Bursitis What is a Bursa A bursa is

Bursitis

What is a Bursa? • A bursa is a soft, fluid-filled closed sac lined with a synovial-like membrane that sometimes contains fluid that develops in the area and is subject to pressure or friction.

What is a Bursa? • Purpose: – Decrease friction by cushioning muscles or tendons and bones that move back and forth across each other – These are typically thin, but may become thickened and fluid-filled with increased stress

What is Bursitis? • Bursitis is an inflammation of a bursa. • Bursitis is characterized by a painful inflammation or irritation of the soft, fluid -filled sac that covers and cushions the movement between the bones, tendons, and muscles near the joints.

Types of Bursitis

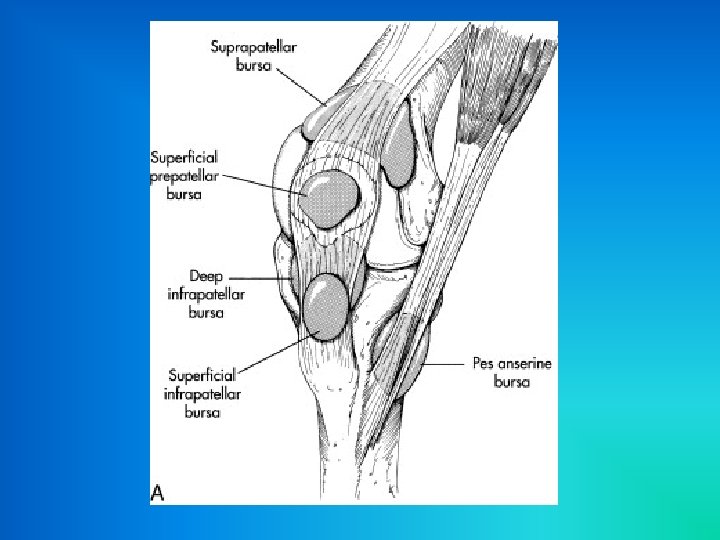
Suprapatellar Bursitis • The bursa is located directly above the knee • The bursa is not a true bursa but rather is an extension of the tibiofemoral joint capsule • Inflammation of this bursa usually results from a mechanical irritation during kneeling activities – Commonly referred to as “Nun’s Knee”

Prepatellar Bursitis • The bursa is located anterior to the patellar tendon • Characterized by swelling with effusion of the superficial bursa overlying the lower pole of the patella • This type of bursitis is caused by injury to the anterior knee, such as a fall directly onto the patella – Commonly referred to as “Housemaid’s Knee”
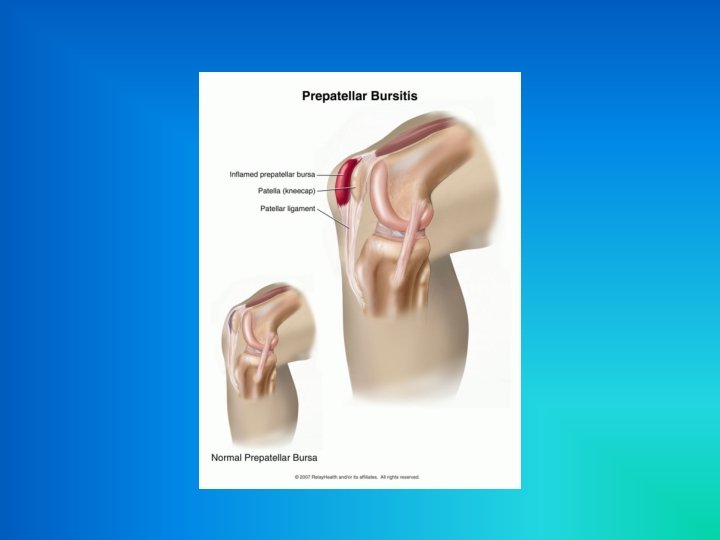

Infrapatellar Bursitis • The bursa is located between the tuberosity of the tibia and the patellar tendon and is separated from the synovium of the knee by a pad of fat

Anserine Bursitis • The bursa separates the Pes Anserinus from the distal portion of the MCL and the medial femoral condyle • Involves pain and tenderness at proximal medial tibia • Characterized by sudden onset of knee pain with localized tenderness and swelling at Pes Anserinus

