Bundled Payments Why and Why Not Outline Why

Bundled Payments: Why and Why Not?

+ Outline Ø Why bundled payments? Ø What are current Medicare Payments? Ø What costing systems need to be developed? Ø What key factors drive bundled cost: MSDRG 469/470 2

+ Bundled Payments Ø A method for shifting payment risk to healthcare providers with the following dimensions? ü The Unit of Payment ü The Time Period ü Number of Providers ü Risk/Return Arrangements 3

+ Bundled Payments ü The Unit of Payment ü Specific Services-service intensity is issue ü Encounter -MSDRG/APCencounters are issue but not services ü Episode-Episodes are issue but not encounters ü Capitation-Episodes are not an issue 4

+ Bundled Payments ü The Time Period ü Specific number of Days 5

+ Bundled Payments ü Number of Providers At Risk ü One –Complete risk shift ü e. g. Hospital in CCJR ü Multiple-Partial risk shift 6

+ Bundled Payments ü Risk/Return Arrangements ü Collaboration Agreements ü Common Ownership-Transfer Pricing 7

+ Why Bundled Payments? Ø Medicare Insolvency 8

+ Medicare Strategies Ø Reduce Benefits Ø Reduce Beneficiaries-Increase age to match retirement Ø Reduced Covered Services Ø Increase Revenue Ø Taxes Ø Premiums Ø Reduce Service Expenditures Ø Cut Provider Payments Ø Reduce Utilization 9
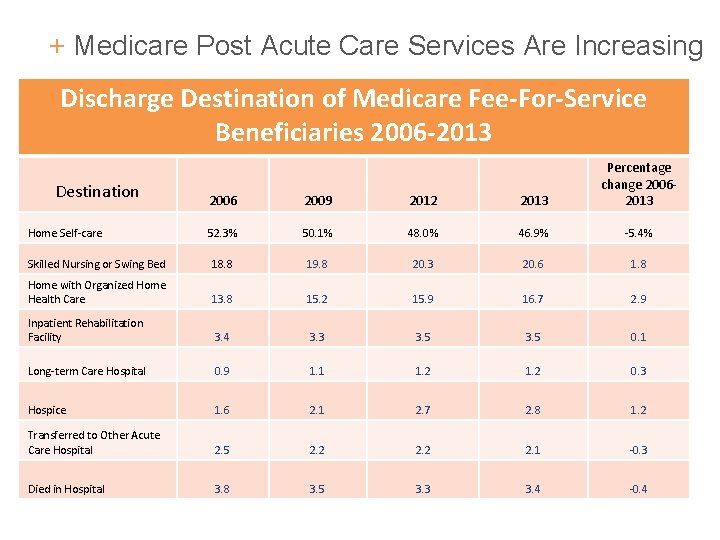
+ Medicare Post Acute Care Services Are Increasing Discharge Destination of Medicare Fee-For-Service Beneficiaries 2006 -2013 2006 2009 2012 2013 Percentage change 20062013 52. 3% 50. 1% 48. 0% 46. 9% -5. 4% Skilled Nursing or Swing Bed 18. 8 19. 8 20. 3 20. 6 1. 8 Home with Organized Home Health Care 13. 8 15. 2 15. 9 16. 7 2. 9 Inpatient Rehabilitation Facility 3. 4 3. 3 3. 5 0. 1 Long-term Care Hospital 0. 9 1. 1 1. 2 0. 3 Hospice 1. 6 2. 1 2. 7 2. 8 1. 2 Transferred to Other Acute Care Hospital 2. 5 2. 2 2. 1 -0. 3 Died in Hospital 3. 8 3. 5 3. 3 3. 4 -0. 4 Destination Home Self-care
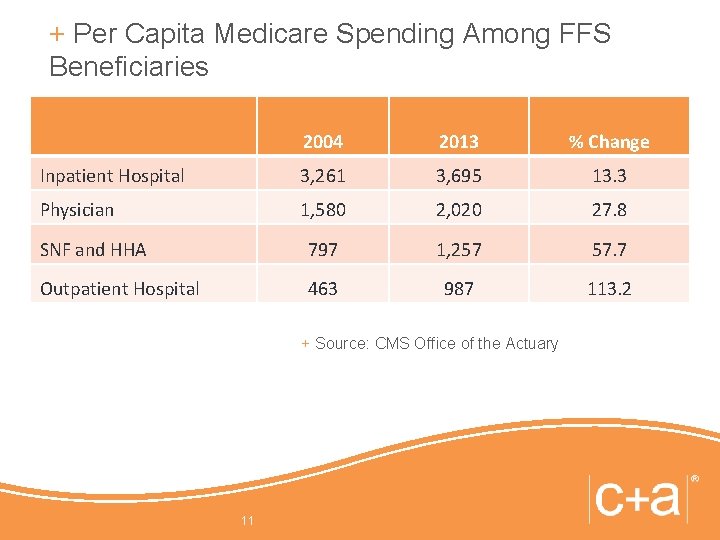
+ Per Capita Medicare Spending Among FFS Beneficiaries 2004 2013 % Change Inpatient Hospital 3, 261 3, 695 13. 3 Physician 1, 580 2, 020 27. 8 SNF and HHA 797 1, 257 57. 7 Outpatient Hospital 463 987 113. 2 + Source: CMS Office of the Actuary 11
