British Thoracic Society Guideline for oxygen use in

British Thoracic Society Guideline for oxygen use in healthcare and emergency settings Key messages for doctors This presentation was last updated on 12/05/2017

BTS guideline for oxygen use in adults in healthcare and emergency settings is endorsed by Association of British Neurologists Association of Chartered Physiotherapists in Respiratory Care Association of Palliative Medicine Association of Respiratory Nurse Specialists Association for Respiratory Technology and Physiology British Association of Stroke Physicians British Geriatric Society College of Paramedics Intensive Care Society Joint Royal Colleges Ambulance Liaison Committee Primary Care Respiratory Society UK Resuscitation Council (UK) Royal College of Anaesthetists The Royal College of Emergency Medicine Royal College of General Practitioners Royal College of Nursing (endorsement until April 2020) Royal College of Obstetricians and Gynaecologists Royal College of Physicians London Royal College of Physicians of Edinburgh Royal College of Physicians and Surgeons of Glasgow Royal Pharmaceutical Society The Society for Acute Medicine O’Driscoll BR et al Thorax 2017; 72: Suppl 1 i 1 -i 89 12/05/2017

BTS guideline for oxygen use in adults in healthcare and emergency settings: Overview • Why have a guideline? • Oximetry as the basis of the guideline • Normal range of oximetry • Effects of hypoxaemia – sudden onset and gradual onset • Aims of oxygen treatment and its place in resuscitation • Recommended target saturations – with rationale • Oxygen Alert cards • Prescribing oxygen • Devices • What device and flow to use • Monitoring Guideline and this lecture available on BTS website www. brit-thoracic. org. uk 12/05/2017

Oxygen - there is a problem Published audits have shown that… • Doctors and nurses have a poor understanding of how oxygen should be used • Oxygen is often given without a prescription (In the 2015 BTS audit, 42% of hospital patients using oxygen had no prescription) • If there is a prescription, patients do not always receive what is specified on the prescription • Where there is a prescription with target range, almost one third of patients are outside the range (9. 5% of Sp. O 2 results below target range and 21. 5% above target range in 2015 BTS audit) 12/05/2017

BTS guideline for oxygen use in adults in healthcare and emergency settings • The British Thoracic Society, together with 21 other Societies and Colleges produced a multi-discipline Guideline for emergency oxygen use in 2008 • This Guideline covers all aspects of emergency oxygen use in pre-hospital care and in emergency hospital care • It has been updated and expanded in 2017 12/05/2017

Basis of the BTS guideline: Prescribing by target oxygen saturation Keep the oxygen saturation normal/near-normal for all patients except pre-defined groups who are at risk from hypercapnic respiratory failure 12/05/2017

What is normal and what is dangerous? 12/05/2017
Normal Range for Oxygen saturation Normal range for healthy young adults is approximately 96 -98% (Crapo AJRCCM, 1999; 160: 1525) There is a slight fall with advancing age A study of 871 subjects showed that age > 60 was associated with minor Sp. O 2 reduction of 0. 4% (Witting MD et al Am J Emerg Med 2008: 26: 131 -136) An audit in Salford and Southend showed mean Sp. O 2 of 96. 7% with SD 1. 9 in 320 stable hospital patients aged >70 without lung disease or heart failure (2 SD range 92. 9 to 100%) (O’Driscoll R et al Thorax 2008; 63(suppl Vii): A 126) 12/05/2017

What is a “normal” nocturnal oxygen saturation? Healthy subjects in all age groups routinely desaturate to an average nadir of 90. 4% during the night (SD 3. 1%) Gries RE et al Chest 1996; 110: 1489 -92 *Therefore, be cautious in interpreting a single oximetry measurement from a sleeping patient. Watch the oximeter for a few minutes if in any doubt (if the patient is otherwise stable) because normal overnight dips are of short duration. 12/05/2017

Effects of sudden hypoxaemia (e. g Removal of oxygen mask at altitude or in a pressure chamber) • Impaired mental function; Mean onset at Sa. O 2 64% No evidence of mental impairment above Sa. O 2 84% • Loss of consciousness at mean saturation of 56% • Test Pilots in decompression chambers do not experience breathlessness when the oxygen tension is lowered, they make mistakes and then pass out Akero A et al Eur Respir J. 2005 ; 25: 725 -30 Cottrell JJ et al Aviat Space Environ Med. 1995 ; 66: 126 -30 Hoffman C, et al. Am J Physiol 1946, 145, 685 -692 12/05/2017

Clinical features of hypoxaemia The effects are often non-specific Depends if onset is chronic or acute • Altered mental state • Dyspnoea, cyanosis, tachypnoea, arrhythmias, coma • Hyperventilation when Pa. O 2 <5. 3 k. Pa (saturation <72%) • Loss of consciousness ~ 4. 3 k. Pa (saturation ~56%) • Death approximately 2. 7 k. Pa 12/05/2017

Assessment/Measurement of hypoxaemia CYANOSIS - Often not recognised, - Absent with anaemia BLOOD GASES - Pa. O 2 and Sa. O 2 Pa. O 2 = Arterial oxygen partial pressure in blood gas specimen Sa. O 2 =Arterial oxygen saturation measured in blood gases OXYGEN SATURATION - Easily measured by pulse oximetry Sp. O 2 is widely available Sp. O 2 = Oxygen saturation measured by pulse oximeter 12/05/2017

What happens at 9, 000 metres (approximately 29, 000 feet) – it depends Atmospheric p. O 2 5. 7 k. Pa (< 1/3 sea level atmospheric oxygen tension) Pa. O 2 ~3. 3 k. Pa Arterial Oxygen Saturation ~54% SUDDEN Passengers unconscious in <60 seconds if depressurised 12/05/2017 ACCLIMATISATION Everest has been climbed without oxygen

