Building Bridges Improving Health through Program Integration Ethnic

Building Bridges: Improving Health through Program Integration Ethnic Myths: Implications for Chronic Care Management Sharon A. Brown, Ph. D, RN, FAAN Professor and Associate Dean for Research Director, Cain Center for Nursing Research The University of Texas at Austin School of Nursing

OBJECTIVES • List 3 cultural myths related to racial, ethnic, or cultural norms about health… • Describe 2 strategies for addressing these myths in chronic care management and their ethical implications • Discuss 3 ethical principles of providing care that is culturally competent
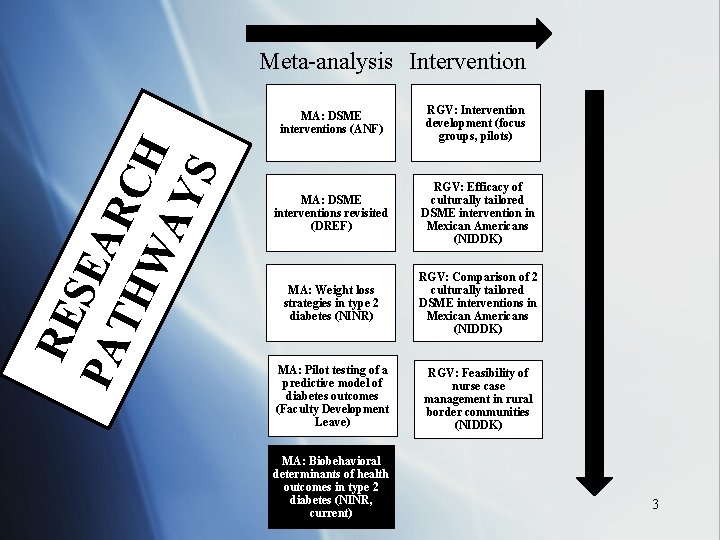
RE S PA EAR TH C WA H YS Meta-analysis Intervention MA: DSME interventions (ANF) RGV: Intervention development (focus groups, pilots) MA: DSME interventions revisited (DREF) RGV: Efficacy of culturally tailored DSME intervention in Mexican Americans (NIDDK) MA: Weight loss strategies in type 2 diabetes (NINR) RGV: Comparison of 2 culturally tailored DSME interventions in Mexican Americans (NIDDK) MA: Pilot testing of a predictive model of diabetes outcomes (Faculty Development Leave) RGV: Feasibility of nurse case management in rural border communities (NIDDK) MA: Biobehavioral determinants of health outcomes in type 2 diabetes (NINR, current) 3

CULTURAL MYTHS • • • Recruitment / Retention Genetic Predisposition / “Fatalism” Gender Roles Acculturation & Dietary Practices Breaking barriers with “Promotoras” (CHWs)

ETHICAL PRINCIPLES RESPECT FOR PERSONS Individuals are autonomous Protect those with diminished autonomy BENEFICIENCE Do no harm Maximize possible benefits / minimize possible harms JUSTICE: to each person… an equal share according to individual need according to merit

RESEARCH MOTIVATION Growing diabetes epidemic Tight glucose control reduces complications by 25%-75% (DCCT, UKPDS) Glucose control —> 6 years of additional life $174 billion spent annually Less than 30% achieve glycemic control

