Bugs and Drugs Solving the Antibiotic Dilemma Catherine

Bugs and Drugs: Solving the Antibiotic Dilemma Catherine Davis, Pharm. D. Exempla Saint Joseph Hospital

Presentation Overview Briefly review sensitivity testing l Review advantages/disadvantages of commonly prescribed antibiotics l Provide recommendations for appropriate indications for various antibiotics l
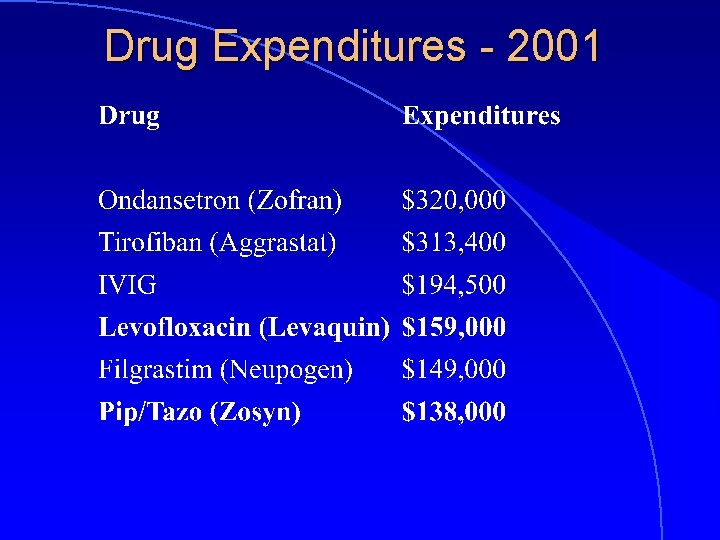
Drug Expenditures - 2001

Challenges in Antimicrobial Selection Changing resistance patterns l New antibiotics from which to select l National Backorders!!! l – Piperacillin/tazobactam – Cefotaxime – Cefotetan – Penicillin – Cefazolin

Sensitivity Testing Minimum Inhibitory Concentration MIC - concentration at which the growth of the organism is inhibited l “breakpoint” is determined based on serum/tissue levels of respective agent l optimum therapy is for peak to achieve > 8 times the MIC l CANNOT compare actual #’s between different classes of antibiotics l

MIC Interpretation If the sensitivity report indicates an MIC less than a specific concentration (i. e. <8), antibiotic in question should achieve adequate concentrations to inhibit growth l Review all agents listed as susceptible and select the most narrow spectrum/cost effective agent that will cover the organism l

Antibiotic Selection: The Right Agent for the Right Patient l l l l l Infecting organism Susceptibility data/local resistance patterns Site of infection Duration of hospitalization/prior antibiotics Allergy history Age Renal/Hepatic status Immunologic status Pregnancy

Antibiotic Classes l Beta-Lactams – penicillins – cephalosporins – carbapenems – monobactams l Quinolones Aminoglycosides l Glycopeptides l Macrolides l Miscellaneous l VRE Antibiotics l

Penicillins: Pen VK, Ampicillin, Amoxicillin Advantages l good oral absorption l good gram + coverage Disadvantages l frequent dosing l increasing resistance – Enterococcus – Streptococcus l inexpensive – gram negatives – Strep pneumo l inactivates aminoglycosides

Penicillin, Ampicillin, Amoxicillin: Indications for Use Strep infections known to be PCN sensitive l Enterococcus infections (dose 2 Gms q 4 h for ampicillin + gentamicin synergy dosed) l Necrotizing fasciitis - PCN 24 MU/day + Clinda 600 mg q 8 h l Renal adjust for Cr. Cl <30 m. L/min l

Anti. Staphylococcal PCN’s Nafcillin, Oxacillin, Dicloxacillin Advantages l excellent Staph aureus coverage – best treatment option for serious MSSA infections l l narrow spectrum (no gram negative coverage) Diclox for Staph Disadvantages l frequent dosing (2 Gms q 4 -6 h) l increasing incidence of MRSA (35% at ESJH) l no Enterococcus coverage

