BRIDGING THE GAP Managing Placement Expenses and Growing

BRIDGING THE GAP : Managing Placement Expenses and Growing Demands Collaboratively.

Does doing your job make you feel like?

With placement expenses increasing at the same time that placement demand student numbers are growing, our work is like this too.

The good news is that effective solutions to really complex issues lie in the COLLECTIVE IMPACT APPROACH

When organisations work together, under the right conditions, we can accomplish great things.

To use a collective impact approach, we need to do the following:

A COMMON AGENDA FOR CHANGE 1. Consider what we know through: • A brief look at the literature • Brainstorming shared issues in breakout groups

What do we know? Higher Education Base Funding Review Final Report. Lomax-Smith, Watson, Webster, Oct. 2011 • Noted the escalating costs associated with sourcing, supporting and funding clinical placements and teaching practicums. Appear to be increasingly unsustainable. • Universities traditionally relied on goodwill and partnerships with organisations to provide clinical placements. However, increasingly universities are being charged a fee by providers. • Identified a lack of transparency with different schemes operating within the public, private and not-for-profit sectors. Differing fees, charges and arrangements made it difficult to understand the costs and subsidies for health and education courses. • Insufficient information to suggest a funding mechanism to resolve the problems. Recommended the Australian Government undertake a detailed assessment of the costs of health and education placements to define the roles of Australian governments and employers/industry in maintaining the relevant workforces and to identify ways to avoid cost escalation.

What do we know? Cost of Delivery of Higher Education Final Report. Deloitte Access Economics, Dec. 2016 • Study involving 700, 000 enrolments on higher education costs. Evidence demonstrated that costs across fields of education remain broadly similar to part of the 2011 costing study. At a sectoral level costs remained stable across the two studies. • Consultations and submissions identified consistently across institutions concerns associated with clinical placements. • Almost all universities noted various difficulties in finding or paying for placements, with the key issues relating to a reduction in the number of placements provided free of charge to the university • The increasing cost and supply issues associated with placements, particularly courses requiring clinical placements. • Clinical placements have increased at a rate faster than inflation. • A general increase in competition for placements as demand exceeds supply, particularly in geographies where multiple universities compete for the same places. • In response to the increasing clinical placements costs to universities, some states developed frameworks to standardise costs and facilitate management of placements eg: Vic Health.

What do we know? The costs and benefits of providing undergraduate student clinical placements for a health service organisation: A rapid review. Bowles, Haines, Et Al, Dec. 2014 • Large volume of literature on costs and benefits of clinical placements for students. • Limited literature assessing aspects for health service providers. • No thorough investigation and analysis into the costs and benefits of clinical placements for health service organisations. • Research established costs of clinical placements only accounted for clinical time: add cost to a health service provider by consuming supervisor time and decreasing work units’ service. Can also add to service provision over the time of the placement, provide a source of future workforce recruitment, add to supervisory capacity and improve the public perception of the health service. • A thorough and holistic listing of agreed costs and benefits of undergraduate clinical placements for all stakeholders has not been established nor collated in evidence based literature. • Future analysis for all stakeholders need to account for differences between professions and disciplines, placement settings, time into the health qualification and placement longevity. need to be assessed against the strategic objectives of these stakeholders. • Any future funding models to move in direction of activity based funding. • A full listing of the costs and benefits need to be identified, agreed and substantiated before analysis. • Imperative if a dollar value of clinical placements is to be determined.

