Bronchial Asthma bronchiale n n n Asthma is

Bronchial Asthma bronchiale

n n n Asthma is characterized by episodic air-flow obstruction in response to a number of stimuli. Patients typically have paroxysms of wheezing, dyspnea and cough. Acute episodes of asthma may alternate with asymptomatic periods or be superimposed on a background of chronic airway obstruction. Severe acute asthma unresponsive to therapy is termed status asthmaticus. Most asthmatic patients, even when apparently well, have some persistent air-flow obstruction and morphologic lesions.

Asthma n n n Chronic inflammatory disorder of bronchi Episodic - Reversible bronchospasm Affects 10% of children & 5% adults Half of cases appear in patients younger than 10 years n Initial attack of the disease can occur at any age n

n Asthma was classically divided into Extrinsic (allergic) n Intrinsic (idiosyncratic) n depending on inciting factors.
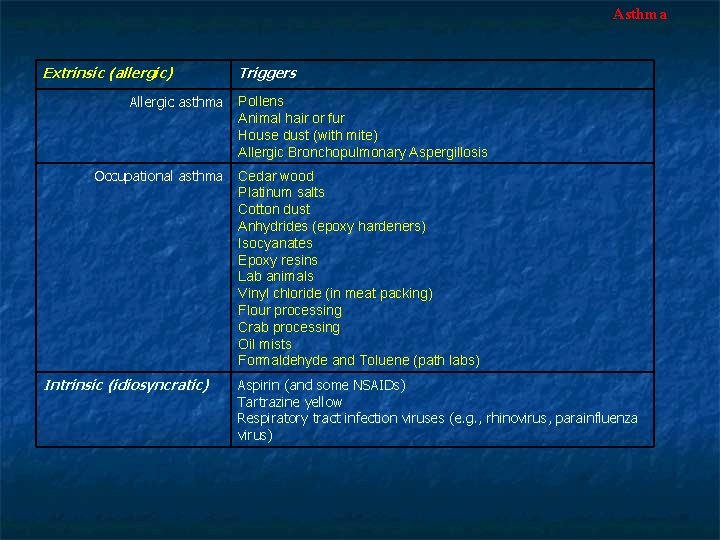
Asthma Extrinsic (allergic) Allergic asthma Occupational asthma Intrinsic (idiosyncratic) Triggers Pollens Animal hair or fur House dust (with mite) Allergic Bronchopulmonary Aspergillosis Cedar wood Platinum salts Cotton dust Anhydrides (epoxy hardeners) Isocyanates Epoxy resins Lab animals Vinyl chloride (in meat packing) Flour processing Crab processing Oil mists Formaldehyde and Toluene (path labs) Aspirin (and some NSAIDs) Tartrazine yellow Respiratory tract infection viruses (e. g. , rhinovirus, parainfluenza virus)

Asthma ALLERGIC ASTHMA n n n Most common form of asthma and is usually seen in children Type I hypersensitivity reaction induced by exposure to an extrinsic antigen. One third to one half of all patients with asthma have known or suspected reactions to such allergens as pollens, animal hair or fur, and house dust contaminated with mites Allergic asthma is strongly correlated with skin-test reactivity Half of all children with asthma have a substantial or complete remission of symptoms by age 20 n but in many, asthma may recur after age 30
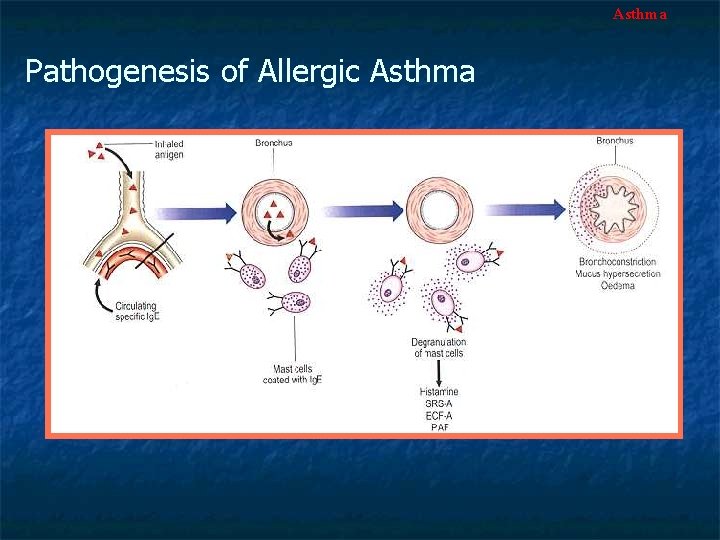
Asthma Pathogenesis of Allergic Asthma

