Brent Arnspiger LCSW Bettie Beckworth M Ed Steven

Brent Arnspiger, LCSW Bettie Beckworth, M Ed Steven Hall, Ph. D Sarah Strang, LCSW 1

Overview • • Suicide Data History of Initiatives in Texas Mayor’s Challenge Governor’s Challenge Rural Veteran’s Initiative Means Safety Initiative Safety Plans 2

Suicide in the United States • 47, 173 U. S. deaths from suicide per year among the population overall (2017) • 19, 510 U. S. deaths from homicide per year – Less than 1/2 the number of annual suicides • Suicide is the 10 th leading cause of death in the U. S. • Homicide is the 16 th leading cause of death in the U. S. [Drapeau, C. W. , & Mc. Intosh, J. L. (for the American Association of Suicidology), (2018)] 3

Suicidal Behavior • Gender: Men take their lives at 3. 5 times the rate of women – Women are 3 times more likely to attempt suicide [Drapeau, C. W. , & Mc. Intosh, J. L. (for the American Association of Suicidology), (2018)] • Age: – 15 – 24 y/o: Suicide is 2 nd leading cause of death – 25 – 34 y/o: Suicide is 2 nd leading cause of death – Persons aged 65 years have a high risk for suicide [Drapeau, C. W. , & Mc. Intosh, J. L. (for the American Association of Suicidology), (2018)] 4

Veteran Population Veteran Status: Veterans may be at even greater risk than those in the general population 18 - 20% of suicide deaths are Veterans (National Violent Death Reporting System) About 20 suicides per day are Veterans (National Violent Death Reporting System) ~ 6 suicides per day among Veterans receiving care in VHA (VA Serious Mental Illness Treatment, Research and Evaluation Center) 5
![Methods of Suicide US Suicides [CATEGOR Suffocation Y NAME] 7% or Hanging 28% Veteran Methods of Suicide US Suicides [CATEGOR Suffocation Y NAME] 7% or Hanging 28% Veteran](http://slidetodoc.com/presentation_image/22f4a1443cc693f14e888bc6a3a4a8cf/image-6.jpg)
Methods of Suicide US Suicides [CATEGOR Suffocation Y NAME] 7% or Hanging 28% Veteran Suicides Suffocation or Hanging 12% Firearms 51% Other 8% Poisoning 13% [CATEGOR Y NAME] 14% Firearms 68% [Drapeau, C. W. , & Mc. Intosh, J. L. (for the American Association of Suicidology), (2018)] 6

History of Service Members, Veteran and their Families (SMVF) Initiatives in Texas State of Texas Named National Leader in Federal Initiative • In 2013, the governor accepted the invitation of the U. S. Substance Abuse and Mental Health Administration (SAMHSA) to participate in the development of policy and best practices to improve services to Texas service members, veterans and their families (SMVF). • The Office of Veteran Services, Texas Health and Human Services Commission, was named State Team Lead by the governor to direct initiatives involving military and civilian collaborations and partnerships across federal, state, local, public-private and faithbased agencies throughout Texas. 7

History of Service Members, Veteran and their Families (SMVF) Initiatives in Texas • Interagency teams have developed policy and initiatives regarding justice-involved service members and veterans, issues facing military and veteran families, statewide suicide prevention among SMVF, employers answering the call to assist veterans transition to civilian jobs and community, homelessness and others critical issues • The SMVF Suicide Prevention Initiative resulted in the passage of Senate Bill 578 in 2017 mandating a statewide suicide prevention plan specifically for that population. • In 2018, the U. S. Veterans Administration (VA) joined SAMHSA to launch the Mayor’s Challenge to Prevent Suicide among SMVF. 8

Mayor’s Challenge 9

Background • “Since 2008, the Substance Abuse and Mental Health Services Administration (SAMHSA) has assisted states and territories to strengthen behavioral health service systems supporting service members, veterans, and their families (SMVF). ” • “Recognizing the importance of addressing these needs at the local level, SAMHSA and the U. S. Department of Veterans Affairs (VA) are sponsoring the 2018 inaugural Mayor’s Challenge to Prevent Suicide among Service Members, Veterans, and their Families. ” Senate Research Center (2017), Bill Analysis, Senate Bill 578. 10

