Bureau of Workers Compensation Subsequent Report of Injury

Bureau of Workers’ Compensation Subsequent Report of Injury EDI Transactions in Pennsylvania

Speaker Introduction Tammy Laughman, manager EDI Unit – Claims Management Division Bureau of Workers’ Compensation Email: RA-CMDEDI@pa. gov

General EDI Information • The Bureau of Workers’ Compensation (BWC) is implementing the IAIABC EDI Release 3 Claims Standard for Subsequent Report of Injury (SROI) claim filings. • EDI is a structured transmission of data between organizations by electronic means. • Implementation date for EDI Release 3 is Sept. 9, 2013.
EDI Claims Tables • EDI reporting requirements are defined on the following tables: 1. Required report(s) 2. Data needed on the report(s) Event Table Element Requirements Table Edit Matrix 3. Applied editing

Subsequent Report of Injury (SROI) Event Table • Establishes the events accepted by Pennsylvania, and • tells claim administrators when to report an event, based on laws and regulations; as well as which, if any, paper forms are required to be sent to BWC and the claimant. Event Table
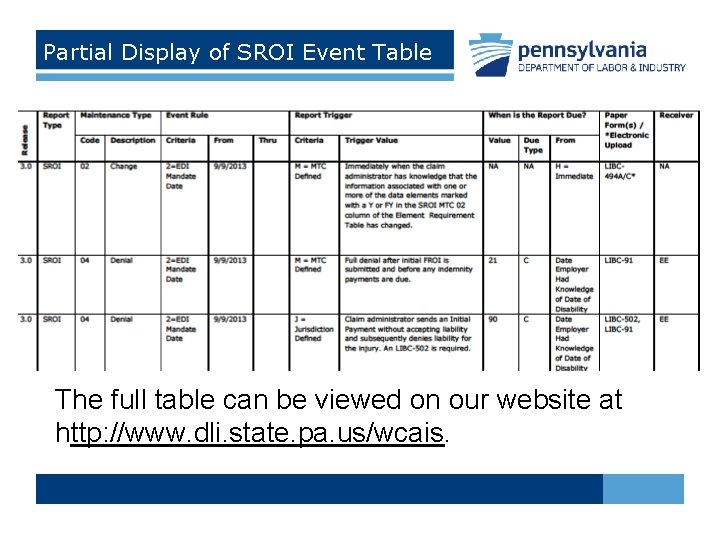
Partial Display of SROI Event Table The full table can be viewed on our website at http: //www. dli. state. pa. us/wcais.

Maintenance Type Codes (MTCs) • The IAIABC defines these as codes defining the specific purpose of individual records within the transaction being submitted. • They are used to report claim events and describe the types of SROI transactions being submitted. • Any MTCs other than those accepted by Pennsylvania will be rejected as not jurisdictionally valid.

Pennsylvania Accepted SROI MTCs • • • 02 – Change 04 – Denial AB – Add Concurrent Benefit Type AP – Acquired/Payment CA – Change Benefit Amount CB – Change Benefit Type FN – Final IP – Initial Payment P 1 – Partial Suspension, Returned to Work or Medically Determined/Qualified to Return to Work

Accepted SROI MTCs, continued • P 4 – Partial Suspension, Claimant Death • P 7 – Partial Suspension, Benefits Exhausted • PJ – Partial Suspension Pending Appeal or Judicial Review • PD – Partial Denial • PY – Payment Report • RB – Reinstatement of Benefits • RE – Reduced Earnings • S 1 – Suspension, Returned to Work, or Medically Determined/Qualified to Return to Work

Accepted SROI MTCs, continued • • S 3 – Suspension, Administrative Non-Compliance S 4 – Suspension, Claimant Death S 5 – Suspension, Incarceration S 7 – Suspension, Benefits Exhausted S 8 – Suspension, Jurisdiction Change SD – Suspension, Directed by Jurisdiction SJ – Suspended Pending Appeal or Judicial Review • UR – Upon Request

SROI Event Table Scenario A claim administrator reduces benefits because an employee has returned to work earning less than their pre-injury wage. The claim administrator chooses to reduce earnings using an agreement. The claim administrator will send a SROI RE with the Award/Order Date (DN 0299) populated with the date of the agreement. He will send a copy of a completed Supplemental Agreement (LIBC-337) to the claimant and BWC. (It can be sent to BWC by electronic batch, by upload in the Workers’ Compensation Automation and Integration System, WCAIS, or by mail. )

Element Requirements Table • This table defines the event data, by data element name and number (DN), required for a Maintenance Type Code (MTC). The SROI components of this table are: – SROI Element Requirements Element Worksheet Requirements Table – SROI Conditional Requirements Worksheet – Event Benefits Segment Requirements Worksheet

Element Requirements Table The Element Requirements Table describes: • MTC Codes associated with one or more of the reportable events defined in the event table, • mandatory conditional (MC) data elements which are mandatory if the condition defined is met, and • business rules that apply to specific data elements when there is an MC indicator.
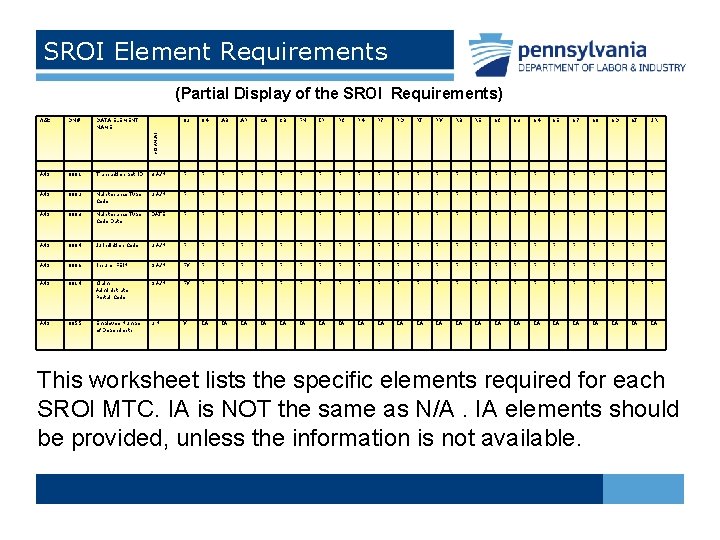
SROI Element Requirements (Partial Display of the SROI Requirements) DN# DATA ELEMENT NAME 02 04 AB AP CA CB FN IP P 1 P 4 P 7 PD PJ PY RB RE S 1 S 3 S 4 S 5 S 7 S 8 SD SJ UR A 49 0001 Transaction Set ID 3 A/N F F F F F F F A 49 0002 Maintenance Type Code 2 A/N F F F F F F F A 49 0003 Maintenance Type Code Date DATE F F F F F F F A 49 0004 Jurisdiction Code 2 A/N F F F F F F F A 49 0006 Insurer FEIN 9 A/N FY F F F F F F A 49 0014 Claim Administrator Postal Code 9 A/N FY F F F F F F A 49 0055 Employee Number of Dependents 2 N Y IA IA IA IA IA IA FORMAT REC This worksheet lists the specific elements required for each SROI MTC. IA is NOT the same as N/A. IA elements should be provided, unless the information is not available.

