BRONCHIAL ASTHMA DR SHYAM SUDHIR PROF YMC ASTHMA

BRONCHIAL ASTHMA DR SHYAM SUDHIR PROF YMC

ASTHMA Epidemiology Pathophysiology Diagnosis

CHILDHOOD ASTHMA � Childhood bronchial asthma is characterized by � Airway obstruction – due to muscle spasm associated with mucosal oedema and stagnation of the mucus - which is reversible � Airway inflammation � Airway hyper responsiveness- virus and irritants � Airway remodeling in uncontrolled asthma.
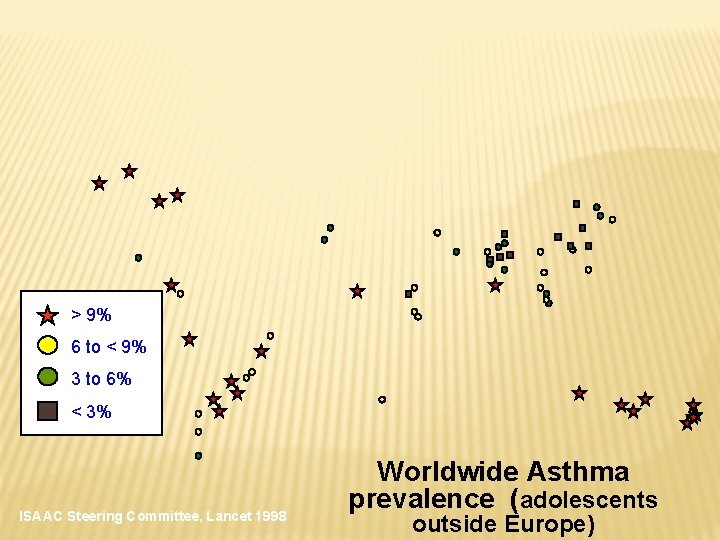
> 9% 6 to < 9% 3 to 6% < 3% ISAAC Steering Committee, Lancet 1998 Worldwide Asthma prevalence (adolescents outside Europe)