Asthma Primary Mediators (1) Histamine (2) Eosinophilic and neutrophilic chemotactic factors (e. g. , leukotriene B 4) Secondary Mediators (1) Leukotrienes: (C 4, D 4, E 4) (2) Prostaglandin D 2 (PGD 2) (3) Platelet-activating factor (PAF) (4) cytokines (IL-1, TNF, IL-6)
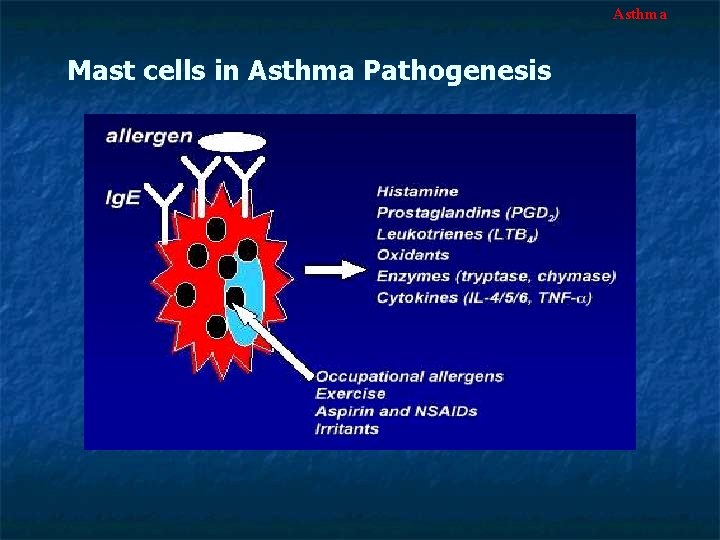
Asthma Mast cells in Asthma Pathogenesis

Asthma Eosinophils in Asthma Pathogenesis

Asthma INFECTIOUS ASTHMA n n n A common precipitating factor in childhood asthma is a viral respiratory tract infection rather than an allergic stimulus. In children under 2 years, Human respiratory syncytial virus (RSV) is the usual agent; in older children, rhinovirus, influenza, and parainfluenza are common inciting organisms. The inflammatory response to viral infection in a susceptible person is believed to trigger the episode of bronchoconstriction.

Asthma EXERCISE-INDUCED ASTHMA n Exercise can precipitate some bronchospasm in more than half of all asthmatics. n n Exercise-induced asthma is related to the magnitude of heat or water loss from the airway epithelium. n n In some patients, exercise is the only inciting factor. The more rapid the ventilation (severity of exercise) and the colder and drier the air breathed, the more likely is an attack of asthma. The mechanisms underlying exercise-induced asthma are unclear.

Asthma OCCUPATIONAL ASTHMA n n n More than 100 different occupational exposures have been linked to the development of asthma. In some instances, these substances provoke allergic asthma via Ig. E-related hypersensitivity. Examples of those so affected are animal handlers, bakers, and workers exposed to wood and vegetable dusts, metal salts, pharmaceutical agents, and industrial chemicals. In other cases, occupational asthma seems to result from direct release of mediators of smooth muscle contraction after contact with an offending agent. Some occupational exposures affect the autonomic nervous system directly.