BREAKOUT GROUPS
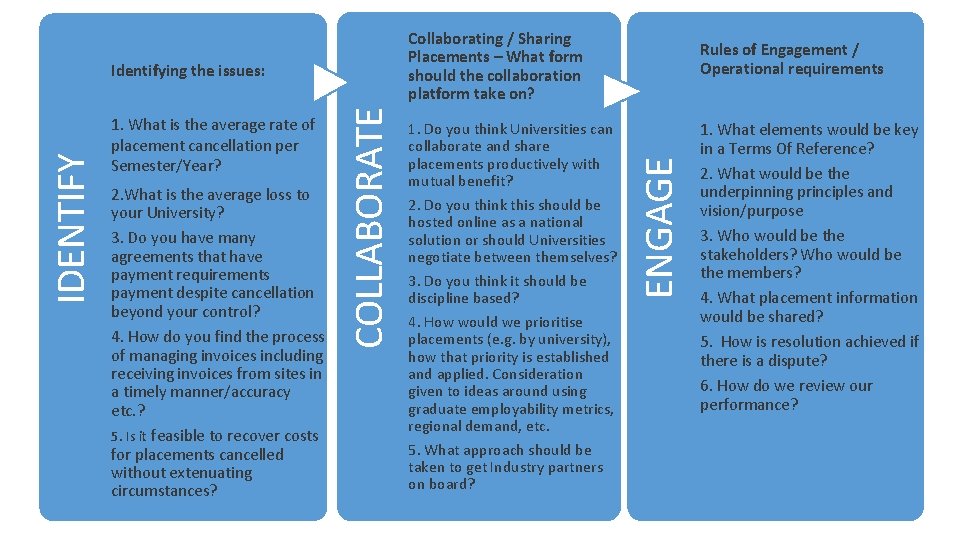
Collaborating / Sharing Placements – What form should the collaboration platform take on? 2. What is the average loss to your University? 3. Do you have many agreements that have payment requirements payment despite cancellation beyond your control? 4. How do you find the process of managing invoices including receiving invoices from sites in a timely manner/accuracy etc. ? 5. Is it feasible to recover costs for placements cancelled without extenuating circumstances? 1. Do you think Universities can collaborate and share placements productively with mutual benefit? 2. Do you think this should be hosted online as a national solution or should Universities negotiate between themselves? 3. Do you think it should be discipline based? 4. How would we prioritise placements (e. g. by university), how that priority is established and applied. Consideration given to ideas around using graduate employability metrics, regional demand, etc. 5. What approach should be taken to get Industry partners on board? ENGAGE 1. What is the average rate of placement cancellation per Semester/Year? COLLABORATE IDENTIFY Identifying the issues: Rules of Engagement / Operational requirements 1. What elements would be key in a Terms Of Reference? 2. What would be the underpinning principles and vision/purpose 3. Who would be the stakeholders? Who would be the members? 4. What placement information would be shared? 5. How is resolution achieved if there is a dispute? 6. How do we review our performance?
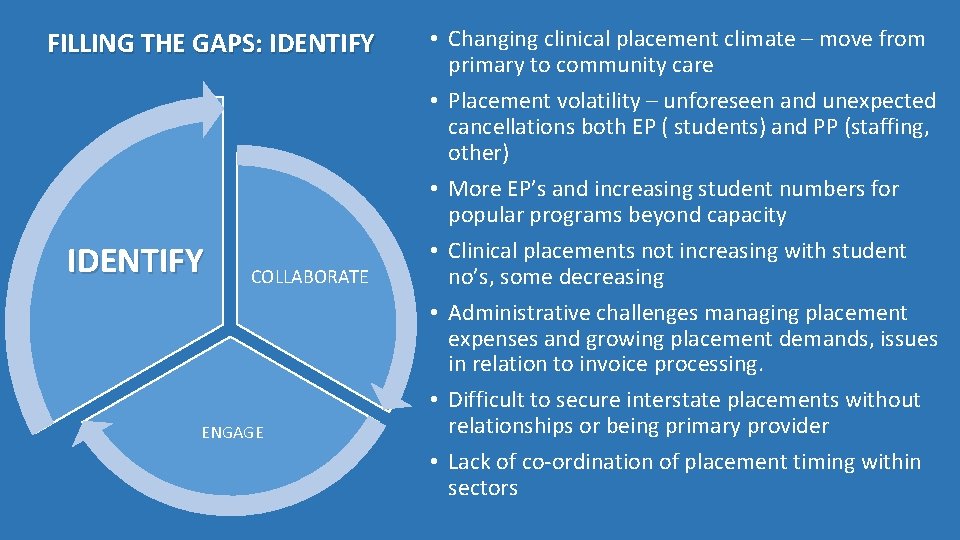
FILLING THE GAPS: IDENTIFY COLLABORATE ENGAGE • Changing clinical placement climate – move from primary to community care • Placement volatility – unforeseen and unexpected cancellations both EP ( students) and PP (staffing, other) • More EP’s and increasing student numbers for popular programs beyond capacity • Clinical placements not increasing with student no’s, some decreasing • Administrative challenges managing placement expenses and growing placement demands, issues in relation to invoice processing. • Difficult to secure interstate placements without relationships or being primary provider • Lack of co-ordination of placement timing within sectors
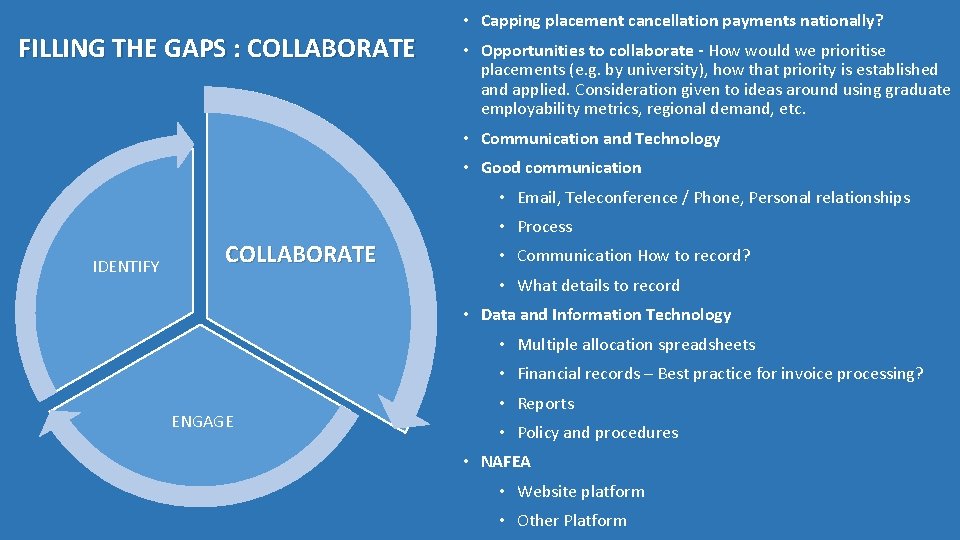
FILLING THE GAPS : COLLABORATE • Capping placement cancellation payments nationally? • Opportunities to collaborate - How would we prioritise placements (e. g. by university), how that priority is established and applied. Consideration given to ideas around using graduate employability metrics, regional demand, etc. • Communication and Technology • Good communication • Email, Teleconference / Phone, Personal relationships • Process IDENTIFY COLLABORATE • Communication How to record? • What details to record • Data and Information Technology • Multiple allocation spreadsheets • Financial records – Best practice for invoice processing? ENGAGE • Reports • Policy and procedures • NAFEA • Website platform • Other Platform
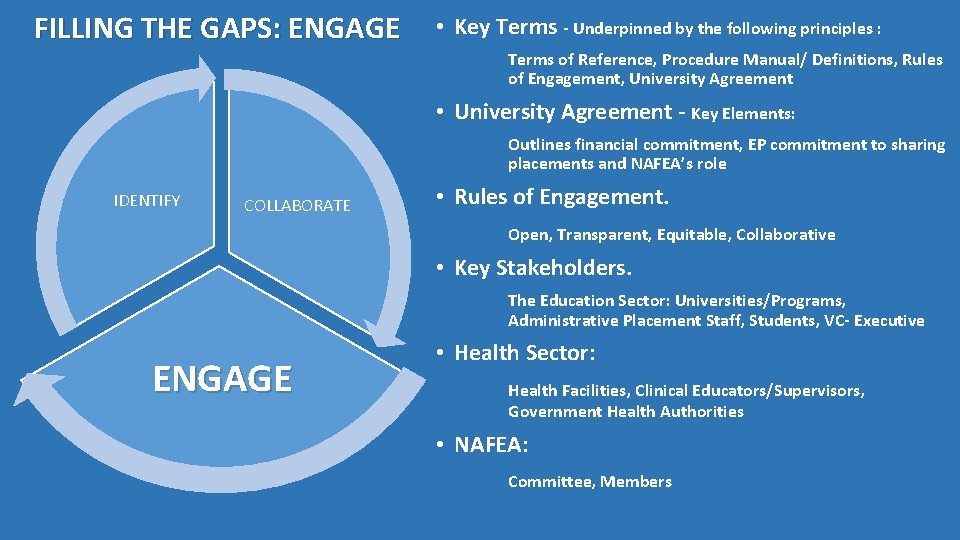
FILLING THE GAPS: ENGAGE • Key Terms - Underpinned by the following principles : Terms of Reference, Procedure Manual/ Definitions, Rules of Engagement, University Agreement • University Agreement - Key Elements: Outlines financial commitment, EP commitment to sharing placements and NAFEA’s role IDENTIFY COLLABORATE • Rules of Engagement. Open, Transparent, Equitable, Collaborative • Key Stakeholders. The Education Sector: Universities/Programs, Administrative Placement Staff, Students, VC- Executive ENGAGE • Health Sector: Health Facilities, Clinical Educators/Supervisors, Government Health Authorities • NAFEA: Committee, Members