Beta-Lactamase Inhibitors Amoxicillin/Clavulanate (Augmentin®) l Ampicillin/Sulbactam (Unasyn®) l Piperacillin/Tazobactam (Zosyn®) l Ticarcillin/Clavulanate (Timentin®) l

Beta-Lactamase Inhibitors Augmentin, Unasyn, Timentin, Zosyn Advantages Disadvantages l stabilization against l GI intolerance beta-lactamases (Augmentin) l excellent broad l Superinfections coverage, including l High cost anaerobes l frequent dosing l Zosyn > Timentin for l E. coli resistance Pseudomonas increasing with Unasyn l Enterococcus coverage (not Timentin)

Unasyn, Zosyn Indications Unasyn Zosyn l l l Intraabdominal prophylaxis + gentamicin for E. coli Mixed infection including Enterococcus 1. 5 -3 Gms q 6 h l Severe mixed infection – workhorse ICU drug l l Ventilator associated pneumonia +/- AG Severe diabetic foot infection suspected of involving mixed flora Narrow as soon as possible 3. 375 Gms q 6 h

Cephalosporins: General Similarities excellent penetration to tissues, including BBB (ceftriaxone, cefotaxime) l coverage based on “generation” l NO ENTEROCOCCUS ACTIVITY l wide therapeutic index l wide range of uses l *historically comprises one of the largest portions of antibiotic budget l

Cephalosporins: First Generations l most active against gram positives – cellulitis l good coverage against selected gram negatives (E. coli, Proteus, Klebsiella) – Good option for pyelonephritis excellent for surgical prophylaxis (cefazolin) l Cefazolin (Ancef®) 1 Gm q 8 h l Cephalexin (Keflex®) higher MIC’s to Staph l

Cephalosporins: Second Generations less gram positive coverage l additional gram negative coverage, respiratory pathogens (Hemophilus, Moraxella) cefuroxime (Zinacef®, Ceftin®) l anaerobes (anti-anaerobic agents - cefotetan, cefoxitin, cefmetazole) l – ~ 75% anaerobic coverage – intraabdominal, GYN prophylaxis

Cefotetan (Cefotan®) , Cefoxitin (Mefoxin®): Indications for Use Surgical Prophylaxis for intraabdominal infections (Cefotan 1 Gm q 12 h) l Intraabdominal infections from community (no Enterococcus coverage) l Diabetic foot infections (E. coli, anaerobes) l

Cephalosporins: Third+ Generations additional gram negative (nosocomial) coverage, some gram positive, anaerobic coverage l Pseudomonas coverage (ceftazidime, cefepime) l excellent BBB penetration (ceftriaxone, cefotaxime and others) l Good coverage against Strep and Staph (except ceftazidime) l

Third Generation Ceph’s: Indication for Use l Cefepime (Maxipime®), ceftazidime (Fortaz®) – Neutropenic Fever (cefepime 2 Gms q 12 h) – Pseudomonas infections l Cefotaxime (Claforan®), ceftriaxone (Rocephin®) – Meningitis (cefotaxime 2 Gms q 8 h) – CAP (cefotaxime 1 Gm q 8 -12 h) – Endocarditis with HACEK organisms or PCN intermediate Strep (cefotaxime 2 Gms q 8 h)

Oral Cephalosporins l 1 st Generation: cephalexin (Keflex®) – 500 mg TID-QID – UTI l 2 nd Generation: None Formulary – Ceftin®, Cefzil®, Lorabid® l 3 rd Generation: cefpodoxime (Vantin®) – Oral transition for CAP, STD’s – 100 - 200 mg BID

Carbapenems l Imipenem/Cilastatin (Primaxin®) – excellent broad spectrum coverage but increasing Pseudomonas resistance – reserve for resistant organisms, seriously ill patients or PCN allergy – potential for seizures - adjust for renal status – beta-lactamase inducer – 500 mg q 6 -8 h l Meropenem (Merrem®) – less seizure risk – fewer indications

