By Agnes Wojdyla Samantha Valerio Kathleen Valerio Each

By: Agnes Wojdyla, Samantha Valerio, & Kathleen Valerio
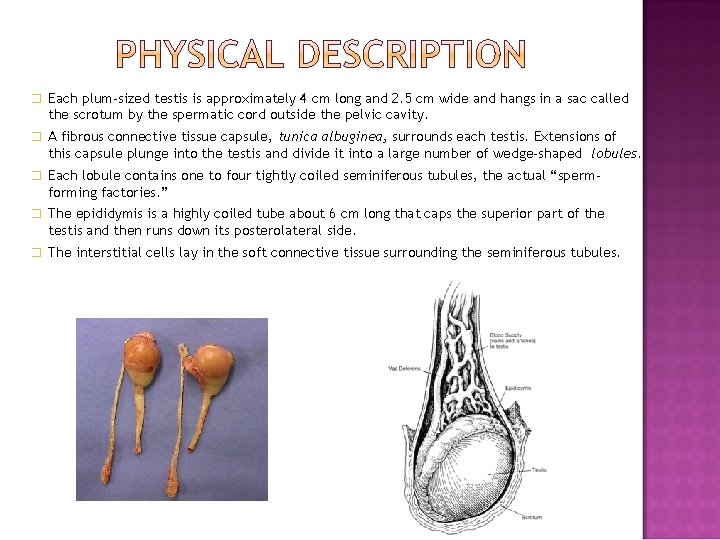
� Each plum-sized testis is approximately 4 cm long and 2. 5 cm wide and hangs in a sac called the scrotum by the spermatic cord outside the pelvic cavity. � A fibrous connective tissue capsule, tunica albuginea, surrounds each testis. Extensions of this capsule plunge into the testis and divide it into a large number of wedge-shaped lobules. � Each lobule contains one to four tightly coiled seminiferous tubules, the actual “sperm- forming factories. ” � The epididymis is a highly coiled tube about 6 cm long that caps the superior part of the testis and then runs down its posterolateral side. � The interstitial cells lay in the soft connective tissue surrounding the seminiferous tubules.
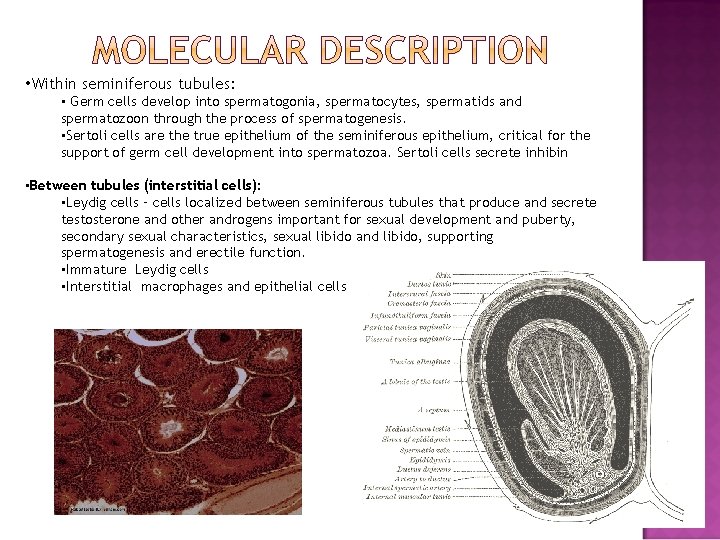
• Within seminiferous tubules: • Germ cells develop into spermatogonia, spermatocytes, spermatids and spermatozoon through the process of spermatogenesis. • Sertoli cells are the true epithelium of the seminiferous epithelium, critical for the support of germ cell development into spermatozoa. Sertoli cells secrete inhibin • Between tubules (interstitial cells): • Leydig cells – cells localized between seminiferous tubules that produce and secrete testosterone and other androgens important for sexual development and puberty, secondary sexual characteristics, sexual libido and libido, supporting spermatogenesis and erectile function. • Immature Leydig cells • Interstitial macrophages and epithelial cells

� Testosterone – � A steroid hormone in the androgen group which is the most important hormonal product of the testes testosterone � Necessary for normal and continuous sperm production � Plays a key role in the male reproductive tissues such as the testes and prostate as well as promoting secondary sexual characteristics such as increased muscle and bone mass and hair growth � On average, an adult human male body produces about forty to sixty times more testosterone than an adult human female body, but females are, from a behavioral perspective (rather than from an anatomical or biological perspective), more sensitive to the hormone. � Luteinizing hormone (Lutropin)� Hormone produced by the anterior pituitary gonadotropins � Essential for reproduction in both males and females � In males, this hormone is also called the Interstitial Cell Stimulating Hormone (ICSH) � Binds to receptors on Leydig cells, stimulating synthesis and secretion of testosterone � Follicle-stimulating hormone – � Hormone also produced by the anterior pituitary gonadotropins � Along with LH, it is critical for sperm production. It supports the function of Sertoli cells, which in turn support many aspects of sperm cell maturation. Follicle-stimulating hormone

� Formation of sperm through spermatogenesis (sperm production) that begins during puberty and continues throughout life. � Stages of Spermatogenesis: � - Spermacytogenesis- spermatogonia (primitive stem cells) go through rapid mitotic dvisions to build up the stem cell line - Spermatidogenesis- the creation of spermatids from secondary spermatocytes. Secondary spermatocytes produced earlier rapidly enter meiosis II and divide to produce haploid spermatids. The brevity of this stage means that secondary spermatocytes are rarely seen in histological preparations - Spermiogenesis- last stage of sperm development; Transformation of a spermatid into a spermatozoon. Producing male sex hormones (testosterone- vital to the normal development of male physical characteristics such as growth of facial hair, development of heavy bones and muscles, and lowering of the voice) through the interstitial cells