Why is oxygen used? 12/05/2017

Aims of emergency oxygen therapy • To correct potentially harmful hypoxaemia • To alleviate breathlessness (only if hypoxaemic) Oxygen has not been proven to have any consistent effect on the sensation of breathlessness in non-hypoxaemic patients 12/05/2017
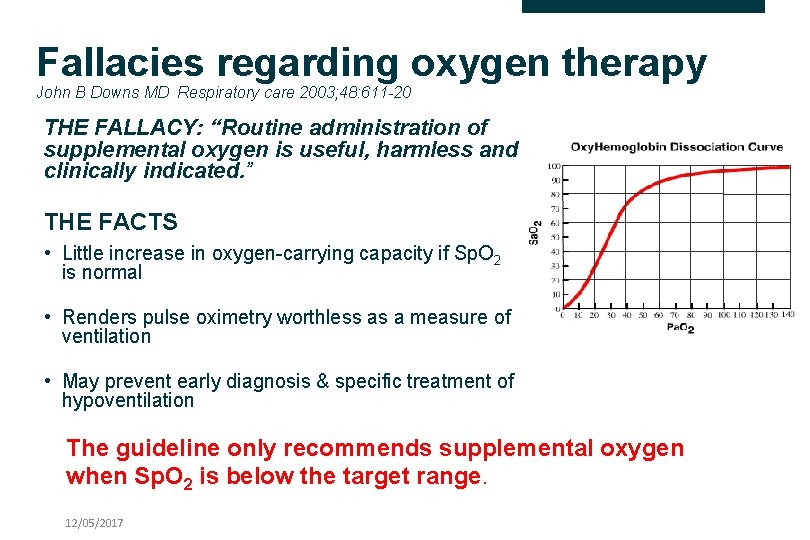
Fallacies regarding oxygen therapy John B Downs MD Respiratory care 2003; 48: 611 -20 THE FALLACY: “Routine administration of supplemental oxygen is useful, harmless and clinically indicated. ” THE FACTS • Little increase in oxygen-carrying capacity if Sp. O 2 is normal • Renders pulse oximetry worthless as a measure of ventilation • May prevent early diagnosis & specific treatment of hypoventilation The guideline only recommends supplemental oxygen when Sp. O 2 is below the target range. 12/05/2017

Oxygen therapy is only one element of resuscitation of a critically ill patient The oxygen carrying power of blood may be increased by • Safeguarding the airway • Enhancing circulating volume • Correcting severe anaemia • Enhancing cardiac output • Avoiding/Reversing Respiratory Depressants • Increasing Fraction of Inspired Oxygen (FIO 2) • Establish the reason for Hypoxia and treat the underlying cause (e. g Bronchospasm, LVF etc) • Patient may need, CPAP or NIV or Invasive ventilation 12/05/2017

Defining safe lower and upper limits of oxygen saturation 12/05/2017

What is the minimum arterial oxygen level recommended in acute illness? Target oxygen Saturation Critical care consensus guidelines Surviving sepsis campaign Minimum 90% Aim at 88 -95% But these patients have intensive levels of nursing & monitoring This guideline recommends a minimum of 94% for most patients – combines what is near normal and what is safe 12/05/2017

Exposure to high concentrations of oxygen may be harmful • • • Harten JM et al J Cardiothoracic Vasc Anaesth 2005; 19: 173 -5 • Kaneda T et al. Jpn Circ J 2001; 213 -8 • Frobert O et al. Cardiovasc Ultrasound 2004; 2: 22 • Haque WA et al. J Am Coll Cardiol 1996; 2: 353 -7 • Thomaon aj ET AL. BMJ 2002; 1406 -7 • Stub D et a; . Circulation 2015’; 131: 2143 -50 • Helmerhorst HJ Crit Care Med 2015; 43: 1508 -19 • Girardis M et al. JAMA 2016; 316: 1583 -89 Absorption Atelectasis even at FIO 2 30 -50% Intrapulmonary shunting Post-operative hypoxaemia Risk to COPD patients Coronary vasoconstriction Increased Systemic Vascular Resistance Reduced Cardiac Index Possible reperfusion injury post MI Increased CK level in STEMI and increased infarct size on MR scan at 3 months Worsens systolic myocardial performance Association of hyperoxaemia with increased mortality in several ITU studies • This guideline recommends an upper limit of 98% for most patients • Combination of what is normal and safe 12/05/2017

Some patients are at risk of CO 2 retention and acidosis if given high dose oxygen* • Chronic hypoxic lung disease • COPD • Severe Chronic Asthma • Bronchiectasis / CF • Chest wall disease • Kyphoscoliosis • Thoracoplasty • Neuromuscular disease • Morbid obesity and OHVS (Obesity Hypoventilation Syndrome) *Blood gases should be checked for all such patients if they need oxygen *Target saturation range is 88 -92% if CO 2 level is elevated (or if it was high in the past) 12/05/2017
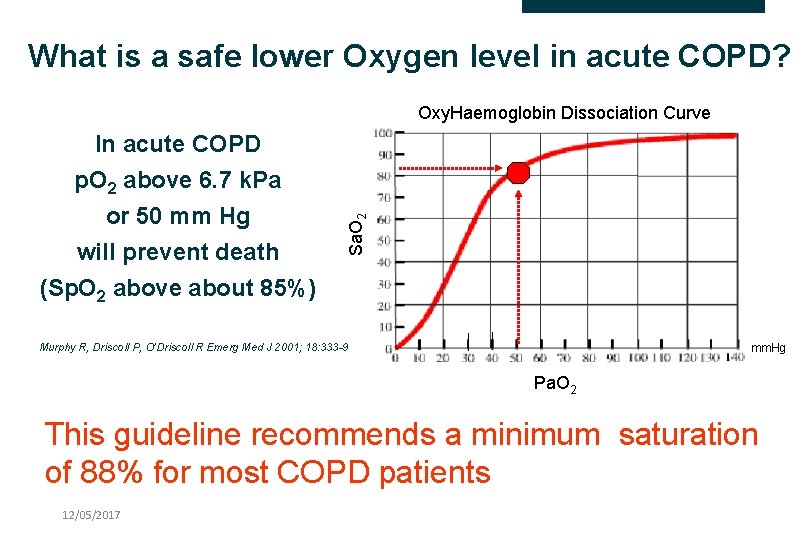
What is a safe lower Oxygen level in acute COPD? In acute COPD p. O 2 above 6. 7 k. Pa or 50 mm Hg will prevent death (Sp. O 2 above about 85%) Sa. O 2 Oxy. Haemoglobin Dissociation Curve Murphy R, Driscoll P, O’Driscoll R Emerg Med J 2001; 18: 333 -9 mm. Hg Pa. O 2 This guideline recommends a minimum saturation of 88% for most COPD patients 12/05/2017