Predicted growth of the Hispanic population U. S. population: 296 million (2005) 438 million (2050, immigrants) Latinos: largest minority group (14%) will triple in size Whites: will become a minority (47%) Elderly: ≥ double in size Source: Passel, J. S. , & Cohn, D. (2008). U. S. population projections: 2005 -2050. Washington, DC: Pew Research Center.
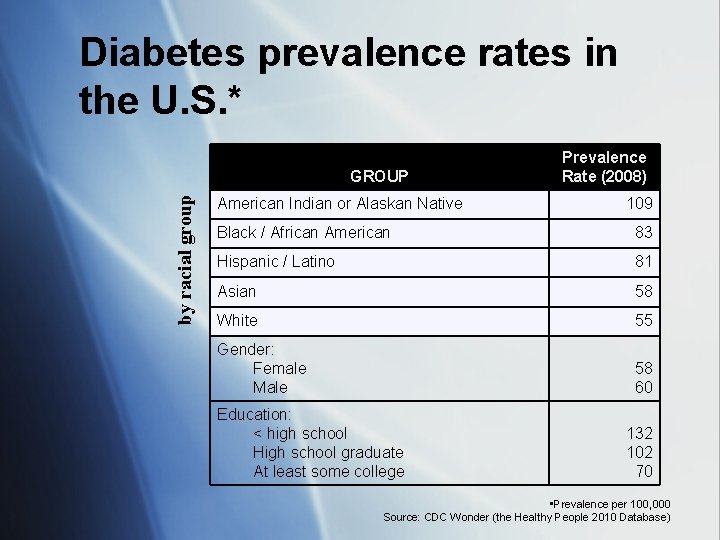
Diabetes prevalence rates in the U. S. * by racial group GROUP American Indian or Alaskan Native Prevalence Rate (2008) 109 Black / African American 83 Hispanic / Latino 81 Asian 58 White 55 Gender: Female Male 58 60 Education: < high school High school graduate At least some college 132 102 70 • Prevalence per 100, 000 Source: CDC Wonder (the Healthy People 2010 Database)
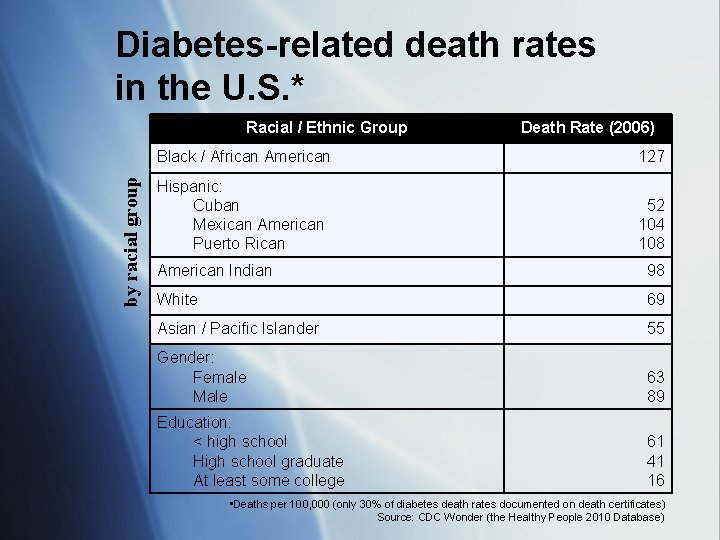
Diabetes-related death rates in the U. S. * by racial group Racial / Ethnic Group Death Rate (2006) Black / African American 127 Hispanic: Cuban Mexican American Puerto Rican 52 104 108 American Indian 98 White 69 Asian / Pacific Islander 55 Gender: Female Male 63 89 Education: < high school High school graduate At least some college 61 41 16 • Deaths per 100, 000 (only 30% of diabetes death rates documented on death certificates) Source: CDC Wonder (the Healthy People 2010 Database)
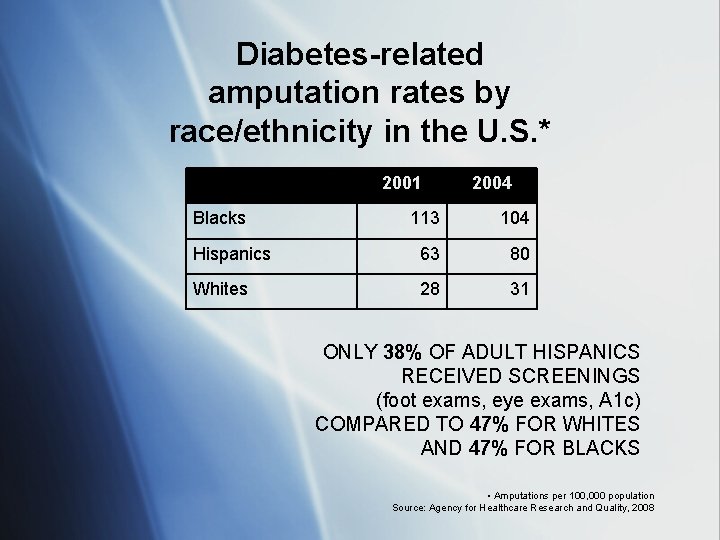
Diabetes-related amputation rates by race/ethnicity in the U. S. * 2001 Blacks 2004 113 104 Hispanics 63 80 Whites 28 31 ONLY 38% OF ADULT HISPANICS RECEIVED SCREENINGS (foot exams, eye exams, A 1 c) COMPARED TO 47% FOR WHITES AND 47% FOR BLACKS • Amputations per 100, 000 population Source: Agency for Healthcare Research and Quality, 2008

