Bursitis Tendonitis Fibromyalgia Objectives 1 Explain how bursitis

Bursitis, Tendonitis, Fibromyalgia

Objectives 1. Explain how bursitis and tendonitis are similar 2. Explain how bursitis and tendonitis differ from another 3. List phases in development and healing of bursitis and tendonitis

Objectives 4. List common types of bursitis and tendonitis found at the: u Shoulder u Elbow u Wrist u. Hip u. Knee u. Ankle 5. List indications / contraindications for injection therapy of bursitis and tendonitis

Objectives 6. Describe typical findings in a patient with fibromyalgia 7. Describe typical findings in a patient with reflex sympathetic dystrophy

Sports • • Society more athletic Physical activity health benefits Overuse syndromes increase 25% to 50% of participants will experience tendonitis or bursitis

Workplace Musculoskeletal disorders from… …repetitive motions …localized contact stress …awkward positions …vibrations …forceful exertions • Ergonomic design incidence

Bursae • • • Closed, round, flat sacs Lined by synovium May or may not communicate with synovial cavity • Occur at areas of friction between skin and underlying ligaments / bone

Bursae • Permit lubricated movement over areas of potential impingement • Many are nameless • ~78 on each side of body • New bursae may form anywhere from frequent irritation

Bursitis Inflamed by… …chronic friction …trauma …crystal deposition …infection …systemic disease: rheumatoid arthritis, psoriatic arthritis, gout ankylosing spondylitis

Bursitis • Inflammation causes bursal synovial cells to thicken • Excess fluid accumulates inside and around affected bursae

Tendons • Tendon sheaths composed of same synovial cells as bursae • Inflamed in similar manner • Tendonitis: inflammation of tendon only • Tenosynovitis: inflammation of tendon plus its sheath

Tendons • Inflammatory changes involving sheath well documented • Inflammatory lesions of tendon alone not well documented • Distinction uncertain: terms tendonitis and tenosynovitis used interchangeably

Tendons • Most overuse syndromes are NOT inflammatory • Biopsy: no inflammatory cells • High glutamate concentrations • NSAIDs / steroids: no advantage • Tendon. ITIS a misnomer

Bursitis / Tendonitis • Most common causes: mechanical overload and repetitive microtrauma • Most injuries multifactorial

Bursitis / Tendonitis • Intrinsic factors: malalignment, poor muscle flexibility, muscle weakness or imbalance • Extrinsic factors: design of equipment or workplace and excessive duration, frequency, or intensity of activity

Immediate Phase • Release of chemotactic and vasoactive chemical mediators • Vasodilation and cellular edema • PMNs perpetuate process • Lasts 48 hours to 2 weeks • Repetitive insults prolong inflammatory stage

Healing Phase • Classic inflammatory signs: pain, warmth, erythema, swelling • Healing goes through proliferative and maturation • 6 to 12 weeks: organization and collagen cross-linking mature to preinjury strength

History • Changes in sports activity, work activities, or workplace • Cause not always found • Pregnancy, quinolone therapy, connective tissue disorders, systemic illness

History • • • Most common complaint: PAIN Acute or chronic Frequently more severe after periods of rest • May resolve quickly after initial movement only to become throbbing pain after exercise
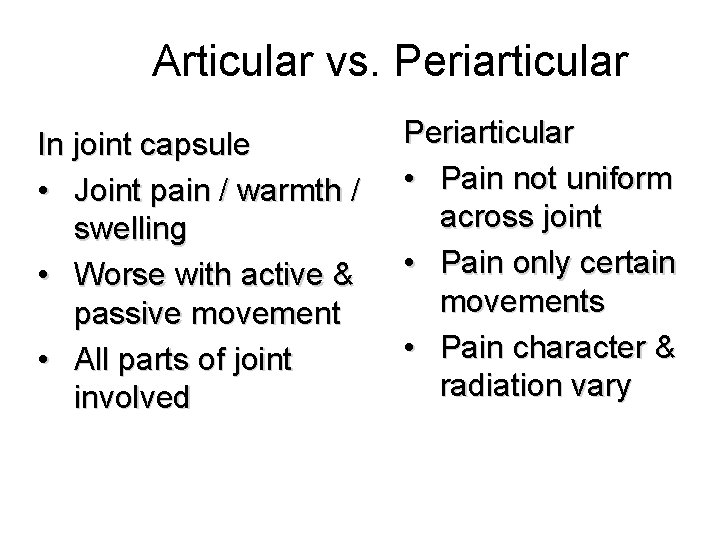