Asthma n Occupational asthma Industrial asthma is a serious problem: n n n cedar wood platinum salt cotton dust anhydrides (epoxy hardeners) isocyanates epoxy resins lab animals vinyl chloride (in meat packing) flour processing crab processing oil mists formaldehyde and toluene (path labs)

Asthma DRUG-INDUCED ASTHMA n n n Drug-induced bronchospasm occurs mostly in patients with known asthma. The best-known offender is aspirin but other nonsteroidal anti-inflammatory agents also have been implicated. Aspirin induce arachidonic acid metabolism and elaboration of the bronchoconstrictor leukotrienes. n It is estimated that up to 10% of adult asthmatics are sensitive to aspirin.

Asthma n n n Immediate hypersensitivity does not seem to be involved, and these patients can be desensitized by daily administrations of small doses of aspirin. Serum Ig. E levels are normal. Skin test results are usually negative. Rhinitis and nasal polyps are also frequent findings in aspirin-sensitive individuals. b-Adrenergic antagonists consistently induce bronchoconstriction in asthmatics and are contraindicated in such patients.

Asthma n n AIR POLLUTION and EMOTIONAL FACTORS in Asthma bronchiale Air pollution n n Odors n n SO 2 Oxides of nitrogen Ozone Foul smelling gases Perfume Temperature inversions Psychological stress n Vagal efferent stimulation

Asthma Pathology From autopsies on patients who have died in status asthmaticus

Asthma Gross Pathology n n n The lungs are overdistended because of overinflation Small areas of atelectasis Occlusion of bronchi and bronchioles by thick, tenacious and adherent mucous plugs
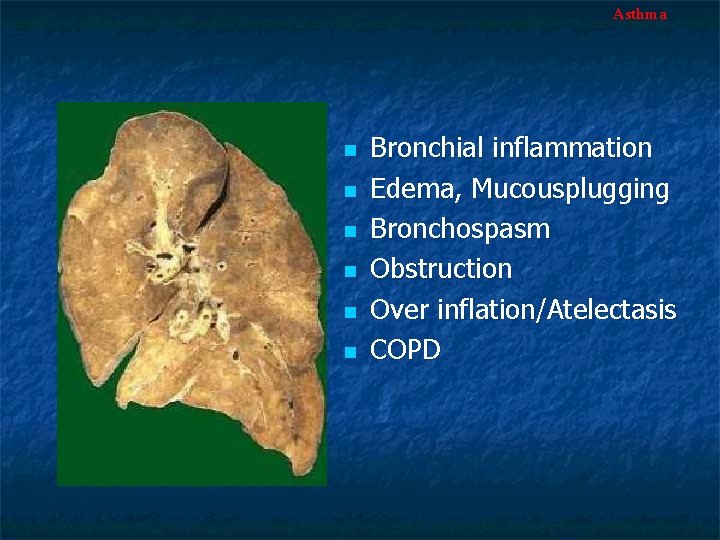
Asthma n n n Bronchial inflammation Edema, Mucousplugging Bronchospasm Obstruction Over inflation/Atelectasis COPD
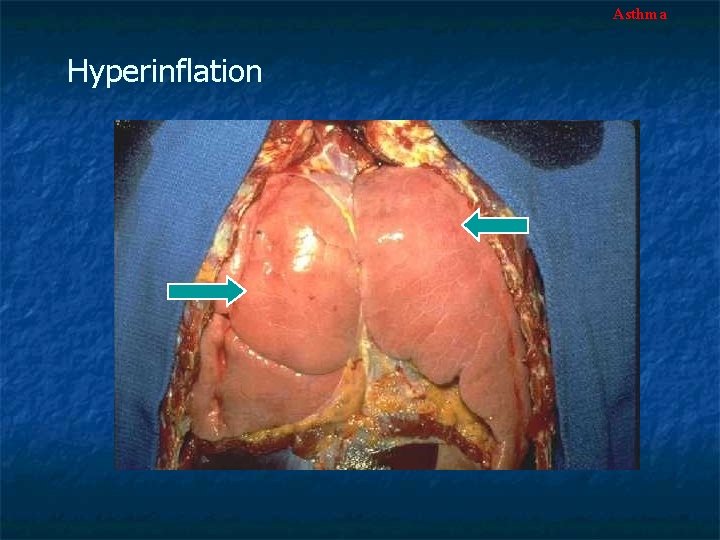
Asthma Hyperinflation