Requirement Codes • • F – Fatal FC – Fatal/Conditional FY – Fatal/Yes Change R – Restricted RC – Restricted/Conditional M – Mandatory MC – Mandatory/Conditional Y – Yes Change • • YC – Yes/Conditional N – No E – Expected EC – Expected/Conditional IA – If Applicable/Available NA – Not Applicable X - Exclude

Data Reporting • Date of Injury (DN 0031) – If a claim administrator is uncertain about this date, use the earliest date for which there is some degree of certainty, or the date you receive notice of the accident, whichever is earlier. • Industry Code (DN 0025) – This is an important data element for BWC’s statistical reports. Claim administrators should report the correct industry code. If doubt exists, reference the NAICS organization’s website at www. naics. com.
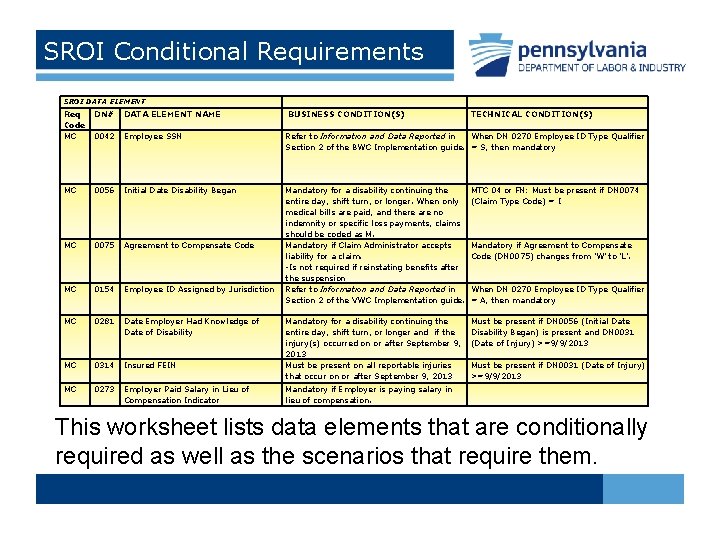
SROI Conditional Requirements SROI DATA ELEMENT Req Code MC DN# DATA ELEMENT NAME BUSINESS CONDITION(S) 0042 Employee SSN Refer to Information and Data Reported in When DN 0270 Employee ID Type Qualifier Section 2 of the BWC Implementation guide. = S, then mandatory MC 0056 Initial Date Disability Began MTC 04 or FN: Must be present if DN 0074 (Claim Type Code) = I MC 0075 Agreement to Compensate Code MC 0154 Employee ID Assigned by Jurisdiction Mandatory for a disability continuing the entire day, shift turn, or longer. When only medical bills are paid, and there are no indemnity or specific loss payments, claims should be coded as M. Mandatory if Claim Administrator accepts liability for a claim. -Is not required if reinstating benefits after the suspension Refer to Information and Data Reported in Section 2 of the VWC Implementation guide. MC 0281 Date Employer Had Knowledge of Date of Disability Must be present if DN 0056 (Initial Date Disability Began) is present and DN 0031 (Date of Injury) >=9/9/2013 MC 0314 Insured FEIN Mandatory for a disability continuing the entire day, shift turn, or longer and if the injury(s) occurred on or after September 9, 2013 Must be present on all reportable injuries that occur on or after September 9, 2013 MC 0273 Employer Paid Salary in Lieu of Compensation Indicator Mandatory if Employer is paying salary in lieu of compensation. TECHNICAL CONDITION(S) Mandatory if Agreement to Compensate Code (DN 0075) changes from 'W' to 'L'. When DN 0270 Employee ID Type Qualifier = A, then mandatory Must be present if DN 0031 (Date of Injury) >=9/9/2013 This worksheet lists data elements that are conditionally required as well as the scenarios that require them.
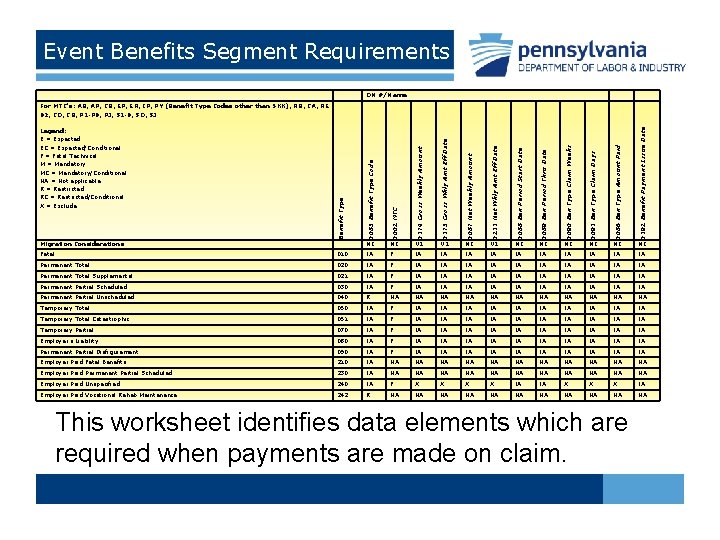
Event Benefits Segment Requirements DN #/Name Benefit Type 0085 Benefit Type Code 0002 MTC 0174 Gross Weekly Amount 0175 Gross Wkly Amt Eff Date 0087 Net Weekly Amount 0211 Net Wkly Amt Eff Date 0088 Ben Period Start Date 0089 Ben Period Thru Date 0090 Ben Type Claim Weeks 0091 Ben Type Claim Days 0086 Ben Type Amount Paid 0192 Benefit Payment Issue Date For MTC's: AB, AP, CB, EP, ER, IP, PY (Benefit Type Codes other than 5 XX), RB, CA, RE 02, CO, CB, P 1 -P 9, PJ, S 1 -9, SD, SJ Migration Considerations NI NI V 1 NI NI NI Fatal 010 IA F IA IA IA Permanent Total 020 IA F IA IA IA Permanent Total Supplemental 021 IA F IA IA IA Permanent Partial Scheduled 030 IA F IA IA IA Permanent Partial Unscheduled 040 R NA NA NA Temporary Total 050 IA F IA IA IA Temporary Total Catastrophic 051 IA F IA IA IA Temporary Partial 070 IA F IA IA IA Employer's Liability 080 IA F IA IA IA Permanent Partial Disfigurement 090 IA F IA IA IA Employer Paid Fatal Benefits 210 IA NA NA NA Employer Paid Permanent Partial Scheduled 230 IA NA NA NA Employer Paid Unspecified 240 IA F X X IA IA X X X IA Employer Paid Vocational Rehab Maintenance 242 R NA NA NA Legend: E = Expected EC = Expected/Conditional F = Fatal Technical M = Mandatory MC = Mandatory/Conditional NA = Not applicable R = Restricted RC = Restricted/Conditional X = Exclude This worksheet identifies data elements which are required when payments are made on claim.

