Bronchial Asthma Emad KORRAA MD Chest Department Ain

Bronchial Asthma Emad KORRAA, MD Chest Department Ain Shams University

Definition of Asthma u Old View Asthma is a disease of the airways characterized by bronchospasm. u New View Asthma, whatever the severity, is a chronic inflammatory disorder of the airways.

Definition of Asthma u A chronic inflammatory disorder of the airways. u Many cells and cellular elements play a role. u Chronic inflammation leads to an increase in airway hyperresponsiveness with recurrent episodes of wheezing, coughing, and shortness of breath. u Widespread, variable, and often reversible airflow limitation.

Definition of Asthma u Asthma is a chronic inflammatory disorder of the airways in which many cells and cellular elements play a role. u Chronic inflammation causes an associated increase in airway hyperresponsiveness that leads to recurrent episodes of wheezing, breathlessness, chest tightness and coughing, particularly at night or in the early morning. u These episodes are usually associated with widespread but variable airflow obstruction that is often reversible with or without treatment.
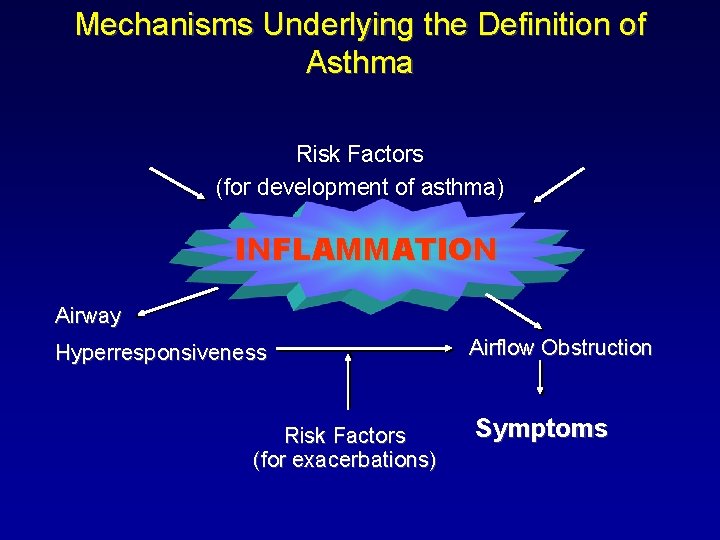
Mechanisms Underlying the Definition of Asthma Risk Factors (for development of asthma) INFLAMMATION Airway Hyperresponsiveness Risk Factors (for exacerbations) Airflow Obstruction Symptoms
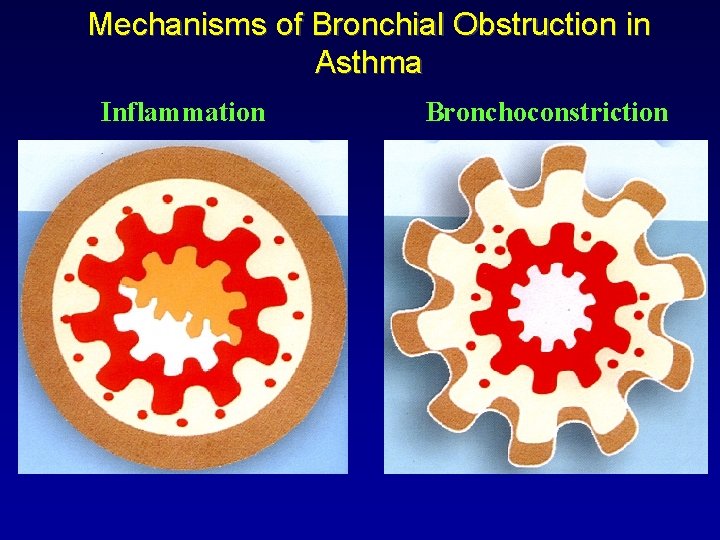
Mechanisms of Bronchial Obstruction in Asthma Inflammation Bronchoconstriction

Risk Factors for Asthma u Host factors: predispose individuals to, or protect them from, developing asthma. u Environmental factors: development of asthma influence susceptibility to in predisposed individuals, precipitate asthma exacerbations, and/or cause symptoms to persist.

