Bronchial asthma as neurogenic paroxysmal inflammatory disease high

Bronchial asthma as neurogenic paroxysmal inflammatory disease high efficacy of antiepileptic drug oxcarbazepine in asthma monotherapy Merab Lomia 1, 3, Manana Pruidze 2, Zaza Chapichadze 3 1“Rea” Rehabilitation Centre, Tbilisi, Georgia 2 Centre of Chinese Medicine, Tbilisi 3 Drug Agency, Ministry of Public Health, Tbilisi ERS Annual Congress, Copenhagen, Sept 17 -21

Asthma and other neurogenic inflammatory diseases n n Neurogenic inflammation may play important role in mechanism of asthma (Joos et al, 2003). Neurogenic inflammation plays important role in mechanisms of migraine (Hardebo, 1992) and trigeminal neuralgia (Strittmatter et al, 1997). Asthma is an inflammatory disease with paroxysmal clinical picture (Canadian asthma consensus report, 1999). Migraine and trigeminal neuralgia are inflammatory diseases with paroxysmal clinical picture (Krzhyzhanovskij, 1980). 2

Neurogenic inflammatory diseases, antiepileptic drugs and asthma n n u The same mediators (glutamate, tryptophane, etc. ) have equal activity in provoking or suppressing of asthma attacks, migraine attacks, trigeminal neuralgia attacks and epileptic seizures. Some antiepileptic drugs are very effective in therapy of migraine (Hering, Kuritzky, 1992; Corbo, 2003) and trigeminal neuralgia (Dalessio, 1987; Spina, Perugi, 2004). Are some antiepileptic drugs also effective in asthma therapy? 3

Antiepileptic drugs and asthma Our previous results and other data confirm our hypothesis: l Carbamazepine and valproates are highly effective in asthma monotherapy (Lomia et al, 2004). l Treatment of children with epilepsy and concomitant asthma by antiepileptic drugs significantly reduces severity of asthma (Ivanova, 1987). 4

The aims and design of the study n n n To establish the efficacy of oxcarbazepine in pharmacotherapy of adult patients with chronic asthma To establish the frequency of EEG and neurological signs in adult patients with bronchial asthma Double-blind, randomized, placebo-controlled study 5

Inclusion criteria n n Adult patients with bronchial asthma (aged 17 -73 years, 23 men, 23 women) were enrolled into the study Bronchial asthma has been known at least for 1 year Absence of long-term remissions of asthma (lasting more than 1 month) Poorly controlled asthma, due to various reasons 6

Exclusion criteria n n Presence of concomitant severe diseases Allergy or intolerance to oxcarbazepine or carbamazepine n Age younger than 16 years old n Permanent use of long-term beta-agonists n Long-term history of smoking n Pregnancy or lactating 7

Methods: randomization and medication u Randomized, placebo-controlled, double-blind study u Randomization: computer-generated u Initial 2 -week run-in period u 3 months (13 weeks) treatment period u Medication (capsules): 4 oxcarbazepine (300 mg) 4 placebo 8

Methods: dose titration and use of other antiasthmatic drugs u = Dose titration till 1 -2 caps. 2 times a day - first 1015 days Patients were allowed to abandon any other previously prescribed routine antiasthmatic treatment in case of asthma symptoms disappearance, lasted at least 1 month after beginning the trial 9

Methods: registered data l l l PEF am, pm - every day (Mini-Wright flow-meters) FEV 1 - every week in the morning FEV 1 before and after use of inhaled salbutamol before and after the study in the morning EEG-mapping and neural signs - before the study Routine blood analysis - every month Diary card: 4 daytime asthma symptom scores (0 -3) 4 nighttime awakening due to asthma (0 -1) 4 PEF am, pm 4 adverse events 10

Patients 55 patients eligible to participate in the trial: n oxcarbazepine group - 35 patients, n placebo group - 20 patients. 9 patients were excluded: w 3 from oxcarbazepine group: w 2 - due to stable side effects - dizziness and somnolence 1 - due to non-compliance 6 from placebo group - due to non-compliance 46 patients (32 of oxcarbazepine group and 14 of placebo group) completed the study. 11

Statistical analysis n n Wilcoxon signed rank test was used throughout for statistical analysis of non-parametric related data Mann-Whithey U-test was used for analysis of nonparametric independent data n Student t-test for parametric data n A p-value 0. 05 was considered significant n n For statistical analysis of data we used SPSS for Windows (Release 11. 0) Data is presented as Mean ± Standard Deviation 12

