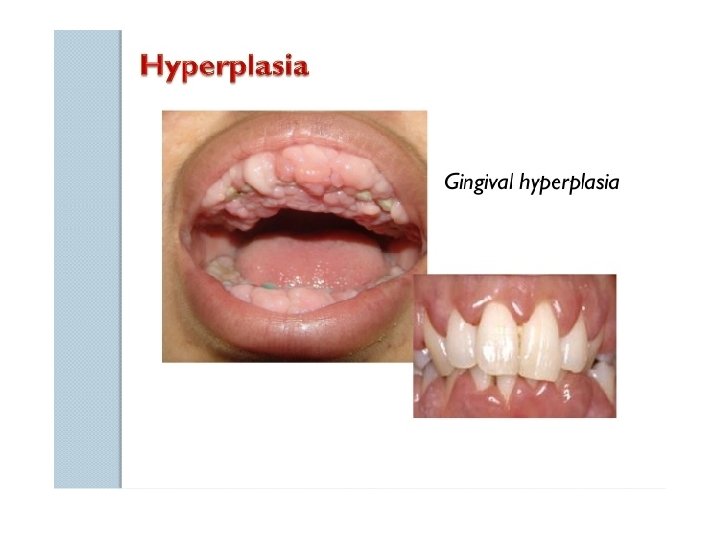
3. Hyperplasia ü Hyperplasia refers to increase in cell number in tissues ü This may eventually lead to neoplasia (cancer) ü Example: Hyperplasia of female breast at puberty, pregnancy and lactation

4. Metaplasia ü Metaplasia refers to reversible change of one epithelial adult cell to another type in response to abnormal stimuli and reverts back to normal on removal of stimulus but if persists then leads to neoplasia ü Example: Urinary bladder is lined with transitional epithelium but in chronic infection it is replaced with squamous epithelium.
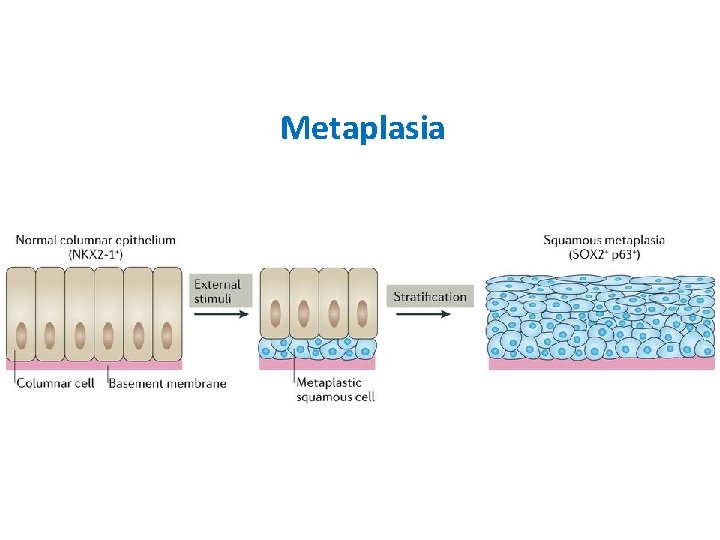
Metaplasia
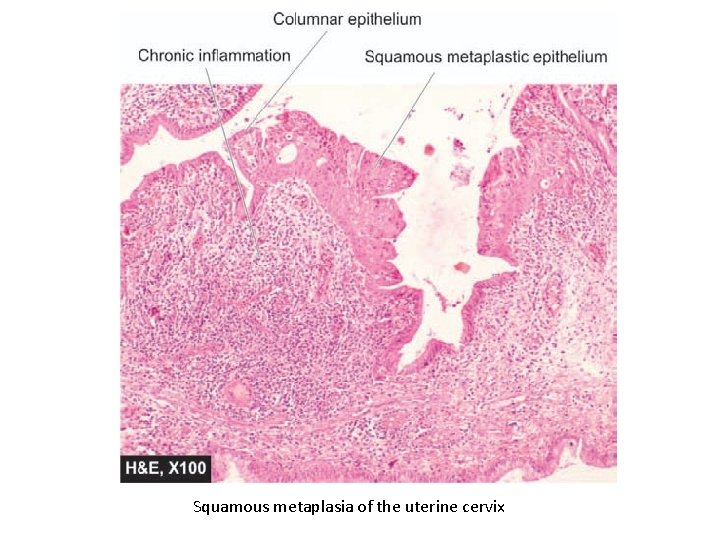
Squamous metaplasia of the uterine cervix