Articular vs. Periarticular In joint capsule • Joint pain / warmth / swelling • Worse with active & passive movement • All parts of joint involved Periarticular • Pain not uniform across joint • Pain only certain movements • Pain character & radiation vary

Physical Exam • • • Careful palpation Range of motion Heat, warmth, redness

Lab Studies • Screening tests: CBC, CRP, ESR • Chronic rheumatic disease: mild anemia • Rheumatoid factor, antinuclear antibody, antistreptolysin O titers, and Lyme serologies for follow-up • Serum uric acid: not helpful

Synovial Fluid • Especially crystalline, suppurative etiology • Appearance, cell count and diff, crystal analysis, Gram’s stain • Positive Gram’s: diagnostic • Negative Gram’s: cannot rule out

Management • • Rest Pain relief: meds, heat, cold No advantage to NSAIDs Exceptions: olecranon bursitis and prepatellar bursitis have a moderate risk of being infected (Staphylococcus aureus)

Management • Shoulder: immobilize few days • Risk of adhesive capsulitis • Lateral epicondylitis: forearm brace • Olecranon bursitis: compression dressing

Management • De Quervain’s: splint wrist and thumb in 20 o dorsiflexion • Achilles tendonitis: heel lift or splint in slight plantar flexion

Local Injection

Local Injection • Lidocaine or steroid injection can overcome refractory pain • Steroids universally given, often with great success • No good prospective data to support or refute therapeutic benefit

Local Injection • Short course of oral steroid may produce statistically similar results • Primary goal of steroid injection: relieve pain so patient can participate in physical rehab

Local Injection • Adjunct to other modalities: pain control, PT, exercise, OT, relative rest, immobilization • Additional pain control: NSAIDs, acupuncture, ultrasound, ice, heat, electrical nerve stimulation

Local Injection • Analgesics + exercise: better results than exercise alone • Eliminate provoking factors • Avoid repeat steroid injection unless good prior response • Wait at least 6 weeks between injections in same site

Indications Diagnosis • Obtain fluid for analysis • Eliminate referred pain Therapy • Give pain relief • Deliver therapeutic agents

Contraindication: Absolute • • Bacteremia Infectious arthritis Periarticular cellulitis Adjacent osteomyelitis Significant bleeding disorder Hypersensitivity to steroid Osteochondral fracture

Contraindication: Relative • • Violation of skin integrity Chronic local infection Anticoagulant use Poorly controlled diabetes Internal joint derangement Hemarthrosis Preexisting tendon injury Partial tendon rupture

Preparations • • Local anesthetic Hydrocortisone / corticosteroid Rapid anti-inflammatory effect Categorized by solubility and relative potency • High solubility short duration • Absorbed, dispersed more rapidly

Preparations • Triamcinolone hexacetonide: least soluble, longest duration • Potential for subcutaneous atrophy • Intra-articular injections only • Methylprednisolone acetate (Depo. Medrol®): reasonable first choice for most ED indications

Dosage • Large bursa: subacromial, olecranon, trochanteric: 40 – 60 mg methylprednisolone • Medium or wrist, knee, heel ganglion: 10 – 20 mg • Tendon sheath: de Quervain, flexor tenosynovitis: 5 – 15 mg

Site Preparation • Use careful aseptic technique • Mark landmarks with skin pencil, tincture of iodine, or thimerosal (Merthiolate®) (sterile Q-tip) • Clean point of entry: povidoneiodine (Betadine®) and alcohol • Do not need sterile drapes

Technique • Make skin wheal: 1% lidocaine or 0. 25% bupivacaine OR… …use topical vapocoolant: e. g. , Fluori-Methane® • Use Z-tract technique: limits risk of soft tissue fistula • Agitate syringe prior to injection: steroid can precipitate or layer

Complications: Acute • Reaction to anesthetic: rare • Treat as in standard textbooks • • Accidental IV injection Vagal reaction: have patient flat Nerve injury: pain, paresthesias Post injection flare: starts in hours, gone in days (~2%)