Risk Factors that Lead to Asthma Development Host Factors Genetic predisposition Atopy Airway hyper-responsiveness Gender Race/Ethnicity Environmental Factors Indoor allergens Outdoor allergens Occupational sensitizers Tobacco smoke Air Pollution Respiratory Infections Parasitic infections Socioeconomic factors Family size Diet and drugs Obesity

Factors that Exacerbate Asthma u Allergens u Air Pollutants u Respiratory infections u Exercise and hyperventilation u Weather changes u Sulfur dioxide u Food, additives, drugs

Asthma Diagnosis u History and patterns of symptoms. u Physical examination. u Measurements of lung function (Peak flow meter reading (reversibility of 15%), spirometry). u Measurements of allergic status to identify risk factors.

Is it Asthma? u Recurrent episodes of wheezing. u Troublesome cough at night. u Cough or wheeze after exercise. u Cough, wheeze or chest tightness after exposure to airborne allergens or pollutants. u Colds “go to the chest” or take more than 10 days to clear.

Goals of Long-term Management u Achieve and maintain control of symptoms. u Prevent asthma episodes or attacks. u Maintain pulmonary function as close to normal levels as possible. u Maintain normal activity levels, including exercise. u Avoid adverse effects from asthma medications. u Prevent development of irreversible airflow limitation. u Prevent asthma mortality.

Goals of Long-term Management u Minimal (ideally no) chronic symptoms. u Minimal (infrequent) exacerbations. u No emergency visits. u Minimal (ideally no) need for “as needed” use of β 2 -agonist. u No limitations on activities, including exercise. u PEF circadian variation of less than 20 percent. u (Near) normal PEF. u Minimal (or no) adverse effects from medicine.

u The most effective management is to prevent airway inflammation by eliminating the causal factors. u Asthma can be effectively controlled in most patients, although it can not be cured. u The major factors contributing to asthma morbidity and mortality treatment. are under-diagnosis and inappropriate

The Treatment Gap in Asthma u u Patients are not detected l do not seek medical attention. l no access to health service. l missed diagnosis (bronchitis, LRTI). Patients do not get treated l they do not want treatment (do not accept diagnosis). l they stop treatment (when they feel well). l health service does not provide treatment.

Factors Associated with Non-Compliance in Asthma Care Medication Usage Patient/Physician Misunderstanding / lack of Difficulties with inhalers Complicated regimens Fears about, or actual side Underestimation of severity effects Cultural factors Cost Poor communication information

Treatment of Bronchial Asthma u Reduce exposure to indoor allergens. u Avoid tobacco smoke. u Avoid vehicle emission. u Identify irritants in the workplace. u Explore role of infections on asthma development, especially in children and young infants. u Pharmacological therapy.

Pharmacologic Therapy Controller Medications: l Inhaled glucocorticosteroids. l Systemic glucocorticosteroids. l Cromones. l Methylxanthines. l Long-acting inhaled β 2 -agonists. l Long-acting oral β 2 -agonists. l Leukotriene modifiers.

Pharmacologic Therapy Reliever Medications: l Rapid-acting inhaled β 2 -agonists l Systemic glucocorticosteroids l Anticholinergics l Methylxanthines l Short-acting oral β 2 -agonists

Classification of Asthma Medication Quick Relief u Short-acting l l b 2 -agonists Preventive u Salbutamol Terbutaline Ipratropium Bromide u Short-acting l theophylline l Fluticasone u Sodium Cromoglycate u Long-acting b 2 -agonists Aminophylline u Adrenaline l Beclomethasone Budesonide l u Anticholinergics l Corticosteroids injections u l Sustained-release salbutamol l Salmeterol l Formoterol Long-acting theophylline

u At present, inhaled glucocorticosteroids are the most effective controller medications and are recommended for persistent asthma at any step of severity. u Long-term treatment with inhaled glucocorticosteroids markedly reduces the frequency and severity of exacerbations.

Inhaler Devices for Young Children u 1 -2 Years: MDI + Spacer + Mask or Nebulizer u 3 -5 Years: MDI + Spacer + Mask or Nebulizer u 5 -8 Years: Rotahaler or MDI + Spacer u >8 Years: Rotahaler or MDI + Spacer Nebuliser only in occasional cases

