Budget Impact Modeling Appropriateness and Determining Quality Input

Budget Impact Modeling: Appropriateness and Determining Quality Input C. Daniel Mullins, Ph. D Professor and Chair, PHSR Dept University of Maryland School of Pharmacy

4 Key Questions When is it appropriate to do a BIA? - and when is it not? What are criteria for a rigorous BIA? What data elements are input into a BIA? How can we ensure quality of BIA models?

Key Question #1 When is it appropriate to do a BIA? - and when is it not?

Appropriate & Inappropriate Ø Short term models Ø Lifetime models Ø Payer perspective Ø Patient/provider Ø Cost-effectiveness Ø Effectiveness

Key Question #2 What are criteria for a rigorous BIA?

Criteria for a Rigorous BIA Model Ø Academy of Managed Care Pharmacy (AMCP) Format: Key Elements of a Good Model ~ Structure ~ Data ~ Outputs

AMCP Checklist for Good Models: Structure ~ Transparent ~ Disease progression model ~ Relevant timeframe ~ Appropriate treatment pathways ~ Good math

AMCP Checklist for Good Models: Data Ø Data quality is critical ~ Clinical ~ Epidemiologic ~ Cost ~ Quality of Life

AMCP Checklist for Good Models: Outputs Ø Face validity ~ Do the results make intuitive sense? Ø Scientific validity ~ Published in a quality peer-reviewed journal?

Key Question #3 What data elements are input into a BIA?

Learn by doing: A Case Study Ø A hypothetical case study for a not so hypothetical new drug

Overview of the presentation of a model - Presentation of the model - A walk through the model - Model assumptions - Model Limitations - Take home messages
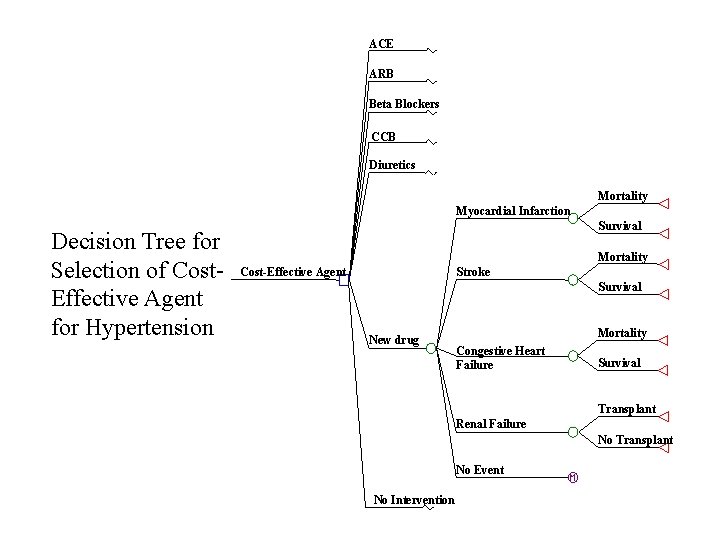
ACE ARB Beta Blockers CCB Diuretics Mortality Myocardial Infarction Decision Tree for Selection of Cost. Effective Agent for Hypertension Survival Mortality Cost-Effective Agent Stroke Survival New drug Mortality Congestive Heart Failure Survival Transplant Renal Failure No Transplant No Event No Intervention
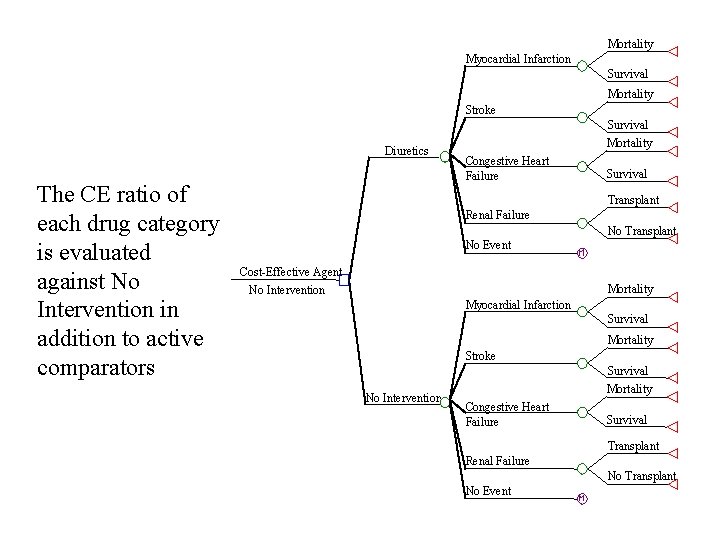
Mortality Myocardial Infarction Survival Mortality Stroke Survival Diuretics The CE ratio of each drug category is evaluated against No Intervention in addition to active comparators Mortality Congestive Heart Failure Survival Transplant Renal Failure No Transplant No Event Cost-Effective Agent No Intervention Mortality Myocardial Infarction Survival Mortality Stroke Survival No Intervention Mortality Congestive Heart Failure Survival Transplant Renal Failure No Transplant No Event

