BY REEJA RASHEED REEJA RASHEED 2002 BATCH 2002
BY REEJA RASHEED, REEJA RASHEED 2002 BATCH 2002 MBBS
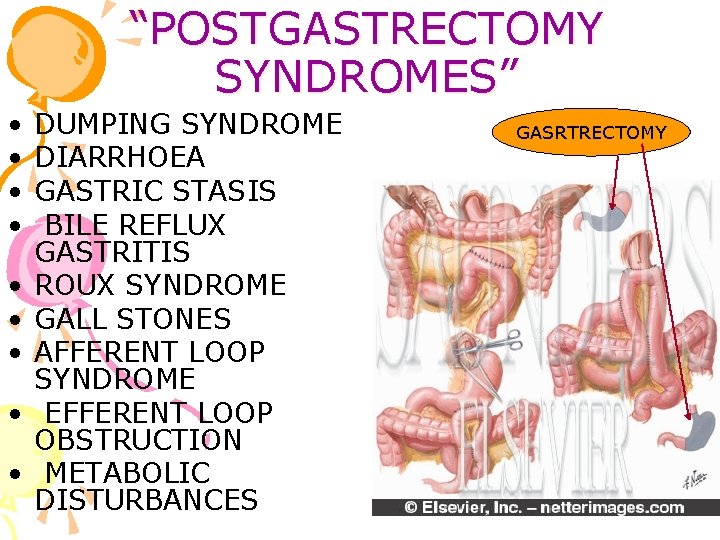
“POSTGASTRECTOMY SYNDROMES” • • • DUMPING SYNDROME DIARRHOEA GASTRIC STASIS BILE REFLUX GASTRITIS ROUX SYNDROME GALL STONES AFFERENT LOOP SYNDROME EFFERENT LOOP OBSTRUCTION METABOLIC DISTURBANCES GASRTRECTOMY
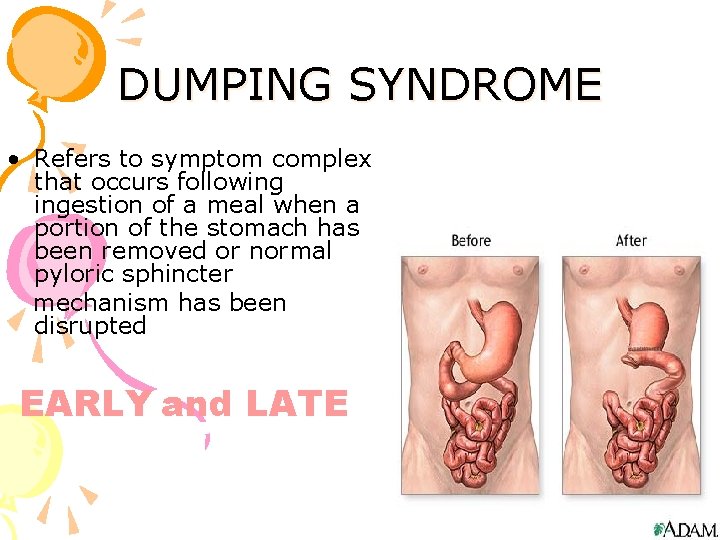
DUMPING SYNDROME • Refers to symptom complex that occurs following ingestion of a meal when a portion of the stomach has been removed or normal pyloric sphincter mechanism has been disrupted EARLY and LATE

