Brief History of Major Advancements in Cardiac Pacing

Brief History of Major Advancements in Cardiac Pacing Mark D. Carlson, MD, MA

2

3

Pacing System Component pulse generator • • Casing (can) • Titanium (biocompatible, lightweight, stronger than steel) Connector (header) • Leads plug into ports in the clear epoxy header Components • Diodes, resistors, oscillator, microchips Battery • The largest single component inside the pulse generator • Lithium iodide 2. Leads 3. Programmer/Remote monitor

Path to Medical Device Innovation and Improved Patient Care § Problem/Opportunity § Population § Therapy (Current and Innovative) § Outcomes 5

Path to Medical Device Innovation and Improved Patient Care § Problem/Opportunity § Etiology and Mechanism § Therapy (Current or Innovative) § Mechanism of action § Population § Risk § Prevalence § Incidence § Outcomes (Clinical/Regulatory/Health Economic) § Measurements § Surrogates § Short/Long Term 6

Problem: Sudden Cardiac Death (1960 s and Now) § SCD: the most common cause of death in the U. S. § Incidence: 300, 000 to 400, 000 each year (U. S. ) § Only 2% – 15% reach the hospital § Half of these early survivors die before discharge

Therapy: SCD prevention the 1960 s, 70 s, and 80 s § Frequent PVCs post MI associated with increased mortality (SCD) § Assumptions: § PVCs trigger life-threatening sustained ventricular arrhythmias § Suppression of PVCs with AAD improves survival § SCD is increased in post-MI patients with low EF § Assumptions: § Induction of sustained VT during EP study identifies patientss at increased risk § Suppression of inducibility by AADs improves survival 8
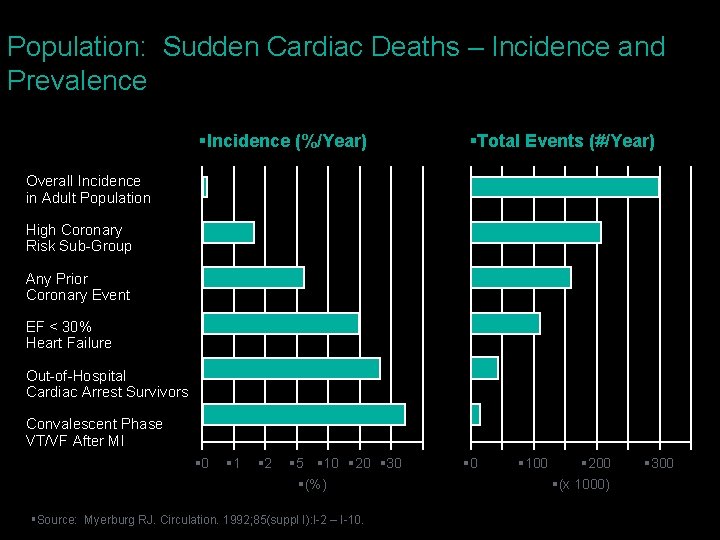
Population: Sudden Cardiac Deaths – Incidence and Prevalence §Incidence (%/Year) §Total Events (#/Year) Overall Incidence in Adult Population High Coronary Risk Sub-Group Any Prior Coronary Event EF < 30% Heart Failure Out-of-Hospital Cardiac Arrest Survivors Convalescent Phase VT/VF After MI § 0 § 1 § 2 § 5 § 10 § 20 § 30 §(%) §Source: Myerburg RJ. Circulation. 1992; 85(suppl I): I-2 – I-10. § 0 § 100 § 200 §(x 1000) § 300

