Bundled Payment 1 Year Later 2014 AAPMR Annual

Bundled Payment: 1 Year Later 2014 AAPM&R Annual Assembly 1
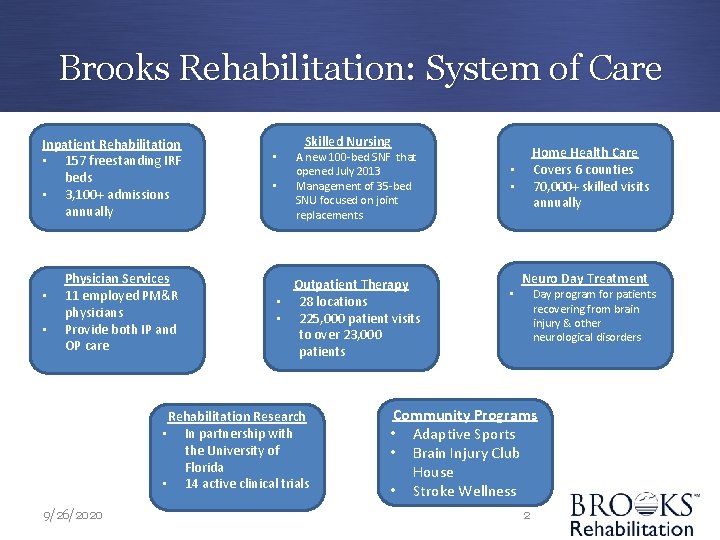
Brooks Rehabilitation: System of Care Inpatient Rehabilitation • 157 freestanding IRF beds • 3, 100+ admissions annually • • Physician Services 11 employed PM&R physicians Provide both IP and OP care • • Skilled Nursing A new 100 -bed SNF that opened July 2013 Management of 35 -bed SNU focused on joint replacements Outpatient Therapy • 28 locations • 225, 000 patient visits to over 23, 000 patients Rehabilitation Research • In partnership with the University of Florida • 14 active clinical trials 9/26/2020 Home Health Care Covers 6 counties 70, 000+ skilled visits annually • • • Neuro Day Treatment Day program for patients recovering from brain injury & other neurological disorders Community Programs • Adaptive Sports • Brain Injury Club House • Stroke Wellness 2
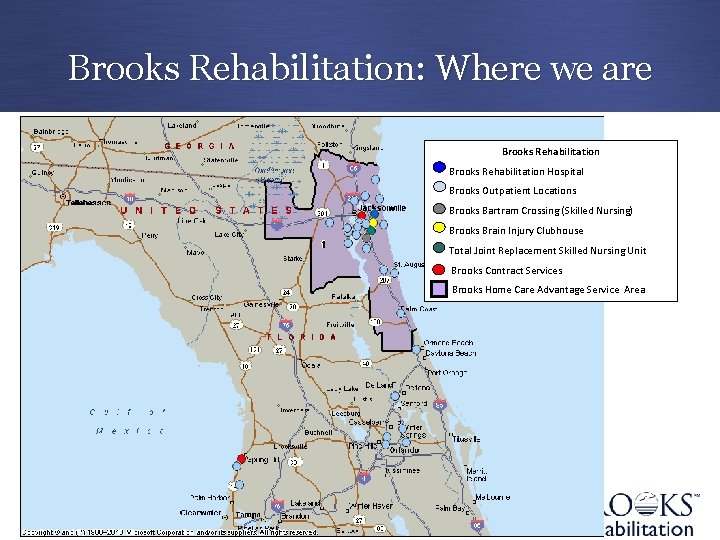
Brooks Rehabilitation: Where we are Brooks Rehabilitation Hospital Brooks Outpatient Locations Brooks Bartram Crossing (Skilled Nursing) Brooks Brain Injury Clubhouse Total Joint Replacement Skilled Nursing Unit Brooks Contract Services Brooks Home Care Advantage Service Area 9/26/2020 3

Participation in Model 3 (Includes Post-Acute Only) • Bundled payment program is referred to as Complete. Care internally & externally with its own branding: • Brooks is an “awardee convener” for a Model 3 program covering the following MS-DRG’s: MS-DRGs Rationale for selecting Hip Fractures • • • Generally a homogenous group albeit frail and elderly Generally predictable path between acute & PAC Historically, manageable rate of readmissions • • High degree of homogeneity Generally healthy Low readmission rate Great variability in PAC use, behavior driven vs. scientifically driven Total Knee & Hip Replacements • • As compared to MS-DRGs covering Stroke, CHF, COPD, etc. As an awardee convener, Brooks is financially liable for excess spending owed to CMS based on episodes that initiate in Brooks owned locations for a episode length of 60 days. Conversely, we have a financial opportunity if the total spend is less than the target • Initial target price based on Brooks 3 year historical data (2009 -2012) • Price adjusted regularly throughout demonstration to account for National trends • Target price is net of a 3% discount guaranteed to Medicare Risk phase began October 1, 2013 9/26/2020 4