Diabetes Prevention Program RESULTS Diet and exercise Group 1 Coaching in healthy lifestyle designed to promote weight loss (diet & physical activity) Diet & physical activity (walking) reduced risk of diabetes by 58% Diabetes drug Group 2 Metformin Reduced risk of diabetes by 31% Consistent across populations Highest reduction Group 3 Placebo achieved by people over age 60 in diet & exercise group – a 71% reduction
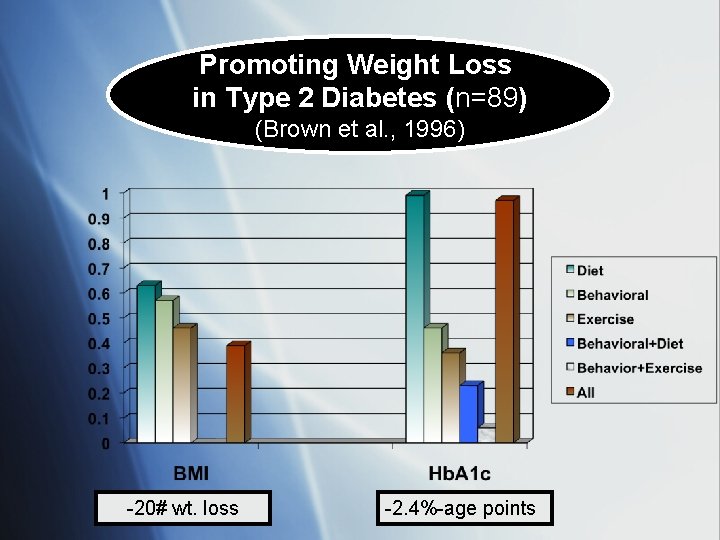
Promoting Weight Loss in Type 2 Diabetes (n=89) (Brown et al. , 1996) -20# wt. loss -2. 4%-age points

DSME EFFECTS At least a 1. 0%-age point reduction in Hb. A 1 c (reduces death by 10%, microvascular end points by 25%) Consistent positive effects in studies that included: • Cultural tailoring • Community educators / lay people • One-on-one interventions w/ individualized assessment • Treatment algorithms • Behavior-related tasks • Feedback • High-intensity interventions (>10 contacts, ≥ 6 mos. ) Glazier et al. (2006). A systematic review of interventions to improve diabetes care in socially disadvantaged populations. Diabetes Care, 29, 1675 -1688.

The Starr County Border Health Initiative 14

STARR COUNTY, TEXAS

SETTING: Starr County Population: 62, 249 97. 5% Hispanic Poorest county in Texas - 3 rd poorest in U. S. Unemployment rate 11. 9% (2008) Per capita income $10, 716 (2008) Young population — 10% > 65 years of age 2, 200+ colonias on the border — 400, 000 people Diabetes affects 50% of adults over age of 35 (Hanis, 1983) 50% of health care obtained in Mexico Lower RGV has highest diabetes-related death rate Native American admixture contributes to risk/ethnic differences Hispanics labeled “noncompliant” — more likely treated with insulin Population: MD = 7657: 1 (3789: 1 rest of TX) Population: RN = 851: 1 (159: 1 rest of TX) Source: Texas Secretary of State, http: //www. sos. state. tx. us/border/colonias/faqs. shtml

SETTING: Starr County 17

SETTING: Starr County 18

COMMUNITY ASSESSMENT Understanding of diabetes: “Blood sugar” or blood glucose testing / results “God’s will” (“fatalism” but generational differences) Will “get diabetes” eventually (“fatalism” or reality? ) Previous diabetes-related experiences: Told not to eat cultural food preferences Previous weight loss “failures” Feared insulin injections Diabetes care from both sides of the border Folk remedies (generational differences) Suggestions for a diabetes intervention: Interested in DSME No complicated exchange lists No brochures (low literacy rates among elderly) Involve family members (low levels of support) Reduce fat intake (lard)

health literacy “a stronger predictor of health than age, income, employment status, education level, and race” Source: Report of the Council of Scientific Affairs, Ad Hoc Committee on Health Literacy for the Council on Scientific Affairs, American Medical Association, JAMA, Feb 10, 1999