Innovative Therapy: Automatic Implantable Defibrillator) 10

Timeline § 1966, Dr. Harry Heller died of SCD in Israel § 1969, Michel Mirowski and Morton Mower performed the first canine transvenous defibrillation at Sinai Hospital, Baltimore § 1975, First canine implants § February 4, 1980, First human implant at Johns Hopkins
Early AIDs § 1980 -1985 clinical trial of first ICDs § 1985 FDA approved first ICD for human use § First pulse generators were 140 cc (similar to a pack of cigarettes) § Abdominal implant § Thoracotomy patch lead implant § Considered tx of last resort § Patients had failed drugs and survived two episodes of SCD
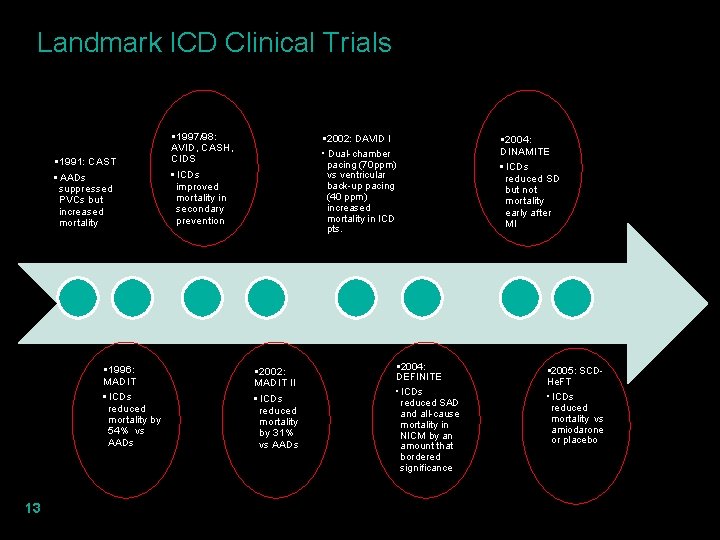
Landmark ICD Clinical Trials § 1991: CAST • AADs suppressed PVCs but increased mortality § 1996: MADIT • ICDs reduced mortality by 54% vs AADs 13 § 1997/98: AVID, CASH, CIDS • ICDs improved mortality in secondary prevention § 2002: DAVID I • Dual-chamber pacing (70 ppm) vs ventricular back-up pacing (40 ppm) increased mortality in ICD pts. § 2002: MADIT II • ICDs reduced mortality by 31% vs AADs § 2004: DEFINITE • ICDs reduced SAD and all-cause mortality in NICM by an amount that bordered significance § 2004: DINAMITE • ICDs reduced SD but not mortality early after MI § 2005: SCDHe. FT • ICDs reduced mortality vs amiodarone or placebo
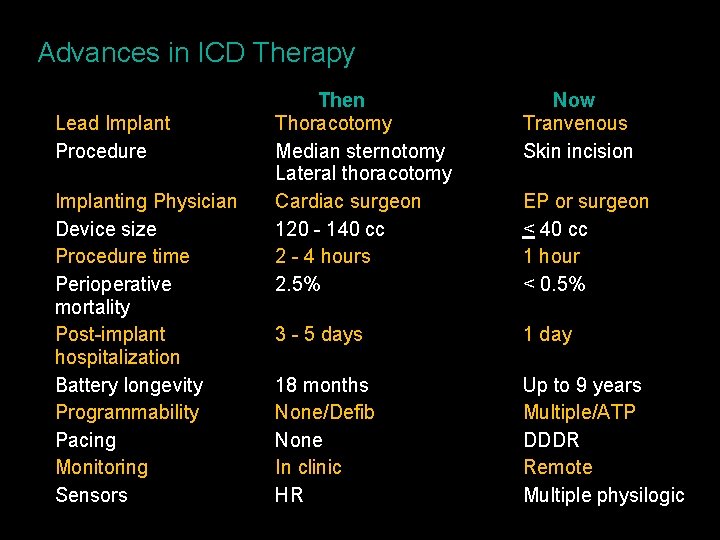
Advances in ICD Therapy Lead Implant Procedure Implanting Physician Device size Procedure time Perioperative mortality Post-implant hospitalization Battery longevity Programmability Pacing Monitoring Sensors Then Thoracotomy Median sternotomy Lateral thoracotomy Cardiac surgeon 120 - 140 cc 2 - 4 hours 2. 5% Now Tranvenous Skin incision 3 - 5 days 1 day 18 months None/Defib None In clinic HR Up to 9 years Multiple/ATP DDDR Remote Multiple physilogic EP or surgeon < 40 cc 1 hour < 0. 5%

Advances in ICD Therapy Then Now Rhythm discrimination none Tx Programmability Pacing Stored Electrograms None/Defib None Monitoring Sensors In clinic HR MRI compatability unproven QRS morphology Onset Rate Stability Multiple/ATP DDDR Atrial and Ventricular At high rates and with therapy Remote Activity Posture Intrathoracic impedance Intracardiac ST segment Intravascular pressure Validated through clinical studies