Key Objectives of the Mayor’s Challenge • Build an interagency military and civilian team of leaders from the city and state that will develop and implement a strategic action plan to prevent and reduce suicide attempts and completions at the local level • Acquire a deeper familiarity with the issues surrounding suicide prevention for SMVF • Increase knowledge about the challenges and lessons learned in implementing strategies by utilizing city to city sharing • Employ promising, best, and evidence-based practices to prevent and reduce suicide attempts and completions at the local level • Define and measure success, including defining assignments, deadlines, and measurable outcomes to be reported 11

Timeline • Houston accepted the challenge December 2017 • Committee members were invited to participate February 2018 • Committee members met in Washington, D. C. , in March 2018 • Local meetings began in May 2018 12

Houston Mayor’s Challenge Composition • City of Houston Veterans Affairs Office • Houston VA Medical Center • Texas Health and Human Services Commission, Veteran Services • Houston Police Department • Houston Fire Department • Houston Health Department • The Harris Center • Mental Health America of Greater Houston, Veterans Behavioral Health • Combined Arms 13

Houston Mayor’s Challenge • Houston Mayor’s Challenge meets monthly – Sub-committees: Communications, Education and Training, Crisis Coordination, and Data – Sub-committees meet prior to the larger meeting • Developed strategic action plan with sub-categories consistent with the Senate Bill requirements 14

Action Plan for Houston Mayor’s Challenge 1. Strengthening Access and Delivery of Suicide Care – Education and Training Committee will conduct military culture training in the community 2. Identify and Support People at Risk – “Ask the question” which is “have you served in the military? ” – Develop coordinated community-wide crisis response – Ensure Veterans discharged from community hospitals have follow-up care 3. Promoting Connectedness – Interagency collaboration activities and outreach 15

Action Plan, cont. 4. Lessoning Harms and Preventing Future Risk – Create a Suicide Prevention Care Package (gun locks, crisis line cards, agency brochures, Safety Plan, etc. ) 5. Teach Coping and Problem Solving Skills – Provide Trainings in the community for how to do Safety Plans 7. Create Protective Environments – Disseminate gun locks throughout the community 16

Memorandum of Understanding (MOU) Between The Harris Center and VA • In August 2018, Tamara Coy from The Harris Center stated we were going to complete an MOU between The Harris Center and the VA and we were going to do it in 30 days. • We completed the MOU, it took a little longer than 30 days. • However, we started coordinating care before the formal signing. • One action on the Governor’s Challenge Action Plan is to expand the MOU with The Harris Center statewide with a master MOU between the VA and the state office which oversees the local mental health authorities (HHSC). 17

Collaboration Between The Harris Center and VA Before the MOU: The VA learns of a Veteran who is not eligible for VA care or of a humanitarian case in need of outpatient MH services and… • Cannot consistently connect them to care without a clear channel for communication with The Harris Center • Instructs them to follow-up with The Harris Center by giving them a phone number without confirmation of engagement in needed MH services The Harris Center learns of a Veteran and… • Cannot consistently connect them to VA care without a clear channel for communication • Is unclear if they can be served by The Harris Center when possibly eligible for VA • Instructs them to follow-up with VA without confirmation of engagement in needed MH services With the MOU: The VA learns of a Veteran who is not eligible for VA care or of a humanitarian case in need of outpatient MH services and… • Can consistently connect to care with a clear channel for warm handoff with The Harris Center • VA Clinicians from all settings can complete referrals to The Harris Center, as needed, which enhances discharge planning and follow-up care The Harris Center learns of a Veteran and… • Can consistently connect them the VA for care with a clear channel for warm handoff • Clarifies if they can be served by The Harris Center until confirmation of eligibility is made with VA and care is initiated • The Northeast Clinic has been designated as a landing spot for Veterans desiring care through The Harris Center 18
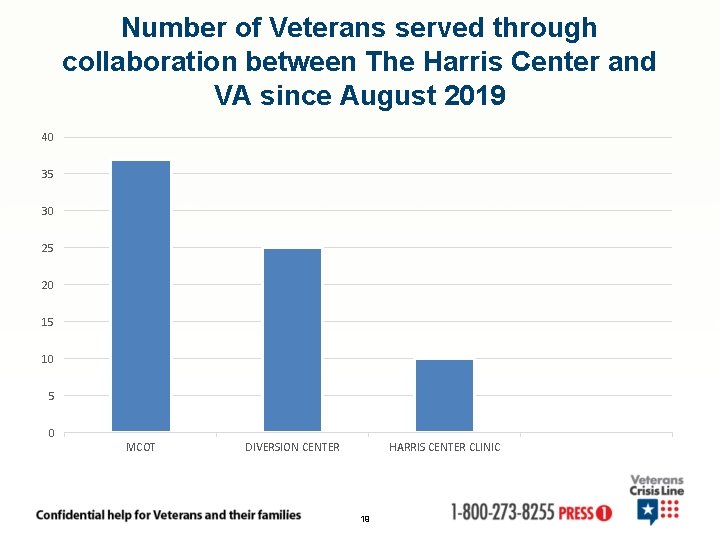
Number of Veterans served through collaboration between The Harris Center and VA since August 2019 40 35 30 25 20 15 10 5 0 MCOT DIVERSION CENTER HARRIS CENTER CLINIC 19

