Bronchopleural Fistula Definition n A bronchopleural fistula BPF

Bronchopleural Fistula

Definition n A bronchopleural fistula (BPF) is a communication between the pleural space and the bronchial tree.

Aetiology n n n n Bulla lung abscess/necrotizing pneumonia Neoplasms peripheral bronchiectasis trauma Postoperative e. g. pneumonectomy Ventilator induced lung injury
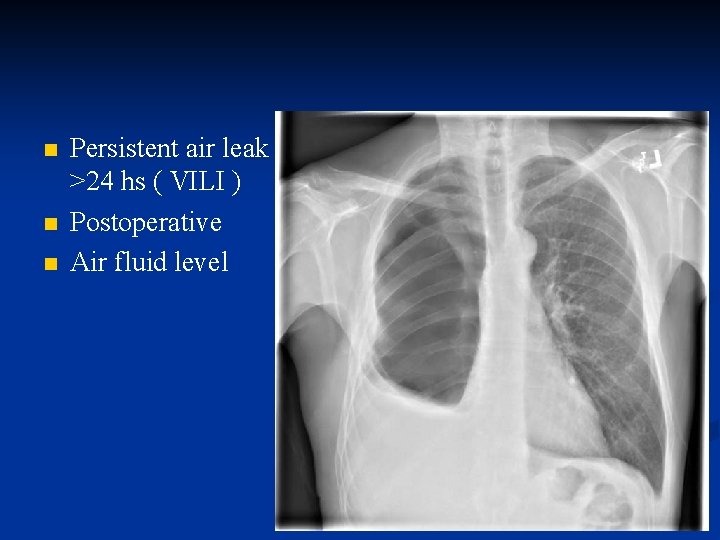
n n n Persistent air leak >24 hs ( VILI ) Postoperative Air fluid level

precise measurement of the leak is not necessary n For clinical purposes, there are three levels of severity of leakage from a BPF: • Bubbling only during inspiration. • Bubbling that continues during both inspiration and expiration • A leak of sufficient magnitude (ie, greater than 100 to 150 m. L per breath) so that differences in inspired and expired tidal volumes can be detected at the ventilator, using an appropriate correction for compressible volume. n

Adverse effects of a BPF n n n incomplete lung expansion; atelectasis, V/Q mismatch ( large leak, restictive lung dis) effective TV; ( compensation exacerbate the problem) respiratory acidosis ( usually due to severity of underlying lung disease) loss of PEEP pleural disease infection factitious ventilator cycling

Managment n n n Conservative Endoscopic surgical

Conservative n n Drainage of the pleural space treatment of infections optimizing nutrition Ventilator management

Ventilator management n n A BPF may be more likely to develop and persist in the presence of a large pressure gradient between the airways and the pleural space (or the airways and the chest tube, once a pneumothorax develops). ventilator management should include decreasing airway pressures as much as clinically feasible and reducing chest tube suction to the lowest level that maintains complete lung inflation.

n n Measures directed at reducing the leak itself (as opposed to therapy for the underlying disorder) seldom make much difference in the patient's clinical course. Even when leaked volume can be reduced, there tends to be little if any effect on gas exchange, as measured by arterial blood gases. In ARDS, the CO 2 content of the leaked gas is usually similar to that of gas exhaled via the endotracheal tube, indicating that this gas participates in gas exchange and is not "lost" or "wasted" volume

n n n Wean early Partial ventilatory support Avoid hypocapnia Consider permissive hypercapnia Reduce insp time ( MAP) I: E = 1: 3; PFR = 70 -100, no pause Effective TV = 5 -8 ml Minimal PEEP Least ICT suckion If movement increase leak, sedation Possition difference Treate bronchospasm Treate the cause of respiratory failure

independent lung ventilation n high-frequency ventilation n inspiratory chest tube occlusion n application of PEEP to the chest tube n


bronchoscopic techniques utilizing the fiberoptic bronchoscope include first identifying the affected bronchus and then occluding it with one of the following: n A balloon (using a Fogarty or Swan-Ganz catheter). n A plug composed of Gelfoam, fibrin, or tissue glue. n Local application of silver nitrate n Local injection of polidocanol sclerosants n Coagulation of the leaking site with the Nd: YAG laser.

n n n n Methylmethacrylate injection of absolute ethanol endobronchial silicone plugs, gluteraldehyde tissue adhesive lead plugs endobronchial valve Success with any of these methods is likely to be dependent on the patient receiving treatment as well as the skill of the bronchoscopist.

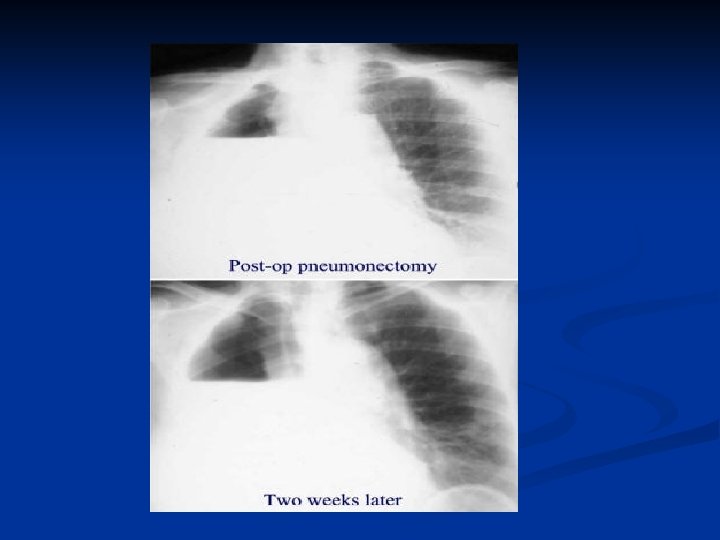
postpneumonectomy n n Necrosis of bronchial stump Dehiscence of suture line Clinical n n Sudden onset of dyspnea Expectoration of bloody fluid Imaging findings n Return to midline of a previously shifted mediastinum n A drop in the fluid level by more than 2 cm is abnormal


- Slides: 19