EARLY DUMPING SYNDROME • 20 -30 MIN after food intake • Characterized by gastrointestinal and cardiovascular symptoms. • Cause : Rapid emptying of hyperosmolar food into small intestine cause fluid shift from intravascular compartment into intestinal lumen to maintain isotonicity. Luminal distension induce autonomic responses.
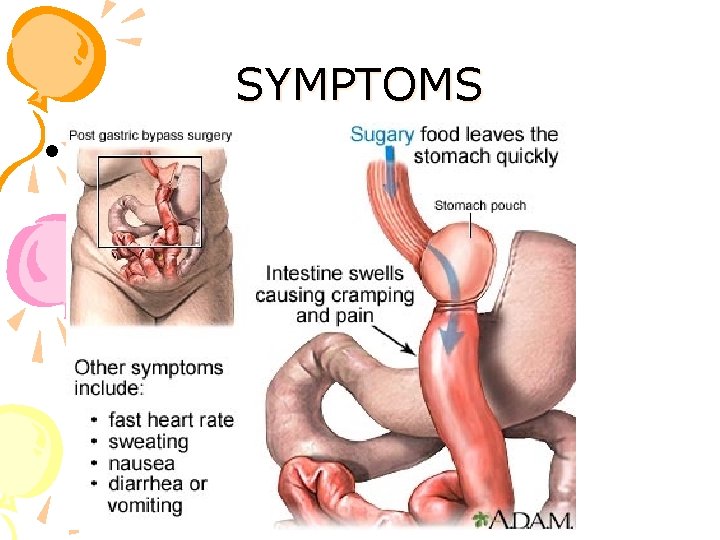
SYMPTOMS •
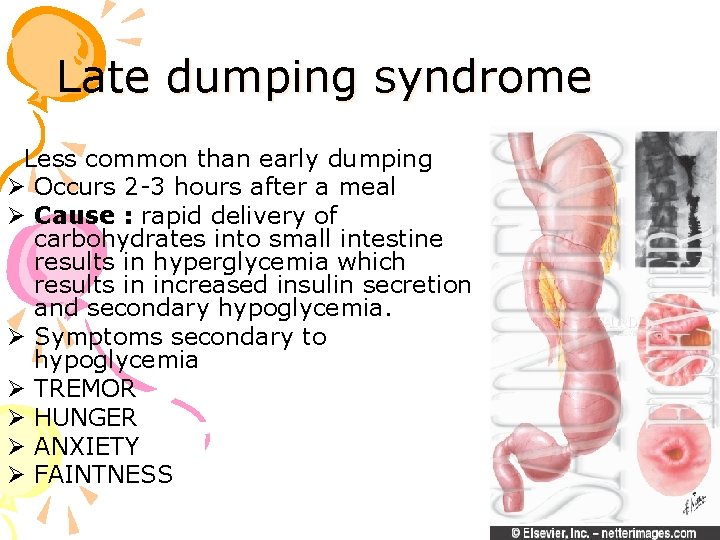
Late dumping syndrome Less common than early dumping Ø Occurs 2 -3 hours after a meal Ø Cause : rapid delivery of carbohydrates into small intestine results in hyperglycemia which results in increased insulin secretion and secondary hypoglycemia. Ø Symptoms secondary to hypoglycemia Ø TREMOR Ø HUNGER Ø ANXIETY Ø FAINTNESS

TREATMENT • MEDICAL THERAPY • 1)DIETARY MANAGEMENT * Avoid food containing large amounts of sugar, *Frequent feeding of small meals rich in protein and fat *Avoid liquids during meals

• • 2)DRUGS OCTREOTIDE-somatostatin analogue 100 microgm subcutaneously twice daily can be increased to 500 microgm twice daily • ACARBOSE (alpha glucosidase inhibitor) delays carbohydrate absorption. • *used in late dumping syndrome
![SURGERY • When conservative JEJUNAL SEGMENT measures fail • 1] Interposing isoperistaltic or antiperistaltic SURGERY • When conservative JEJUNAL SEGMENT measures fail • 1] Interposing isoperistaltic or antiperistaltic](http://slidetodoc.com/presentation_image/3700faa1bb31fcdc1bc092d3bdce8ac1/image-9.jpg)
SURGERY • When conservative JEJUNAL SEGMENT measures fail • 1] Interposing isoperistaltic or antiperistaltic 10 -20 cm jejunal segment between stomach and small bowel.
![SURGERY • 2]ROUX-en. Y GASTROJEJUNOST OMY • Done in • severe dumping following gastric SURGERY • 2]ROUX-en. Y GASTROJEJUNOST OMY • Done in • severe dumping following gastric](http://slidetodoc.com/presentation_image/3700faa1bb31fcdc1bc092d3bdce8ac1/image-10.jpg)
SURGERY • 2]ROUX-en. Y GASTROJEJUNOST OMY • Done in • severe dumping following gastric resection Roux-en Y Gastrojejunostomy

DIARRHOEA • CAUSES • 1. Truncal vagotomy • 2. Dumping • 3. Malabsorption • POSTVAGOTOMY DIARRHOEA • Incidence – 30 -70% following truncal vagotomy
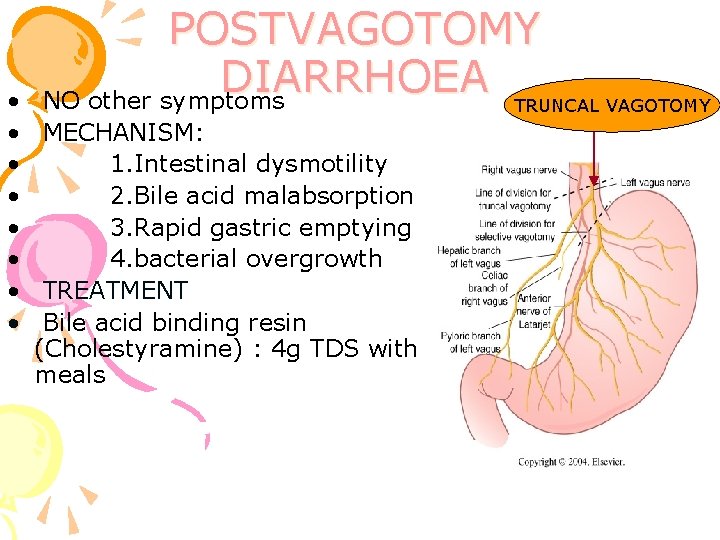
POSTVAGOTOMY DIARRHOEA NO other symptoms TRUNCAL VAGOTOMY • • MECHANISM: • 1. Intestinal dysmotility • 2. Bile acid malabsorption • 3. Rapid gastric emptying • 4. bacterial overgrowth • TREATMENT • Bile acid binding resin (Cholestyramine) : 4 g TDS with meals
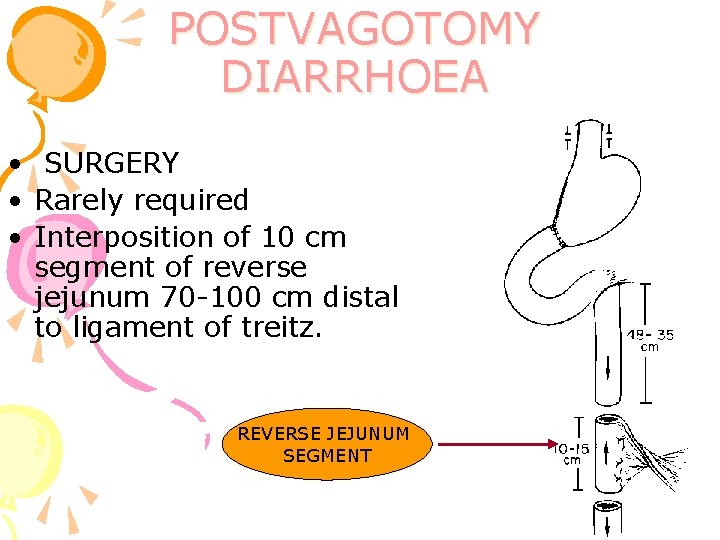
POSTVAGOTOMY DIARRHOEA • SURGERY • Rarely required • Interposition of 10 cm segment of reverse jejunum 70 -100 cm distal to ligament of treitz. REVERSE JEJUNUM SEGMENT