PREVALENCE OF BRONCHIAL ASTHMA � Worldwide variation in prevalence � Variation within countries ISAAC study – prevalence up to 25% � More than 180, 000 people die of asthma each year � 5, 000 deaths in the United States �
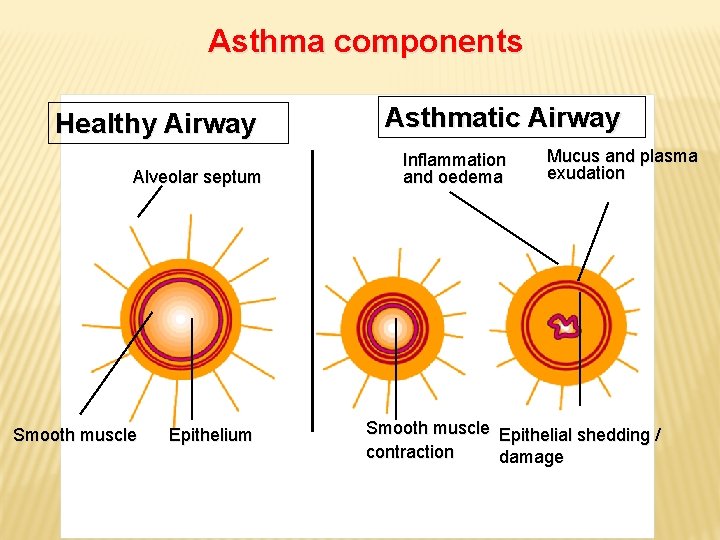
Asthma components Healthy Airway Alveolar septum Smooth muscle Epithelium Asthmatic Airway Inflammation and oedema Mucus and plasma exudation Smooth muscle Epithelial shedding / contraction damage
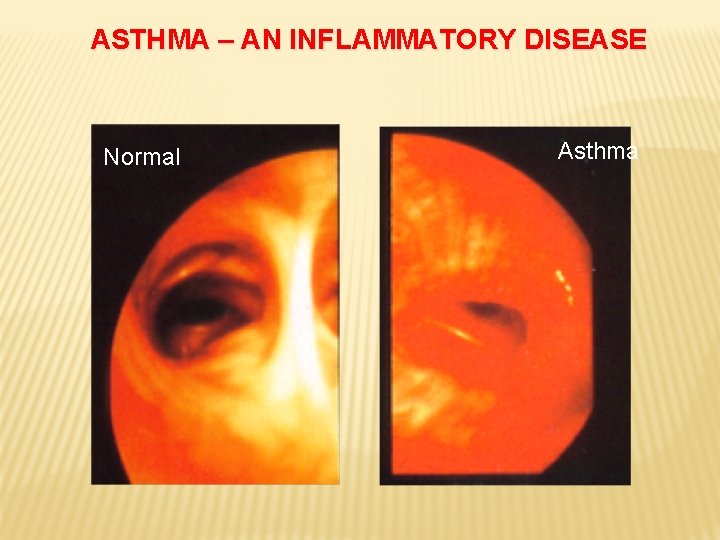
ASTHMA – AN INFLAMMATORY DISEASE Normal Asthma
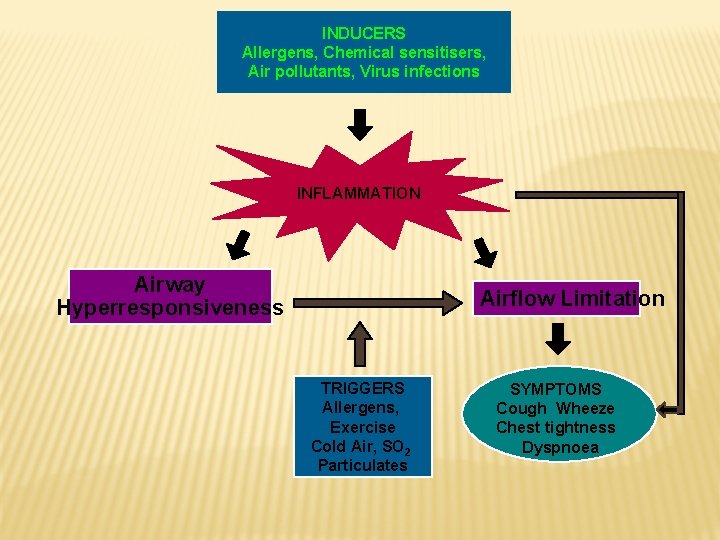
INDUCERS Allergens, Chemical sensitisers, Air pollutants, Virus infections INFLAMMATION Airway Hyperresponsiveness Airflow Limitation TRIGGERS Allergens, Exercise Cold Air, SO 2 Particulates SYMPTOMS Cough Wheeze Chest tightness Dyspnoea
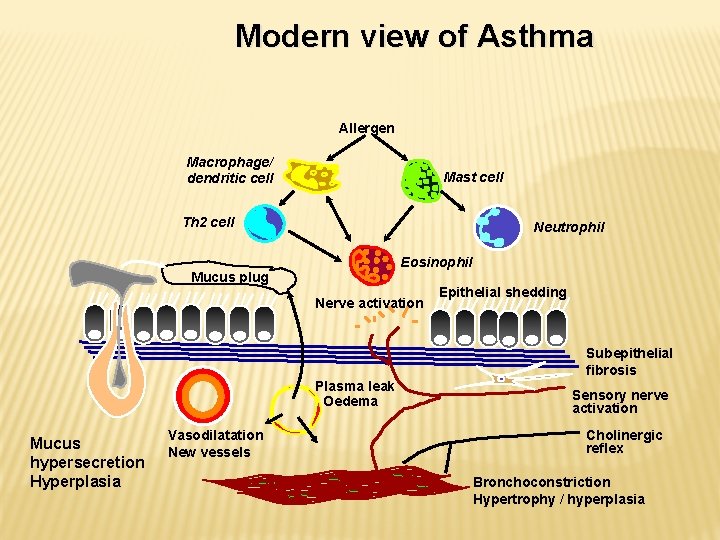
Modern view of Asthma Allergen Macrophage/ dendritic cell Mast cell Th 2 cell Neutrophil Eosinophil Mucus plug Nerve activation Epithelial shedding Subepithelial fibrosis Plasma leak Oedema Mucus hypersecretion Hyperplasia Vasodilatation New vessels Sensory nerve activation Cholinergic reflex Bronchoconstriction Hypertrophy / hyperplasia
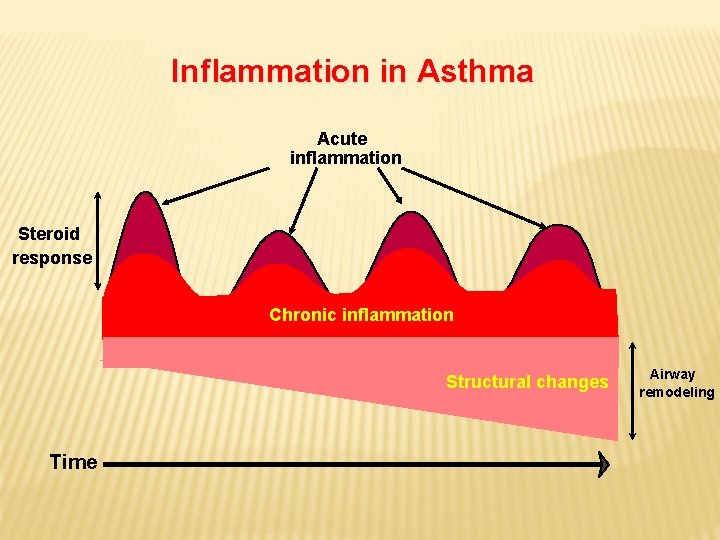
Inflammation in Asthma Acute inflammation Steroid response Chronic inflammation Structural changes Time Airway remodeling