Rationale for Participation in BPCI Ø Be on the forefront of possible payment reform and healthcare policy changes that might effect post-acute providers Ø Serve as a catalyst for our businesses to begin working together as a system Ø Experiment with clinical redesign Ø Have a stronger “voice” regarding future policy and payment reform changes Ø Prove that post-acute care providers have the sophistication to take “risk” and play a primary role in the continuum of care 5

Original Expectations Ø Bundled Payment would be an experiment, a form of “research” Ø Breakeven financial performance Ø Would require diversion of patients traditionally seen in Brooks Rehabilitation Hospital thereby challenging belief systems Ø We would be able to back-fill loss of patients from Brooks Rehabilitation Hospital Ø Development of the care navigator, we were not sure what it would mean Ø The need for tools that would facilitate communication between settings – we never envisioned Care. Compass Ø Would we have the ability to self-manage Medicare claims data and Brooks clinical data? 6

What has Brooks changed internally as a result of Bundled Payment? Four Primary Domains for Change Areas of Change 1. Assessment Phase • • 2. Care Coordination • • • 3. Patient and Caregiver Engagement • • • 4. Information Solutions • Nurse Liaison uses standardized tool to holistically assess patient for most appropriate first site of care (IRF, SNF, Home Health) Collaboration with acute care hospitals to better coordinate care transitions and standardize transfer paperwork Patient assigned a dedicated Care Navigator to coordinate care and educate throughout the episode Standardized evidence-based assessments used in all settings and across all clinicians at pre-determined intervals Longitudinal Care Plan developed for each patient by clinical team that spans the episode of care Patients made aware of enrollment in bundle program early on and sets expectations Care Navigator provides patient/caregiver standardized evidence-based education Care Navigator stays connected to patient post discharge via phone and home visits One IT tool (Care Compass) that brings information from disparate systems and is a repository for all information; helps monitor patient throughout episode
Care Compass - Assists clinical team in prioritizing patients, predicting future needs, and alerts of declining status - Updates every 2 -4 hours with key metrics

