Bronchiectasis Khaled AlAsad M D JUH 2018 2019

Bronchiectasis Khaled Al-Asad, M. D JUH 2018 / 2019

Definition • Bronchiectasis • is a permanent dilatation and thickening of the airways characterized by chronic cough, excessive sputum production, bacterial colonization, and recurrent acute infections • a guide for primary care. Aust Fam Physician. 2012 Nov; 41(11): 842 -50.

Definition • COPD • Asthma • common, preventable • Heterogeneous disease and treatable disease that characterized by chronic is characterized by airway inflammation. it is persistent respiratory defined by history of symptoms and airflow respiratory symptoms, limitation that is due to wheezes, cough, and airway and/or alveolar shortness of breath and abnormalities, usually chest tightness that vary caused by significant over time in intensity exposure to noxious together with variable particles or gases expiratory airflow limitation

Obstructive lung Physiology • • • COMMON COPD Asthma Bronchiectasis Cystic fibrosis • • • Uncommon / combined Sarcoidosis LAM Early Scoliosis Bronchiolitis Obliterans Alpha Antitrypsin

Pathology • Dilatation : reflection of inflammatory mediators with oxidative stress, and damage of peribronchial tissue • Bronchial hypersecretion from mucus gland hypersecretions of mucus glands • Bacterial colonization ciliary dysfunction and impaired local immune response • It is – Permanent – Chronic – Persistent symptoms

Expected physiology • Obstructive – Mucus plugs – Airway disease • High airway resistance – Obstruction – Collapsibility airways – Surface area involved • Air trapping • Restrictive – Peribronchial fibrosis – Recurrent infections of parenchyma • Muscles and diaphragm dysfunction due to malnourishment

Pathogenesis • affected airways are inflamed and easily collapse. • There is an impairment of airflow and drainage of secretions, leading to the accumulation of a large amount of mucus in the lungs. • mucus collects bacteria, predisposing to frequent and often severe LRT infections. • severity of bronchiectasis used to be classified according to the volume of sputum produced but this has now largely been superseded by using the radiological appearance on CT scan

Aetiology & Mechanism • The disease is caused by chronic inflammation of the airways. • Therefore – be caused by a large number of disorders which cause inflammation and infection – particularly conditions that facilitate infections • tend to be recurrent and more severe with time and cause damage to the lungs

Epidemiology • study across 640 general practices in the UK – Prevalence in 2011 in men was 227/100, 000, and 309/100, 000 in women. – Incidence increased each year between 2004 and 2011, from 18/100, 000 person-years at risk, to 32/100, 000 person-years at risk. – Prevalence was higher in women than in men. – Prevalence was higher in the older age groups (>60 years). – Time trends in incidence and prevalence of bronchiectasis in the UK. Thorax. 2012; 67
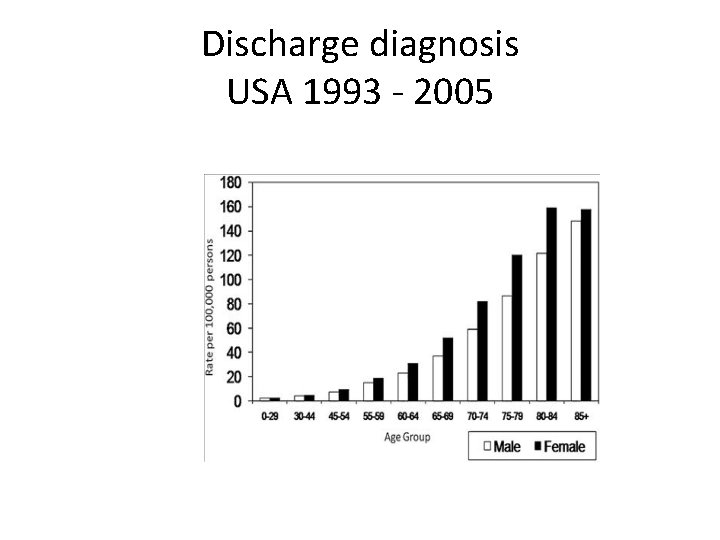
Discharge diagnosis USA 1993 - 2005

Classification • Bronchiectasis can be classified into the following forms morphologically (all three forms may be present in the same patient): • Cylindrical bronchiectasis: – bronchi are enlarged and cylindrical. • Varicose bronchiectasis: – bronchi are irregular with areas of dilatation and constriction. • Saccular or cystic: – dilated bronchi form clusters of cysts. This is the most severe form of bronchiectasis and is often found in patients with cystic fibrosis