Asthma Mucous plugs
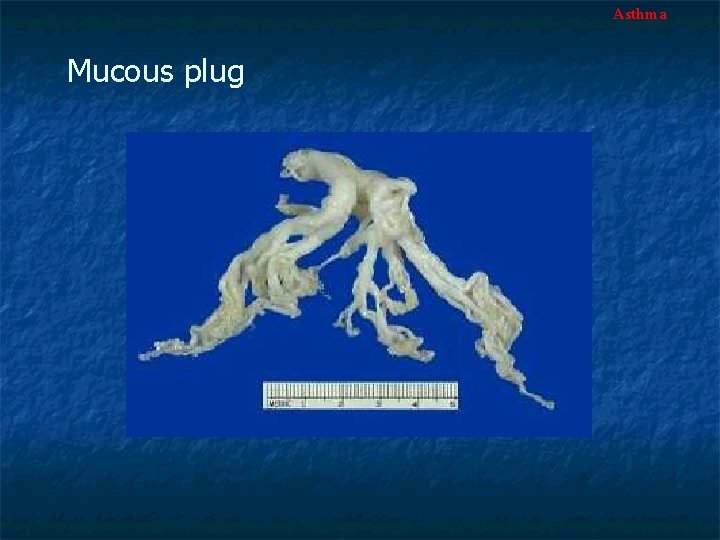
Asthma Mucous plug

Asthma Microscopy n n n n n Mucous plugs (strips of epithelium and many eosinophils) Curschmann spirals (mucoid exudate casts - may be expelled with coughing) Charcot Layden crystals (phospholipids of the eosinophil cell membrane) Creola bodies (compact clusters of epithelial cells in the sputum) Patchy necrosis of epithelium Submucosal glandular hyperplasia Goblet cell hyperplasia Hypertrophy of bronchial smooth muscle Mixed inflammatory infiltrate: Eosinophils (5 -50%) + Lympho (TH 2, CD 4) Mast cells