Complications: Delayed • Localized subcutaneous or cutaneous atrophy at injection site • Small depression in skin with depigmentation, transparency, and occasional telangiectasia • • • Evident in 6 weeks to 3 months Usually resolve within 6 months Can be permanent

Complications: Delayed • • Tendon rupture: low risk (<1%) Dose-related Related to direct tendon injection? Limit injections to no more than once every 3 to 4 months • Avoid major stress-bearing tendons: Achilles, patellar

Complications: Delayed • Systemic absorption slower than with oral steroids • Can suppress hypopituitaryadrenal axis for 2 to 7 days • Can exacerbate hyperglycemia in diabetes • Abnormal uterine bleeding reported

Some specific entities…

Bicipital Tendonitis • Risk: repeatedly flex elbow against resistance: weightlifter, swimmer • Tendon goes through bicipital (intertubercular) groove • Pain with elbow at 90° flexion, arm internally / externally rotated

Bicipital Tendonitis • Range of motion: normal or restricted • Strength: normal • Tenderness: bicipital groove • Pain: elevate shoulder, reach hip pocket, pull a back zipper

Bicipital Tendonitis • Lipman test: "rolling" bicipital tendon produces localized tenderness • Yergason test: pain along bicipital groove when patient attempts supination of forearm against resistance, holding elbow flexed at 90° against side of body

Calcific Tendonitis Supraspinatus Tendonitis Subacromial Bursitis • Calcific (calcareous) tendonitis: hydroxyapatite deposits in one or more rotator cuff tendons • Commonly supraspinatus • Sometimes rupture into adjacent subacromial bursa • Acute deltoid pain, tenderness

Calcific Tendonitis Supraspinatus Tendonitis Subacromial Bursitis • Clinically similar: difficult to differentiate • Rotator cuff: teres minor, supraspinatus, infraspinatus, subscapularis • Insert as conjoined tendon into greater tuberosity of humerus

Calcific Tendonitis Supraspinatus Tendonitis Subacromial Bursitis Jobe’s sign, AKA “empty can test” • Abduct arm to 90 o in the scapular plane, then internally rotate arms to thumbs pointed downward • Place downward force on arms: weakness or pain if supraspinatus

Calcific Tendonitis Supraspinatus Tendonitis Subacromial Bursitis • Other tests: Neer, Hawkins • Passively abduct arm to 90°, then passively lower arm to 0° and ask patient to actively abduct arm to 30°

Calcific Tendonitis Supraspinatus Tendonitis Subacromial Bursitis • If can abduct to 30° but no further, suspect deltoid • If cannot get to 30°, but if placed at 30° can actively abduct arm further, suspect supraspinatus • If uses hip to propel arm from 0° to beyond 30°, suspect supraspinatus

Calcific Tendonitis Supraspinatus Tendonitis Subacromial Bursitis • Subacromial bursa: superior and lateral to supraspinatus tendon • Tendon and bursa in space between acromion process and head of humerus • Prone to impingement

Calcific Tendonitis / Supraspinatus Tendonitis / Subacromial Bursitis • Patient holds arm protectively against chest wall • May be incapacitating • All ROM disturbed, but internal rotation markedly limited • Diffuse perihumeral tenderness • X-ray: hazy shadow

Rotator Cuff Tear • Drop arm test: arm passively abducted at 90 o, patient asked to maintain dropped arm represents large rotator cuff tear • Shrug sign: attempt to abduct arm results in shrug only

Elbow and Wrist

Lateral Epicondylitis • Pain at insertion of extensor carpi radialis and extensor digitorum muscles • Radiohumeral bursitis: tender over radiohumeral groove • Tennis elbow: tender over lateral epicondyle

Lateral Epicondylitis • History repetitive overhead motion: golfing, gardening, using tools • Worse when middle finger extended against resistance with wrist and the elbow in extension • Worse when wrist extended against resistance

Medial Epicondylitis • “Golfer's elbow” or “pitcher’s elbow” similar • Much less common • Worse when wrist flexed against resistance • Tender medial epicondyle

Cubital Tunnel Syndrome • Ulnar nerve passes through cubital tunnel just behind ulnar elbow • Numbness and pain small and ring fingers • Initial treatment: rest, splint