What is a safe upper limit of oxygen target range in acute COPD patients who need oxygen therapy? • 47% of 982 patients with exacerbation of COPD were hypercapnic on arrival in hospital • 20% had Respiratory Acidosis (p. H < 7. 35) • 5% had p. H < 7. 25 (and were likely to need ICU care) • Most hypercapnic patients with p. O 2 > 10 k. Pa were acidotic (equivalent to oxygen saturation of above ~ 92%) i. e. they had been given too much oxygen Plant et al Thorax 2000; 55: 550 RECOMMENDED UPPER LIMITS Keep Pa. O 2 below 10 k. Pa and keep Sp. O 2 ≤ 92% in acute COPD pending blood gas results (Maintain target range 88 -92% if hypercapnic) 12/05/2017

High concentration oxygen may double the risk of death in acute exacerbations of COPD (AECOPD) • 405 patients with presumed AECOPD were randomised to high concentration oxygen or controlled oxygen (target range 88 -92%) • Mortality 9% on high concentration O 2 V 4% on controlled O 2 • Titrated oxygen treatment reduced mortality compared with high flow oxygen by 58% for all patients (relative risk 0. 42, 95% confidence interval 0. 20 to 0. 89; P=0. 02) • Less acidosis and less hypercapnia on controlled oxygen therapy Austin M et al BMJ 2010; 341: c 5642 12/05/2017

Danger of Rebound Hypoxaemia • If you find a patient who is severely hypercapnic due to excessive oxygen therapy…… • Do NOT stop oxygen therapy abruptly • The Pa. CO 2 is very high which will cause low PAO 2 as soon as oxygen is removed as demonstrated by the Alveolar Gas Equation (PAO 2 ≈ PIO 2 –Pa. CO 2/RER ) It is safest to step down to 35% oxygen if the patient is fully alert or call your Critical Care team to provide mechanical ventilation if the patient is drowsy 12/05/2017

Use of target ranges 12/05/2017

Target Saturation Scheme • O 2 prescribed by target saturation • Oxygen delivery device and flow are changed if necessary to keep the Sp. O 2 in the target range • Target oxygen saturation prescription integrated into patient drug chart and monitoring 12/05/2017

Recommended target saturations The target ranges are a consensus agreement by the guidelines group and the endorsing colleges and societies Rationale for the target saturations is combination of what is normal or near-normal and what is safe Most patients 94 - 98% Risk of hypercapnic respiratory failure 88 – 92%* *Or patient specific saturation on Alert Card 12/05/2017

Safeguarding patients at risk of type 2 respiratory failure • Lower target saturation range for these patients (88 -92%) • Education of patients and health care workers • Use of controlled oxygen via Venturi masks or low flow nasal O 2 • Use of oxygen alert cards • Issue of personal Venturi masks to high-risk patients 12/05/2017

OXYGEN ALERT CARD Name: _________________________ I have a chronic respiratory condition and I am at risk of having a raised carbon dioxide level in my blood during flare-ups of my condition (exacerbations) Please use my ______% Venturi mask to achieve an oxygen saturation of _____ % to _____ % during exacerbations of my condition Use compressed air to drive nebulisers (with nasal oxygen a 2 l/min) If compressed air is not available, limit oxygen-driven nebulisers to 6 minutes 12/05/2017
Oxygen Alert Cards and 24% masks can avoid hypercapnic respiratory failure associated with high flow oxygen masks • Oxygen alert card (and a 24% Venturi mask) given to patients admitted with hypercapnic acidosis with a PO 2 > 10 k. Pa • Patients instructed to show these to ambulance and A&E staff After introduction of alert cards • Use of 24% oxygen: 63% in Ambulance 94% in Emergency Department Gooptu B, Ward L, Davison A et al. Oxygen alert cards and controlled oxygen masks: Emerg Med J 2006; 23: 636 -8 12/05/2017