Edit Matrix Table This table is made up of five worksheets which: • Communicate the edits that will be applied to the data being sent to BWC, as well as the standard error messages for those edits when the data is not acceptable, and Edit Matrix • describes the proper sequence of submissions, acceptable code values, data used for matching to existing claims and the error messages associated with these edits.

Five Worksheets in Edit Matrix • • • DN-Error Message – contains “standard” edits and error messages. Value Table – lists BWC’s acceptable code values. Match Data – describes which data elements will be used to determine if the information matches an existing claim or if a new claim must be created. Population Restrictions – is a listing of restrictions applied to the data element(s). SROI Sequencing Tables – describes how BWC will apply sequencing edits and the order in which specific events are expected to be reported.
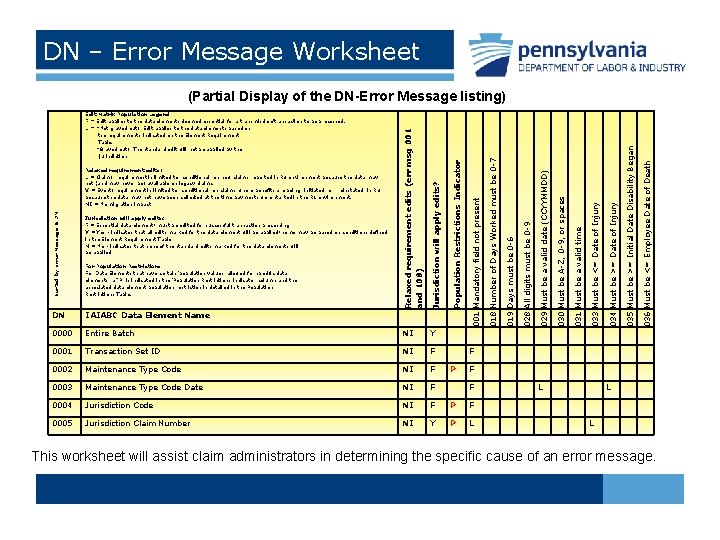

DN – Error Message Worksheet (Partial Display of the DN-Error Message listing) Jurisdiction will apply edits? DN IAIABC Data Element Name 001 Mandatory field not present 018 Number of Days Worked must be 0 -7 019 Days must be 0 -6 028 All digits must be 0 -9 029 Must be a valid date (CCYYMMDD) 030 Must be A-Z, 0 -9, or spaces 031 Must be a valid time 033 Must be <= Date of Injury 034 Must be >= Date of Injury 035 Must be >= Initial Date Disability Began 036 Must be <= Employee Date of Death 0000 Entire Batch NI Y 0001 Transaction Set ID NI F F 0002 Maintenance Type Code NI F P F 0003 Maintenance Type Code Date NI F F L L 0004 Jurisdiction Code NI F P F 0005 Jurisdiction Claim Number NI Y P L Sorted by Error Message & DN Relaxed requirement edits: L = Claim: requirement is limited to "conditional" on new claims reported in R 3 environment because the data may not (and may never be) available on legacy claims. V = Event: requirement is limited to "conditional" on claims where benefits are being "initiated" or "reinstated" in R 3 because the data may not have been collected at the time payments were started in the R 1 environment. NI = No migration impact Jurisdiction will apply edits? : F = Essential data element; must be edited for successful transaction processing Y = Yes - indicates that all edits marked for the data element will be applied; some may be based on conditions defined in the Element Requirement Table N = No - indicates that none of the standard edits marked for the data elements will be applied For Population Restrictions: For Data Elements that have certain ‘population values’ allowed for specific data elements, a “P” is indicated in the ‘Population Restrictions Indicator’ column and the associated data element population restriction is detailed in the Population Restrictions Table. Population Restrictions Indicator Relaxed requirement edits (err msg 001 and 108) Edit Matrix Population Legend: F = Edit applies to the data elements deemed essential for a transmission/transaction to be processed. L = *Not grayed out: Edit applies to the data elements based on the requirements indicated on the Element Requirement Table. *Grayed out: The standard edit will not be applied by the jurisdiction This worksheet will assist claim administrators in determining the specific cause of an error message.