DIAGNOSIS Bronchial asthma is an iceberg disease Classical features � Persistent cough, wheezing and dyspnoea are seen in 30% Atypical features � Cough-variant asthma � Nocturnal asthma � Activity-induced asthma � Persistent cough after an URI � Recurrent pneumonia at different sites/ same site (middle lobe)

GUIDELINES FOR DIAGNOSIS Diagnosis is mainly clinical � Episodic symptoms of airflow obstruction, more than 3 episodes are present � Airway obstruction is reversible � Alternative diagnoses are excluded

Ask about Triggers Symptoms can occur or worsen in the presence of: ALLERGENS � animal dander � dust mites � pollen � fungi OTHERS l exercise l viral infection l smoke l changes in temperature l strong emotional expression l aerosol chemicals l drugs (NSAIDs, ß-blockers)

INVESTIGATIONS � � � � Routine blood counts may not help Peripheral smear may show eosinophilia X–ray chest to rule out tuberculosis Sputum examination for eosinophils and Curschmanns spiral bodies – rarely needed Pulmonary function tests – Gold Standard Spirometry Peak Expiratory flow rate

PEAK EXPIRATORY FLOW RATE (PEFR) � Simple, Cheap and convenient � It is the fastest rate at which air can move through the airways during a forced expiration starting with fully inflated lungs � PEFR correlates well with FEV 1 � Used in children above 6 years � Useful for monitoring the patient both at home and office

PEAK FLOW METER

USES OF PEFR � For diagnosis and monitoring of asthma. � PEFR taken regularly can give a warning of an impending attack of bronchospasm before it starts. One can prevent it by stepping up the preventive therapies. � Long term follow up: Personal-best PEFR persistently below 20– 30% would indicate worsening of control of the disease.
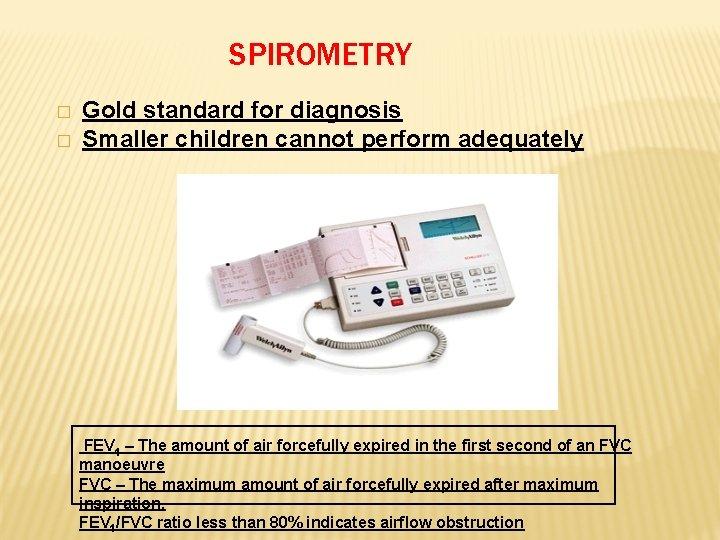
SPIROMETRY � � Gold standard for diagnosis Smaller children cannot perform adequately FEV 1 – The amount of air forcefully expired in the first second of an FVC manoeuvre FVC – The maximum amount of air forcefully expired after maximum inspiration. FEV 1/FVC ratio less than 80% indicates airflow obstruction
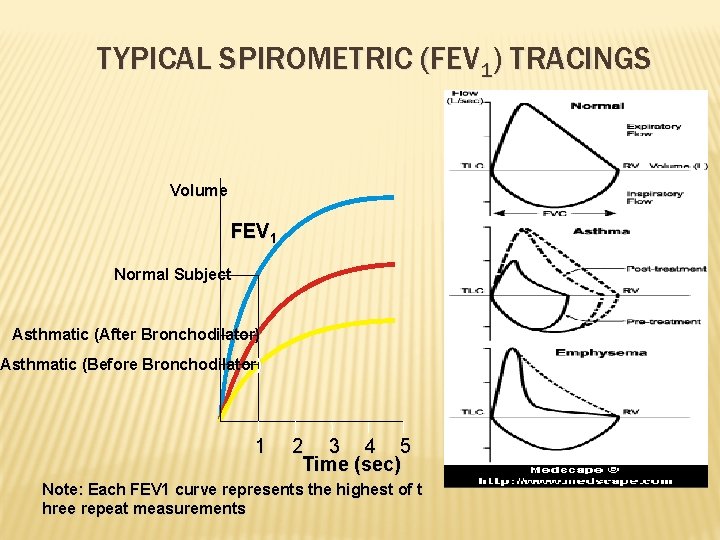
TYPICAL SPIROMETRIC (FEV 1) TRACINGS Volume FEV 1 Normal Subject Asthmatic (After Bronchodilator) Asthmatic (Before Bronchodilator) 1 2 3 4 5 Time (sec) Note: Each FEV 1 curve represents the highest of t hree repeat measurements