Olecranon Bursitis • • • “Student's” or “barfly elbow” Most frequent site of septic bursitis Aseptic: motion at elbow joint complete and painless • Septic: all motion usually painful

Olecranon Bursitis Aseptic olecranon bursitis • Cosmetically bothersome, usually resolves spontaneously • If bothersome, aspiration and steroid injection speed resolution • Oral NSAID after steroid injection does not affect outcome

Septic Olecranon Bursitis • Most common septic bursitis: olecranon and prepatellar • 2 o to acute trauma / skin breakage • Impossible to differentiate acute gouty olecranon bursitis from septic bursitis without laboratory analysis

Ganglion Cysts • Swelling on dorsal wrist • ~60% of wrist and hand soft tissue tumors • Etiology obscure • Lined with mesothelium or synovium • Arise from tendon sheaths or near joint capsule

Carpal Tunnel Syndrome • Median nerve compression in fibroosseous tunnel of wrist • Pain at wrist that sometimes radiates upward into forearm • Associated with tingling and paresthesias of palmar side of index and middle fingers and radial half of the ring finger

Carpal Tunnel Syndrome • Patient wakes during night with burning or aching pain, numbness, and tingling • Positive Tinel sign: reproduce tingling and paresthesias by tapping over median nerve at volar crease of wrist

Carpal Tunnel Syndrome • Positive Phalen test: flexed wrists held against each other for several minutes in effort to provoke symptoms in median nerve distribution

Carpal Tunnel Syndrome • May be idiopathic • Known causes: rheumatoid arthritis pregnancy, diabetes, hypothyroidism, acromegaly

Carpal Tunnel Syndrome • Insert needle just radial or ulnar to palmaris longus and proximal to distal wrist crease • Ulnar preferred: avoids nerve • Direct needle at 60° to skin surface, point toward tip of middle finger

de Quervain’s Disease • Chronic teno-synovitis due to narrowed tendon sheaths around abductor policis longus and extensor pollicis brevis muscles

de Quervain’s Disease • • • 1 st dorsal compartment Radial border of anatomic snuffbox 1 st compartment may cross over 2 nd compartment (ECRL/B) proximal to extensor retinaculum • Steroid injections relieve most symptoms

Trigger Finger • Digital flexor tenosynovitis • Stenosed tendon sheath • Palmar surface over MC head • Intermittent tendon “catch” • “Locks” on awakening • Most frequent: ring and middle

Trigger Finger • Tendon sheath walls lined with synovial cells • Tendon unable to glide within sheath • Initial treatment: splint, moist heat, NSAID • Steroid for recalcitrant cases

Hip and Groin

Trochanteric Bursitis • Second leading cause of lateral hip pain after osteoarthritis • Discrete tenderness to deep palpation • Principal bursa between gluteus maximus and posterolateral prominence of greater trochanter

Trochanteric Bursitis • • • Pain usually chronic Pathology in hip abductors May radiate down thigh, lateral or posterior • Worse with lying on side, stepping from curb, descending steps

Trochanteric Bursitis • Patrick fabere sign (flexion, abduction, external rotation, and extension) may be negative • Passive ROM relatively painless • Active abduction when lying on opposite side pain • Sharp external rotation pain

Ischiogluteal Bursitis • Weaver's bottom / tailor’s seat: pain center of buttock radiating down back of leg • Often mistaken for back strain, herniated disk • Pain worse with sitting on hard surface, bending forward, standing on tiptoe

Ischiogluteal Bursitis • Tenderness over ischial tuberosity • Ischiogluteal bursa adjacent to ischial tuberosity, overlies sciatic / posterior femoral cutaneous nerves

Legs and Feet

Prepatellar Bursitis • Housemaid’s knee / nun’s knee: swelling with effusion of superficial bursa over lower pole of patella • Passive motion fully preserved • Pain mild except during extreme knee flexion or direct pressure

Prepatellar Bursitis • Pressure from repetitive kneeling on a firm surface: rug cutter's knee • Rarely direct trauma • Second most common site for septic bursitis

Baker’s Cyst • Pseudothrombophlebitis syndrome • Herniated fluid-filled sacs of articular synovial membrane that extend into popliteal fossa • Causes: trauma, rheumatoid arthritis, gout, osteoarthritis • Pain worse with active knee flexion