Overview of the presentation of a model - Presentation of the model - A walk through the model - Model assumptions - Model Limitations - Take home messages

Inputs are entered into the model, these are processed and out comes the costeffectiveness results Inputs Results

The model inputs - Initially 100, 000 patients enter the model - Characteristics of population evaluated in the model - Event probabilities for each of the possible population groups evaluated in the model - Persistency rate for each of the drug treatment categories - Anti-hypertensive drug treatment costs and office visit costs - Initial event treatment costs - Annual average treatment costs after event (the model runs for 5 years)
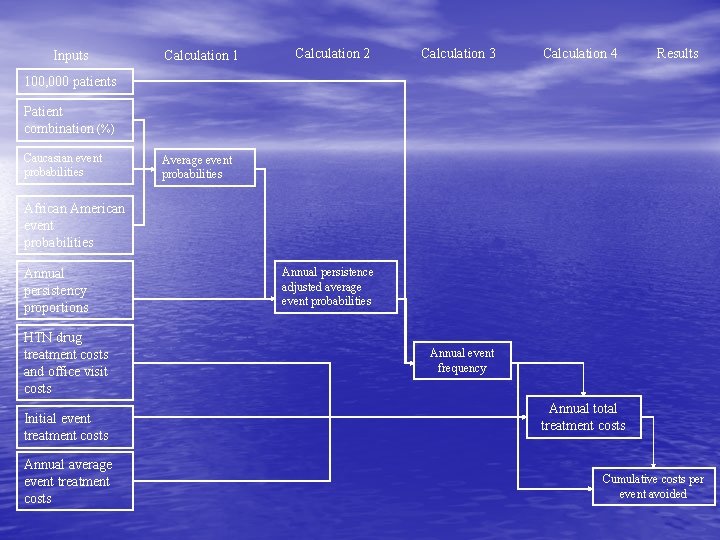
Inputs Calculation 1 Calculation 2 Calculation 3 Calculation 4 Results 100, 000 patients Patient combination (%) Caucasian event probabilities Average event probabilities African American event probabilities Annual persistency proportions HTN drug treatment costs and office visit costs Initial event treatment costs Annual average event treatment costs Annual persistence adjusted average event probabilities Annual event frequency Annual total treatment costs Cumulative costs per event avoided
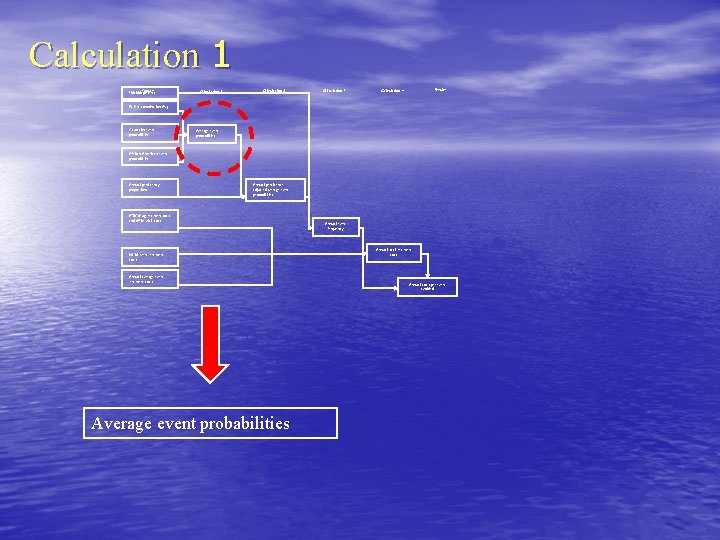
Calculation 1 100, 000 Inputs patients Calculation 1 Calculation 2 Calculation 3 Results Calculation 4 Patient combination (%) Caucasian event probabilities Average event probabilities African American event probabilities Annual persistency proportions Annual persistence adjusted average event probabilities HTN drug treatment costs and office visit costs Initial event treatment costs Annual average event treatment costs Average event probabilities Annual event frequency Annual total treatment costs Annual costs per event avoided

