BREATHE PULMONARY REHAB What is pulmonary rehabilitation PR

BREATHE PULMONARY REHAB

What is pulmonary rehabilitation (PR) According to NICE (2010) PR is: • An MDT programme of care for patients with chronic respiratory impairment • Individually tailored • Designed to optimise the individual’s physical and social performance and autonomy • Physical training, disease education, nutritional, psychological and behavioural intervention.

Who is appropriate for Breathe? • Confirmed diagnosis of a chronic respiratory disease • Functionally disabled by respiratory disease (MRC Dyspnoea Score > 3) • Cardiovascularly stable • Compliant with clinical management

Aims of Breathe • Increase exercise tolerance & functional ability • Reduce/control dyspnoea & disability • Improve quality of life • Promote self management & independence • Promote long term commitment to exercise • Reduce hospital admissions & cost to the NHS

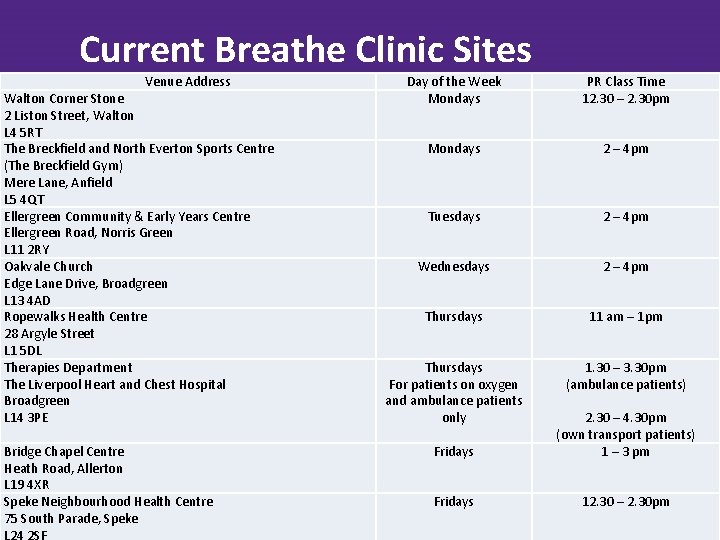
Current Breathe Clinic Sites Venue Address Walton Corner Stone 2 Liston Street, Walton L 4 5 RT The Breckfield and North Everton Sports Centre (The Breckfield Gym) Mere Lane, Anfield L 5 4 QT BODY COPY Ellergreen Community & Early Years Centre Ellergreen Road, Norris Green L 11 2 RY Oakvale Church Edge Lane Drive, Broadgreen L 13 4 AD Ropewalks Health Centre 28 Argyle Street L 1 5 DL Therapies Department The Liverpool Heart and Chest Hospital Broadgreen L 14 3 PE Bridge Chapel Centre Heath Road, Allerton L 19 4 XR Speke Neighbourhood Health Centre 75 South Parade, Speke L 24 2 SF Day of the Week Mondays PR Class Time 12. 30 – 2. 30 pm Mondays 2 – 4 pm Tuesdays 2 – 4 pm Wednesdays 2 – 4 pm Thursdays 11 am – 1 pm Thursdays For patients on oxygen and ambulance patients only 1. 30 – 3. 30 pm (ambulance patients) 2. 30 – 4. 30 pm (own transport patients) 1 – 3 pm Fridays 12. 30 – 2. 30 pm