Baseline characteristics of patients 13
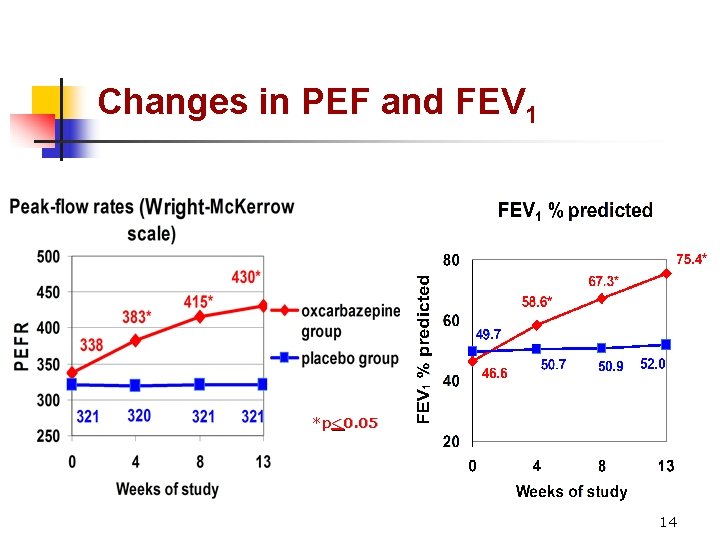
Changes in PEF and FEV 1 *p<0. 05 14
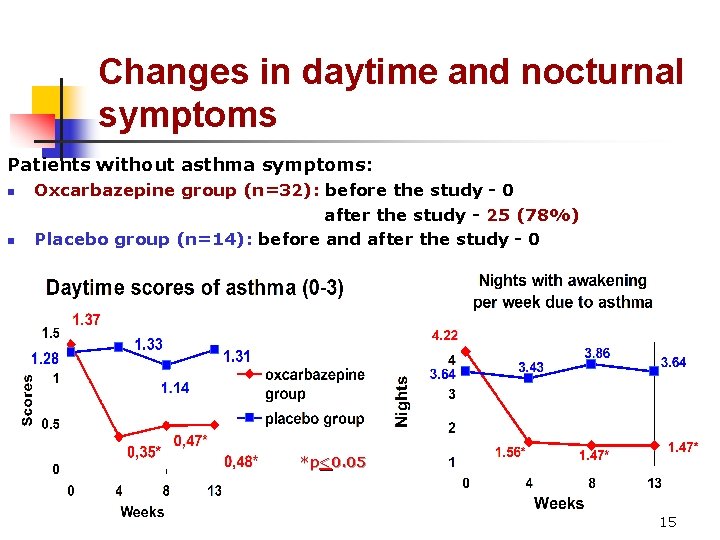
Changes in daytime and nocturnal symptoms Patients without asthma symptoms: n n Oxcarbazepine group (n=32): before the study - 0 after the study - 25 (78%) Placebo group (n=14): before and after the study - 0 *p<<0. 05 *p 15
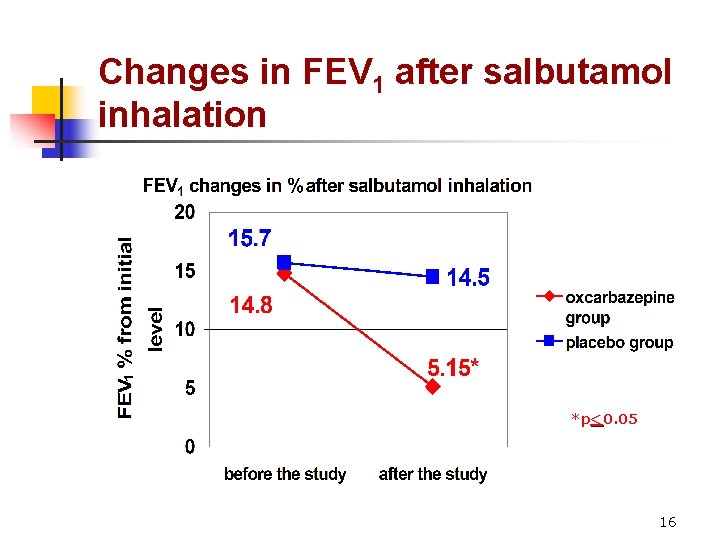
Changes in FEV 1 after salbutamol inhalation *p<0. 05 16
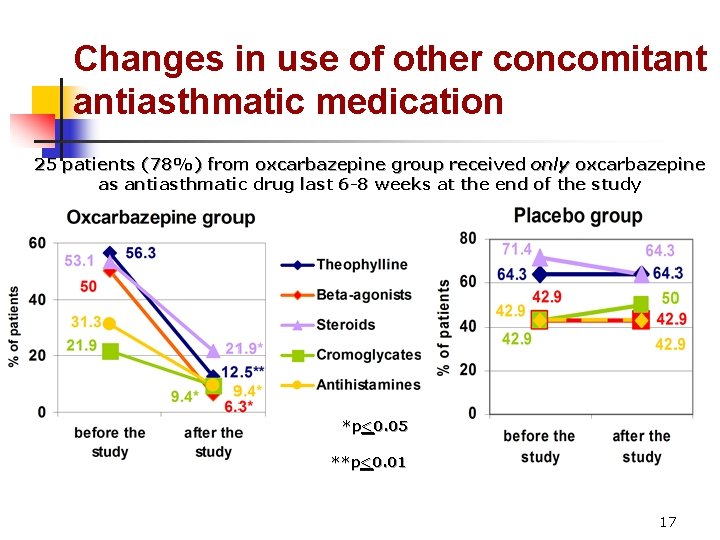
Changes in use of other concomitant antiasthmatic medication 25 patients (78%) from oxcarbazepine group received only oxcarbazepine as antiasthmatic drug last 6 -8 weeks at the end of the study *p<0. 05 **p<0. 01 17
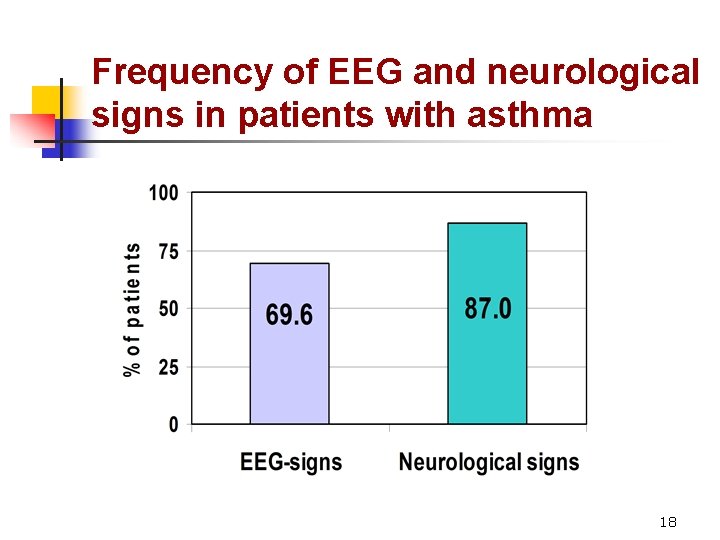
Frequency of EEG and neurological signs in patients with asthma 18