Carbapenems: Ertapenem (Invanz®) Recently approved agent for community infections l Intraabdominal or complicated skin and skin structure infections l No Enterococcus or Pseudomonas coverage l 1 Gm IV q 24 h l Adjust for Cr. Cl <30 m. L/min (500 mg qd) l

Monobactam: Aztreonam (Azactam®) ONLY gram-negative coverage l moderate Pseudomonas activity l safe to use in PCN allergic patients l excellent safety profile l 1 -2 Gms q 8 h l Adjust for Cr. Cl <30 m. L/min l

Quinolones Another Class with Generations excellent tissue penetration l excellent bioavailabilty l convenient dosing l some resistance to Pseudomonas developing l potential for overuse due to many factors l avoid with sucralfate, separate from antacids l

Quinolones: “First Generations” Norfloxacin, Ciprofloxacin l primarily gram negative, including Pseudomonas l some atypical l poor gram positive, no anaerobic l Cipro - interactions with theophylline, warfarin, phenytoin l

Quinolones: “Second Generations” Levofloxacin, Lomefloxacin, Gatifloxacin, Moxifloxacin l additional gram positive and atypical coverage, including Strep pneumoniae l moderate gram negative l excellent bioavailability l Levofloxacin - warfarin interactions l Moxifloxacin - no Pseudomonas coverage, good anaerobic coverage (KP formulary) l

Levofloxacin (Levaquin®) Indications for Use l CAP, especially patients with comorbidities – Doxycycline for pts with no comorbidities Complicated UTI infections (resistant to first generation ceph’s, sulfa) l Gram negative infections in patient allergic to PCN (+/- AG or anaerobic coverage) l Not preferred for cellulitis (750 mg dose) l 500 mg IV/PO qd (adjust for Cr. Cl < 50) l Add metronidazole for anaerobes l

Aminoglycosides: Gentamicin, Tobramycin, Amikacin l excellent gram negative coverage – amikacin > tobramycin > gentamicin l synergistic activity – low levels for gram positive synergy (1 mg/kg) – therapeutic levels for gram negative synergy l (5 -7 mg/kg once daily) NO Anaerobes - requires 02 to get into cell l dosing strategies dependent on indication l toxicities well defined l

Glycopeptides: Vancomycin excellent gram positive l reserve for resistant organisms, PCN/Ceph allergic patients l VRE l GISA? ? l nephrotoxicity no longer a real concern l only monitor trough’s except for select situations l oral ONLY for Flagyl failures l

Macrolides: erythro-, clarithro-, azithromycin moderate gram positives (Strep developing resistance - now up to 35%) l good atypical l use for lower respiratory tract infections l erythro and clarithro interactions l – theophylline, warfarin (+ azithro) l azithromycin - STD coverage (1 Gm x 1) – CAP: 250 - 500 mg qd x 5 -7 days

Antianaerobic Agents l Metronidazole (Flagyl®) – excellent anaerobic, first line C. difficile – 500 mg q 12 h except C. diff and bowel preps l half-life = 8 hours – Excellent bioavailability – warfarin interaction, disulfiram reactions l Clindamycin (Cleocin®) – gram positive, anaerobic (600 mg IV q 8 h max) – Use with PCN for nec fasciitis (Gp A Strep) – ? Pseudomembranous colitic

Miscellaneous l SMX/TMP (Septra®, Bactrim®) – excellent tissue penetration, broad uses – gram positive and “easy” gram negative – warfarin interaction – Some GI intolerance in elderly