DAVID § Dual chamber atrial based pacing could be beneficial by allowing for § Optimal medical management § Increased heart rate and cardiac output § Reduced incidence of AF § Hypothesis: Dual chamber pacing (70 bpm) decreases mortality and HF hospitalization for heart failure compared to ventricular backup pacing (40 bpm). 16
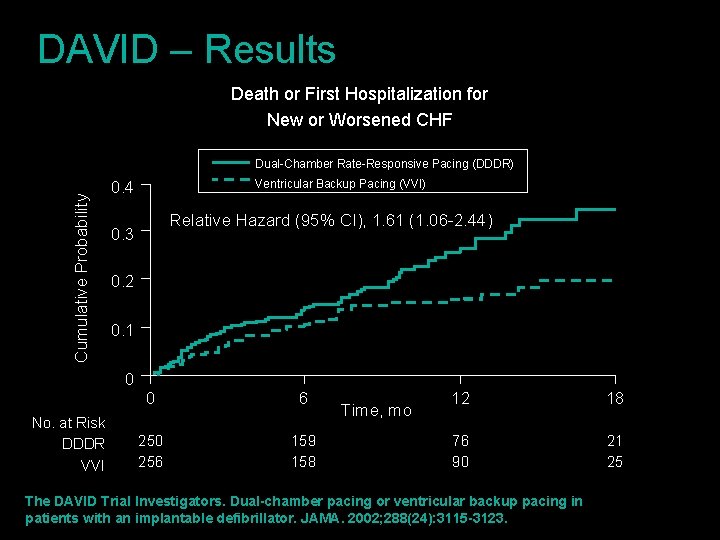
DAVID – Results Death or First Hospitalization for New or Worsened CHF Cumulative Probability Dual-Chamber Rate-Responsive Pacing (DDDR) 0. 4 Ventricular Backup Pacing (VVI) Relative Hazard (95% CI), 1. 61 (1. 06 -2. 44) 0. 3 0. 2 0. 1 0 No. at Risk DDDR VVI 0 6 250 256 159 158 Time, mo 12 18 76 90 21 25 The DAVID Trial Investigators. Dual-chamber pacing or ventricular backup pacing in patients with an implantable defibrillator. JAMA. 2002; 288(24): 3115 -3123.

SCD-He. FT Hypothesis § Determine if amiodarone or ICD* will decrease the risk of death from any cause in patients with mild-tomoderate heart failure Bardy GH. N Engl J Med. 2005; 352: 225 -237.
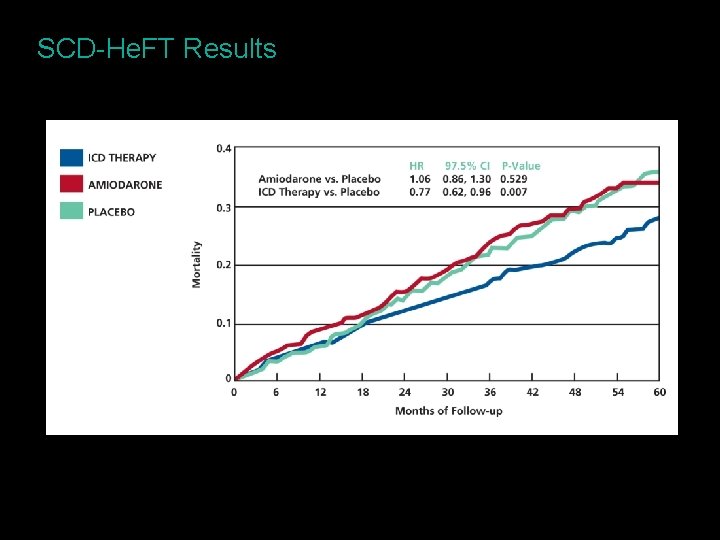
SCD-He. FT Results