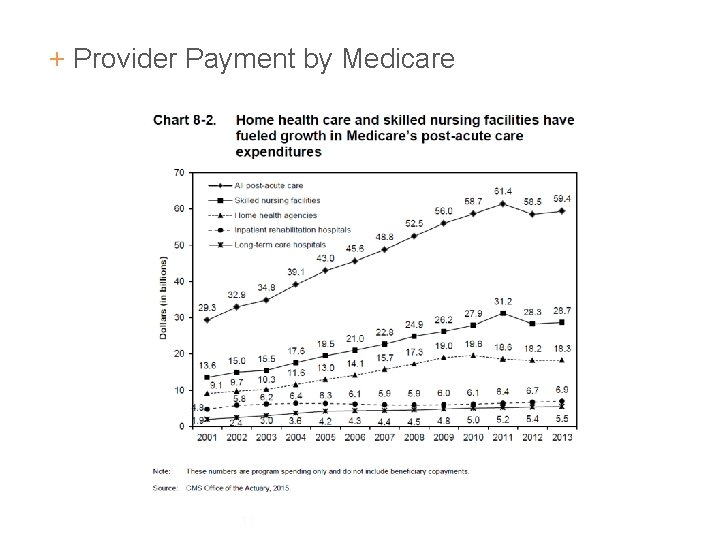
+ Provider Payment by Medicare 12
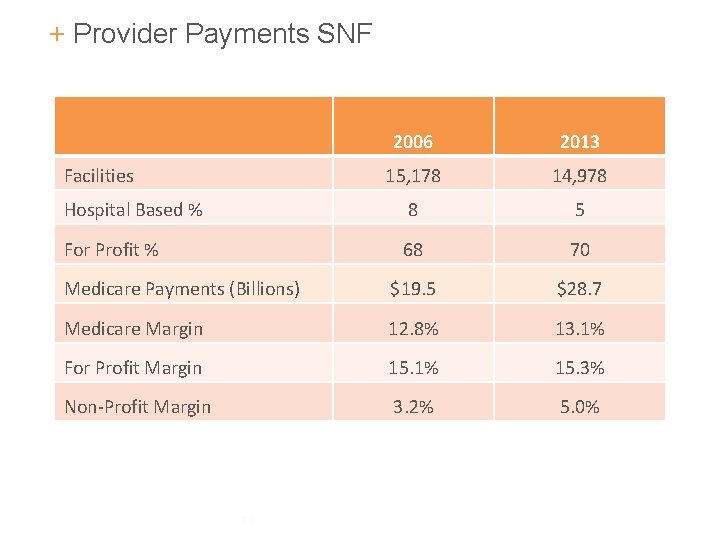
+ Provider Payments SNF 2006 2013 15, 178 14, 978 Hospital Based % 8 5 For Profit % 68 70 Medicare Payments (Billions) $19. 5 $28. 7 Medicare Margin 12. 8% 13. 1% For Profit Margin 15. 1% 15. 3% Non-Profit Margin 3. 2% 5. 0% Facilities 13
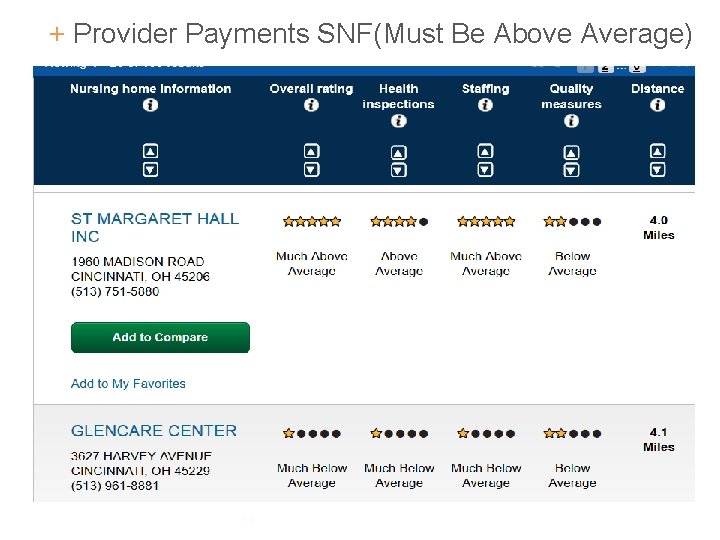
+ Provider Payments SNF(Must Be Above Average) 14
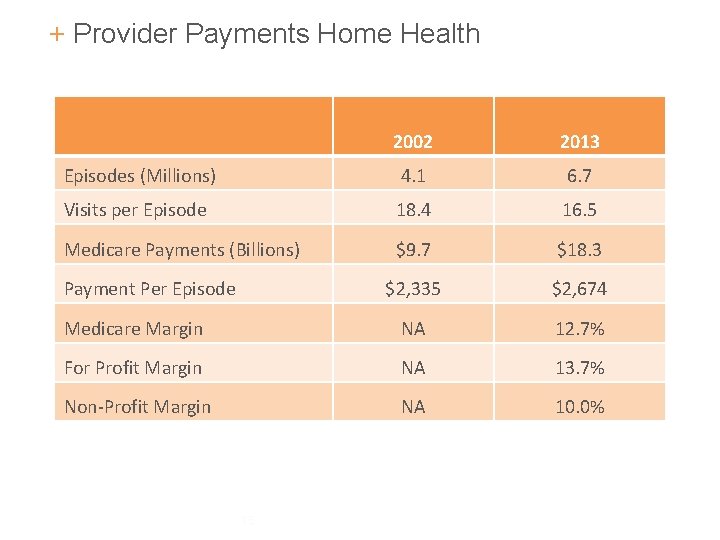
+ Provider Payments Home Health 2002 2013 Episodes (Millions) 4. 1 6. 7 Visits per Episode 18. 4 16. 5 Medicare Payments (Billions) $9. 7 $18. 3 $2, 335 $2, 674 Medicare Margin NA 12. 7% For Profit Margin NA 13. 7% Non-Profit Margin NA 10. 0% Payment Per Episode 15

+ Provider Payments Inpatient Rehab 2004 2013 495, 000 373, 000 Average LOS 12. 7 12. 9 Medicare Payments (Billions) $6. 6 $6. 8 Payment Per Case $13, 290 $18, 258 Medicare Margin 16. 7 11. 4 For Profit Margin 24. 4 23. 4 Non-Profit Margin 12. 8 1. 5 Number of IRF Cases 16
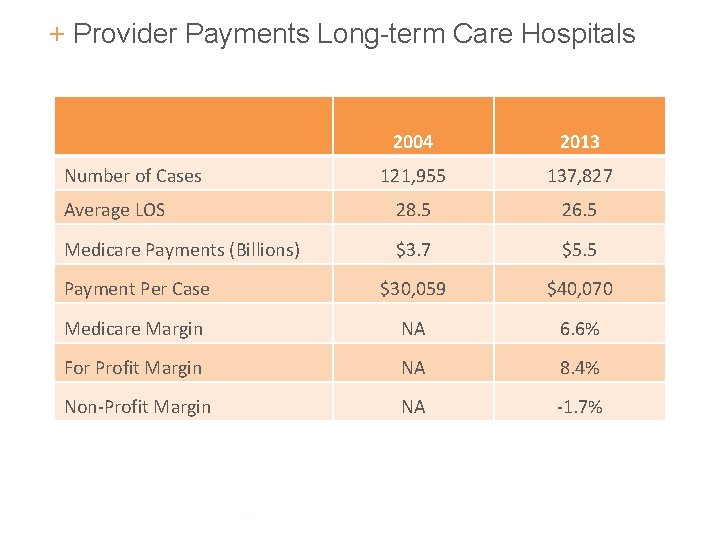