BILE REFLUX GASTRITIS Ø Due to reflux of bile into stomach Ø SYMPTOMS Ø Abdominal pain Ø Biliousvomiting Ø weight loss Ø More common after BILLROTH 2 GASTRECTOMY Ø LEAST after vagotomy &pyloroplasty
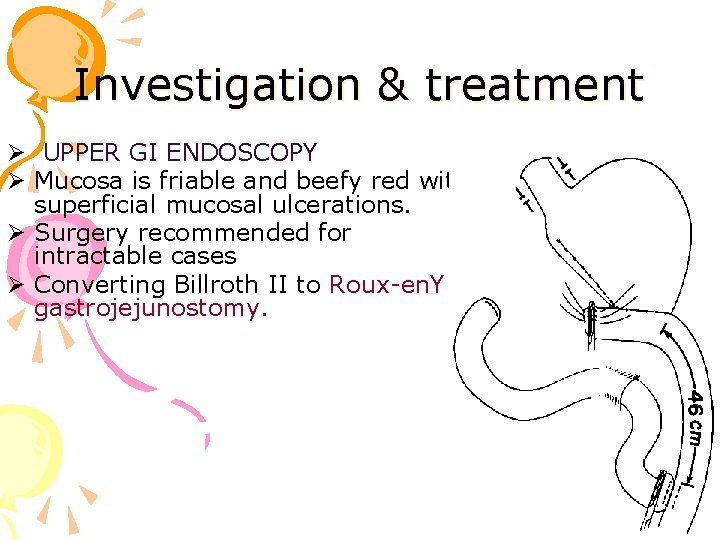
Investigation & treatment Ø UPPER GI ENDOSCOPY Ø Mucosa is friable and beefy red with superficial mucosal ulcerations. Ø Surgery recommended for intractable cases Ø Converting Billroth II to Roux-en. Y gastrojejunostomy.

TREATMENT • Interposition of a 40 cm isoperistaltic jejunal loop between gastric remnant and duodenum • BILLROTHIIGASTROJEJUNOSTOMY with BRAUNenterostomy

GASTRIC STASIS • CAUSES • Problem with gastric motor function • Obstruction: 1. Mechanical{anastomotic stricture} 2. Functional{retrograde peristalsis in a roux limb} • Due to deliberate or unintentional vagotomy
![SYMPTOMS & EVALUATION • • VOMITING[undigested food] EPIGASTRIC PAIN BLOATING WEIGHT LOSS Evaluation: 1. SYMPTOMS & EVALUATION • • VOMITING[undigested food] EPIGASTRIC PAIN BLOATING WEIGHT LOSS Evaluation: 1.](http://slidetodoc.com/presentation_image/3700faa1bb31fcdc1bc092d3bdce8ac1/image-18.jpg)
SYMPTOMS & EVALUATION • • VOMITING[undigested food] EPIGASTRIC PAIN BLOATING WEIGHT LOSS Evaluation: 1. Endoscopy 2. Upper GI SERIES 3. Gastric emptying scan

