Breathing Pattern Dysfunction Sarah Butler Physiotherapist NZRSI June

Breathing Pattern Dysfunction Sarah Butler Physiotherapist NZRSI June 2018

“Breathing which is unable to perform its various functions efficiently for the needs of the individual at that time” Courtney R, The functions of breathing and its dysfunctions and their relationship to breathing therapy (2009) International journal of osteopathic medicine 12(3), 78 -85

History Mid 1800 s: ‘The Vapours’ 1871: Da Costa’s syndrome; Irritable heart 1918: Effort Syndrome / Soldiers heart 1933: Metabolic ; “A common affliction of sedentary town dwellers” 1935: Neurosis 1976: Physiological basis 2016: Multi factorial

Prevalence in Adults • • • USA GP practise: 10% General population: 5 -11% Asthma: 30% Anxiety sufferers: 83% Female: Male ratio: 7: 1 – 2: 1 26. 9% children with Ex induced asthma found to have Ex Induced BPD and not asthma
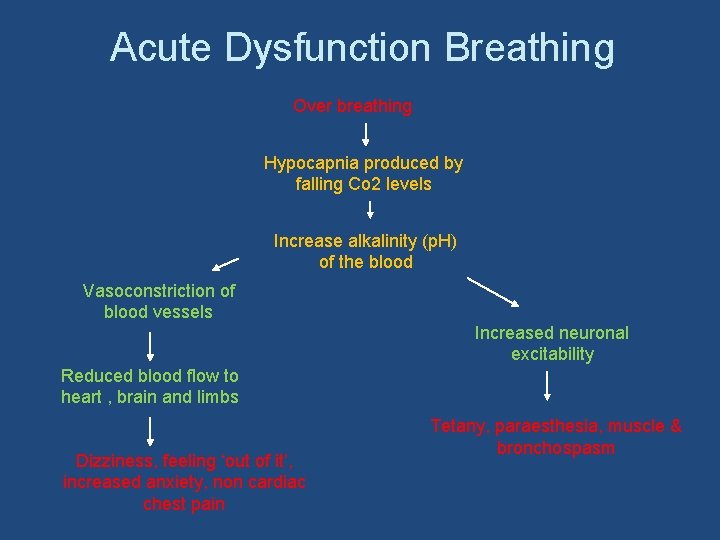
Acute Dysfunction Breathing Over breathing Hypocapnia produced by falling Co 2 levels Increase alkalinity (p. H) of the blood Vasoconstriction of blood vessels Increased neuronal excitability Reduced blood flow to heart , brain and limbs Dizziness, feeling ‘out of it’, increased anxiety, non cardiac chest pain Tetany, paraesthesia, muscle & bronchospasm

Chronic Dysfunctional Breathing HV for a few hours+; CO 2 (acid) is expelled & blood becomes more alkaline Kidneys retain acid and excrete more bicarbonate to stabilise p. H balance p. H returns to false, fragile equilibrium but bicarbonate levels are low N breathing difficult; Hyperventilation needs to continue to maintain p. H as much of the bicarbonate buffer has gone. Therefore returning to normal breathing is difficult. N Breathing feels insufficient, requiring person to persist with BPD to try to maintain feeling of equilibrium

Common adult symptoms • • Chest pain Feeling tense Blurred vision Dizzy spells Feeling confused Faster or deeper breathing Short of breath Tight feelings in chest • • Bloated feeling in stomach Tingling fingers Unable to breathe deeply Stiff fingers or arms Tight feelings round mouth Cold hands or feet Palpitations Feeling of anxiety

Typical BPD symptoms in Teens • Hard to breath in (or out) • Paraesthesia / anaesthesia in muzzle area, hands and feet • Feeling dizzy, ‘out of it’ • Tremor / muscle spasm • Palpitations / chest pain • SOB at rest • Poor sleep

Assessment • Nijmegen Questionnaire 23/64 - Validated • Breath hold following normal exhalation (N=25 -30 sec, most BPD pts < 10— 12 sec) • Assessment of comorbidities; Particularly Cardiac, Respiratory and Psychological • Assessment of ‘simple fixes’ • Assessment of ‘other factors’

‘Quick Fix’ Treatments • Regular food & fluid intake • Clear nose • Minimize stimulants • Regular exercise • Screen time • Stressors • Good sleep habits

Breathing and Food • Strong link between BPD and anxiety • Limiting caffeine & alcohol in susceptible individuals • Increasing evidence to show high glucose levels may increase panic/BPD in susceptible people

Breathing and Food • Hypocapnia and hypoglycaemia = reduced cerebral blood flow • Effects of hypocapnia on EEG = much more significant during periods of hypoglycaemia

ENT • Nose - Triggers a relaxed diaphragmatic breathing pattern MUST BE CLEAR

Breathing and Sleep • • • Fixed bed time routine Screen time Screen free bedroom Breathing practise ‘ 20 Min’ rule

Other factors to consider….