Populations Vulnerable to Poor Health Literacy • Minority / immigrant populations • Low income: 1/2 Medicare/Medicaid recipients read <5 th grade level • People w/ chronic health conditions • Elderly: 2/3 have inadequate literacy Source: National Network of Libraries of Medicine (nnlm. gov) Williams, MV. JAMA, December 1995

Consequences of poor health literacy • Take meds. on erratic schedules • Miss follow-up appointments • Do not understand instructions (81% of patients ≥ 60 years of age at public hospital could not read or understand basic materials such as prescription labels) Source: IOM, Health Literacy: A Prescription to End Confusion Williams, MV. JAMA, December 1995
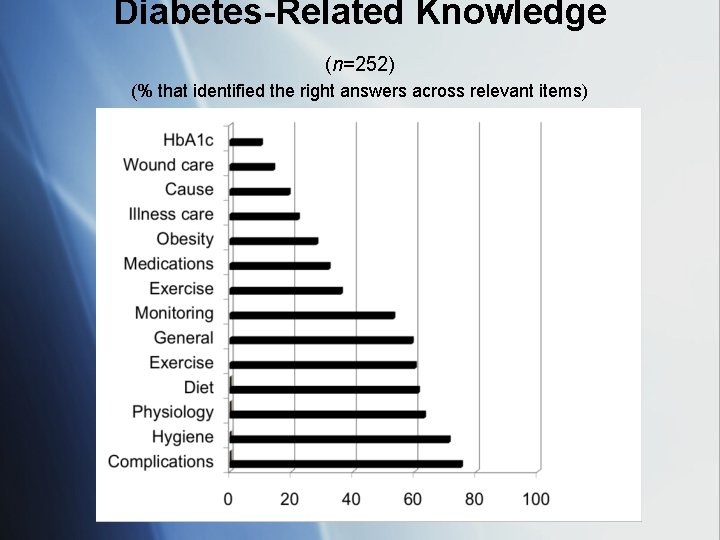
Diabetes-Related Knowledge (n=252) (% that identified the right answers across relevant items)

Consequences of poor health literacy in Starr County § Self-prescribing of medications and other treatments § Misinterpretation of symptoms — did not perceive symptoms as serious § Misinterpretation of HCP recommendations § Misunderstanding of health experiences of family and friends

CULTURAL MYTHS? • • • Recruitment / Retention Genetic Predisposition / “Fatalism” Gender Roles Acculturation & Dietary Practices Breaking barriers with “Promotoras” (CHWs)

STARR COUNTY STUDIES Recruitment: 95% Retention: 81 -90% Language Family-centered Non-judgmental approach Transportation CULTURAL COMPETENCE Matches superficial characteristics of the culture (e. g. , food, music) Integrates deep structure of the culture (social, historical, environmental, psychological factors) Flexible scheduling Reminders — telephone, calendars Benefits — feedback, intervention, monitoring, rewards Snacks of healthy Mexican American foods

SAMPLE CHARACTERISTICS 64% female 54 years of age on average (range 35 -70) 20% on insulin 38% use alternative remedies (garlic, chaya) 8 years average diabetes duration (range 1 -25) Scored low (1. 0) on acculturation scale (0 -4) 90% preferred speaking Spanish

CULTURAL MYTHS? • • • Recruitment / Retention Genetic Predisposition / “Fatalism” Gender Roles Acculturation & Dietary Practices Breaking barriers with “Promotoras” (CHWs)

INTERVENTIONS Culturally tailored education + group support: 52 contact hours (“extended”) 22 contact hours (“compressed”) Series of Spanish-language videotapes Instructors: RNs & RDs + promotoras Social support: family members, friends, groups Community-based settings (churches, schools) 1, 100+ study participants

“Diabetes y Su Salud”