Average event probabilities calculation example Calculation done for each drug (D) category and the No Intervention (NI) category Input 70% Caucasian (C) and 30%African American (AA): Calculation done for each event i NI Average Event i Probability PNI, A, Event i=. 7 * PNI, C, Event i +. 3 * PNI, AA, Event i Drug Average Event i Probability PD, A, Event i =. 7 * PD, C, Event i +. 3 * PD, AA, Event i
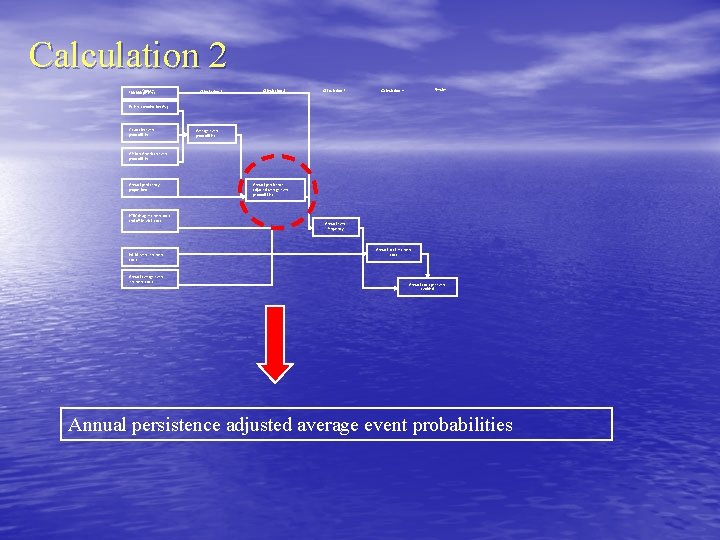
Calculation 2 100, 000 Inputs patients Calculation 1 Calculation 2 Calculation 3 Results Calculation 4 Patient combination (%) Caucasian event probabilities Average event probabilities African American event probabilities Annual persistency proportions HTN drug treatment costs and office visit costs Initial event treatment costs Annual average event treatment costs Annual persistence adjusted average event probabilities Annual event frequency Annual total treatment costs Annual costs per event avoided Annual persistence adjusted average event probabilities

Persistence adjusted average event probabilities calculation example Calculation done for each year, since persistence can change from year to year Input for year 2: 80% fully persistent, 20% not persistent Persistence adjusted average event probabilities for year 2 (y 2): PP, Event i, y 1 =. 8 * PD, A, Event i +. 2 * PNI, A, Event i
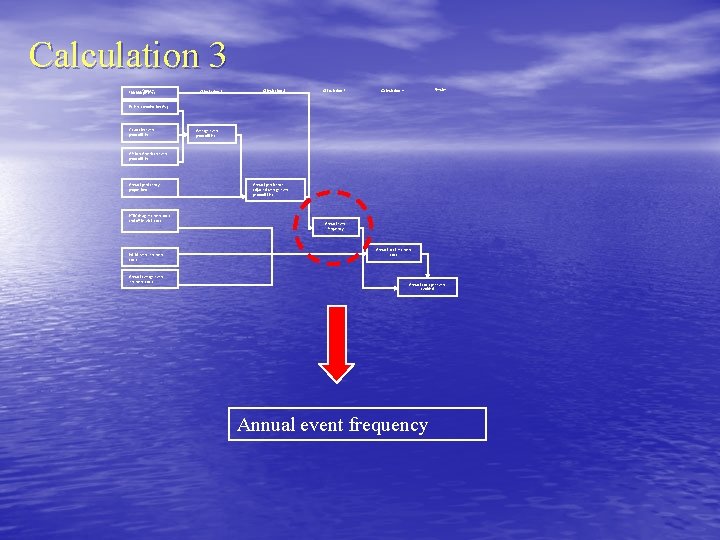
Calculation 3 100, 000 Inputs patients Calculation 1 Calculation 2 Calculation 3 Results Calculation 4 Patient combination (%) Caucasian event probabilities Average event probabilities African American event probabilities Annual persistency proportions HTN drug treatment costs and office visit costs Initial event treatment costs Annual average event treatment costs Annual persistence adjusted average event probabilities Annual event frequency Annual total treatment costs Annual costs per event avoided Annual event frequency