5. Dysplasia ü Dysplasia refers to disordered cellular development. It is always accompanied with metaplasia and hyperplasia and thus also referred as atypical hyperplasia. ü Example: 1) disorderly arrangement of cells 2) nuclei lying away from basement membrane

Characteristic changes in epithelial dysplasia 1. Increased number of layers of epithelial cells 2. Disorderly arrangement of cells from basal layer to the surface layer 3. Loss of basal polarity i. e. nuclei lying away from basement membrane 4. Cellular and nuclear pleomorphism 5. Increased nucleocytoplasmic ratio
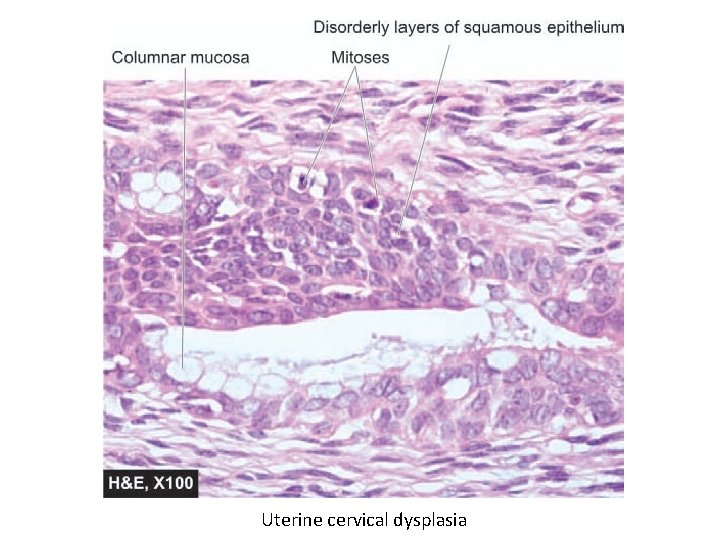
Uterine cervical dysplasia
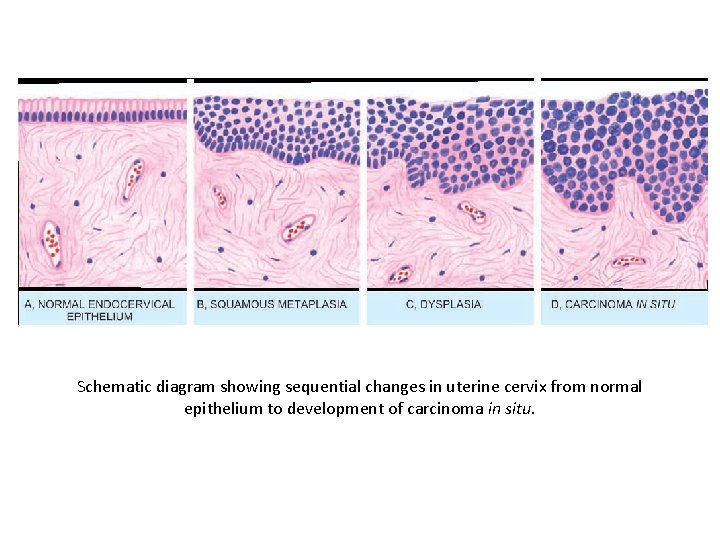
Schematic diagram showing sequential changes in uterine cervix from normal epithelium to development of carcinoma in situ.