Oral Therapy vs Inhaled Therapy High dose required (mg) Much lower dose required (mcg) GI tract Oral cavity Systemic circulation Targeted therapy to the airway Airways Higher incidence of adverse effect Lower incidence of adverse effects
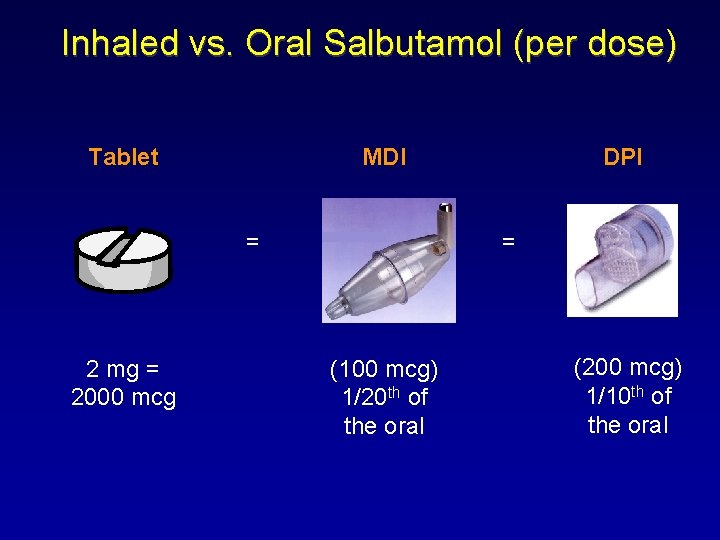
Inhaled vs. Oral Salbutamol (per dose) Tablet MDI = 2 mg = 2000 mcg DPI = (100 mcg) 1/20 th of the oral (200 mcg) 1/10 th of the oral
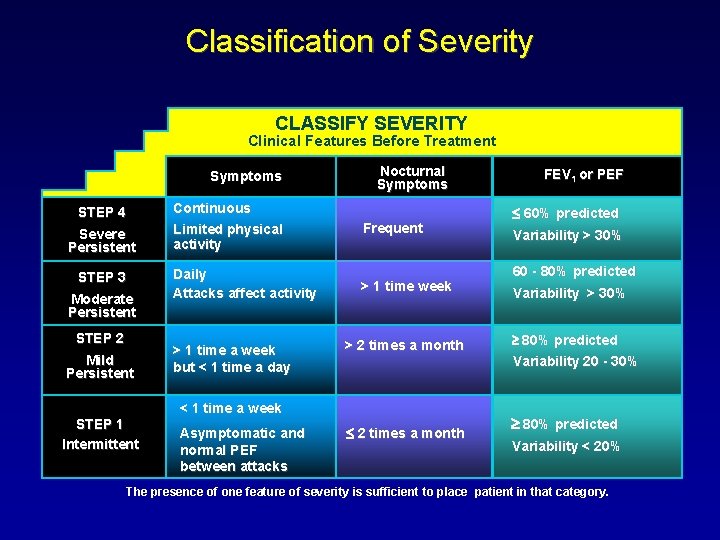
Classification of Severity CLASSIFY SEVERITY Clinical Features Before Treatment Symptoms STEP 4 Severe Persistent STEP 3 Moderate Persistent STEP 2 Mild Persistent Continuous Limited physical activity Daily Attacks affect activity > 1 time a week but < 1 time a day Nocturnal Symptoms Frequent > 1 time week > 2 times a month Asymptomatic and normal PEF between attacks 60% predicted Variability > 30% 60 - 80% predicted Variability > 30% 80% predicted Variability 20 - 30% < 1 time a week STEP 1 Intermittent FEV 1 or PEF 2 times a month 80% predicted Variability < 20% The presence of one feature of severity is sufficient to place patient in that category.
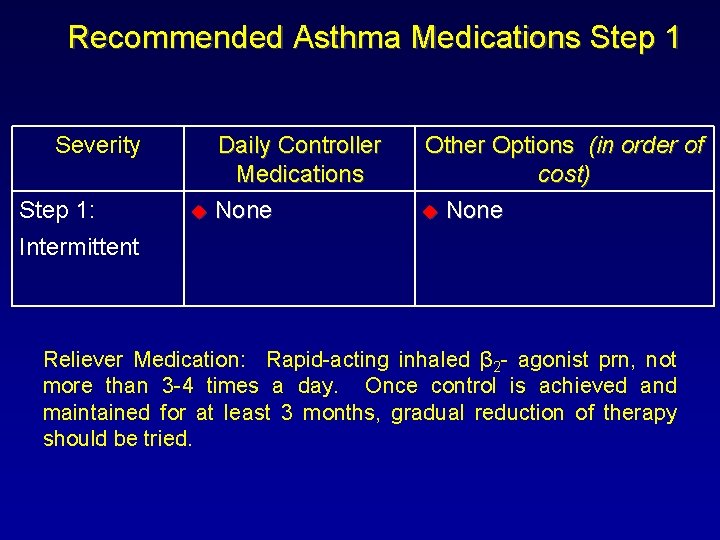

Recommended Asthma Medications Step 1 Severity Step 1: Daily Controller Medications u None Other Options (in order of cost) u None Intermittent Reliever Medication: Rapid-acting inhaled β 2 - agonist prn, not more than 3 -4 times a day. Once control is achieved and maintained for at least 3 months, gradual reduction of therapy should be tried.