Event frequency (EF) Calculation done for each year, since persistence change and so does the cohort size Event frequency for year 1, Event i EFy 1, Event i = 100, 000 * PP, Event i, y 1 Number of Event i deaths year 1 # Event i deaths in year 1 # Dy 1, Event i = EFy 1, Event i * Event i Mortality rate Number of Event i survivors in year 1 # Sy 1, Event i = EFy 1, Event i - # Dy 1, Event i Size of year 2 cohort Y 2 C = 100, 000 - EFy 1, total events
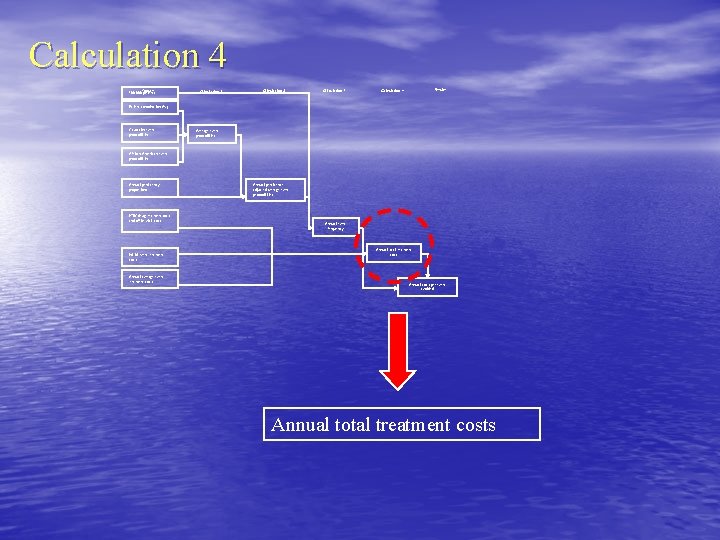
Calculation 4 100, 000 Inputs patients Calculation 1 Calculation 2 Calculation 3 Results Calculation 4 Patient combination (%) Caucasian event probabilities Average event probabilities African American event probabilities Annual persistency proportions HTN drug treatment costs and office visit costs Initial event treatment costs Annual average event treatment costs Annual persistence adjusted average event probabilities Annual event frequency Annual total treatment costs Annual costs per event avoided Annual total treatment costs

Annual total treatment costs Calculation done for each year, since event frequency change over time due to the decreasing cohort size Year 1 total treatment costs TCy 1, event i =[EFy 1, event i * Event i initial costs] + [100, 000 * yearly Drug/Office visit costs] Year 2 total treatment costs TCy 2, event i =[EFy 2, event i * Event i initial costs] + [Y 2 C * yearly Drug/Office visit costs] + [# Sy 1, Event i * Year 1 Event i average event treatment costs]
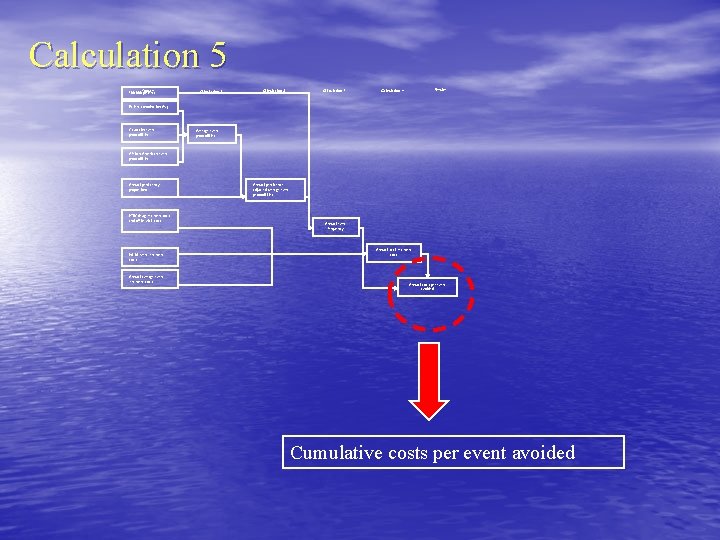
Calculation 5 100, 000 Inputs patients Calculation 1 Calculation 2 Calculation 3 Results Calculation 4 Patient combination (%) Caucasian event probabilities Average event probabilities African American event probabilities Annual persistency proportions HTN drug treatment costs and office visit costs Initial event treatment costs Annual average event treatment costs Annual persistence adjusted average event probabilities Annual event frequency Annual total treatment costs Annual costs per event avoided Cumulative costs per event avoided