DIFFERENTIAL DIAGNOSIS OF WHEEZING Early infancy Birth– 6 months Aspiration syndromes (Gastroesophageal Reflux etc) Bronchiolitis Foreign body inhalation (Rarely) Infancy–Early childhood 6 months– 3 years Bronchiolitis Late childhood > 3 years Transient wheezing of childhood (TWC) Foreign body inhalation, Congenital heart disease, Infection e. g. , TB TWC Asthma Congenital heart disease

TREATMENT OF BRONCHIAL ASTHMA

TREATMENT OBJECTIVES � � � Freedom from � Acute asthma attacks � Symptoms including nocturnal cough � Emergency doctor/hospital visits Minimal need for quick relief (as needed) ß 2 -agonist Minimal (or no) adverse effects from medicine Normal � Physical activity including participation in sports � Maintain lung function as close to normal as possible Growth Charts

TREATMENT STRATEGY � Identify and avoid triggers that make asthma worse � Achieve control by selecting appropriate medication � Treat asthma attacks promptly and effectively � Educate patients to manage their condition � Monitor and modify asthma care to maintain effective long-term control
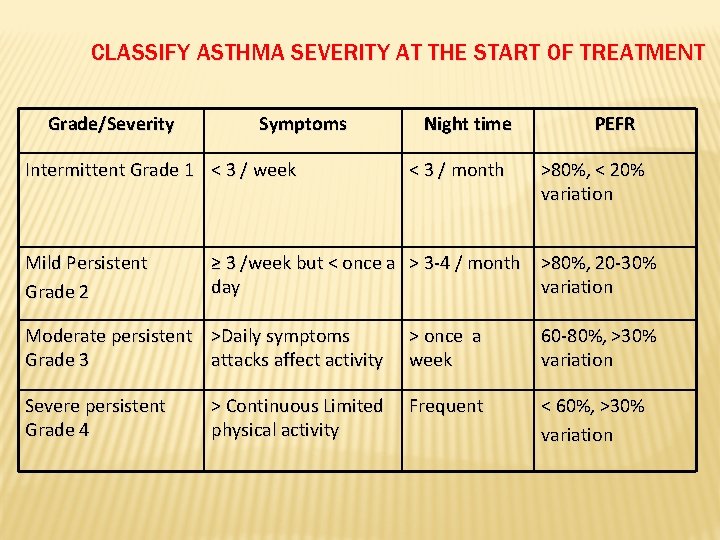
CLASSIFY ASTHMA SEVERITY AT THE START OF TREATMENT Grade/Severity Symptoms Intermittent Grade 1 < 3 / week Mild Persistent Grade 2 Night time < 3 / month PEFR >80%, < 20% variation ≥ 3 /week but < once a > 3 -4 / month >80%, 20 -30% day variation Moderate persistent >Daily symptoms Grade 3 attacks affect activity > once a week 60 -80%, >30% variation Severe persistent Grade 4 Frequent < 60%, >30% variation > Continuous Limited physical activity

DRUGS Relievers � To treat Controllers � For prevention of bronchospasm and further attacks relieve acute attacks
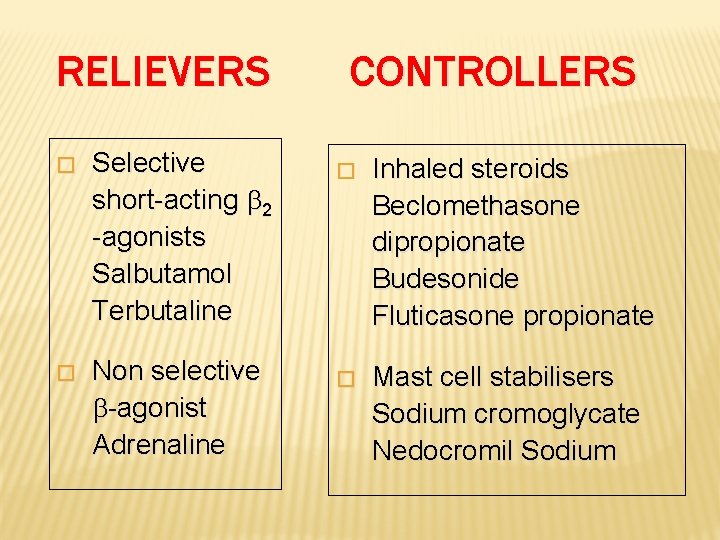

RELIEVERS � Selective short-acting 2 -agonists Salbutamol Terbutaline � Non selective -agonist Adrenaline CONTROLLERS � Inhaled steroids Beclomethasone dipropionate Budesonide Fluticasone propionate � Mast cell stabilisers Sodium cromoglycate Nedocromil Sodium