Core Principles of Breathe 1. Exercise 2. Self-Management Education
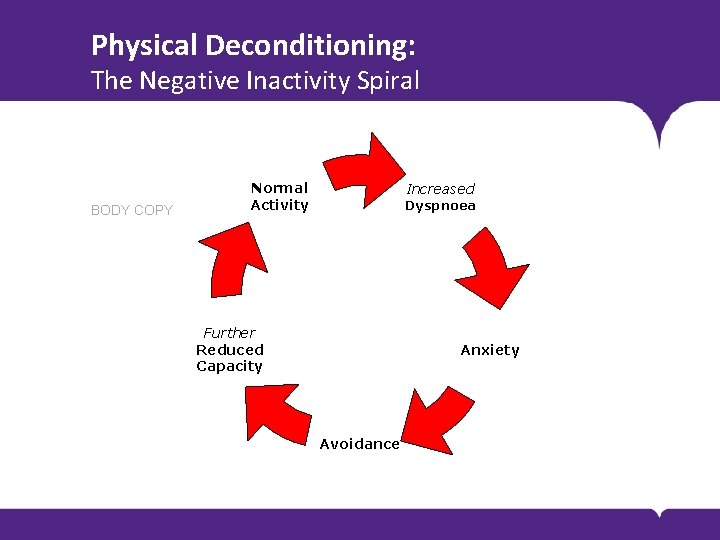
Physical Deconditioning: The Negative Inactivity Spiral BODY COPY Normal Activity Increased Dyspnoea Further Reduced Capacity Anxiety Avoidance
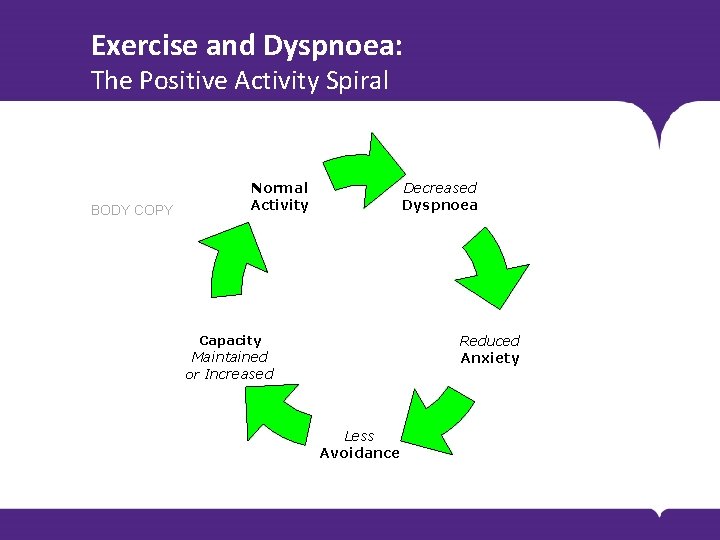
Exercise and Dyspnoea: The Positive Activity Spiral BODY COPY Normal Activity Decreased Dyspnoea Reduced Anxiety Capacity Maintained or Increased Less Avoidance

What’s Different about BREATHE? Traditional PR pathway+ Evidence based MECC – Brief Interventions Flexible programme (access, t/f, on hold scheme) Bespoke modules of care - pods Provide bespoke CRD education and exercise Hands on intervention Link in with other health/social care/voluntary services to ensure true holistic care • Stepping stone for further progress for life style changes • Ongoing support and access to care • •

BREATHE HEP Format • Endurance training for functional gains • Strength training for specific activities • Respiratory muscle training and chest clearance routine • Progressive exercise prescription


Aims of Self-Management Education • • • Know and understand their condition Understand what different medication are for Know how and when to use different medication Know what is “normal” for them in terms of symptoms Can recognise when symptoms are worsening Know what to do when symptoms are worsening Know who to contact and how to contact them when symptoms are worsening Know when to call for emergency help Know what support is available