Clinical presentation • Episodes of expectoration • Daily postural drainage • Putrid sputum • Cough • Dyspnea • Wheezes • Chest pain hemoptysis • • Localized vs. diffuse Crackles Wheezes Repeated pneumonia Sinusitis Situs inversus Clubbing ? Systemic disease
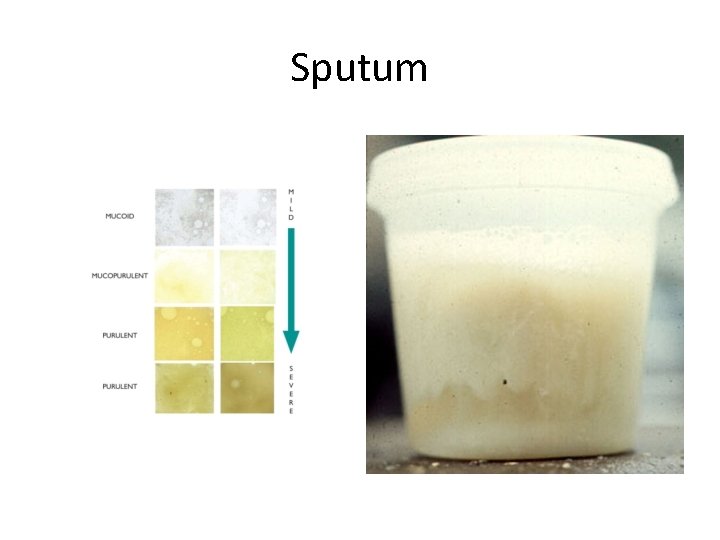
Sputum
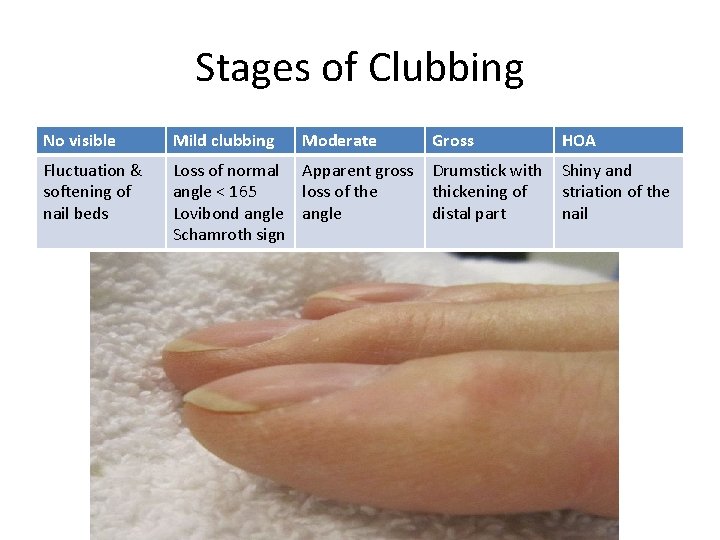
Stages of Clubbing No visible Mild clubbing Moderate Gross HOA Fluctuation & softening of nail beds Loss of normal Apparent gross Drumstick with Shiny and angle < 165 loss of the thickening of striation of the Lovibond angle distal part nail Schamroth sign

Causes of clubbing • Lung diseases – lung CA, interstitial dis, TB, mesothelioma, lung abscess, bronchiectasis • Heart diseases – chronic hypoxia, cyanotic heart disease, SBE, A. myxoma, Tetralogy • GI diseases – malabsorption, crohn’s & UC, rimary biliary c. hepatopulmonary syndrome • Thyroid ; Grave’s – Platelet Derived Growth factor – Upregulation of PGE 2

CAUSE • • • Post infectious Immune defeciency Collagen vascular dis. Gastric aspiration ABPA, IBD Congenital • Bronchial obstruction • • • Measles, TB, pertusis HIV RA, SLE 3 -8% 4% 1 -7% Cystic F 4%, Kartagener yellow nail syndrome