RELIEVERS CONTROLLERS � Anticholinergics � Long acting 2 -agonist Ipratropium bromide � Oral steroids � � Theophylline Salmeterol, Formoterol Methyl Xanthines Sustained-release theophylline Oral Prednisolone Leukotriene antagonists Montelukast, Zafirlukast, Pranlukast

NEW DRUGS Omalizumab—a recombinant humanised monoclonal anti-Ig. E antibody Ø Soft steroids– Ciclesonide ) Ø Phosphodiesterase 4 inhibitor-cilomilast. Ø Anti IL-5 therapy. Ø Vaccine. . Ø

Soluble cytokine receptors as thearapeutic agents. Nuvance Nebulisation Ø Single Isomer -agonists Levalbuterol (S-albuterol) Dose required is less than that of R-albuterol Ø Respirable antisense oligonucleotides eg: EPI- 2010 Ø

GRADE 1 Step 1: Intermittent asthma Controller None required Reliever n Inhaled 2 -agonist prn (not more than 3 times a week) n Inhaled 2 -agonist or cromone prior to exercise or allergen exposure Avoid or control triggers

Management of Persistent Asthma

INHALED STEROIDS – FIRST LINE TREATMENT Beclomethasone Propionate (BDP) � Budesonide (BUD) � Fluticasone (FP) Dose � Low dose < 400 mcg � Medium dose < 400– 800 mcg � High dose > 800 mcg. �

GRADE 2 Step 2: Mild persistent asthma Controller Reliever §Daily low dose inhaled corticosteroid (<400 g) OR §Inhaled sodium cromoglycate § Inhaled 2 -agonist prn (but less than 3 -4 times per day) §Nedocromil or leukotriene ↑ use may indicate need for modifier, sustained release long term control therapy theophylline Avoid or control triggers

GRADE 3 Step 3: Moderate persistent asthma Preventer ØDaily low dose inhaled steroid Reliever § Inhaled 2 -agonist prn + a) inhaled long-acting ß 2 §↑use may indicate need for agonist (may provide better long term control therapy control of symptoms) OR + n b) LTM, SR Theophylline and long acting ß agonist OR Ø Daily medium dose corticosteroid 400 -800 g Avoid or control triggers LTM: Leukotriene modifier

GRADE 4 Step 4: Severe persistent asthma Controller n Daily high dose inhaled corticosteroid > 800 g OR n Daily medium dose ICS + n Daily long-acting bronchodilator + theophylline or LTM n Daily oral corticosteroid tablets or syrup during acute exacerbation of asthma Reliever § Inhaled 2 -agonist prn (but less than 3 -4 times per day) §↑use may indicate need for long term control therapy Avoid or control triggers

ROLE OF LEUKOTRIENE ANTAGONISTS The only drug recommended in children is Montelukast – for children > 1 year Dose – 4 -5 mg once daily Indications – Mild persistent Asthma – Exercise induced Asthma – Aspirin induced Asthma -- As an add-on agent at steps 2, 3, and 4 when inhaled steroids are not enough Disadvantage – Poor efficacy (compared to inhaled steroids) – Few responders (unpredictable) – Expensive – Headaches (in 10%) – Weak anti–inflammatory effect
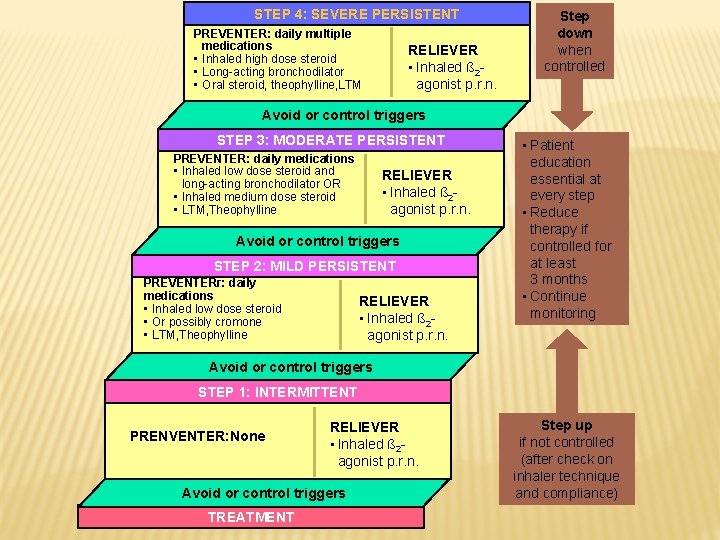
STEP 4: SEVERE PERSISTENT PREVENTER: daily multiple medications • Inhaled high dose steroid • Long-acting bronchodilator • Oral steroid, theophylline, LTM RELIEVER • Inhaled ß 2 agonist p. r. n. Step down when controlled Avoid or control triggers STEP 3: MODERATE PERSISTENT PREVENTER: daily medications • Inhaled low dose steroid and long-acting bronchodilator OR • Inhaled medium dose steroid • LTM, Theophylline RELIEVER • Inhaled ß 2 agonist p. r. n. Avoid or control triggers STEP 2: MILD PERSISTENT PREVENTERr: daily medications • Inhaled low dose steroid • Or possibly cromone • LTM, Theophylline RELIEVER • Inhaled ß 2 agonist p. r. n. • Patient education essential at every step • Reduce therapy if controlled for at least 3 months • Continue monitoring Avoid or control triggers STEP 1: INTERMITTENT PRENVENTER: None RELIEVER • Inhaled ß 2 agonist p. r. n. Avoid or control triggers TREATMENT Step up if not controlled (after check on inhaler technique and compliance)