Prescribing Oxygen 12/05/2017
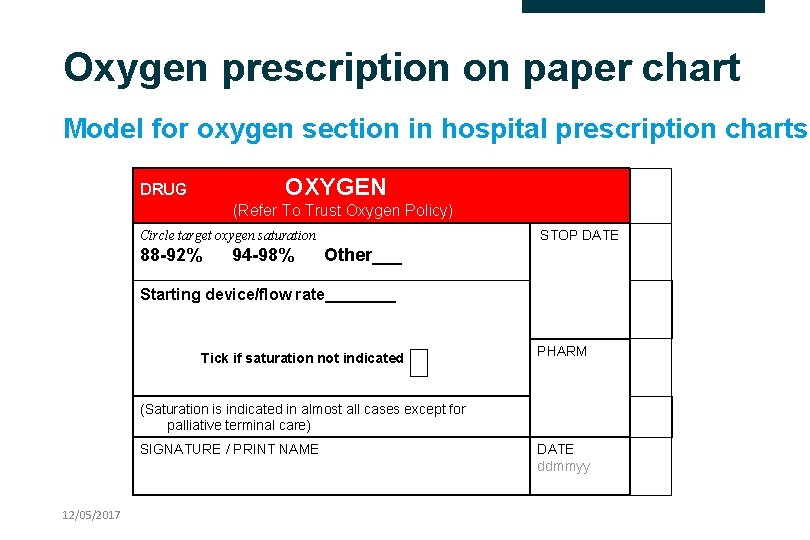

Oxygen prescription on paper chart Model for oxygen section in hospital prescription charts OXYGEN DRUG (Refer To Trust Oxygen Policy) STOP DATE Circle target oxygen saturation 88 -92% 94 -98% Other___ Starting device/flow rate____ Tick if saturation not indicated PHARM (Saturation is indicated in almost all cases except for palliative terminal care) SIGNATURE / PRINT NAME 12/05/2017 DATE ddmmyy
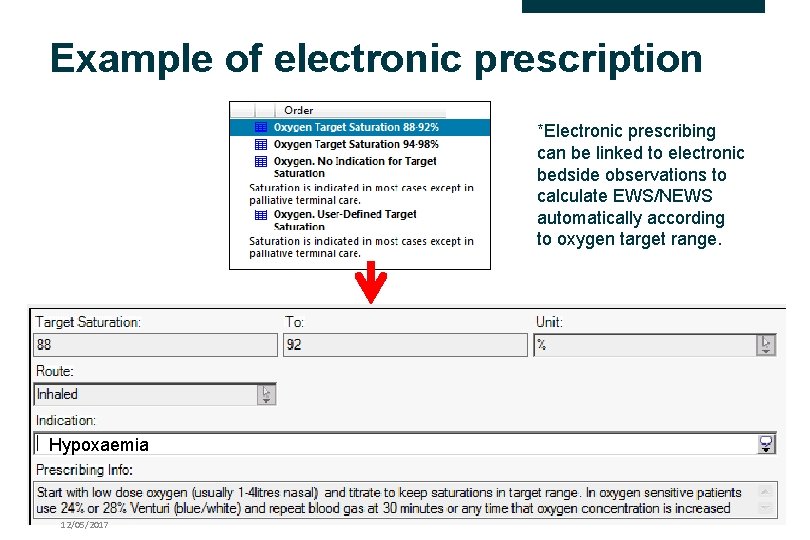

Example of electronic prescription *Electronic prescribing can be linked to electronic bedside observations to calculate EWS/NEWS automatically according to oxygen target range. Hypoxaemia 12/05/2017

Oxygen prescription and Administration • Clinician (usually a doctor) prescribes oxygen by circling the desired oxygen saturation target range (or by selecting a range in electronic prescribing) • Nurses and PAMs* use appropriate devices and flow rates to maintain saturation within the target range *PAMs = Professions allied to medicine 12/05/2017

Oxygen use in palliative care • Most breathlessness in cancer patients is caused by specific issues such as airflow obstruction, infections or pleural effusions and the main issue is to treat the cause • Oxygen has been shown to relieve dyspnoea in hypoxaemic cancer patients but not if Pa. O 2 is >7. 3 k. Pa (saturation above about 90%) • Morphine and Midazolam also relieve breathlessness and are probably more effective 12/05/2017

Devices 12/05/2017
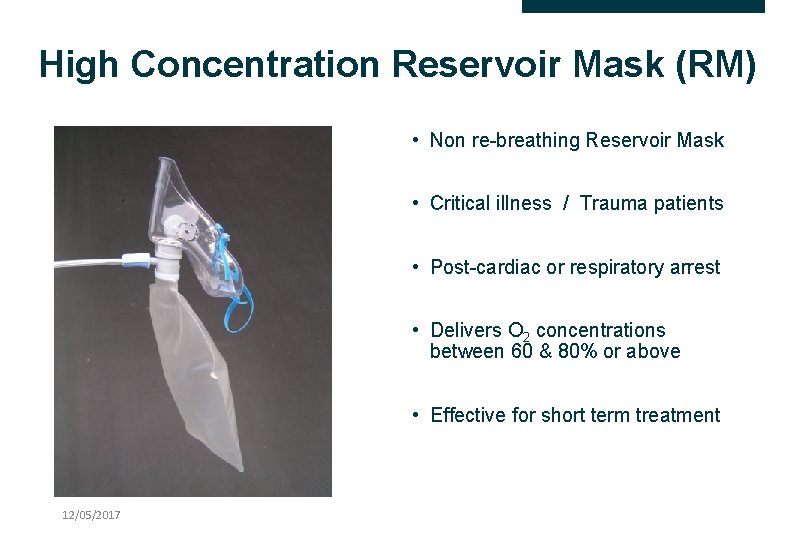
High Concentration Reservoir Mask (RM) • Non re-breathing Reservoir Mask • Critical illness / Trauma patients • Post-cardiac or respiratory arrest • Delivers O 2 concentrations between 60 & 80% or above • Effective for short term treatment 12/05/2017

Nasal Cannulae (N) • Recommended in the Guideline as suitable for most patients with both type I and II respiratory failure. • 1 -6 L/min gives approx 24 -50% FIO 2 • FIO 2 depends on oxygen flow rate and patient’s minute volume and inspiratory flow and pattern of breathing. • Comfortable and easily tolerated • No re-breathing • Low cost product • Preferred by patients (vs simple mask) 12/05/2017