Adverse events Transient and mild adverse events in 6 patients (2 men and 4 women) only in first 2 weeks after the beginning of the study n n dizziness - in 2 cases (women)* somnolence - in 1 cases (man)** headache - in 2 cases (1 man, 1 woman)* somnolence and headache - in 1 case (woman)* * - oxcarbazepine group, ** - placebo group 19

Next open-label observation - I n n All 25 responder patients from oxcarbazepine group continued therapy with oxcarbazepine After 1 -3 months from the end of the study 20 patients gradually changed oxcarbazepine to carbamazepine (due to economical reason) 20

Next open-label observation - II After 3 years: ® All 25 responder patients (78%) from 33 patients of oxcarbazepine group have no symptoms of asthma ® 20 patients do not receive any drugs, including oxcarbazepine or capbamazepine ® 5 patients still receive only carbamazepine as antiasthmatic drug 21

Conclusions I Oxcarbazepine as antiasthmatic drug in 78% of cases: l Increases PEF and FEV 1 rates up to normal level l Reduces asthma symptoms down to complete remission l Reduces need of any other antiasthmatic therapy as far as complete abandoning n l l EEG and neurological signs in adult patients with asthma: 69. 6% have EEG-signs 87% have neurological signs 22

Conclusions II Some antiepileptic drugs are much better in comparison with other antiasthmatic drugs, because antiepileptic drugs in 70 -80% of cases show next results: ® No asthma symptoms ® Nearly normal lung function ® No need of other antiasthmatic drugs ® Minimal or no side effects ® No limitation of physical activities ® No emergency visits to doctors ® No limitation of trigger factors, including allergens 23

Hypothesis: asthma as neurogenic inflammatory paroxysmal disease - I Bronchial asthma is a paroxysmal neurogenic inflammatory disease with the complex pathogenic mechanism, including two levels of components: 1) multiple trigger components (including allergy, exercises, weather, etc. ), and 2) central neurogenic generator component of paroxysmal attacks of bronchial constriction and concomitant inflammation 24