Management of Acute Severe Asthma

SEVERE ACUTE ATTACK � � � Too breathless to feed Respiratory rate > 50 min Heart rate > 140 / min PEFR < 50% of the best Poor or only transient (<2 hr) response to bronchodilator Worsening despite 2– 3 doses of recent dose of bronchodilator at 15 minutes interval

LIFE-THREATENING ASTHMA IS CHARACTERIZED BY � � � � Unable to talk or cry Cyanosis Feeble chest movements Absent breath sounds Fatigue or exhausted Agitated Altered sensorium Oxygen saturation < 91% in pulse oximeter

Assessment of severity of an acute attack of bronchial asthma can be done by a simple scoring system called pulmonary score Index (PSI)–(PCNA December ‘ 99)
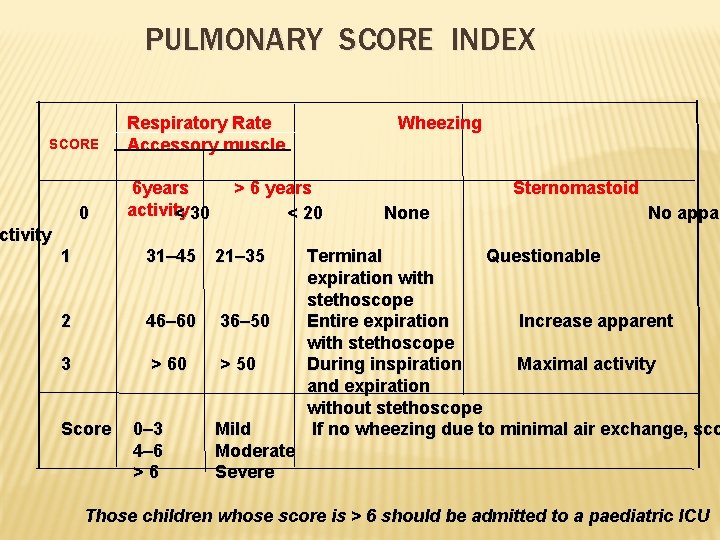
PULMONARY SCORE INDEX SCORE Respiratory Rate Accessory muscle Wheezing 6 years > 6 years Sternomastoid activity 0 < 30 < 20 None No appar ctivity 1 31– 45 21– 35 Terminal Questionable expiration with stethoscope 2 46– 60 36– 50 Entire expiration Increase apparent with stethoscope 3 > 60 > 50 During inspiration Maximal activity and expiration without stethoscope Score 0– 3 Mild If no wheezing due to minimal air exchange, sco 4– 6 Moderate > 6 Severe Those children whose score is > 6 should be admitted to a paediatric ICU

MANAGEMENT � � � Oxygen Adequate hydration Nebulised 2 -agonist, Intravenous beta agonist Electrolyte balance (hypokalemia due to repeated salbutamol nebulisations) Anticholinergic drugs Steroids S. C. inj of Epinephrine or S. C. inj agonists in severe cases Magnesium sulphate Ketamine IV Aminophylline Heliox Mechanical Ventilation

OXYGEN � � � Hypoxia is due to ventilation perfusion mismatch. –agonists may increase hypoxia by attenuating the hypoxic pulmonary vasoconstriction, hence oxygen should always be administered along with nebulised agonist. Maintain oxygen saturation between 90– 95%.

NEBULISED 2 -AGONISTS � � –agonists are the drug of choice in asthma. Patients with acute severe asthma will require and tolerate higher doses Dose of salbutamol - 0. 15 mg/kg, minimum 0. 25 ml for < 6 months, 0. 5 ml for > 6 months, 0. 5 – 1 ml for older children and adults. Dilute in normal saline only, never distilled water.