Venturi or Fixed Performance Masks (V) • Aim to deliver constant oxygen concentration within and between breaths. • 24 -40% Venturi Masks operate accurately A 60% Venturi mask gives ~50% FIO 2 • With TACHYPNOEA (RR >30/min) the oxygen flow rate should be increased by above the minimum flow rate shown on the packaging - see next slide • Increasing flow does not increase oxygen concentration because it is a fixed dose device 12/05/2017
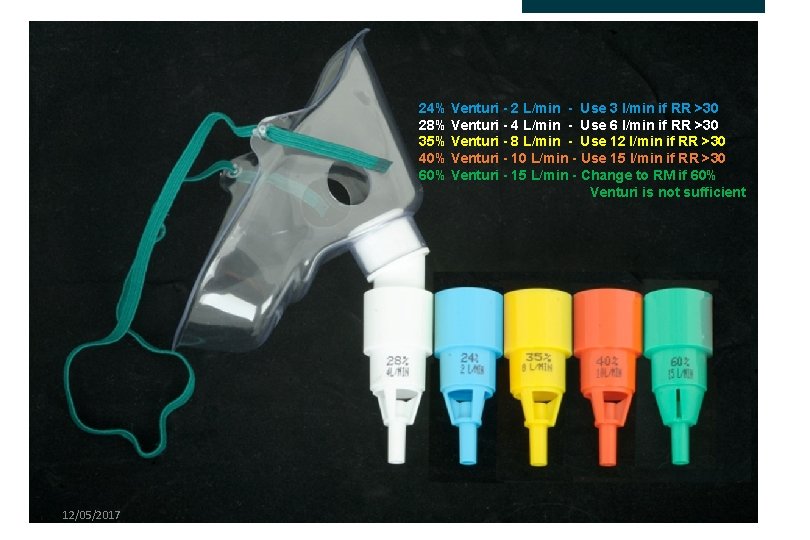
24% Venturi - 2 L/min - Use 3 l/min if RR >30 28% Venturi - 4 L/min - Use 6 l/min if RR >30 35% Venturi - 8 L/min - Use 12 l/min if RR >30 40% Venturi - 10 L/min - Use 15 l/min if RR >30 60% Venturi - 15 L/min - Change to RM if 60% Venturi is not sufficient 12/05/2017
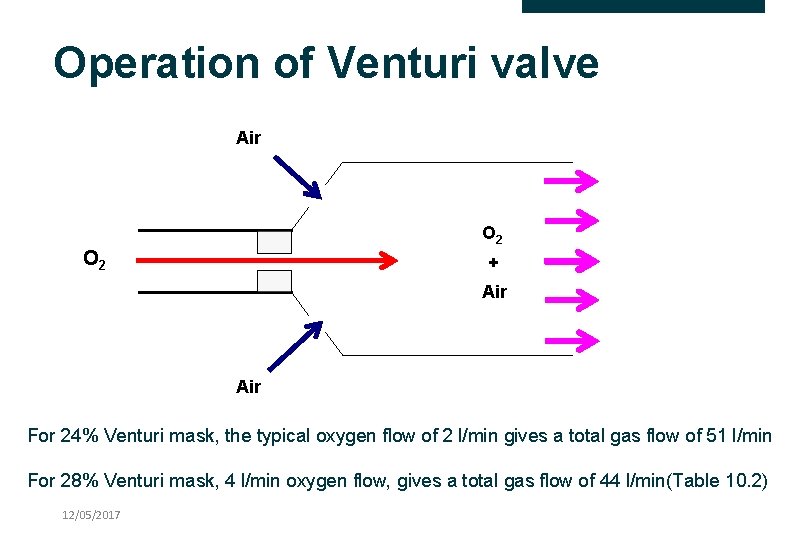
Operation of Venturi valve Air O 2 + Air For 24% Venturi mask, the typical oxygen flow of 2 l/min gives a total gas flow of 51 l/min For 28% Venturi mask, 4 l/min oxygen flow, gives a total gas flow of 44 l/min(Table 10. 2) 12/05/2017
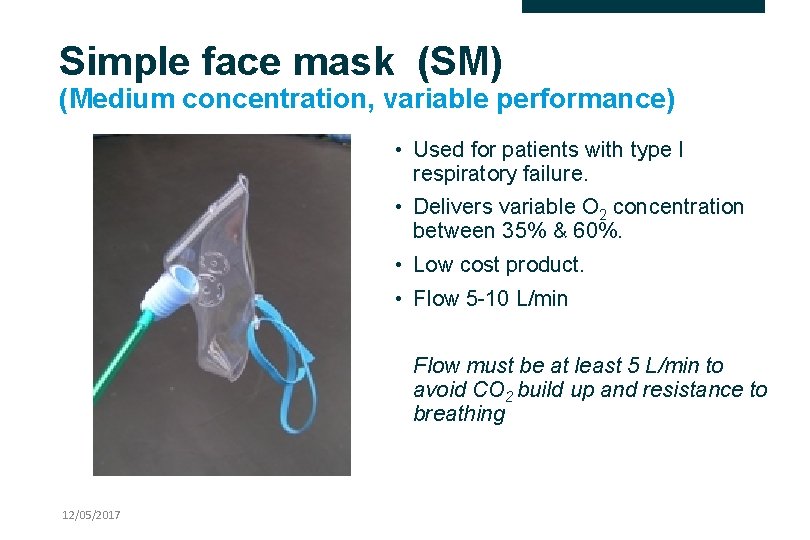
Simple face mask (SM) (Medium concentration, variable performance) • Used for patients with type I respiratory failure. • Delivers variable O 2 concentration between 35% & 60%. • Low cost product. • Flow 5 -10 L/min Flow must be at least 5 L/min to avoid CO 2 build up and resistance to breathing 12/05/2017

Humidified Oxygen (H) • • Tracheostomy Bronchiectasis Cystic Fibrosis patients Physiotherapists may advise humidification • Patients on High flow whisper CPAP • Humidification may be provided by cold or warm humidifiers • ( H 24, H 28, H 35 etc ) The illustration shows a cold humidifier delivering 28% oxygen at 5 l/min flow N. B. There is little evidence for humidification in routine oxygen therapy 12/05/2017
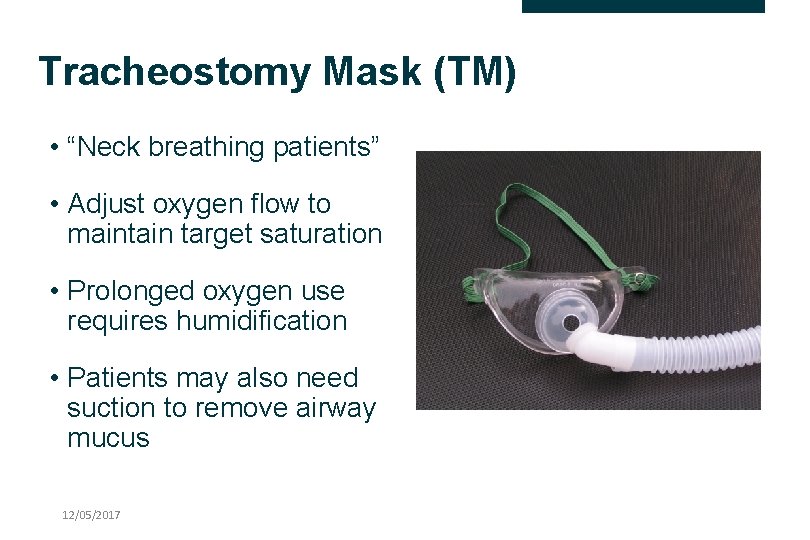
Tracheostomy Mask (TM) • “Neck breathing patients” • Adjust oxygen flow to maintain target saturation • Prolonged oxygen use requires humidification • Patients may also need suction to remove airway mucus 12/05/2017

High flow humidified nasal oxygen (HFN) • High flow nasal oxygen using specialised equipment may be used as an alternative to reservoir mask treatment in patients with acute respiratory failure without hypercapnia • It is mostly used in Intensive Care Units, High Dependency Units and other specialised areas 12/05/2017