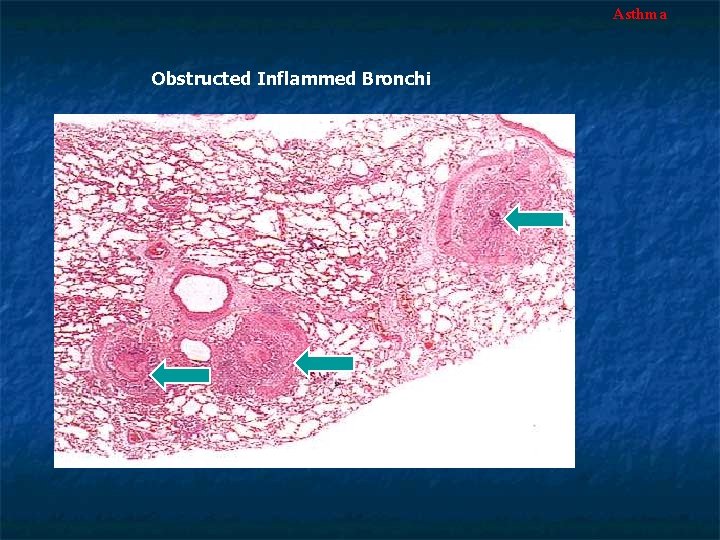
Asthma Obstructed Inflammed Bronchi
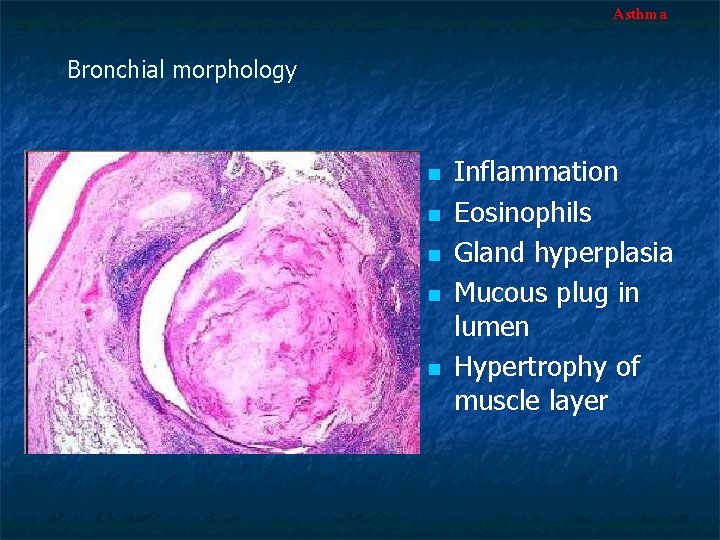
Asthma Bronchial morphology n n n Inflammation Eosinophils Gland hyperplasia Mucous plug in lumen Hypertrophy of muscle layer
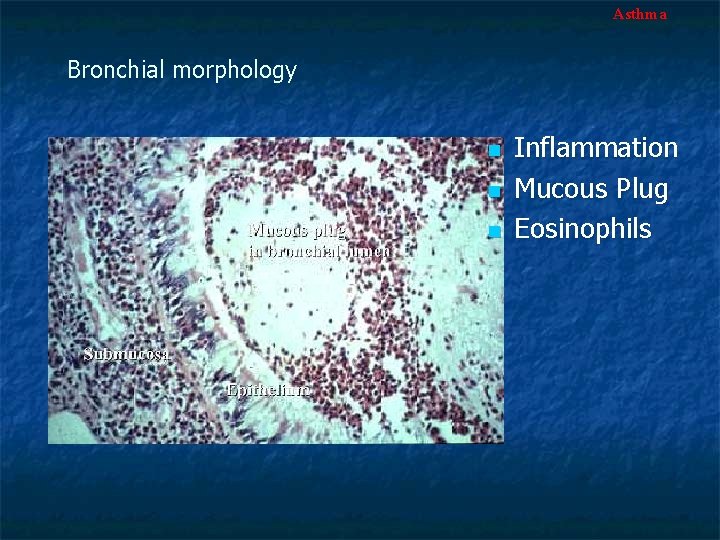
Asthma Bronchial morphology n n n Inflammation Mucous Plug Eosinophils
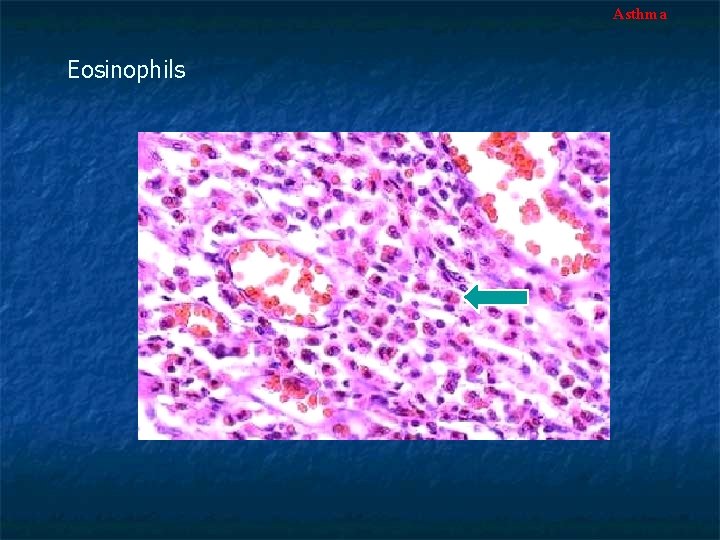
Asthma Eosinophils
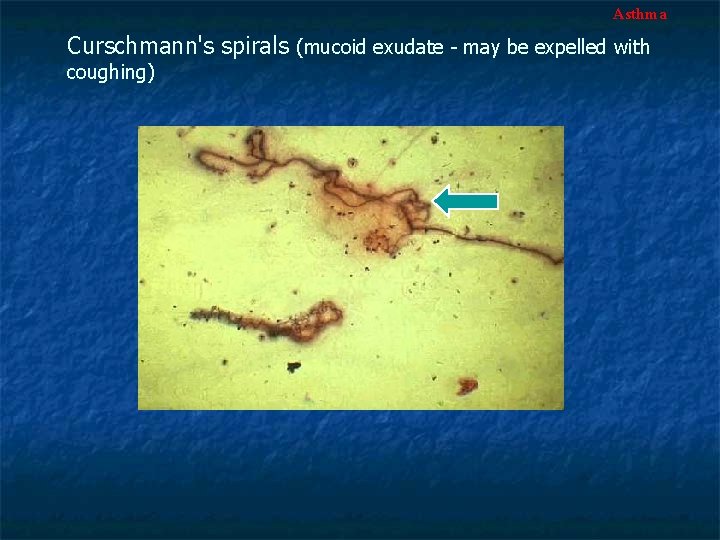
Asthma Curschmann's spirals (mucoid exudate - may be expelled with coughing)