General BPCI Volume Statistics • Cases triggering a Brooks Model 3 bundle since going live October 1, 2 o 13 through August 31, 2014 – Joint replacement cases = 665 – Hip fracture cases = 182 – Total cases = 847 9
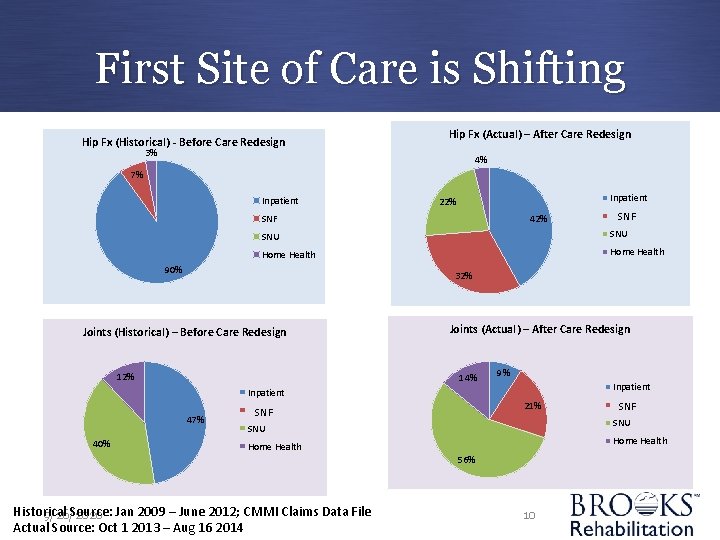
First Site of Care is Shifting Hip Fx (Historical) - Before Care Redesign Hip Fx (Actual) – After Care Redesign 3% 4% 7% Inpatient 22% 42% SNF SNU Home Health 90% 32% Joints (Historical) – Before Care Redesign 12% Joints (Actual) – After Care Redesign 14% 9% Inpatient 47% 40% Bartram SNF Crossing 21% Bartram SNF Crossing SNU Home Health 56% Historical Source: Jan 2009 – June 2012; CMMI Claims Data File 9/26/2020 Actual Source: Oct 1 2013 – Aug 16 2014 Bartram SNF Crossing 10
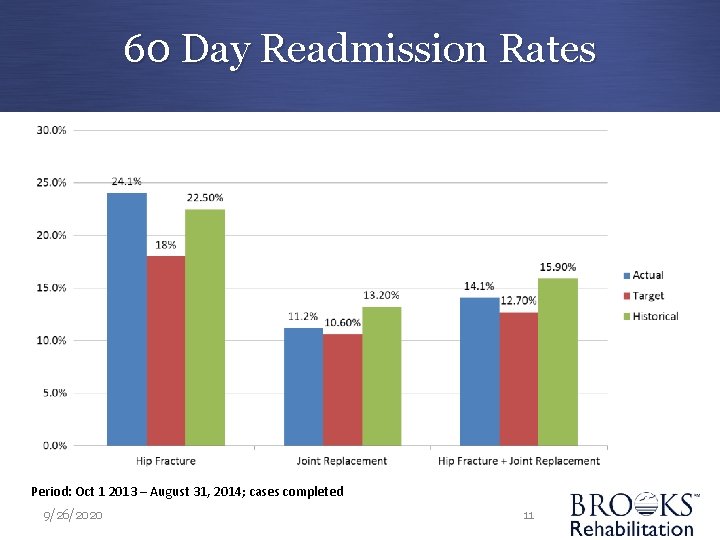
60 Day Readmission Rates Period: Oct 1 2013 – August 31, 2014; cases completed 9/26/2020 11
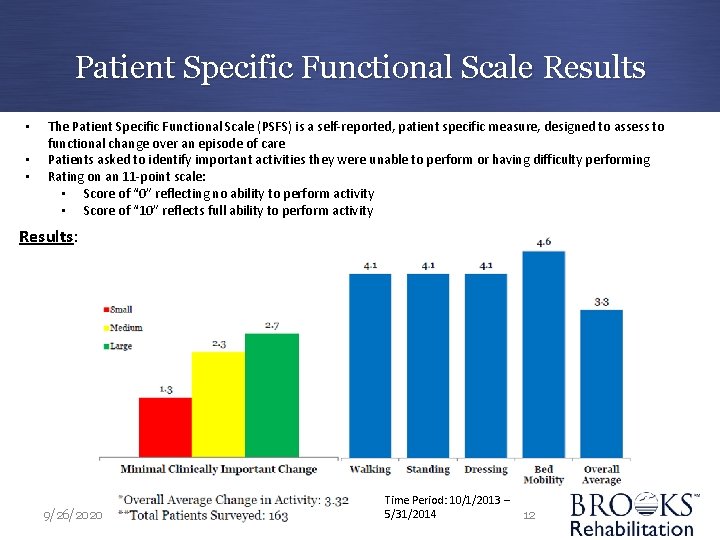
Patient Specific Functional Scale Results • • • The Patient Specific Functional Scale (PSFS) is a self-reported, patient specific measure, designed to assess to functional change over an episode of care Patients asked to identify important activities they were unable to perform or having difficulty performing Rating on an 11 -point scale: • Score of “ 0” reflecting no ability to perform activity • Score of “ 10” reflects full ability to perform activity Results: 9/26/2020 Time Period: 10/1/2013 – 5/31/2014 12
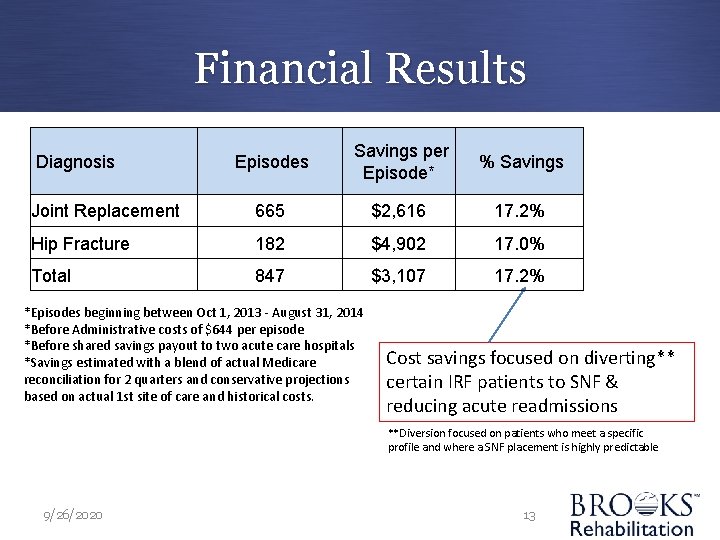
Financial Results Episodes Savings per Episode* % Savings Joint Replacement 665 $2, 616 17. 2% Hip Fracture 182 $4, 902 17. 0% Total 847 $3, 107 17. 2% Diagnosis *Episodes beginning between Oct 1, 2013 - August 31, 2014 *Before Administrative costs of $644 per episode *Before shared savings payout to two acute care hospitals *Savings estimated with a blend of actual Medicare reconciliation for 2 quarters and conservative projections based on actual 1 st site of care and historical costs. Cost savings focused on diverting** certain IRF patients to SNF & reducing acute readmissions **Diversion focused on patients who meet a specific profile and where a SNF placement is highly predictable 9/26/2020 13