MEASURES Hb. A 1 c FBG BMI Cholesterol BP Leptin Triglycerides Microalbuminuria Complications Demographics Health history Acculturation Diabetes knowledge Health beliefs Family history Medication history Fat intake Food frequency Physical activity
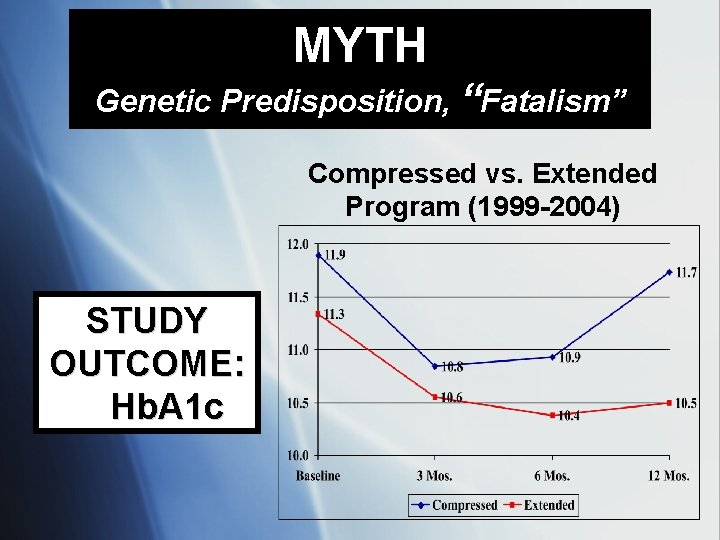
MYTH Genetic Predisposition, “Fatalism” Compressed vs. Extended Program (1999 -2004) STUDY OUTCOME: Hb. A 1 c
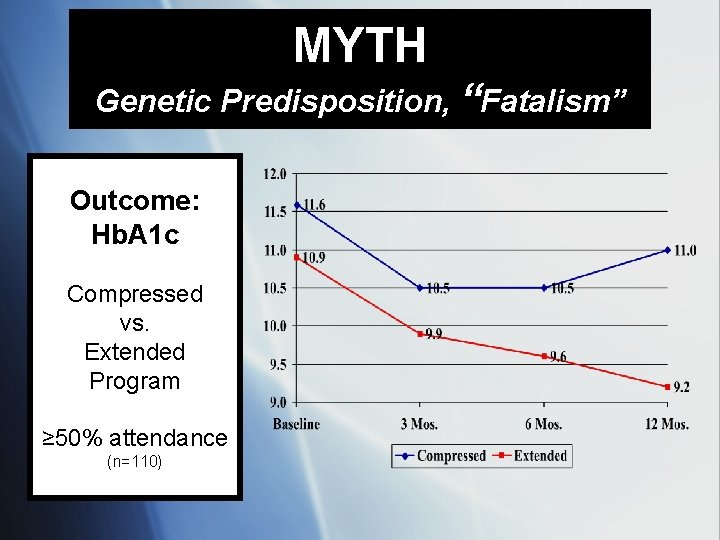
MYTH Genetic Predisposition, “Fatalism” Outcome: Hb. A 1 c Compressed vs. Extended Program ≥ 50% attendance (n=110)
Dosage Effects of Program Attendance Top 10% achievers in reducing Hb. A 1 c Bottom 10% achievers in reducing Hb. A 1 c n=20 • Attended 57% • -6%-age pts • Mean age: 54. 8 • Attended 37% • +3%-age pts • Mean age: 53. 9

CULTURAL MYTHS? • • • Recruitment / Retention Genetic Predisposition / “Fatalism” Gender Roles Acculturation & Dietary Practices Breaking barriers with “Promotoras” (CHWs)

MYTH: Gender Roles HEALTH BELIEFS § Control over diabetes males (F=4. 1, p=. 05) § Social support males (F=6. 1, p=. 01) METABOLIC CONTROL § Hb. A 1 c levels lower in males (t=3. 11, p=. 002) § Males with greater attendance achieved greater improvements in Hb. A 1 c

CULTURAL MYTHS? • • • Recruitment / Retention Genetic Predisposition / “Fatalism” Gender Roles Acculturation & Dietary Practices Breaking barriers with “Promotoras” (CHWs)

MYTH: Acculturation & Dietary Practices (weight & type 2 diabetes) Returning native cultures to traditional cultural diets significantly improves glucose intolerance and insulin resistance Recommendations: • Walk 30 minutes per day • Lose 5 -7% body wt ( 500 -1000 kcal)