HF Prevalence U. S. § § 5. 8 M heart failure patients in 2006 in the US 1 Prevalence: 2. 6%1 670, 000 people are newly diagnosed each year. 1 30% will die in the first year (US and EU)3 -5 § 60% will die within 5 years (US)5 § 1. 1 M HF hospitalizations annually; readmission rate is 25% and 50% at 30 days and 6 months § Annual Medicare costs of ~$37 B for hospitalizations with ~$17. 4 B of costs for readmissions within 30 days Europe § 15 M heart failure patients in the ESC 51 member countries 2 § Overall 2 -3% prevalence 2 1. 2. 3. 4. 5. AHA 2010 Statistics at a Glance, 2010 The European Society of Cardiology, ESC HF Guideline, 2008 Curtis et al, Arch Intern Med, 2008. Roger et al. JAMA, 2004. Cowie et al, EHJ, 2002.
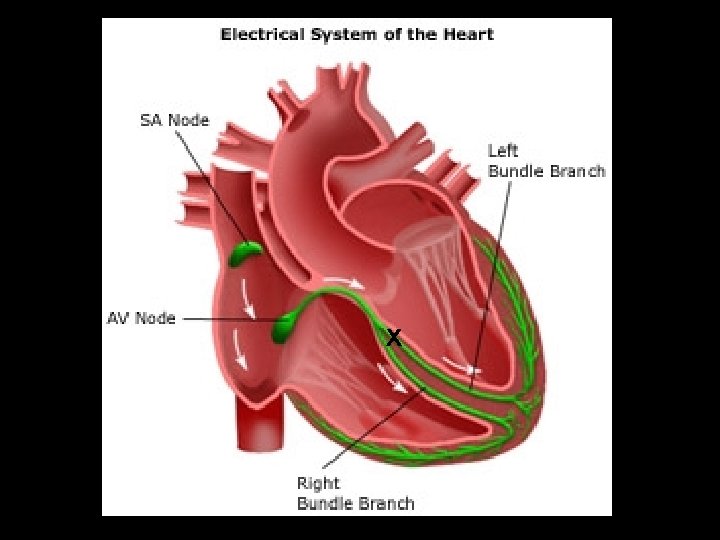
x
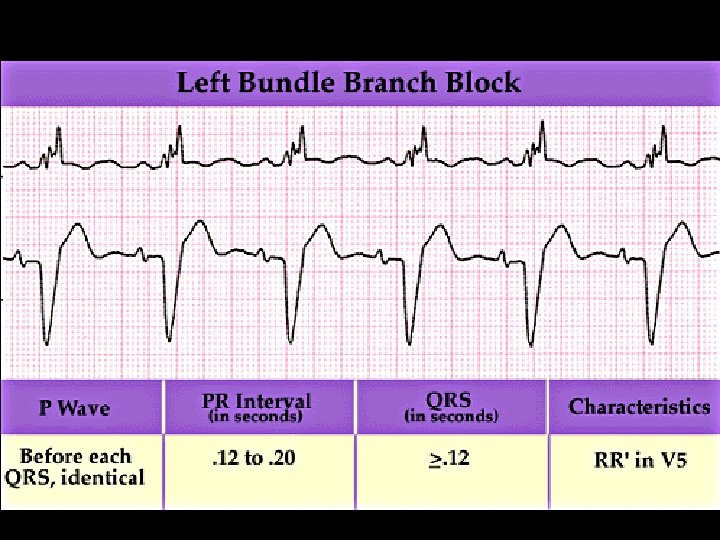