‘If a patient uses quick-relief medications every day, or even more than three or four times a week, daily longterm preventive medications should be added to the treatment plan. ’

Recommended Asthma Medications Step 2 Severity Daily Controller Medications Other Options (in order of cost) Step 2: u Inhaled glucocorticosteroid u (< 500 μg BDP or equivalent) u Cromone, or u Leukotriene modifier Mild Persistent Sustained-release theophylline, or Reliever Medication: Rapid-acting inhaled β 2 - agonist prn, not more than 3 -4 times a day. Once control is achieved and maintained for at least 3 months, gradual reduction of therapy should be tried.

Recommended Asthma Medications Step 3 Severity Daily Controller Medications Step 3: u Moderate persistent Inhaled glucocorticosteroid (200 – 1000 μg BDP or equivalent) u plus long-acting inhaled β 2 - agonist Other Options (in order of cost) u Inhaled glucocorticosteroid (500 – 1000 μg BDP or equivalent) plus sustained- release theophylline, or u Inhaled glucocorticosteroid (500 – 1000 μg BDP or equivalent) plus long-acting inhaled β 2 - agonist, or u Inhaled glucocorticosteroid at higher doses (> 1000 μg BDP or equivalent), or u Inhaled glucocorticosteroid (500 – 1000 μg BDP or equivalent) plus leukotriene modifier Reliever Medication: Rapid-acting inhaled β 2 - agonist prn, not more than 3 -4 times a day. Once control is achieved and maintained for at least 3 months, gradual reduction of therapy should be tried.

Recommended Asthma Medications Step 4 Severity Daily Controller Medications Step 4 u Inhaled glucocorticosteroid ( > 1000 μg BDP or equivalent) plus long-acting inhaled β 2 - agonist u plus one or more of the following, if needed: Severe persistent Other Options - Sustained-release theophylline - Leukotriene modifier - Long-acting inhaled β 2 - agonist - Oral glucocorticosteroid Reliever Medication: Rapid-acting inhaled β 2 - agonist prn, not more than 3 -4 times a day. Once control is achieved and maintained for at least 3 months, gradual reduction of therapy should be tried.

u A stepwise approach to pharmacological therapy is recommended u The aim is to accomplish the goals of therapy with the least possible medication u Although in many countries traditional methods of healing are used, their efficacy has not yet been established and their use can therefore not be recommended
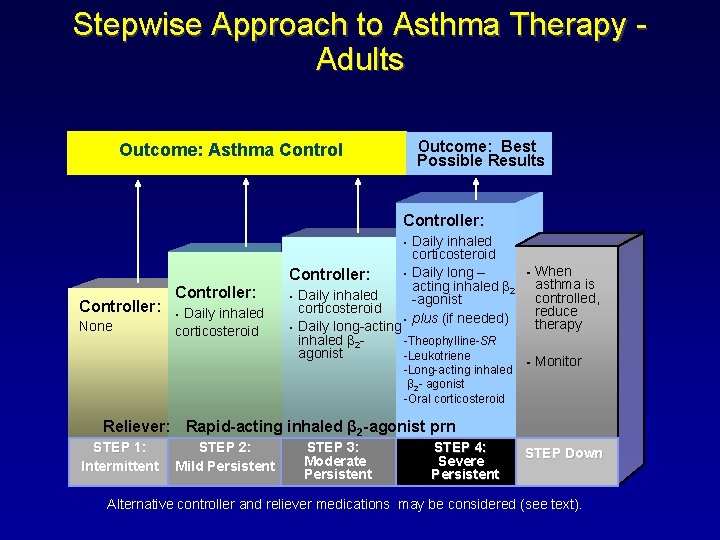
Stepwise Approach to Asthma Therapy Adults Outcome: Best Possible Results Outcome: Asthma Controller: § Controller: None Controller: Daily inhaled corticosteroid § § Daily inhaled corticosteroid Daily long – acting inhaled β 2 -agonist plus (if needed) Daily inhaled corticosteroid § Daily long-acting inhaled β 2 -Theophylline-SR agonist -Leukotriene -Long-acting inhaled β 2 - agonist -Oral corticosteroid § § When asthma is controlled, reduce therapy Monitor Reliever: Rapid-acting inhaled β 2 -agonist prn STEP 1: Intermittent STEP 2: Mild Persistent STEP 3: Moderate Persistent STEP 4: Severe Persistent STEP Down Alternative controller and reliever medications may be considered (see text).

