Breathlessness in the Emergency Department Dr Orlaith Scullion

Breathlessness in the Emergency Department Dr Orlaith Scullion 11/09/15

Dyspnoea in the Emergency Department • Aims • To consider common presentations of dyspnoea in adults presenting to the ED • To describe appropriate initial management and treatment • To identify patients with severe or life threatening conditions • To recognise when to involve ICU

BTS Guidelines - CAP • Community aquired • No pre-disposing conditions eg. cancer, immunosuppression • Does NOT apply to those with non-pneumonic LRTI eg. acute exacerbations of COPD / chest infections without CXR changes BTS guidelines for the management of community acquired pneumonia in adults. Thorax 2001: 56; iv 1 -iv 64

BTS Guidelines - pathogens • • • S pneumoniae H influenzae Legionella spp S aureus M catarrhalis Gram negitive enteric bacilli M pneumoniae C psittaci All viruses Influenza A and B mixed

BTS Guidelines – Clinical and Radiological Features • Not able to predict aetiological agent from clinical / radiological features • Elderly patients are more likely to present with non-specific symptoms and less likely to have fever than younger patients • Radiological resolution often lags behind clinical improvement • Radiological changes caused by atypical pathogens clear more quickly than bacterial pathogens

BTS Guidelines • Investigations (Community Rx) • CXR not necessary • Sa. O 2 • Microbiology not recommended, mycobacterium tuberculosis and Legionella if indicated • Investigations (Hospitalise Rx) • CXR / FBC / U+E / LFT / CRP / oxygenation • Blood culture and other microbiology as indicated eg. sputum, urine, serology

BTS Guidelines - severity • Confusion (abb MSE 8 or less) • Urea > 7 mmol/l • Resp rate ≥ 30/min • BP > 90 systolic and / or ≥ 60 diastolic • Pre-existing: • Age ≥ 50 • Co-existing disease

CURB-65 • • • Confusion (abb MSE 8 or less) Urea > 7 mmol/l Resp rate ≥ 30/min BP > 90 systolic and / or ≥ 60 diastolic Age ≥ 65

AAH Antimicrobial Guidelines • CURB-65 score • Rountine investigations for all RTI • FBC / CRP / Blood cultures (x 2) / CXR / oximetry • Additional investigations when CURB-65 >3 • Urinary antigen for Streptococcus pneumoniae and Legionella sp. / atypical pneumonia and Legionella serology / ABG

CURB-65 = 0 or 1 • • Not severe Consider discharge and home treatment 1 st: amoxicillin 500 mg – 1 g TID oral 7/7 Alt: clarithromycin or doxycycline

CURB-65 = 2 • • Not severe Consider hospital supervised treatment 1 st: amoxicillin 500 mg – 1 g TID oral 7/7 Alt: clarithromycin or doxycycline

CURB-65 = 3 • • Severe Inpatient treatment 1 st: amoxicillin 1 g TID IV plus clarithromycin 500 mg BD IV 7/7 Alt: teicoplanin plus clarithromycin IV

CURB-65 = 4 or 5 • Very severe • Assess for ICU admission • 1 st: co-amoxiclav 1. 2 g TID IV plus clarithromycin 500 mg BD IV 7/7 • Alt: discuss with microbiology / ICU

Aspiration CAP • 1 st: amoxicillin 500 mg – 1 g TID IV plus metrondiazole 500 mg TID IV • Alt: clarithromycin plus metrondiazole

Managing Exacerbations of COPD Further Reading: NICE guideline 101 COPD in primary and secondary care 2010 • Treat in hospital: • • • Unable to cope at home / living alone Severe breathlessness Deteriorating / poor general condition Cyanosis Worsening peripheral oedema Impaired level of consciousness / acute confusion Already receiving LTOT Significant co-morbidities Significant CXR changes Sats < 90%, p. H < 7. 35 Pa. O 2 <7

Initial Management • Nebulisers: Salbutamol and ipratropium • Oxygen to maintain sats 92% • Antibiotics if purulent sputum or pneumonic changes on CXR: clarithromycin 500 mg oral / iv +/- co-amoxiclav 1. 2 g iv • Steriods: prednisolone 30 mg daily (100 mg hydrocortisone iv)

Further Management • Consider iv aminophylline • Magnesium 2 g iv (not in guideline) • NIV if persistent hypercapnic ventilatory failure despite optimal medical treatment (MAU) • IPPV (ICU) • Chest physio to help clear secretions

Severe Asthma in Adults • Moderate • ↑ symptoms • PEF >50 -75% best or predicted • Severe • • PEF 33 -50% best or predicted RR ≥ 25 / min HR ≥ 110 / min Inability to complete full sentences in one breath

Severe Asthma in Adults • Life threatening • • • PEF < 33% best or predicted Sp. O 2 < 92% Pa. O 2 < 8 k. Pa normal Pa. CO 2 Silent chest Cyanosis Poor respiratory effort Arrhythmia Exhaustion, altered conscious level.