• endoscopy shows gastritis &retained food or BEZOARS #67 year-old man with post -surgical gastroparesis, having undergone partial gastrectomy several years previously. Phytobezoar found at endoscopy. The gastric outlet was widely patent.
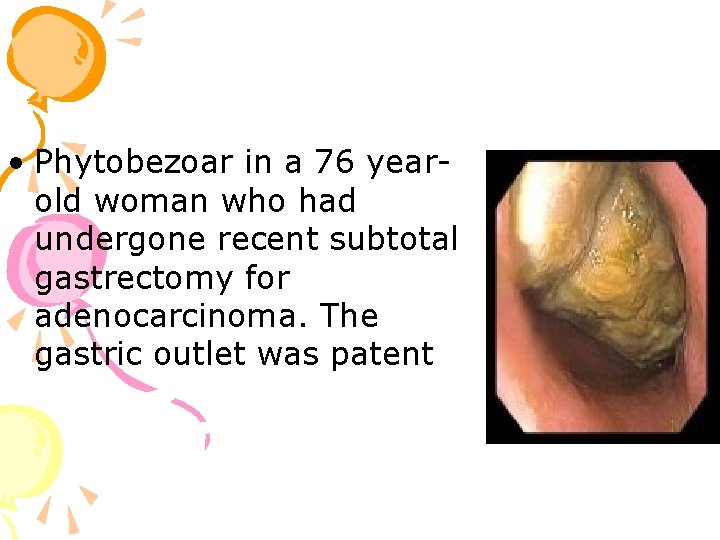
• Phytobezoar in a 76 yearold woman who had undergone recent subtotal gastrectomy for adenocarcinoma. The gastric outlet was patent

TREATMENT MEDICAL USED IN 1. Motor dysfunction following surgery 2. When mechanical obstruction has been ruled out TREATMENT INCLUDES: 1. Dietary modification 2. Promotility agent 3. Intermitten oral antibiotic

SURGICAL TREATMENT • In Gastric Stasis following VAGOTOMY & DRAINAGE • *SUBTOTAL GASTRECTOMY{75%} • Following SUBTOTAL GASTRIC resection • *NEAR TOTAL RESECTION{95%} • *TOTAL GASTRECTOMY & ROUX-en-Y reconstruction • Following ULCER SURGERY • anastomotic stricture • *ENDOSCOPIC DILATATION

TOTAL GASTRECTOMY

ROUX SYNDROME • patients who have had distal gastrectomy and ROUX-en-Y gastrojejunostomy have difficulty with gastric emptying in the absence of mechanical obstruction • SYMPTOMS • 1. VOMITING • 2. EPIGASTRIC PAIN • 3. WEIGHT LOSS

INVESTIGATIONS • ENDOSCOPY: • 1. BEZOARformation • 2. Dilatation of gastric remnant • 3. dilatation of roux limb • CONFIRMED BY UPPER GI SERIES • shows delayed Gastric MOTILITY • GASTROINTESTINAL MOTILITY TEST • abnormal motility in the ROUX limb with propulsive activity towards stomach

TREATMENT • MEDICAL • Promotility agents • SURGICAL • 1. Paring down the gastric remnant • 2. 95% Gastrectomy • 3. ROUX limb is resected{if dilated & flaccid} and continuity re-established with • a] another ROUX • b] Billroth. II with Braun • c] Henley Loop
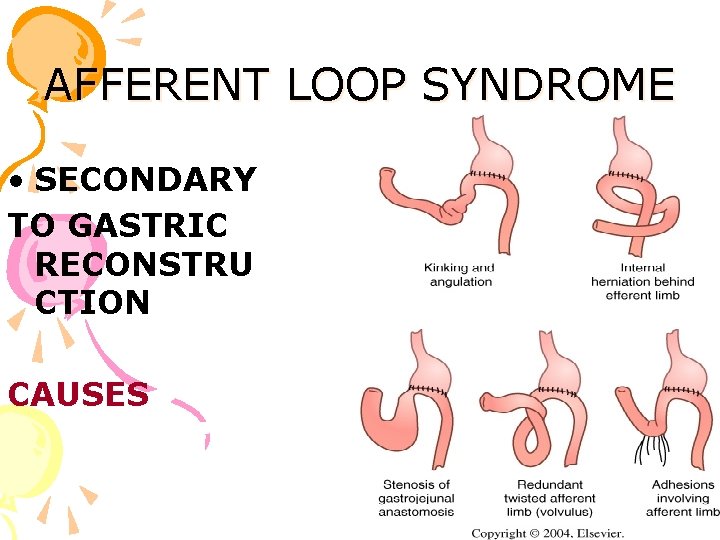
AFFERENT LOOP SYNDROME • SECONDARY TO GASTRIC RECONSTRU CTION CAUSES