1. Reversible cell injury a. Cellular swelling b. Fatty change 2. Irreversible cell injury/cell death a. Apoptosis b. Necrosis

1. Reversible cell injury Ultra structural changes of reversible cell injury are • Plasma membrane -Blebbing, blunting, distortion of microvilli and loosening of intracellular attachments • Mitochondria – swelling, formation of phospholipid bodies in matrix • ER- dilation of ER, detachment of ribosomes and dissociation of polysomes • Nucleus – disaggregation of granular and fibrillar elements
Ø It is an intracytoplasmic accumulation of water due to incapacity of the cells to maintain the ionic and fluid homeostasis. Ø It is the first manifestation of cellular injury. Ø Causes: Cellular hypoxia (inadequate oxygen), Hypokalemia Ø Effects: Damage to the sodium potassium pump, Increase in weight of the organ, cell necrosis.

• It is abnormal intracellular accumulation of triglycerides mostly in liver, heart, skeletal muscle and kidney • Causes- reduced apoprotein synthesis and fattyacid oxidation, accelerated lipolysis and disruption of mitochondrial function • Effects – fat vacuoles, enlargement of organ (fatty liver, tigered effect in heart)

2. Irreversible cell injury • Irreversible cell injury results in cell death by necrosis and apoptosis • Causes- Prolonged insult • Effects – disruption of physical integrity of cell membrane and organelles, calcification of cytoplasm and coagulation of proteins

• It is a pattern of cell death • Cause: Hypoxia, pathogens and Toxins • Necrotic cells are destroyed by phagocytes. If not they undergo calcification • Effect- Cell degeneration

Cytoplasmic changes in necrosis • • • Increases eosinophilia Glassy appearance Granular or vacuolated cytoplasm Swollen mitochondria Also calcification

Nuclear changes in necrosis • DNA degradation leads to 3 types of nuclear changes – Karyolysis – Psychosis – Karyorrhexis


Types of necrosis • Based on appearance and changes in necrotic cells necrosis is classified as follows – Coagulative necrosis : Free radicals / hypoxia – Liquifactive necrosis: Acids/alkalis, snake venom – Caseous necrosis : TB, fungal infections – Fat necrosis: Lipases


• Apoptosis is a form of ‘coordinated and internally programmed cell death’ having significance in a variety of physiological and pathological conditions Eg: Ø Destruction of implantation and developmental involution Ø Cell death in tumours Ø Deletion of auto reactive T cells in thymus Ø Cell killing by cytotoxic T cells Ø Endometrium during menstruation Ø Lactating breast after weaning


Biochemical changes in apoptosis Biochemical processes underlying the morphologic changes in apoptosis are: 1. Proteolysis of cytoskeletal proteins 2. Protein-protein cross linking 3. Fragmentation of nuclear chromatin by activation of nuclease 4. Appearance of phosphatidylserine on the outer surface of cell membrane 5. In some forms of apoptosis, appearance of an adhesive glycoprotein thrombospondin on the outer surface of apoptotic bodies

MOLECULAR MECHANISMS OF APOPTOSIS 1. Initiators of apoptosis Ø Ø Ø Transmembrane (absence of certain hormones, growth factors, cytokines) Extracellular (Heat, radiation, hypoxia) Intracellular (FAS receptor activation) 2. Process of programmed cell death Ø Ø Activation of caspases : Caspase 3, 9, 8, 12 etc… Activation of death receptors : FAS receptor Activtion of growth controlling genes : BCL-2 and p 53 Cell death 3. Phagocytosis