+ Provider Payments Long-term Care Hospitals 2004 2013 121, 955 137, 827 Average LOS 28. 5 26. 5 Medicare Payments (Billions) $3. 7 $5. 5 Payment Per Case $30, 059 $40, 070 Medicare Margin NA 6. 6% For Profit Margin NA 8. 4% Non-Profit Margin NA -1. 7% Number of Cases 17
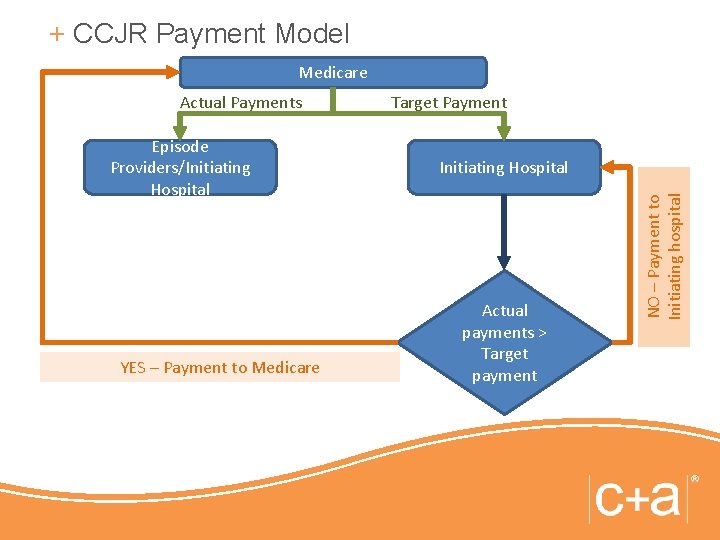
+ CCJR Payment Model Medicare Episode Providers/Initiating Hospital YES – Payment to Medicare Target Payment Initiating Hospital Actual payments > Target payment NO – Payment to Initiating hospital Actual Payments

+ Bundled Care Costing Ø Critical Questions in Cost Design Ø What are we trying to cost? Ø Episode of Care Across Providers Ø What time period is being costed? Ø Historical – Management Control Ø Future – Budgeting/Planning 19

+ Bundled Care Costing Ø Costing Framework for Bundled Payments Ø Cost= Sum of all Provider Costs Ø Costs Incurred by Hospital Ø Variable and Fixed Ø Direct Payments to Other Providers Ø By Medicare Ø By Hospital to Contracted Providers 20
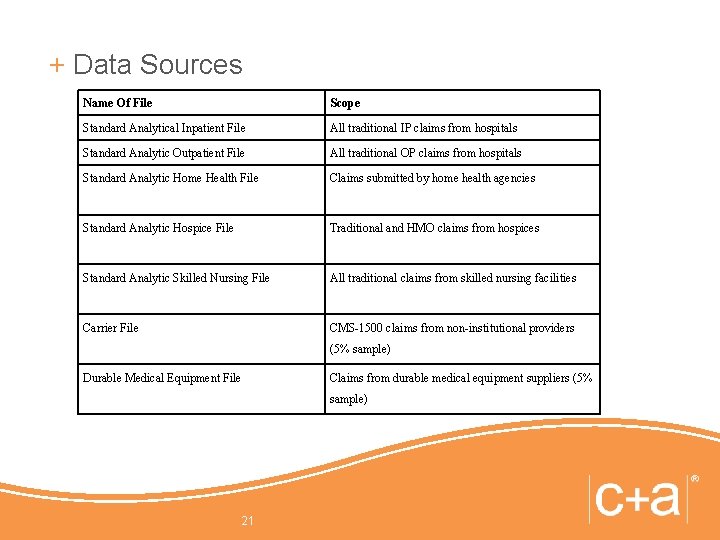