• Afferent loop syndrome usually occurs when the afferent limb is longer than 30 -40 cm and anastomosed to stomach in an antecolic fashion. • Characterized by bilious vomiting without food.
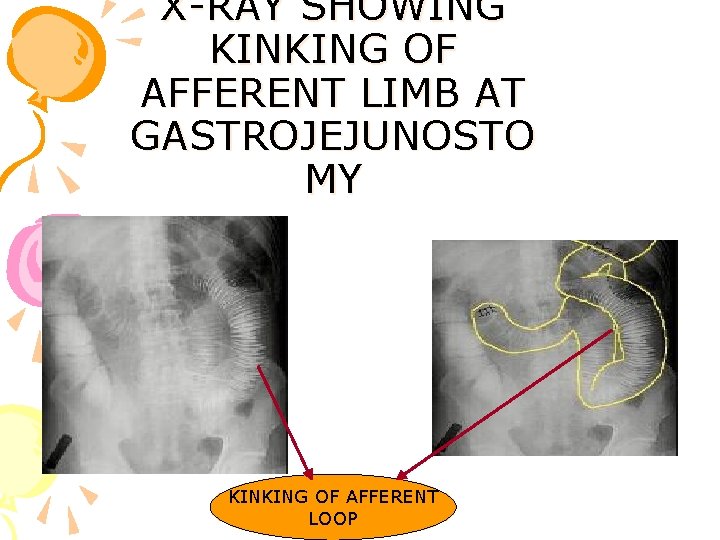
X-RAY SHOWING KINKING OF AFFERENT LIMB AT GASTROJEJUNOSTO MY KINKING OF AFFERENT LOOP
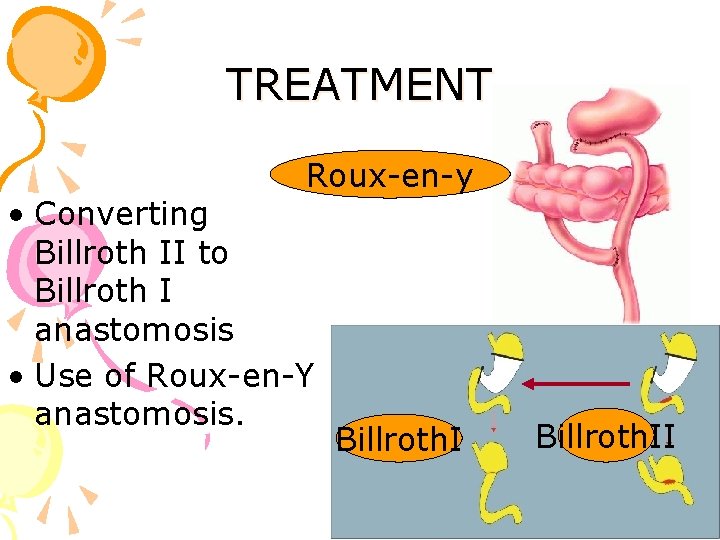
TREATMENT Roux-en-y • Converting Billroth II to Billroth I anastomosis • Use of Roux-en-Y anastomosis. Billroth. II

BILLROTH I & II ROUX-EN-Y BRAUN ENTEROENT EROSTOMY

EFFERENT LOOP SYNDROME Ø Most common cause : herniation of the limb behind the anastomosis in a right to left fashion. Ø Usually occurs within first post-op month Ø Characterized by abdominal pain, bilious vomiting and abdominal distension
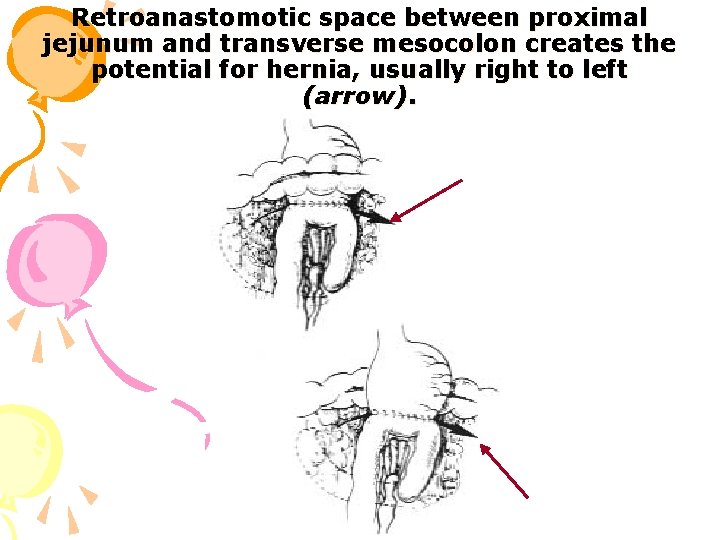
Retroanastomotic space between proximal jejunum and transverse mesocolon creates the potential for hernia, usually right to left (arrow).

EFFERENT LOOP SYNDROME Ø Diagnosis : Ø Barium meal : Contrast fails to enter efferent loop. Ø Treatment : Reducing retroanastomotic hernia and closing retroanastomotic space to prevent recurrence.
GALLSTONES CAUSE: VAGAL DENERVATION GALLBLADDER DYSMOTILITY STASIS OF BILE GALLSTONES

OTHER CAUSES • POST OPERATIVE AMPULLARYDYSFUNCTION • CHANGES IN BILE • TREATMENT CHOLECYSTECTOMY Done along with gastrectomy 1. gall bladder appears abnormal 2. stones on pre/intra operative evaluation

METABOLIC DISTURBANCES Ø Anemia : Iron deficiency or megaloblastic anemia secondary to B 12 deficiency. Ø Fat malabsorption and steatorrhoea (common after Billroth II reconstruction) due to inadequate mixing of bile salts and pancreatic lipase with ingested fat secondary to duodenal bypass. Ø Hypocalcemia : Due to precipitation of calcium by unabsorbed fatty acids.