STEROIDS � Steroids reduce inflammation in this predominantly inflammatory illness � Should be used early in all patients with acute severe asthma � Hydrocortisone or methylprednisolone (MPS) may be administered IV if patient is unable to take oral steroids

RESCUE STEROIDS � Dose: MPS 2 mg/kg stat followed by 1 mg/kg q 6 hr OR Hydrocortisone 10 mg/kg stat followed by 5 mg/kg q 6 hr � IV steroids may be stopped after 48 hours or after improvement commences to thrice daily dosages � Oral or IV steroids are of more therapeutic value in the treatment of acute severe asthma � Inhaled or nebulised steroids are generally used as preventive therapy. However, some reports show benefits even in acute asthma

ANTICHOLINERGIC AGENTS: IPRATROPIUM � � Useful as an adjunct with salbutamol in the treatment of acute severe asthma Dose: < 1 year – 0. 5 ml , > 1 year – 1 ml Has longer duration of action and less systemic side effects compared to atropine Smaller children with spasmodic cough respond well to Ipratropium as compared to Salbutamol

MAGNESIUM SULPHATE � � Useful in severe asthmatics Mechanism: Calcium channel modulation results in decreased acetylcholine and histamine release Efficacy, dose and frequency have not been clearly worked out To be reserved for use in severe resistant asthma not responding to routine therapy

Suggested dose � 25– 50 mg/kg to be diluted in normal saline and administered as an infusion over ½ hour � Side effects � Tachycardia/bradycardia, hypotension, muscle weakness at higher serum level

INTRAVENOUS 2 AGONISTS � IV terbutaline or IV salbutamol may be used if patient fails to improve with nebulized 2 -agonists � Dose: Terbutaline, initial bolus of 5– 10 g/ kg over 10 minutes followed by 2– 10 g/kg/hour. Higher infusion rates may be used with caution

… CONTINUE � Continuous ECG monitoring. If HR 180/minute, arrhythmias or ST changes develop, dose � Discontinue nebulisation at higher infusion rate if signs of toxicity develop � Preparation of terbutaline: 1 ampoule (1 ml) contains 500 mcg. Dissolve 1 ampoule in 50 ml of 5% dextrose so that 1 ml = 10 mcg terbutaline

AMINOPHYLLINE � Doubtful additional bronchodilatation if optimal – agonists used � Possible role in improving diaphragmatic contractility and inflammatory modulation may confer additional benefit � Dose: Loading dose 5– 10 mg/kg/hr followed by 0. 5– 1. 0 mg/kg/hr � Avoid loading dose if patient already receiving theophylline � Dose of terbutaline to be decreased by 50% when concurrently infused with aminophylline

AMINOPHYLLINE – CONTD. . � � Monitor levels if possible, keep between 10 – 20 mcg/dl. Watch for drug interactions– anticonvulsants (decrease levels), H 2 blockers, macrolides (increase levels). Infections, especially viral also modify theophylline levels Toxicity – Gl (vomiting, gastritis), cardiac (tachycardia, arrhythmias), CNS (irritability, seizures)

ANTIBIOTICS Limited role. If there is fever and evidence of bacterial infection, the addition of antibiotics will help. Bacterial infections Seldom trigger asthmatic exacerbation

INDICATIONS FOR INTUBATION Absolute � Cardiac arrest � Comatose child � Severe respiratory distress � Silent chest, exhaustion Relative � Hypoxemia p. O 2<60 mm Hg in 60% oxygen � p. Co 2> 65 mm Hg & or p. Co 2 rising by > 5 mm Hg/hr � Metabolic acidosis (–BE > 8 – 10)

ALGORITHM FOR MANAGEMENT OF ACUTE SEVERE ASTHMA 1. Establish diagnosis, consider differential diagnosis particularly if first presentation 2. Assess severity Initial treatment � Oxygen to maintain saturation > 90– 95% � Nebulized salbutamol 3 doses at 20 minute intervals, < 20 kg: 0. 5 ml salbutamol with 3 ml N Saline. >20 kg: 1 ml salbutamol with 3 ml N Saline � Nebulized ipratropium: < 1 year – 0. 5 ml, > 1 year – 1 ml � Steroids: Methylprednisolone 2 mg/kg stat, followed by 1 mg/kg q 6 hr or Hydrocortisone– 10 mg/kg stat followed by 5 mg/kg x 6 th hourly daily O