FACT • 42% of cases develop post-infection. However, there is no identifiable underlying cause in about 50% of adults and 25% of children – Characterisation of the onset and presenting clinical features of adult bronchiectasis. Respir Med. 2006 Dec; 100(12): 2183 -9
FACT – COPD 57. 6% • elevated prevalence of bronchiectasis in patients with moderate to severe COPD • associated with severe airflow obstruction • at least one hospital admission for exacerbations in the previous year • Miguel Ángel Martínez-García – Nov 2011
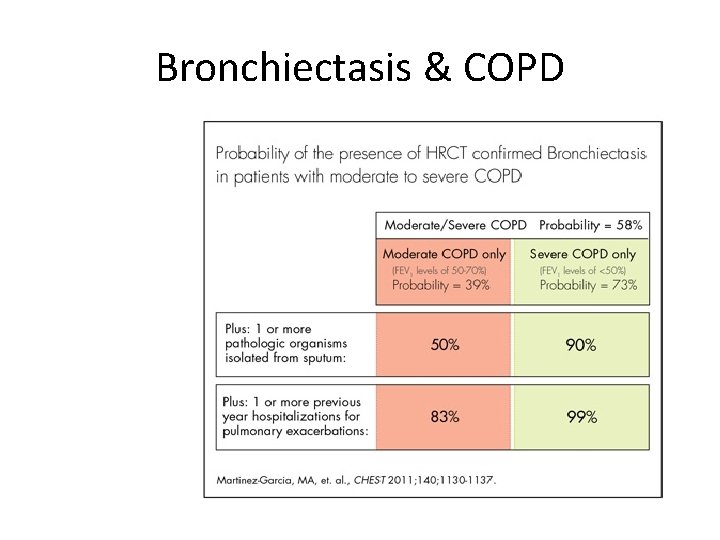
Bronchiectasis & COPD

Review Natural history 842 patients Follow up 12 years Mean admission per year 2. 2 • Mortality 28% • Asthma 20 % • COPD 38 % • • • Registry Finland Kiestinen et al • • • Mortality study Advanced age CT involevement Functional status Respiratory Failure both types • Onen et al

FACT - pediatrics • A child with chronic respiratory symptoms and a single positive sputum culture for Staphylococcus aureus, Haemophilus influenzae, Pseudomonas aeruginosa, nontuberculous mycobacteria or Burkholderia cepacia complex • ==== BRONCHIECTASIS

FACT - adults • Assessment of symptoms in patients with bronchiectasis should include a record of both sputum purulence and estimated or measured 24 -hour sputum volume when clinically stable • Pseudomonas growth
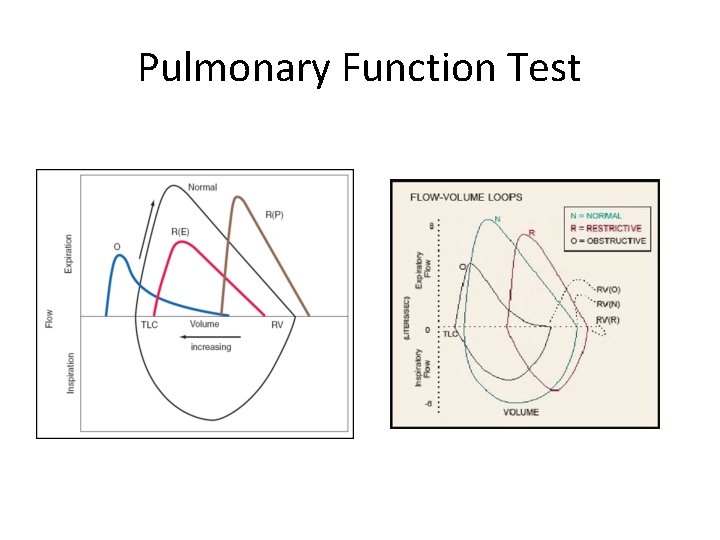
Pulmonary Function Test

BRONCHIECTASIS DIAGNOSIS

Diagnosis • Clinical suspicion : chronic symptoms, cough, sputum variable in amount and consistency and content, wheezes and shortness of breath • Physical exam : wheezes, squeaking sounds, variable air entry and added sounds. Clubbing • Chest radiograph : 20 – 40 % patients with mild bronchiectasis may have normal or non specific findings