Acute Severe Asthma § Exacerbations of asthma (acute severe asthma, status asthmaticus) are episodes of rapidly progressive increase in shortness of breath, cough, wheezing, or chest tightness, or some combination of these symptoms. u All patients with asthma are at risk of episodic deterioration in lung function to variable degrees. Acute severe asthma accounts for 4% of all emergency room visits annually.

Acute Severe Asthma u It is important to differentiate the underlying condition from the recurrent exacerbations. Asthma is a chronic disorder of the airways resulting in variable symptoms and airflow limitation over time. Exacerbations of asthma (attacks or worsening of asthma symptoms and lung function) are acute; they can be rapid in onset or occur gradually.

Acute Severe Asthma § However, under both circumstances exacerbations can be severe and even result in death in the absence of effective treatment. More often, presenting symptoms are less severe, and occasionally they may be totally absent.

Managing Acute Severe Asthma Primary therapies for exacerbations: u Repetitive administration of rapid-acting inhaled β 2 -agonist u Early introduction of systemic glucocorticosteroids u Oxygen supplementation Closely monitor response to treatment with serial measures of lung function
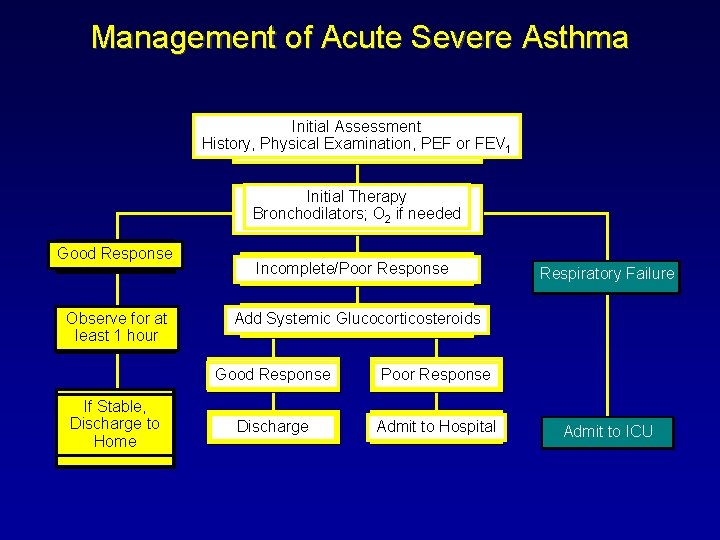
Management of Acute Severe Asthma Initial Assessment History, Physical Examination, PEF or FEV 1 Initial Therapy Bronchodilators; O 2 if needed Good Response Observe for at least 1 hour If Stable, Discharge to Home Incomplete/Poor Response Respiratory Failure Add Systemic Glucocorticosteroids Good Response Poor Response Discharge Admit to Hospital Admit to ICU
Conclusion Bronchodilator drugs Education of the patients Antiinflammatory drugs

Key Messages u Asthma is a common disorder. u It can happen to anybody. u It is not caused by supernatural forces. u Asthma is not contagious. u It produces recurrent attacks of cough with or without wheeze. u Asthma can be effectively treated. u Between attacks people with asthma lead normal lives as anyone else. u In most cases there is some history of allergy in the family.

Summary u Asthma can be effectively controlled, although it cannot be cured. u Effective asthma management programs include education, objective measures of lung function, environmental control, and pharmacologic therapy. u A stepwise approach to pharmacologic therapy is recommended. The aim is to accomplish the goals of therapy with the least possible medication.

Summary (continued) u Anything more than mild, occasional asthma is more effectively controlled by suppressing inflammation than by only treating acute bronchospasm u The availability of varying forms of treatment, cultural preferences, and differing health care systems need to be considered

THANK YOU
- Slides: 42