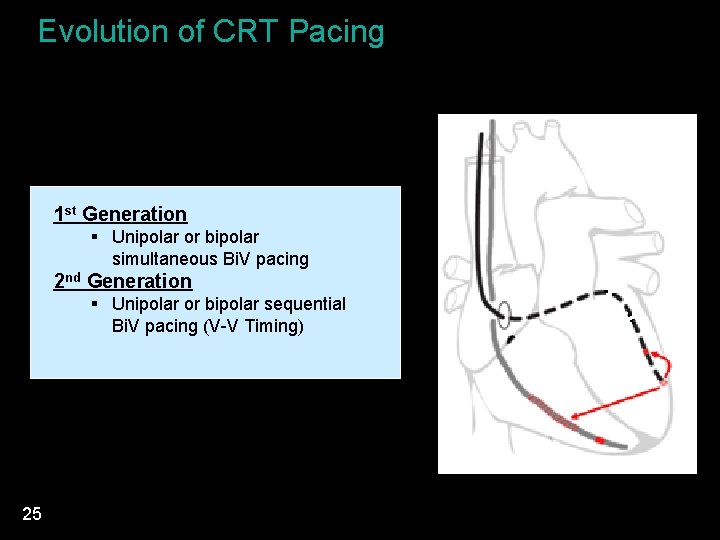
Evolution of CRT Pacing 1 st Generation § Unipolar or bipolar simultaneous Bi. V pacing 2 nd Generation § Unipolar or bipolar sequential Bi. V pacing (V-V Timing) 25
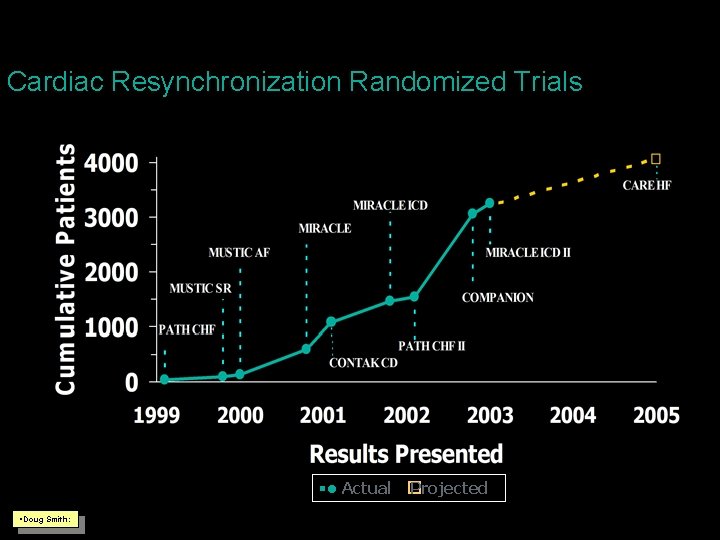
Cardiac Resynchronization Randomized Trials § • Actual � Projected §Doug Smith:
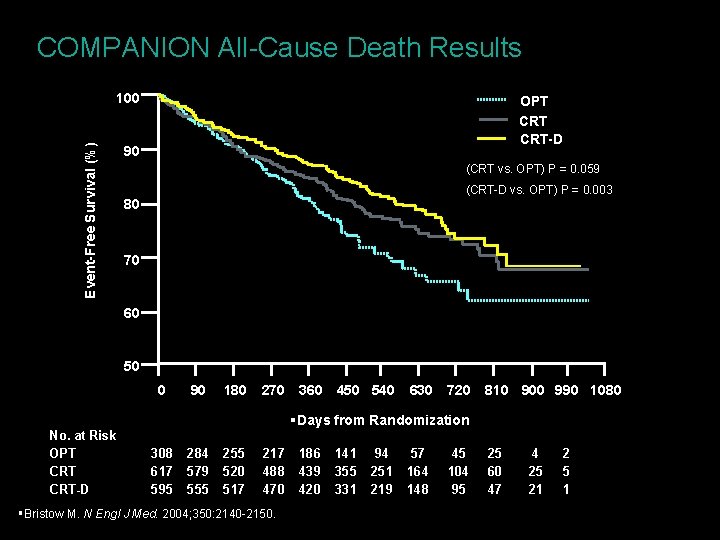
COMPANION All-Cause Death Results Event-Free Survival (%) 100 OPT CRT-D 90 (CRT vs. OPT) P = 0. 059 (CRT-D vs. OPT) P = 0. 003 80 70 60 50 0 No. at Risk OPT CRT-D 90 180 270 360 450 540 630 720 810 900 990 1080 §Days from Randomization 308 617 595 284 579 555 255 520 517 217 488 470 §Bristow M. N Engl J Med. 2004; 350: 2140 -2150. 186 439 420 141 355 331 94 251 219 57 164 148 45 104 95 25 60 47 4 25 21 2 5 1