Hypothesis: asthma as neurogenic inflammatory paroxysmal disease - II l Under the influence of trigger components the paroxysmal generator component is induced and pathologic process appears: u with manifestation of periodic paroxysmal bronchial smooth muscles spasms, induced by the central structures of autonomic nervous system, and u with concomitant chronic neurogenic inflammation 25

Hypothesis: asthma as neurogenic inflammatory paroxysmal disease - III l Vicious cycle is formed: trigger components provoke activity of generator component and vice versa l This is a mechanism of sustaining of asthma as a chronic disease. Abnormally increased vagal tone during asthma prevents generalization of paroxysmal activity into other parts of central nervous system l Constitutional predisposition to the development of neurogenic generator component is necessary for asthma development 26
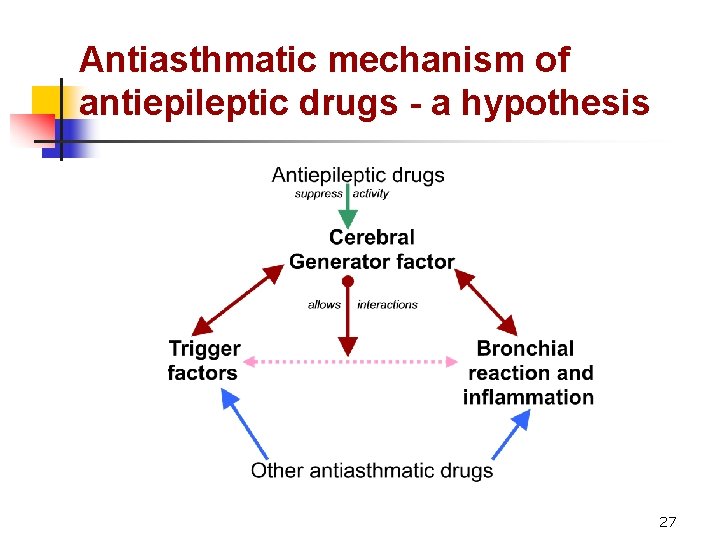
Antiasthmatic mechanism of antiepileptic drugs - a hypothesis 27

Nature of bronchial asthma u Is bronchial asthma peripheral disease with definite central mechanism? 28

Next studies in this direction are necessary Thank you 29

References n n n Joos GF, De Swert KO, Schelfhout V , Pauwels RA. The Role of Neural Inflammation in Asthma and Chronic Obstructive Pulmonary Disease. Ann NY Acad Sci 2003: 992: 218 -230. Hardebo JE. A cortical excitatory wave may cause both the aura and the headache of migraine [review]. Cephalalgia 1992: 12(2): 75 -80. Strittmatter M, Grauer M, Isenberg E, Hamann G, Fischer C, Hoffmann KH, et al. Cerebrospinal fluid neuropeptides and monoaminergic transmitters in patients with trigeminal neuralgia. Headache 1997: 37(4): 211 -216. Canadian asthma consensus report. CMAJ 199: 161 (11 Suppl): S 1 -S 5. Kryzhanovskii GN. Determinant structures in pathologic conditions of the nervous system. Generator mechanisms of neuropathologic syndromes. Meditsina, Moscow, 1980. Hering R. Kuritzky A. Sodium valproate in the prophylactic treatment of migraine: a double-blind study versus placebo. Cephalalgia 1992: 12(2): 81 -84. Corbo J. The role of anticonvulsants in preventive migraine therapy. Curr Pain Headache Rep 2003: 7(1): 63 -66. Dalessio DJ. The major neuralgias, postinfection neuritis, and atypical facial pain. In: Dalessio DJ, ed. Wolff’s Headache and Other Head Pain. Oxford University Press, Oxford, New York 1987; 266 -288. Spina E, Perugi G. Antiepileptic drugs: indications other than epilepsy (review). Epileptic Disorders 2004: 6(2): 57 -75. Lomia M, Chapichadze Z. , Pruidze M. Efficacy of monotherapy with anticonvulsive drugs topiramate and carbamazepine in bronchial asthma: is asthma a neurological disease? Eur Respir J 2004: 24 Suppl 48: S 130. Lomia M, Pruidze M, Chapichadze Z. Bronchial asthma as neurogenic paroxysmal disease - high effectiveness of carbamazepine in asthma monotherapy. Eur Respir J 2004: 24 Suppl 48: S 221. Ivanova NA. Epilepsy in structure of concomitant diseases in children with bronchial asthma and principles of complex therapy [Russian]. In: Modern principles of treatment of children with relapsing and chronic bronchial and lungs 30 diseases. Leningrad, 1987, 89 -91.

