Bridgend Community Weight Management Programme 18 July 2012

Bridgend Community Weight Management Programme 18 July 2012 Welsh Public Health Conference Presenters: Peter Mannion, Beth Preece ABM Public Health Team and Dr Sean Young (GP/ CD for Primary Care Bridgend)

How it started Initiated by GP in Cwm Garw Practice with support from chronic conditions management in HB Perception of need due to – Increase in prescribing of antiobesity medication (and limited effectiveness) Lack of community based provision
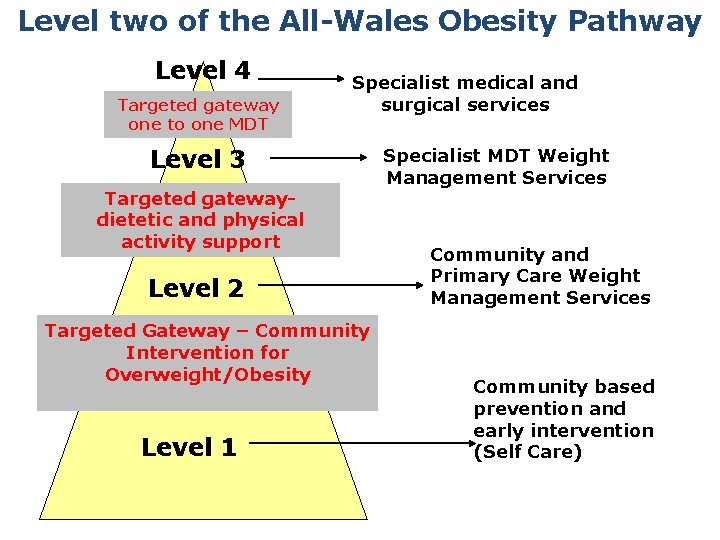
Level two of the All-Wales Obesity Pathway Level 4 Targeted gateway one to one MDT Specialist medical and surgical services Level 3 Targeted gatewaydietetic and physical activity support Level 2 Targeted Gateway – Community Intervention for Overweight/Obesity Level 1 Specialist MDT Weight Management Services Community and Primary Care Weight Management Services Community based prevention and early intervention (Self Care)

NICE Guidelines (2006) • It is unlikely that the problem of obesity can be addressed through primary care management alone • The clinical management of obesity cannot be viewed in isolation from the environment in which people live. • Multicomponent interventions are the treatment of choice: behaviour change strategies to increase people's physical activity levels and improve eating behaviour

NICE Guidelines (2006) • Weight loss programmes (including commercial or self-help groups, slimming books or websites) are recommended only if they: • are based on a balanced healthy diet • encourage regular physical activity • expect people to lose no more than 0. 5– 1 kg (1– 2 lb) a week.

Community Based Model Primary Care Leadership Assess motivation GP contract Monitoring Community Weight Group Set target weight, Monitor weight Peer support Weekly discussion topics Exercise on Referral Provision of structured programme of physical activity under guidance of suitable qualified exercise professional Community Wellbeing Broker Signposting Motivating Supporting engagement Aim: to provide a community weight management programme delivered in a non-clinical environment that gives individuals support to make sustainable changes to their lifestyle and reduce prescribing of anti-obesity medication.
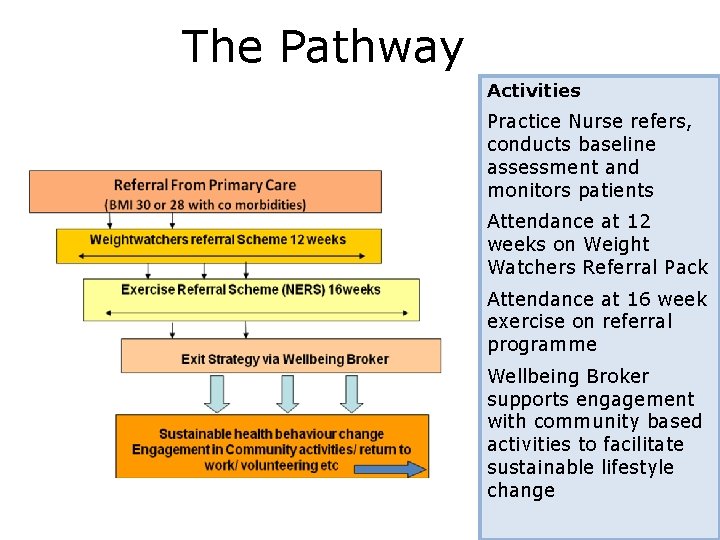
The Pathway Activities Practice Nurse refers, conducts baseline assessment and monitors patients Attendance at 12 weeks on Weight Watchers Referral Pack Attendance at 16 week exercise on referral programme Wellbeing Broker supports engagement with community based activities to facilitate sustainable lifestyle change

Service Evaluation Method Mixed method approach (real life context): • Satisfaction – 3 patient stories • Constraints and supporting factors to maintaining a behaviour change – Wellbeing Wales Wellbeing Assessment (focus groups and questionnaires) • Cardiovascular parameters measured and self report healthy eating and quality of life questionnaire for 66 pilot participants and analysed by Swansea University • Monitoring of prescribing levels of weight loss medication (Orlistat)