Chest radiograph • Ring opacities or cystic spaces as large as 2 cm in diameter resulting from cystic bronchiectasis, sometimes with air-fluid levels – Cysts related to cystic bronchiectasis, sometimes with fluid levels (demilunes) • Tubular opacities – caused by dilated, fluid-filled bronchi - These may occur as Y or V shapes or as "finger-in-glove" opacities, which radiate from the pulmonary hilum • Increased size and loss of definition of the pulmonary vessels in the affected areas as a result of peribronchial fibrosis • Crowding of pulmonary vascular markings from the associated loss of volume, usually caused by mucous obstruction of the peripheral bronchi • Oligemia as a result of reduction in pulmonary artery perfusion (severe disease) • Signs of compensatory hyperinflation of the unaffected lung
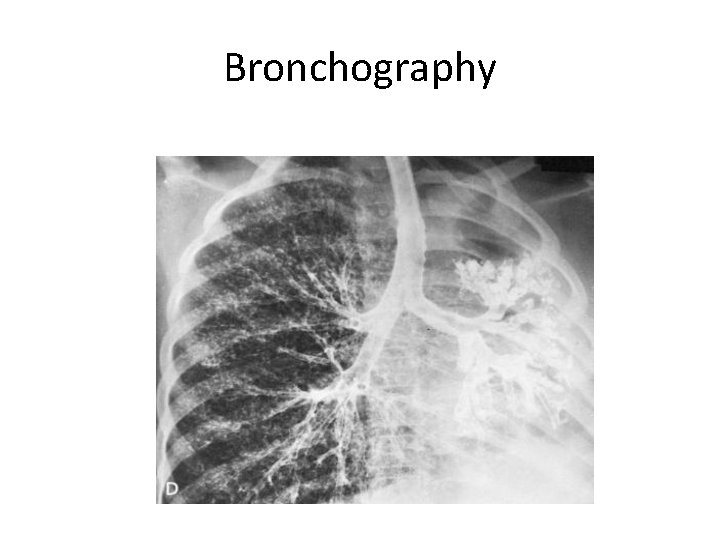
Bronchography
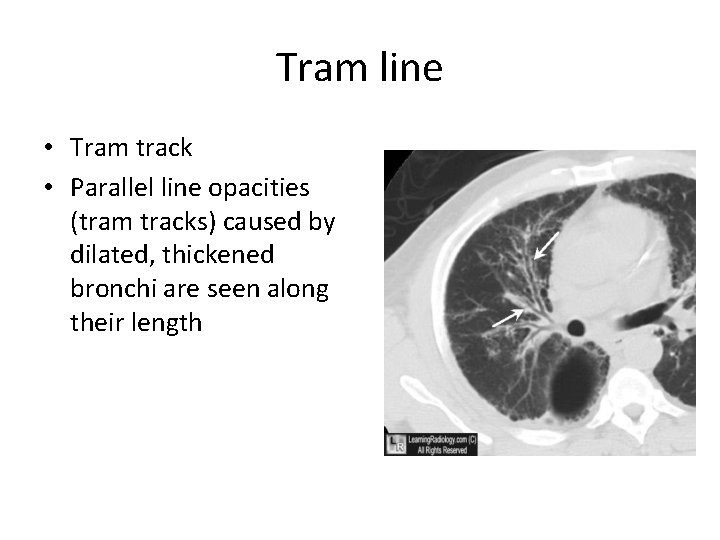
Tram line • Tram track • Parallel line opacities (tram tracks) caused by dilated, thickened bronchi are seen along their length
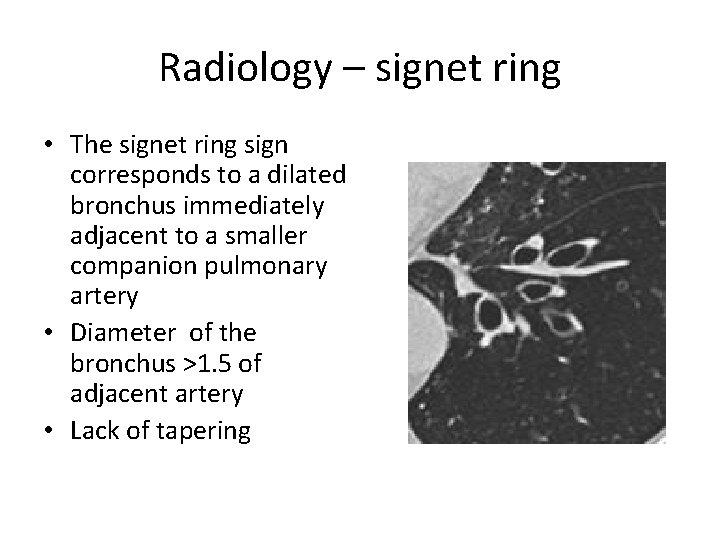
Radiology – signet ring • The signet ring sign corresponds to a dilated bronchus immediately adjacent to a smaller companion pulmonary artery • Diameter of the bronchus >1. 5 of adjacent artery • Lack of tapering