�Pituitary Gland- This gland provides hormones to the testes to help with its functions. The anterior pituitary gland secretes increasing amounts of folliclestimulating hormone (FSH) (which induces the formation of sperm) and also luteinizing hormone (LH) (which activates the interstitial cells that produce testosterone).
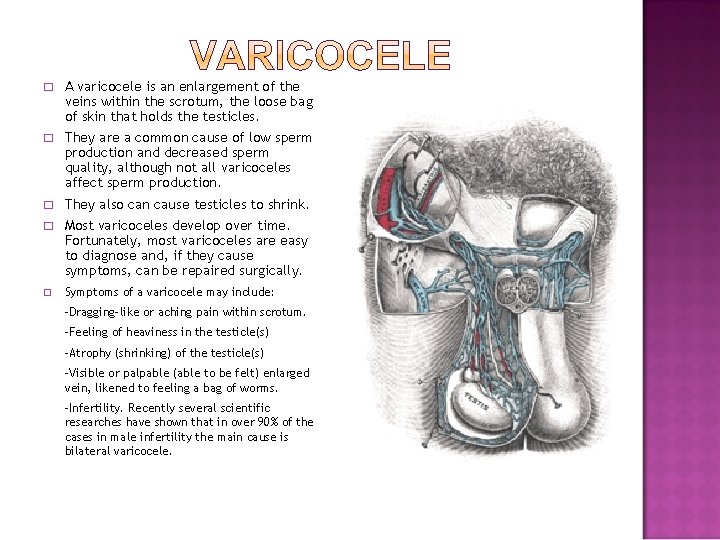
� A varicocele is an enlargement of the veins within the scrotum, the loose bag of skin that holds the testicles. � They are a common cause of low sperm production and decreased sperm quality, although not all varicoceles affect sperm production. � They also can cause testicles to shrink. � Most varicoceles develop over time. Fortunately, most varicoceles are easy to diagnose and, if they cause symptoms, can be repaired surgically. � Symptoms of a varicocele may include: -Dragging-like or aching pain within scrotum. -Feeling of heaviness in the testicle(s) -Atrophy (shrinking) of the testicle(s) -Visible or palpable (able to be felt) enlarged vein, likened to feeling a bag of worms. -Infertility. Recently several scientific researches have shown that in over 90% of the cases in male infertility the main cause is bilateral varicocele.

Hypogonadism in men is a disorder that occurs when the testicles (gonads) do not produce enough testosterone. Primary hypogonadism occurs when there is a problem or abnormality in the testicles themselves. Secondary hypogonadism occurs when there is a problem with the pituitary gland in the brain, which sends chemical messages to the testicles to produce testosterone. Hypogonadism can occur during fetal development, at puberty, or in adult men. Symptoms include: erectile dysfunction, infertility, impaired growth of the penis and testicles Treatment for hypogonadism depends on the cause. Male hormone replacement (testosterone replacement therapy or TRT) often is used to treat disorders of the testicles. If the problem is related to the pituitary gland, pituitary hormones may help increase testosterone levels and sperm production.
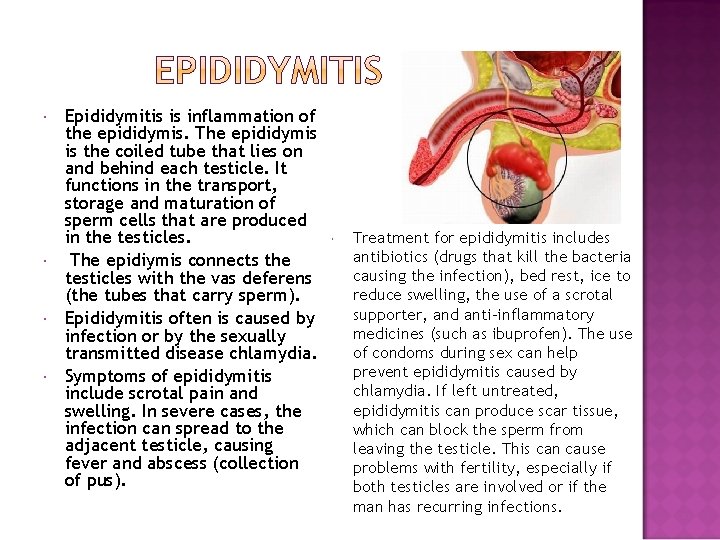
Epididymitis is inflammation of the epididymis. The epididymis is the coiled tube that lies on and behind each testicle. It functions in the transport, storage and maturation of sperm cells that are produced in the testicles. The epidiymis connects the testicles with the vas deferens (the tubes that carry sperm). Epididymitis often is caused by infection or by the sexually transmitted disease chlamydia. Symptoms of epididymitis include scrotal pain and swelling. In severe cases, the infection can spread to the adjacent testicle, causing fever and abscess (collection of pus). Treatment for epididymitis includes antibiotics (drugs that kill the bacteria causing the infection), bed rest, ice to reduce swelling, the use of a scrotal supporter, and anti-inflammatory medicines (such as ibuprofen). The use of condoms during sex can help prevent epididymitis caused by chlamydia. If left untreated, epididymitis can produce scar tissue, which can block the sperm from leaving the testicle. This can cause problems with fertility, especially if both testicles are involved or if the man has recurring infections.

- Slides: 10