DN – Error Message Worksheet, continued • Shows data elements that have specific data population restrictions and/or accepted values. These are marked with a “P” and are described in the Population Restrictions worksheet. • An “L” in this worksheet indicates that this edit is being applied by the jurisdiction. If the information provided does not meet the requirement, the listed error number will be returned to the sender. This worksheet explains the definition of each error number.
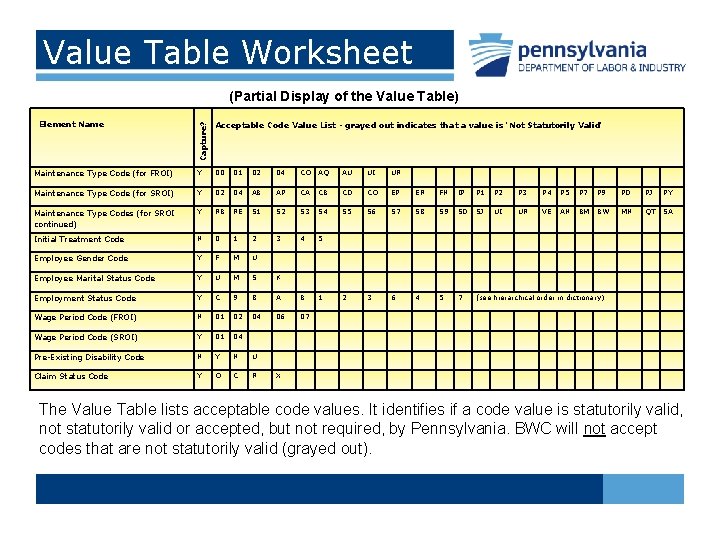
Value Table Worksheet (Partial Display of the Value Table) Capture? Element Name Acceptable Code Value List - grayed out indicates that a value is 'Not Statutorily Valid' Maintenance Type Code (for FROI) Y 00 01 02 04 CO AQ AU UI UR Maintenance Type Code (for SROI) Y 02 04 AB AP CA CB CD CO EP ER FN IP P 1 P 2 P 3 P 4 P 5 P 7 P 9 PD PJ PY Maintenance Type Codes (for SROI continued) Y RB RE S 1 S 2 S 3 S 4 S 5 S 6 S 7 S 8 S 9 SD SJ UI UR VE AN BM BW MN QT SA Initial Treatment Code N 0 1 2 3 4 5 Employee Gender Code Y F M U Employee Marital Status Code Y U M S K Employment Status Code Y C 9 8 A B 1 2 3 6 4 5 7 (see hierarchical order in dictionary) Wage Period Code (FROI) N 01 02 04 06 07 Wage Period Code (SROI) Y 01 04 Pre-Existing Disability Code N Y N U Claim Status Code Y O C R X The Value Table lists acceptable code values. It identifies if a code value is statutorily valid, not statutorily valid or accepted, but not required, by Pennsylvania. BWC will not accept codes that are not statutorily valid (grayed out).
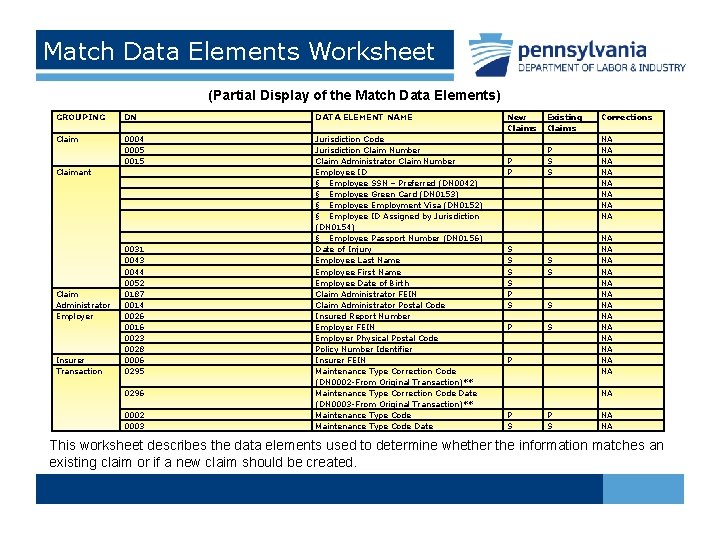
Match Data Elements Worksheet (Partial Display of the Match Data Elements) GROUPING Claimant Claim Administrator Employer Insurer Transaction DN 0004 0005 0015 0031 0043 0044 0052 0187 0014 0026 0016 0023 0028 0006 0295 0296 0002 0003 DATA ELEMENT NAME Jurisdiction Code Jurisdiction Claim Number Claim Administrator Claim Number Employee ID § Employee SSN – Preferred (DN 0042) § Employee Green Card (DN 0153) § Employee Employment Visa (DN 0152) § Employee ID Assigned by Jurisdiction (DN 0154) § Employee Passport Number (DN 0156) Date of Injury Employee Last Name Employee First Name Employee Date of Birth Claim Administrator FEIN Claim Administrator Postal Code Insured Report Number Employer FEIN Employer Physical Postal Code Policy Number Identifier Insurer FEIN Maintenance Type Correction Code (DN 0002 -From Original Transaction)** Maintenance Type Correction Code Date (DN 0003 -From Original Transaction)** Maintenance Type Code Date New Claims P P Existing Claims P S S Corrections S S P S P P S S S S NA NA NA NA P S NA NA NA This worksheet describes the data elements used to determine whether the information matches an existing claim or if a new claim should be created.