OTHER COMPLICATIONS…. . • Some complications which occur in the immediate post op period • 1. HAEMORRHAGE • 2. ANASTOMOTIC LEAK • HAEMORRHAGE *occurs from the suture line

OTHER COMPLICATIONS…. . *continuous gastric lavage with 1 ml 1: 1000 adrenalin stops bleeding *blood transfusion *abdomen reopened &suture reinforced{if bleeding persists} *stomach opened & actual bleeding points are under run

OTHER COMPLICATIONS ANASTOMOTIC LEAK *occur in up to 20% of patients after upper gastrointestinal surgery *represent a significant source of postoperative morbidity and mortality. • breakdown of a suture line in a surgical anastomosis with leakage of gastric or intestinal fluid
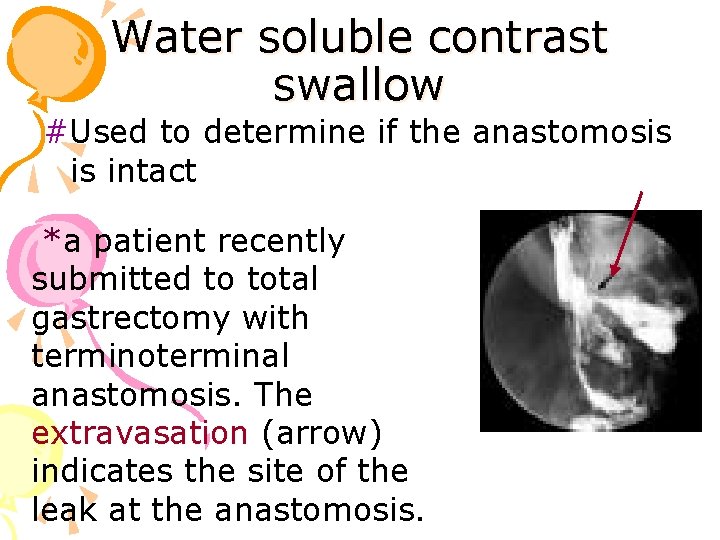
Water soluble contrast swallow #Used to determine if the anastomosis is intact *a patient recently submitted to total gastrectomy with terminoterminal anastomosis. The extravasation (arrow) indicates the site of the leak at the anastomosis.
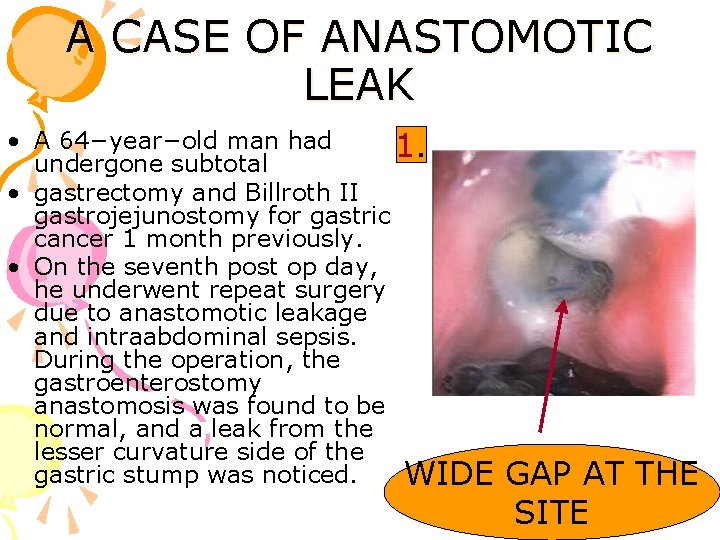