Causes of Bursitis: • Overuse • Direct blow to the knee • Repeated stress – i. e. repetitive kneeling • Infection

Patient population affected by Bursitis: • It frequently develops based on the patient’s occupation, not sports. • Commonly occurs from overuse injuries – i. e. runners, wrestling, volleyball • Commonly occurs in obese women in association with osteoarthritis

Diagnosis • Radiographic imaging may reveal tissue swelling • Ultrasound imaging may detect fluid collection • MRI may be helpful but is not required on an urgent basis

Clinical Presentation • Localized tenderness with pain on pressure against bursa • Swelling • Restricted internal or external rotation • Joint movement that is accompanied by pain • Referred pain • Palpable occasional fibro-cartilaginous bodies
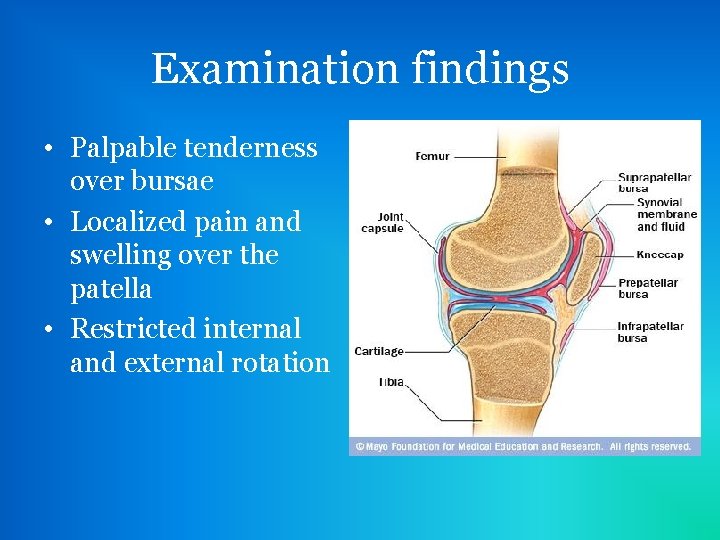
Examination findings • Palpable tenderness over bursae • Localized pain and swelling over the patella • Restricted internal and external rotation

Goals of Treatment • Reduce pain levels • Reduce inflammation and swelling • Return patient to normal activities as soon as possible without risk for further injury

Non-operative Treatment

Two types of Bursitis Treatment • Bacterial: – Involves antibiotic treatment with operative drainage • Inflammatory: – Involves ice, rest, anti-inflammatories, injection of corticosteriods

Physical Therapy • Strengthening exercises – Focus on Isometrics • Stretching exercises – Focus on Quadriceps, Hamstrings, Gastrocnemius

Modalities • RICE therapy (Rest, Ice, Compression, Elevation) – Used to control pain and swelling • Compression dressings – Used to control the level of swelling around the knee • Knee protection pads – Use with certain sports/activities that perform repetitive motions • i. e volleyball, wrestling, construction worker

Pharmacology • Anti-inflammatory medications – Used to control pain and inflammation • Non-steroidal anti-inflammatory medications – Used to control inflammation • Corticosteroid injections – Used to help reduce swelling of the bursa

Operative Treatment

Surgery • Various surgical procedures for treating Bursitis: – Aspiration and injection of drugs – Incision and drainage when acute bursitis fails to respond to nonsurgical treatment – Excision of chronically infected and thickened bursae – Removal of underlying bony prominence

Recommendations • Avoid direct blows to the kneecap • Avoid prolonged kneeling • Use proper protective kneepads to help prevent inflammation of the bursae • Take your time with return to normal activities. – Returning too soon may worsen the injury • Note: The longer you have symptoms before you start treatment, the longer it will take to recover

Resources • Ferri: Ferri’s Clinical Advisor 2011, 1 st Edition. Copyright © 2010 Mosby, An Imprint of Elsevier. • Lazoff, Marie. First Consult. Elseiver Inc. Copyright © 2011 • Marx: Rosen’s Emergency Medicine, 7 th Edition. Copyright © 2009 Mosby, An Imprint of Elsevier. • Dutton M. Orthopaedic Examination, Evaluation, and Intervention. 2 nd Edition 2008. • De. Lee: De. Lee and Drez’s Orthopaedic Sports Medicine, 3 rd Edition. Copyright © 2009 Saunders, An Imprint of Elsevier.
- Slides: 26