Asthma The Reality n n n Asthma is not yet curable * Underdiagnosis & Undermanagement Therapy is still evolving Hope n n Better understanding of Pathology n New line of Promissing Drugs Proper management Normal life
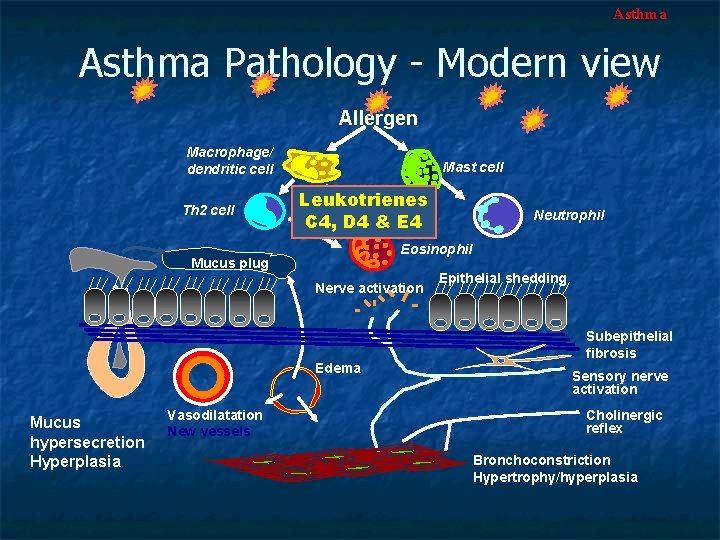
Asthma Pathology - Modern view Allergen Macrophage/ dendritic cell Th 2 cell Mast cell Leukotrienes C 4, D 4 & E 4 Eosinophil Mucus plug Nerve activation Edema Mucus hypersecretion Hyperplasia Vasodilatation New vessels Neutrophil Epithelial shedding Subepithelial fibrosis Sensory nerve activation Cholinergic reflex Bronchoconstriction Hypertrophy/hyperplasia

Asthma n An important clinical finding: Wheezing Asthma bronchiale n Foreign body or tumor in the upper airway n Pulmonary edema (especially left-sided congestive heart failure) n Pulmonary embolus n Chronic bronchitis n Carcinoid syndrome n
- Slides: 32