Baker’s Cyst • Can mimic deep venous thrombosis • Ultrasound eseential • Many resolve over weeks • May require surgery • Steroid injections not performed: risk of neurovascular injury

Anserine Bursitis • Cavalryman's disease / pes bursitis / goosefoot bursitis: obese women with large thighs, athletes who run • Anteromedial knee, inferior to joint line at insertion of sartorius, semitendinous, and gracilis tendon

Anserine Bursitis • Abrupt knee pain, local tenderness 4 to 5 cm below medial aspect of tibial plateau • Knee flexion exacerbates

Iliotibial Band Syndrome • Lateral knee pain • Cyclists, dancers, distance runners, football players • Pain worse climbing stairs • Tenderness when patient supine, knee flexed to 90 o

Ankle and Foot

Peroneal Tendonitis • Peroneal tendons cross behind lateral malleolus • Running, jumping, sprain • Holding foot up and out against downward pressure causes pain

Peroneal Tendon Rupture • Torn retinaculum • Have patient dorsiflex and plantar flex with foot in inversion • Feel for “snapping” behind lateral malleolus

Retrocalcaneal Bursitis • Ankle overuse: excessive walking, running, or jumping • Heel pain: especially with walking, running, palpation • Haglund disease: bony ridge on posterosuperior calcaneus • Treatment: open heels (clogs), bare feet, sandals, or heel lift

Plantar Fasciitis • Policeman's heel / soldier's heel: associated with heel spurs • Degenerated plantar fascial band at origin on medial calcaneous • Heel pain worse in morning and after long periods of rest • May be relieved with activity

Plantar Fasciitis • Microtears in fascia from overuse? • Eliminate precipitators, rest, strength and stretching exercises, arch supports, and night splints • Sometimes need steroid injection • Risk of plantar fascia rupture and fat pad atrophy

Tarsal Tunnel Syndrome • Between medial malleolus and flexor retinaculum • Vague pain in sole of foot: burning or tingling • Worse with activity, especially standing, walking for long periods • Tender along course of nerve

Tarsal Tunnel Syndrome • Between medial malleolus and flexor retinaculum • Vague pain in sole of foot: burning or tingling • Worse with activity, especially standing, walking for long periods • Tender along course of nerve

Fibromyalgia

Fibromyalgia • Pain in muscles, joints, ligaments and tendons • “Tender points“ • Knees, elbows, hips, neck • • 5% of population, including kids Main symptom: sensitivity to pain

Fibromyalgia • Pain: chronic, deep or burning, migratory, intermittent • Fatigue, poor sleep • Numbness or tingling • “Poor blood flow” • Sensitivity to odors, bright lights, loud noises, medicines

Fibromyalgia • • Jaw pain Dry eyes Difficulty focusing Dizziness Balance problems Chest pain Rapid or irregular heartbeat

Fibromyalgia • • Shortness of breath Difficulty swallowing Heartburn Gas Cramping abdominal pain Alternating diarrhea & constipation Frequent urination