CRT Challenges § CRT pacing complications at implant and follow-up § Phrenic nerve stimulation 1 § High pacing thresholds 2 § Lead dislodgement 3 § Surgical lead revision increases risks 5 -7 § Tradeoff: Lead stability vs optimal pacing location 4 § Efficacy 1. 2. 3. 4. 5. 6. 28 7. Biffi M, et al. CICEP, 2009. Gurevitz O, et al. PACE, 2005. Leon AR, et al. J Am Coll Cardiol, 2005. Duray, et al. J of Cardio Electro, 2008. Klug et al. Circulation, 2007. Poole JE, et al. Circulation, 2010. Romeyer-Bouchard et al. EHJ, 2010.
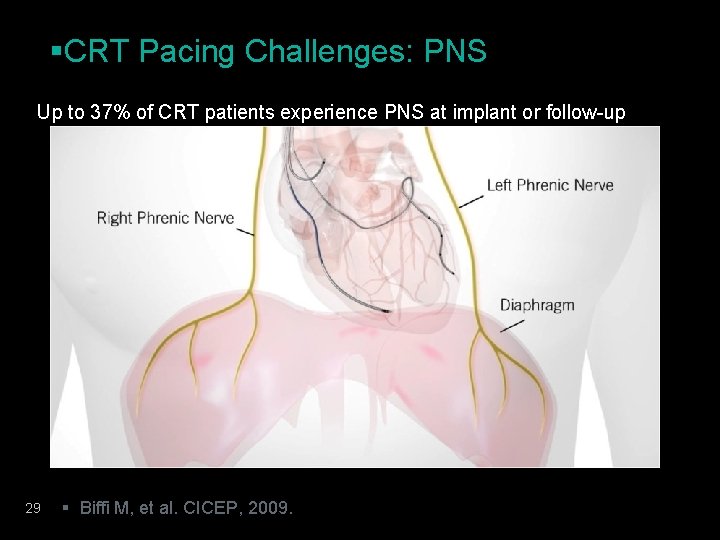
§CRT Pacing Challenges: PNS Up to 37% of CRT patients experience PNS at implant or follow-up 29 § Biffi M, et al. CICEP, 2009.
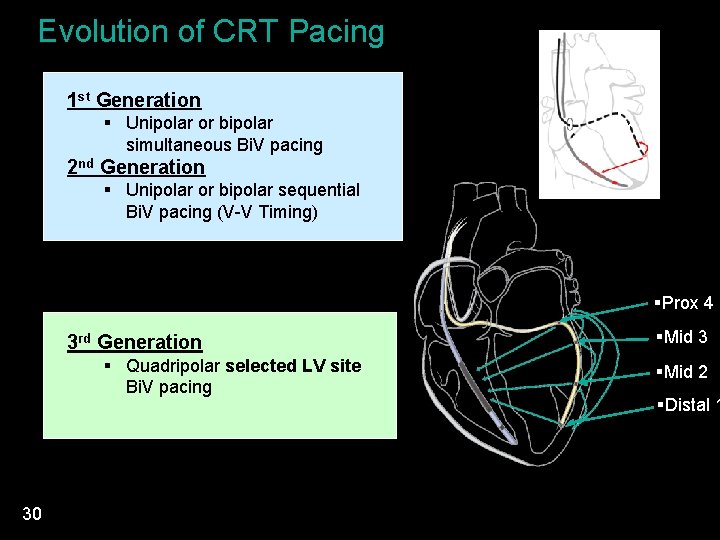
Evolution of CRT Pacing 1 st Generation § Unipolar or bipolar simultaneous Bi. V pacing 2 nd Generation § Unipolar or bipolar sequential Bi. V pacing (V-V Timing) §Prox 4 3 rd Generation § Quadripolar selected LV site Bi. V pacing 30 §Mid 3 §Mid 2 §Distal 1
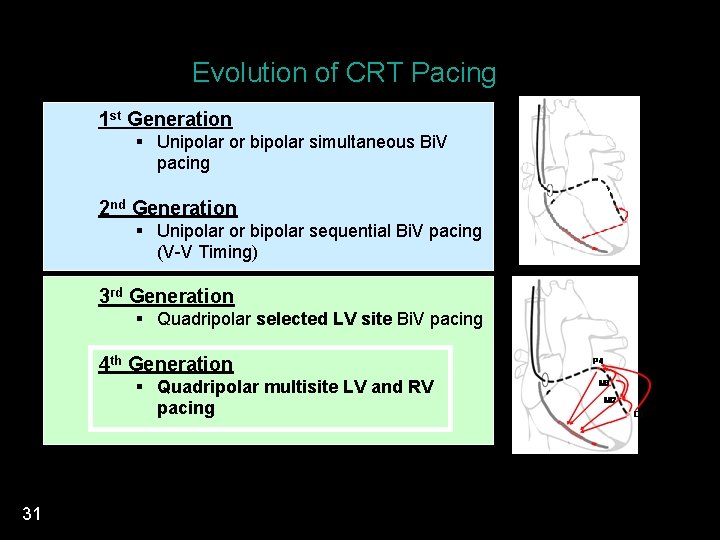
Evolution of CRT Pacing 1 st Generation § Unipolar or bipolar simultaneous Bi. V pacing 2 nd Generation § Unipolar or bipolar sequential Bi. V pacing (V-V Timing) 3 rd Generation § Quadripolar selected LV site Bi. V pacing 4 th Generation § Quadripolar multisite LV and RV pacing 31