+ Data Sources Name Of File Scope Standard Analytical Inpatient File All traditional IP claims from hospitals Standard Analytic Outpatient File All traditional OP claims from hospitals Standard Analytic Home Health File Claims submitted by home health agencies Standard Analytic Hospice File Traditional and HMO claims from hospices Standard Analytic Skilled Nursing File All traditional claims from skilled nursing facilities Carrier File CMS-1500 claims from non-institutional providers (5% sample) Durable Medical Equipment File Claims from durable medical equipment suppliers (5% sample) 21
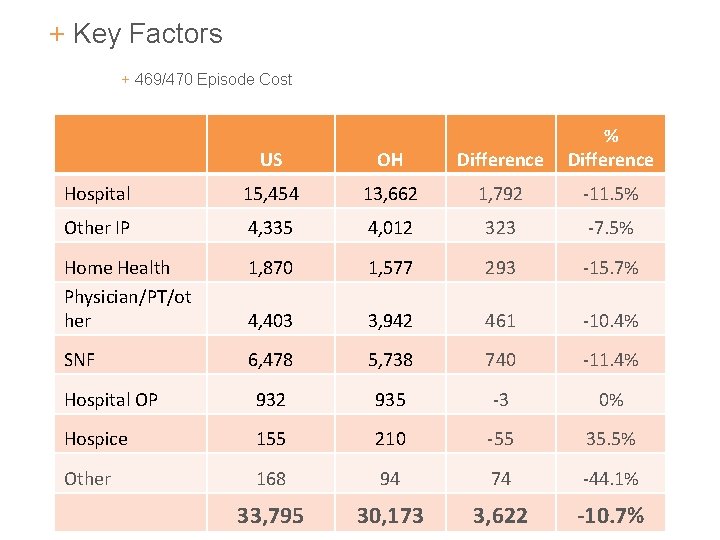
+ Key Factors + 469/470 Episode Cost US OH Difference % Difference Hospital 15, 454 13, 662 1, 792 -11. 5% Other IP 4, 335 4, 012 323 -7. 5% Home Health Physician/PT/ot her 1, 870 1, 577 293 -15. 7% 4, 403 3, 942 461 -10. 4% SNF 6, 478 5, 738 740 -11. 4% Hospital OP 932 935 -3 0% Hospice 155 210 -55 35. 5% Other 168 94 74 -44. 1% 33, 795 22 30, 173 3, 622 -10. 7%
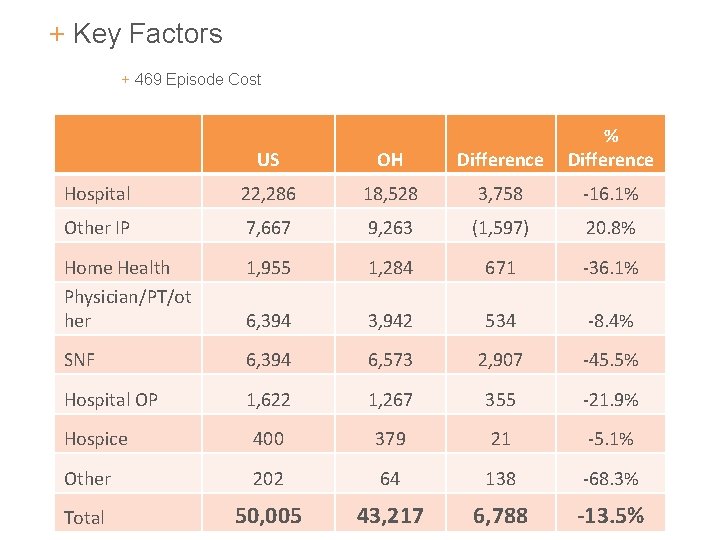