HRCT findings • internal bronchial diameter may be greater than that of the adjacent artery, and there may be a lack of bronchial tapering (the same diameter as the parent branch for >2 cm). • bronchial wall thickening may be seen (in 68% of patients). • A cystic cluster of thin-walled cystic spaces may be present, often with air-fluid levels

When to suspect CF • Cystic fibrosis: – All children and all adults up to the age of 40, presenting with bronchiectasis, should have investigations for cystic fibrosis. – Screening investigations should include both two measurements of sweat chloride, and cystic fibrosis transmembrane regulator (CFTR) genetic mutation analysis – In adults, investigations should also be considered in those with: • • • Age at presentation >40 years and no other identified cause. Persistent isolation of S. aureus in the sputum. Features of malabsorption. Male primary infertility. Upper lobe bronchiectasis. A history of childhood steatorrhoea

Yellow nail syndrome • • • Rare disease Lymphedema Pleural effusion Yellow nails Bronchiectasis in 40% Chronic sinusitis

bronchiectasis GUIDELINE IN MANAGEMENT

Mortality M. R. Loebinger et al • 91 patients were examined for – Aetiology – Pulmonary function tests – High-resolution computed tomography – Sputum microbiology • Quality of life scores • Follow up over 13 yrs. • Overall, 29. 7% of the patients died.

Mortality M. R. Loebinger et al • On multivariate analysis – – Age St George’s Respiratory Questionnaire activity score, Pseudomonas aeruginosa infection Total lung capacity (TLC), residual volume/TLC and the transfer factor coefficient were • all independently associated with mortality. • In patients with moderate to severe bronchiectasis, mortality is associated with a degree of restrictive and obstructive disease, poor gas transfer and chronic pseudomonas infection

End Stage Bronchiectasis • Postbronchodilator FEV 1 <30% (especially young females with cystic fibrosis) • Exacerbation of pulmonary disease requiring intensive care unit admission Increasing frequency of exacerbations requiring intravenous antibiotics • Refractory and/or recurrent pneumothorax • Recurrent hemoptysis not controlled by embolization • Other factors to consider: Hypercarbia (Pa. CO 2 >45 mm. Hg) Rapidly progressive decline in lung function Resting hypoxemia (Pa. O 2 <55 mm. Hg

Worse complications • • Repeated infections Repeated exacerbations Lung abscess Major hemoptysis

Guideline in the management • • Stop smoking Influenza and pneumococcal vaccine Postural drainage Sputum culture – Stapylococcus – Pseudomonas – Tuberculosis : typical vs. atypical

Antibiotics • If there is no previous bacteriology, first-line treatment is amoxicillin 500 mg three times a day or clarithromycin 500 mg twice daily (in patients who are penicillin-allergic) for 14 days. • High-dose oral regimens (eg, amoxicillin 1 g three times a day or amoxicillin 3 g twice daily) may be needed in patients with severe bronchiectasis chronically colonised with H. influenzae. • Ciprofloxacin should be used in patients colonised with P. aeruginosa

Antibiotics • Long-term oral antibiotics: – Patients having three or more exacerbations per year requiring antibiotic therapy or patients with fewer exacerbations that are causing significant morbidity should be considered for long-term antibiotics. Again, choice will be dictated by sensitivities and local microbiology advice from sputum test results. – Azithromycin is emerging as a useful option for preventing exacerbations in adults and children

New trend • Nebulizer therapy – Tobramycin – Aztreonam – RDNAse • • • Immune globulin therapy Intravenous antitrypsin Intra bronchial surfactant Bronchial artery embolization and coiling VATS segment resection Thymosin alpha 1

SURGERY • Evaluate if bronchiectasis is focal, bilateral and diffuse • Must evaluate pulmonary reserve: – PFT – V/Q – Split lung function • Identify syndromes • Evaluate cardiac function

Indication for surgery • • • Failure of medical/conservative therapy Recurrent respiratory infections Persistent sputum production Hemoptysis Chronic cough Persistent lung abscess
- Slides: 43