How Do We Know BREATHE Works • Patient testimonials • Outcome measures

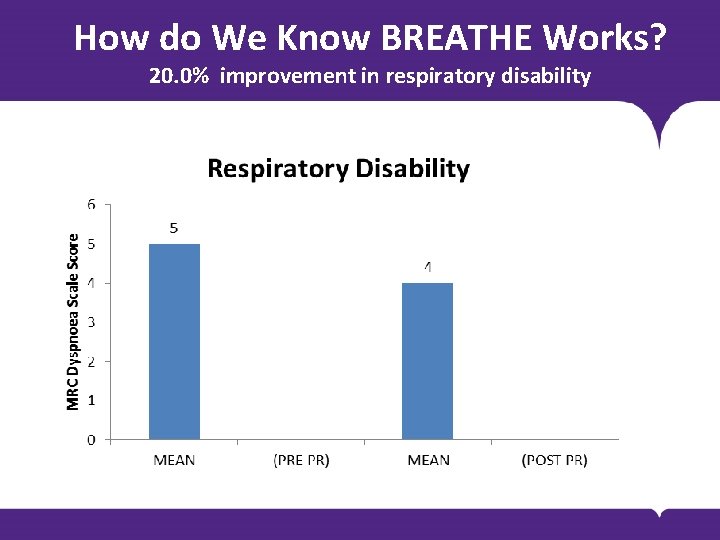
How do We Know BREATHE Works? 20. 0% improvement in respiratory disability BODY COPY
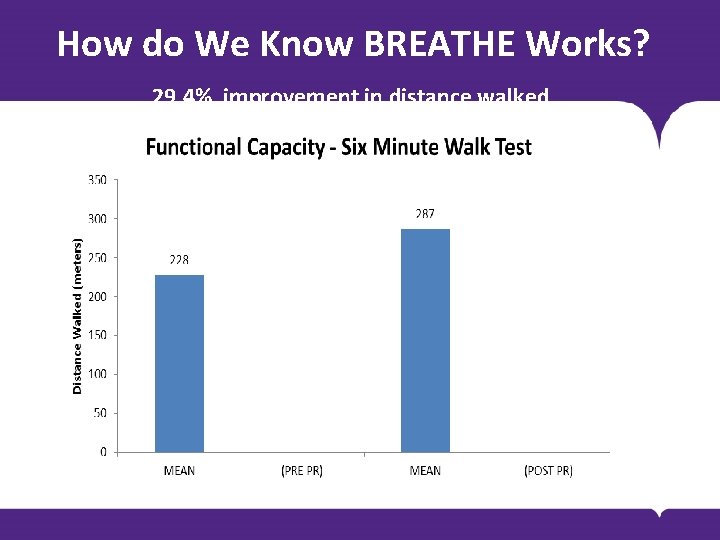
How do We Know BREATHE Works? 29. 4% improvement in distance walked BODY COPY
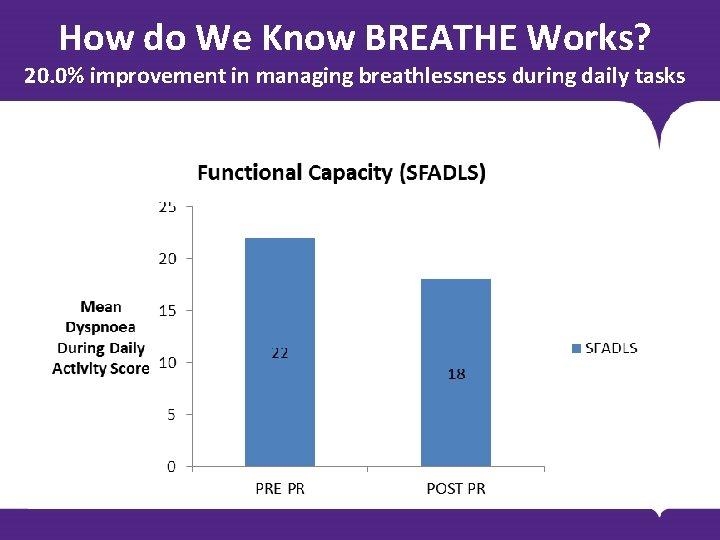
How do We Know BREATHE Works? 20. 0% improvement in managing breathlessness during daily tasks BODY COPY
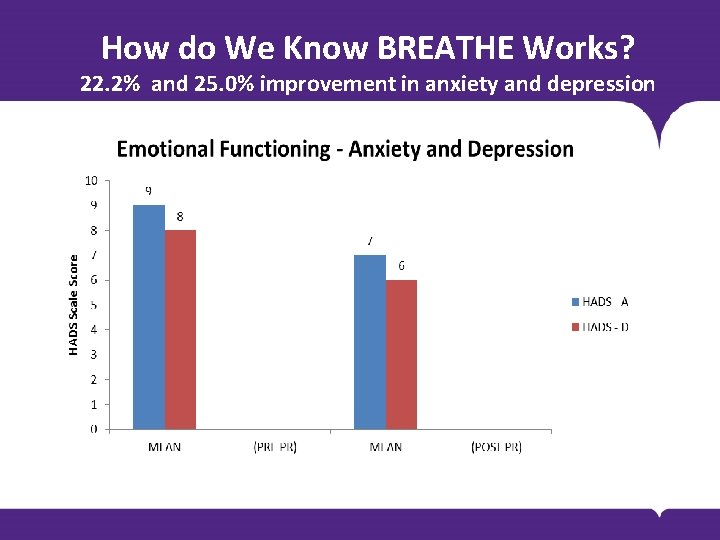
How do We Know BREATHE Works? 22. 2% and 25. 0% improvement in anxiety and depression BODY COPY
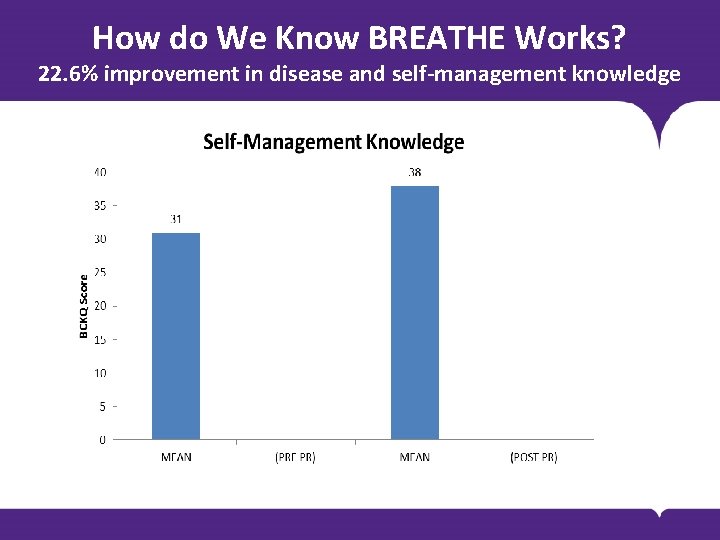
How do We Know BREATHE Works? 22. 6% improvement in disease and self-management knowledge BODY COPY

Thank You for Your Time and Attention Any Questions? Contact the BREATHE team on: 0151 600 1950 or Breathe. lhch@nhs. net
- Slides: 21