Research Evidence • Jebb et al ‘commercial weight loss programme - clinically useful early intervention for weight management in overweight and obese people that can be delivered at large scale’ Lancet 2011 • Jolly et al- ‘Commercially provided weight management services are more effective and cheaper than primary care based services led by specially trained staff, which are ineffective’ BMJ 2001

Progress • Launched Cwm Garw Practice September 2010 , Ogmore Vale March 2011, Nantymoel June 2011 • 372 total number of participants • Average 48 years (min 18 – max 81) • Average BMI at start 38. 6 kg/m 2 • Average BMI at end (for those that complete 24 weeks) – 35. 2 kg/m 2 • 81% completing 10 weeks or more of Weight Watchers • 58% taking up exercise on referral, most popular activities walking, gym and exercise class (e. g. Zumba)

Results • Statistically significant mean weight loss – 7. 2 kg • Statistically significant mean BMI reduction – 7% • Statistically significant reduction in waist circumference • 58 % (25) achieved 5% or more weight loss at twelve weeks • Diabetic cohort (15) achieved the most health benefits with greater mean weight loss and significant reduction in Hba 1 C • Reductions in blood pressure and cholesterol but not significant
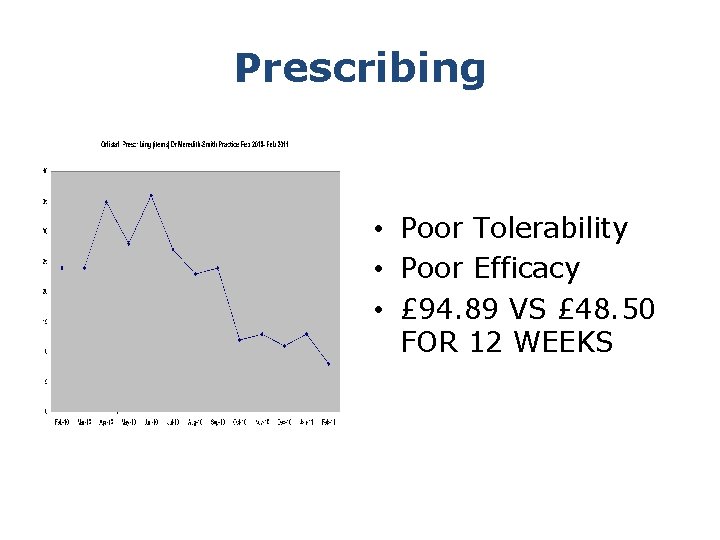
Prescribing • Poor Tolerability • Poor Efficacy • £ 94. 89 VS £ 48. 50 FOR 12 WEEKS

Patient Story “They said if my blood sugar didn’t come down I was going to be put on insulin. I didn’t want to be a pincushion, so when they suggested Weight. Watchers, I said I would give it a go” For my diabetes, they’ve stopped everything bar two tablets where I used to have eight” hba 1 c 8. 2% on gliclazide/ metformin hba 1 c 6. 1% on metformin alone bmi 45 to 37 (weight loss 18 kg)

Patient Story “My blood pressure was high and I’ve got asthma and arthritis. My blood pressure tablets have now stopped. I still have aches and pains, but after losing three stone I feel good about myself” wt loss on orlistat 3/12 - 1 kg wt loss on scheme 3/12 - 7 kg bmi 44 now 38 (weight loss 14 kg) felodipine 10 mg/ perindopril 4 mg – both stopped- bp satisafactory of medication

Patient Story “When I lost the weight, one of the first things I did was come off painkillers. I’m still on blood pressure tablets, but it’s under control, my cholesterol is good, my pain has gone, I’m moving easier and sleeping” bmi 45 31. 5 kg) now 31 (weight loss

Wellbeing Results • The following are supportive of participants subjective wellbeing: Ø being part of a group or community Ø a supportive co-ordinator, family and friends Ø being able to take control of weight Ø recognising physical and medical benefits The role of the environment in supporting wellbeing could be enhanced

Lessons Learnt • Requires primary care ownership to actively manage patient compliance and review contract between patient and GP practice • Individuals require support to make sustainable lifestyle changes which have to be relevant to their life within their community • The focus needs to be that this is a healthy lifestyle programme and not a diet • Developing and maintaining the links between components requires a strong sustained collaborative effort • Careful consideration of data collection protocols from the outset is very important especially when data will be used from different organisations; retrospective collation is difficult.

Future Plans • Roll-out to other GP practices in Bridgend • Assessing the longer term sustainability of this programme – monitoring of weight and cardiovascular parameters up to 12 months • Build evidence of cost effectiveness through prescribing savings • Increasing uptake to exercise on referral • Further development and evaluation of the Wellbeing Broker role • Agree place within pathway

Feedback from the NHS Wales Awards Judges: “This is a creative, yet practical, response to the health and well-being needs of the local community – and it made a real and tangible difference to the lives of the participants, and in turn to their families. This clearly set out to address health inequalities and succeeded in introducing new ways of thinking about lifestyle, improving health and avoiding disease. ”

Any Questions?

Discussion How important do you feel is a level 2 weight management programme compared to actions at other levels of the obesity pathway, to make the most impact on obesity levels?

What type of evidence would you want to support a programme like this?

How transferable do you feel the Bridgend Community Weight Management Programme is to other communities? What would need to be considered?

Are there other effective options for providing support at level two- which can deliver volume and efficacy?
- Slides: 24