Match Data Elements Worksheet, continued • These data elements can only be changed on a SROI 02 (Change) transaction. • Only one primary or secondary match data element can be changed on the same SROI 02 transaction. • Additional match data elements are used as confirmation that a claim is a duplicate.
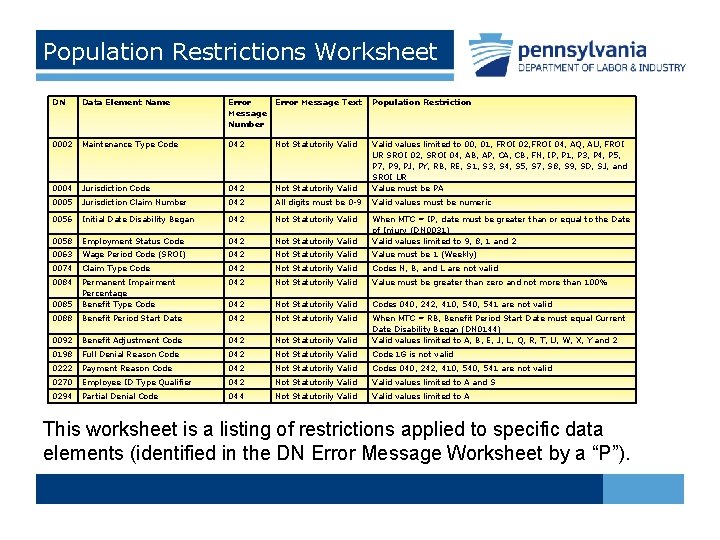
Population Restrictions Worksheet DN Data Element Name Error Message Text Message Number Population Restriction 0002 Maintenance Type Code 042 Not Statutorily Valid 0004 Jurisdiction Code 042 Not Statutorily Valid values limited to 00, 01, FROI 02, FROI 04, AQ, AU, FROI UR SROI 02, SROI 04, AB, AP, CA, CB, FN, IP, P 1, P 3, P 4, P 5, P 7, P 9, PJ, PY, RB, RE, S 1, S 3, S 4, S 5, S 7, S 8, S 9, SD, SJ, and SROI UR Value must be PA 0005 Jurisdiction Claim Number 042 All digits must be 0 -9 Valid values must be numeric 0056 Initial Date Disability Began 042 Not Statutorily Valid 0058 Employment Status Code 042 Not Statutorily Valid When MTC = IP, date must be greater than or equal to the Date of Injury (DN 0031) Valid values limited to 9, 8, 1 and 2 0063 Wage Period Code (SROI) 042 Not Statutorily Valid Value must be 1 (Weekly) 0074 Claim Type Code 042 Not Statutorily Valid Codes N, B, and L are not valid 0084 042 Not Statutorily Valid Value must be greater than zero and not more than 100% 0085 Permanent Impairment Percentage Benefit Type Code 042 Not Statutorily Valid Codes 040, 242, 410, 541 are not valid 0088 Benefit Period Start Date 042 Not Statutorily Valid 0092 Benefit Adjustment Code 042 Not Statutorily Valid When MTC = RB, Benefit Period Start Date must equal Current Date Disability Began (DN 0144) Valid values limited to A, B, E, J, L, Q, R, T, U, W, X, Y and 2 0198 Full Denial Reason Code 042 Not Statutorily Valid Code 1 G is not valid 0222 Payment Reason Code 042 Not Statutorily Valid Codes 040, 242, 410, 541 are not valid 0270 Employee ID Type Qualifier 042 Not Statutorily Valid values limited to A and S 0294 Partial Denial Code 044 Not Statutorily Valid values limited to A This worksheet is a listing of restrictions applied to specific data elements (identified in the DN Error Message Worksheet by a “P”).
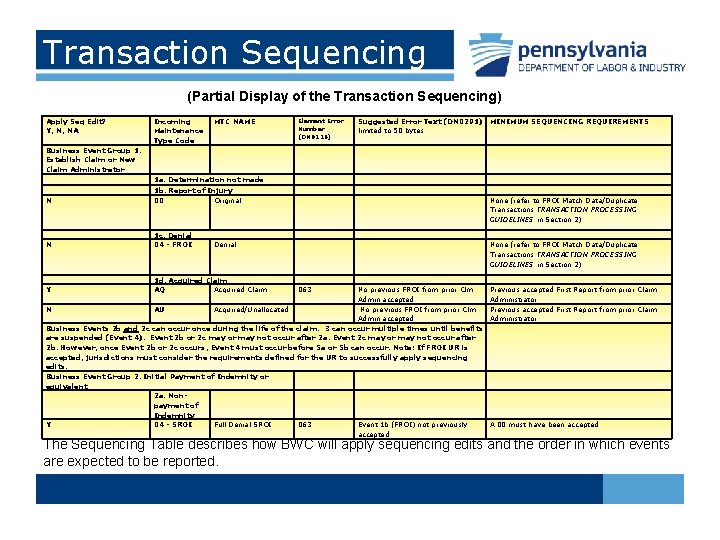
Transaction Sequencing (Partial Display of the Transaction Sequencing) Apply Seq Edit? Y, N, NA Business Event Group 1. Establish Claim or New Claim Administrator Incoming Maintenance Type Code MTC NAME Element Error Number (DN 0116) Suggested Error Text (DN 0291) limited to 50 bytes MINIMUM SEQUENCING REQUIREMENTS 1 a. Determination not made N 1 b. Report of Injury 00 Original None (refer to FROI Match Data/Duplicate Transactions TRANSACTION PROCESSING GUIDELINES in Section 2) N 1 c. Denial 04 - FROI None (refer to FROI Match Data/Duplicate Transactions TRANSACTION PROCESSING GUIDELINES in Section 2) Y 1 d. Acquired Claim AQ Acquired Claim Denial 063 No previous FROI from prior Clm Admin accepted N AU Acquired/Unallocated No previous FROI from prior Clm Admin accepted Business Events 2 b and 2 c can occur once during the life of the claim. 3 can occur multiple times until benefits are suspended (Event 4). Event 2 b or 2 c may or may not occur after 2 a. Event 2 c may or may not occur after 2 b. However, once Event 2 b or 2 c occurs, Event 4 must occur before 5 a or 5 b can occur. Note: If FROI UR is accepted, jurisdictions must consider the requirements defined for the UR to successfully apply sequencing edits. Business Event Group 2. Initial Payment of Indemnity or equivalent 2 a. Non payment of Indemnity Y 04 - SROI Full Denial SROI 063 Event 1 b (FROI) not previously accepted Previous accepted First Report from prior Claim Administrator A 00 must have been accepted The Sequencing Table describes how BWC will apply sequencing edits and the order in which events are expected to be reported.
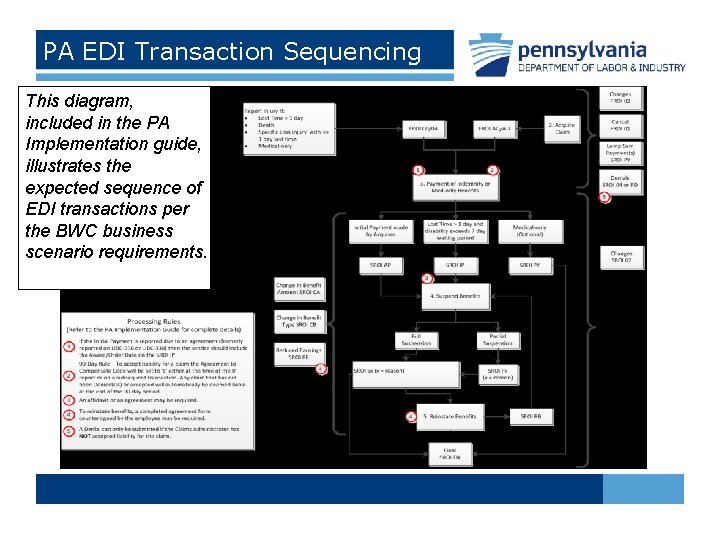
PA EDI Transaction Sequencing This diagram, included in the PA Implementation guide, illustrates the expected sequence of EDI transactions per the BWC business scenario requirements.