+ Key Factors + 469 Episode Cost US OH Difference % Difference Hospital 22, 286 18, 528 3, 758 -16. 1% Other IP 7, 667 9, 263 (1, 597) 20. 8% Home Health Physician/PT/ot her 1, 955 1, 284 671 -36. 1% 6, 394 3, 942 534 -8. 4% SNF 6, 394 6, 573 2, 907 -45. 5% Hospital OP 1, 622 1, 267 355 -21. 9% Hospice 400 379 21 -5. 1% Other 202 64 138 -68. 3% Total 50, 005 23 43, 217 6, 788 -13. 5%
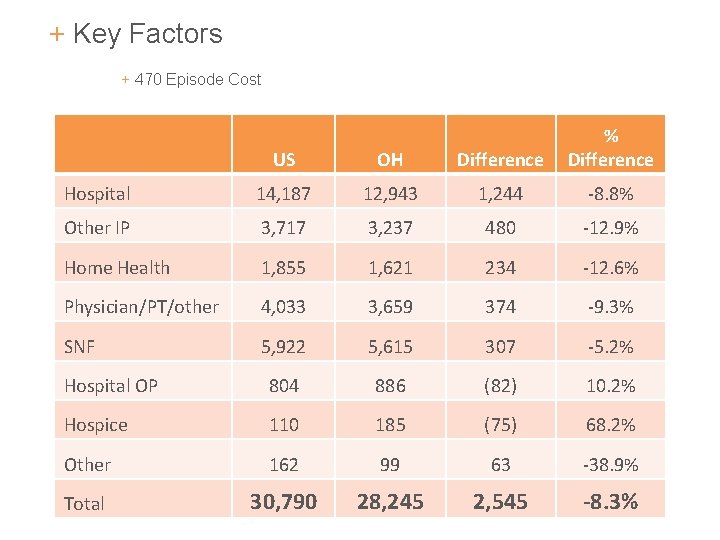
+ Key Factors + 470 Episode Cost US OH Difference % Difference Hospital 14, 187 12, 943 1, 244 -8. 8% Other IP 3, 717 3, 237 480 -12. 9% Home Health 1, 855 1, 621 234 -12. 6% Physician/PT/other 4, 033 3, 659 374 -9. 3% SNF 5, 922 5, 615 307 -5. 2% Hospital OP 804 886 (82) 10. 2% Hospice 110 185 (75) 68. 2% Other 162 99 63 -38. 9% Total 30, 790 28, 245 2, 545 -8. 3% 24
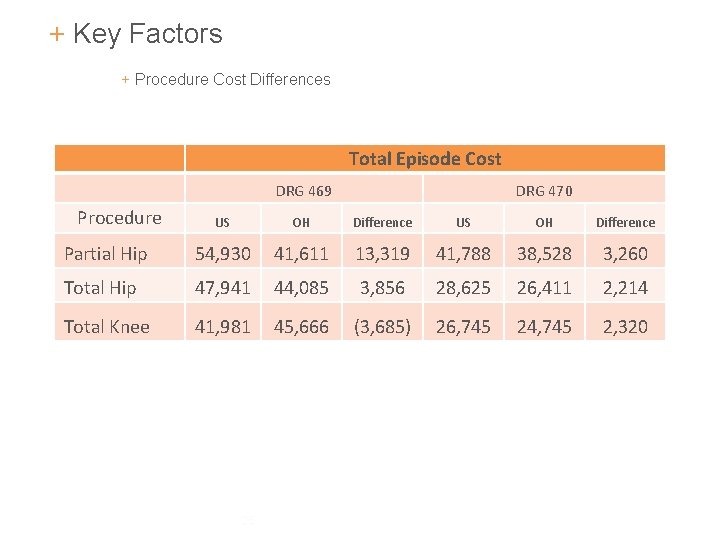
+ Key Factors + Procedure Cost Differences Total Episode Cost DRG 469 Procedure DRG 470 US OH Difference Partial Hip 54, 930 41, 611 13, 319 41, 788 38, 528 3, 260 Total Hip 47, 941 44, 085 3, 856 28, 625 26, 411 2, 214 Total Knee 41, 981 45, 666 (3, 685) 26, 745 24, 745 2, 320 25
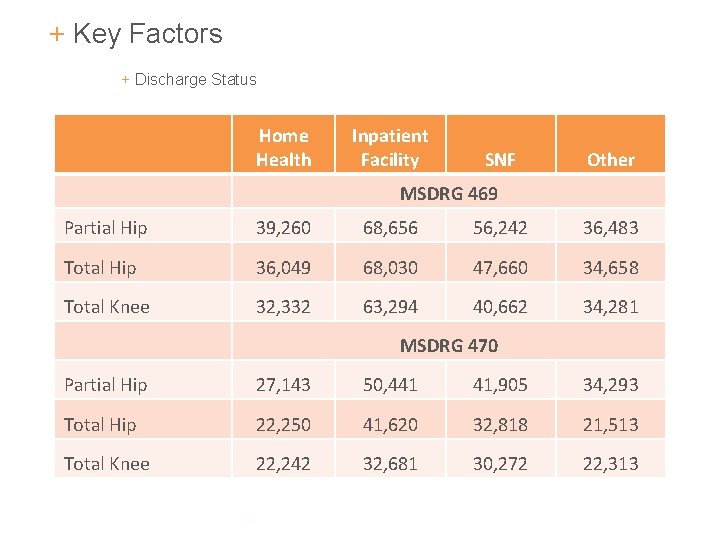