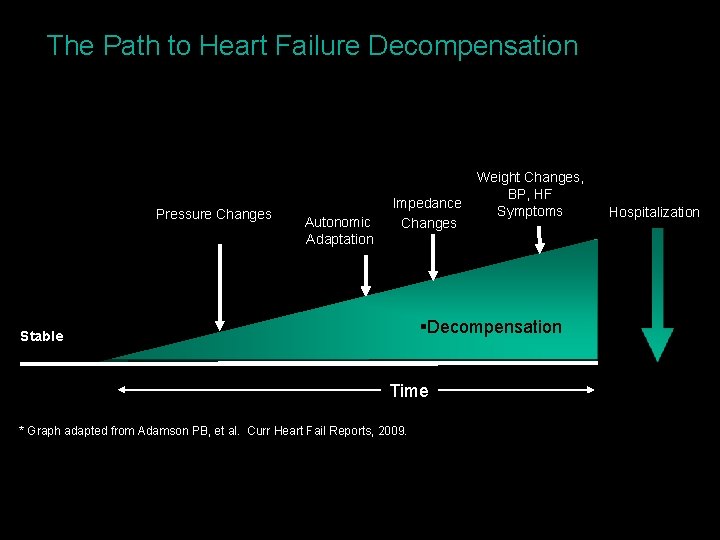
The Path to Heart Failure Decompensation Pressure Changes Autonomic Adaptation Impedance Changes Weight Changes, BP, HF Symptoms §Decompensation Stable Time * Graph adapted from Adamson PB, et al. Curr Heart Fail Reports, 2009. Hospitalization
Implanted LAP Systems Standalone LAP and Combination CRT/D/LAP §CAUTION: Investigational Device, Limited by Federal (or United States) Law to Investigational Use
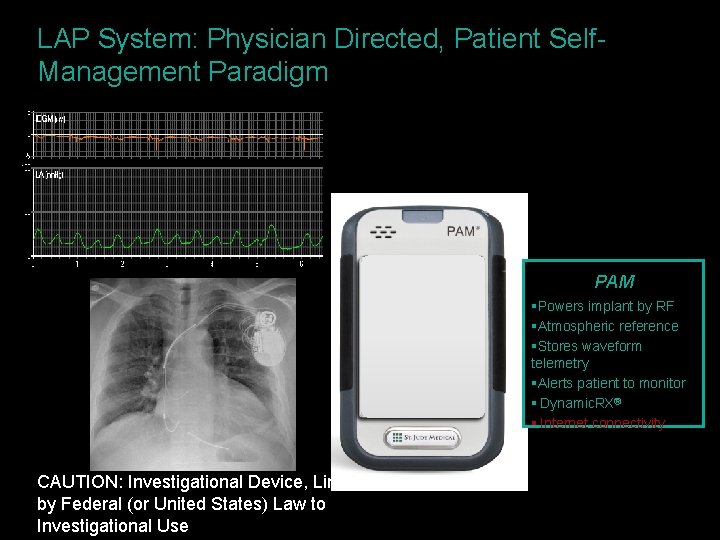
LAP System: Physician Directed, Patient Self. Management Paradigm §Jack PAM §Powers implant by RF §Atmospheric reference §Stores waveform telemetry §Alerts patient to monitor § Dynamic. RX® § Internet connectivity CAUTION: Investigational Device, Limited by Federal (or United States) Law to Investigational Use
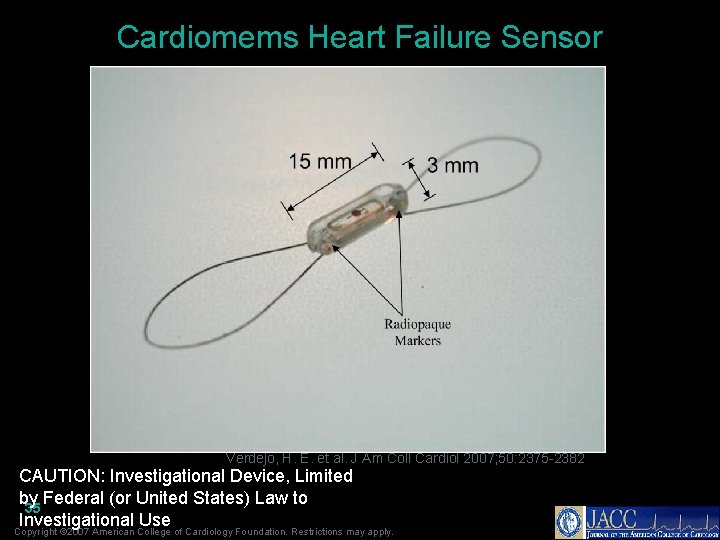
Cardiomems Heart Failure Sensor Verdejo, H. E. et al. J Am Coll Cardiol 2007; 50: 2375 -2382 CAUTION: Investigational Device, Limited by Federal (or United States) Law to 35 Investigational Use Copyright © 2007 American College of Cardiology Foundation. Restrictions may apply.