Antifungals: Fluconazole Not effective against non-albicans strains l Indications for use l – C. albicans from sterile body site – C. albicans from multiple non-sterile sites (urine, wound, sputum) – Prophylaxis for recurrent intraabdominal rupture or anastomotic leak Systemic infections: 800 mg load, 400 mg qd l UTI: 100 mg qd x 5 days l Excellent bioavailability l
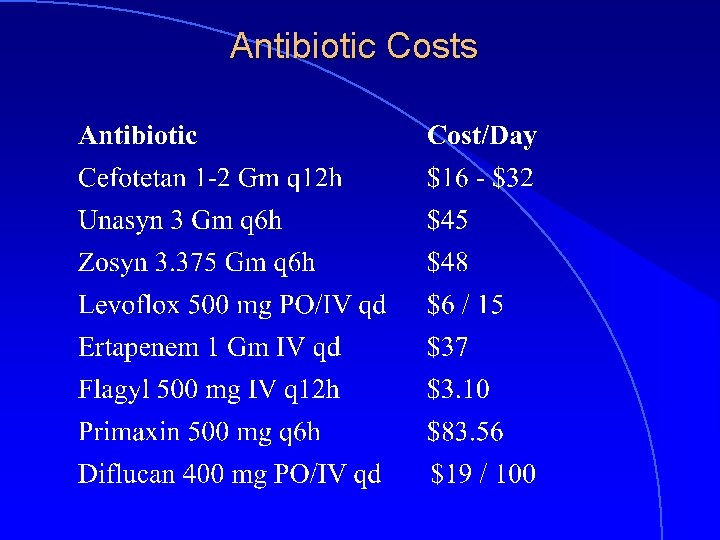

Antibiotic Costs

New Agents for VRE: l Quinupristin/Dalfopristin (Synercid®) – Streptogramin antibiotics – Effective against VREF (not E. faecalis), Staph aureus (MRSA and MSSA) – Dosing: 7. 5 mg/kg q 8 h – Infusion related ADR’s - central line preferred – Potential to elevate liver enzymes – Cyt P 450 3 A 4 interaction l Non-Formulary

New Agents for VRE Linezolid (Zyvox®) Oxazolidinone antibiotic l Effective against E. faecalis & E. faecium, MRSA, MSSA, Strep pneumo l IV, PO, Suspension - 100% absorption l 600 mg BID l Thrombocytopenia (> 2 weeks duration of therapy), GI intolerance l MAOI - weak inhibitor l Dopamine, epinephrine - adjust dose down l
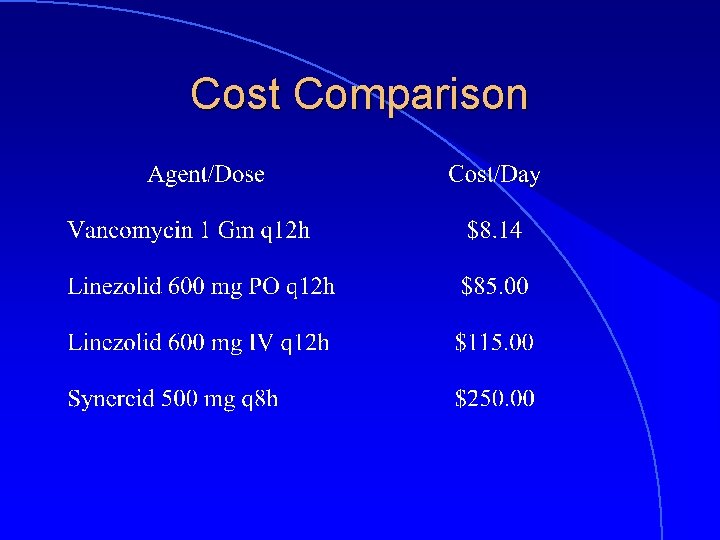
Cost Comparison

Linezolid (Zyvox®): Indications for Use l VREF – likely will be considered preferred therapy in place of Synercid® – need to carefully evaluate for potential colonization l MRSA Infections ONLY for Vanco intolerant patients – after trial of continuous infusion +/- Benadryl if possible l ID Consult

Resistance: A National Concern Often result of inappropriate or overuse of antibiotics l Significant financial impact on healthcare l Selecting out multi-drug resistance l Narrow coverage as soon as possible l ? Rotation of preferred classes of antibiotics l Don’t treat colonizations or contaminations l
- Slides: 40