+ Key Factors + Discharge Status Home Health Inpatient Facility SNF Other MSDRG 469 Partial Hip 39, 260 68, 656 56, 242 36, 483 Total Hip 36, 049 68, 030 47, 660 34, 658 Total Knee 32, 332 63, 294 40, 662 34, 281 MSDRG 470 Partial Hip 27, 143 50, 441 41, 905 34, 293 Total Hip 22, 250 41, 620 32, 818 21, 513 Total Knee 22, 242 32, 681 30, 272 22, 313 26
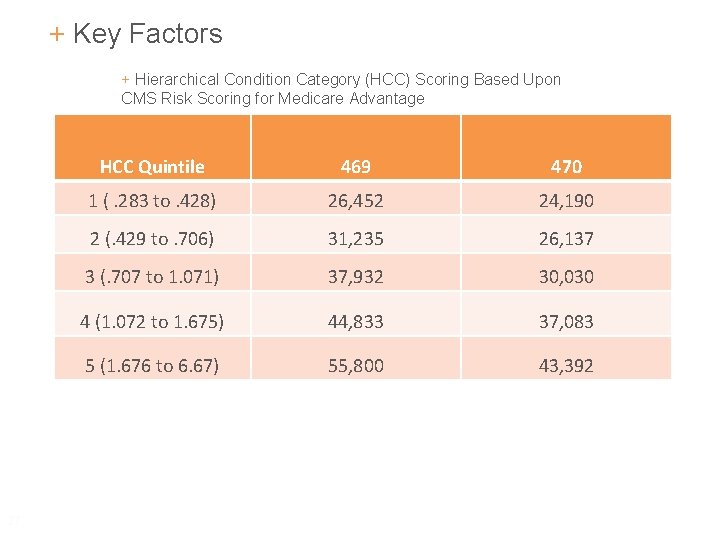
+ Key Factors + Hierarchical Condition Category (HCC) Scoring Based Upon CMS Risk Scoring for Medicare Advantage 27 HCC Quintile 469 470 1 (. 283 to. 428) 26, 452 24, 190 2 (. 429 to. 706) 31, 235 26, 137 3 (. 707 to 1. 071) 37, 932 30, 030 4 (1. 072 to 1. 675) 44, 833 37, 083 5 (1. 676 to 6. 67) 55, 800 43, 392
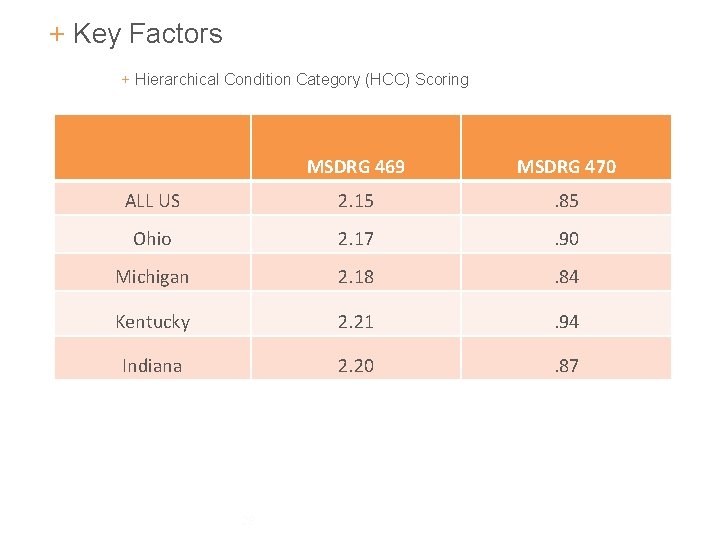
+ Key Factors + Hierarchical Condition Category (HCC) Scoring MSDRG 469 MSDRG 470 ALL US 2. 15 . 85 Ohio 2. 17 . 90 Michigan 2. 18 . 84 Kentucky 2. 21 . 94 Indiana 2. 20 . 87 28
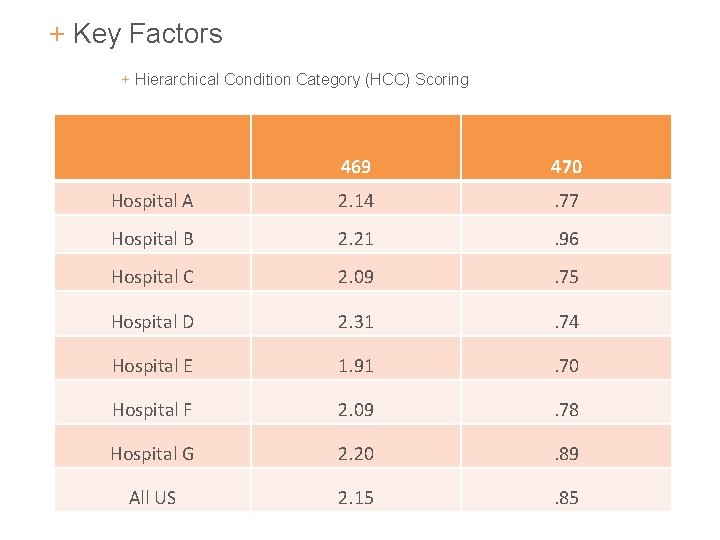
+ Key Factors + Hierarchical Condition Category (HCC) Scoring 469 470 Hospital A 2. 14 . 77 Hospital B 2. 21 . 96 Hospital C 2. 09 . 75 Hospital D 2. 31 . 74 Hospital E 1. 91 . 70 Hospital F 2. 09 . 78 Hospital G 2. 20 . 89 All US 2. 15 . 85 29