Overall Performance Ø Financial performance has far exceeded expectations Ø It is extremely difficult to make large meaningful improvements in hospital readmissions rates – we have barely scratched the surface of the work we need to do Ø Patient self reporting of their functional improvements is extremely strong Ø Patient experience matches our overall high performance of our individual businesses Ø We have gained tremendous experience managing Medicare claims data and internal clinical data Ø Savings is very asymmetrical across our different referral partners 14
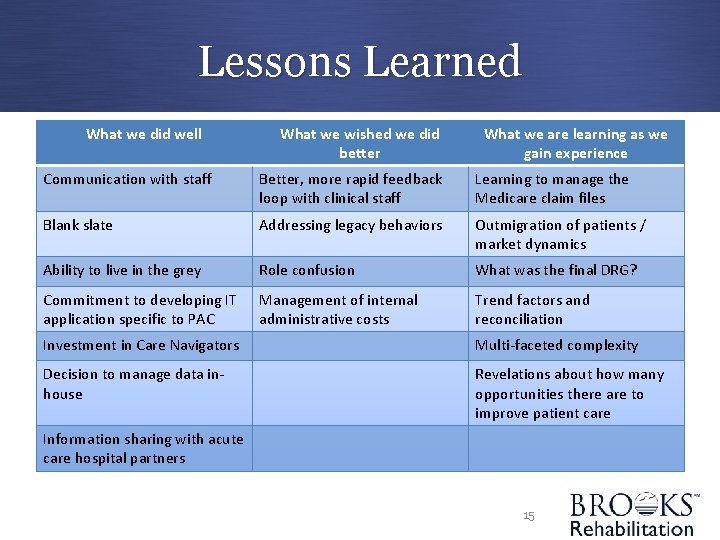
Lessons Learned What we did well What we wished we did better What we are learning as we gain experience Communication with staff Better, more rapid feedback loop with clinical staff Learning to manage the Medicare claim files Blank slate Addressing legacy behaviors Outmigration of patients / market dynamics Ability to live in the grey Role confusion What was the final DRG? Commitment to developing IT application specific to PAC Management of internal administrative costs Trend factors and reconciliation Investment in Care Navigators Multi-faceted complexity Decision to manage data inhouse Revelations about how many opportunities there are to improve patient care Information sharing with acute care hospital partners 15

Next Steps for Brooks Rehabilitation • Evaluate BPCI expansion to other diagnoses • Possibilities include CHF, Stroke, and Spinal Fusions • Would go at risk for the new episodes on April 1, 2015 • Use Complete. Care To Serve as the Brooks “System of Care Roadmap (regardless of BPCI participation) • Use learnings with other patient populations as best practice model • Begin adoption of the Complete Care Clinical Model With Other Inpatient Populations • New thinking and training for clinicians • Standardization in clinical programming • Competencies in care planning and coordination • Longitudinal care planning - Thinking beyond own setting 16

Observations and Possible Future Implications for Post-Acute Providers and Physicians • Post Acute represents a large portion of the cost of an episode of care and the increased scrutiny of PAC utilization will continue • Will lead to a decline in utilization of high cost settings – Less IRF admissions – Will require IRFs to develop new programs to offset loss of volume • Increased attention on physician driven metrics which drive costs – LOS, Discharge settings, Readmission rates • Physician gain sharing opportunities • Dramatic shifts in physician referral patterns • Physician differentiation based on being a high quality low cost provider • Close coordination and buy in from surgeons and PM&R physicians is a key success factor
- Slides: 17