Contrasting features of Apoptosis and Necrosis



Ø Cells accumulate abnormal amounts of various substances which may be harmful to the cell. Ø The substance may be located in nucleus or within cytoplasm or within organelles (typically lysosomes).
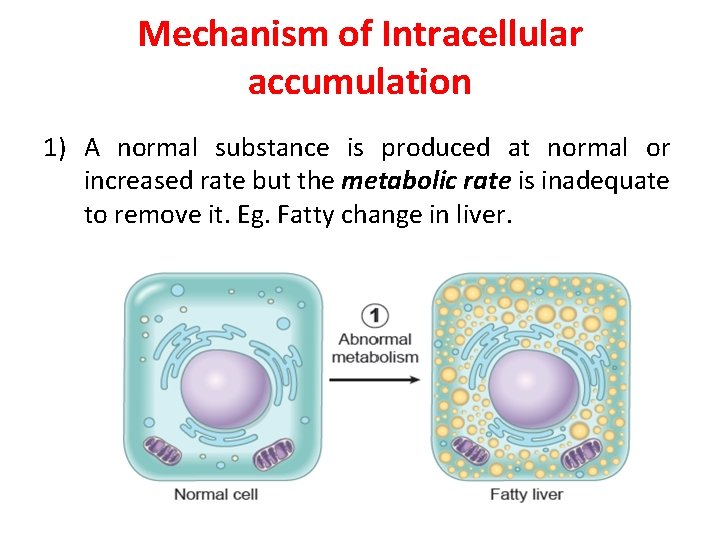
Mechanism of Intracellular accumulation 1) A normal substance is produced at normal or increased rate but the metabolic rate is inadequate to remove it. Eg. Fatty change in liver.
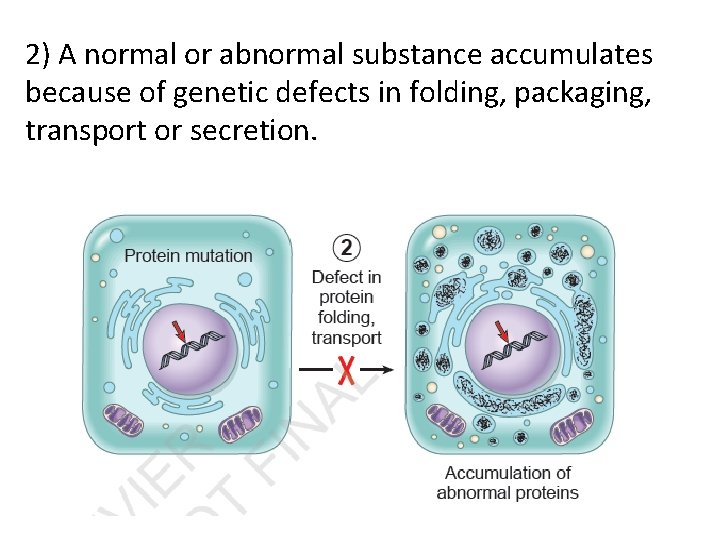
2) A normal or abnormal substance accumulates because of genetic defects in folding, packaging, transport or secretion.
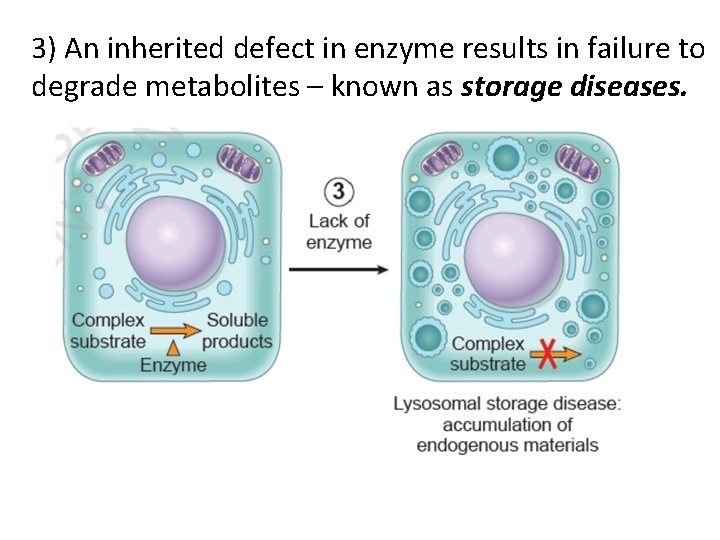
3) An inherited defect in enzyme results in failure to degrade metabolites – known as storage diseases.
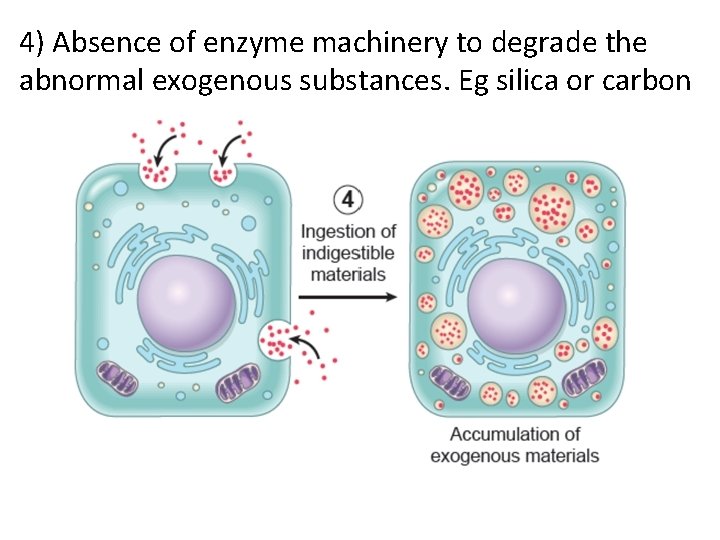
4) Absence of enzyme machinery to degrade the abnormal exogenous substances. Eg silica or carbon