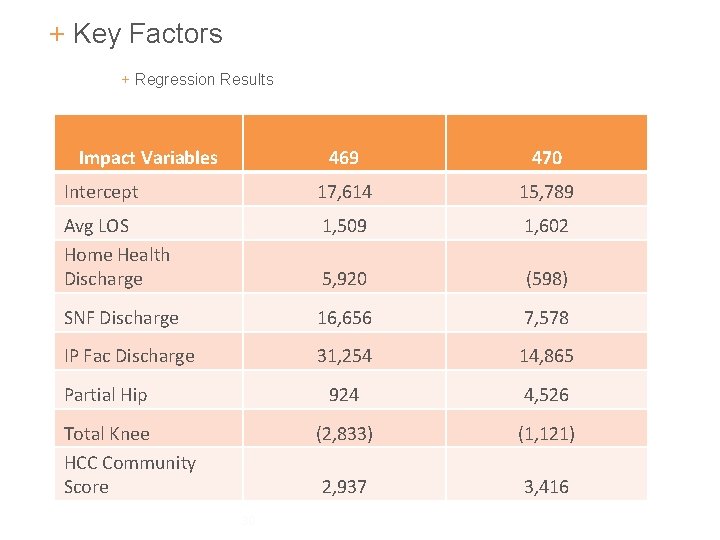
+ Key Factors + Regression Results Impact Variables 469 470 Intercept 17, 614 15, 789 Avg LOS Home Health Discharge 1, 509 1, 602 5, 920 (598) SNF Discharge 16, 656 7, 578 IP Fac Discharge 31, 254 14, 865 924 4, 526 (2, 833) (1, 121) 2, 937 3, 416 Partial Hip Total Knee HCC Community Score 30

+ Summary Ø Medicare post acute care payments are rising rapidly Ø Post acute care payments often exhibit the greatest variability in total episode cost Ø Medicare profit margins for post acute care providers have been significantly higher than hospital Medicare margins. Ø Budgeting and management control require the development of realistic benchmarks for post acute care. Ø Critical drivers of episodic cost require extensive data analysis 31

+ Thank you! Cleverley + Associates ADDRESS 438 E Wilson Bridge Rd Worthington OH 43085 WEB www. cleverleyassociates. com EMAIL info@cleverleyassociates. com PHONE 888 -779 -5663 FAX 614 -413 -3455
- Slides: 32