A CASE OF ANASTOMOTIC LEAK • A 64−year−old man had 1. undergone subtotal • gastrectomy and Billroth II gastrojejunostomy for gastric cancer 1 month previously. • On the seventh post op day, he underwent repeat surgery due to anastomotic leakage and intraabdominal sepsis. During the operation, the gastroenterostomy anastomosis was found to be normal, and a leak from the lesser curvature side of the gastric stump was noticed. WIDE GAP AT THE SITE
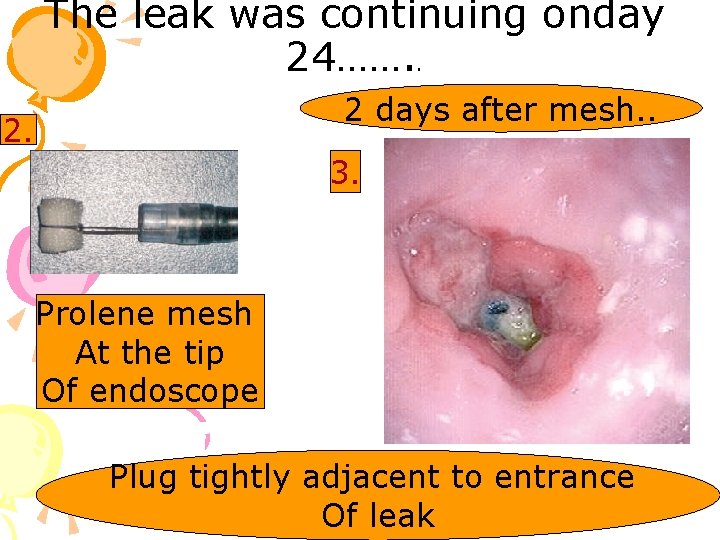
The leak was continuing onday 24……. . 2 days after mesh. . 2. 3. Prolene mesh At the tip Of endoscope Plug tightly adjacent to entrance Of leak
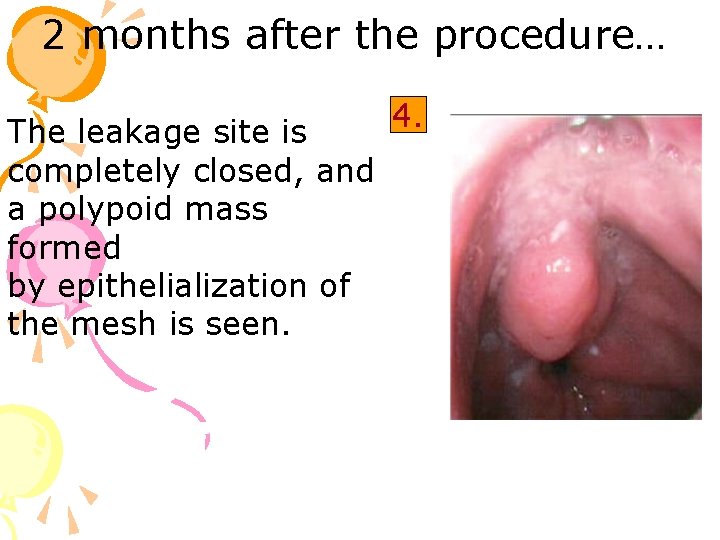
2 months after the procedure… The leakage site is completely closed, and a polypoid mass formed by epithelialization of the mesh is seen. 4.
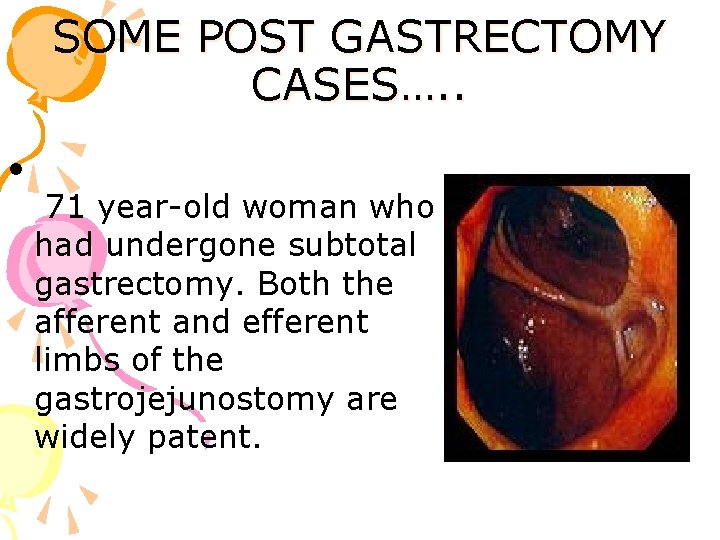
SOME POST GASTRECTOMY CASES…. . • 71 year-old woman who had undergone subtotal gastrectomy. Both the afferent and efferent limbs of the gastrojejunostomy are widely patent.
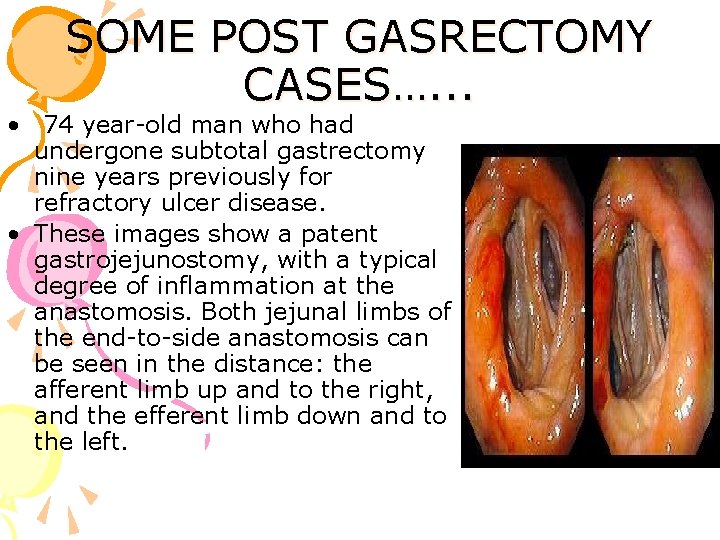