Reporting Data • Claim administrators should always submit the most current data on each MTC. • Data may be removed in BWC’s system if a space is sent on the MTC where data had previously been sent. • The cut-off time for processing files will be 11: 59 p. m. Eastern Time. All files located in the “IN” directory will be processed by BWC. Data that arrives after this cut-off time will be processed with the next day’s file date.
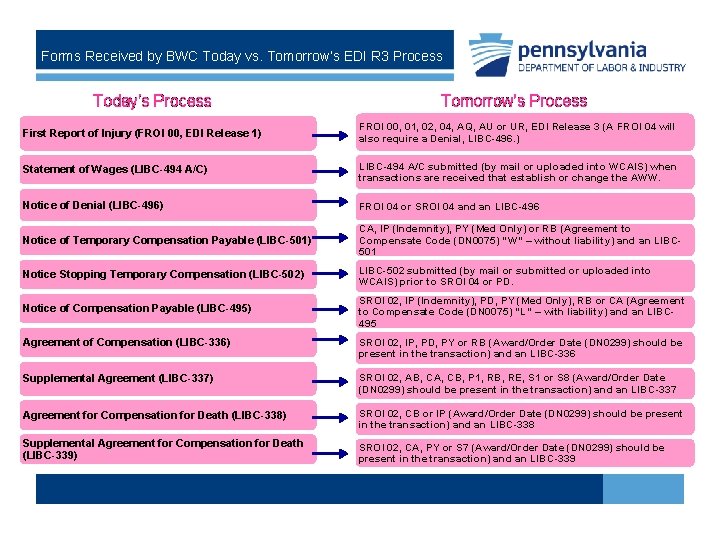
Forms Received by BWC Today vs. Tomorrow’s EDI R 3 Process Today’s Process Tomorrow’s Process First Report of Injury (FROI 00, EDI Release 1) FROI 00, 01, 02, 04, AQ, AU or UR, EDI Release 3 (A FROI 04 will also require a Denial, LIBC-496. ) Statement of Wages (LIBC-494 A/C) LIBC-494 A/C submitted (by mail or uploaded into WCAIS) when transactions are received that establish or change the AWW. Notice of Denial (LIBC-496) FROI 04 or SROI 04 and an LIBC-496 Notice of Temporary Compensation Payable (LIBC-501) CA, IP (Indemnity), PY (Med Only) or RB (Agreement to Compensate Code (DN 0075) “W” – without liability) and an LIBC 501 Notice Stopping Temporary Compensation (LIBC-502) LIBC-502 submitted (by mail or submitted or uploaded into WCAIS) prior to SROI 04 or PD. Notice of Compensation Payable (LIBC-495) SROI 02, IP (Indemnity), PD, PY (Med Only), RB or CA (Agreement to Compensate Code (DN 0075) “L” – with liability) and an LIBC 495 Agreement of Compensation (LIBC-336) SROI 02, IP, PD, PY or RB (Award/Order Date (DN 0299) should be present in the transaction) and an LIBC-336 Supplemental Agreement (LIBC-337) SROI 02, AB, CA, CB, P 1, RB, RE, S 1 or S 8 (Award/Order Date (DN 0299) should be present in the transaction) and an LIBC-337 Agreement for Compensation for Death (LIBC-338) SROI 02, CB or IP (Award/Order Date (DN 0299) should be present in the transaction) and an LIBC-338 Supplemental Agreement for Compensation for Death (LIBC-339) SROI 02, CA, PY or S 7 (Award/Order Date (DN 0299) should be present in the transaction) and an LIBC-339