Treatment of Acute Asthma • Admit if signs of life threatening asthma • Admit if persistent signs of severe asthma after initial treatment • Pts whose PEF > 75% best or predicted one hr after treatment may be d/c home from ED unless other reasons for admission

Treatment of Acute Asthma • Oxygen (sats 94 – 98%) • B 2 agonists: • Nebulised salbutamol 5 mg (oxygen driven) stat • ? Need for continuous nebs • IV if not able to tolerate nebuliser • • Ipratropium 500 mcg neb 4 -6 hrly Steroids: 40 – 50 mg prednisolone Magnesium 2 g iv over 20 mins Routine antibiotics not indicated

Referral to ICU • Requiring ventilatory support • Acute severe or life threatening asthma failing to respond to therapy • • Deteriorating PEF Persisting / worsening hypoxia Hypercapnea Resp acidosis Exhaustion / poor resp effort ↓ GCS or confusion Resp arrest

Summary • • • BTS guidelines Good initial assessment with obs Treat appropriately Get senior help early Consider ICU

Pneumothorax • the presence of air or gas in the cavity between the lungs and the chest wall, causing collapse of the lung. Symtoms • Pleuritic Chest Pain • SOB • Decreased exercise tolerance • Cough • Palpitations

Signs • Decreased expansion on affected side • Hyper-resonant percussion note • Tachycardia Tension Pneumothorax • Cyanosis • Displaced Trachea • Distended neck veins
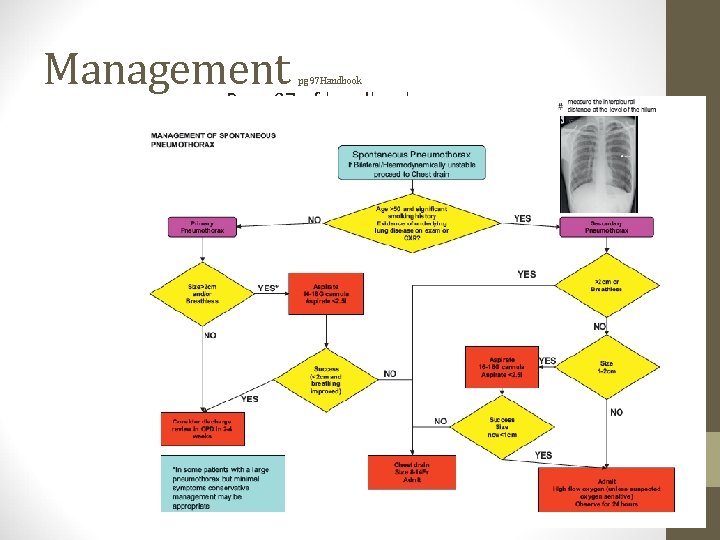
Management pg 97 Handbook • Page 97 of handbook

Chest Drain Insertion • Not required for most patients • Should only be performed under guidance from experienced ED staff • Use the triangle of safety

Acute Cardiogenic Pulmonary Oedema • Cardiogenic (or hydrostatic) pulmonary oedema caused by an elevated pulmonary capillary pressure from left-sided heart failure • Most commonly due to an acute ischaemic event • Other causes include acute AR, MR, Tamponade, RAS, AKI • Iatrogenic

Signs • • Acutely dyspnoeic Sweaty Distressed/ agitated Cough with frothy sputum Tachycardia Elevated JVP Widespread crackles throughout chest

Management • • • ABC apply 02 ECG if acute STEMI refer for PCI give frusemide Bloods including Tn. T ABG BNP Drugs-Frusemide, Nitrate infusion ? Low dose diamorphine, Consider CPAP

ICU • If patient not responding to treatment persistant severe hypoxaemia despite CPAP and appropriate medical management • Need for Ultrafiltration • Periarrest • Ensure Cardiology team also involved

Pulmonary Embolism • Pulmonary embolism is a condition in which one or more emboli, usually arising from a blood clot formed in the veins (or, rarely, in the right heart), are lodged in and obstruct the pulmonary arterial system. • This results in reduced gas exchange of the affected lung tissue, causing hypoxaemia and a reduction in cardiac output. • Large or multiple emboli may result in hypotension, syncope, shock, and sudden death.

Signs and Symptoms • • • Pleuritic chest pain Shortness of breath Palpitations Leg swelling Dizziness Collapse

Management Suspect PE Examination Wells Score-high(>6) CTPA Med/low -D-dimer: if elevated CTPA Treatment dose enoxaparin unless contraindicated. PESI score to decide if suitable for outpatient management If score greater than 85 admit medically. If negative find alternative diagnosis

Lifethreatening PE • • Call senior ED staff Associated with collapse Severe hypoxia Lifethreatening arrhythmia Severe Hypotension despite fluid resuscitation Call ICU team Alteplase 50 mg thrombolysis

Any Questions? . .
- Slides: 36