Mobil Crisis Outreach Team (MCOT) Referral Process • How to get help? – MCOT Referrals are made by contacting The Harris Center Crisis Line – To place an MCOT referral call 713 -970 -7000 & press #1 for Crisis Line – Callers reach a Crisis Line specialist who completes a telephone assessment to determine need and assess for safety – Crisis Line specialist sends MCOT the referral and MCOT clinicians follow up with consumer to assess for need and work to resolve the crisis in the least restrictive environment appropriate – MCOT provides services to help with stabilization and linkage to long term mental health services in the community 20

Veteran Success Stories w/MCOT • • Client is 20 year old white male referred to MCOT program by VA Hospital due to reporting feelings of depression, suicidal ideations, and anxiety. Client also reported being homeless and living out of his car. Client was informed he is not eligible for VA benefits due to the short amount of time in the armed services. Client served 6 months in the military and was injured during basic training. While receiving services with MCOT, client was linked to The Harris Center adult clinic for medication management and therapy. Client is stable on medication. Client was also linked with a homeless Gold Card which allows him to go to The Harris Health Clinics for any medical needs. Client was referred to housing assistance and the furniture bank. Client successfully completed all goals and was discharged from MCOT. Upon discharging from MCOT, client informed clinician he was able to reach out to his grandparents who are going to allow him to relocate to Dallas, TX. He was excited that he could move in with his grandparents while he looked for employment and live in the same city as his children. Client reported having a positive outlook on life and motivation to make the changes he needed to be successful. 21

Veteran Success Stories w/MCOT • Female client referred by VA hospital due to being ineligible to receive benefits at the time. Client was waiting on benefits to activate after filing for Military Sexual Trauma (MST) through the VA. Client was stabilized on medication after meeting with MCOT psychiatrist. • While waiting to be eligible for VA services, MCOT clinician linked client to The Harris Center adult clinic where she can continue to see a psychiatrist and a therapist. • Clinician helped client gain employment by sending her information a job fair and helping client to update her resume. • Clinician helped her with her living situation and filing for housing resources. 22

Crisis Collaboration Committee Care Coordination Agreements Completed • The VA Hospital and The Harris Center • STAR of Hope homeless programs and The Harris Center • Combined Arms and The Harris Center • The Houston Health Department and The Harris Center • Pending with Easter Seals and The Harris Center 23

Collaboration after a Suicide Attempt • In February 2019, we added collaboration between the Houston Police Department and The Harris Center for “suicide related events” in Houston. • HPD will provide the individual person’s contact information to The Harris Center • Harris Center staff will attempt to contact the person and assist with connections to services and treatment • We plan to expand this to Houston Fire Department as well. • Will attempt to work with local hospitals for events not reported to HPD/HFD to connect people to services following a suicide attempt or after visiting an ED due to mental health concerns. 24

Houston Mayor’s Challenge Accomplishments • Multiple agencies come together to coordinate our efforts to assist Veterans and help identify how we can work together with the available resources we each have to create a spectrum of care. • Coordination of care between the VA and The Harris Center (the local county mental health authority) through a Memorandum of Understanding (MOU) which provides a mechanism for warm handoffs to ensure Veterans receive needed services. 25

Houston Mayor’s Challenge Accomplishments • The Houston Police Department and Fire Department will begin providing patient information to The Harris Center when a suicide related behavior is the reason for the call. The Harris Center will triage, assess the patient and assist with connecting to follow up services in the community or the VA to ensure people, including Veterans and their families, are connected to services following suicidal behaviors. 26