Cumulative costs per event avoided Calculation done for each drug treatment category evaluated Cumulative costs per event avoided for a drug treatment category CPEA = [ TCy 1, all events, NI - TCy 1, all events, drug treatment] [#EFy 1, all events, NI - #EFy 1, all events, drug treatment] - The lower the “costs per event avoided” the better

Overview of the presentation of a model - Presentation of the model - A walk through the model - Model assumptions - Model Limitations - Take home messages

Model assumptions - The baseline event probabilities represents an average American hypertensive population (age, gender, co-morbidities) - Same annual event probability applied each model year - Same event survival probability applied to each treatment category - Immediate effect of drug treatment persistency status - Once patients become non persistent with drug treatment, they stay so - Same annual office visit costs across treatment categories - Linear event treatment costs interpolated from missing data

Overview of the presentation of a model - Presentation of the model - A walk through the model - Model assumptions - Model Limitations - Take home messages

Limitations - Future events modeled by down stream event treatment costs - Patients with multiple factors are not considered in the model (LVH/diab. ) - Average event treatment costs may not be constant in years after the event - Partial drug treatment persistency is not considered - Drug treatment switch is not considered

Overview of the presentation of a model - Presentation of the model - A walk through the model - Model assumptions - Model Limitations - Take home messages

Take Home Messages - Drug A reduces DBP by x mm HG and SPB by y mm Hg - Drug A provides a favorable safety profile - Drug A improves patient functioning based on physical domain of ABC - Drug A reduces down stream event treatment costs

Lessons learned and tricks of the trade # 1 Be transparent # 2 Describe limitations (see #1) # 3 Describe the model in a simple form (see #1) # 4 Get to the point # 5 Stick to the point

Key Question #4 How can we ensure quality of BIA models?

Testing the quality Ø Test for face validity ~ Do the results make intuitive sense? ~ Do the results seem believable? Ø Try to “break the model” ~ Put in “outlier” values ~ Does the model “explode”? ~ Does the model always give the same result?

Ensuring the quality Ø Consider local practice patterns ~ ~ ~ Local prevalence Compare to “standard of care” Use inputs that reflect local § Costs § Hospital length of stay § Physician practices Ø Allow for Plan-specific values ~ Do the results reflect Plan demographics? ~ Do the results reflect Plan costs?

Provide transparent inputs and results so that decision-maker can Ø Perform their own assessment Ø Feel comfortable with assumptions Ø Feel comfortable with inputs Ø Feel comfortable with calculations Ø Feel comfortable with what’s in the “black box”

Summary Ø BIA should be performed over short to midrange time periods – not lifetime Ø AMCP guidance focuses on: ~ Structure ~ Data ~ Outputs Ø Present an overview of your model ~ A picture is worth a thousand words ~ Walk the decision-maker through the analysis

Conclusion Ø BIA should reflect the appropriate perspective and what they care about Ø BIA calculations should be transparent and provide insight into change in costs: ~ Drug Costs ~ Total Medical Costs Ø Make the user interface user friendly Ø Allow the decision-maker to see or understand what’s in the “black box”

- Slides: 42