Fibromyalgia • • Pain in bladder area Urgency Pelvic pain Painful menstrual periods Painful sexual intercourse Depression Anxiety
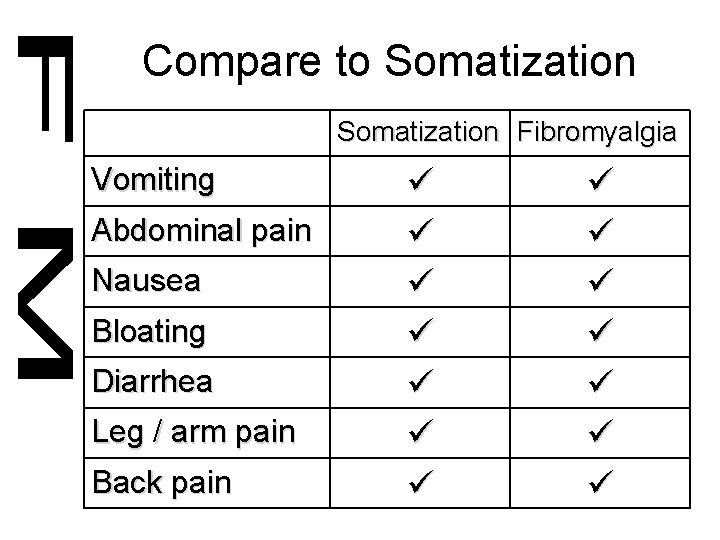
Compare to Somatization Fibromyalgia Vomiting Abdominal pain Nausea Bloating Diarrhea Leg / arm pain Back pain
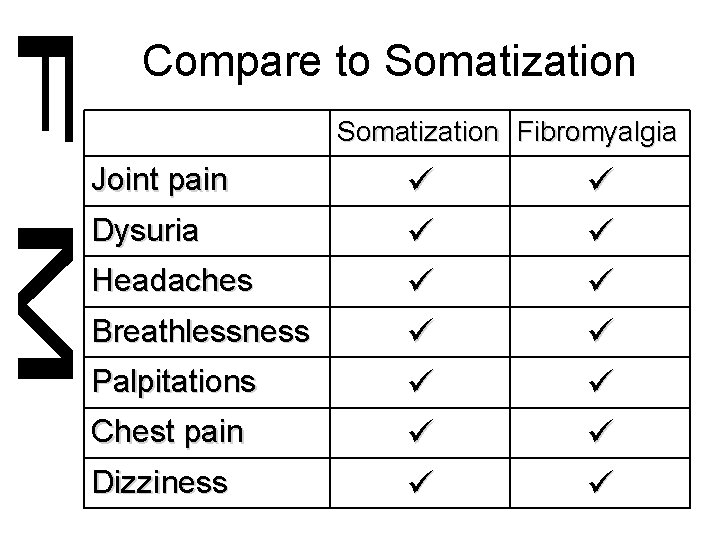
Compare to Somatization Fibromyalgia Joint pain Dysuria Headaches Breathlessness Palpitations Chest pain Dizziness
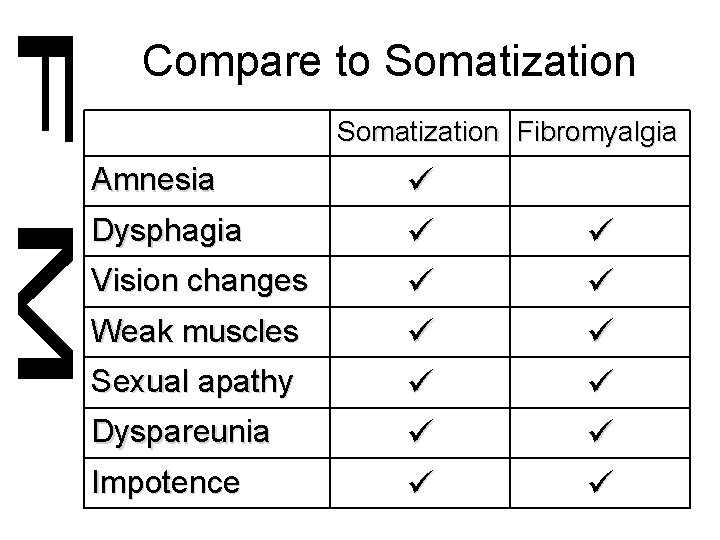
Compare to Somatization Fibromyalgia Amnesia Dysphagia Vision changes Weak muscles Sexual apathy Dyspareunia Impotence

Compare to Somatization Fibromyalgia Dysmenorrhea Irregular menstruation Excessive menstrual flow
Fibromyalgia • Treatment

Reflex Sympathetic Dystrophy • • • Causalgia Shoulder-hand syndrome Sudeck's atrophy Post-traumatic pain syndrome Complex regional pain syndrome type I and type II • Sympathetically maintained pain

Reflex Sympathetic Dystrophy • Distal extremity pain, tenderness • Bone demineralization, trophic skin changes, vasomotor instability • Precipitating event in 2/3: injury, stroke, MI, local trauma, fracture • Associated with emotional liability, depression, anxiety

Reflex Sympathetic Dystrophy • Treatments: medication, physical therapy, sympathetic nerve blocks, psychological support • Possible sympathectomy or dorsal column stimulator • Pain Clinic with coordinated plan may be helpful
- Slides: 109