Additional Actions for the Mayor’s Challenge • Most of the actions have been completed on the current plan • Using the VA National Strategy to Prevention Suicides, the committee is developing further actions at the monthly meetings to additional actions to the plan 27

Governor’s Challenge 28

Governor’s Challenge • Texas Governor’s Challenge began in December 2018 • Committee members met in Washington, D. C. , in February and May 2019 • The committee is meeting monthly to develop a statewide action plan • Action Plan – 5 priorities – Multiple strategies under each priority 29

Governor’s Challenge 1. Expand Support Texas Suicide Prevention Council 2. Improve and Increase connection to DOD’s Transition Assistance Program 3. Create a Unified Communication Strategy with Consistent Messaging 4. Formalize Coordination of Services Between the VA and Community Health Agencies Statewide 5. Improve Available Information about Service Member Suicides and Attempts through Data Sharing 30

NY Times Interview • The New York Times wrote an article about suicide prevention efforts throughout the VA. • As part of this interview, I was interviewed by phone to discuss the MOU between the Houston VA and The Harris Center with plan to extend this statewide. • I’m calling it “Tamara’s Legacy” since she was the driving force behind the MOU. • I also discussed the Governor’s Challenge with some of the ideas for the state action plan 31

VA Rural Veterans Initiative 32

VA Rural Veterans Initiative • First meeting scheduled for 3 rd week of April in Washington, D. C. • Will be similar to Mayor’s and Governor’s Challenges, but will work with rural communities • Tri County Services is participating in the initiative 33

VA Means Safety Initiative 34

VA Means Safety Initiative • The VA, the National Shooting Sports Foundation (NSSF), and the American Foundation for Suicide Prevention (AFSP) have compiled tips for safely storing firearms as well as best practices for sharing these guidelines in the community. • Responsible firearm ownership begins by understanding safe storage and the steps for properly securing firearms in your home. • The other VA initiatives are incorporating the information from the tool kit into action plans 35
![Methods of Suicide US Suicides [CATEGOR Suffocation Y NAME] 7% or Hanging 28% Veteran Methods of Suicide US Suicides [CATEGOR Suffocation Y NAME] 7% or Hanging 28% Veteran](http://slidetodoc.com/presentation_image/22f4a1443cc693f14e888bc6a3a4a8cf/image-36.jpg)
Methods of Suicide US Suicides [CATEGOR Suffocation Y NAME] 7% or Hanging 28% Veteran Suicides Suffocation or Hanging 12% Firearms 51% Other 8% Poisoning 13% [CATEGOR Y NAME] 14% Firearms 68% [Drapeau, C. W. , & Mc. Intosh, J. L. (for the American Association of Suicidology), (2018)] 36
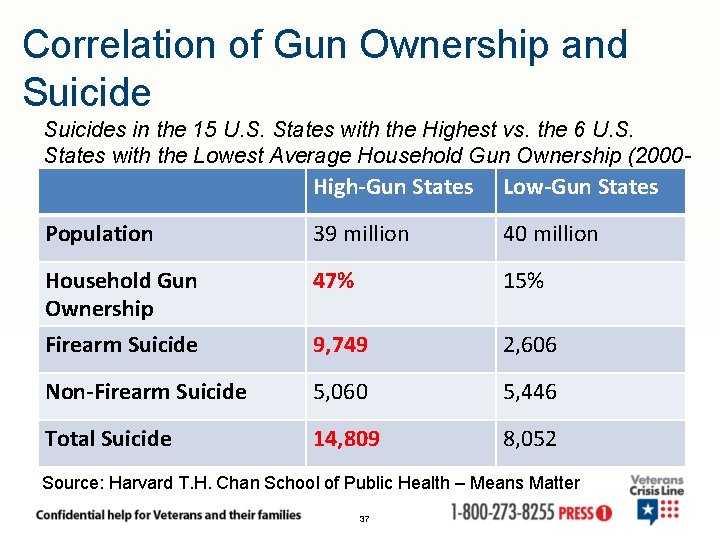

Correlation of Gun Ownership and Suicides in the 15 U. S. States with the Highest vs. the 6 U. S. States with the Lowest Average Household Gun Ownership (20002002) High-Gun States Low-Gun States Population 39 million 40 million Household Gun Ownership 47% 15% Firearm Suicide 9, 749 2, 606 Non-Firearm Suicide 5, 060 5, 446 Total Suicide 14, 809 8, 052 Source: Harvard T. H. Chan School of Public Health – Means Matter 37