Oxygen Flow Meter The centre of the ball indicates the correct flow rate. This diagram illustrates the correct setting of the flow meter to deliver a flow of 2 litres per minute 12/05/2017

Beware of air outlets They may be mistaken for oxygen outlets Oxygen outlet (Usually white) 12/05/2017 Air outlet (usually black) Use a cover for air outlets or else remove the flow meter for air when not in use

What device and flow rate should you use in each situation? 12/05/2017

Many patients need high-dose oxygen to normalize saturation • Severe Pneumonia • Severe LVF • Major Trauma • Sepsis and Shock • Major atelectasis • Pulmonary Embolism • Lung Fibrosis • Etc etc 12/05/2017

Oxygen use in specific illnesses 4 Major groups of patients See Tables 1 -4 and Charts 1 -2 in BTS Emergency Oxygen Guideline • Critical illness requiring high levels of supplemental oxygen • Serious illness requiring moderate levels of supplemental oxygen if a patient is hypoxaemic • COPD and other conditions requiring controlled or low-dose oxygen therapy • Conditions for which patients should be monitored closely but oxygen therapy is not required unless the patient is hypoxaemic (This group includes most cases of chest pain, heart attacks, stroke etc) 12/05/2017

Chart 1 Oxygen prescription for acutely hypoxaemic patients in hospital • Is the patient critically ill (see Table 1 and section 8. 10 in Guideline) Yes Commence treatment with reservoir mask or bag-valve mask and manage as advised in Table 1 No Is this patient at risk of hypercapnic respiratory failure (Type 2 Respiratory Failure)? YES NO Target saturation is 88 -92% whilst awaiting blood gas results Aim for Sp. O 2 94 -98% Specific instructions are given for each category of patient depending on blood gas results etc 12/05/2017
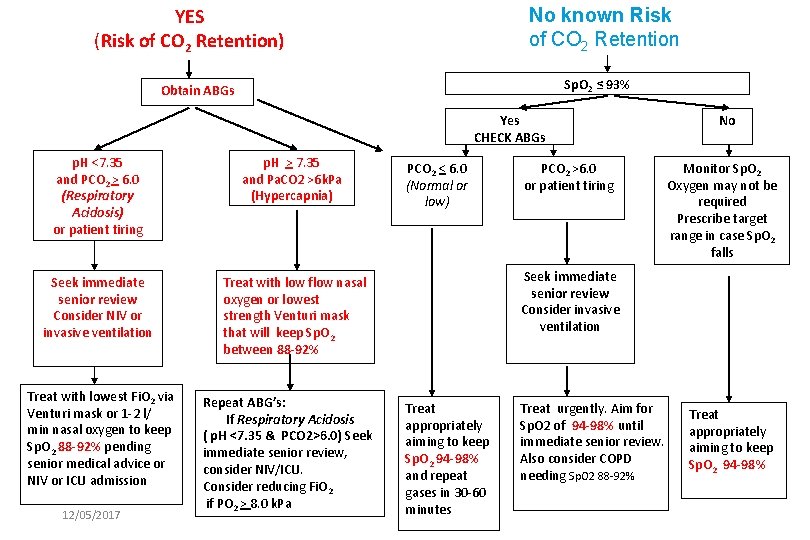
YES (Risk of CO 2 Retention) No known Risk of CO 2 Retention Sp. O 2 ≤ 93% Obtain ABGs Yes CHECK ABGs p. H <7. 35 and PCO 2 > 6. 0 (Respiratory Acidosis) or patient tiring p. H > 7. 35 and Pa. CO 2 >6 k. Pa (Hypercapnia) Seek immediate senior review Consider NIV or invasive ventilation Treat with low flow nasal oxygen or lowest strength Venturi mask that will keep Sp. O 2 between 88 -92% Treat with lowest Fi. O 2 via Venturi mask or 1 -2 l/ min nasal oxygen to keep Sp. O 2 88 -92% pending senior medical advice or NIV or ICU admission 12/05/2017 Repeat ABG’s: If Respiratory Acidosis ( p. H <7. 35 & PCO 2>6. 0) Seek immediate senior review, consider NIV/ICU. Consider reducing Fi. O 2 if PO 2 > 8. 0 k. Pa PCO 2 < 6. 0 (Normal or low) PCO 2 >6. 0 or patient tiring No Monitor Sp. O 2 Oxygen may not be required Prescribe target range in case Sp. O 2 falls Seek immediate senior review Consider invasive ventilation Treat appropriately aiming to keep Sp. O 2 94 -98% and repeat gases in 30 -60 minutes Treat urgently. Aim for Sp. O 2 of 94 -98% until immediate senior review. Also consider COPD needing Sp. O 2 88 -92% Treat appropriately aiming to keep Sp. O 2 94 -98%
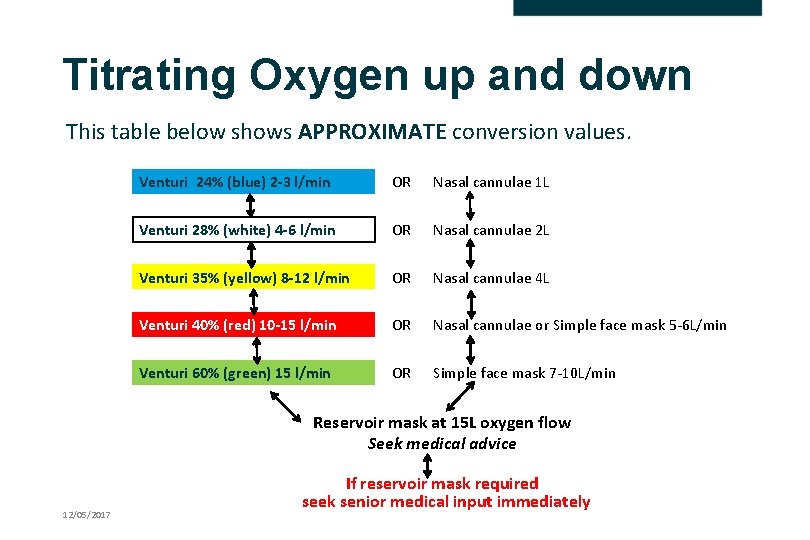
Titrating Oxygen up and down This table below shows APPROXIMATE conversion values. Venturi 24% (blue) 2 -3 l/min OR Nasal cannulae 1 L Venturi 28% (white) 4 -6 l/min OR Nasal cannulae 2 L Venturi 35% (yellow) 8 -12 l/min OR Nasal cannulae 4 L Venturi 40% (red) 10 -15 l/min OR Nasal cannulae or Simple face mask 5 -6 L/min Venturi 60% (green) 15 l/min OR Simple face mask 7 -10 L/min Reservoir mask at 15 L oxygen flow Seek medical advice 12/05/2017 If reservoir mask required seek senior medical input immediately
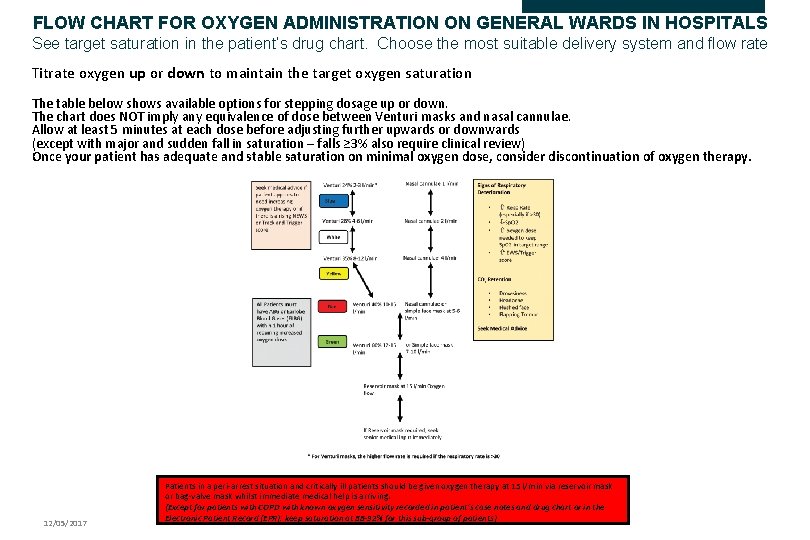
FLOW CHART FOR OXYGEN ADMINISTRATION ON GENERAL WARDS IN HOSPITALS See target saturation in the patient’s drug chart. Choose the most suitable delivery system and flow rate Titrate oxygen up or down to maintain the target oxygen saturation The table below shows available options for stepping dosage up or down. The chart does NOT imply any equivalence of dose between Venturi masks and nasal cannulae. Allow at least 5 minutes at each dose before adjusting further upwards or downwards (except with major and sudden fall in saturation – falls ≥ 3% also require clinical review) Once your patient has adequate and stable saturation on minimal oxygen dose, consider discontinuation of oxygen therapy. 12/05/2017 Patients in a peri-arrest situation and critically ill patients should be given oxygen therapy at 15 l/min via reservoir mask or bag-valve mask whilst immediate medical help is arriving. (Except for patients with COPD with known oxygen sensitivity recorded in patient’s case notes and drug chart or in the Electronic Patient Record (EPR): keep saturation at 88 -92% for this sub-group of patients)