Breathing and Progesterone • BPD more common in women • Associated with rise in progesterone on day 22 which stimulates respiratory drive - increase minute volume - increases sensitivity of CO 2 receptors in the brain; urge to breath • Progesterone high through out pregnancy
Abdominals and BPD • Weak abdominals • Hyper mobility • Dyspraxia

Abdominals and BPD Strong abdominals can = corseting - diaphragmatic movement - Pilates - Gym - Growing up in Lycra

Breathing and Sport

Treatment

Progression of breathing re training • • Beach pose Supine or side lying Sitting Standing Walking Running All of the above with talking
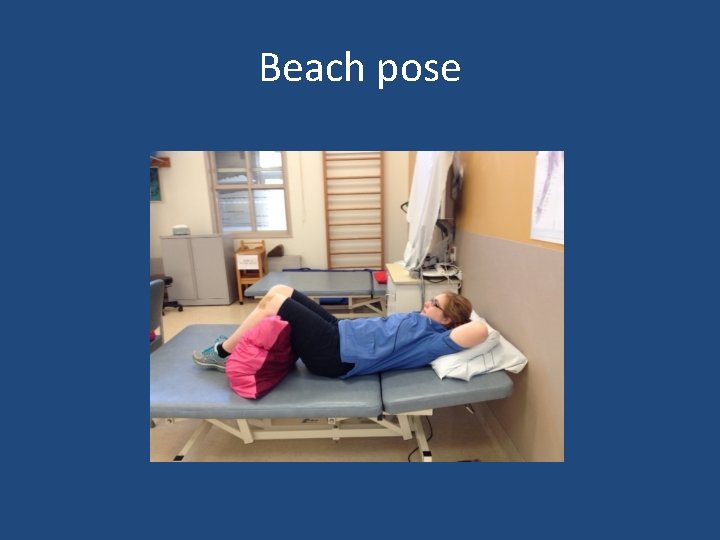
Beach pose

‘Specialist’ Treatments • Correct breathing pattern in supine/ side lying/ sitting/ standing and moving; - Nose V mouth - Inspiration V expiration - Expiratory pause - Respiratory rate • Trunk posture, strength & stretch • Management of anxiety

Basic breathing exercise • • • Lying on your back supported by pillows, place one hand on your upper abdomen and one on your upper chest Take a slow, normal breath in through your nose Feel your abdomen moves up gently as you breathe in and your upper chest should remain relaxed Then you breath out comfortably with your abdomen moves down gently. Practice this for 10 minutes, twice a day

Progression • Slow breathing rate down, aiming for 12 -14 b/min as you feel more comfortable • Practice the exercise in a sitting position or standing position • Practice 1 -2 minutes/ h Changing disordered breathing pattern takes time, particularly if you have been doing this for a while. Be patient and keep practising

Sometimes it’s ok if the only thing you did today was breathe

References 1. 2. 3. 4. 5. 6. 7. 8. 9. King, J. (1988). Hyperventilation - a therapist point of view : discussion paper. [Hypervent]. Journal of the Royal Society of Medicine, 81, 532 -536 Chaitow, L. (2004). Breathing pattern disorders, motor control, and back pain. Journal of Osteopathic Medicine, 7(1), 34 -41. Courtney, R. (2009). The functions of breathing and its dysfunctions and thier relationship to breathing therapy. International Journal of Osteopathic Medicine, 12(3), 78 - 85. Humphriss, R. L. , Baguley, D. M. , Andersson, G. , & Wagstaff, S. (2004). Hyperventilation in the vestibular clinic; use of the Nijmegen score. Clinical Otolaryngol, 29, 232 -237. Gilbert, C. (2005). Better Chemistry Through Breathing: The story of Carbon Dioxide and How It Can Go Wrong. Biofeedback, 33(3), 100 -105. Lum, L. (1975). Hyperventilation: the tip of the iceberg. Journal of PSychsomatic Research, 19, 375 -383. Chaitow, L. , Bradley, D. , & Gilbert, C. (2002). Multidisciplinary approaches to breathing disorders (first ed. ): Churchill Livingstone. Bradley, D. (2012). Hyperventilation Syndrome, Breathing Pattern disorders and how to overcome them (20 ed) Random House. Van Dixhoorn, J. , Folgering, H. , (2015) The Nijmegen questionnaire and dysfunctional breathing. European Respiratory Journal Open Res, 1: 00001 -2015. DOI : 10. 1183/23120541. 00001 -2015
- Slides: 27