Forms Received by BWC Today vs. Tomorrow’s EDI R 3 Process, continued Today’s Process Tomorrow’s Process Notification of Suspension or Modification (LIBC-751) P 1, RE or S 1 and an LIBC-751 Notice of Change of Workers’ Compensation Disability Status (LIBC-764) CB Final Receipt (LIBC-340) SROI 02 or S 1 and an LIBC-340 Commutation of Compensation (LIBC-498) PY Third-Party Settlement (LIBC-380) SROI 02 or CA (if change is due to Subrogation/Third Party Offset) and an LIBC-380 Notice of Workers’ Compensation Benefit Offset (LIBC 761) CA Notice of Suspension – Failure to Return Form LIBC-760 (LIBC-762) S 3 Notice of Reinstatement of Workers’ Compensation Benefits (LIBC-763) Final Statement of Account (LIBC-392 A) RB S 4 (with a death certificate or Coroner’s Report sent to BWC) or FN
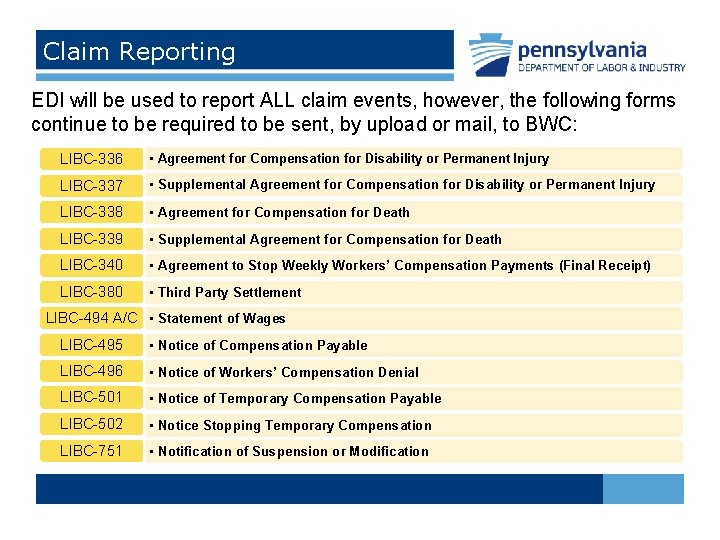
Claim Reporting EDI will be used to report ALL claim events, however, the following forms continue to be required to be sent, by upload or mail, to BWC: LIBC-336 • Agreement for Compensation for Disability or Permanent Injury LIBC-337 • Supplemental Agreement for Compensation for Disability or Permanent Injury LIBC-338 • Agreement for Compensation for Death LIBC-339 • Supplemental Agreement for Compensation for Death LIBC-340 • Agreement to Stop Weekly Workers’ Compensation Payments (Final Receipt) LIBC-380 • Third Party Settlement LIBC-494 A/C • Statement of Wages LIBC-495 • Notice of Compensation Payable LIBC-496 • Notice of Workers’ Compensation Denial LIBC-501 • Notice of Temporary Compensation Payable LIBC-502 • Notice Stopping Temporary Compensation LIBC-751 • Notification of Suspension or Modification

Claim Reporting, continued Written notice to the employee has not changed due to EDI. Paper forms must be sent to the claimant for ALL transactions, whether they are forms currently generated by insurer systems, the SROI Template (LIBC-91)* available in WCAIS or LIBC forms downloaded from the department’s website. * The LIBC-91 cannot be used in place of the Notice of Compensation Payable (LIBC-495), Notice of Workers’ Compensation Denial (LIBC-496) or the Notice of Temporary Compensation Payable (LIBC-501). These forms can be submitted to BWC by electronic batch, attaching the form to the individual claim or by mail.

Claim Reporting, continued • • The LIBC-502, Notice Stopping Temporary Compensation, can be submitted electronically thru WCAIS or it will be available for download from the department’s website, to be completed offline. If the LIBC-502 is not submitted thru WCAIS, it can be submitted to BWC by electronic batch, attaching the form to the individual claim by upload or mailed. The LICB-494 (both A and C), Statement of Wages, will be available for download from the department’s website, to be completed offline, and then either submitted to BWC by electronic batch, attaching the form to the individual claim by upload or mailed.

Claim Reporting, continued • The LIBC-751, Notification of Suspension or Modification can be prepared and printed in WCAIS or downloaded and completed offline. Once the form is notarized and signed, it can be submitted to BWC by electronic batch, attaching the form to the individual claim by upload or by mail. • Agreements, which can be the current form in insurer systems or a form downloaded from the department’s website, can be submitted to BWC by electronic batch, attaching the form to the individual claim by upload or by mail.

Claim Reporting, continued • If a claim administrator chooses to use an agreement to initiate payment or to change, stop or reinstate benefits paid on a claim, in addition to the appropriate EDI transaction, an agreement must be uploaded or mailed to BWC, as required by Pennsylvania Law. • This should be done as close to the transaction date as possible, preferably the same day.

Claim Reporting, continued • The presence of an agreement should be indicated by populating the Award/Order Date (DN 0299) with the date the parties entered into the agreement in their EDI transaction. • If a claim administrator chooses to use a Notification of Suspension or Modification (LIBC-751) to modify or suspend benefits, the signed, dated and notarized form MUST be filed within seven days of the modification/suspension date, per the Workers’ Compensation Act.

Reporting Temporary Compensation on the Initial Payment (SROI IP) • When a claim administrator begins paying on a claim, the claim administrator is required to report those payments on a SROI IP (Initial Payment) transaction. • When submitting the transaction, the claim administrator should populate the Agreement to Compensate Code (DN 0075) with a “W” to indicate they are not accepting liability for the claim.

Complying with the 90 -Day Rule for Temporary Indemnity Claims • • • When paying a claim under temporary compensation, a claim administrator has 90 days to determine whether or not to accept liability. To accept liability, a claim administrator should file a SROI 02 (Change) to update the Agreement to Compensate Code to an “L. ” To deny a claim, a claim administrator must file a Notice Stopping Temporary Compensation (LIBC 502) electronically through WCAIS and submit a SROI 04 (Denial) transaction.

Complying with the 90 -Day Rule for Temporary Indemnity Claims, continued • If at the end of the 90 -day period the claim administrator has neither accepted or denied liability for a claim, the claim will automatically convert to a fully compensable claim and insurer will be held liable for payment. • Once a claim is accepted with liability, the claim administrator will be prevented from submitting a SROI 04 Denial.

Complying with the 90 -Day Rule for Temporary Medical-Only Claims • • • When paying a claim for only medical bills under temporary compensation, a claim administrator has 90 days to determine whether or not to accept liability. The SROI PY (Payment) transaction must indicate the claim administrator is not accepting liability by setting the Agreement to Compensate Code to “W. ” To accept liability, the claim administrator should file a SROI 02 (Change) transaction to update the Agreement to Compensate Code from “W” to “L. ”

Complying with the 90 -Day Rule for Temporary Medical-Only Claims, continued • To deny liability, the claim administrator should file a Notice Stopping Temporary Compensation (LIBC 502) electronically through WCAIS and submit a SROI 04 (Denial) transaction. • If at the end of the 90 -day period the claim administrator has neither accepted or denied the claim, it will automatically convert to a compensable medical-only claim and insurer will be held liable for medical payment.