Means Safety • Most people who die by suicide die on their first attempt (VA Safety Plans – Stanley & Brown, 2008) • Attempts with firearms have an 85% fatality rate (Vyrostek, Annest, & Ryan, 2004) • Drug overdose, the most widely used method in suicide attempts, is fatal in less than 3% of cases (Source: Harvard T. H. Chan School of Public Health – Means Matter) • Firearms in the home double the odds for death by suicide (Brent & Bridge, 2003; Brent et al. , 1991; Brent et al. , 1993; Kellermann et al. , 1992) • Potential impact for means safety probably greatest for firearm-related suicides (Bryan, et al. , 2011) 38

Means Safety Obstacles • Clinicians who view means safety as ineffective are five times less likely to provide it. • Clinicians have an inaccurate perception regarding effectiveness. – Means-safety counseling significantly increased the likelihood of action taken on restricting availability. – 63% of those counseled reported securing firearms. (Bryan, et. al. , 2011) 39

Language Matters • • Veterans likely to be pro-rights and personal freedoms “Restriction” not a popular concept “Safety” more benign and general term Can be applied not just to the at-risk individual but also their family, children, and grandkids • Military training strong emphasis on weapons safety • Fits better with safety plan concept • Opens door for collaboration (VA Department of Veterans Affairs, Rocky Mountain MIRREC) 40

Weapons Safety • Assume own weapons, ask “how many? ” rather than “do you have? ” • How currently stored? • What additional storage options are acceptable and feasible? • Not trying to take away their guns or limit their rights • Focus is on their safety and of others in the home (if relevant) • Create more distance between at-risk individual and (VA Department of Veterans Affairs, Rocky Mountain MIRREC) weapon than currently exists 41

Means Safety Counseling • Present a menu of options for restricting access when there is a risk of suicide: – Ideal solution is to remove from home until crisis passes – Removing by giving to a supportive family or friend – Locking the means up in a safe or other secured manner (with keys/combinations held by a supportive other) – Separate ammunition from the gun • INVOLVE SIGNIFICANT OTHER AND/OR FRIEND – Make every effort to confirm removal (Bryan, et. al, 2011) 42

Suicide Prevention Safety Plans 43

Suicide Prevention Safety Plans • Safety Plans are not “no-suicide contracts” • No-suicide contracts ask clients to promise to stay alive without telling them how to stay alive • No suicide contracts may appear to the client to be an attempt to “protect” the institution or therapist more than the client • Virtually no empirical evidence to support effectiveness of no-suicide contracts VA Safety Plans – Stanley & Brown (2008) 44 44

Suicide Prevention Safety Plans • The Safety Plan is a collaboration between the client and the clinician – It is the client’s Safety Plan, not the clinician’s – The Safety Plan helps them to know what to do in a crisis – Sit next to the person – Ask the client to write out each step on a paper copy – Assist the client with each step 45

Overview of Safety Planning: 6 Steps 1. Recognizing warning signs 2. Employing internal coping strategies without needing to contact another person 3. Socializing with family members or others who may offer support as well as distraction from the crisis 4. Contacting family members or friends who may help to resolve a crisis 5. Contacting mental health professionals or agencies 6. Lethal means (firearms and methods) VA Safety Plans – Stanleysafety & Brown (2008) 46 46

Implementation: 1. Give the original to the patient. Make a copy for the clinical record. 2. Ask: “Where will you keep your safety plan? ” 3. Offer additional copies to keep in multiple places for easy access (wallet, night stand, refrigerator, etc. ) 4. Ask: “How likely is it that you will use the safety plan? ” 5. Ask: “What might get in the way or serve as a barrier to you using the safety plan? ” 6. Review and update the Safety Plan often, especially after a suicide attempt or hospitalization (both medical and psychiatric. ) VA Safety Plans – Stanley & Brown (2008) 47

There’s an App for That! (VA Virtual Hope Box) Remind Me • Store supportive photos, videos, recorded messages, music Distract Me • Sudoku puzzles, photo puzzles, word search, mahjong solitaire Inspire Me • Inspirational quotes Relax Me • Controlled breathing, muscle relaxation, guided meditation Coping Tools • Coping cards and positive activity planner Support Contacts • Quick access to preselected contacts 48

Questions 49
- Slides: 49