Not improved Improved Reassess diagnosis Inj Magnesium Sulphate 25 -30 mg/kg in 10 ml N saline over 30 mins May be repeated after 6 hrs Not improved after 1 st dose Mg. SO 4 Terbutaline infusion Load with 5– 10 g/kg followed by 2 -10 g/kg (Increase dose every 15 minutes) Not improved Aminophylline infusion (Reduce terbutaline infusion by 50%) Not improved Mechanical ventilation Nebulised Salbutamol hourly Increased interval between doses as tolerated to Q-4 H Continue steroids, ipratropium
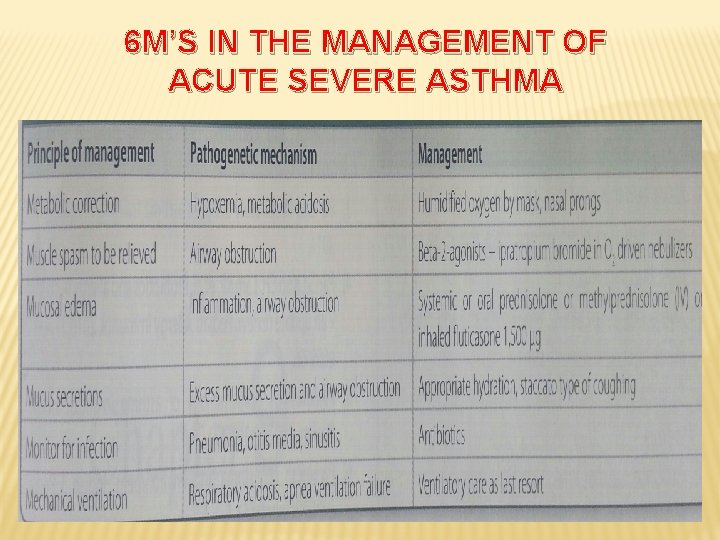
6 M’S IN THE MANAGEMENT OF ACUTE SEVERE ASTHMA

PATIENT EDUCATION

THE IMPORTANCE OF PATIENT EDUCATION IN ASTHMA Once patients understand about the disease and its treatment, control becomes easy � Pediatricians should handle commonly asked queries by patients ‘Physicians who give clear explanations to their patients are likely to be seen as competent and caring’ D L Roter and JA Hall. Doctors talking with patients, � patients talking with doctors: Improving communication in medical visits, page 13, Auburn House Publishers, USA

KEY FEATURES OF PATIENT EDUCATION Acceptance of diagnosis � Control but not necessarily cure � Understanding of pathophysiology and trigger factors � Concept of relievers and preventers � Advantages of inhalation therapy and its myths and misconceptions � Allay fears of steroids � Asthma monitoring All the above may not be done in one visit. � Reinforcement at regular intervals is important

ADDITIONAL INFORMATION � Asthma and exercise or activity � Consider informing school teachers and/or peers especially in severe cases

ACCEPTANCE OF DIAGNOSIS � � Asthma is like the tip of an iceberg If presents with classical features, parent acceptance easy If presents with atypical features (cough variant asthma), parent acceptance difficult. Wheeze associated lower respiratory infections – patients can be given a good prognosis.

FEAR OF STEROIDS � Patients should be reassured that steroids are completely safe when given by the inhaled route at therapeutic doses � Children with asthma who have been treated for up to 13 years have attained normal adult height � Uncontrolled asthma may itself lead to growth retardation

Allergen avoidance and avoidance of trigger factors

HOUSE DUST MITE Remove carpets or upholstery that tend together dust. � Use cotton sheets rather than woolen blanket. � Sun the room. � Dust mattresses periodically and expose them to Sunlight. Encase mattress in air tight cover. � Keep soft toys away from sleeping area and wash weekly with hot water � Vacuuming – not proven �

COCKROACHES � General hygiene measures to limit cockroach population. � Insecticide spraying to be done while child is away.

PETS (ANIMAL DANDER) � Gentle persuasion to give pet away � Pets not to be allowed in sleeping area /bed room. � Bathe pet weekly

MOULDS OR INDOOR FUNGAL SPORES: � Attend damp walls/ leakages. � Clear air conditioner filters monthly.

OUT DOOR ALLERGENS � Pollen (Flower) � Avoid flowering plants indoor � Stay indoor during harvesting and flowering season.

IRRITANTS & CHEMICALS � Passive smoking, Tobacco smoke � Fumes from kerosene stove, chulla, wood, cow dung � Agarbattis � Strong odors � Mosquito repellent mats & coils (Advice use of mosquito nets, long cloths) � Chalk, fine dust, sprays

OTHER IMPORTANT FACTORS � Food additives – (Sulphites, benzoate, monosodium glutamate) � Drugs: Avoid Aspirin, NSAIDs, Propranalol

ADJUVANT THERAPY � Yoga � Breathing exercises � Exercises such as swimming

TREATMENT FOR ASSOCIATED DISEASES 1. Allergic Rhinitis/Sinusitis a. Intranasal steroid spray Budesonide 100 mcg twice a day or Fluticasone 50 mcg once a day b. Oral antihistamines 2. Gastroesophagal Reflux Antireflux treatment. Oral Theophylline to be avoided.

But, this is not enough…

1) Classification of bronchial asthama? 2) Name some triggering factors of bronchial asthama? 3) Management of acute severe asthama? 4) Name the drugs used in bronchial asthama? 5) Montelukast.

1) 2) 3) 4) 5) Name one long acting bronchodilator_______. Expand RAST _____ Expand PEFR _____ Name two newer drugs used in the treatment of bronchial asthama? Repeated salbutomol nebulisation causes _______.

Thank you
- Slides: 79