Complying with the 90 -Day Rule for Temporary Medical-Only Claims, continued • The filing of a suspension while the Agreement to Compensate Code is set to “W” will be prohibited. • The Act requires a FROI be filed within seven days of the loss of a full day, turn or shift. However, in EDI Release 3, a FROI 00 (Original) must be filed first to initiate a claim. Once it’s on file, a SROI PY (Payment) transaction with the Claim Type Code (DN 0074) marked with “M” can be submitted to report the initial payment of medical expenses.

Partial Denials (PD) • • • Partial Denials can be used to deny liability for indemnity benefits but continue the payment of medical bills only if an IP (Initial Payment) transaction is on file with the Agreement to Compensate Code set to “W. ” If the claim administrator accepts liability for medical expenses, the Agreement to Compensate Code must be set to “L. ” If an agreement is entered by the parties, the Award/Order Date (DN 0299) should be populated with the date the parties entered into the agreement in their EDI transaction.

Reporting Agreement to Compensate on the Initial Payment (SROI IP) • When an initial payment is made to a claimant, the claim administrator should file a SROI IP (Initial Payment) transaction with the Agreement to Compensate Code set to “L” to indicate that they have accepted liability for the claim. • If the claim administrator is sending the claimant a Notice of Compensation Payable (LIBC-495), the SROI IP is filed without populating the Award/Order Date (DN 0299).

Reporting Fatalities • The FROI 00 (Original) should be filed within 48 hours of every injury resulting in death. • To temporarily accept liability for a fatality, file a SROI IP (Initial Payment) with the Agreement to Compensate Code set to “W. ” • To accept liability, file a SROI IP with the Agreement to Compensate Code set to “L. ”

Reporting Fatalities, continued • If an agreement is entered by the parties, the Award/Order Date (DN 0299) should be populated with the date the parties entered into the agreement in their EDI transaction. • When the claim administrator has knowledge that information associated with one or more data elements marked with a Y or FY in the Elements Requirement Table has changed, SROI 02 (Change) transaction must be filed.

Reporting Fatalities, continued • • • If a spouse remarries, the payment of a dowry is due; this requires a SROI PY (Payment Report). If a spouse dies and there are no dependents, a SROI S 4 (Suspension, Claimant Death) transaction must be filed. A change in the benefit amount paid to a dependent requires a SROI CA (Change in Benefit Amount) transaction.

Reporting Fatalities, continued • If a spouse remarries and there are no other dependents on the claim, a SROI S 7 (Suspension, Benefits Suspended) transaction is required to suspend the claim. If there are other dependents, a SROI CA is required to change the benefit amounts for the remaining dependents. • In the event the employee dies as a result of an injury and payments begin, a SROI CB (Change in Benefits) transaction must be filed and the Death Result of Injury Code should be populated.

Suspending Benefits • A Return to Work (SROI S 1) transaction must be filed when a claimant returns to work with no loss in earnings. • An Administrative Non-Compliance (SROI S 3) transaction must be filed if a claimant fails to return form LIBC-760 (Employee Verification of Employment, Self. Employment or Change in Physical Condition) to the claim administrator and benefits are suspended. • A Claimant Death (SROI S 4) transaction must be filed if a claimant has died and benefits are no longer due. A Death Certificate or Coroner’s Report must also be filed with BWC.

Suspending Benefits, continued • An Incarceration (SROI S 5) transaction must be filed when benefits are suspended because a claimant has been incarcerated. • Benefits Exhausted (SROI S 7) transaction must be filed when benefits are exhausted. This includes being suspended because there are no longer any dependents entitled to benefits. In case of a death, a Supplemental Agreement for Death (LIBC-339) must be uploaded or mailed to BWC.

Suspending Benefits, continued • Jurisdiction Change (SROI S 8) transaction must be filed when there is a jurisdiction change. • Directed by Jurisdiction (SROI SD) transaction must be filed when a judge, the Appeal Board or court issues a decision, opinion or an order. • Pending Appeal or Judicial Review (SROI SJ/PJ) transaction must be filed when a judge grants Supersedeas while a case is under review.

Complying with the 21 -Day Requirement • The Workers’ Compensation Act requires insurers to either make a first payment or deny a claim no later than 21 days after the employer has knowledge or notice of a claimant’s disability. • Additionally, the Rules and Regulations require that a form indicating payment or denial must be sent to the claimant, or claimant’s dependent, and the information must be filed with BWC no later than 21 days after the employee has notice or knowledge of a claimant’s disability.

Complying with the 21 -Day Requirement, continued • Medical-only claims, and claims where the employer pays salary in lieu of compensation are not reviewed for 21 -Day compliance. • For a claim to be recognized as a medical-only claim, the Claim Type Code (DN 0074) must be marked with an “M. ” • When only medical bills are paid, and there are no indemnity or specific loss payments, claims should be coded as “M” (only medical).

Complying with the 21 -Day Requirement, continued • If a claim later converts to an indemnity claim, it will be reviewed for timeliness when the first indemnity event is reported. • For a claim to be recognized as an employer paid salary in lieu of compensation claim, the Employer Paid Salary in Lieu of Compensation indicator (DN 0273) must be used.

Computation of Time When computing time, per Section 121. 3 a of the Rules and Regulations: • the day of the act, event or default is not included when computing time. • if the last day of a period falls on a Saturday, Sunday or legal state holiday, it will be calculated as the next business day.

Acknowledgements • The acknowledgement record is a transaction returned by the jurisdiction which contains information to identify the original report sent and communicates any technical business issues found. • Transactions must be analyzed so the appropriate data can be sent in the next file, including the Jurisdiction Claim Number (JCN), which must be used on subsequent transactions.

Acknowledgements, continued One of the following codes would be returned to the sender: • • • TA – Transaction Accepted – no errors TR – Transaction Rejected – errors were found and the transaction was NOT accepted HD – Batch Rejected

Resources • For further information regarding EDI Release 3 and the PA EDI Claims Implementation Guide: http: //www. dli. state. pa. us/wcais. • For information about IAIABC EDI Claims Release 3 Implementation: www. iaiabc. org. • Questions or comments: RA-CMDEDI@pa. gov.

- Slides: 60