Unity is strength. . . When there is teamwork and collaboration, wonderful things can be achieved. - Mattie Stepanek

A ‘BACKBONE’ COORDINATING ORGANISATION/S • NAFEA Endorsed placement costs and billing recommendations for Placement providers including cancellations • Consider Capacity Building • NAFEA project opportunity to identify the costs and contributions associated with clinical placement. Respectful collaboration with EP’s to enhance efficiency, clarity and transparency in the management and funding of clinical placements. • NAFEA facilitation of placement trading/collaboration via website and develop model rules for using this facility.

Tackling complex problems through collective impact: 1. Agree on common goals – we started that process here today. 2. Agree to track progress in the same way which allows for continuous improvement 3. Do what we all do best, while identifying new ways to work together 4. Have consistent communication 5. Have skill and dedicated resources to support ongoing efforts

Our INDUSTRY’S toughest problems are not going away. In fact, many experts predict they will continue to grow in NUMBERS & COMPLEXITY.

Solving these problems require a range of expertise from a number of diverse organisations.

COLLECTIVE IMPACT is a proven approach, helping organisations WORK TOGETHER to MOVE MOUNTAINS.
THANK YOU FOR YOUR PARTICIPATION FEEDBACK WELCOME Ina Kotze Placements Coordinator USQ E: Ina. Kotze@usq. edu. au Katie Cosh Placements Lead, Nursing USQ E: Katie. Cosh@usq. edu. au Wendy Harris Paramedicine Placements Officer GU E: w. harris@griffith. edu. au
- Slides: 22