Asthma and breath-holding spells: paroxysmal respiratory diseases Bronchial asthma and breath-holding spells (BHS): | vagal tone is high due to autonomic dysregulation | paroxysmal clinical picture | expiratory flow is impaired (dyspnoea in asthma and temporary apnoea in BHS) | antiepileptic agents are highly effective in monotherapeutic mode Is BHS an intermediate form between asthma and epilepsy? 31
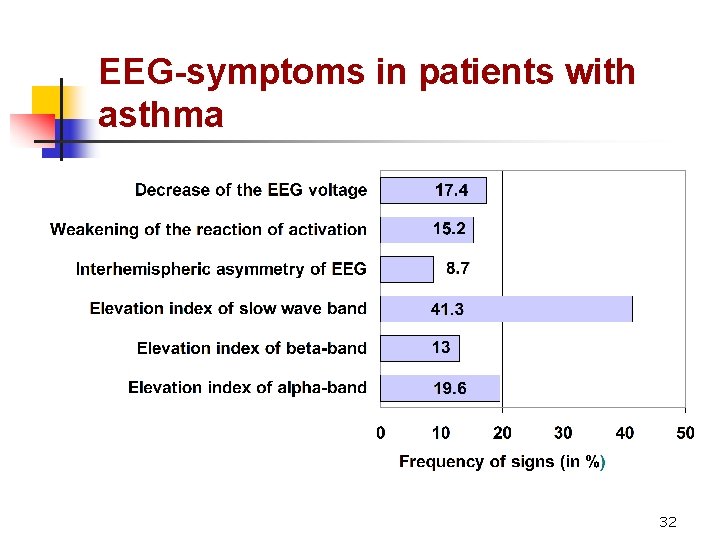
EEG-symptoms in patients with asthma 32
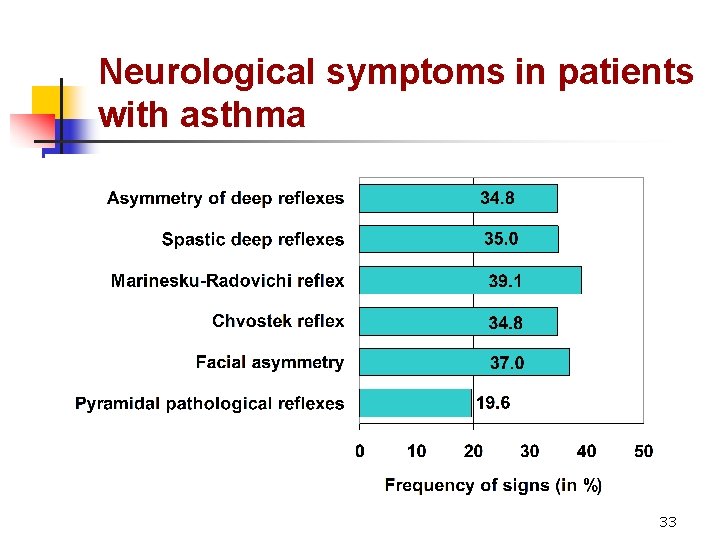
Neurological symptoms in patients with asthma 33
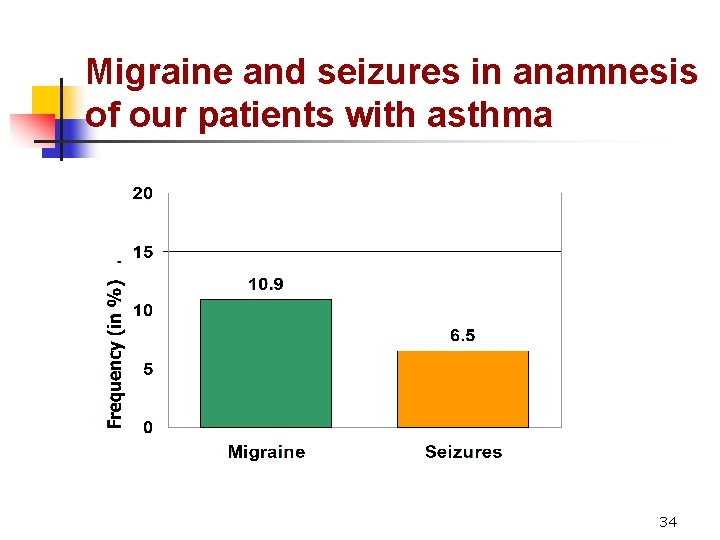
Migraine and seizures in anamnesis of our patients with asthma 34
- Slides: 34