Example of Intracellular accumulation Fatty change in liver (Steatosis) § It refers to any abnormal accumulations of triglycerides within cells. § Commonly seen in liver as it is the major organ of fat metabolism but also may occur in heart, kidneys, muscles. § Causes: Protein malnutrition, toxins (alcohol), diabetes mellitus, obesity.

Substances accumulated in the cell • • Cholesterol and cholesteryl esters Proteins Glycogen Pigments: lipofuscin, melanin, hemosiderin


v Calcification is the abnormal deposition of calcium salts together with small amounts iron, magnesium and other minerals. v 2 Types of Calcification 1) Dystrophic calcification- is calcium deposition in dead or dying tissues & occurs in the absence of calcium metabolic dearrangements ie. with normal serum levels of calcium. 2) Metastatic calcification- is calcium in normal tissues & occurs in dearrangements in calcium metabolism (hypercalcemia)


v. Normal body p. H=7. 4 & this level is very important for normal biological activity. v. On an average, the p. H range may fluctuate from 7. 35 -7. 45. v During normal metabolic activity, body produces both acid and bases but the acid production is greater than the base production.
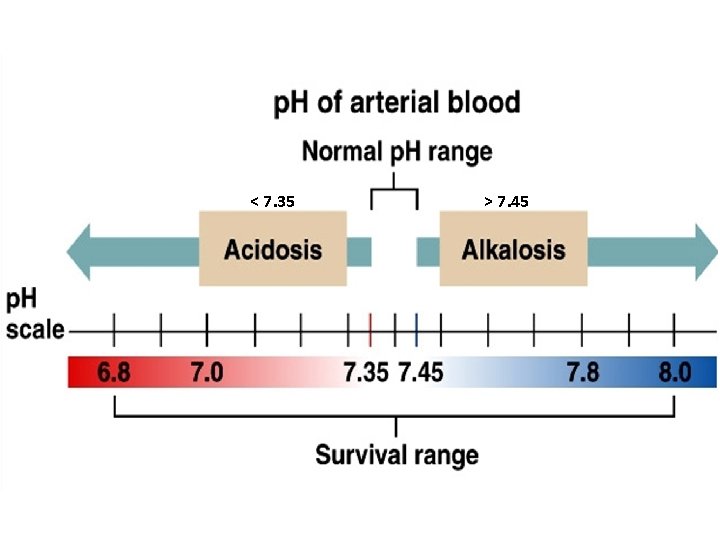
< 7. 35 > 7. 45


Metabolic acidosis • It is a fall in the blood p. H due to metabolic component which is brought about by fall in bicarbonate level and excess of H+ ions in the blood • It occurs in following conditions ØLactic acidosis ØDiabetes mellitus ØStarvation ØChronic renal failure ØAdministration of Ammonium chloride or acetazolamide

Metabolic alkalosis • It is a rise in the blood p. H due to rise in the bicarbonate levels of plasma and loss of H+ ions • It occurs in following conditions Ø Severe and prolonged vomiting Ø Administration of alkaline salts like sodium bicarbonate Ø Hypokalemia in cushing’s syndrome and increased secretion of aldosterone
- Slides: 87