Cardio. Mems PAP Sensor Deployment and Data Collection CAUTION: Investigational Device, Limited by Federal (or United States) Law to Investigational Use
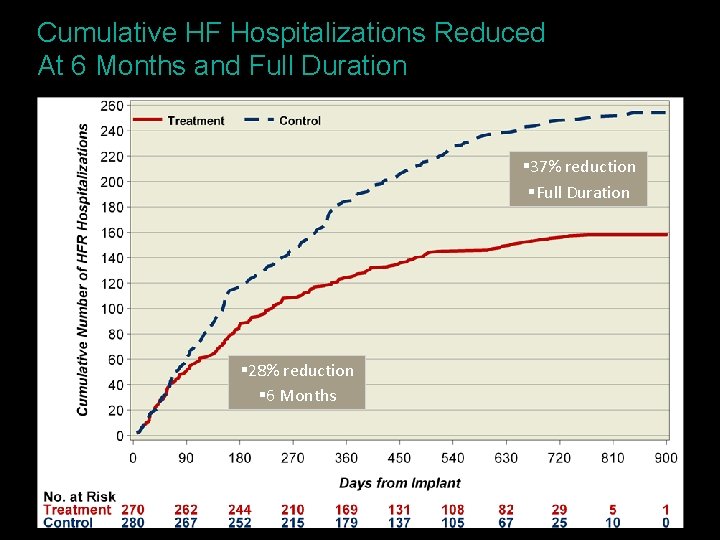
Cumulative HF Hospitalizations Reduced At 6 Months and Full Duration § 37% reduction §Full Duration § 28% reduction § 6 Months §Caution: Investigational Device. Limited by U. S. law to investigational use only.
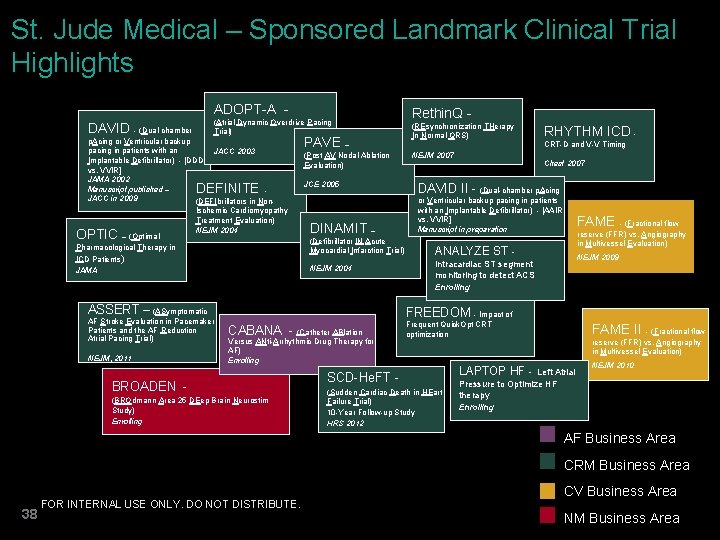
St. Jude Medical – Sponsored Landmark Clinical Trial Highlights ADOPT-A (Atrial Dynamic Overdrive Pacing Trial) DAVID - (Dual-chamber p. Acing or Ventricular backup pacing in patients with an JACC 2003 Implantable Defibrillator) - [DDDR vs. VVIR] JAMA 2002 Manuscript published – JACC in 2009 (DEFIbrillators in Non- DEFINITE OPTIC – (Optimal Ischemic Cardiomyopathy Treatment Evaluation) NEJM 2004 PAVE – (Post AV Nodal Ablation Evaluation) JCE 2005 DINAMIT – (Defibrillator IN Acute Myocardial Infarction Trial) Pharmacological Therapy in ICD Patients ) JAMA NEJM 2004 ASSERT – (ASymptomatic AF Stroke Evaluation in Pacemaker Patients and the AF Reduction Atrial Pacing Trial) NEJM, 2011 Rethin. Q (REsynchronization THerapy In Normal QRS) NEJM 2007 RHYTHM ICD CRT-D and V-V Timing Chest 2007 DAVID II - (Dual-chamber p. Acing or Ventricular backup pacing in patients with an Implantable Defibrillator) - [AAIR vs. VVIR] Manuscript in preparation FAME - (Fractional flow reserve (FFR) vs. Angiography in Multivessel Evaluation) ANALYZE ST - NEJM 2009 Intracardiac ST segment monitoring to detect ACS Enrolling FREEDOM - Impact of CABANA - (Catheter ABlation Versus ANti-Arrhythmic Drug Therapy for AF) Enrolling BROADEN (BROdmann Area 25 DEep Brain Neurostim Study) Enrolling Frequent Quick. Opt CRT optimization SCD-He. FT (Sudden Cardiac Death in HEart Failure Trial) 10 -Year Follow-up Study HRS 2012 LAPTOP HF - FAME II - (Fractional flow reserve (FFR) vs. Angiography in Multivessel Evaluation) Left Atrial Pressure to Optimize HF therapy Enrolling NEJM 2010 AF Business Area CRM Business Area 38 FOR INTERNAL USE ONLY. DO NOT DISTRIBUTE. CV Business Area NM Business Area
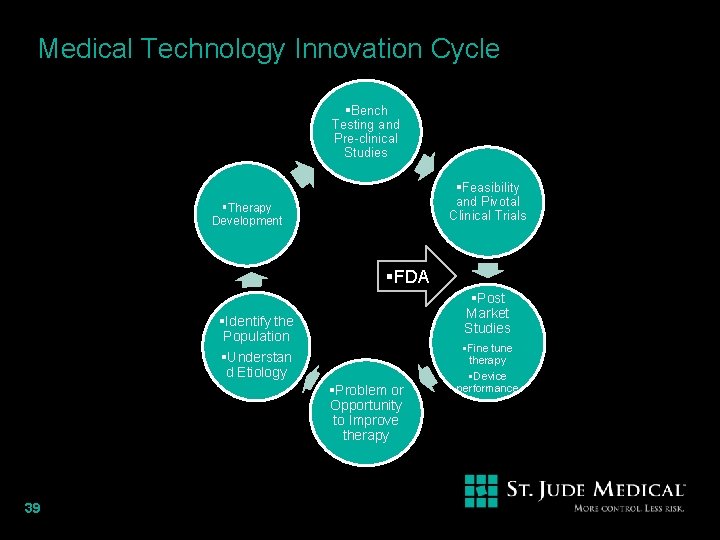
Medical Technology Innovation Cycle §Bench Testing and Pre-clinical Studies §Feasibility and Pivotal Clinical Trials §Therapy Development §FDA §Post Market Studies §Identify the Population §Understan d Etiology §Problem or Opportunity to Improve therapy 39 §Fine tune therapy §Device performance
Thank You 40
- Slides: 40