Monitoring patients • Oxygen saturation and delivery system should be recorded on the bedside monitoring chart or EPR • Delivery devices and/or flow rates should be adjusted to keep oxygen saturation in target range 12/05/2017
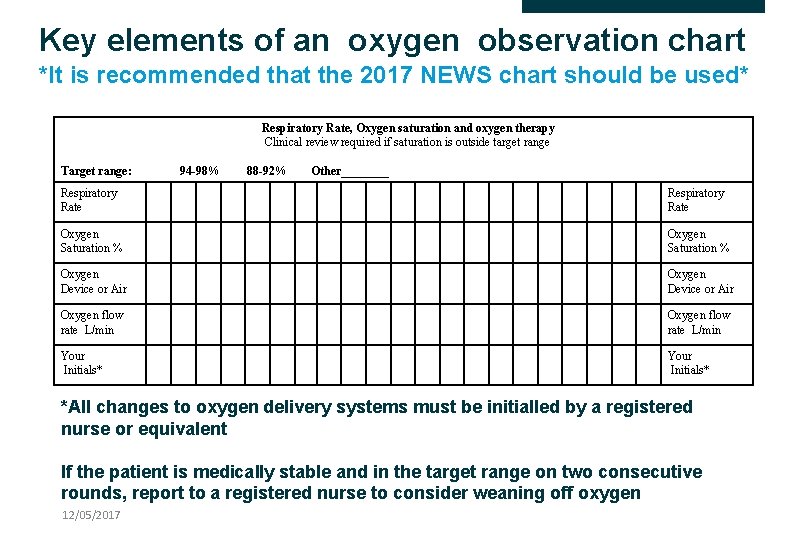

Key elements of an oxygen observation chart *It is recommended that the 2017 NEWS chart should be used* Respiratory Rate, Oxygen saturation and oxygen therapy Clinical review required if saturation is outside target range Target range: 94 -98% 88 -92% Other____ Respiratory Rate Oxygen Saturation % Oxygen Device or Air Oxygen flow rate L/min Your Initials* *All changes to oxygen delivery systems must be initialled by a registered nurse or equivalent If the patient is medically stable and in the target range on two consecutive rounds, report to a registered nurse to consider weaning off oxygen 12/05/2017