SOME POST GASRECTOMY CASES…. . . • 74 year-old man who had undergone subtotal gastrectomy nine years previously for refractory ulcer disease. • These images show a patent gastrojejunostomy, with a typical degree of inflammation at the anastomosis. Both jejunal limbs of the end-to-side anastomosis can be seen in the distance: the afferent limb up and to the right, and the efferent limb down and to the left.
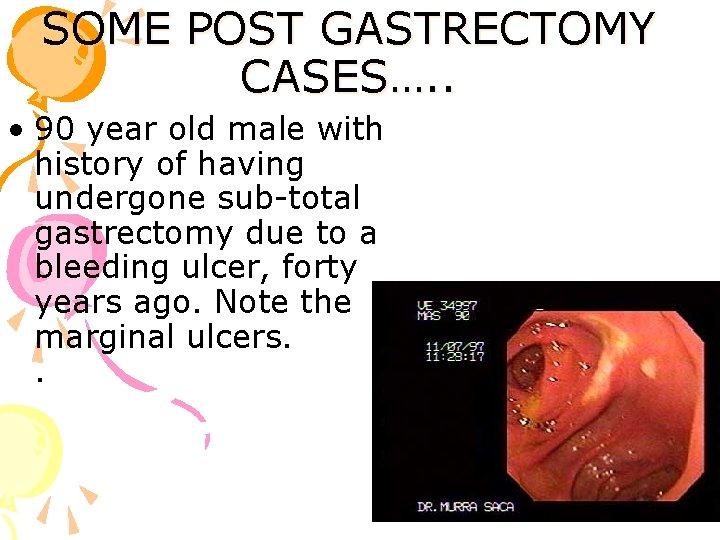
SOME POST GASTRECTOMY CASES…. . • 90 year old male with history of having undergone sub-total gastrectomy due to a bleeding ulcer, forty years ago. Note the marginal ulcers. .
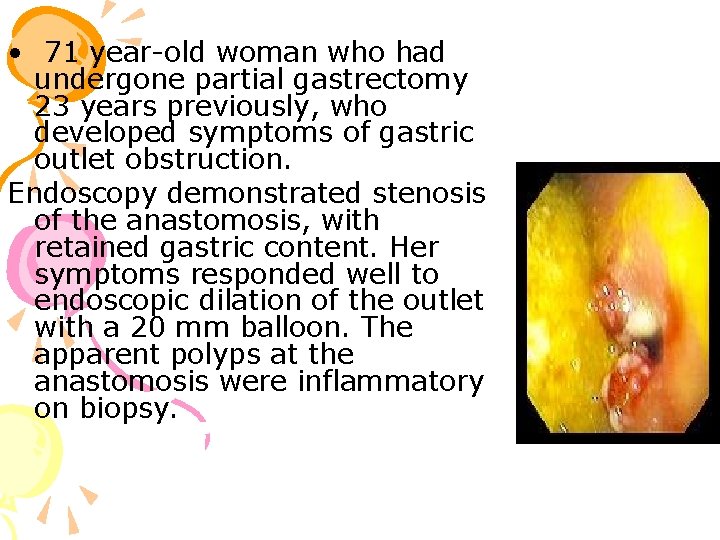
• 71 year-old woman who had undergone partial gastrectomy 23 years previously, who developed symptoms of gastric outlet obstruction. Endoscopy demonstrated stenosis of the anastomosis, with retained gastric content. Her symptoms responded well to endoscopic dilation of the outlet with a 20 mm balloon. The apparent polyps at the anastomosis were inflammatory on biopsy.
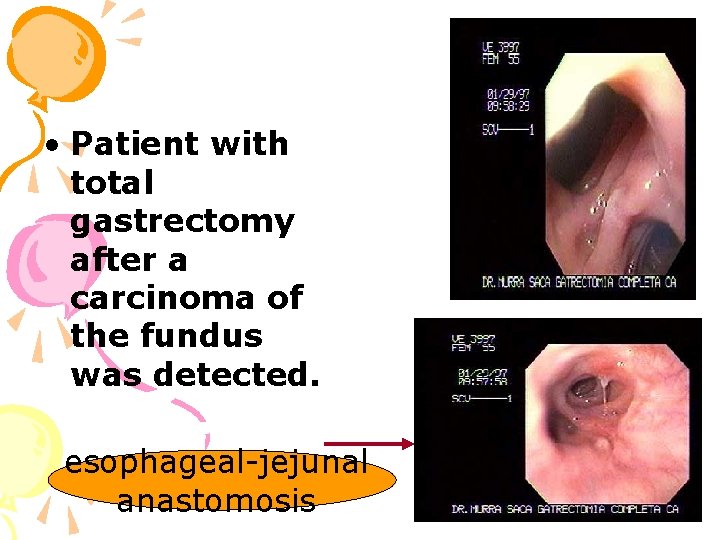
• Patient with total gastrectomy after a carcinoma of the fundus was detected. esophageal-jejunal anastomosis

- Slides: 50