CULTURAL MYTHS? • • • Recruitment / Retention Genetic Predisposition / “Fatalism” Gender Roles Acculturation & Dietary Practices Breaking barriers with “Promotoras” (CHWs)

MYTH — Breaking barriers: “Promotoras” (CHW) “…a community health safety net and a natural extension of the health and human services agencies, improve health at the neighborhood level. ” • Latin American program-type for underserved populations • peer liaisons — advocacy, interpersonal relations, capacity building, communication, knowledge, organization, teaching, service coordination • beyond community health worker model: speak the same language come from the same neighborhood • tend to be women [Nichols et al. , Prev Chronic Dis, Nov 2005]

Promotoras: a cautionary tale Focus group input: promotoras not acceptable as group leaders Anecdotal evidence: individuals consider the use of the promotora model as racial Starr County promotora role: • Data collection • Recruitment • Telephone contact / reminders • Transportation • Motivation • Logistical support (intervention sites, materials) • Grocery shopping / preparation of snacks

ETHICAL PRINCIPLES RESPECT FOR PERSONS Individuals are autonomous Protect those with diminished autonomy Best predictor of health — health literacy Cultural myths — “fatalism, ” generational differences Promotora model Heterogeneity within cultures Use of focus groups Language issues

Community-based research • takes place in community settings • involves community members in the design and implementation of research projects Principles: Community involved at the earliest stages Community influences project Research processes & outcomes benefit community Community hired and trained whenever possible Community part of data interpretation; input into how results are distributed Partnerships should last beyond the project Community empowered to initiate their own projects Source: http: //sph. washington. edu/research/community. asp

ETHICAL PRINCIPLES BENEFICIENCE Do no harm Maximize possible benefits / minimize possible harms Alarming self-management practices Integrate DSME into other aspects of treatment Family involvement / social support Home glucose self-monitoring Socioeconomic constraints Real environmental barriers Physiologic barriers to improved glycemia

ETHICAL PRINCIPLES JUSTICE: to each person… Mexican Americans / Hispanics least studied group Hispanic health disparities: ü lower rates of health screenings — 38% vs. 47% for whites and blacks ü higher diabetes prevalence rates — 1. 5 x whites ü higher diabetes-related deaths — 1. 5 x whites Average Hb. A 1 c reduction with effective DSME interventions across all groups — 2. 4%-age points Average Hb. A 1 c reduction attained with DSME culturally tailored for socially disadvantaged groups — ≥ 1. 0%-age points Few minority health professionals

Estimated Intervention Costs Extended Care Compressed Care (RN, RD, & promotora) (RN or RD and promotora) • 26 sessions • $384/person • 11 sessions • $131/person

RESEARCH TEAM Craig Hanis, Ph. D, Co-PI (Professor, UT-Houston School of Public Health) Alexandra García, RN, Ph. D, Co-I (Associate Professor, UT Austin School of Nursing) Kamiar Kouzekanani, Ph. D, Co-I (Statistician, UT Austin [previously]) Philip Orlander, MD, Consultant / Co-I (Chair, Division of Endocrinology, UT-Houston Medical School) Research Associates Maria Winchell, MS Mary Winter, MSN

RIO GRANDE VALLEY STAFF Intervention Staff Evangelina Villagomez, MSN, RN Mario Segura, MSN, RN Lilia Fuentes, MSN, RN Lita Silva, MSN, RN, CDE Nora Morín Siller, RD, LD Maria Olivia Garza, RD, LD Ana Gonzalez, MS, RD, CDE Norma Cottrell, RD Mila Villareal, MSN, RN Juan Jesús Treviño, BS, LD Patricia Ramírez, RD, LD Rogelio Contreras, RN Celia Zuñiga, RN Emiliana Guerra, RD Sylvia Cardenas, RN, FNP Ventura Huerta, RN, BSN, MPH Starr County Field Office Hilda Guerra, Manager Sylvia Hinojosa Marie López Imelda Martínez Alma Martínez Jesusa L. Salmón Maricela Garza Maria Coder Umbelina Reyna Minerva Margo Elva Yolanda Morado Maria Garza Clara Treviño Elizabeth Peña

e d un F . . . y db State of Texas University of Texas at Austin University of Texas at Houston Office of Research in Minority Health
- Slides: 49