Example of 2017 NEWS chart when available 12/05/2017
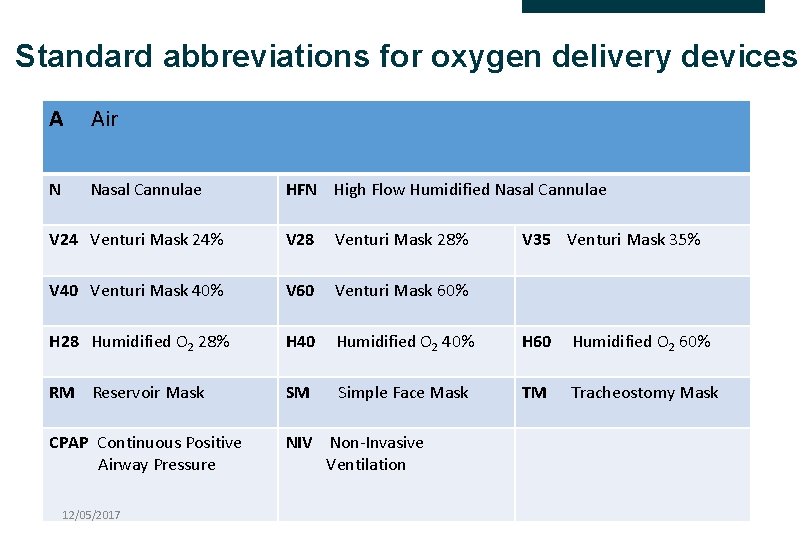
Standard abbreviations for oxygen delivery devices A Air N Nasal Cannulae HFN High Flow Humidified Nasal Cannulae V 24 Venturi Mask 24% V 28 Venturi Mask 28% V 40 Venturi Mask 40% V 60 Venturi Mask 60% H 28 Humidified O 2 28% H 40 Humidified O 2 40% H 60 Humidified O 2 60% RM Reservoir Mask SM Simple Face Mask TM Tracheostomy Mask CPAP Continuous Positive Airway Pressure NIV Non-Invasive Ventilation 12/05/2017 V 35 Venturi Mask 35%

From the BTS Emergency Oxygen Guideline To the patient • Guideline agreed by the whole UK medical, nursing and AHP community (endorsed by 23 Colleges and Societies) • Medical and Nurse/Physio Champions in every Hospital Trust • Clear prescription charts and monitoring charts in every hospital • Training packages on BTS website • Audit tools on BTS website: audits. brit-thoracic. org. uk 12/05/2017
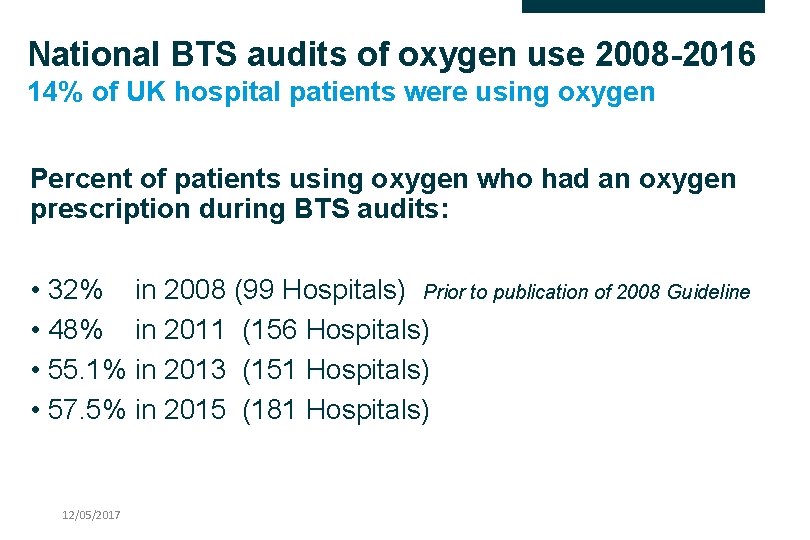

National BTS audits of oxygen use 2008 -2016 14% of UK hospital patients were using oxygen Percent of patients using oxygen who had an oxygen prescription during BTS audits: • 32% in 2008 (99 Hospitals) Prior to publication of 2008 Guideline • 48% in 2011 (156 Hospitals) • 55. 1% in 2013 (151 Hospitals) • 57. 5% in 2015 (181 Hospitals) 12/05/2017
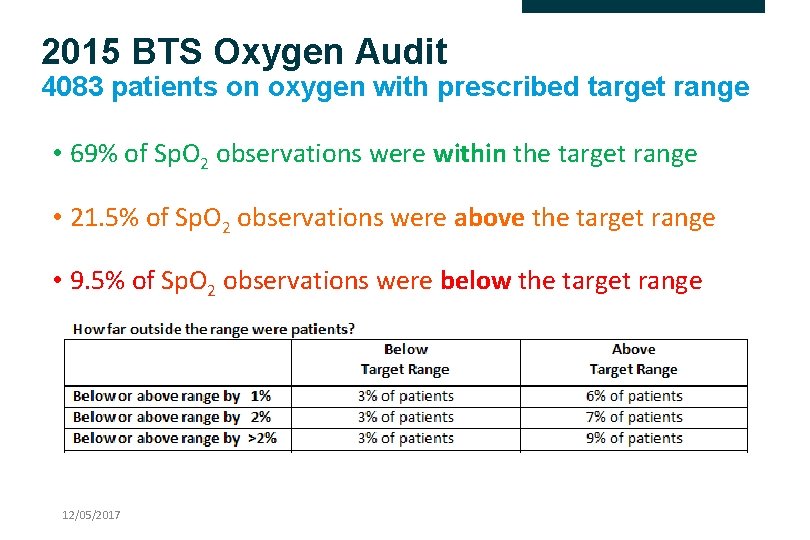

2015 BTS Oxygen Audit 4083 patients on oxygen with prescribed target range • 69% of Sp. O 2 observations were within the target range • 21. 5% of Sp. O 2 observations were above the target range • 9. 5% of Sp. O 2 observations were below the target range 12/05/2017

Summary 1. Prescribe oxygen to a target saturation for each group of patients • 94 - 98% for most adult patients • 88 - 92% if risk of hypercapnia (or patient-specific target on alert card) 1. Administer oxygen to achieve target saturation 2. Monitor oxygen saturation and keep in target range 3. Taper oxygen dose and stop when stable 4. Audit your practice 5. All information on www. brit-thoracic. org. uk 12/05/2017

These slides are provided for use on a local basis – permission is not request to use these and additional material may be added depending on local circumstances. The BTS Guidelines for oxygen use in adults in healthcare and emergency settings should be acknowledged and referenced as follows: O’Driscoll BR et al Thorax 2017; 72: Suppl 1 i 1 -i 89 Healthcare providers need to use clinical judgement, knowledge and expertise when deciding whether it is appropriate to apply recommendations for the management of patients. The recommendations cited here a guide and may not be appropriate for use in all situations. The guidance provided does not override the responsibility of healthcare professionals to make decisions appropriate to the circumstances of each patient, in consultation with the patient and/or their guardian or carer.
- Slides: 64